GRAM POSITIVE COCCI Staphylococci TAXONOMY Family Micrococcaceae Genus

































- Slides: 46

GRAM POSITIVE COCCI

Staphylococci

TAXONOMY Family: Micrococcaceae Genus: Staphylococcus Coagulase positive Coagulase negative Micrococcus

GENUS STAPHYLOCOCCUS Coagulase positive S. aureus Coagulase negative S. epidermidis S. saprophyticus S. haemolyticus S. albus S. citrus

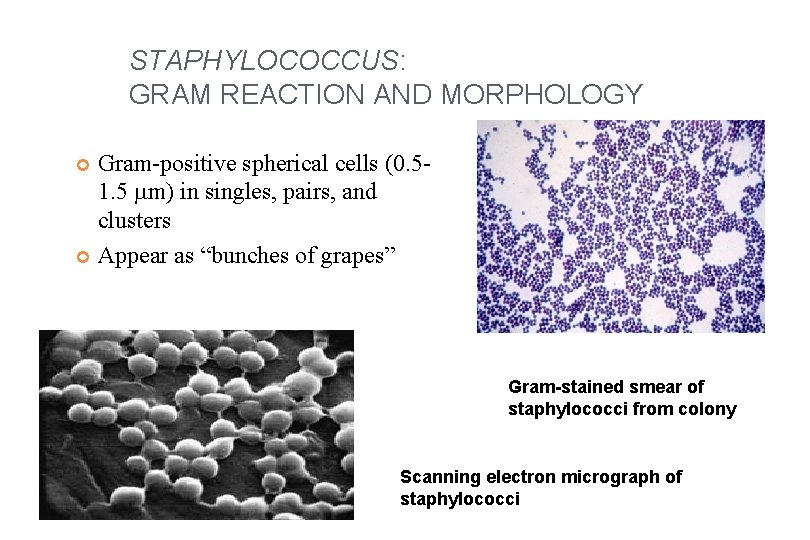
STAPHYLOCOCCUS: GRAM REACTION AND MORPHOLOGY Gram-positive spherical cells (0. 51. 5 mm) in singles, pairs, and clusters Appear as “bunches of grapes” Gram-stained smear of staphylococci from colony Scanning electron micrograph of staphylococci

STAPHYLOCOCCUS: GENERAL CHARACTERISTICS Nonmotile Non–spore-forming Nonencapsulated Catalase-producing Oxidase: negative Glucose fermenters Primarily aerobic, some facultatively anaerobic

STAPHYLOCOCCUS: GENERAL CHARACTERISTICS Bacitracin resistant Grow on agar that contains peptone Inhibited by media that has high bile salt concentration Some are ß-hemolytic Colony morphology: buttery looking, cream or white colored

STAPHYLOCOCCUS AUREUS Primary pathogen of the genus Habitat: Anterior nares (carriers) Colonization: axilla, vagina, pharynx Produce superficial to systemic infections Skin Bacterial sepsis Hospital acquired infections

VIRULENCE FACTORS OF S. AUREUS Enterotoxins Cytolytic toxins Enzymes Protein A

VIRULENCE FACTORS: ENTEROTOXINS Enterotoxins: Heat-stable exotoxins that cause diarrhea and vomiting Exotoxin: protein produced by a bacteria and released into environment Heat stable @ 100 o C for 30 minutes Implications Food poisoning Toxic shock syndrome Pseudomembranous enterocolitis

TYPES OF ENTEROTOXINS Epidermolytic toxin: Exfoliatin TSST-1: Toxic shock syndrome toxin-1 Multisystem disease Stimulates T cell production & cytokines Cytolytic Toxins Affects RBCs and WBCs Hemolytic toxins: alpha, beta, gamma, delta Panton-Valentine leukocin, lethal to WBCs

VIRULENCE FACTORS: EXTRACELLULAR ENZYMES Hyaluronidase: Staphylokinase: Fibrinolysin which allows spread of infection Coagulase: Hydrolyzes hyaluronic acid in connective tissue allowing spread of infection Virulence marker Lipase: Allows colonization by acting on lipids present on the surface of the skin.

