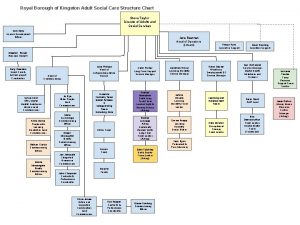
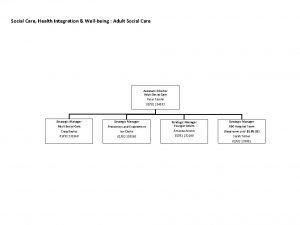
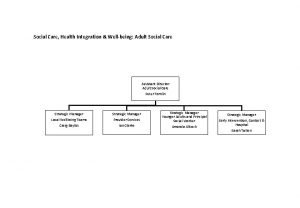
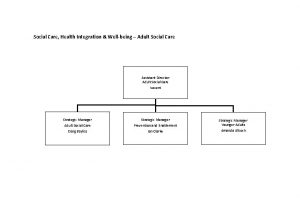
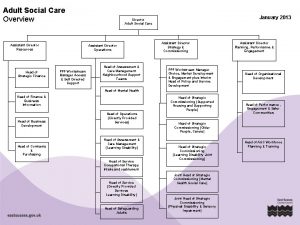
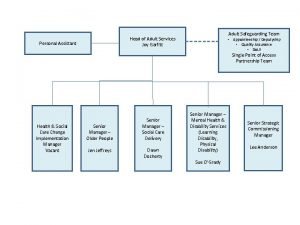
Health Adult Social Care Paul Little Head of



















- Slides: 22

Health & Adult Social Care Paul Little Head of Strategic Commissioning Suffolk County Council - Adult and Community Services

Today we I will be covering: How Health and Social Care services are working together to deliver the best services we can for the people of Suffolk The progress we are making in West Suffolk How we plan to develop things in the future

The Health and Social Care System • Acute Services – clinical care delivered in and from Hospitals • Community Health Care – GPs, Occupational Therapy, District Nurses, Physio Therapy etc. • Social Care Services – Home Care, Specialist Support Services, Supported Housing, Day, evening and weekend services, Care Homes and Social Work

The Health and Social Care System Our Aims are: • To make sure people have access to the right services for their needs • Prevent unnecessary hospital admissions • Help people to fully recover independence following hospital treatment • Enable people to managed their own care and wellbeing • To provide Integrated Care

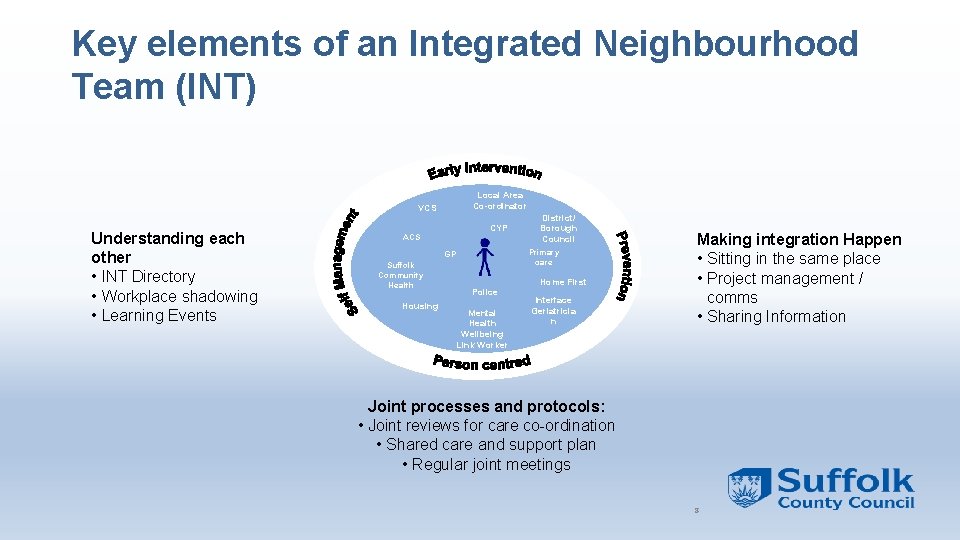
What do we mean by Integrated Care At its heart, it can be defined as an approach that seeks to improve the quality of care for individual patients, customers and carers by ensuring that partners understand the needs of the local population and services are well co-ordinated around their needs. The Integrated Neighbourhood Team is a multi-agency team, committed to this approach 5

Working Together – Integrated Neighbourhood Teams The Background: • Health and Social Care have fully signed up to integrated care providing better health and care system for people – but this is not easy • The Health and Care Review created a shared view of a future integrated system • The vision and service model has been signed up to by all partners, and has informed the Suffolk Better Care Fund Plan • Partners are now committed to delivering the new model of care – Connect Sudbury and Connect East Ipswich were the forerunners for the new system • Connect is strapline for Integration of health and care services

