GLYCOGEN METABOLISMII GLYCOGEN SYNTHESIS GLYCOGEN SYNTHESIS GLYCOGENOLYSIS GLYCOGENOLYSIS

GLYCOGEN METABOLISMII
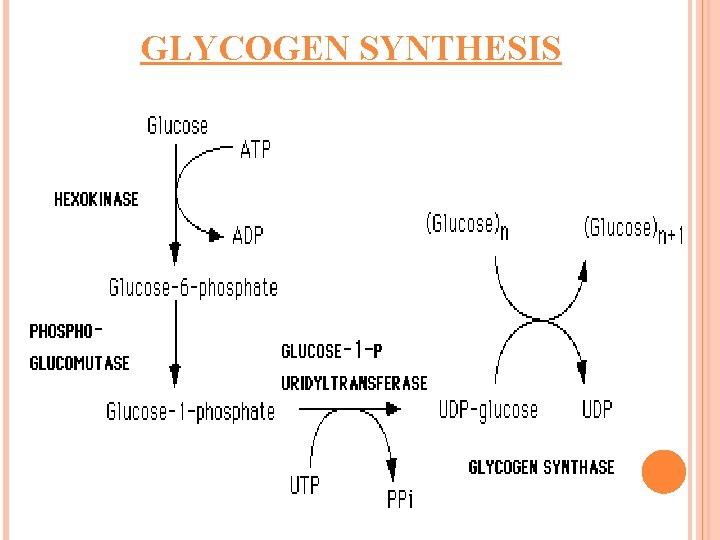
GLYCOGEN SYNTHESIS
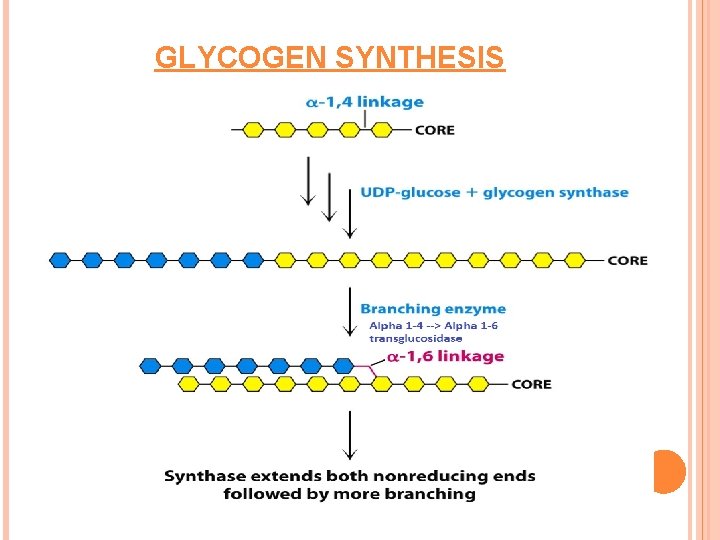
GLYCOGEN SYNTHESIS
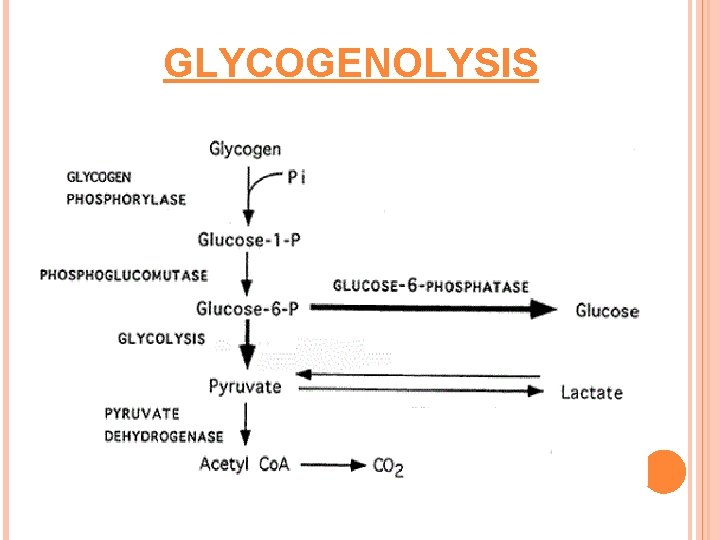