VIRULENCE FACTORS: EXTRACELLULAR ENZYMES (CON’T) Penicillinase: Confers resistance DNase: Degrades DNA Beta-lactamase: Cuts the beta lactam wall of certain antibiotics

VIRULENCE FACTORS: PROTEIN A Protein A: Found in cell wall Binds to Fc part of Ig. G Blocks phagocytosis

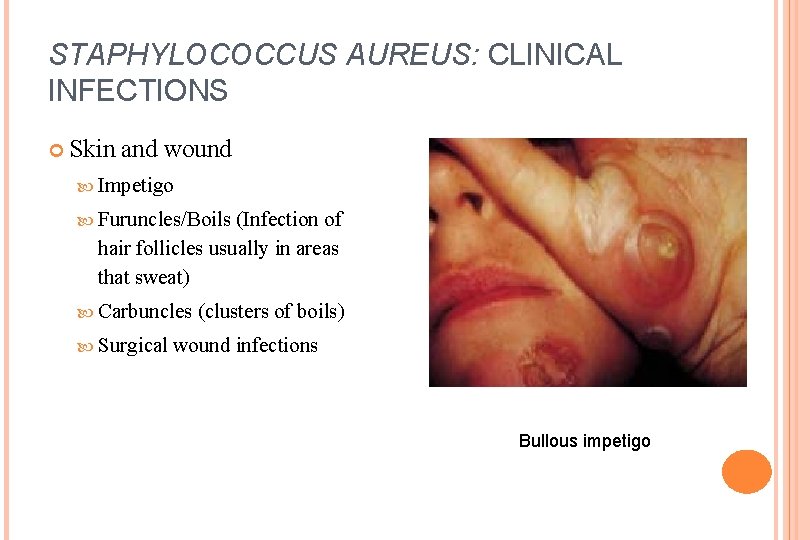
STAPHYLOCOCCUS AUREUS: CLINICAL INFECTIONS Skin and wound Impetigo Furuncles/Boils (Infection of hair follicles usually in areas that sweat) Carbuncles Surgical (clusters of boils) wound infections Bullous impetigo

STAPHYLOCOCCUS AUREUS: CLINICAL INFECTIONS (CON’T) Skin and wound Scalded skin syndrome= Ritter’s disease Extensive exfoliative dermatitis Young children and newborns Toxic Shock Syndrome Multisystem disease Affects women, and children

STAPHYLOCOCCUS AUREUS: CLINICAL INFECTIONS Food poisoning Source is infected food handler Enterotoxin A the most common cause Foods affected include meat, dairy products, bakery goods with cream fillings, and salads made with eggs.