The Connect Programme A community based approach for a new way of working Care Act 2014 Introduces new responsibilities for LAs • Prevention • Information & advice • The provision of high quality, appropriate services LAs need to; • Consider services & resources in their area e. g. voluntary & community • Work with other partners, like the NHS Community Resilience INT Suffolk Health & Wellbeing Board Health & SC Review • People Manage their own health + care • Communities are supportive places to live • Health + care system is co-ordinated • Interventions are matched to people’s needs INT Vision • Promote + enable self-care • Prevent ill health + crisis intervention • Provide access to local multi agency services

Key elements of an Integrated Neighbourhood Team (INT) Local Area Co-ordinator VCS Understanding each other • INT Directory • Workplace shadowing • Learning Events CYP ACS Primary care GP Suffolk Community Health Housing District/ Borough Council Police Mental Health Wellbeing Link Worker Home First Interface Geriatricia n Making integration Happen • Sitting in the same place • Project management / comms • Sharing Information Joint processes and protocols: • Joint reviews for care co-ordination • Shared care and support plan • Regular joint meetings 8

Impact of INTs Patients / clients and their family carers will experience: • • Improved managed or coordinated care with fewer handoffs and service duplication Consistency in how care is delivered Improved local delivery in their own home or usual place of residence Improved empowerment through delivery of shared decision making, integrated focus of self management and reablement The health and care system will experience: • • Improved collaboration and communication Better understanding of pathways and operational processes Reduction in administration Local ownership of integrated delivery 9

INTs Progress so far West • Sudbury – Home. First, OTs, LAC all hotdesking in ACS offices. OT joint working practices established. SCH & ACS delivery of joint training. Active links with VCS in place. • Forest Heath – Mildenhall Joint OT meetings and case management in place. Connect Wednesdays events held in Mildenhall District Council Offices & Newmarket Hospital • Haverhill - INT established, work started on directory, ‘Lunch and Learn’ sessions scheduled, INT engaged with Social Prescribing project • Bury Rural – Care co-ordinator appointed to aid MDT performance , work started on directory, ‘Lunch and Learn’ sessions scheduled • Bury Town – INT established, Frail elderly project launched, work started on directory, ‘Lunch and Learn’ sessions scheduled

People being Discharged from West Suffolk Hospital Sometimes people are delayed from leaving hospital (“delayed transfers of care”) Delays at West Suffolk Hospital are much lower than other hospitals and the situation is improving with a 62% reduction in delays (comparing September and latest figures available for Jan) The primary reason for delays is usually getting people the support they need so that they can go home Delays can also arise when arranging 24 hr care for someone when they are the responsibility of Social Care. This is one reason why we are doing so much work to improve the care market Delays also arise through delays in arranging appropriate health care to support people post a period in hospital

What is being done about these delays – A Planned Response Part of the reason for the delays arise from the volume of people being admitted to hospital in the first place Health and Social Care working together to develop Integrated Neighbourhood Teams (INTs) who can more readily recognise emerging escalating needs and address these, rather than allow needs to escalate to a point where hospital admission is required: Prevention is the key

What is being done about these delays – The Reactive Response Integrated Early Intervention Team (EIT) provided by West Suffolk Hospital but including nursing staff, therapists, social workers, support workers and voluntary sector support EIT responds to crisis situations that might lead to a hospital admission taking referrals for people at home or who have attended A&E, with a view to avoiding hospital admission, stabilising the situation and drawing in ongoing care and support where necessary

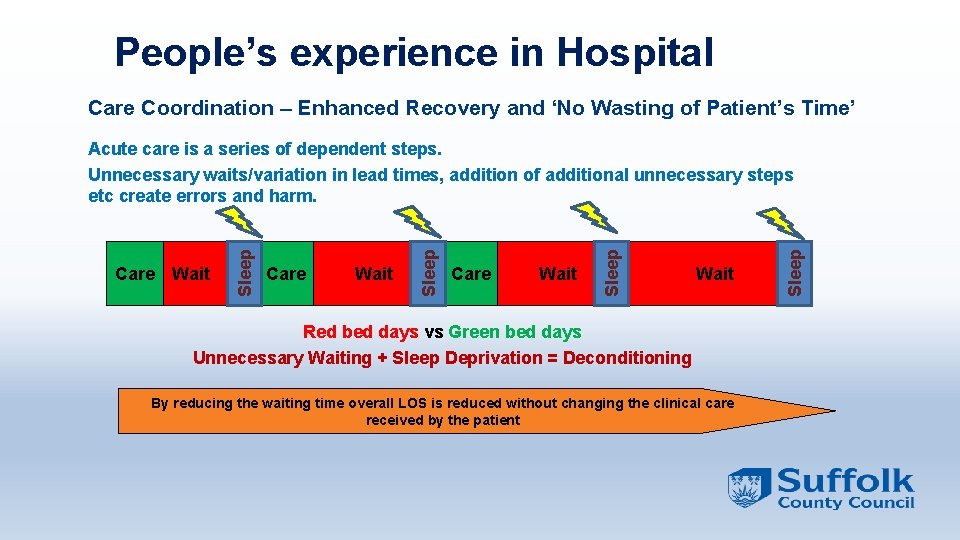
People’s experience in Hospital Care Coordination – Enhanced Recovery and ‘No Wasting of Patient’s Time’ Care Wait Red bed days vs Green bed days Unnecessary Waiting + Sleep Deprivation = Deconditioning By reducing the waiting time overall LOS is reduced without changing the clinical care received by the patient Sleep Wait Sleep Care Wait Sleep Acute care is a series of dependent steps. Unnecessary waits/variation in lead times, addition of additional unnecessary steps etc create errors and harm.

