Gut microbiota and immunity CONTE NTS immunity microor
Gut microbiota and immunity 答辩人:本硕二班二组
CONTE NTS immunity →microor ganism Background Modulate immune cell differentiation Tweak the production of immune mediators Induce the development of lymphoid structure
Role Function Challenge Background

Background Role In adult intestine, a total of about 1014 bacterial cells are present, which is ten times the number of human cells in the body. In fact, the metabolic capacity of gut microbiota equals that of the liver, and the gut microbiota can therefore be considered as an additional organ. 1. Facilitate the metabolism of otherwise indigestible polysaccharides and produce essential vitamins. 2. They are required for the development and differentiation of host’s intestinal epithelium and immune system. 3. They confer protection against invasion by opportunistic pathogens. ect Funct ion

Background Challe nge The dynamic fluctuations in the microbiota and their close proximity to epithelial tissue represent a massive challenge to immune system as microbial growth has to be restricted to a beneficial homeostasis. Furthermore, activation of the host immune system has to be controlled to circumvent the detrimental effects of chronic inflammation.

Self or non-self Mucosal immune system → Immunity~microbiota Requirements

Immunity~ microbiota Self 1. The realization that we live in a microbially dominated world and in fact benefit greatly from our microbiota has led to a paradigm shift in immunology. 2. Thus the definition of self in the superorganism theory has been extended to incorporate the constituents of both our own body and our microbiota. 3. Tolerance rather than responsiveness 1. Mucosal immune system has to be tolerant towards the huge number of mutualistic microorganisms. 2. It has to assure a beneficial microbiota composition by keeping pathobionts in check, restricting microbial overgrowth and reacting to penetrating microorganisms. Requir ement s

Gut-associated lymphoid tissue → microbiota~lymphoid structure
Inclusion Peyer's patches,(PP) Mesenteric lymph nodes Isolated lymphoid follicles,(ILFs) GALT Vermiform appendix,(VA). . .

