HAND EMERGENCIES Rutvi Patel GOALS AND OBJECTIVES The
HAND EMERGENCIES Rutvi Patel

GOALS AND OBJECTIVES The goal of this presentation is for the audience to review and understand: A proper clinical hand examination Selected traumatic hand injuries Selected infectious hand emergencies When treatment in the ED is sufficient and when hand surgery consult is needed. The functional position of the hand with the appropriate splints Different anesthesia techniques for the hand

TOPICS COVERED Clinical examination of the hand Finger tip injury/Finger amputation Nail bed injury/laceration/avulsion High pressure Injection Injury Flexor tenosynovitis Felon Paronychia Splints Metacarpal fractures Phalanx fractures Anesthesia techniques

CLINICAL HAND EXAM Inspection: �Swelling, deformity, cuts/lacerations, color change �Natural lie of the hand Palpation: �Temperature: warm – infection/inflammation, cool -vascular pathology �For tenderness, Crepitus (fracture), Joint effusion (infection, inflammation, trauma)

CLINICAL HAND EXAM Range of Motion/strength: � Active and passive � Flexion/extension at DIP/PIP/MCP joint of each finger checking for tendon injury MCP: 0° extension to 85° of flexion PIP: 0° extension to 110° of flexion DIP: 0° extension to 65° of flexion � Abduction/adduction of all fingers � Flexion/extension of wrist 60° flexion, 60° extension, 50° radioulnar deviation arc
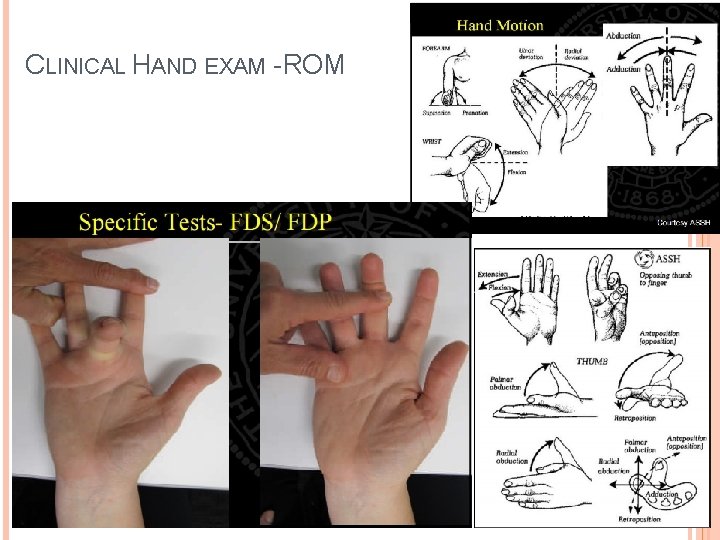
CLINICAL HAND EXAM - ROM
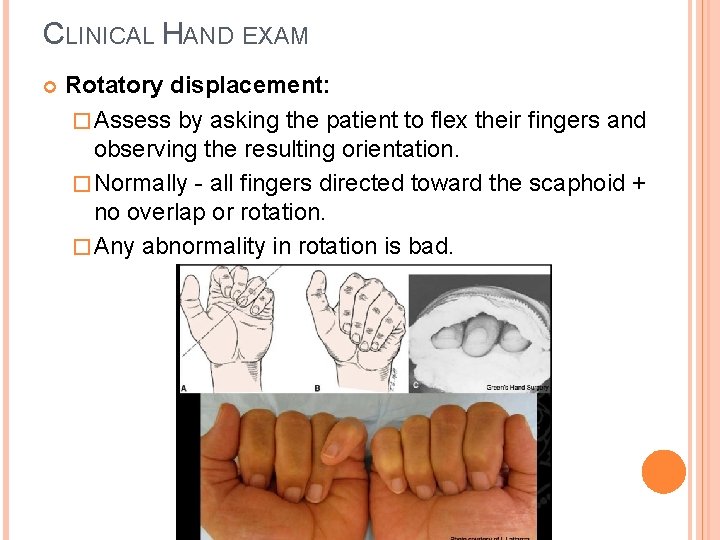
CLINICAL HAND EXAM Rotatory displacement: � Assess by asking the patient to flex their fingers and observing the resulting orientation. � Normally - all fingers directed toward the scaphoid + no overlap or rotation. � Any abnormality in rotation is bad.
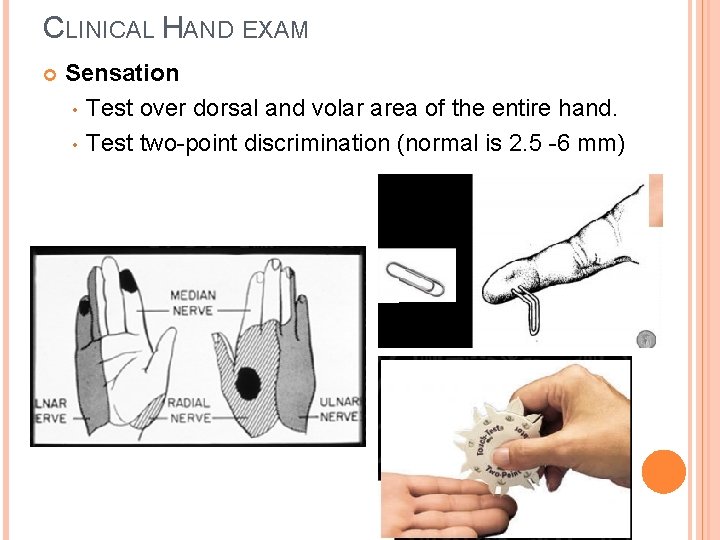
CLINICAL HAND EXAM Sensation • Test over dorsal and volar area of the entire hand. • Test two-point discrimination (normal is 2. 5 -6 mm)

