Head Injury Chapter 57 Copyright 2014 by Mosby

Head Injury Chapter 57 Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Head Injury • Any trauma to the • Skull • Scalp • Brain • Traumatic brain injury (TBI) • High incidence Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Head Injury • Causes • Motor vehicle collisions • Falls • Firearm-related injuries • Assaults • Sports-related injuries • Recreational accidents • War-related injuries Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Head Injury • High potential for poor outcome • Deaths occur at three points in time after injury: 1. Immediately after the injury 2. Within 2 hours after the injury 3. 3 weeks after the injury. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • K. D. , a 33 -year-old woman, is brought by paramedics to ED following a motor vehicle collision. • She has a laceration to her forehead and bruises from her seat belt. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • She is stuporous and does not answer questions. • What is the most likely cause of her change in LOC? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Types of Head Injuries • Scalp Lacerations • External head trauma • Scalp is highly vascular → Profuse bleeding • Major complications – blood loss and infection Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Skull Fractures • Linear or depressed • Simple, comminuted, or compound • Closed or open Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Skull Fractures • Location determines manifestations. • Complications • Infections • Hematoma • Tissue damage Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
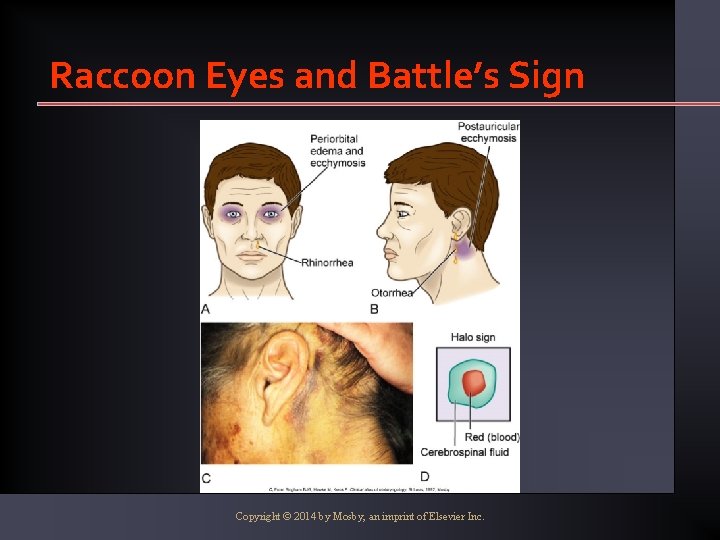
Raccoon Eyes and Battle’s Sign Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Diffuse (generalized) • Focal (localized) • Minor (GCS 13 -15) • Moderate (GCS 9 -12) • Severe (GCS 3 -8) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Diffuse Injury • Concussion • Brief disruption in LOC • Retrograde amnesia • Headache • Short duration • May result in postconcussion syndrome Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Postconcussion Syndrome • Persistent headache • Lethargy • Personality and behavior changes • Shortened attention span, decreased short-term memory • Changes in intellectual ability Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Diffuse Axonal Injury • Widespread axonal damage • Decreased LOC • Increased ICP • Decortication, decerebration • Global cerebral edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Focal Injury • Lacerations • Contusions • Hematomas • Cranial nerve injuries Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Lacerations • Tearing of brain tissue • With depressed and open fractures and penetrating injuries • Intracerebral hemorrhage • Subarachnoid hemorrhage • Intraventricular hemorrhage Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Contusion • Bruising of brain tissue • Associated with closed head injury • Can cause hemorrhage, infarction, necrosis, edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
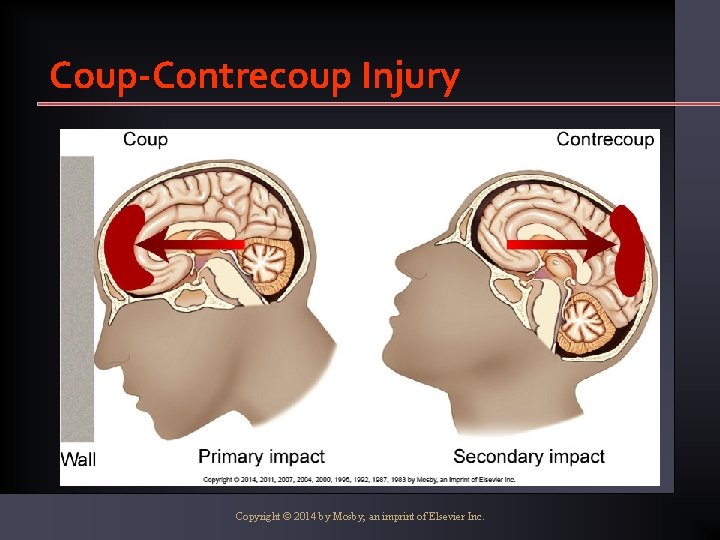
Coup-Contrecoup Injury Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Types of Head Injuries • Contusion • Can rebleed • Focal and generalized manifestations • Monitor for seizures • Potential for increased hemorrhage if on anticoagulants Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Complications • Epidural Hematoma • Bleeding between the dura and the inner surface of the skull • Neurologic emergency • Venous origin slow • Arterial origin rapid Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • An emergent CT scan on K. D. reveals an epidural hematoma. • What is an epidural hematoma? • What type of emergency treatment would you expect the health care provider to order? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Complications • Epidural Hematoma • Initial period of unconsciousness • Brief lucid interval followed by decrease in LOC • Headache, nausea, vomiting • Focal findings • Requires rapid evacuation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
