Harsh Golwala MD Advanced Interventional Cardiology Fellow Brigham

Harsh Golwala, MD Advanced Interventional Cardiology Fellow, Brigham and Women’s Hospital, Boston, MA www. brighamandwomens. org/heart

Disclosures None


Learning Objectives • Discuss the prevalence, anatomical distribution and clinical presentation of patients with acute total occlusion of culprit artery in non-ST segment elevation myocardial infarction (NSTEMI) as compared with those without total occlusion of culprit artery. • Discuss the implications of acute total occlusion of culprit artery in NSTEMI on long term major adverse cardiac events and all-cause mortality.

Rationale • Acute coronary syndrome (STEMI, NSTEMI, Unstable angina) is a major cause of mortality and morbidity. • A subset of patients who present with NSTEMI are found to have 100% stenosis of the culprit artery on diagnostic coronary angiography. • Due to lack of classic ECG findings of ST-segment elevation, these patients often do not receive timely coronary angiography and/or intervention. • The prevalence and prognosis of these patients is not entirely known. Mozafferian D, Circulation 2016

Study Question We performed a systematic review and meta-analysis of available studies in the literature to estimate the difference in clinical outcomes of patients with NSTEMI with acute total occlusion of the culprit artery vs. patients with NSTEMI without acute total occlusion of the culprit artery.

Outcomes of interest • All-cause mortality [short-term (in-hospital/30 day) as well as intermediate term (6 -12 m)] • Major adverse cardiac events [short-term (in-hospital/30 day) as well as intermediate term (6 -12 m)] • Clinical presentation assessed via Killip classification • Left ventricular ejection fraction at presentation • Time to angiography/coronary intervention
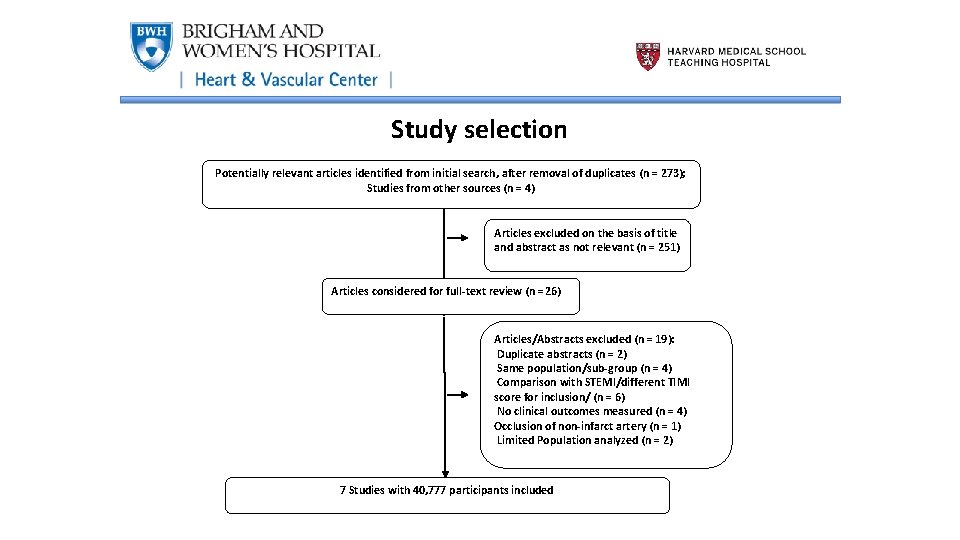
Study selection Potentially relevant articles identified from initial search, after removal of duplicates (n = 273); Studies from other sources (n = 4) Articles excluded on the basis of title and abstract as not relevant (n = 251) Articles considered for full-text review (n =26) Articles/Abstracts excluded (n = 19): Duplicate abstracts (n = 2) Same population/sub-group (n = 4) Comparison with STEMI/different TIMI score for inclusion/ (n = 6) No clinical outcomes measured (n = 4) Occlusion of non-infarct artery (n = 1) Limited Population analyzed (n = 2) 7 Studies with 40, 777 participants included

Statistical analysis • The definition of MACE followed the outcome as defined in each study. • Adjusted relative risk (RR) or hazards ratio (HR) reported by individual studies were used for the analysis. A cumulative RR was calculated by pooling the RR and HR reported from the studies for all-cause mortality and MACE separately. • The inverse-variance method was used to pool the effect estimate in a fixed or random effects model based on the associated heterogeneity.

