HEAD TO TOE FRONT LINE ANTIBIOTIC CHOICES FOR

HEAD TO TOE: FRONT LINE ANTIBIOTIC CHOICES FOR PRIMARY CARE INFECTIONS A Ben Appenheimer MD Infectious Diseases University of Iowa Hospitals and Clinics alpheus-appenheimer@uiowa. edu

CONFLICTS OF INTEREST • No disclosures

GOALS AND OBJECTIVES • Discuss first line antibiotic therapies for common infections seen in clinic and the hospital • Review Infectious Disease Society of America (IDSA) guidelines for these infections • Outline practical approaches to these infections • Discuss areas of focus for antimicrobial stewardship, including the role of penicillin skin testing

TOPICS • Skin and Soft Tissue Infections • Respiratory Tract Infections • Rhinosinusitis • Bronchitis • Community-acquired pneumonia • Clostridium difficile • Dealing with reported penicillin allergies

SKIN AND SOFT TISSUE INFECTIONS Clin Infect Dis (2014) 59 (2): e 10
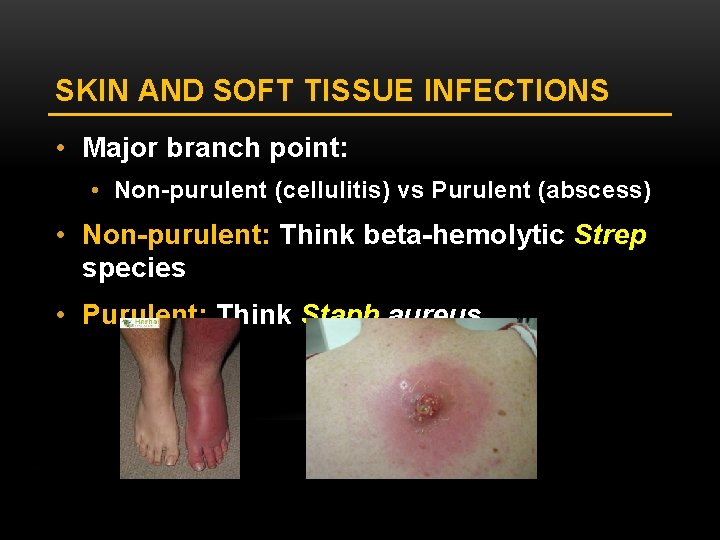
SKIN AND SOFT TISSUE INFECTIONS • Major branch point: • Non-purulent (cellulitis) vs Purulent (abscess) • Non-purulent: Think beta-hemolytic Strep species • Purulent: Think Staph aureus
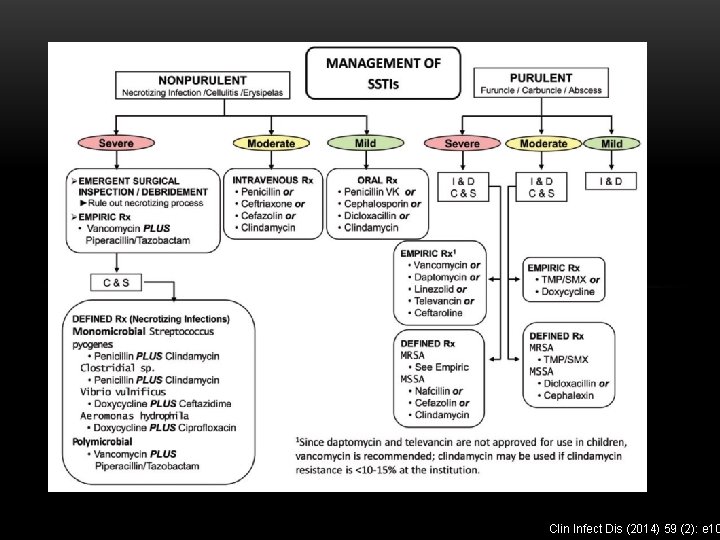
Clin Infect Dis (2014) 59 (2): e 10
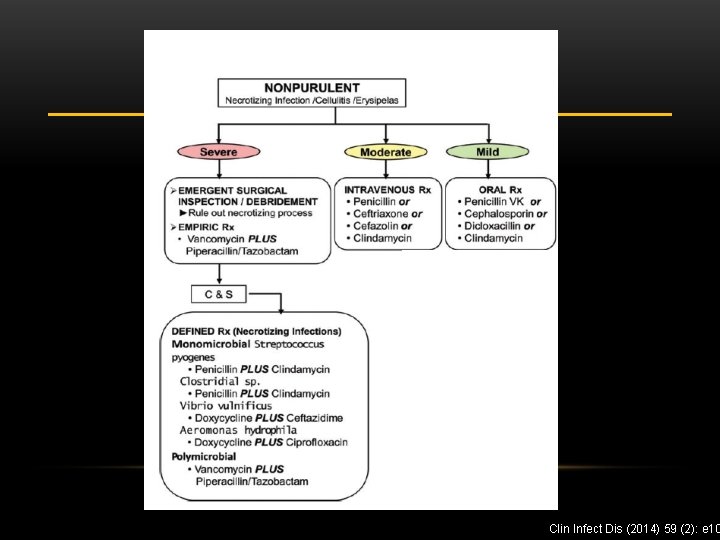
Clin Infect Dis (2014) 59 (2): e 10
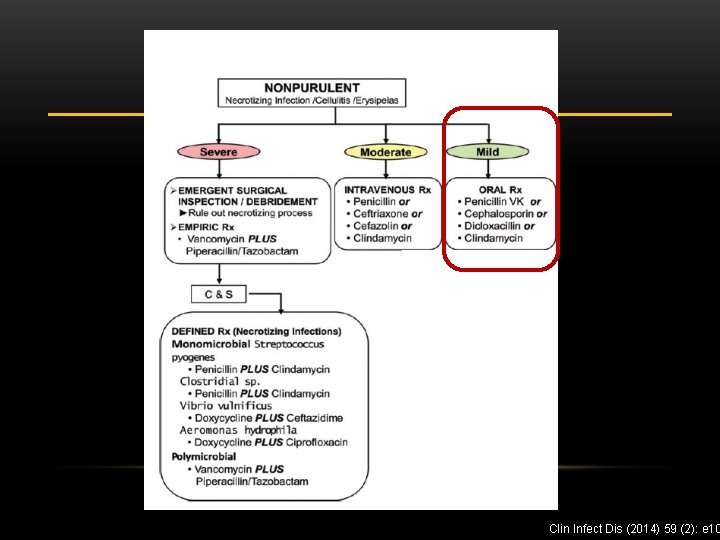
Clin Infect Dis (2014) 59 (2): e 10
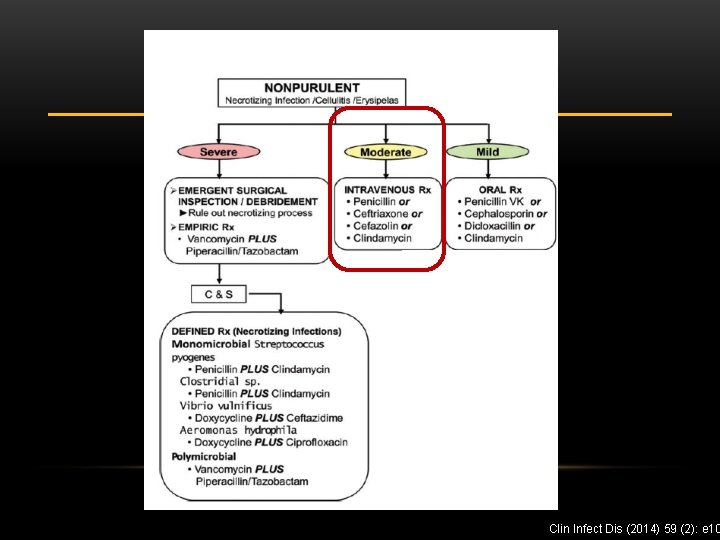
Clin Infect Dis (2014) 59 (2): e 10
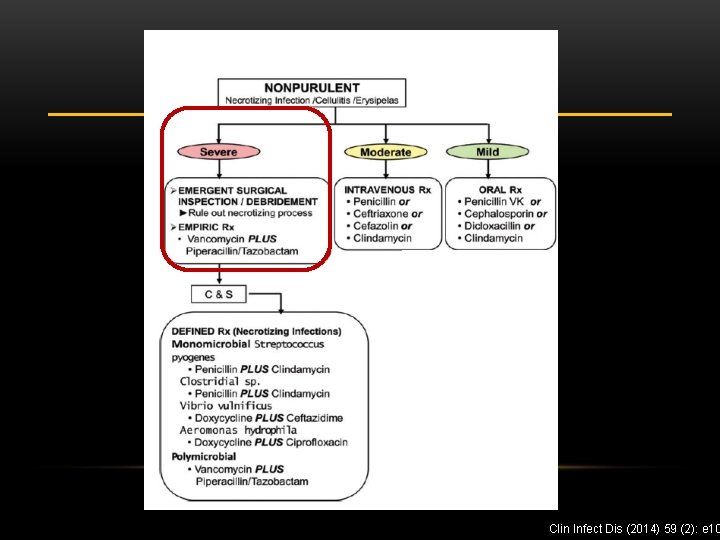
Clin Infect Dis (2014) 59 (2): e 10

