Goldmann Applanation Tonometry Ted Barnett E M B

Goldmann Applanation Tonometry Ted Barnett E. M. B. Sept. 2000

Introduction • Applanation tonometry: measures IOP by providing force which flattens the cornea. • Variable force applanation tonometers (Goldmann, Perkins, Draeger, Mac. Kay. Marg, and Tono-Pen and Pneumatonometer): area of the cornea being applanated held constant, variable for applied. E. M. B. Sept. 2000

Principles • based on Imbert-Fick law: pressure within a sphere (P) is roughly equal to the external force (f) needed to flatten a portion of the sphere divided by the area (A) of trhe sphere which is flattened: P = f / A • applies to surfaces which are perfectly spherical, dry, flexible, elastic and infinitely thin E. M. B. Sept. 2000

Principles (cont. ) • include force of cornea which pushes applanating surface away from eye (N), subtract surface tension of tear film toward the eye (M) • since cornea has thickness, consider only flattening of inner corneal area (A 1) • P = f / A 1 + M - N • when A 1 = 7. 35, M and N cancel out so: • P = f / 7. 35 mm 2 E. M. B. Sept. 2000

Principles (cont. ) • this internal area achieved when diameter of external area of corneal applanation is 3. 06 mm • at this external diameter, grams of force applied multiplied by 10 is directly converted to mm. Hg • measured pressure is 3% greater than IOP before applanation (not corrected) • minimal displacement (0. 5 ul) of fluid or increase in IOP with applanation, thus unaffected by ocular rigidity E. M. B. Sept. 2000

E. M. B. Sept. 2000

Technique of measurement • plastic biprism which contacts cornea creates two semicircles • edge of corneal contact is visible after placing fluorescein into tear film & viewing with cobalt blue light • manually rotate the dial calibrated in grams, force is adjusted by changing the length of a spring within the device. • inner margins of semicircles touch when 3. 06 mm of cornea is applanated. E. M. B. Sept. 2000
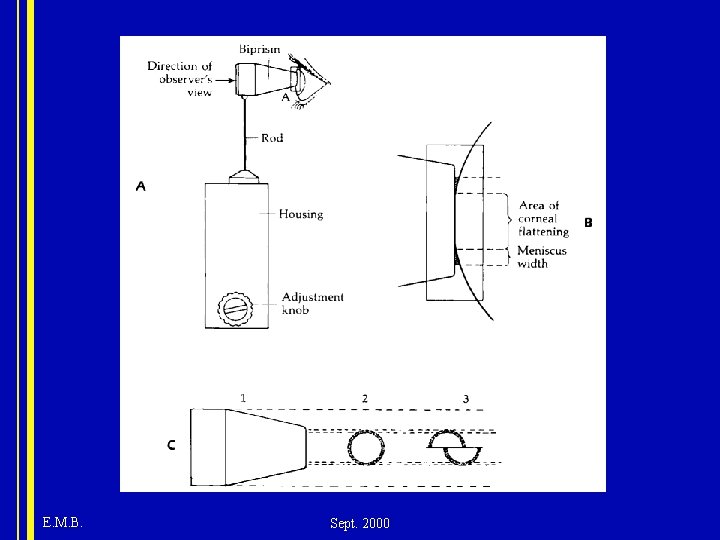
E. M. B. Sept. 2000

Instructions to patient • press head firmly against chin and forehead rest. • look straight ahead and fixate on a target (e. g. examiners opposite ear) • breathe normally, do not hold your breath • blink immediately prior to measurement to moisten cornea. E. M. B. Sept. 2000

Measurement (cont. ) • position patient’s head with forehead rest well above eyebrows, allowing raising of eyebrows. • anesthetic & fluorescein (0. 25%) , separately, or as mixture (preserved) placed in inferior cul-de-sac. • with maximal illumination of biprism the lamp is moved toward the eye until the tip of biprism contacts the apex of the cornea • stop moving forward when limbus shines with light, best observed with naked eye E. M. B. Sept. 2000

