GOING ON A BEAR HUNT WE RE GOING

GOING ON A BEAR HUNT WE’ RE GOING T O CA TC H A BI G ONE WHA T A BE AU TI FUL D AY! WE ’R E NO T SC AR ED We can’t go over it We can’t go under it We have to go through it Dr Lyndy Matthews 2019 PCL Psychiatrist HPHO Education Day March 23 rd

THE TWO HOURS AHEAD • Welcome • Presentation with breakout tasks • 1. 55 - 2 pm Mini break • Cases and discussion • Self care • 3 pm Close

THINGS WE’LL COVER • Context • Concepts and Models • Mind and Body • Tools & Pathways • Walking the Talk – Self Care

© 2012 Atlantis Healthcare | Commercial in Confidence 4


• 50% of NZ-ers with a diagnosable and treatable mental disorder do not present at all • 30% of primary care presentations have a primary psychological or addiction issue • 95% of those will present with a physical complaint • 30 -70% of those with a diagnosable MH & A condition will go undetected initially…. 14% at 3 years. • 75% of Maori don’t receive any form of treatment, similar for Pacific • Only 13% of MH care in primary settings is “minimally adequate” • Those with mental disorder have 2 -3 x risk of premature death • Two-thirds of this premature mortality is due to cardiovascular disease, cancer, and other physical illnesses

J Baker Pegasus 2014

TASK In groups of 6 or 7 • Discuss the commonest reason you might not ask a person about their about mental health/mood/wellbeing • Share the strategy you use most often to raise the subject

GPs TELL ME • Business Model: Time = money. On average you see 3050 patients a day for 7 to 15 minutes each • Undifferentiated patient: GPs need to know something about all conditions. They pick when something is ‘wrong’ but have a very short time within the consultation to action. Knowing when, where and how to engage resources beyond the consulting room is crucial • Worldview- normalising and humanistic perspective, lifestage and lifetime approach. Care is most commonly delivered in the context of an ongoing and enduring relationship between GP and patient/family. • Common things occur commonly,
GP MANAGEMENT OF MENTAL DISORDER • GPs were comfortable managing common but not serious mental disorders. • GPs based their treatment of mental disorders on pharmacotherapy, support therapy and psycho-education. • GP’s rely on clinical intuition with few clinical tools • Practice features: Salary or hourly fees payment; psycho-social teams on-site; strong informal networks enhance the delivery of mental health care • GPs characteristics: CPD, exposure and interest in mental health; BMC Fam Pract. 2012; 13: 19. traits like empathy favoured mental disorder management. International Open access Peer reviewed Publication for Primary Care

GP MANAGEMENT OF MENTAL DISORDER • Collaboration with psychologists and psychiatrists was considered key to good management. Limited access to specialists, system fragmentation, and underdeveloped group practice and shared-care models were impediments. • Mental disorder management was seen as burdensome because it required more time, flexibility, and emotional investment. • Strategies exist to reduce the burden - one-problem-per-visit rule; longer time slots. • GPs found managing mental health patients rewarding: patients were seen as grateful and more compliant with recommendations, generally leading to positive outcomes.

CURRENT PRIMARY MENTAL HEALTH PATHWAYS • GPs, Practice Nurses, Practice staff • Local community including Marae and NGOs? • Primary Mental Health Packages of Care counselling 4 sessions per patient • PHO psychiatrist (0. 7 FTE) – long arm advice, decision support, advocacy • Coming soon – 9/12 trial of e-coaching – phone and online using the JK Journal. Lifestyle and problemsolving coaching.
MODELS AND CONCEPTS THE LIFE COURSE APPROACH child infan t adult
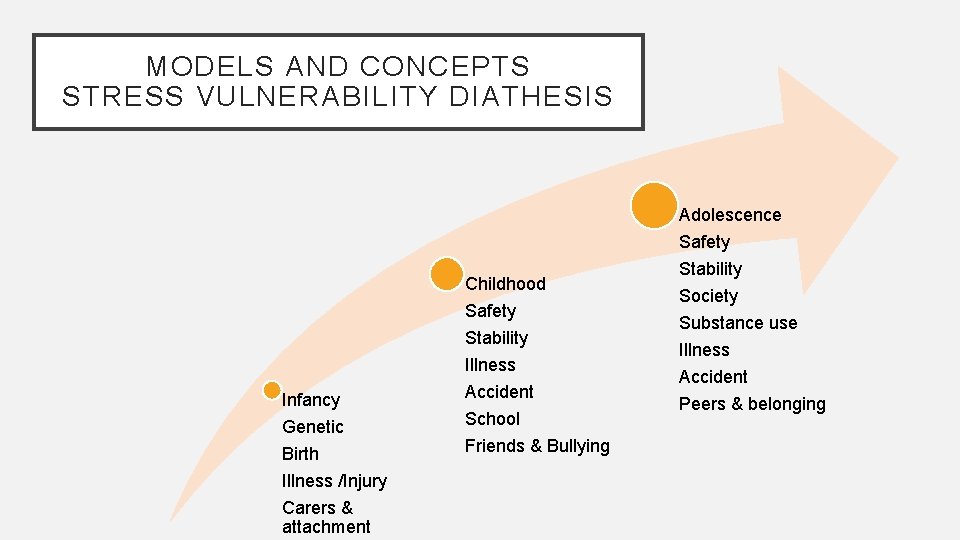
MODELS AND CONCEPTS STRESS VULNERABILITY DIATHESIS Adolescence Childhood Infancy Genetic Birth Illness /Injury Carers & attachment Safety Stability Illness Accident School Friends & Bullying Safety Stability Society Substance use Illness Accident Peers & belonging

