HAEMOPOEISIS DEFINITION formation of blood cells from stem

HAEMOPOEISIS
![DEFINITION: [formation of blood cells from stem cells] Process which involves origin, development & DEFINITION: [formation of blood cells from stem cells] Process which involves origin, development &](http://slidetodoc.com/presentation_image_h/fbc1dd23c3f52af8d19ca604f3029e92/image-2.jpg)
DEFINITION: [formation of blood cells from stem cells] Process which involves origin, development & maturation of ØErythrocytes (ERYTHROPOIESIS) Ø leucocytes (LEUCOPOIESIS) Ø& platelets (THROMBOPOIESIS)

Theories of hemopoeisis: i) Monophyletic theory-. (most accepted) ii) All the cell lines originate from a single precursoriii) Pluripotent stem cells i) ii) Polyphyletic theory-. each cell line has a separate precursor stem cell evidence- bone marrow of rat is destroyed using radiation & pluripotent stem cell is injected colonies of all cell lines formed in spleen

Totipotent stem cells- blastocysts of embryo Pluripotent (uncommitted) stem cell- can give rise to any type of blood cell. Best source- umbilical cord blood Committed (progenitor) stem cell- can give rise to a particular cell line
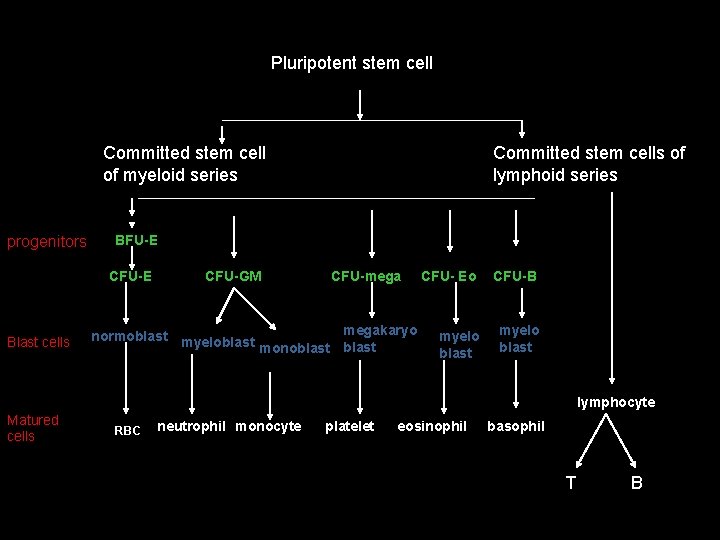
Pluripotent stem cell Committed stem cell of myeloid series progenitors BFU-E CFU-E Blast cells Committed stem cells of lymphoid series CFU-GM CFU-megakaryo normoblast myeloblast monoblast CFU- Eo CFU-B myelo blast lymphocyte Matured cells RBC neutrophil monocyte platelet eosinophil basophil T B
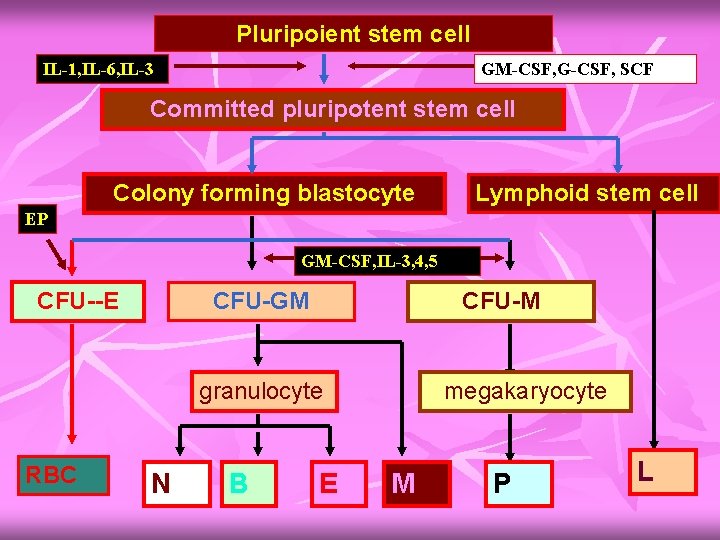
Pluripoient stem cell IL-1, IL-6, IL-3 GM-CSF, G-CSF, SCF Committed pluripotent stem cell Colony forming blastocyte Lymphoid stem cell EP GM-CSF, IL-3, 4, 5 CFU--E CFU-GM CFU-M granulocyte RBC N B E megakaryocyte M P L

n About 75% of cells belong to WBC producing ‘myeloid series’ and only 25% belong to RBC ‘erythroid series’ n Types of differentiation determined by the influence of various ‘Interleukins’ and ‘colony stimulating factors’.