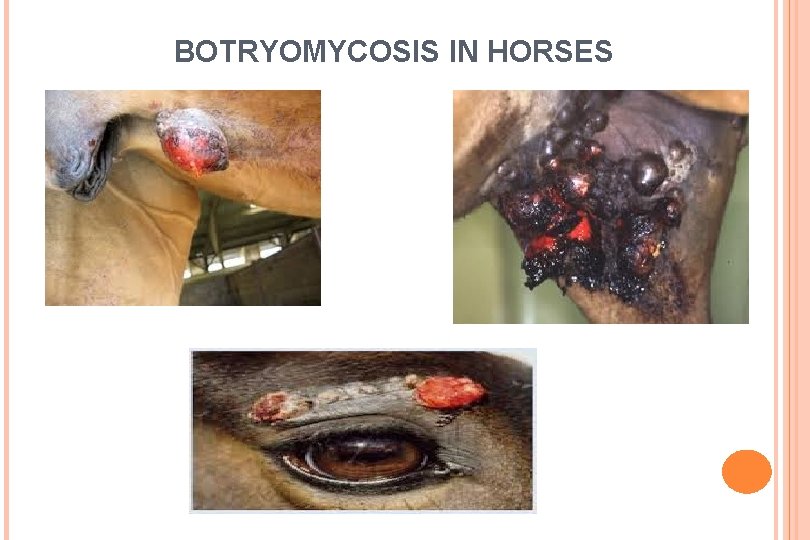
BOTRYOMYCOSIS IN HORSES

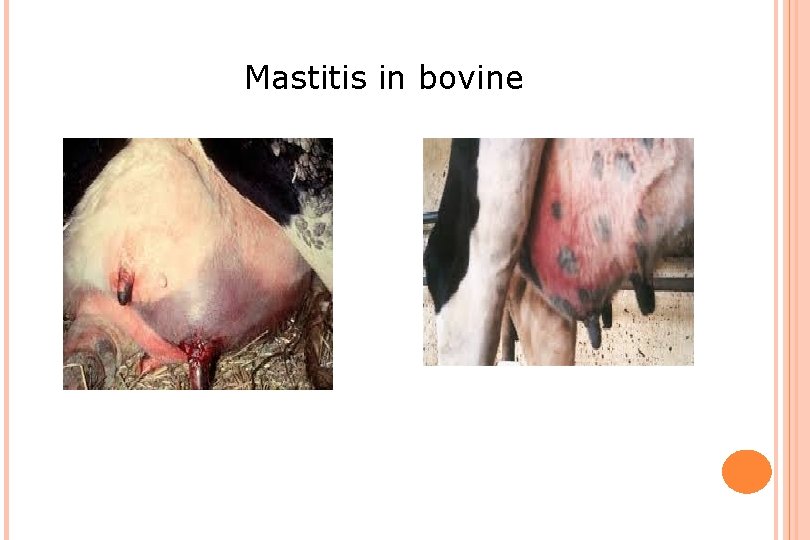
BACTERIAL INFECTION: STAPHYLOCOCCI Staph aureus Gangrenous mastitis: alpha toxin Spread by milking equipment and milker’s hands Fibrous tissue replacement low production Dry cow therapy Persistent, difficult to eliminate Other staph Found normally on skin Lowers milk yield Easily responds to antibiotics Relapse frequently seen

Mastitis in bovine

Bumble foot in birds

COAGULASE-NEGATIVE STAPHYLOCOCCI Found as indigenous flora Presence can indicate contamination Seeing an increase in immunocompromised

COAGULASE-NEGATIVE STAPHYLOCOCCI Habitat: Skin and mucous membranes Common human isolates S. epidermidis S. saprophyticus S. haemolyticus S. albus

COAGULASE-NEGATIVE STAPHYLOCOCCI: STAPHYLOCOCCUS EPIDERMIDIS Predominantly hospital acquired infections Skin flora gets introduced by catheters, heart valves, CSF shunts Produces a slime layer that helps adherence and avoidance of phagocytosis

COAGULASE-NEGATIVE STAPHYLOCOCCI: STAPHYLOCOCCUS SAPROPHYTICUS urogenital tract Rarely present in other skin areas or mucous membranes Urine cultures If present in low amounts, it is still considered significant

COAGULASE-NEGATIVE STAPHYLOCOCCI: STAPHYLOCOCCUS HAEMOLYTICUS Habitat: skin and mucous membranes Rarely implicated in infections Associated with wound infections, bacteremia, and endocarditis

LABORATORY DIAGNOSIS: SPECIMEN COLLECTION AND HANDLING Samples must be taken from the actual site of infection Prevent delay in transport of collected material from infected sites Transport in appropriate collection device that would prevent drying and minimize growth of contaminating organisms