Process Forma tion GALT is initiated pre-natally in the sterile environment of the fetus through induction by lymphoid tissue inducer (LTi) cells. Maturation of these tissues, including an increase in tissue size and the development of germinal centres, depends on postnatal microbial colonization Matura tion
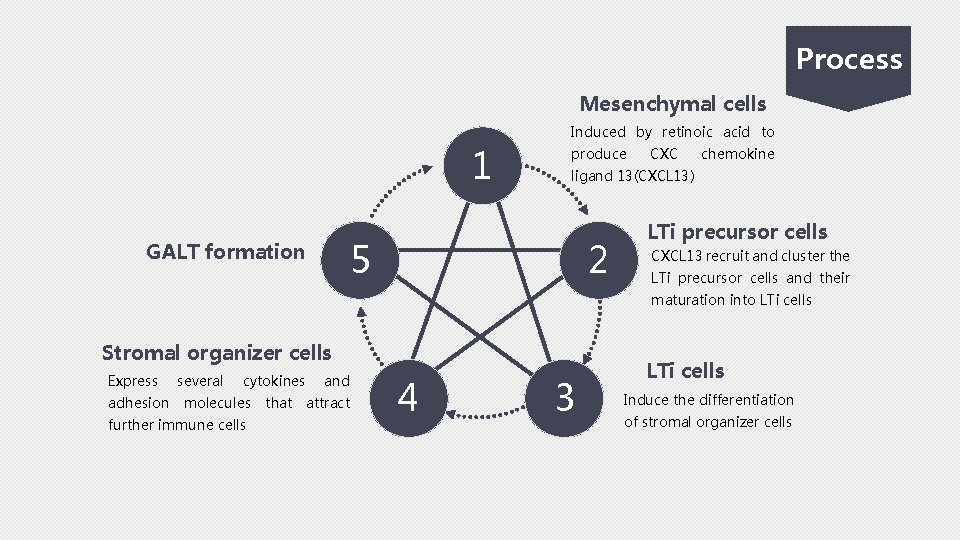
Process Mesenchymal cells 1 Induced by retinoic acid to produce chemokine ligand 13(CXCL 13) 5 GALT formation CXC 2 LTi precursor cells CXCL 13 recruit and cluster the LTi precursor cells and their maturation into LTi cells Stromal organizer cells Express adhesion several cytokines molecules further immune cells that and attract 4 3 LTi cells Induce the differentiation of stromal organizer cells
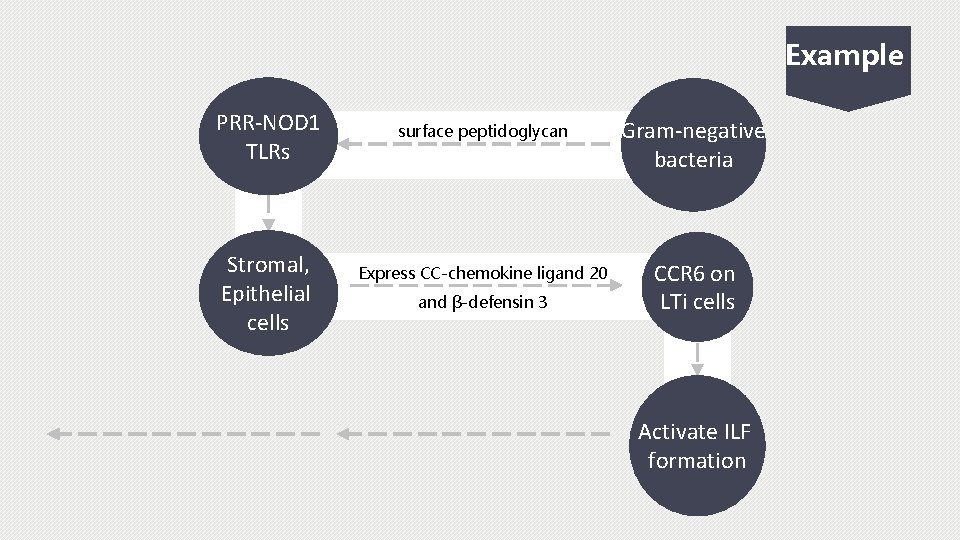
Example PRR-NOD 1 TLRs Stromal, Epithelial cells surface peptidoglycan Gram-negative bacteria Express CC-chemokine ligand 20 CCR 6 on LTi cells and β-defensin 3 Activate ILF formation

Ig. A AMPs microbiota~immune mediators
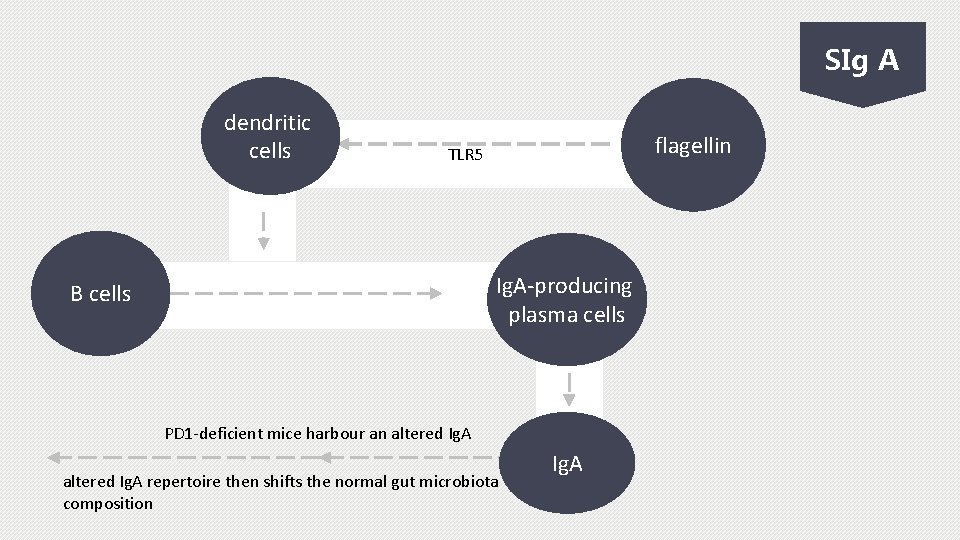
SIg A dendritic cells flagellin TLR 5 Ig. A-producing plasma cells B cells PD 1 -deficient mice harbour an altered Ig. A repertoire then shifts the normal gut microbiota composition Ig. A