GLYCOGENOLYSIS
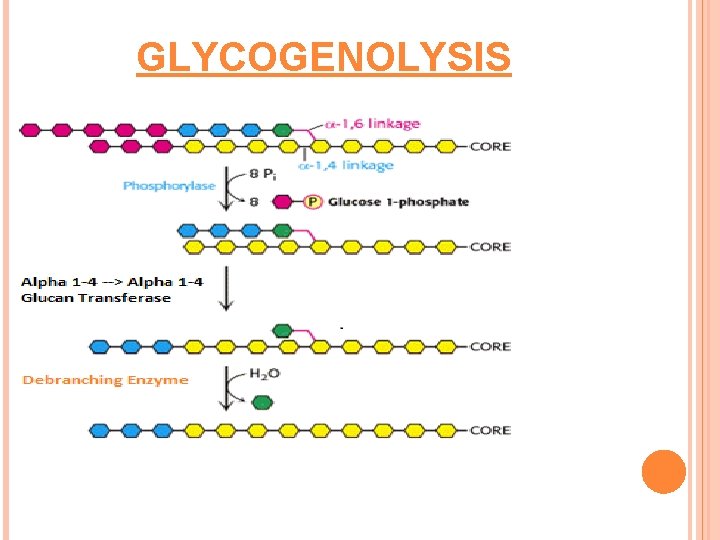
GLYCOGENOLYSIS
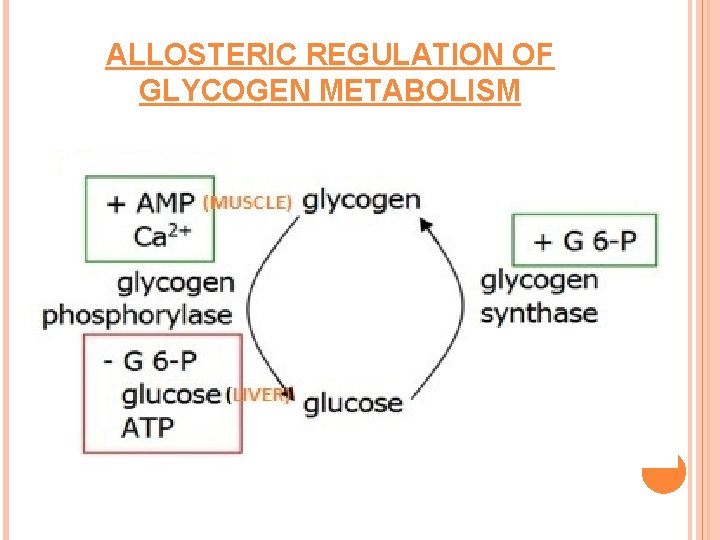
ALLOSTERIC REGULATION OF GLYCOGEN METABOLISM
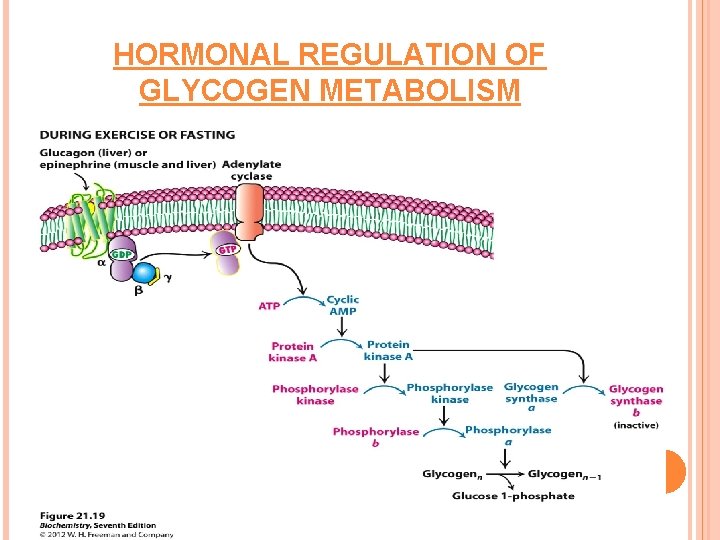
HORMONAL REGULATION OF GLYCOGEN METABOLISM
