Health and Social Care Btec TECH Level 12

Health and Social Care Btec TECH Level 1/2 ◦ ◦ Current focus is Public Exam 8: 45 7 th February Some students have coursework to complete There are many resources on students google classroom. Please email aurelieelder@varndean. co. uk with any questions.

Top Tips: Exam Strategy ◦ Part A ◦ Read the Case Study. ◦ Highlight the key pieces of information. ◦ Identify the factors then use your knowledge to EXPLAIN how it affects.
◦ Top most tip: Before answering any question make sure you look at the following information; ◦ What is the command word? In most cases it’s ‘EXPLAIN’ so you need to provide a factor and give further information about how it effects the individual. Your answer should use the word ‘so’ or ‘this means’. ◦ How many marks are given and how many pieces of information are needed? 2 marks need a cause and effect EXPLAIN type answer. ◦ What content is required? Is it two positive factors affecting health and wellbeing? , if so you need to recall Learning Aim A and pick out examples from the information on your case study.
Section A – Question 1 ◦ Explain factors that could have a negative effect on your client’s health and wellbeing ◦ 8 Marks (1 mark for factor + 1 mark for explanation) ◦ Explain factors that could have a positive effect on your client’s health and wellbeing ◦ 4 Marks (1 mark for factor + 1 mark for explanation) Ho w m a fac tors ny ? r o tive e? i s Po ativ neg What is the impact? ? PIES

What should you revise? Factors affecting health and wellbeing. ◦ Definition of health and wellbeing ◦ Physical and lifestyle factors ( genetic inheritance, ill health, diet, exercise, substance use, personal hygiene) ◦ Social, emotional and cultural (Social interactions – supportive / unsupportive, stress, willingness es to seek help or access services) n o ich e case h W o th ◦ Economic factors (Financial resources) ly t dy? p p a stu ◦ Environmental factors (pollution, noise, housing, location) ◦ The impact of life events relating to relationship changes and changes in life circumstances Expected (school, moving house, starting work, parenthood, marriage, retirement) and Unexpected (sudden death, accident, injury, redundancy, exclusion)
Section A – Question 2 ◦ Explain effects a the recent life event could have had on them ◦ 6 Marks (1 mark for effect + 1 mark for explanation) Wh at i s eve the lif e nt? Expected or unexpected? r o tive e? i s Po ativ neg PIES What is the impact? ? it d i d Who t? affec

Top Tips ◦ Question 2 gives even more information about the individual you need to read carefully and highlight/underline again. ◦ The question requirements change here as you must EXPLAIN factors how they impact on the case studies’ social and emotional wellbeing. ◦ Use the terminology from the textbook glossary as much as possible. ◦ Keep answers clear and precise i. e. 1 factor and its impact per section – don’t waffle! No marks awarded for repetition.
Exam strategy for Section B – Question 3 ◦ Read the new information given about data and lifestyle Peak Flow? ? ? Blood Pressure? ? ? BMI? ? ? Pulse rate? ? ? Lifestyle data? ? ? Smoking / Alcohol / Inactive lifestyles