AMPs produ ction 1. They are produced by IECs as a consequence of their tight contact with a dense and highly diverse microbial community. 2. It not only help to sustain host–microorganism segregation, but also affect the microbiota composition. 1. defensins C-type lectins (such as REG 3β and REG 3γ) 2. ribonucleases (for example, angiopoietin 4 (ANG 4)) 3. S 100 proteins (for example, psoriasin (also known as S 100 A 7)) classi ficati on
RORγt+Nkp 46 -LTi-like cell i. NKT cells → microbiota~immune cell differentiation specific T cell

1. Promote intestinal barrier function by modulating mucosal homeostasis RORγt+Nkp 46 -LTi-like cell ↓IL-23 and intestinal microbiota RORγt+Nkp 46+NK-like cell ↓ IL-22

IL-22 1. Promote the integrity of the intestinal barrier Reduce bacterial infiltration by inducing epithelial repair (1)STAT 3 (2)Produce antimicrobial proteins 2.
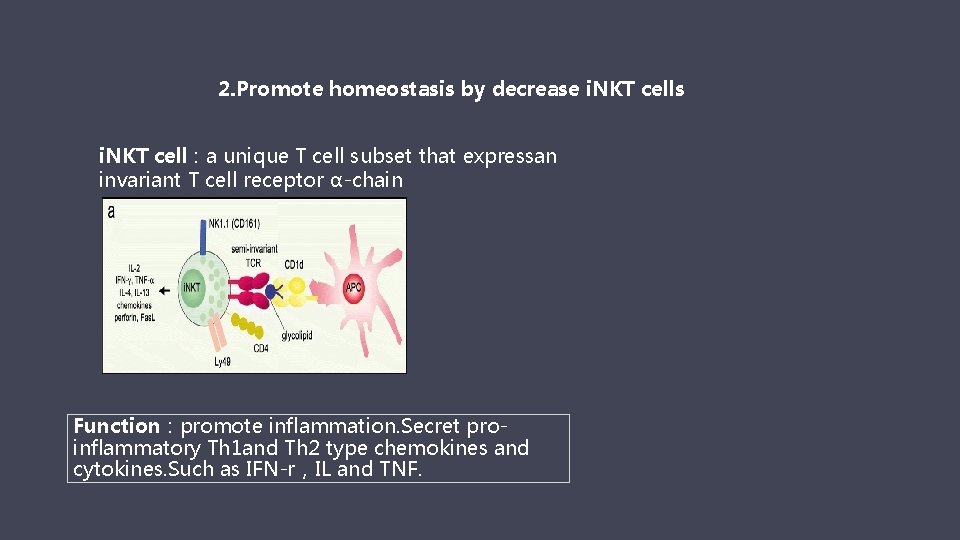
2. Promote homeostasis by decrease i. NKT cells i. NKT cell:a unique T cell subset that expressan invariant T cell receptor α-chain Function:promote inflammation. Secret proinflammatory Th 1 and Th 2 type chemokines and cytokines. Such as IFN-r,IL and TNF.
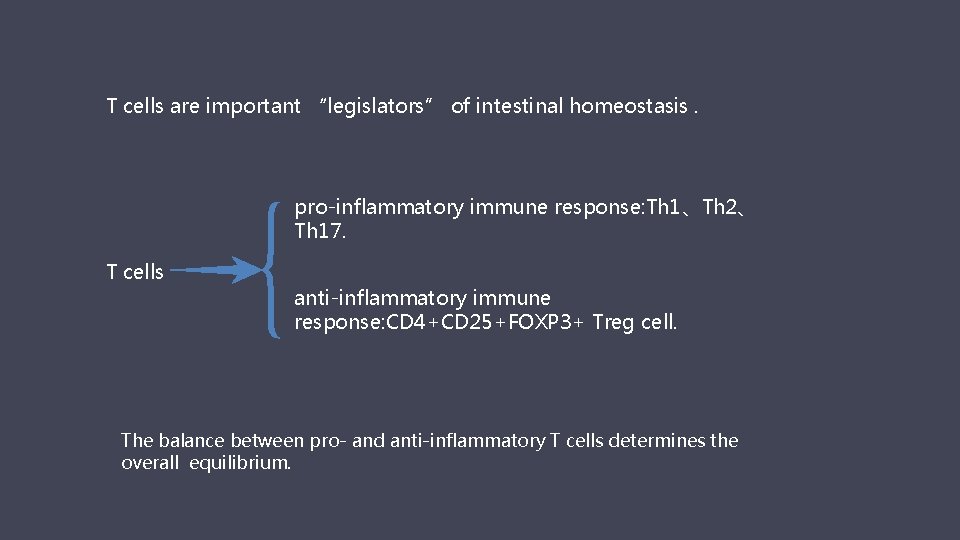
T cells are important “legislators” of intestinal homeostasis. pro-inflammatory immune response: Th 1、Th 2、 Th 17. T cells anti-inflammatory immune response: CD 4+CD 25+FOXP 3+ Treg cell. The balance between pro- and anti-inflammatory T cells determines the overall equilibrium.