ERYTHROPOISIS v. DEFINITION v. SITE OF ERYTHROPOIESIS v. STAGES OF ERYTHROPOIESIS v. CHANGES DURING ERYTHROPOIESIS v. FACTORS REGULATING ERYTHROPOIESIS

DEFINITION: production & maturation of RBCs Site of production: A) During intra-uterine life: starts in 3 rd week -mesoblastic stage: 3 rd week to 3 rd month; occurs in mesoderm of yolk sac; intravascular and nucleated RBCs -hepatic stage: 3 rd to 5 th month; occurs in liver and spleen -myeloid stage: bone marrow starts producing RBCs B) After birth: - exclusively in bone marrow Up to 5 yrs- all bones >20 yrs- flat bones and ends of long bones.
In fetal life Mesoblastic stage Hepatic stage Myeloid stage
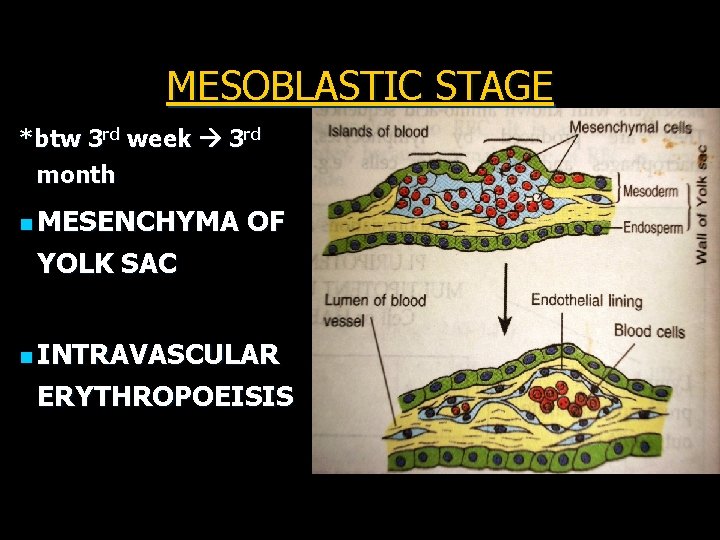
MESOBLASTIC STAGE *btw 3 rd week 3 rd month n MESENCHYMA OF YOLK SAC n INTRAVASCULAR ERYTHROPOEISIS
n. HEPATIC STAGE Liver, Spleen and Lymph nodes n. MYELOID STAGE Red bone marrow
In post natal life: In new born: All bones , red bone marrow (mainly) Liver and spleen In children: Red bone marrow In adults: 18 tp 20 yrs- from red bone marrow of skull, vertebrae, ribs, sternum, pelvis
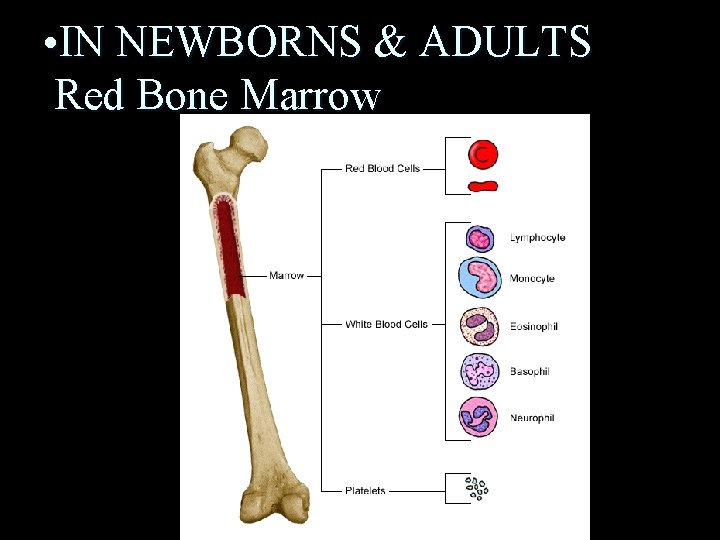
• IN NEWBORNS & ADULTS Red Bone Marrow