CLINICAL HAND EXAM Motor � Radial nerve: test thumb IP joint extension against resistence (thumbs-up sign) � Median nerve recurrent motor branch: palmar abduction of thumb anterior interosseous branch: flexion of thumb IP and index DIP ("A-OK sign") � Ulnar nerve: cross-fingers or abduct fingers against resistence Vascular � Radial and Ulnar pulse � Allen’s test � Capillary refill
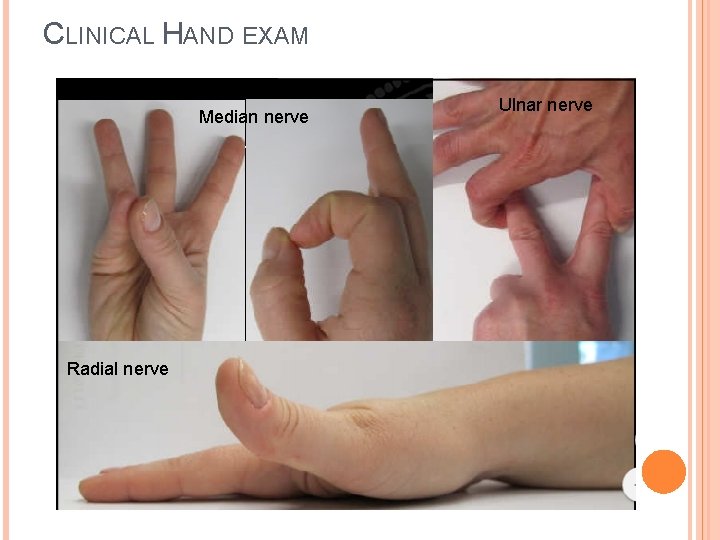
CLINICAL HAND EXAM Median nerve Radial nerve Ulnar nerve
FINGERTIP AVULSIONS/MINOR AMPUTATIONS Irrigate the wound thoroughly Hemorrhage control, Analgesia, Tetanus PPx, ABx, Assess the neurovascular status. Assess for exposure of bone, if laceration/avulsion or complete amputation. Assess for flexor and extensor tendon involvement Prompt referral to a hand surgeon is mandated if there is tendon involvement. (consult immediately if available; or follow-up within 5 days).
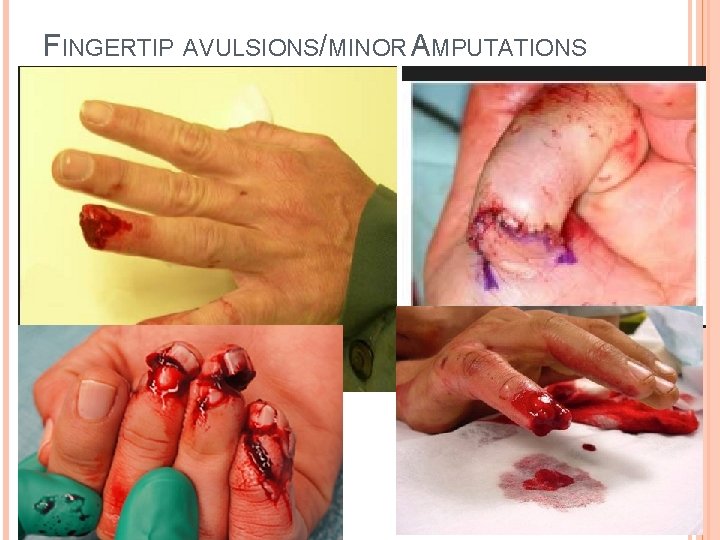
FINGERTIP AVULSIONS/MINOR AMPUTATIONS
FINGERTIP AVULSIONS/MINOR AMPUTATIONS- TREATMENT OPTIONS 1. 2. 3. Healing by secondary intention - no bone or tendon exposed with < 2 cm of skin loss Revision amputation with primary skin closure in the ED (Rongeuring) If � < 0. 5 cm bone is exposed � Minor amputation distal to the DIP joint Prompt evaluation and operative Tx by Hand surgery if – � No exposed bone and > 2 cm of tissue loss � Exposed bone or tendon where rongeuring bone proximally is not an option � Consult in the ED if available , or f/u within 5 days