What to revise for Section B – Question 3? ◦ B 1: Physiological indicators ◦ Physiological indicators that are used to measure health: ◦ - pulse (resting and recovery rate after exercise) ◦ - blood pressure ◦ - peak flow ◦ - body mass index (BMI). ◦ Using published guidance to interpret data relating to these physiological indicators ◦ The potential significance of abnormal readings: risks to physical health ◦ B 2: Lifestyle indicators ◦ Interpretation of lifestyle data, specifically risks to physical health associated with: ◦ smoking ◦ alcohol consumption ◦ inactive lifestyles
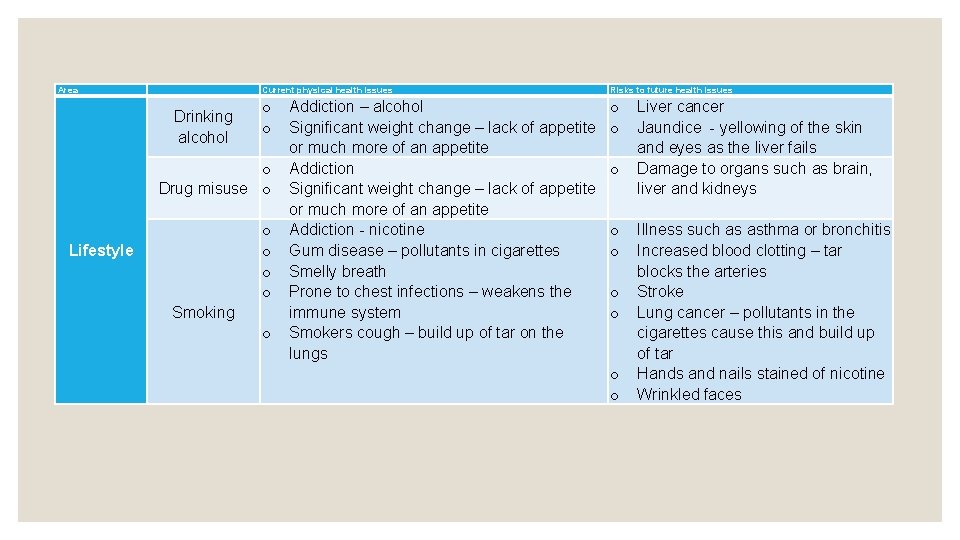
Area Current physical health issues Drinking alcohol o o o Drug misuse o o o Lifestyle Smoking o Addiction – alcohol Significant weight change – lack of appetite or much more of an appetite Addiction - nicotine Gum disease – pollutants in cigarettes Smelly breath Prone to chest infections – weakens the immune system Smokers cough – build up of tar on the lungs Risks to future health issues o o o o o Liver cancer Jaundice - yellowing of the skin and eyes as the liver fails Damage to organs such as brain, liver and kidneys Illness such as asthma or bronchitis Increased blood clotting – tar blocks the arteries Stroke Lung cancer – pollutants in the cigarettes cause this and build up of tar Hands and nails stained of nicotine Wrinkled faces
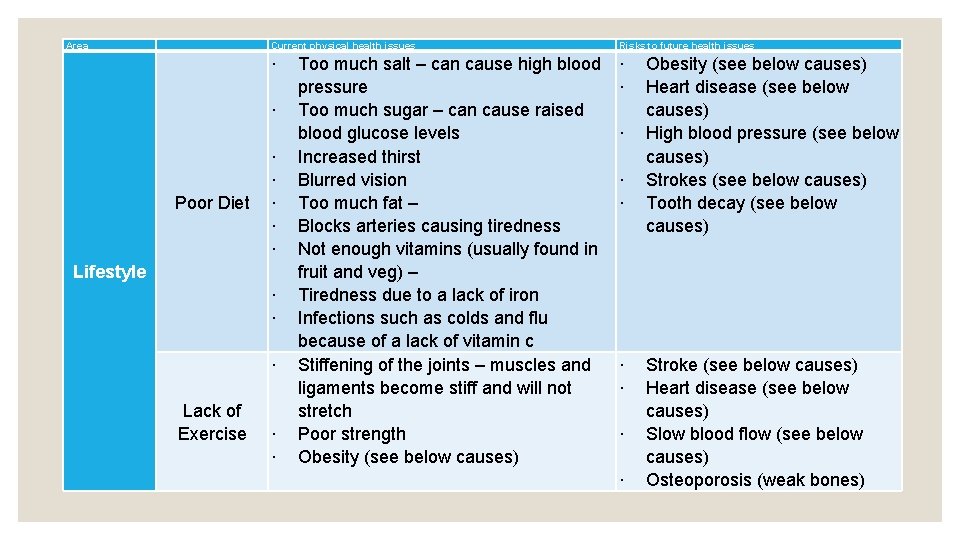
Area Current physical health issues Risks to future health issues ∙ ∙ Poor Diet ∙ ∙ ∙ Lifestyle ∙ ∙ ∙ Lack of Exercise ∙ ∙ Too much salt – can cause high blood pressure Too much sugar – can cause raised blood glucose levels Increased thirst Blurred vision Too much fat – Blocks arteries causing tiredness Not enough vitamins (usually found in fruit and veg) – Tiredness due to a lack of iron Infections such as colds and flu because of a lack of vitamin c Stiffening of the joints – muscles and ligaments become stiff and will not stretch Poor strength Obesity (see below causes) ∙ ∙ ∙ ∙ Obesity (see below causes) Heart disease (see below causes) High blood pressure (see below causes) Strokes (see below causes) Tooth decay (see below causes) Stroke (see below causes) Heart disease (see below causes) Slow blood flow (see below causes) Osteoporosis (weak bones)