NON-PURULENT CELLULITIS: MY APPROACH • Focus mainly on beta-hemolytic Strep unless there are reasons to suspect otherwise • Oral options • Amoxicillin 500 mg TID • Penicillin VK 500 mg QID • Cephalexin 500 mg QID • IV options • IV penicillin 18 -24 million units via continuous infusion • Cefazolin 2 g every 8 hours Clin Infect Dis (2014) 59 (2): e 10
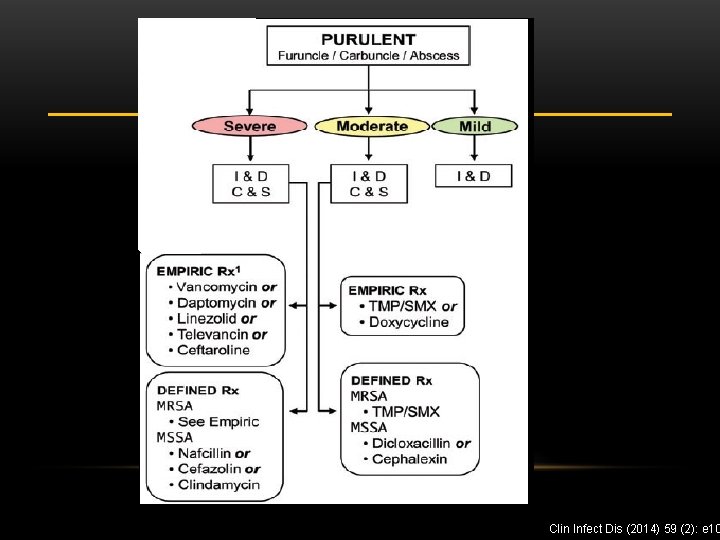
Clin Infect Dis (2014) 59 (2): e 10

