Haemostasis Tiffany Shaw MBCh B II 2002 Haemostasis

Haemostasis Tiffany Shaw MBCh. B II 2002

Haemostasis Pathway Injury Collagen exposure Platelet adhesion Release reaction Platelet aggregation Primary haemostatic plug Tissue Factor Coagulation Cascade Secondary haemostatic plug Fibrin
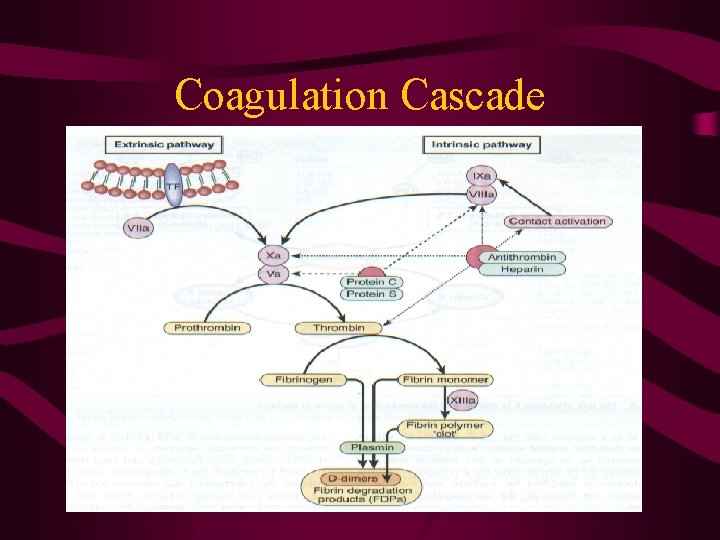
Coagulation Cascade

Integrity of Haemostasis Depends on: 1. Vessel wall 2. Platelets (no. and function) 3. Coagulation factors

Vessel Wall • Release tissue factor that initiates coagulation cascade. • Exposed collagen results in platelet adhesion (using v. WF as a bridge). • Hereditary haemorrhagic telangiectasia • Scurvy • Senile purpura
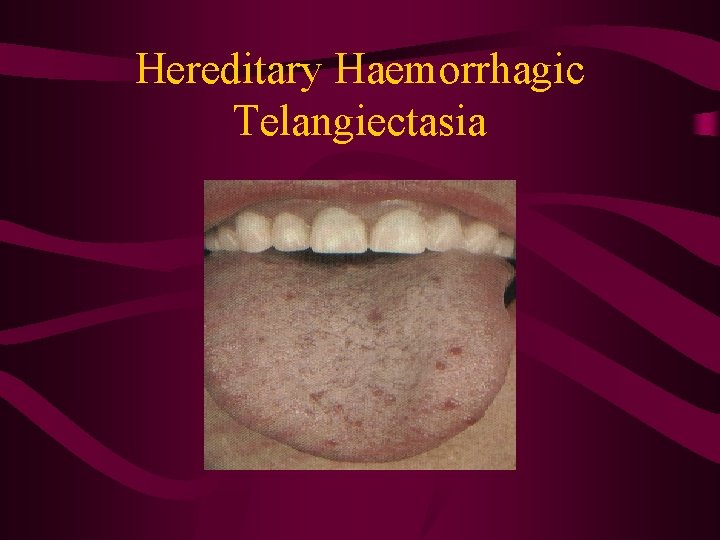
Hereditary Haemorrhagic Telangiectasia

Low Platelet Number • N = 150 – 450 • Excessive bleed / Spontaneous bleed • Mucosal surfaces / Skin • • Immune Mediated Thrombocytopenia Drug induced Haemolytic Uraemic Syndrome DIC

Platelet Dysfunction • • Abnormal platelet aggregation Normal platelet count Excessive / spontaneous bleed Mucosa / Skin • Inherited disorders • Drug induced
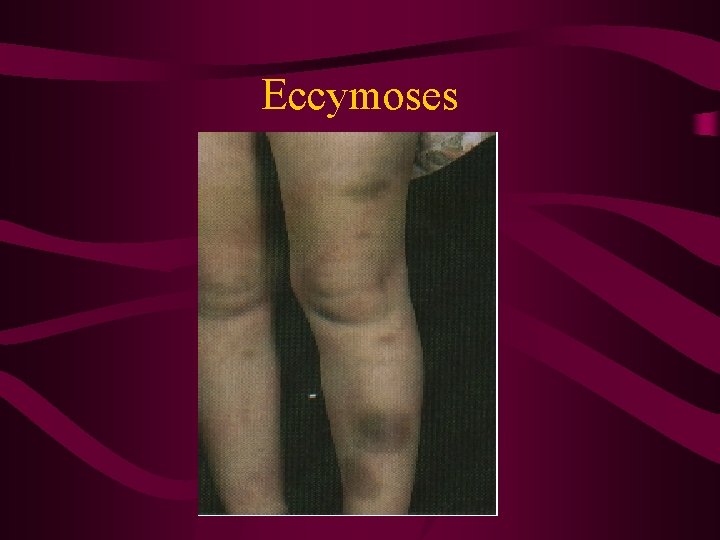
Eccymoses
Coagulation Factors Deficiency • • • Spontaneous bleeding into deep tissues Increased post-traumatic haemorrhage Factor 8 – Haemophilia A Factor 9 – Haemophilia B v. WF – Von Willebrand’s disease Von Willebrand’s Factor: • Protein produced by endothelial cells which mediates platelet adhesion to endothelium and carries factor 8 in plasma.

