HCA LVAD Program October 2019 Be LVAD Aware
HCA LVAD Program October 2019 Be LVAD Aware

Course Objectives The student will have an understanding of: 1. 2. 3. 4. What an LVAD is as well as its history. The type of patient that might require an LVAD. Important information to be aware of when working with an LVAD patient. How to contact the LVAD Team.

What is a Left Ventricular Assist Device (LVAD)? An LVAD is a surgically implanted blood pump that assists the heart with pumping blood to the body. It does not replace the heart. It works with the heart.

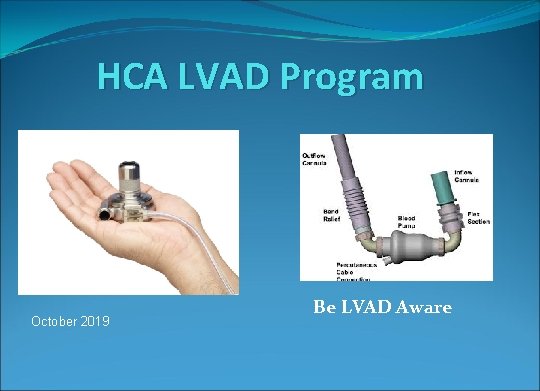
What does it look like? We have two. The on the left is the Heartware device manufactured by Medtronic; the on the right is the Heartmate II device made by Abbott. There are internal and external components for both.

Intro to Heart. Mate II and Heartware INTERNAL COMPONENTS Implantable Pump Both devices are continuous flow and are inserted by a cardiac surgeon. The Heart. Mate II is placed right next to the native heart (see picture at right). The Heartware device is placed directly into the heart (see picture next slide). Batteries

Heartware device
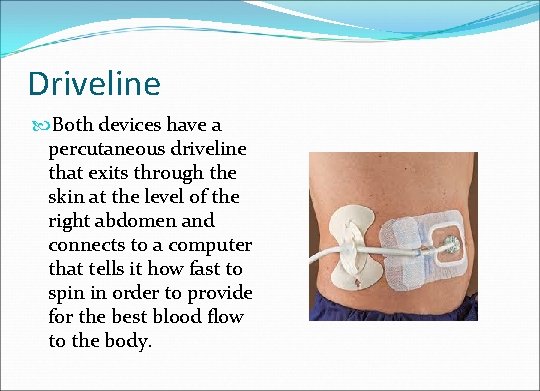
Driveline Both devices have a percutaneous driveline that exits through the skin at the level of the right abdomen and connects to a computer that tells it how fast to spin in order to provide for the best blood flow to the body.

Introduction (cont. ) EXTERNAL COMPONENTS The percutaneous driveline is connected to a system controller that is the brain of the unit. It tells the pump how fast to move the blood. Heartmate II The system controller needs power to work. An external power source of either lithium ion batteries or AC power is used to power the system controller. Heartware

LVAD Therapy is considered: Patients with systolic heart failure with an EF <30 When heart failure gets to a point that physical activity is limited Patients may be uncomfortable with any activity, and have trouble breathing when resting or lying down. Patients with symptoms who have optimal medical management should be considered for referral to the Advanced Heart Failure Clinic for additional therapy including consideration of LVAD placement.

Advanced Heart Failure • Patients feel weak and tired. Because a weak heart pumps less blood, the body gets less oxygen. Fluid builds up in the lungs, legs, ankles and feet. This extra fluid stresses the heart even more.

The Impact of Heart Failure Growing with an aging population § 5. 7 million adults in the US § Mortality is 50% at five years (CDC, 2019) § #1 reason for hospitalization in people >65 years of age. § Greater than 1 million hospitalizations every year § Costs an estimated $30. 7 billion each year. § 87% of CHF patients have three additional comorbidities. § Lifetime risk of developing HF is 20% in Americans >40 yrs. § 25% will be readmitted to the hospital in 30 days. § After 4 hospital stays, median survival <6 months.

Indications for LVAD Therapy Bridge to Transplant • An LVAD may help patients who are waiting for a heart transplant until a donor heart is found. This is known as Bridgeto –Transplantation or BTT. Destination Therapy • Some advanced heart failure patients may not be candidates for a transplant because of other diseases or age. • These patients may benefit from long term LVAD support. • This is called Destination Therapy or DT.

LVAD Multidisciplinary Team A multidisciplinary team meets on a regular basis. Some of their responsibilities include: Ø Reviewing patients both for selection criteria as well as optimizing their current care. ØDeveloping and maintaining clinical guidelines and order sets. ØReviewing policies and procedures. ØMonitoring and improving patient and program outcomes. ØEnsuring performance improvement for the LVAD program.

Who are some of the LVAD team members? Dr. Leo Gazoni - Lead Surgeon Dr. Andrew Keller-Medical Director, Advanced Heart Failure Clinic Dr. Ramesh Kundur-Heart Failure physician with VCS Taylor Fricke-Lead Surgical PA Emily Mochan-LVAD Director Joan Recher-LVAD Coordinator LVAD Pharmacist Jennifer O’Connell-LVAD Social Worker Lisa Mayer–Palliative Care Nurse and Cardiac Nurse Navigator Transplant Partner-VCU Health System

How to get in touch with an LVAD Coordinator Call the LVAD Coordinator in the office, 483 -1270. After-hours calls will be answered by the service and paged. OR Call 1 -804 -560 -LVAD (5823)

What you should know if you are working with an LVAD patient LVADs are continuous flow devices. Therefore, the patient may not have a palpable pulse. ASSESSMENT IS IMPORTANT and expected. If you are involved in the patient’s care, it is all about assessing the patient. If they are awake and talking with you, it is a different situation then if they are not.

What you should know if you are working with an LVAD patient (cont. ) The driveline/percutaneous lead is the lifeline of the pump for control and power. It needs to be protected. If undergoing tests or procedures, make sure that the driveline is free and clear and not at risk for being pulled, tugged or twisted.

What you should know if you are working with an LVAD patient (cont. ) The LVAD patient and/or caregiver should know about their system and how it works. If the patient is here for a procedure or test that requires sedation, an LVAD trained person must be with them. Please notify the LVAD coordinator as soon as possible when the procedure or test is scheduled.

What you should know if you are working with an LVAD patient (cont. ) The LVAD patient should always travel with back-up equipment. Each patient is given a travel bag to keep their back-up equipment in.

What you should know if you are working with an LVAD patient (cont. ) The LVAD travel bag contains 1 pair of back up batteries and 1 backup system controller. If a patient is in your department for a test or procedure, be aware of where the bag is and make sure it stays and leaves with the patient.

References 1. 2. 3. 4. 5. 6. 7. 8. Peura JL, Colvin-Adams M, Francis GS, et al. Recommendations for the use of mechanical circulatory support: device strategies and patient selection a scientific statement from the American heart association, Circulation. 2012; 126. Thoratec Heart. Mate II Instructions for Use Thoratec Heart. Mate II Operating Manual Medtronic Heartware Operating Manual CDC website / heart failure https: //www. cdc. gov/dhdsp/data_statistics/fact_sheets/fs_heart_failure. htm www. thoratec. com www. abbott. com https: //www. medtronic. com/us-en/healthcareprofessionals/products/cardiac-rhythm/ventricular-assist-devices/heartware -hvad-system. html

Questions or Concerns Contact: Lisa Mayer, MSN, RN, CHFN Heart Failure Coordinator 804 -483 -2368 Or call the Advanced Heart Failure Clinic: 483 -1270 (clinic office)
- Slides: 22