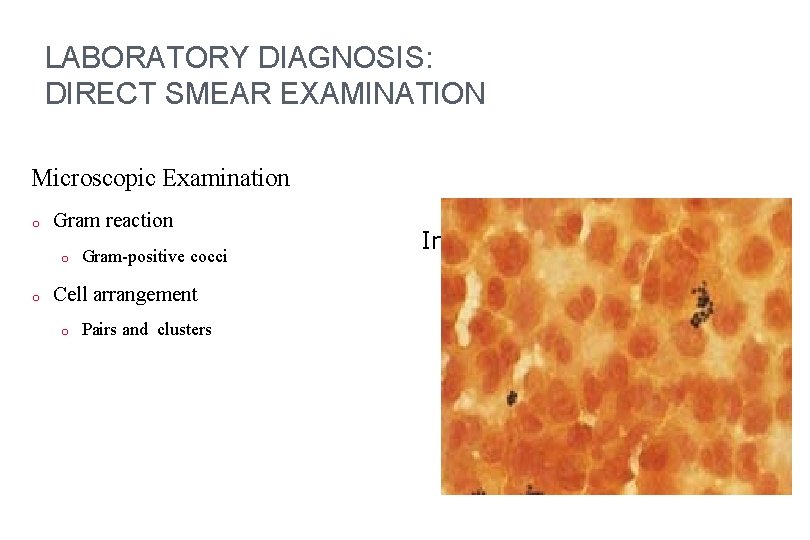
LABORATORY DIAGNOSIS: DIRECT SMEAR EXAMINATION Microscopic Examination o Gram reaction o o Gram-positive cocci Cell arrangement o Pairs and clusters Insert Figure 10 -1

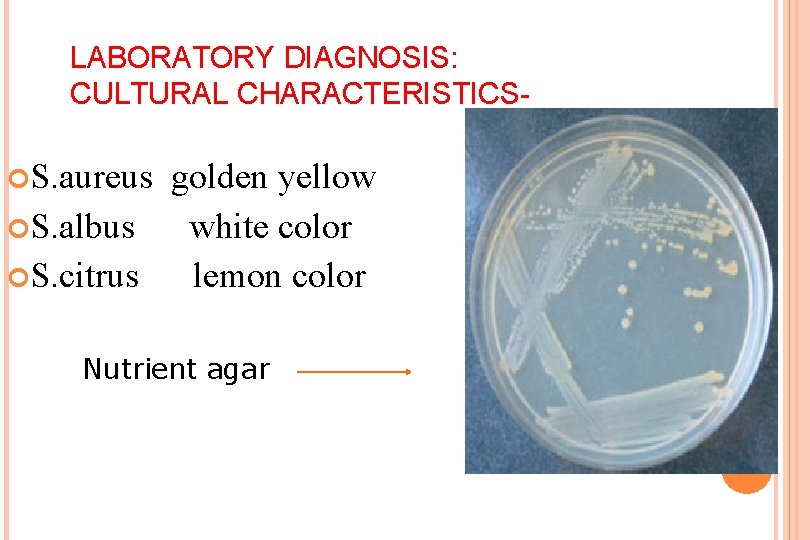
LABORATORY DIAGNOSIS: CULTURAL CHARACTERISTICS S. aureus golden yellow S. albus white color S. citrus lemon color Nutrient agar

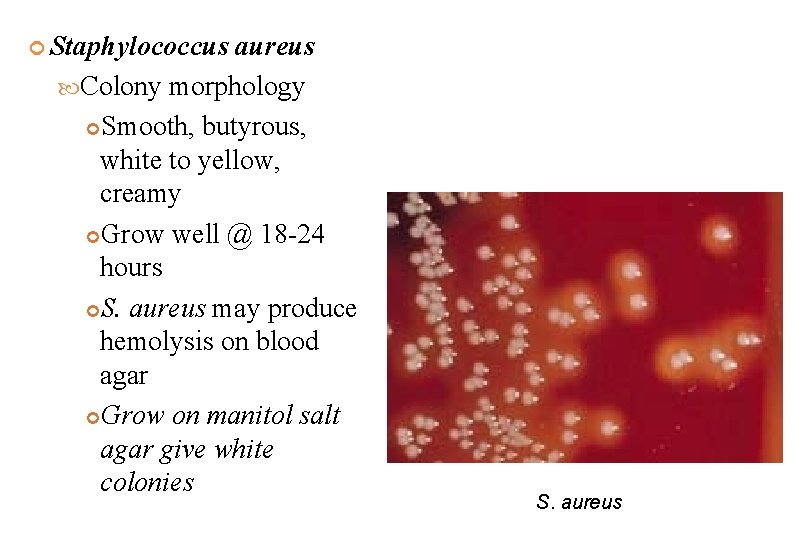
Staphylococcus aureus Colony morphology Smooth, butyrous, white to yellow, creamy Grow well @ 18 -24 hours S. aureus may produce hemolysis on blood agar Grow on manitol salt agar give white colonies S. aureus