Baseline characteristics • 40, 777 patients included in the analysis, of which 10, 415 (25. 5%) had total occlusion of culprit artery whereas 30, 262 (74. 5%) had non-occluded culprit vessel. • Most included patients were male with a mean age of 63 years

Identification of culprit artery • Primarily with the angiographic appearance in six studies. • In three studies, EKG and echocardiographic changes supported angiography in assessment of the culprit artery. • Assessment of the culprit artery was validated in two studies: by the angiographic core lab in one study and two experienced cardiologists who were blinded by clinical presentation in two studies.
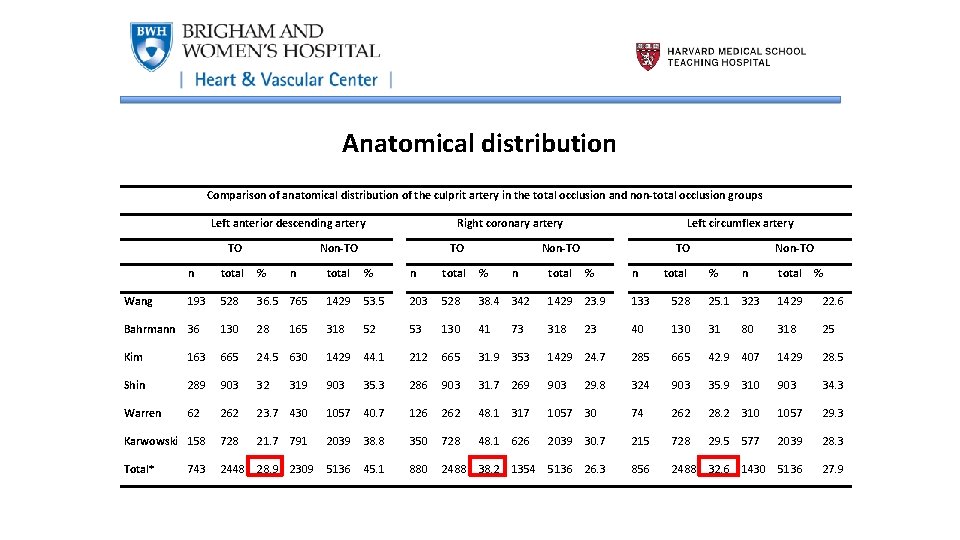
Anatomical distribution Comparison of anatomical distribution of the culprit artery in the total occlusion and non-total occlusion groups Left anterior descending artery TO Right coronary artery Non-TO n total % Wang 193 528 Bahrmann 36 Kim Non-TO total % n total % 36. 5 765 1429 53. 5 203 528 130 28 318 52 53 163 665 24. 5 630 1429 44. 1 Shin 289 903 32 903 Warren 62 23. 7 430 Karwowski 158 728 Total* 2448 743 n TO Left circumflex artery % n 38. 4 342 1429 23. 9 133 528 25. 1 323 1429 22. 6 130 41 318 23 40 130 31 318 25 212 665 31. 9 353 1429 24. 7 285 665 42. 9 407 1429 28. 5 35. 3 286 903 31. 7 269 903 29. 8 324 903 35. 9 310 903 34. 3 1057 40. 7 126 262 48. 1 317 1057 30 74 262 28. 2 310 1057 29. 3 21. 7 791 2039 38. 8 350 728 48. 1 626 2039 30. 7 215 728 29. 5 577 2039 28. 3 28. 9 2309 5136 45. 1 880 2488 38. 2 1354 5136 26. 3 856 2488 32. 6 1430 5136 27. 9 319 73 total Non-TO total 165 n TO % n 80 total %
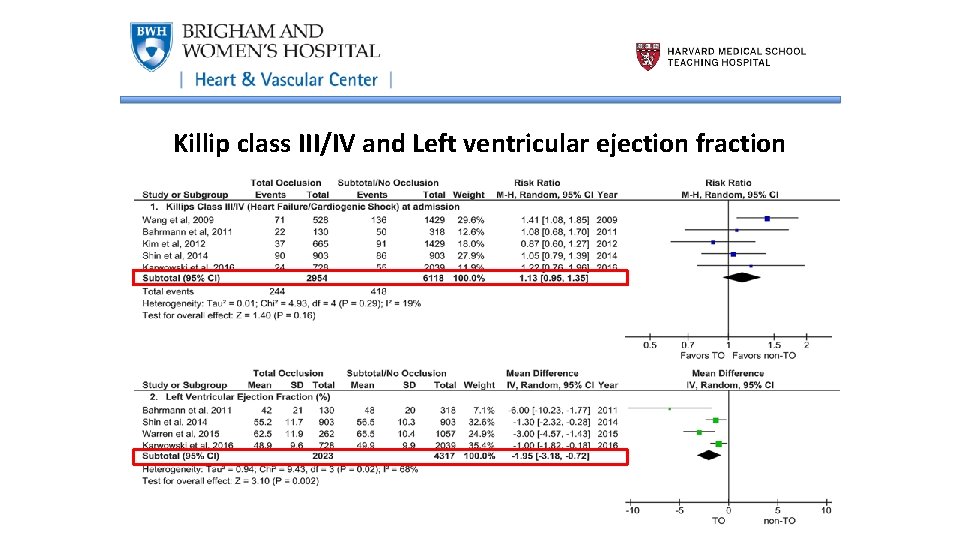
Killip class III/IV and Left ventricular ejection fraction
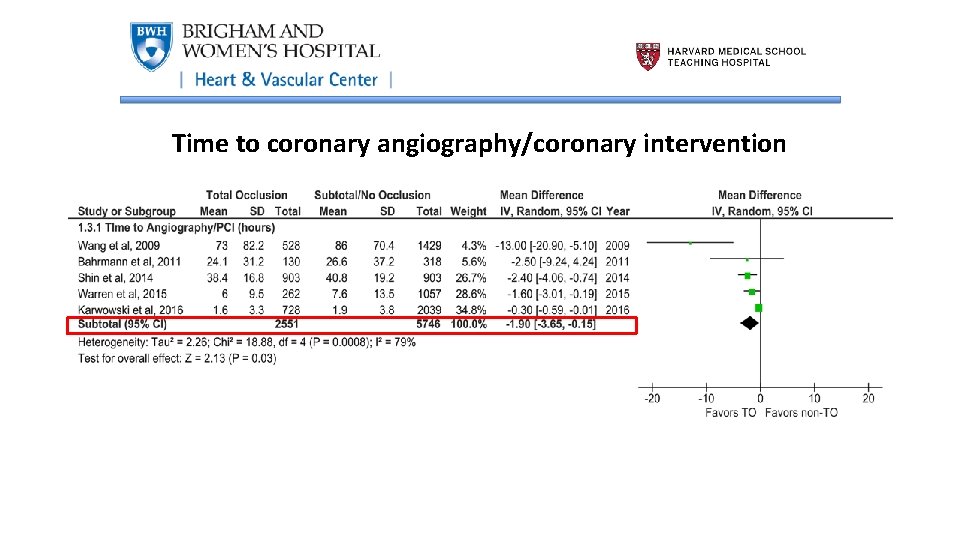
Time to coronary angiography/coronary intervention