REVISION AMPUTATION AND PRIMARY CLOSURE (RONGEURING) 1. 2. 3. If a small bony protuberance (<0. 5 cm in length) distal to the DIP is exposed in a wound, skin closure may not be possible without cutting back the bone. Perform digital block + oral/IV pain meds Use a rongeur bone cutter to slowly cutback the bone until enough soft tissue or skin over the bone for closure with simple interrupted sutures.

FINGERTIP AVULSIONS/MINOR AMPUTATIONS- TREATMENT OPTIONS All of the Tx options require following steps before discharge Apply antibiotic ointment and cover with dressing. 24 -48 hour wound recheck in the ED, as well as F/U with hand surgery within 1 week. Discharge with Abx course (for example, Keflex) effective against skin pathogens. Consider splinting the finger if fractured or to allow for soft tissue rest.
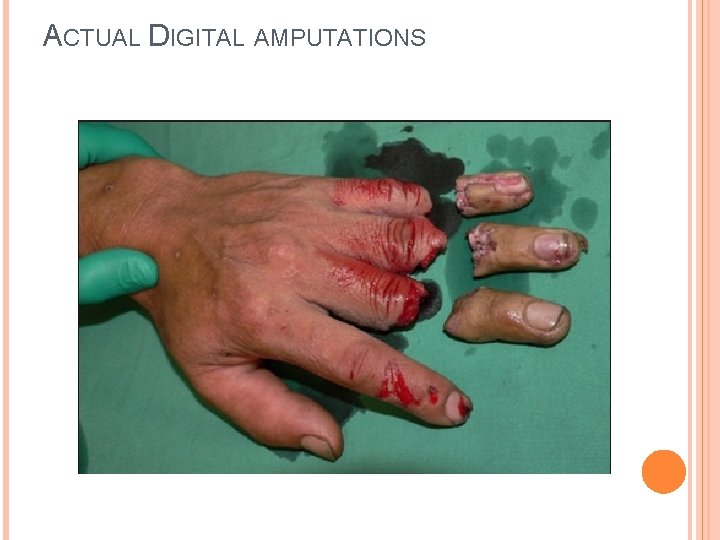
ACTUAL DIGITAL AMPUTATIONS

ACTUAL DIGITAL AMPUTATIONS Wrap the Amputated digit in a moistened sterile gauze, Place in sealed water tight bag and then place the bag on ICE. Note the time digit went on ICE. Assess the viability of an amputation for replantation Contact hand-surgeon immediately, to review and arrange for urgent re-implantation if digit is still viable. Replantation should nearly always be considered, and surgical repair is required even if replantation is contraindicated.