N Engl J Med 2016; 374: 823 -832 Acad Emerg Med. 2009 May; 16(5): Clin Infect Dis (2014) 59 (2): e 10 -e 5
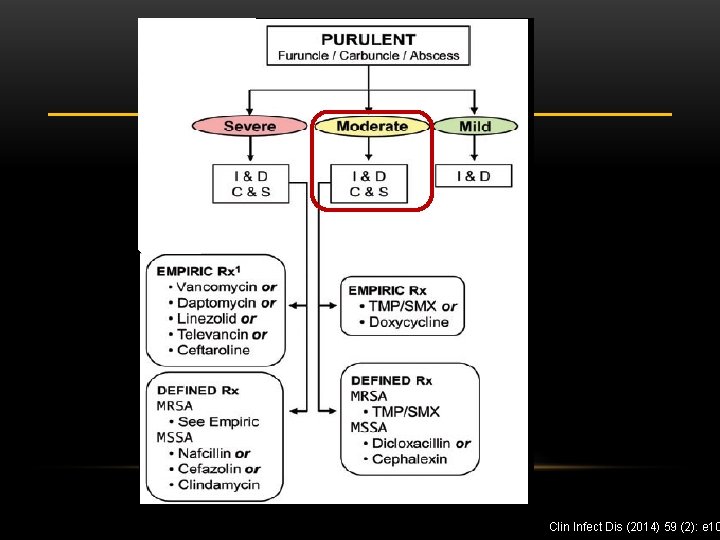
Clin Infect Dis (2014) 59 (2): e 10
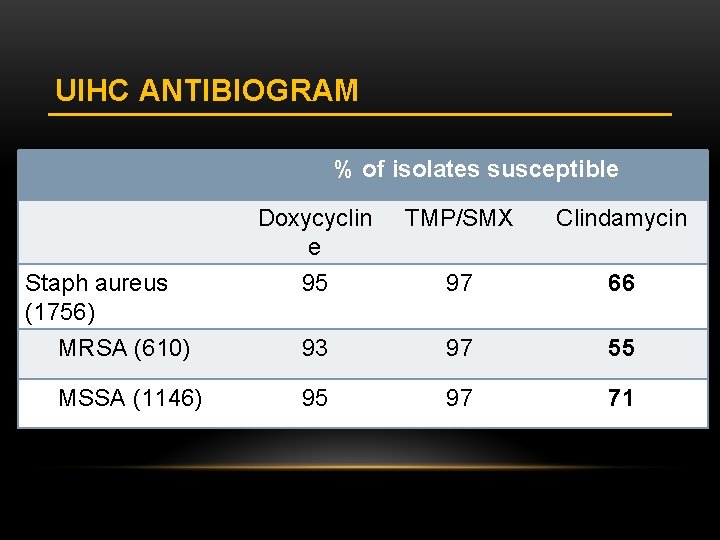
UIHC ANTIBIOGRAM % of isolates susceptible Doxycyclin e 95 TMP/SMX Clindamycin 97 66 MRSA (610) 93 97 55 MSSA (1146) 95 97 71 Staph aureus (1756)
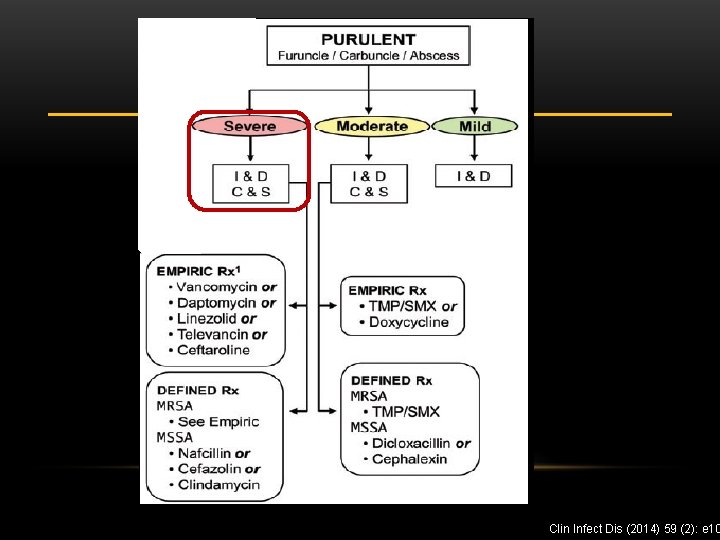
Clin Infect Dis (2014) 59 (2): e 10

RECURRENT SKIN AND SOFT TISSUE INFECTIONS • Nonpurulent • Overall recurrence rate is high (8 -20%) • Identify predisposing conditions • With 3 -4 episodes/year, consider prophylactic therapy targeting Strep • Penicillin 500 mg PO BID, amoxicillin 250500 mg PO BID, or IM penicillin q 2 -4 wk • Clindamycin 150 -300 mg QD, Erythromycin 250 mg PO BID Clin Infect Dis (2014) 59 (2): e 10