PATIENT TRAJECTORY Eriksons Stages of Psychological Development Baby Trust v Mistrust (Hope) Toddler Autonomy v Shame (Will) Preschooler Initiative v Guilt (Purpose) 5 -12 Industry v Inferiority (Competence) Adolescence (Fidelity) Identity v Role Confusion 18 -35 Intimacy v Isolation (Love) 35 -65 (Care) Generativity v Stagnation Stages build one on another, but every stage may be reworked to a degree at later stages. Failure at any stage is likely to rear its head later and can render the person more vulnerable, less resilient
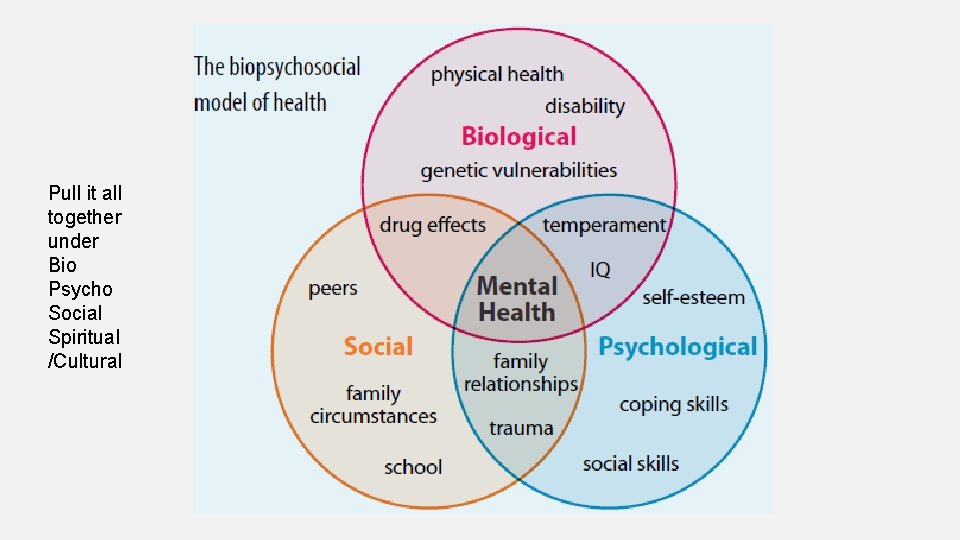
Pull it all together under Bio Psycho Social Spiritual /Cultural

MIND & BODY. WHAT COMES FIRST?
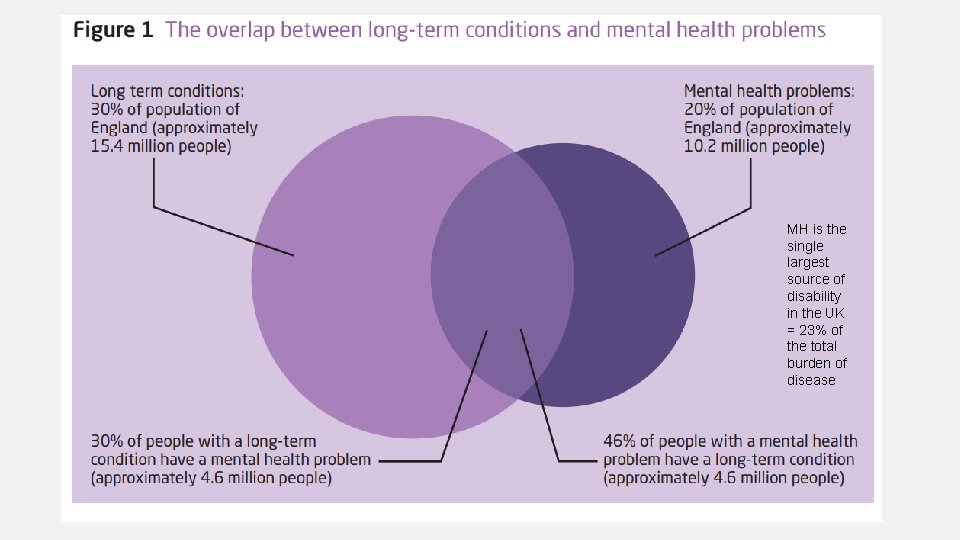
MH is the single largest source of disability in the UK = 23% of the total burden of disease