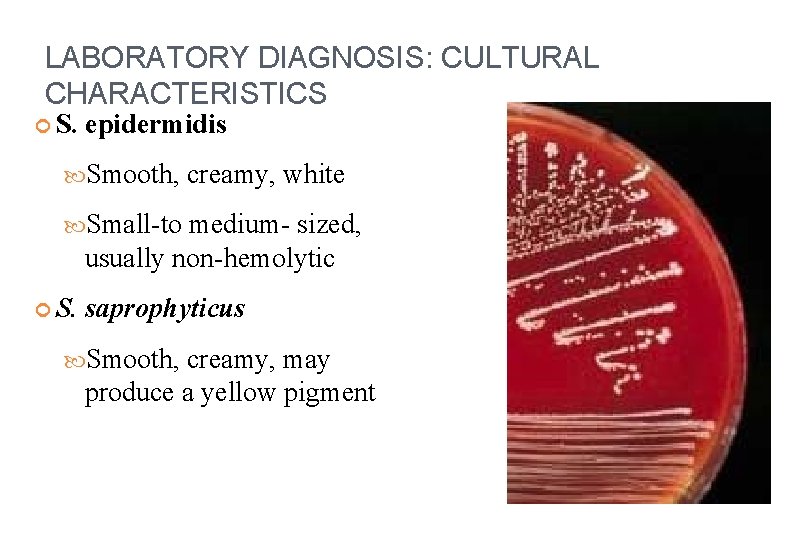
LABORATORY DIAGNOSIS: CULTURAL CHARACTERISTICS S. epidermidis Smooth, creamy, white Small-to medium- sized, usually non-hemolytic S. saprophyticus Smooth, creamy, may produce a yellow pigment

S. Albus give white colonies S. Citrus give lemon colonies

IDENTIFICATION TESTS: CATALASE Principle: tests for enzyme catalase 2 H 2 O 2 2 H 2 O + O 2 Procedure Smear a colony of the organism to a slide Drop H 2 O 2 onto smear Observe

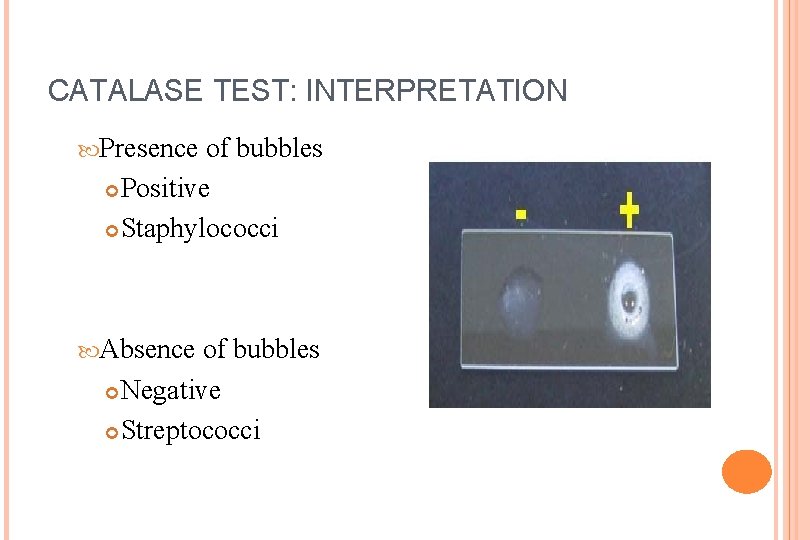
CATALASE TEST: INTERPRETATION Presence of bubbles Positive Staphylococci Absence of bubbles Negative Streptococci

IDENTIFICATION TEST: SLIDE COAGULASE TEST Differentiates members within the Staphylococci Detects clumping factor found in S. aureus Procedure Place a drop of sterile water on a slide and emulsify a colony Add a drop of rabbit plasma to the suspension Observe Agglutination = Positive No agglutination= Negative