Haemaphilia A • • • Factor 8 deficiency 50 / million people Sex-linked Most detected in childhood Mild symptoms ~ spontaneous bleed Chronic joint disease after repeated bleed

Haemophilia B • • • Factor 9 deficiency = Christmas disease Also sex-linked Similar presentation as haemophilia A Much rare
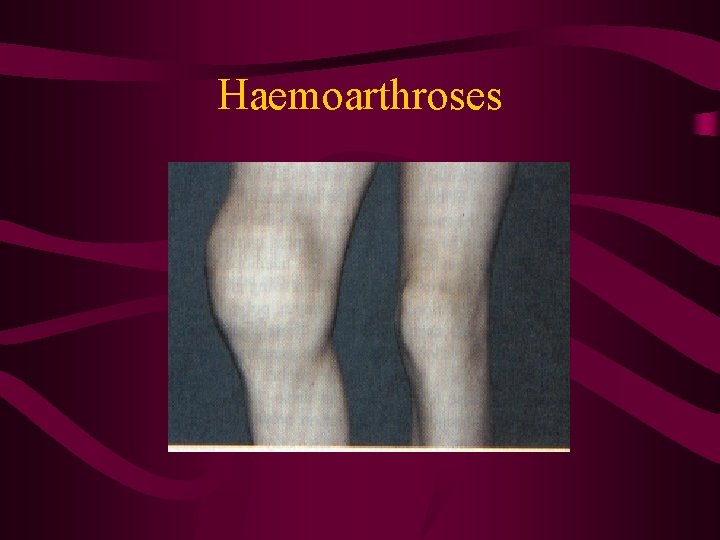
Haemoarthroses

Von Willebrand’s Disease • • • v. WF deficiency Autosomal dominant (F = M) Most common inherited bleeding disorder Bleeding from mucosa Excessive blood loss in trauma Bleeding into deep tissue (rarer)
Liver Disease • Mixed – both coag deficiency and platelet problem • Reduced coag factor synthesis (1, 2, 5, 7, 9, 10) • Cirrhosis Hypersplenism Thrombocytopenia

DIC Generalised activation of coag cascade Wide-spread fibrin formation Thrombosis Low coag factor Bleeding

DIC Consequence of Thrombosis: 1. 2. 3. 4. Tissue infarction Renal impairment CVA PE DVT Consequence of Bleeding: 1. 2. Purpura GI Bleed

DIC Causes of coag cascade activation: 1. Sepsis 2. Disseminated cancer 3. Obstetric complications (e. g. retained product of conception) 4. Fulminant liver disease 5. Anaphylaxis 6. AML

Drug Induced Coag Factor Def Heparin: • Inactivates certain coag factors (e. g. 9 a, 10 a, 11 a, 2) • Also impairs platelet function Warfarin: • Block synthesis of Vit K dependent factors (2, 7, 9, 10)

Other Disorders • • Vitamin K deficiency Autoantibodies to coag factors Haemorrhagic disease of the newborn Massive transfusion

Investigations for Bleeding 1. 2. 3. 4. 5. Platelet Count Bleeding time Activated Partial Thromboplastin Time Prothrombin Time (INR) Plasma level assay

Investigations for Bleeding Condition Test Wall Defect All tests are normal. Low Platelet Low platelet count + Platelet Dysf Normal platelet count + bleeding time Haemophilia APPT + Plasma level v. WD APPT + bleeding time + Liver Disease INR + APPT + platelet count Drug Induced INR + APPT + plasma level DIC All tests are abnormal. plasma level

Management 1. 2. 3. 4. Replace deficiency Treat underlying cause Reversal of drug effects Supportive therapy

Extra Notes on ITP • • • Platelets become coated by autoantibodies Removed by RES reduced lifespan Low platelet count Acute / Chronic Purpura / Spontaneous bleed / Asymptomatic • May resolve spontaneously or require medical treatment
Extra Notes on ITP • Isolated low platelet count < 20 • Increased megakaryocytes in bone marrow • Normal INR + APPT • Increased bleeding time

Extra Notes on ITP Mx: 1. 2. 3. 4. Do nothing Prednisolone Splenectomy Other immunosuppresives

Extra Notes on IPT May be associated with: • Haematological malignancies • Viral infections (e. g. HIV) • C. T. disorders (e. g. SLE) Test for c. t. disorders.

70 -Year-Old with ITP • • Incidental finding in 1993 Platelet count = 60 Asymptomatic Referred to haematologist Test for c. t. disorders U/S for spleen size Bone marrow biopsy

70 -Year-Old with ITP • • Negative for c. t. disorders Spleen size normal Bone marrow: increased megakaryoccytes Continue monitoring (weekly FBC)

70 -Year-Old with ITP • • December 1993 Bruising with minimal trauma Platelet count = 43 Start Prednisolone After 6/52 platelet count 190 Slowly dropped again after withdrawal Asymptomatic

70 -Year-Old with ITP • Continue monitoring • Platelet transfusion if serious bleeding occurs • Consider splenectomy if worsens • Discharged to GP last week
- Slides: 31