Measurement (cont. ) • After contact, semicircles visible through left (or right) ocular. Center in field of view. • Adjust vertically until semicircles equal in size. • Tension dial adjusted so that inner edge of upper and lower semicircles are aligned. • Multiply dial reading (grams of force) by 10 to obtain IOP (mm. Hg) • Read at median over which arcs glide to control for excursions due to ocular pulsations. E. M. B. Sept. 2000
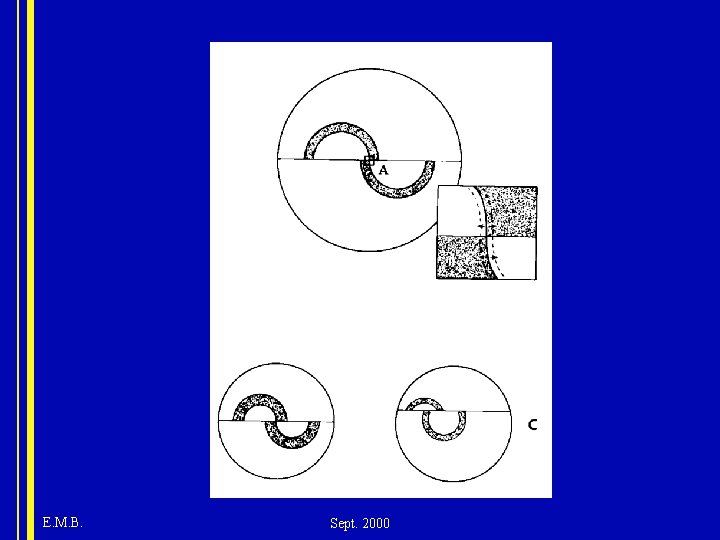
E. M. B. Sept. 2000

Measurement (cont. ) • If slit-lamp moved too far toward patient the pressure arm will push against a spring which will press against the eye with a low inoffensive force. • Mires (flattened area) too large, moving dial doen’t alter appearance. • Solution: Draw back until regular pulsation noted and appearance of mires normalizes. E. M. B. Sept. 2000

Measurement (cont. ) • Blue central area represents applanated cornea, green semicircles are fluorescein-stained tears, inner border of ring is demarcation between flattened and non-flattened cornea. • Without staining of tears, bright reflection from air -cornea interface is seen; leads to underestimation of IOP. • Mires should be approximately 10% of circle width. E. M. B. Sept. 2000

Errors in Measurement • The fluorescein ring is too wide or too narrow: • Too wide: occurs if prism not dried after cleaning or lids touch prism. Overestimates IOP. Solution: dry prism • Too narrow: inadequte fluorescein concentration may cause hypofluorescence. Underestimates IOP. Solution: patient blinks or additional fluorescein added. E. M. B. Sept. 2000

Errors (cont. ) • thin corneas produces underestimate • thick cornea d/t increased collagen gives overestimate, if d/t edema gives underestimate. • inadequate vertical alignment of semicircles leads to overstimate of IOP. • distortion d/t irregular cornea influences accuracy, less useful with corneal scarring. E. M. B. Sept. 2000

Errors (cont. ) • squeezing of eyelids, breath holding or other Valsalva maneuvers, pressure on globe, excessive EOM force applied to restricted globe, vertical gaze, tight collars, retreating patient, inaccurately calibrated tonometer. • repeated tonometry may induce decline in estimated IOP. E. M. B. Sept. 2000

Error d/t corneal curvature • increase of 1 mm. Hg for every 3 D increase in corneal power. • more fluid displaced under steep cornea, increases contribution of ocular rigidity in overestimating IOP. • the steeper the cornea, the more cornea must be indented to produce standard area of contact. • >3 D astigmatism produces elliptical rather than circular area E. M. B. Sept. 2000

Correction for astigmatism • With semicircles displaced horizontally, IOP underestimated by 1 mm. Hg for every 4 D of WTR astigmatism, vice versa for ATR astigmatism. • To minimize, prisms should be rotated so that axis of least corneal curvature is opposite red line on prism holder (i. e. align negative cylinder axis). • Can average reading with vertical and horizontal alignment of prism. E. M. B. Sept. 2000

Sterilization • CDC recommendation (HIV, HSV, and adenovirus): wipe tip clean and disinfect tip only with bleach (1: 10 dilution x 5”, changed once daily). • Alternative is 3% H 2 O 2, changed at least twice daily (affects tip less than bleach or ETOH). • Alternative #2: wiping tip with 70% ETOH E. M. B. Sept. 2000

Reliability • Goldmann applanation is standard against which others measured. • Good accuracy in gas-filled eyes. • Inter- and intraobserver variability (>30% varied by 2 -3 mm. Hg), due to subjective nature of optical endpoint. • Assume error of 2 mm. Hg. E. M. B. Sept. 2000

Calibration: Wessels & Oh (1990) • Tested tonometers in ophthalmologists offices. • 19% outside range of manufacturers specifications (1 mm. Hg of calibration), 4. 5% > 2 mm. Hg error. • Annual recalibration in 86% of instruments. • Practitioners who themselves performed calibration had the most accurate instruments. • Less than 15% knew how to perform calibration check. • Calibration here done 4 times/year E. M. B. Sept. 2000
- Slides: 22