Discharge to Assess – A new Approach Hospital is the wrong place to assess people’s ongoing needs: • It takes time to do properly • People’s presenting needs in a hospital bed are different (and often higher) than those outside of hospital • Glastonbury Court as a “step-down facility”: 24 beds to facilitate people being able to be discharged from hospital to recover, regain optimum independence with a view to being able to return home • Home First (Suffolk County Council’s reablement service) working more closely together with local health care services (see INTs) to support people to return home

The Discharge to Access Appproach 16

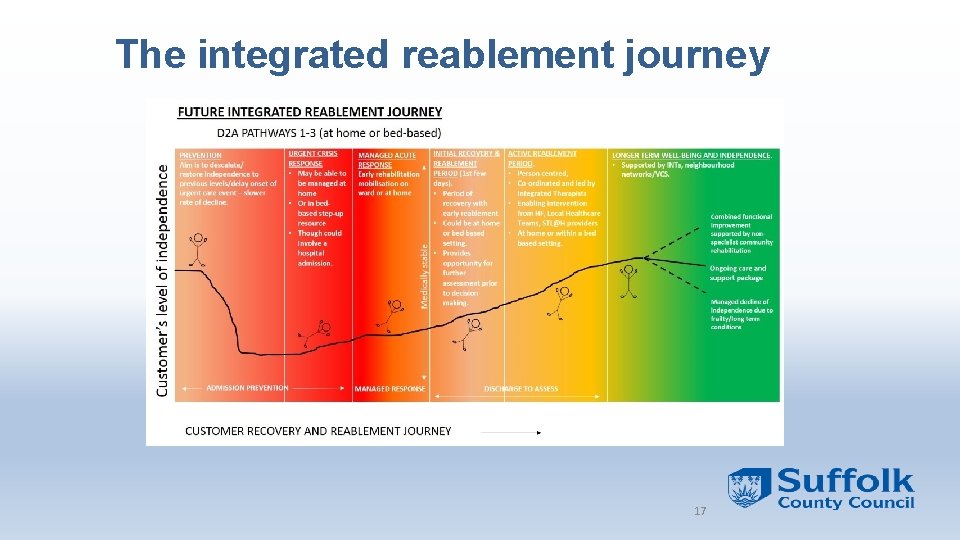
The integrated reablement journey 17

Supporting People to go home Discharge to Assess Glastonbury Court – Step Down facility Development of Home First domiciliary care service (“provider of last resort”) with increased capacity Support to Live at Home Programme development Support to Go Home service development (joint funded between West Suffolk Hospital and ACS)

Our approach to the Home Care Market • We are committed to ensuring there is guaranteed good quality and reliable care for customers at all times and across all areas that allow them to remain independent for as long as possible • We are working together with all interested parties to develop solutions that work for and across the whole system • We are increasing the rates we pay providers for care

Support to Live at Home

Support to Live at Home

Support to Live at Home
 Health and social care values unit 2
Health and social care values unit 2 Stit sheffield
Stit sheffield Adult social care kingston
Adult social care kingston Health and social care component 3
Health and social care component 3 1 little 2 little 3 little indians
1 little 2 little 3 little indians 1 little 2 little 3 little indian
1 little 2 little 3 little indian Primary, secondary, tertiary care
Primary, secondary, tertiary care Bakersfield adult school
Bakersfield adult school Northern nevada adult mental health
Northern nevada adult mental health Unit 6 work experience in health and social care level 3
Unit 6 work experience in health and social care level 3 Unit 2 health and social care
Unit 2 health and social care Unit 2 working in health and social care past papers
Unit 2 working in health and social care past papers Physiological disorders and their care
Physiological disorders and their care Pearson btec level 3 health and social care
Pearson btec level 3 health and social care Ocr health and social care level 3
Ocr health and social care level 3 Ocr health and social care level 3
Ocr health and social care level 3 Robert vischer empathy theory disadvantages
Robert vischer empathy theory disadvantages Example of appraisal in health and social care
Example of appraisal in health and social care Ocr cambridge national health and social care
Ocr cambridge national health and social care Gm health and social care partnership
Gm health and social care partnership Argyle theory of communication in health and social care
Argyle theory of communication in health and social care Health and social care level 3 unit 5
Health and social care level 3 unit 5 Health and social care unit 2
Health and social care unit 2