ACTUAL DIGITAL AMPUTATIONS Approximate allowable ischemia times are: � Digits - 12 hours warm , 24 hours cold ischemia � Major body parts - 6 hours warm, 12 hours cold ischemia Radiograph and Photograph both amputated part + stump pre-operatively for planning. Success rates for reimplantation depend on ischemia time, degree of tissue damage, and mechanism of injury

ASSESSING VIABILITY FOR REIMPLANTATION Patients who benefit functionally are : � Thumb at any level � Multiple digits � Through the palm � Wrist level or proximal to wrist � Possibly single digit amputations in setting of prior finger amputations of the same hand, � Almost all parts in children Contraindications: � Severe vascular disorder � Mangled limb or crush injury � Segmental amputation � Prolonged ischemia time with large muscle content (>6 hours)

NAIL BED INJURIES – SUBUNGAL HEMATOMA o o o Crushing-type injury causing bleeding beneath nail If < 50% nail involved - drainage of hematoma by perforation � Puncture nail using sterile needle electrocautery to perforate nail If > 50% nail involved –nail removal, D&I, nail bed repair � Usually involves nailbed laceration as well. � Remove nail and soak in Betadine while repairing nail bed � Repair nail bed with ≤ 6. 0 absorbable suture or dermabond – equal results � Splint eponychial fold with original nail, aluminum, or non-adherent gauze for protection

NAIL BED INJURIES – NAILBED LACERATION/AVULSION Avulsion of nail and portion of underlying nail bed Commonly associated with distal phalanx fracture Treatment � Nail removal, Nail bed repair, +/- fx fixation � Tetanus and Abx prophylaxis � Splint eponychial fold with original nail, aluminum, or non-adherent gauze for protection � Consult Hand surgery (in the ED if available or F/U within 5 days) If Extensive injury, Significant loss of nail matrix, complicated fractures, as it may require split thickness graft vs. nail matrix transfer
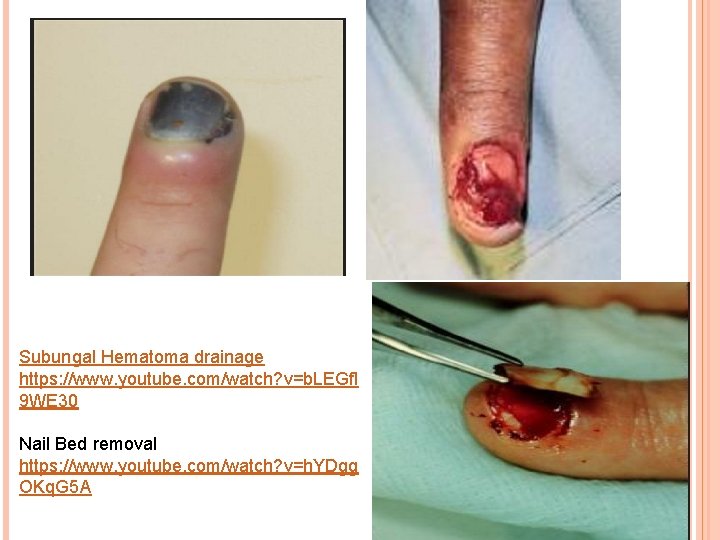
Subungal Hematoma drainage https: //www. youtube. com/watch? v=b. LEGfl 9 WE 30 Nail Bed removal https: //www. youtube. com/watch? v=h. YDgg OKq. G 5 A

HIGH PRESSURE INJECTION INJURY High-pressure injection device - paint or grease gun. Up to 50% amputation rate for organic solvents (paint, paint thinner, diesel fuel, jet fuel, oil) Benign Entry wound + extensive internal soft tissue damage Dissection along planes of least resistance (along neurovascular bundles) Vascular occlusion → local soft tissue necrosis Severity of the injury depends on � Time to treatment + Force of injection + Volume injected � Composition of material

HIGH PRESSURE INJECTION INJURY - MANAGEMENT Imaging to rule out foreign bodies/Bony injuries Non Operative - only for air or water injection. � TDAP, broad spectrum ABx, limb elevation, early mobilization, monitoring for compartment syndrome Operative (Emergent hand surgery consult) - most cases � Immediate irrigation & surgical debridement Transfer if ortho/Hand surgery unavailable Higher rates of amputation seen when surgery delayed > 10 hours after injury
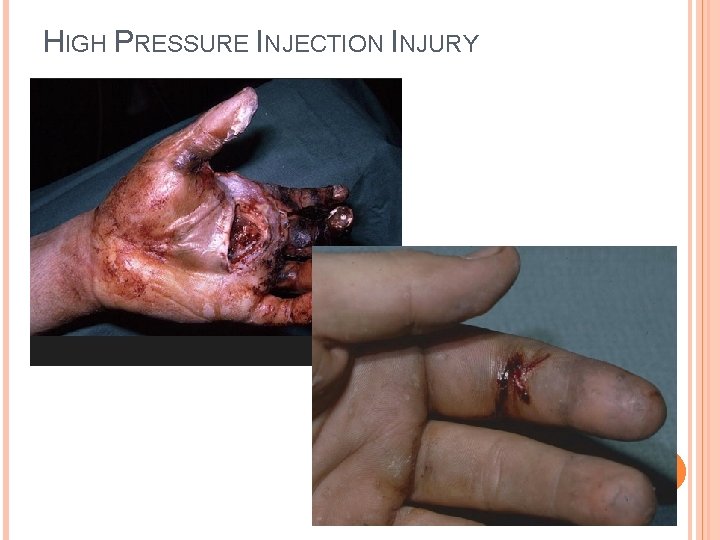
HIGH PRESSURE INJECTION INJURY