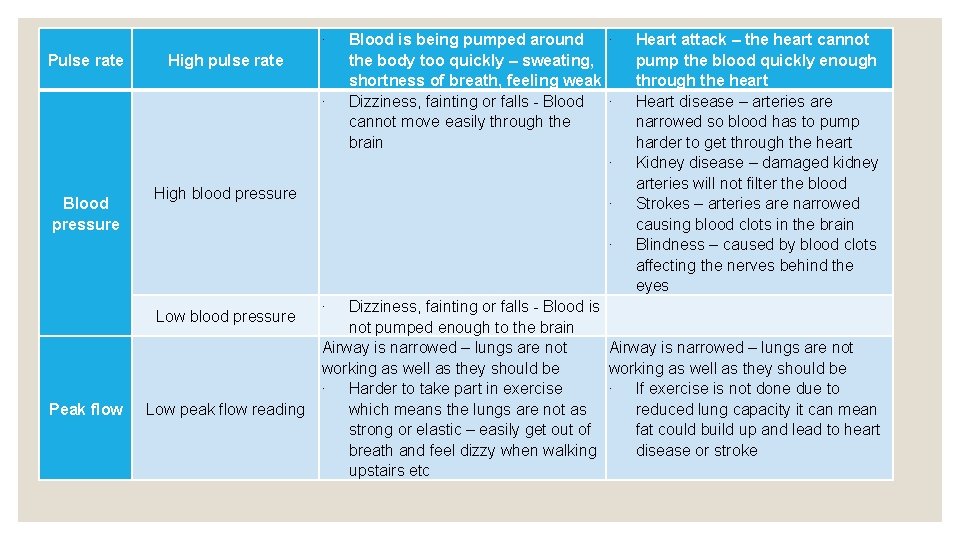
∙ Pulse rate High pulse rate ∙ Blood pressure High blood pressure Blood is being pumped around ∙ the body too quickly – sweating, shortness of breath, feeling weak Dizziness, fainting or falls - Blood ∙ cannot move easily through the brain ∙ ∙ ∙ Low blood pressure Peak flow Low peak flow reading ∙ Heart attack – the heart cannot pump the blood quickly enough through the heart Heart disease – arteries are narrowed so blood has to pump harder to get through the heart Kidney disease – damaged kidney arteries will not filter the blood Strokes – arteries are narrowed causing blood clots in the brain Blindness – caused by blood clots affecting the nerves behind the eyes Dizziness, fainting or falls - Blood is not pumped enough to the brain Airway is narrowed – lungs are not working as well as they should be ∙ Harder to take part in exercise ∙ If exercise is not done due to which means the lungs are not as reduced lung capacity it can mean strong or elastic – easily get out of fat could build up and lead to heart breath and feel dizzy when walking disease or stroke upstairs etc
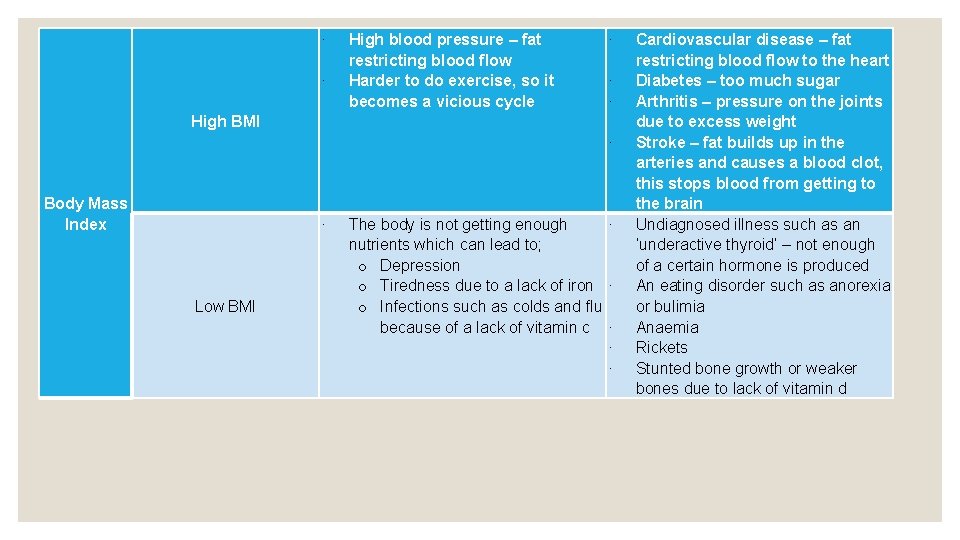
∙ ∙ High blood pressure – fat restricting blood flow Harder to do exercise, so it becomes a vicious cycle ∙ ∙ ∙ High BMI ∙ Body Mass Index ∙ Low BMI The body is not getting enough ∙ nutrients which can lead to; o Depression o Tiredness due to a lack of iron ∙ o Infections such as colds and flu because of a lack of vitamin c ∙ ∙ ∙ Cardiovascular disease – fat restricting blood flow to the heart Diabetes – too much sugar Arthritis – pressure on the joints due to excess weight Stroke – fat builds up in the arteries and causes a blood clot, this stops blood from getting to the brain Undiagnosed illness such as an ‘underactive thyroid’ – not enough of a certain hormone is produced An eating disorder such as anorexia or bulimia Anaemia Rickets Stunted bone growth or weaker bones due to lack of vitamin d