n n n Red Bone Marrow: hematopoietically active. The marrow contains both Erythroid (RBC) and leukocyte (WBC) precursors as well as platelet precursors Yellow Bone Marrow: is inactive, fatty marrow.
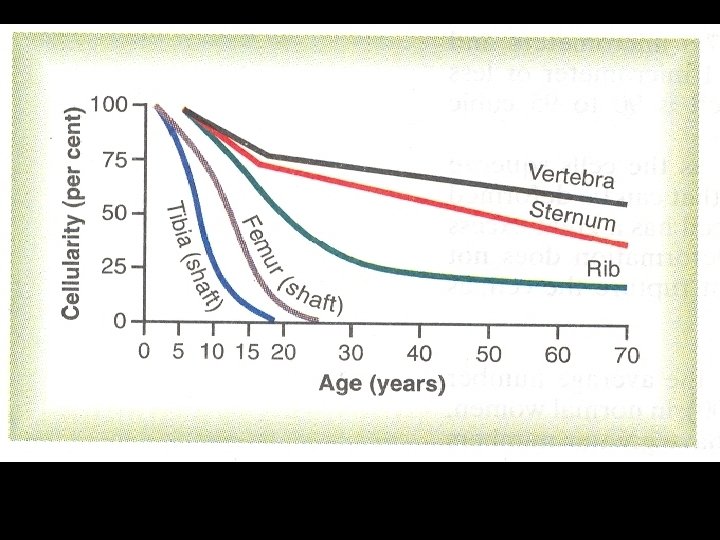

Stages of erythropoiesis: 1. 2. 3. 4. 5. 6. Proerythroblast Early normoblast Intermediate normoblast Late normoblast Reticulocyte Mature RBC

Stages of erythropoiesis Proerythroblast (megaloblast) : diameter 15 -20µ Ø-cytoplasm basophilic Ø-nucleus large and occupies most of the cell, distinct nucleoli Ø-Hb absent Ø-active mitoses only during stress Ø-vit B 12 & folic acid required for conversion to next stage Early Normoblast (basophilic erythroblast) : -diameter 11µ -17µ -nucleoli absent or rudimentary -dense nucleus & chromatin -cytoplasm basophilic -active mitoses
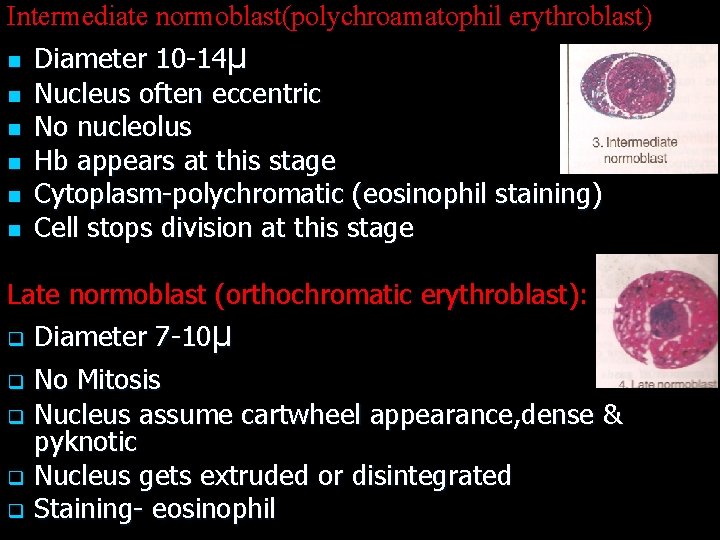
Intermediate normoblast(polychroamatophil erythroblast) n Diameter 10 -14µ n Nucleus often eccentric n No nucleolus n Hb appears at this stage n Cytoplasm-polychromatic (eosinophil staining) n Cell stops division at this stage Late normoblast (orthochromatic erythroblast): q Diameter 7 -10µ q q No Mitosis Nucleus assume cartwheel appearance, dense & pyknotic Nucleus gets extruded or disintegrated Staining- eosinophil

Reticulocyte n Almost same size as mature RBC(8 -9µ) n On vital staining, a network of reticulum seen in cytoplasm n Normal count is about 1% of total RBCs n In New born-2 -6% n Haemolysis- 25 -30% Mature RBC Diameter-7. 2µ Circular & non-nucleated, biconcave disc n

RBC (erythrocyte) Normal count-men- 5. 4 millon/mm 3 -women- 4. 8 millon/mm 3 Life span: about 120 days Site of destruction- RES (predominantly in spleen) General changes Reduction in the cell size Disappearance of nucleus Appearance of Hb Changes in staining characteristics Duration: about 7 days