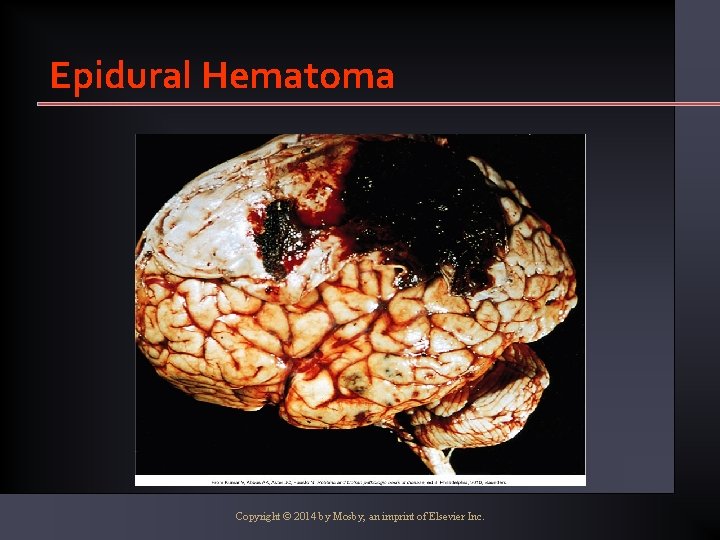
Epidural Hematoma Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Complications • Subdural Hematoma • Bleeding between the dura mater and the arachnoid • Most common source is the veins that drain the brain surface into the sagittal sinus. • Can also be arterial Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Complications • Acute Subdural Hematoma • Within 24 to 48 hours of the injury • Symptoms related to increased ICP • ↓ LOC, headache • Ipsilateral pupil dilated and fixed if severe Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Complications • Subacute Subdural Hematoma • Within 2 to 14 days of the injury • May appear to enlarge over time Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Complications • Chronic Subdural Hematoma • Weeks or months after injury • More common in older adults • Presents as focal symptoms • ↑ Risk for misdiagnosis Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
Intracerebral Hematoma • Bleeding within the brain tissue • Usually within frontal and temporal lobes • Size and location of hematoma determine patient outcome. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
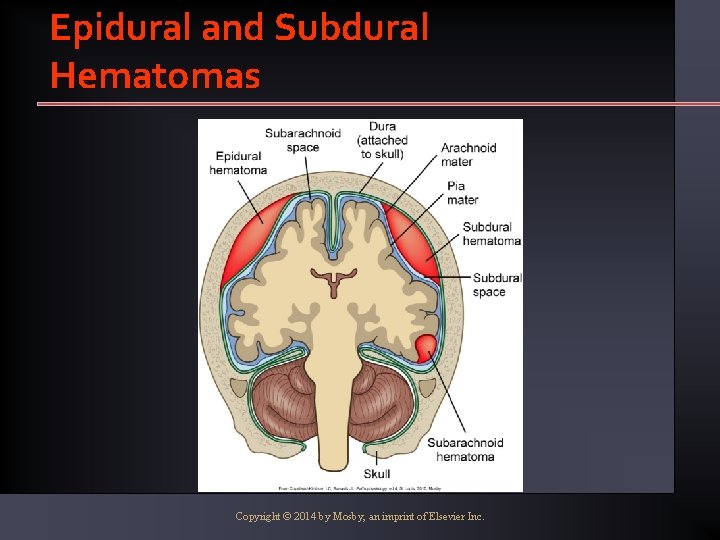
Epidural and Subdural Hematomas Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Diagnostic Studies • CT scan • Best diagnostic test to determine craniocerebral trauma • MRI, PET, evoked potential studies • Transcranial Doppler studies • Cervical spine x-ray • Glasgow Coma Scale (GCS) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • What would be the initial priority care for K. D. upon admission to the ED? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Treatment • Patent airway • Stabilize cervical spine. • Oxygen • IV access • Intubate if GCS <8. • Control external bleeding. • Remove patient’s clothing. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care Emergency Treatment • Maintain patient warmth. • Ongoing monitoring • Anticipate possible intubation. • Assume neck injury. • Administer fluids cautiously. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Treatment principles • Prevent secondary injury • Timely diagnosis • Surgery if necessary • Concussion and contusion • Observation and management of ICP Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Collaborative Care • Skull fractures • Conservative treatment • Surgery if depressed • Subdural and epidural hematomas • Surgical evacuation • Craniotomy, burr-holes • Craniectomy if extreme swelling Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Subjective Data • Past medical history • Mechanism of injury • Medications • Anticoagulants Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Subjective Data • Alcohol/drug use; risk-taking behaviors • Headache • Mood or behavioral changes • Mentation changes; impaired judgment • Aphasia, dysphasia • Fear, denial, anger, aggression, depression Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • K. D. ’s past medical history is negative except for the births of two children. • Her family denies any drug or alcohol use. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • She was not taking any anticoagulant medications. • What objective data will you assess K. D. for when she is admitted to the ICU after surgery? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Objective Data • Altered mental status • Lacerations, contusions, abrasions • Hematoma • Battle’s sign • Periorbital edema and ecchymosis • Otorrhea • Exposed brain Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Objective Data • Rhinorrhea • Impaired gag reflex • Altered/irregular respirations • Cushing’s triad • Vomiting • Bowel and bladder incontinence Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Objective Data • Uninhibited sexual expression • Altered LOC • Seizures • Pupil dysfunction • Cranial nerve deficit(s) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Objective Data • Motor deficit • Palmar drift • Paralysis • Spasticity • Posturing • Rigidity or flaccidity • Ataxia Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment • Objective Data • Abnormal CT scan or MRI • Abnormal EEG • Positive toxicology screen or alcohol level • ↑ or ↓Blood glucose level • ↑ ICP Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • K. D. arrives in the ICU with a head dressing and Jackson Pratt drain in place. • She responds to painful stimuli by withdrawing but does not follow commands. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • What nursing diagnoses related to K. D. ’s neurologic status would be most appropriate when planning her care? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Diagnoses • Risk for ineffective cerebral tissue perfusion • Hyperthermia • Impaired physical mobility • Anxiety • Potential complication: increased ICP Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Planning • Overall Goals • Cerebral oxygenation & perfusion • Normothermic • Control pain and discomfort • Free of infection • Adequate nutrition • Maximal cognitive, motor, and sensory function Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Health Promotion • Prevent car and motorcycle accidents. • Wear safety helmets. • Use seat belts and child car seats. • Home safety to prevent falls Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • You invite K. D. ’s family into her room once you have her settled in. • What would be important to explain to the family at this point? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Acute Intervention • Maintain cerebral perfusion. • Prevent secondary cerebral ischemia. • Monitor for changes in neurologic status. • Patient and family teaching Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Acute Intervention • Major focus of nursing care relates to increased ICP. • Eye problems • Eye drops, compresses, patch • Hyperthermia • Goal 36°to 37° C • Prevent shivering Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Acute Intervention • Measures for patients leaking CSF • Head of bed elevated • Loose collection pad • No sneezing or blowing nose • No NG tube • No nasotracheal suctioning Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Acute Intervention • Measures for immobilized patients • Antiemetics • Analgesics • Pre-op preparation, if needed Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • K. D. survives the initial traumatic brain injury and surgery. • She is hemodynamically stable, extubated, and breathing on her own. • She opens her eyes spontaneously and follow commands. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • K. D. remains confused and restless. • She also has some balance and motor deficits. • She is dependent on others for activities of daily living. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Case Study Jupiterimages/Comstock/Thinkstock • The family asks what the next step in her care will be and if she will ever return to her ‘original self. ’ • How will you respond? Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Ambulatory and Home Care • Acute rehabilitation • Motor and sensory deficits • Communication issues • Memory and intellectual functioning • Nutrition • Bowel and bladder management Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Implementation • Ambulatory and Home Care • Seizure disorders • Mental and emotional difficulties • Progressive recovery • Family participation and education Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Evaluation • Expected Outcomes • Maintain normal cerebral perfusion pressure. • Achieve maximal cognitive, motor, and sensory function. • Experience no infection or hyperthermia. • Achieve pain control. Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Audience Response Question The nurse is caring for a patient after a head injury. How should the nurse position the patient in bed? a. b. c. d. Prone with the head turned to the right side High-Fowlers position with the legs elevated Supine position with the head on two pillows Side-lying with the head elevated 30 degrees Copyright © 2014 by Mosby, an imprint of Elsevier Inc.
- Slides: 63