Short term major adverse cardiac events
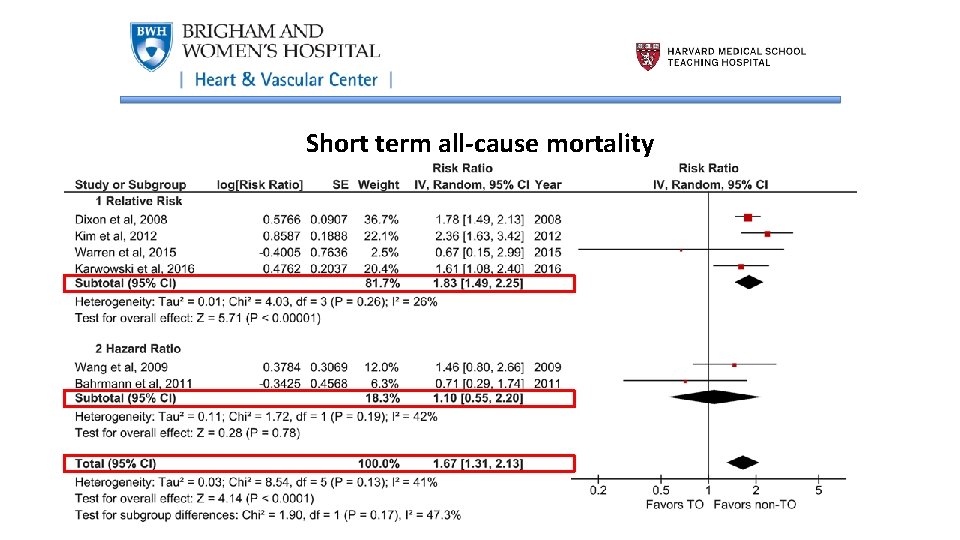
Short term all-cause mortality
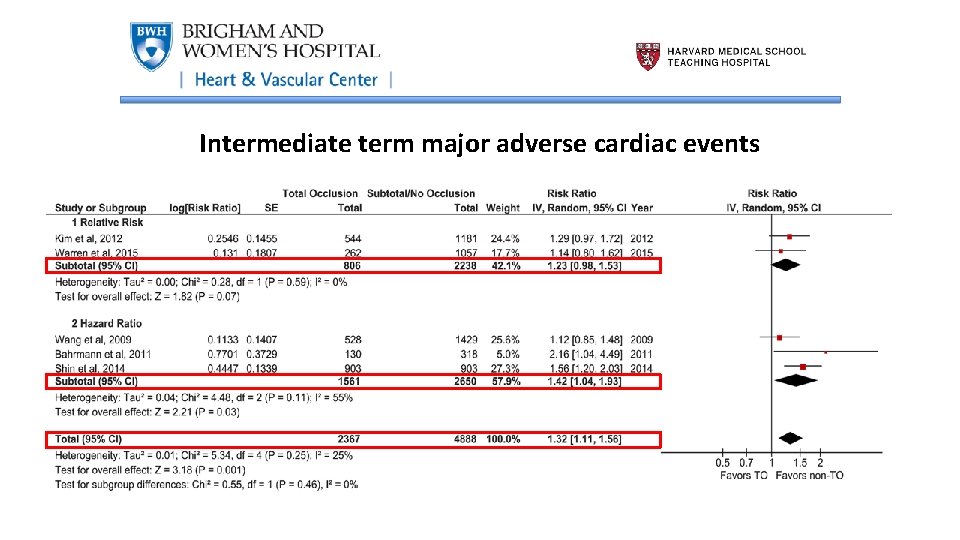
Intermediate term major adverse cardiac events
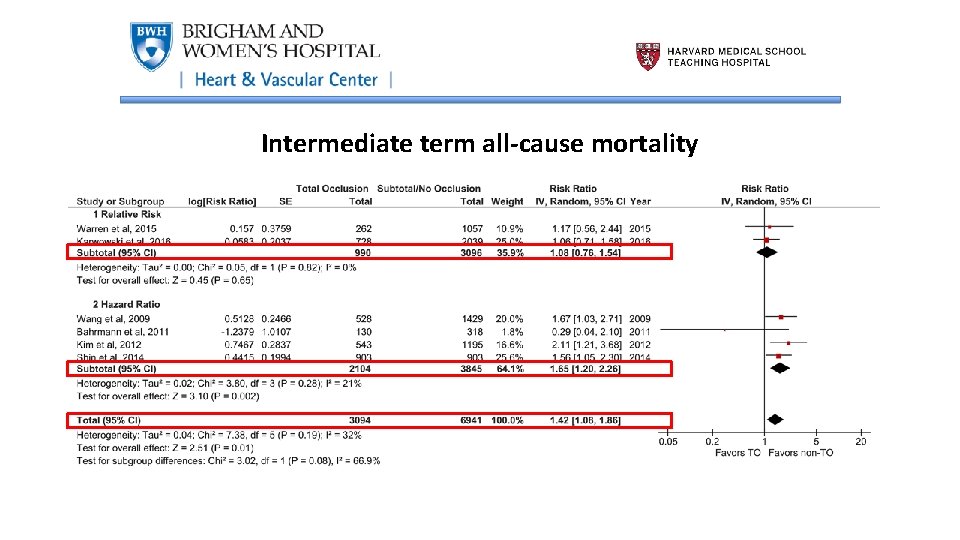
Intermediate term all-cause mortality