RECURRENT SKIN AND SOFT TISSUE INFECTIONS • Purulent • Look for local cause (i. e. pilonidal cyst, hidradenitis, or foreign material) • Consider 5 day decolonization with BID mupirocin, daily chlorhexidine, and daily decontamination of personal items • If occurs in childhood, consider sending for evaluation of neutrophil disorders Clin Infect Dis (2014) 59 (2): e 10

SKIN AND SOFT TISSUE INFECTIONS: MISCELLANEOUS • Duration: 5 days minimum, based on resolution of signs/symptoms of infection • Some erythema can remain after infection is treated • Keep affected area elevated • Can consider short course of prednisone for non-diabetics • We do not routinely do this Clin Infect Dis (2014) 59 (2): e 10

RESPIRATORY TRACT INFECTIONS • Rhinosinusitis • Bronchitis • Community-acquired pneumonia

RHINOSINUSITIS • Major branch point • Viral vs Bacterial • Interesting numbers • Estimate 2 -10% bacterial, 90 -98% viral • 81% prescribed antibiotics, 70% respond spontaneously • Clues suggesting bacterial cause (antibiotics indicated) • Persistent symptoms for 10 days without improvement • Severe symptoms for 3 -4 consecutive days • Fever > 39, purulent drainage early • Double sickening Clin Infect Dis (2012) 54 (8): e 72 -e 1

ANTIBIOTIC CHOICES IN RHINOSINUSITIS • First line • Amoxicillin/clavulanate 875 mg/125 mg BID • Consider high dose (2 g BID) in certain circumstances • High endemic rates of penicillin resistance (>10%), severe infection (Fever >39 o. C), age <2, age >65, recent hospitalization, recent antibiotic use, immunocompromised, daycare • Alternative agents (i. e. for penicillin allergy) • Doxycycline 100 mg BID • Respiratory fluoroquinolones (moxifloxacin or levofloxacin) • Duration Clin Infect Dis (2012) 54 (8): e 72 -e 1

ANTIBIOTIC CHOICES IN RHINOSINUSITIS • Antibiotics to avoid • Macrolides (azithromycin, clarithromycin) • High rates of resistance in Strep pneumo • TMP/SMX • Resistance of Strep pneumo and H. influenza up to 40% • Oral 3 rd generation cephalosporins (cefdinir, cefpodoxime) • Variable rates of resistance for Strep pneumo Clin Infect Dis (2012) 54 (8): e 72 -e 1

BRONCHITIS • Interesting numbers • 90% are viral, ~67% receive antibiotics • ~25% of patients have self-treated an URI with antibiotics in the past year • Usefulness of antibiotics • No significant change in outcomes • Decreases cough by ½ day over an 8 -10 day period • Number needed to harm 16. 7 Cochrane Database Syst Rev. 2014 Mar 1; (3): CD 000245. doi: 10. 1002/14651858. CD 000245. pub 3 Am Fam Physician. 2010 Dec 1; 82(11): 134

BRONCHITIS • Where antibiotics may have benefit • COPD Exacerbation • Frail, elderly, multiple comorbidities • Excluded from many of the studies • Pertussis • Decrease in shedding, no change in symptoms BMJ 2007; 335: 982 Am Fam Physician. 2010 Dec 1; 82(11): 134

COMMUNITY-ACQUIRED PNEUMONIA Clin Infect Dis (2007) 44 (Supplement_2): S 27 -S 72 Am Fam Physician. 2016 Nov 1; 94(9): 69

COMMUNITY-ACQUIRED PNEUMONIA • How to treat • Stratified by where treatment is occurring • Outpatient • Healthy • Some comorbidities • Inpatient ward • ICU Clin Infect Dis (2007) 44 (Supplement_2): S 27 -S 72