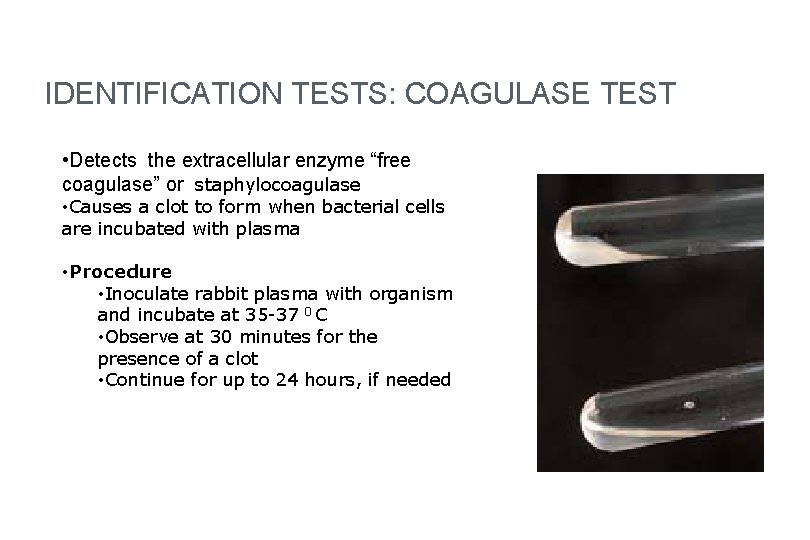
IDENTIFICATION TESTS: COAGULASE TEST • Detects the extracellular enzyme “free coagulase” or staphylocoagulase • Causes a clot to form when bacterial cells are incubated with plasma • Procedure • Inoculate rabbit plasma with organism and incubate at 35 -37 0 C • Observe at 30 minutes for the presence of a clot • Continue for up to 24 hours, if needed

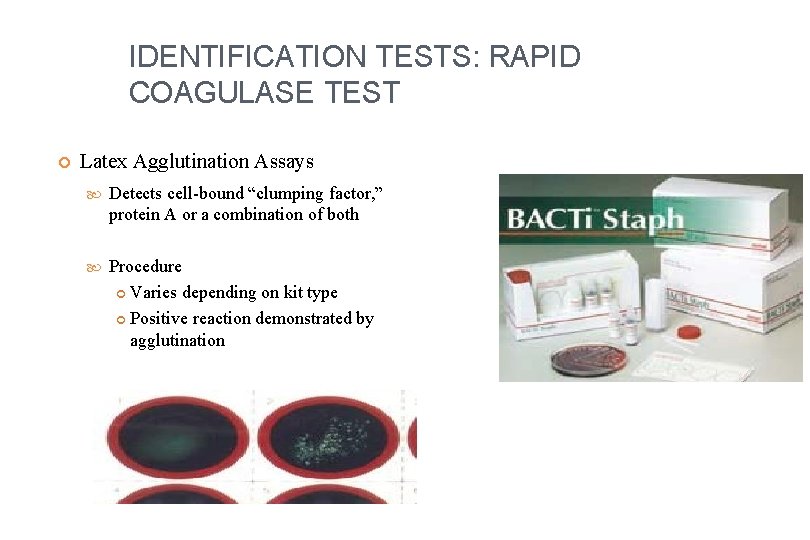
IDENTIFICATION TESTS: RAPID COAGULASE TEST Latex Agglutination Assays Detects cell-bound “clumping factor, ” protein A or a combination of both Procedure Varies depending on kit type Positive reaction demonstrated by agglutination

NOVOBIOCIN SUSCEPTIBILITY TEST Test to differentiate coagulasenegative staphylococci from S. saprophyticus from urine samples S. saprophyticus is resistant (top) Other CNS are susceptible

MICROCOCCUS Rarely produces disease Found in environment and indigenous skin flora Catalase + Coagulase Produces yellow pigment Microdase disc differentiate between Staph & Micrococcus

ANTIMICROBIAL SUSCEPTIBILITY For non–beta-lactamase producing S. aureus Use pencillin Penicillinase-resistant synthetic penicillins (methicillin, nafcillin, oxacillin, dicloxacillin) Beta-lactamase producers break down the beta-lactam ring of penicillin so it inactivates antibiotic before it acts on bacterial cells