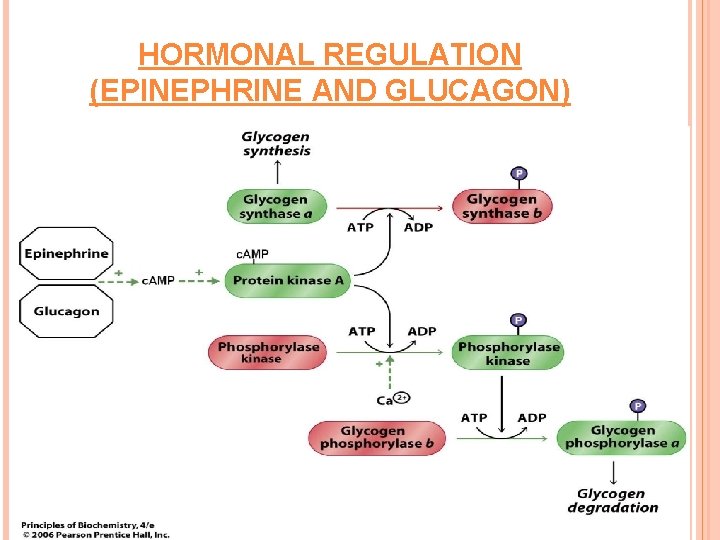
HORMONAL REGULATION (EPINEPHRINE AND GLUCAGON)
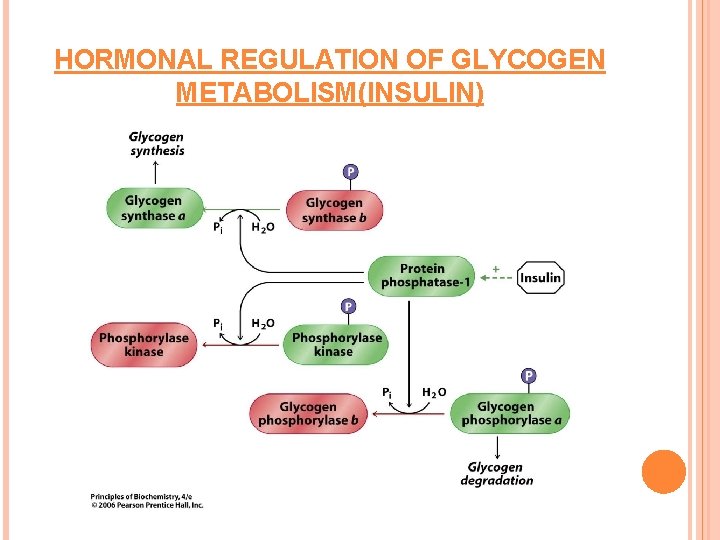
HORMONAL REGULATION OF GLYCOGEN METABOLISM(INSULIN)
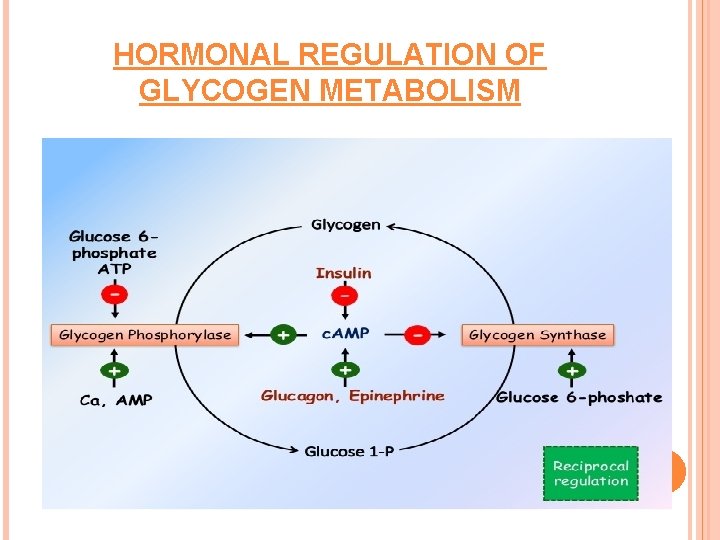
HORMONAL REGULATION OF GLYCOGEN METABOLISM