MENTAL HEALTH CONDITIONS IN PHYSICAL HEALTH • ~ 30% of people with a long term condition (LTC) have a co-morbid mental health problem leading to more severe illness and earlier death • Disproportionately affects people facing inequity (living in areas of deprivation, reduced access to resources of all forms) – cultural inequity

PHYSICAL HEALTH WITH MENTAL CONDITIONS People with mental illness: • Are more likely to smoke, use alcohol, engage in risky behaviours • Are less able to self regulate, motivate and socially integrate • Have a life expectancy reduced by up to 25 years • Are less able to engage in self management/self care • May turn to maladaptive coping strategies • Are more likely to miss appointments • Are more likely to be re-hospitalised
THE LINKS Adversity and disadvantage (life course) • Epigenetics – environment switches genes on or off • Someone to love and be loved by, food/nutrition, a safe place to sleep & ‘be’ • Chronic stress & depression – inflammatory response • Psycho-immunology mediates immune response • Some medication side effects include weight gain – metabolic syndrome • Increased rates of smoking, alcohol & other substance use • Diabetes + depression - worse symptoms of diabetes, poorer self management, dementia • Heart attack and depression – higher chances , lower survival rates • Cancer and depression – lowered survival times
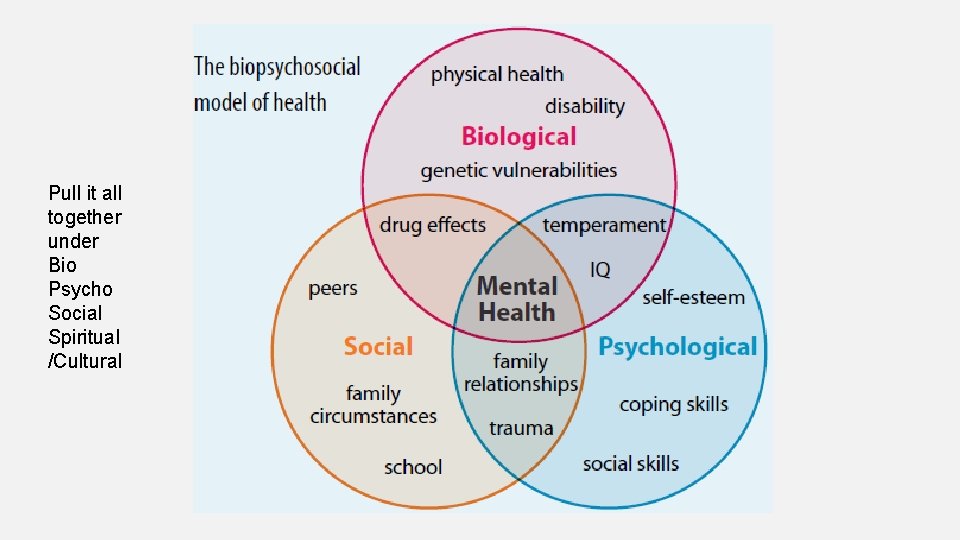
Pull it all together under Bio Psycho Social Spiritual /Cultural
IMPACT Anticipate the impact of a MH condition on treatment adherence: Impaired concentration, self motivation, organisation, cognition • Taking tablets, coming to appointments, • Impaired self care including nutrition & activity Impact of a Physical condition on mental health • Pain, injury or infirmity leading to loss of mobility and activity (esp where exercise is often a coping strategy) and loss of role • Existential threat (early death and incapacity)