FLEXOR TENOSYNOVITIS Infection of the synovial sheath that surrounds the flexor tendon Organisms – � Staph aureus/strep (most common), Eikenella/ Pasteurella for dog/human bites, MRSA (Iv drug users), Mixed flora/Gram negatives (immunocompromised pts) Symptoms/PE - Kanavel signs (4 total): � Flexed posturing of the involved digit � Tenderness to palpation over the tendon sheath � Marked pain with passive extension of the digit � Fusiform swelling of the digit along with warmth/erythema Imaging – looking for injury/foreign bodies/evidence of gas or osteomyelitis.
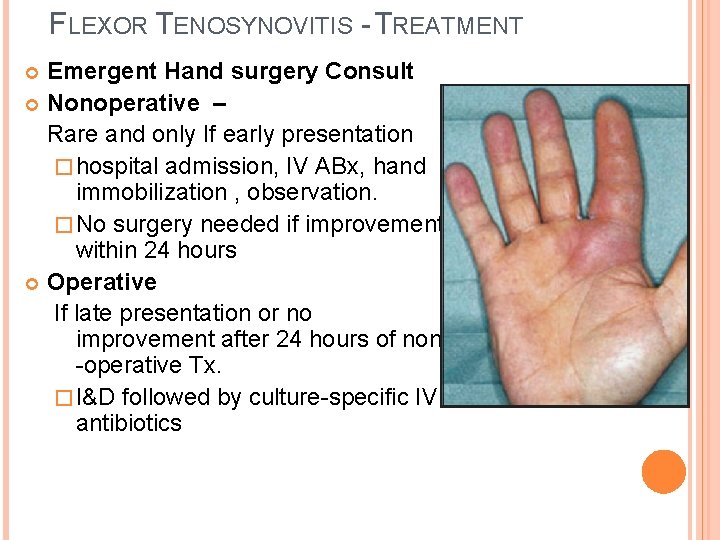
FLEXOR TENOSYNOVITIS - TREATMENT Emergent Hand surgery Consult Nonoperative – Rare and only If early presentation � hospital admission, IV ABx, hand immobilization , observation. � No surgery needed if improvement within 24 hours Operative If late presentation or no improvement after 24 hours of non -operative Tx. � I&D followed by culture-specific IV antibiotics

FELON Infection of the finger tip pulp From penetrating injury - blood glucose needle stick , splinters, local spread Swelling and pressure within micro-compartments, leading to "compartment syndromes" of the pulp Treatment: � I&D of the finger pulp in the ER. May need I&D in the OR if extensive or not improving. � Keep incision distal to DIP crease � Loose dressing + finger splint + Tdap + oral Abx. � IV ABx only for very extensive cases � F/U for wound recheck in 48 hours with hand surgery/ortho/ER/PCP
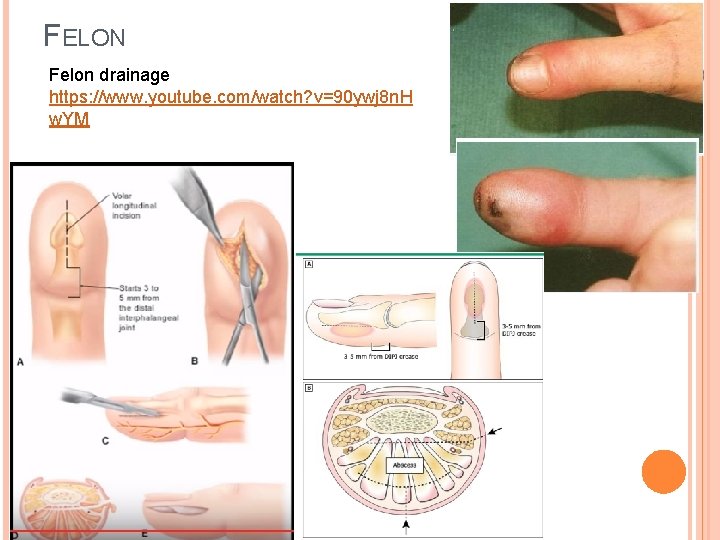
FELON Felon drainage https: //www. youtube. com/watch? v=90 ywj 8 n. H w. YM