TREATMENT OF COMMUNITY ACQUIRED PNEUMONIA Location First Line Second Line Outpatie nt Otherwise healthy • Azithromycin or • Doxycycline Recent ABX or comorbidities 1 • Moxifloxacin/levofloxacin or • High-dose (HD) beta lactam 2 + azithro Inpatient General Floor • Moxifloxacin/levofloxacin or • Ceftriaxone 3 + either azithro or doxy HD beta-lactam + doxy ICU - no risk • Ceftriaxone + either moxi or factors levo - MRSA RF • Add vancomycin or linezolid - Known • Anti-Ps. A beta-lactam + cipro or 1. Chronic heart, lung, liver, or renal disease; diabetes, alcoholism, malignancy, asplenia, immunocompromised state Ps. A 4 levo 2. High-dose beta lactam = amoxicillin 1 g TID or amox/clav 2 g BID 3. Could also use cefotaxime or ampicillin Clin Infect Dis (2007) 44 (Supplement_2): S 27

COMMUNITY ACQUIRED PNEUMONIA: MISCELLANEOUS • When to narrow • After established microbiologic diagnosis • After blood and sputum cultures are negative, can remove coverage for MRSA and Ps. A if they were being covered • Transition to oral therapy • Hemodynamically stable, improving clinically, normally functioning GI tract • No need to monitor inpatient Clin Infect Dis (2007) 44 (Supplement_2): S 27 -S 72

COMMUNITY ACQUIRED PNEUMONIA: MISCELLANEOUS • Duration • Minimum of 5 days of active therapy • 48 -72 hours afebrile • < 1 sign of clinical instability • Sputum – get on all hospitalized patients with CAP • Looks for causes not covered with usual ABX • Helps identify changes in susceptibility profile for usual pathogens such as Strep pneumo

CLOSTRIDIUM DIFFICILE Infection Control and Hospital Epidemiology. Vol. 31, No. 5 (May
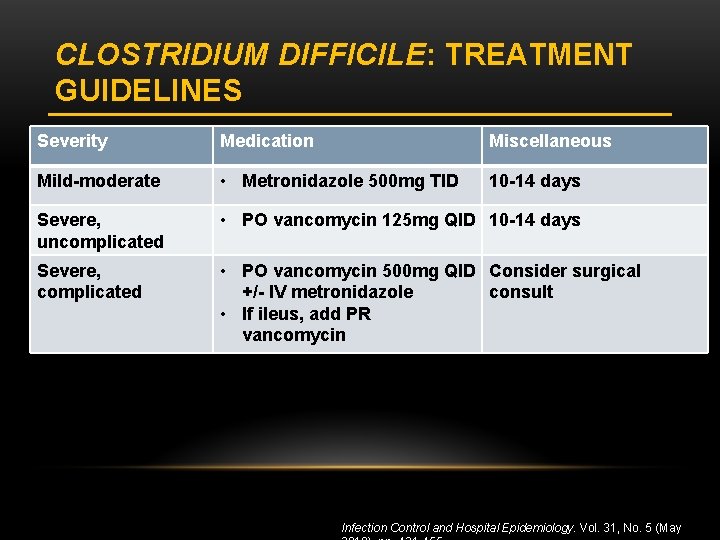

CLOSTRIDIUM DIFFICILE: TREATMENT GUIDELINES Severity Medication Miscellaneous Mild-moderate • Metronidazole 500 mg TID 10 -14 days Severe, uncomplicated • PO vancomycin 125 mg QID 10 -14 days Severe, complicated • PO vancomycin 500 mg QID Consider surgical +/- IV metronidazole consult • If ileus, add PR vancomycin Infection Control and Hospital Epidemiology. Vol. 31, No. 5 (May

CLOSTRIDIUM DIFFICILE: CURRENT GUIDELINES • Recurrent CDI • First recurrence, use same regimen as initial episode • Second recurrence • Avoid metronidazole • Risk of cumulative neurotoxicity • Consider tapered vancomycin Infection Control and Hospital Epidemiology. Vol. 31, No. 5 (May