Section B – Question 3
Top Tips ◦ Use the subheadings given and ensure your answer addresses exactly what is being asked for i. e. current health and future health risks ◦ There are 12 marks available and 6 subsections so each one requires two marks worth of writing ◦ Don’t waffle – you may have lots to say but be selective and stay within the space given – it’s plenty for full marks - and still no marks for repetition!

Exam Strategy: Part B – Health and Wellbeing Improvement Plan ◦ Health and Wellbeing Plans ◦ The importance of a person-centred approach that takes into account an individual’s needs, wishes and circumstances. ◦ Information to be included in plan: ◦ recommended actions to improve health and wellbeing ◦ short-term (less than 6 months) and long-term targets ◦ appropriate sources of support (formal and/or informal). This is your fourth set of information to read so you must go back and re-cap on the first three sections to be able to answer this next question

Question 4 - Read the new information ◦ ◦ Design a health and wellbeing improvement plan for your client. ◦ Your plan should: ◦ • DESCRIBE three recommended actions ◦ For each action: ◦ Set short-term LESS THAN 6 months ◦ Set a long-term target MORE THAN 6 months ◦ Give one source of support for each recommended action ◦ • Explain how the source of support will help your client achieve the target

What to revise: Appropriate sources of support. ◦ Formal Support ◦ Informal Support GP, Pharmacist, Dentist (Primary services) Family Help groups such as quit smoking, weight watchers, alcohol anonymous. Friends Neighbours Hospital departments (Secondary services). Hospice care. Physiotherapist, dietician. Voluntary groups : N I LA hey P X E ill t w W HO elp? ? ? h
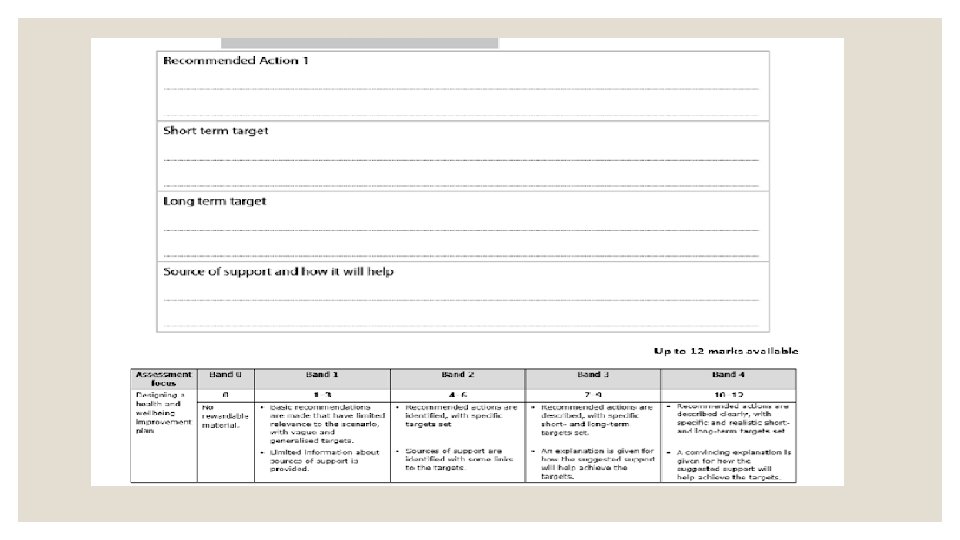