PARONYCHIA Inflammatory/Infectious involvement of nail fold with Pus + erythema + swelling + pain Treatment - Drainage � Longitudinal incision parallel to the nail edge across the nail fold to release the pus � Soak in a saline solution → irrigate debris → apply dressing � Warm water soaks + elevate digit at home � Abx only needed for immunocompromised, DM, cellulitis, PVD � F/U in 48 hours with PCP or ER.
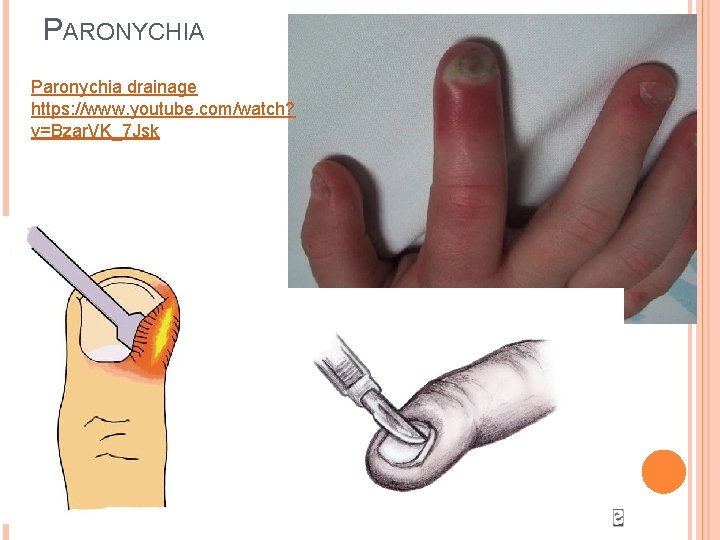
PARONYCHIA Paronychia drainage https: //www. youtube. com/watch? v=Bzar. VK_7 Jsk

FUNCTIONAL POSITION FOR HAND FRACTURE SPLINTS Wrist – 10 to 20 degrees of extension. Avoids contracture and maintain maximum hand strength. (MCP) joint – 60 to 70 degrees of flexion to keep the ligaments taut. (PIP) joint –Full extension to avoid contracture of ligaments (DIP) joint – Full extension to avoid stressing the terminal tendon and prevent contracture of the oblique retinacular ligament. Hand joints prone to stiffness. Do not immobilize > 3 weeks
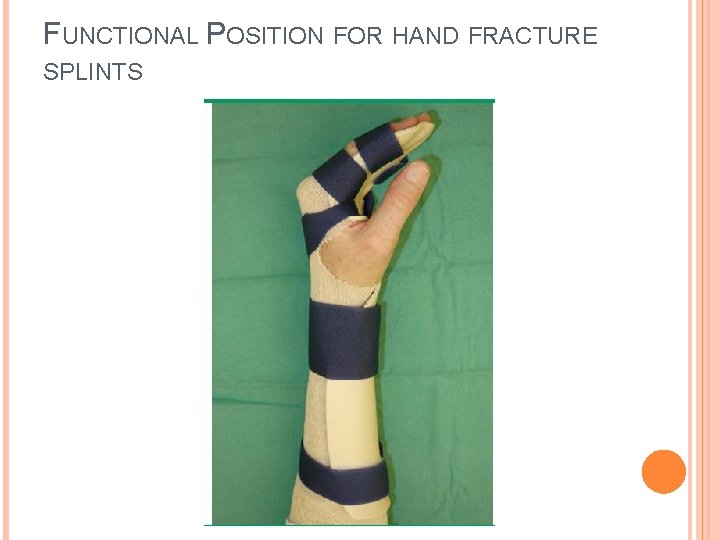
FUNCTIONAL POSITION FOR HAND FRACTURE SPLINTS

METACARPAL FRACTURES Divided into head, neck, shaft Tx based on which metacarpal is involved and location of fracture Acceptable angulation varies by location No degree of malrotation acceptable Inspect for open wounds and associated injuries Fight wounds over MCP joint are open until proven otherwise Extensor tendon can be lacerated and retracted Dorsal wounds are almost always open fractures