METHICILLIN-RESISTANT STAPHYLOCOCCI MRSA Methicillin-resistant S. epidermidis MRSE Infection control Barrier protection Contact isolation Handwashing Treat with vancomycin Test for susceptibility with cefoxitin disk

METHICILLIN-RESISTANT STAPHYLOCOCCI (CONT’D) mec. A gene Encodes penicillin-binding proteins (PBPs) Causes drug ineffectiveness Gold standard Nucleic acid probe or PCR for the mec A gene

VANCOMYCIN-RESISTANT STAPHYLOCOCCI VRSA= vancomycin resistant Staphylococcus aureus VISA= vancomycin intermediate Saphylococcus aureus Detection Vancomycin screening media

ANTIMICROBIAL SUSCEPTIBILITY Macrolide Resistance Clindamycin sensitivity often requested by physician to treat Staph skin infection. Referred to as “D” test Clindamycin resistance is often inducible meaning it only is detectable when bacteria are also exposed to erythromycin

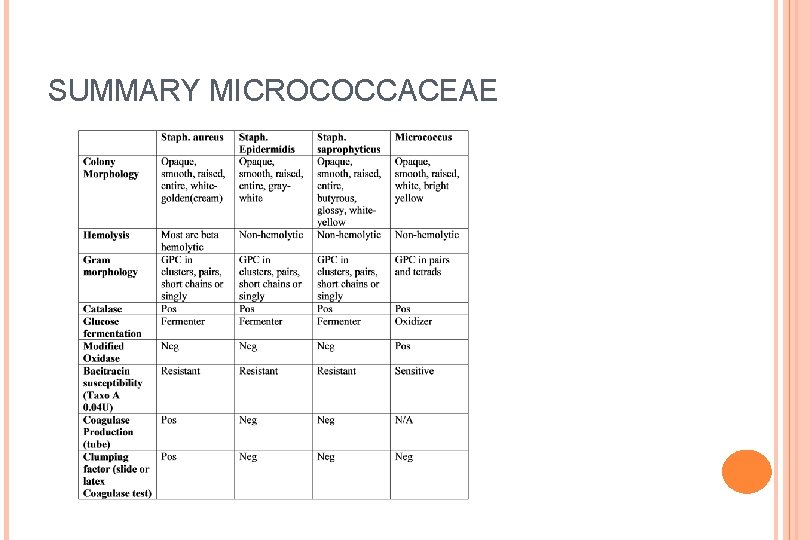
SUMMARY MICROCOCCACEAE

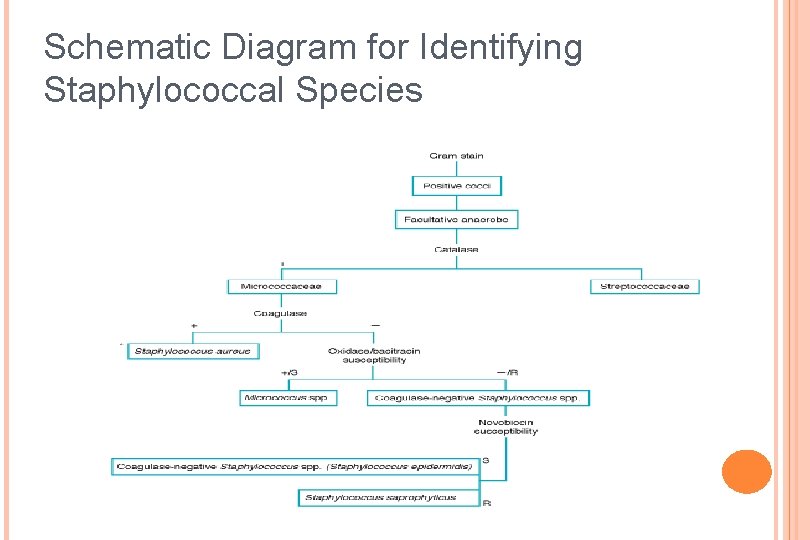
Schematic Diagram for Identifying Staphylococcal Species