Question 4 Examples ◦ The client has a high BMI ◦ Recommended action – To reduce BMI to between 18. 5 – 24. 9 ◦ Short term target – to decrease the amount of takeaways you eat to a maximum of 1 per week within 4 weeks ◦ Long term target – To join a weight loss class such as Slimming World or Weight Watchers for as long as it takes to reduce BMI, and longer if necessary ◦ Sources of support – Ask for an appointment with the nurse at your GP surgery. She will give you advice and information about how to lose weight healthily

Question 4 Examples ◦ The client is a heavy smoker ◦ Recommended action – To quit smoking ◦ Short term target – To reduce the number of cigarettes being smoked each day from 20 to 5 within 4 weeks ◦ Long term target – to have quit smoking completely within 8 weeks ◦ Sources of support - Go to your GP and tell them you want help to quit smoking. The doctor or nurse will be able to provide you with advice and also nicotine patches or even medication to help you to quit smoking completely

Question 4 Examples ◦ The client drinks a lot of alcohol ◦ Recommended action – To reduce alcohol consumption ◦ Short term target – Within 4 weeks, reduce the days that you are drinking alcohol to only at the weekends ◦ Long term target – Within 6 -12 months, find a hobby that you can take up that doesn’t involve alcohol and that you do at least once a week, for example playing football ◦ Sources of support – your nurse at your GP surgery can give you information on how alcohol may be affecting your body and can give you advice and strategies to help you to cut down

Exam strategy: Question 5 - Health and wellbeing improvement plans. ◦ Give a rationale for your plan that explains how it takes into account their needs, wishes and circumstances. Be specific to your case study ◦ Go back to the description. Think about the case study. Think in reality what that person is like. ◦ What do they want? ◦ What don’t they want? ◦ Link back to your short and longterm targets. ◦ Do the things you suggest match up with their life/style/circumstances?

Exam strategy: Top Tips ◦ ‘Rationale’ means the reasons behind the plan i. e. why the actions and targets will help improve health and wellbeing whilst also taking into account the person’s needs, wishes and circumstances (i. e. a person-centred approach) ◦ This is an extended writing task, but that doesn’t mean that you can’t break down the marks into sections. ◦ There were three parts to your plan in question 4, so you need to justify each in turn with enough for 3+ marks for each ◦ You can link to why you have given the short and long-term targets as well as the source of support you identified

Exam strategy: Question 6 – Health and Wellbeing Plans ◦ Describe possible obstacles that they may face when trying to follow your health and wellbeing improvement plan and suggest how these could be minimised. ◦ Choose from: emotional/psychological, time constraints, availability of resources, unachievable targets, lack of support, specific to the individual (disability or addiction) ◦ Barriers to accessing services (geographical, financial, physical, culture, language, psychological)

Exam strategy: Top Tips ◦ Question 6 asks you to ‘describe’, which means you need to give a detailed account of the barrier and then make a logical suggestion for minimising it ◦ Again, this is an extended writing task, so you need to have a plan for breaking your response down. ◦ For 8 marks it would make sense to describe 4 barriers with a suggestion for minimising each ◦ Try to use the terms from the spec to demonstrate your knowledge

◦ What to revise? Learning Aim C - Health and wellbeing improvement plans ◦ Obstacles to implementing plans ◦ emotional/psychological – lack of motivation, low self-esteem, acceptance of current state ◦ time constraints – work and family commitments ◦ availability of resources – financial, physical, e. g. equipment ◦ unachievable targets – unachievable for the individual or unrealistic timescale ◦ lack of support, e. g. from family and friends ◦ other factors specific to individual – ability/disability, addiction ◦ barriers to accessing identified services.