Other outcomes • There was significant variability in the levels of CK-MB and troponins as different units were used to measure them and at different time points. Hence the results were not pooled. However, three studies reported statistically significant difference in biomarkers between the two groups, with increased levels in patients who present with total occlusion.

Limitations • Risk of bias is high due to the observational design of the studies included. • The results may be affected by differences in the baseline characteristics of patients included in the individual studies, infarct size, and the use of antiplatelet and anti-coagulant agents at presentation. • Independent core lab validation of the culprit artery was not available in most studies.

Conclusions • Our meta-analysis suggests that NSTEMI patients with acute total occlusion of the culprit coronary artery may represent a higher risk group as they may suffer from increased risk of both short-term and intermediate-term major adverse cardiac events and all-cause mortality. • In addition, we did not find any significant difference in high risk clinical features based on Killip class at presentation between the two groups which may have in turn resulted in no difference in time to angiography or PCI between the two groups.

Conclusions • Although we did not pool differences in biomarker level because of associated variability in reporting between studies, qualitative analysis suggests that there may be an increased burden of myocardial injury in patients with acute total occlusion of the culprit artery.

Clinical implications and future directions • Patients presenting with NSTEMI who have an acutely occluded culprit artery may represent a subset of ACS patients whose identification based on clinical and electrocardiographic criteria remains challenging. • Better risk stratification tools such as routine employment of V 7 -V 8 or V 4 R ECG leads, as well as point of care echocardiography may aid in early identification of these patients who may benefit from early angiography and/or intervention to reduce short and long term major adverse cardiac events.


Thank you
- Slides: 25