PHSC Pluripotent Hemopoietic stem cell IL-1, IL-6, IL-3 GM CSF erythro BFU-E Burst Forming Unit Erythrocyte E R Y CFU-E Colony Forming Unit Erythrocyte GM CSF erythro PROERYTHROBLAST BASOPHILIC ERYTHROBLAST POLYCHROMATOPHILIC ERYTHROBLAST T H R O P O I ORTHOCHROMATIC ERYTHROBLAST RETICULOCYTE ERYTHROCYTE E S I S
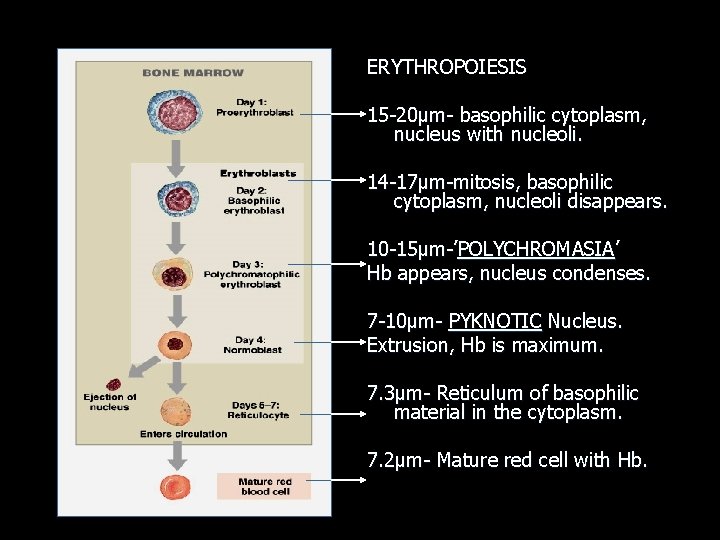
ERYTHROPOIESIS 15 -20µm- basophilic cytoplasm, nucleus with nucleoli. 14 -17µm-mitosis, basophilic cytoplasm, nucleoli disappears. 10 -15µm-’POLYCHROMASIA’ Hb appears, nucleus condenses. 7 -10µm- PYKNOTIC Nucleus. Extrusion, Hb is maximum. 7. 3µm- Reticulum of basophilic material in the cytoplasm. 7. 2µm- Mature red cell with Hb.
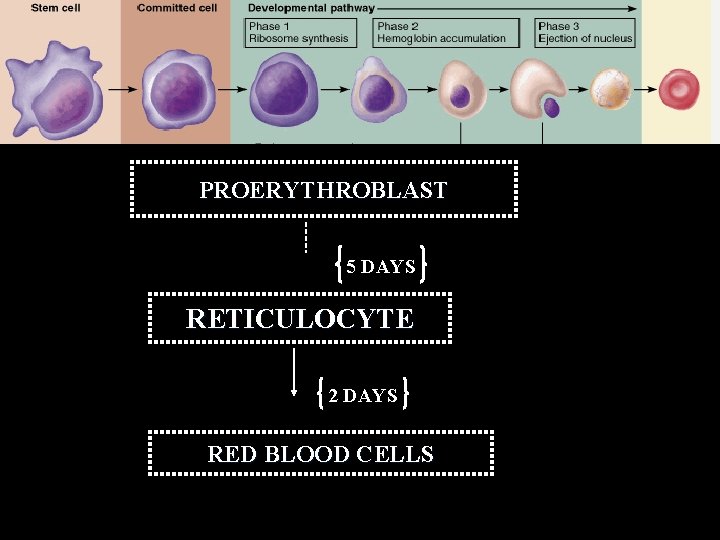
PROERYTHROBLAST 5 DAYS RETICULOCYTE 2 DAYS RED BLOOD CELLS

