Head Injuries PHED 120 Krzyzanowicz Fall 12 Cerebral

Head Injuries PHED 120 Krzyzanowicz – Fall ‘ 12

Cerebral Concussion � Injury associated with virtually every sport � A thorough and consistent approach to evaluate patients suspected of a concussion will aid in improving diagnosis and return-to-play decisions ◦ Must identify severity in order to develop a treatment plan ◦ Early detection, diagnosis and follow-up are critical

Pathomechanics � Transient neurological dysfunction resulting from applied force to the head ◦ Forceful blow to the resting movable head produces brain injury beneath point of cranial impact �Coup injury ◦ Forceful blow to the moving head produces brain injury opposite of cranial impact �Contrecoup injury ◦ Differences are the result of brain lag and distribution of cerebrospinal fluid (CSF) ◦ Concussion experienced in sports tends to be a combination

Pathomechanics � Stresses Applied to Brain ◦ Compressive ◦ Tensile ◦ Shearing � Types of Pathology ◦ Traumatic brain injury �Focal = post-traumatic intracranial mass lesions that include subdural hematomas, epidural hematomas, cerebral contusions, intracerebral hemorrhages and hematomas �Diffuse = disruption of neurological function, not usually associated with macroscopic brain lesions �Result of brain being “shaken” �Tissue damage, the result of acceleration-deceleration �Includes cerebral concussions (mild traumatic brain injury)

Concussions � No universal agreement on definition or nature of concussions � Caused by direct blow to head, resulting in sudden mechanical loading of head � Impact between cortex and bony skull walls results in immediate/short-term neurological impairment ◦ Long-term effects = post-concussion syndrome � May cause neuropatholgical changes or temporary tissue deformation

Concussions � Causes a gradient of clinical syndromes including LOC � Most often associated with normal results during conventional neuroimaging � Is “getting his bell rung” a concussion? � Important for AT to recognize and classify concussive injury � Athlete must also understand signs and symptoms and their negative consequences

Classification of Cerebral Concussion � Grading concussions � Clinicians should focus on the duration of symptoms associated with injury � Important to emphasize other signs and symptoms, in addition to LOC and amnesia � Athlete’s condition should be graded after symptoms have resolved

Classification of Cerebral Concussion � Mild Concussion ◦ Most frequent and most difficult to recognize and diagnose ◦ Transient aberration in brain electrophysiology results in impaired mental status ◦ No LOC; impaired cognitive function (post-traumatic amnesia) ◦ Dizziness, tinnitus, possible decline in coordination (Romberg test), headache ◦ Headache can be used to determine if condition is improving or worsening

Classification of Cerebral Concussion � Moderate Concussion ◦ Associated with transient mental confusion, tinnitus, moderate dizziness & unsteadiness, prolonged posttraumatic amnesia (>30 minutes) ◦ Momentary loss of consciousness (up to 1 minute) ◦ Blurred vision, balance disturbances, nausea ◦ Requires careful consideration and clinical observation ◦ Must also be cautious and use skillful judgment when making return-to-play decisions

Classification of Cerebral Concussion � Severe Concussion ◦ Signs and symptoms last considerably longer than those of mild and moderate concussions ◦ Will likely include more significant LOC ◦ Post-traumatic amnesia lasting >24 hours; retrograde amnesia (memory loss of events prior to injury) ◦ Decreased neuromuscular coordination ◦ Serial observations should be conducted � Management ◦ Serial observations ◦ Rest ◦ Evaluation by physician in the event of prolonged LOC �Should consider neuroimaging of the brain ◦ Athletes should not be returned to participation while still experiencing symptoms

Cerebral Contusion � Brain tissue suffers bruising when an object hits the skull � Results in injured vessels, internal bleeding, and LOC � May be associated with partial paralysis or hemiplegia; one-sided pupil dilation, altered vital signs � Progressive swelling may continue to compromise brain tissue & cerebral function � Prognosis is dependent on care

Cerebral Hematoma � Little space for swelling and blood clots between brain and skull � Results in increased intracranial pressure and possible shifting of cerebral hemispheres � Causes a decline in neurologic function � Two types ◦ Epidural ◦ Subdural