METACARPAL FRACTURES- GENERAL MANAGEMENT Nonoperative immobilization if - Nondisplaced and Stable pattern No rotational deformity Acceptable angulation & shortening All F/U within 1 -2 weeks with PCP or ortho/hand surgery for splint removal and reevaluation

METACARPAL FRACTURES- GENERAL MANAGEMENT Operative treatment (Hand surgery consult) if Intra-articular fxs Rotational malalignment of digit Neurovascular compromise Significantly displaced fractures Multiple metacarpal shaft fractures Tendon lacerations Hand surgery consult � In the ED if available. � OP F/U within 5 days If not immediately available Unacceptable angulation requires reduction and then splinting
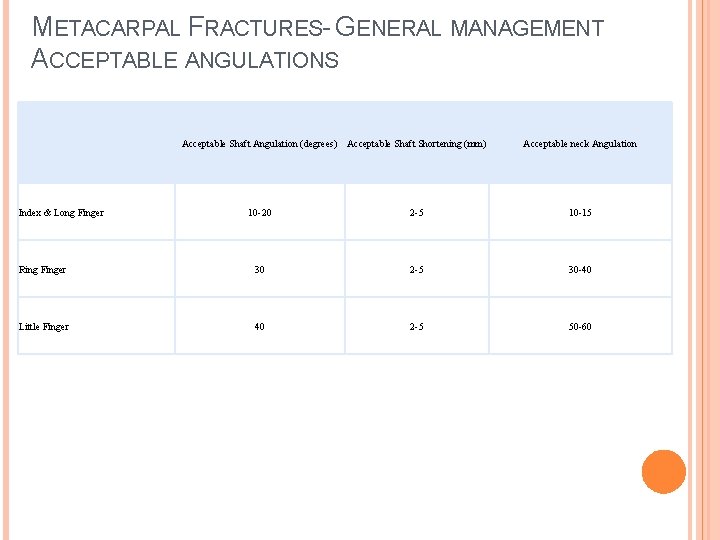
METACARPAL FRACTURES- GENERAL MANAGEMENT ACCEPTABLE ANGULATIONS Index & Long Finger Acceptable Shaft Angulation (degrees) Acceptable Shaft Shortening (mm) Acceptable neck Angulation 10 -20 2 -5 10 -15 Ring Finger 30 2 -5 30 -40 Little Finger 40 2 -5 50 -60
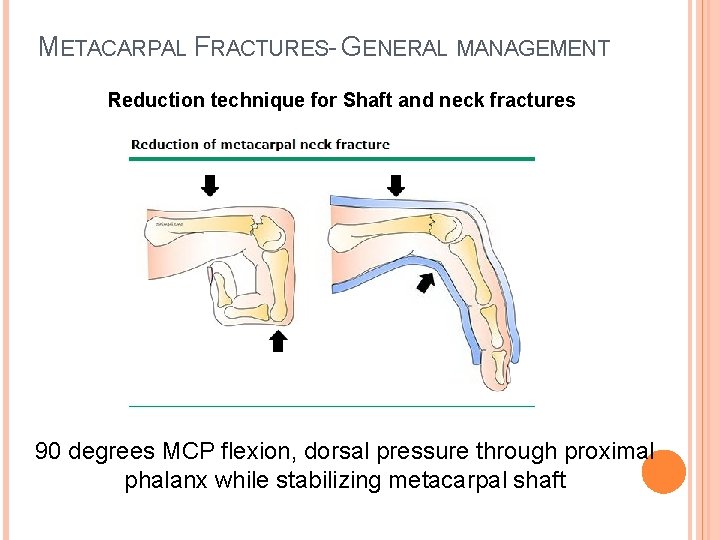
METACARPAL FRACTURES- GENERAL MANAGEMENT Reduction technique for Shaft and neck fractures 90 degrees MCP flexion, dorsal pressure through proximal phalanx while stabilizing metacarpal shaft

WHICH SPLINT TO USE?