AT RISK AT A GLANCE NO EASY FIX • Age • Medication: • Opioid Quetiapine Benzodiazepine Antidepressant Bronchodilators (CVS) • • BMI Ethnicity Living situation School/Employment/Role
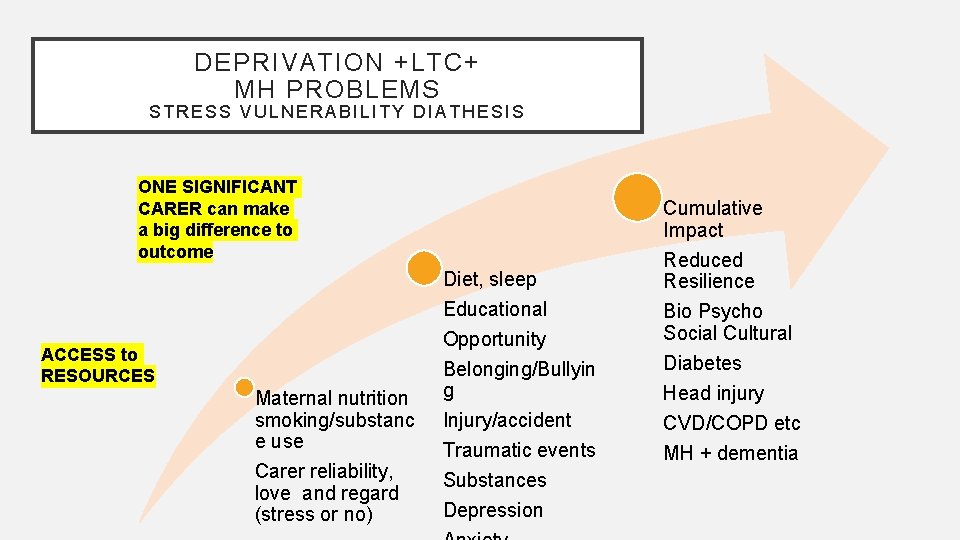
DEPRIVATION +LTC+ MH PROBLEMS STRESS VULNERABILITY DIATHESIS ONE SIGNIFICANT CARER can make a big difference to outcome ACCESS to RESOURCES Maternal nutrition smoking/substanc e use Carer reliability, love and regard (stress or no) Diet, sleep Educational Opportunity Belonging/Bullyin g Injury/accident Traumatic events Substances Depression Cumulative Impact Reduced Resilience Bio Psycho Social Cultural Diabetes Head injury CVD/COPD etc MH + dementia

TOOLS AND INTERVENTIONS MAINTAINING HOPE

EFFECTIVE INTERVENTIONS: DETERMINANTS OF GOOD HEALTH • Bio Able bodied, fit for purpose • Psycho Hopeful, good enough, coping skills • Social Connected, meaningful activities & relationships • Spiritual/Cultural Meaning, identity, belonging Strengths based approach

HELPFUL TOOLS IN PRACTICE Screening Questionnaires: PHQ 9 GAD 7 DASS 21 AUDIT Love ACE Work Play • Benchmark current symptom level – a reference point • Indication of severity (sometimes surprising) • Tohunga effect of measuring the ‘immeasurable’ and making the patient feel heard • ----------- Visual analogue rating scales are easy

CASE DISCUSSION • Case one • Case three

IS THE MEDICAL MODEL OF MANAGEMENT THE RIGHT ONE ? • Person identifies as being unwell, seeks medical help to get well • Consults with health practitioner (expert) • Accepts explanation for the problem • Follows treatment instructions • Recovers or improves

INTERVENTIONS THAT WORK • People like me (People at the Centre) • Closer to home (increase choices) • Increase access and support options • Prevent problems and increase social wellbeing • See the big picture!

POTENTIAL PATHWAYS For consideration: • Health coach/Wellness Advisors in practices (0. 2+ FTE) • Chronic Disease Self Management groups & online (Stanford) • Depression and Anxiety, Mindfulness group programmes • Integrate mental & physical healthcare • GPs with a special interest in MH Under discussion:

IN THE FACE OF PATIENT DISTRESS OR COMPLEXITY • Pause and think: BIO PSYCHO SOCIAL CULTURAL – see the whole person in their context • Use tools: PHQ 9 GAD 7 AUDIT • Don’t be in a rush to fix – Small steps and Basic Advice • Phone for a chat or send a BPAC referral for input or support (psychiatrist advice). There is no such thing as a ‘stupid’ request or question • Engage the patient in the problem solving & treatment planning

SELF-CARE • How do you manage the intensity of time & demand at work? • How do you manage sadness and despair? • Who do you share with? • What re-fuels you? • What gives you joy? • Do you have your own GP? • Do you take your tablets? • WORK PLAY LOVE

REFERENCES • Te Rau Hinengaro: NZ Mental Health Survey 2006 Mo. H • Ma. GPie Studies multiple on line • King’s Fund The Centre for Mental Health February 2012 Long Term Conditions & Mental Health; the cost of comorbidities • BMC Family Practice March 2012 General practitioners' management of mental disorders: A rewarding practice with considerable obstacles Recommended reading - The Body Keeps the Score by Bessel van der Kolk 2017
- Slides: 35