Factors affecting erythropoises
Regulation of Erythropoiesis General Factors Hypoxia Maturation Factors 1. Dietary Factors 2. Castles intrinsic Factor 3. Extrinsic Factor
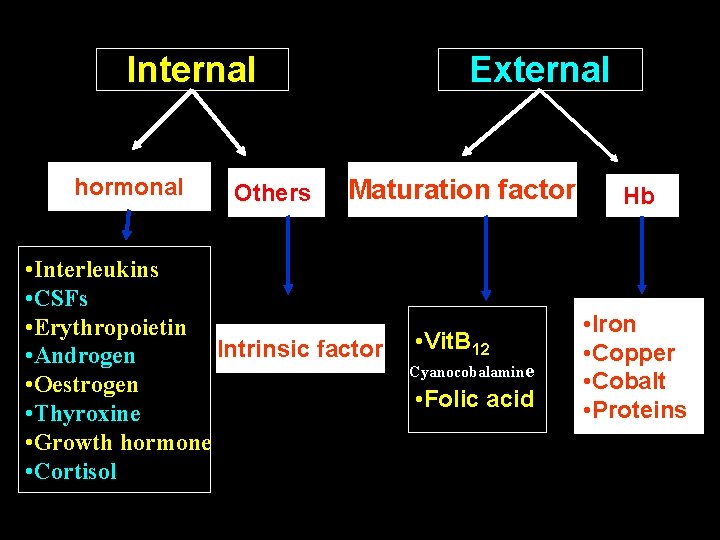
Internal hormonal Others External Maturation factor • Interleukins • CSFs • Erythropoietin Intrinsic factor • Androgen • Oestrogen • Thyroxine • Growth hormone • Cortisol • Vit. B 12 Cyanocobalamine • Folic acid Hb • Iron • Copper • Cobalt • Proteins
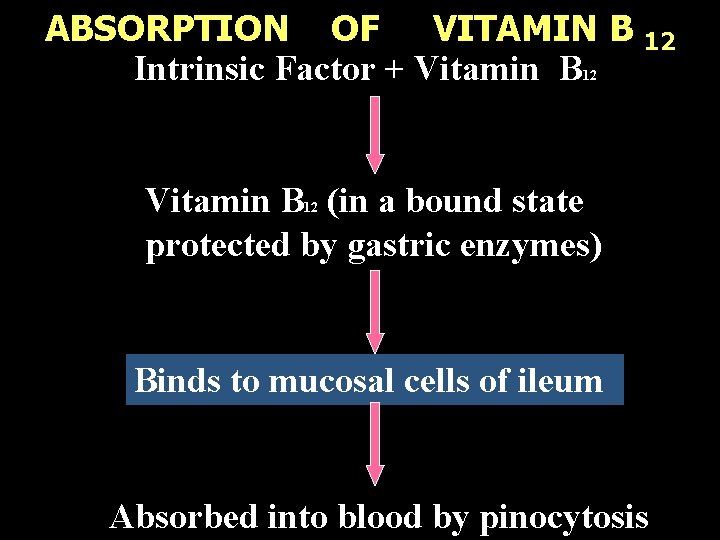
ABSORPTION OF VITAMIN B Intrinsic Factor + Vitamin B 12 12 Vitamin B (in a bound state protected by gastric enzymes) 12 Binds to mucosal cells of ileum Absorbed into blood by pinocytosis
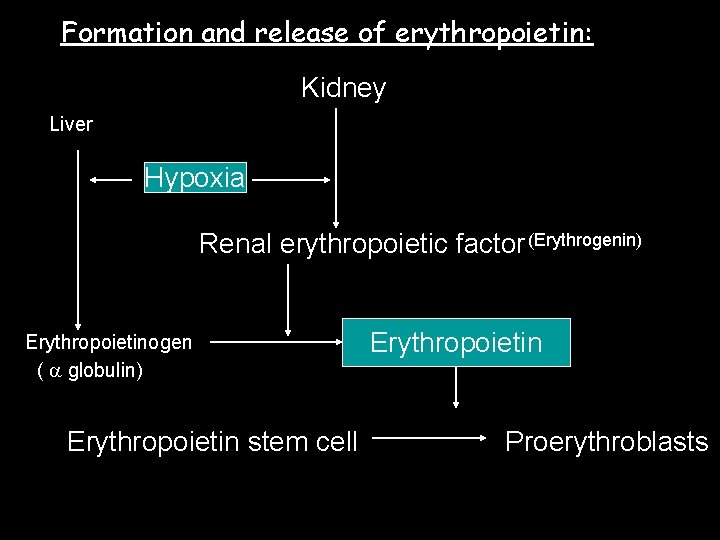
Formation and release of erythropoietin: Kidney Liver Hypoxia Renal erythropoietic factor (Erythrogenin) Erythropoietinogen ( globulin) Erythropoietin stem cell Proerythroblasts

ERYTHROPOEITIN n Stimuli for production v hypoxia, v high altitude, v anemia, v chronic lung or heart diseases, v catecholamines, v prostaglandins & v androgens. n Formed in hours, RBC’s take 2 -3 days to appear in peripheral blood.

- Slides: 31