PROXIMAL/MIDDLE PHALANX FRACTURE Splint/Buddy tape in the ED � Extraarticular � < 10° angulation or < 2 mm shortening � No rotational deformity � F/U with ortho/hand surgery in 1 -2 weeks Consult Hand surgery for Operative management � irreducible or unstable fracture pattern � transverse fractures (all angulate volarly) � > 10° angulation or 2 mm shortening � Rotationally deformed � Long oblique proximal phalanx fractures � F/U with hand surgery within 1 week if immediately not available

PROXIMAL/MIDDLE PHALANX FRACTURE - REDUCTION Unacceptable angulation must be reduced before splinting using a three point technique. Flex the MCP and PIP joints to 90 degrees. Apply gentle traction to reduce the proximal fragment dorsally and the distal fragment volarly. The fragment ends should meet at the fracture line. Finger dislocation reduction - https: //www. youtube. com/watch? v=y 00 Wjt. V_El. U
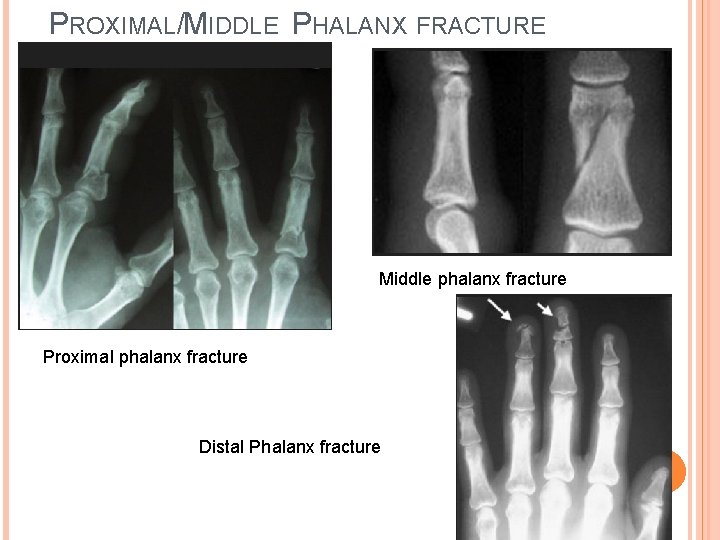
PROXIMAL/MIDDLE PHALANX FRACTURE Middle phalanx fracture Proximal phalanx fracture Distal Phalanx fracture

DISTAL PHALANX FRACTURE Nonoperative reduction and splinting in the ED � most nondisplaced fractures � Splint for 3 weeks with joint motion afterwards � F/U with PCP in 1 -2 weeks Operative with hand surgery consult � Concomitant nail bed injuries/nail matrix damage/complicated fracture. � F/U with hand surgery within 1 week for reevaluation
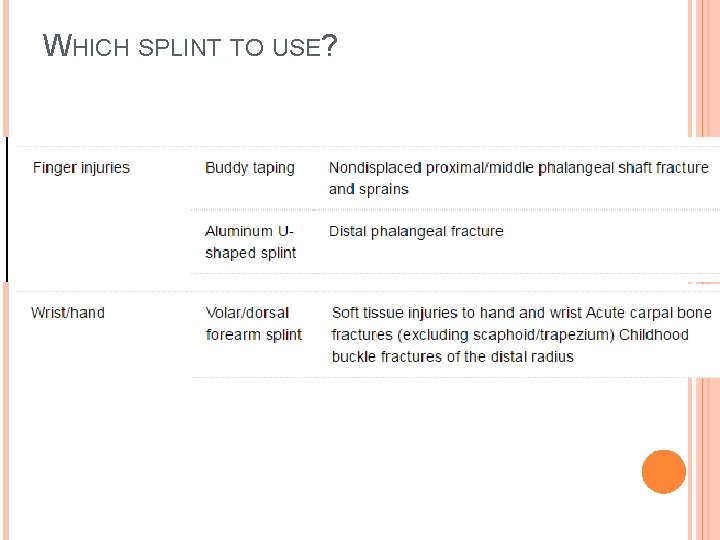
WHICH SPLINT TO USE?

ANESTHESIA TECHNIQUES FOR THE HAND Digital block http: //lifeinthefastlane. com/minor-injuries 007/ Hematoma block https: //www. youtube. com/watch? v=tjnsdjfw. Mm. Y Median and Ulnar nerve block https: //www. youtube. com/watch? v=6 NKkzs 9 FA 5 I Radial nerve block https: //www. youtube. com/watch? v=Pl. F 4 btt. KWds

RESOURCES Ortho Bullets Uptodate Medscape Life in the Fast lane American family Physician http: //www. aafp. org/afp/2009/0901/p 491. html Youtube

THE END
- Slides: 47