CLOSTRIDIUM DIFFICILE: MY TAKE • Initial treatment • PO vancomycin 125 mg QID • First recurrence • PO vancomycin 125 mg QID • Second recurrence • PO vancomycin taper (125 mg QID x 14 d, 125 mg BID x 7 d, 125 mg QOD x 7 days, 125 mg every 3 days x 14 d) • Could consider fidaxomicin (very costly, less recurrences) • Third recurrence • Fecal microbiota transfer (stool transplant)

CLOSTRIDIUM DIFFICILE: MISCELLANEOUS • Do not test for cure • Can remain positive for 6 weeks • If no improvement with vancomycin • Consider alternative diagnoses • Probiotics • Unclear if there is a benefit, studies have not been homogenous The Lancet. Volume 382, Issue 9900, 12– 18 October 2013, Pages 1249– 1257 Open Forum Infect Dis. 2016 Jan 29; 3(1)
DEALING WITH PENICILLIN ALLERGIES
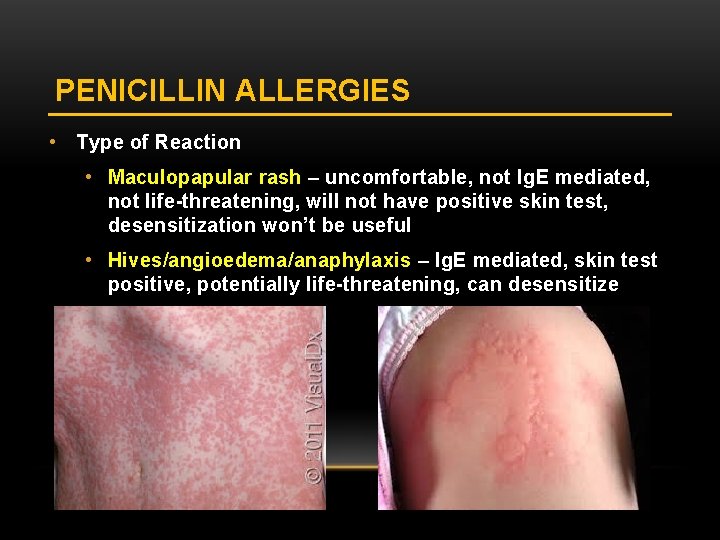
PENICILLIN ALLERGIES • Type of Reaction • Maculopapular rash – uncomfortable, not Ig. E mediated, not life-threatening, will not have positive skin test, desensitization won’t be useful • Hives/angioedema/anaphylaxis – Ig. E mediated, skin test positive, potentially life-threatening, can desensitize

PENICILLIN ALLERGIES • Importance of clarifying penicillin allergy • Allows for use of more narrow-spectrum antibiotics with better side effect profiles • Reliability of documented penicillin allergies • In preliminary studies, <1% of people who report allergy to penicillin have true Ig. E mediated allergic reaction • If patients have penicillin allergy documented, consider referring for penicillin skin testing • If negative, can safely give a trial of beta-lactam therapy

TAKE HOME POINTS • For non-purulent SSTIs, focus on covering beta-hemolytic Strep species • Use penicillin, amoxicillin, or cephalexin • For purulent SSTIs, focus on covering Staph • Use TMP/SMX or doxycycline empirically • Most cases of acute rhinosinusitis are viral and do not require antibiotics • The decision to treat should be based on duration > 10 days, severe symptoms, or ‘double-worsening’

TAKE HOME POINTS • Treatment of routine bacterial rhinosinusitis should start with amoxicillin/clavulanate • Most cases of bronchitis do not require antibiotic treatment • Antibiotic choices for community-acquired pneumonia depend on where the patient is located • If covering for MRSA, Pseudomonas, consider de-escalating if blood and sputum cultures negative

TAKE HOME POINTS • Guidelines for C diff treatment suggest metronidazole for mild-moderate infections and vancomycin for severe • Some physicians have moved towards using oral vancomycin for all cases, new guidelines are coming soon • For multiple recurrences, consider vancomycin taper or referral for fecal transplant • Patients with reported penicillin allergies should be skin tested so optimal therapy

QUESTIONS? Thank you for your attention!
- Slides: 43