Cerebral Hematoma � Epidural Hematoma ◦ Result of severe blow to head, producing skull fracture in temporoparietal region �Tend to be isolated injuries (skull sustains major impact forces and absorbs resultant kinetic energy) ◦ Accumulation of blood between dura mater and inner surface of skull due to arterial bleed from middle meningeal artery ◦ Fast developing, which cause neurologic deterioration in 10 – 120 minutes ◦ Possible LOC; period of lucidity ◦ Slow accumulation of blood resulting in neurologic compromise as hematoma becomes critically large = compresses brain tissue ◦ Clinical manifestation is dependent on type and amount of energy transferred, time course of hematoma formation, concurrent brain injuries
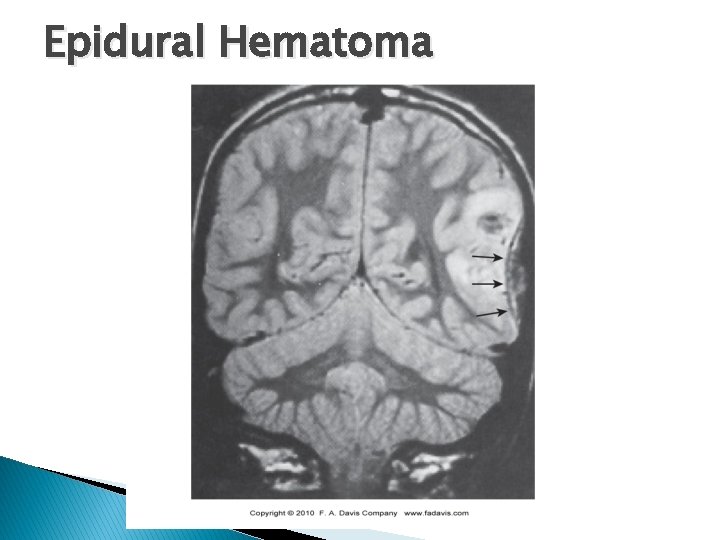
Epidural Hematoma

Cerebral Hematoma � Subdural Hematoma ◦ Caused by blow to head resulting in brain being thrust against point of contact ◦ Subdural vessels stretch and tear leading to hematoma in subdural space �Typically venous in origin resulting in slow developing hematoma �Acute = 48 -72 hours development �Chronic = later time frame, variable clinical manifestations ◦ Signs & symptoms will develop slowly �Altered consciousness (coma or major focal neurological deficits) ◦ Treatment �Prolonged observation and monitoring due to the risks associated with slowly developing brain bleeds and deterioration in mental status �Surgical intervention may be necessary to evacuate hematoma and decompress brain

Second Impact Syndrome � Occurs when an athlete sustains a second head injury prior the symptoms resolving from a previous injury ◦ Often first injury was unreported or unrecognized � Results in rapid brain swelling & herniation; brain stem failure occurs in 2 -5 minutes; pupil dilation and loss of eye movement, respiratory failure and ultimately coma � Mortality of SIS is 50% and morbidity is 100%

Immediate Management of Sport. Related Concussion � Recognize injury & severity � Determine if athlete requires additional attention/assessment � Decide when it is safe for the athlete to return to sports activity � Well-developed protocol is key to successful initial evaluation

Initial On-Site Assessment � Athlete down vs. Ambulatory conditions � Primary survey ◦ Assess basic life support needs � Secondary ◦ ◦ ◦ ◦ survey History Observation Palpation Special tests Active/passive range of motion Strength tests Functional tests

Initial On-Site Assessment � History ◦ Must be thorough ◦ Determine level of mental confusion, LOC and amnesia (anterograde vs. retrograde) ◦ Consider cervical spine involvement ◦ Monitor vital signs at regular intervals � Observation & Palpation ◦ Check for deformities and abnormal facial expressions (cranial nerve involvement) ◦ Speech patterns, respiration patterns, movement of extremities ◦ Palpation of skull and C-spine �Exercise additional caution if patient is unconscious

Sideline Assessment � More detailed examination � Cranial nerve assessment � Check for basilar skull fractures ◦ Battle’s sign, otorrhea, rhinorrhea, raccoon eyes � Continue to monitor vital signs ◦ Slowing heart rate or changes in blood pressure could suggest intracranial involvement

Special Tests for Assessment of Coordination � Balance Error Scoring System (BESS) ◦ Provides objective, rapid and cost-effective means of assessing postural stability �Reliable and valid assessment tool ◦ Utilizes three stances on both firm and foam surfaces ◦ Results from test are best used when compared to a baseline � Other tests ◦ Sensory Organization Testing & force plate recommended for return-to-play decisions ◦ Finger-to-nose test also considered a good means of assessing cognitive processing and balance

Special Tests for Assessment of Cognition � Begin with giving athlete 3 unrelated words ◦ Ask athlete to repeat words at end of assessment � Standardized Assessment of Concussion (SAC) ◦ Used to assess mental status ◦ Brief screening for those with no expertise in neuropsychological testing ◦ Assesses 4 domains of cognition (orientation, immediate memory, concentration, delayed recall) ◦ Most helpful when baseline scores have been obtained prior to injury

Special Tests for Assessment of Cognition � Computerized ◦ ◦ ◦ ◦ Neuropsychological Test Automated Neuropsychological Assessment Metrics Cog. State Concussion Resolution Index Immediate Post-concussion Assessment and Cognitive Testing (Im. PACT) Primary advantages �Ability to assess reaction time �Establishing baselines for large number of athletes in short period of time �Multiple forms within testing paradigm Challenges �Best follow-up assessment protocol �Interpretation of results �Cost Clinicians should be trained in administration of test Must identify neuropsychologist that will aid in clinical interpretation of post-injury test results

Return to Competition � Grading scales ◦ Lack of consensus as many scales have been based on anecdotal literature and clinical experience ◦ Cantu Evidence Based Grading Scale is recommended because it emphasizes all signs and symptoms without placing undue emphasis on LOC and amnesia � Athlete should not return to play if still symptomatic
- Slides: 24