In All Questions ◦ Refer to the case study. ◦ Refer to the data. ◦ Make it specific to the data you have. ◦ Read the question ◦ Read it again! ◦ Highlight important information in the question and the case study ◦ ‘EXPLAIN’ – this is because… ◦ This could lead to…. ◦ The impact of this could be…. . ◦ By doing this they would be able to…. . Because………. .

Case Studies ◦ Apply students own knowledge! ◦ Do you use a gym? ◦ Have you shared problems with a friend? The following slides have Case studies to practice. Their are further Case Study and Exam style papers on google classroom.

Pamela Jones (68) ◦ You are a health care assistant at your local health centre. You have been asked to assess the health and wellbeing of one of the service users. Read the information and then answer the questions below: ◦ Location ◦ Pamela Jones is 68 years old. She lives in a two-bedroom bungalow in a small, countryside village. Her bungalow is located at the top of a steep hill. ◦ Medical history ◦ Pamela has suffered with bad hips for several years. She has recently had a hip replacement operation. Since her operation, she has noticed an improvement in her mobility. ◦ Family, friends and social interactions ◦ The district nurse visits Pamela three times a week. This is to change the dressing on her hip and check her health after the operation. Pamela employs a gardener to help assist with the maintaining of her garden. Pamela’s next door neighbour visits each week to look after her finances, organise medical appointments and to assist with any household tasks that Pamela is unable to do. However, none of these visitors are Pamela’s age and she misses the company of people her own age. ◦ Day-to-day life ◦ Pamela now uses a walking stick to help her move around her bungalow and is so far managing to be independent. She is able to do her day-to-day chores, like getting herself dressed, maintaining her hygiene and completing her own washing. However, Pamela is struggling to make her own food due to her being unable to stand for long periods of time. Therefore she has started eating a lot of takeaways and fast food. She finds asking for help difficult because she is a very proud woman. Pamela prides herself on being independent.

Jordan Pilkington (58) ◦ Location: Jordan Pilkington is 58 years old. He lives in a flat in a busy city centre on a high up floor. Jordan has good transport links around his flat. Jordan lives with his daughter who is 10 and is disabled. ◦ Medical history: Jordan has just had both of his knees replaced so is currently using crutches. Last year Jordan had contracted pneumonia which has left him with occasional breathing difficulties when he is under strain. ◦ Family, Friends and social interactions: Jordan is the sole carer for his daughter and is a single parent. His own parents help him with her childcare throughout the week however they are aging and Jordan feels that it is unfair to constantly as for help. Jordan attends a snooker club once a week with his friends but is unable to go at the moment due to his knee operation. ◦ Day-to-day life: Jordan is unemployed as he is the sole carer of his daughter. He is currently finding this stressful as he is on his own and his inability to walk around. He is in a lot of pain and has started taking double the daily amount of his prescribed painkillers. Jordan is finding that at the minute, he is not leaving his flat for days at a time and he is starting to become irritable towards his daughter as a result.

Susan Jones (82) ◦ Location: Susan Jones is 82 years old. She lives in a one-bedroom terraced house with a small garden and a short but steep driveway on the edge of a small town. ◦ Medical history: Susan has osteoarthritis and her mobility has recently started to deteriorate and she now uses her stick for support. ◦ Family, Friends and social interactions: An old friend comes on the bus once a fortnight to visit and to help her use her laptop, so she is able to keep organised and shop for food and other items online. Her niece visits her every fortnight and does jobs like keeping the garden tidy. Her neighbour, who is 73 years old, is often on hand if she needs any day-to-day practical help but she has quite a busy life with her own family and friends. Susan has no children and most of her friends have either died, in a care home or unable to drive or travel. She is often very lonely. ◦ Day-to-day life: Susan uses a walking stick to get around her house. She manages her steep stairs by going up sideways with her back to the handrail. She now finds day-to-day life difficult. For example, getting dressed, washing and cooking. She does not like to ask visitors for help as she does not want to be a burden.
- Slides: 32