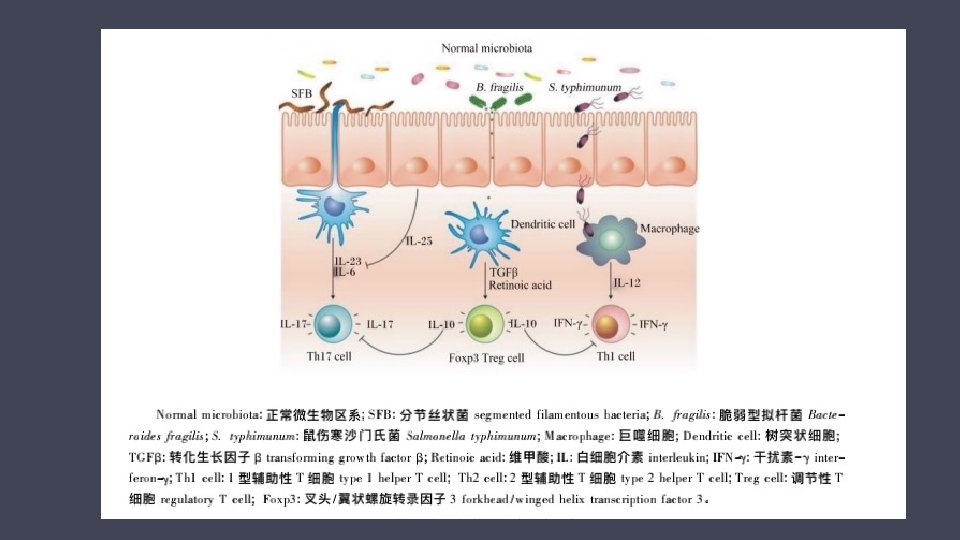
3. Several gut microbiota drive specific T cell response. (1)Bacteroides fragilis(脆弱拟杆菌) (2)Clostridia(梭状芽孢杆菌) (3)Segmented filamentous bacteria/SFB (分节丝状菌)
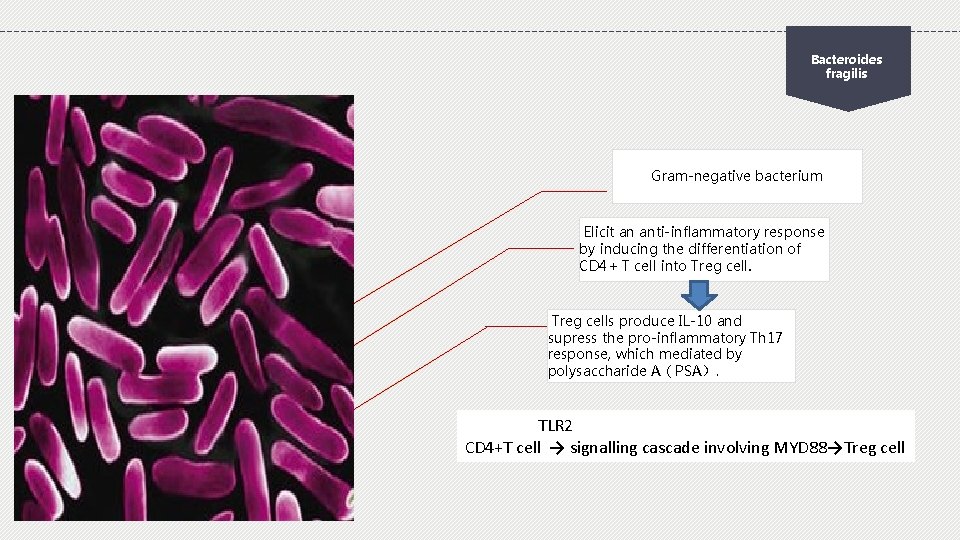
Bacteroides fragilis Gram-negative bacterium Elicit an anti-inflammatory response by inducing the differentiation of CD 4+ T cell into Treg cells produce IL-10 and supress the pro-inflammatory Th 17 response, which mediated by polysaccharide A(PSA). TLR 2 CD 4+T cell → signalling cascade involving MYD 88→Treg cell
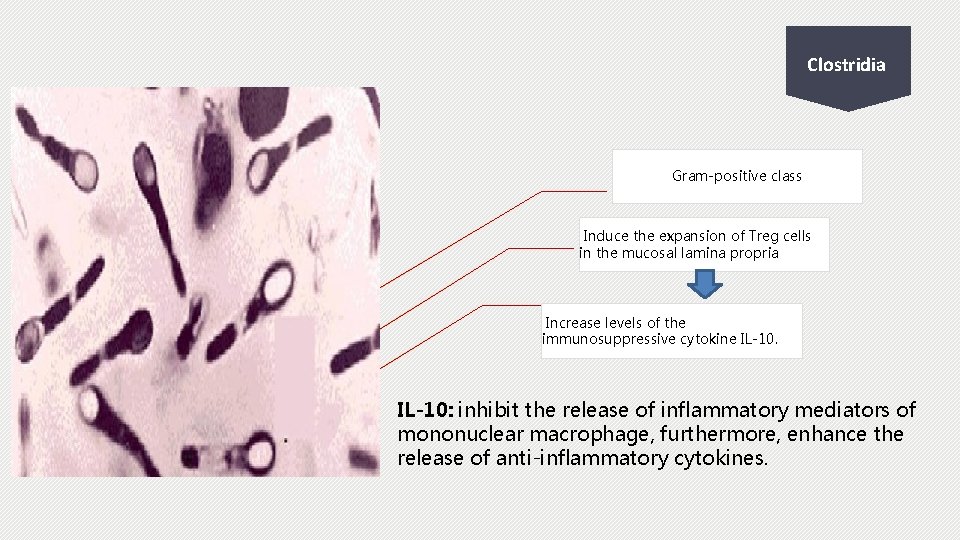
Clostridia Gram-positive class Induce the expansion of Treg cells in the mucosal lamina propria Increase levels of the immunosuppressive cytokine IL-10: inhibit the release of inflammatory mediators of mononuclear macrophage, furthermore, enhance the release of anti-inflammatory cytokines.

SFB Elicit a pro-inflammatory immune response by promoting the differention of Th 17 cell and, to a lesser extent, Th 1 cell SFB reside are in contact with epithelial cells to invade those cells Local actin poymerization in the epithelium Initiate a signalling events that activate the differentiation of Th 17 cell. Scanning electron microscopy of intestine in mice colonized with SFB

THANKS!
- Slides: 26