GLYCOGEN STORAGE DISEASES ARE A GROUP OF INHERITED DISORDERS Inborn metabolic errors (genetically defective enzymes) Abnormal metabolism (Glycogenesis or/and Glycogenolysis) within muscles, liver, Kidney and other cell types.

CLINICAL FINDINGS BASED ON THE ENZYME THAT IS ABSENT OR DEFICIENT Signs and Symptoms usually result because of: The buildup of Glycogen or Glycogen not being able to produce glucose. Mostly occurs in muscles and the liver so those areas show the most symptoms: Poor growth. Muscle weakness and Muscle Hypoglycemia. Hepatomegaly. Swollen belly. May result in early death. cramps.

MULTPLE DISTINCT DISEASES THAT ARE COMMONLY CONSIDERED TO BE GLYCOGEN STORAGE DISEASES Designated as GSD type 0, GSD type II, GSD type III, GSD type IV and so on. Some important examples are: GSD GSD type I von Gierke's disease. type II Pompe's disease. type III Cori's disease. type IV Andersen disease. type V Mc. Ardle disease. type VI Hers' disease.

GLYCOGEN STORAGE DISEASE(GSD TYPE I) (VON GIERKE DISEASE OR HEPATORENAL GLYCOGENOSIS) Defect: Deficiency of the enzyme Glucose-6 -Phosphatase (type Ia). Deficiency of Endoplasmic Reticulum Glucose 6 Phosphatase Transporter (type Ib) Effect: Glycogen(normal structure) accumulation in liver and renal tubule cells. Therefore, enlarged liver and kidneys dominate the clinical presentation of the disease.

LARGE QUANTITIES OF METABOLIC ALTERATIONS IN GSD TYPE I STRUCTURALLY NORMAL GLYCOGEN Decreased blood glucose level (hypoglycemia) Increased free fatty acids in blood Increased lactate in blood Increased uric acid in blood

METABOLIC ALTERATION IN GSD TYPE I: HYPOGLYCEMIA FASTING HYPOGLYCEMIA Insufficient Glucose 6 Phosphatase activity, G 6 P cannot be converted into free glucose. In hypoglycemia, the deficiency of Glucose 6 Phosphatase blocks the process of glycogen degradation and gluconeogenesis in the liver, preventing the production of free glucose molecules. As a consequence, patients with GSD type I have fasting hypoglycemia.

METABOLIC ALTERATION IN GSD TYPE I: HYPOGLYCEMIA Hypoglycemia inhibits the secretion of insulin. Reduced insulin inhibits protein synthesis and this causes reduced growth (dwarfism) in infants. Hypoglycemia stimulates the secretion of catecholamines. These result in the breakdown of muscle glycogen producing lactic acid and hence lactic acidosis. o

METABOLIC ALTERATION IN GSD TYPE I: LACTIC ACIDEMIA Glucose 6 Phosphate is metabolized to lactic acid.

METABOLIC ALTERATION IN GSD TYPE I HYPERLIPEMIA AND KETOSIS Hypoglycemia inhibits insulin secretion and stimulates glucagon and cortisol release. Increased fat is used as a source of energy. Increased fat mobilization results in hyperlipemia and increased free fatty acid levels. Ketosis results due to increased Lipolysis. Triglycerides increase the risk of fatty liver infiltration, which contributes to the enormous amount of liver enlargement. Xanthomas

METABOLIC ALTERATION IN GSD TYPE I HYPERURICEMIA Blood uric acid levels are raised because of: Increased endogenous production. (As glucose-6 -phosphate is diverted towards HMP shunt Ribose 5 Phosphate and eventually uric acid. Reduced urinary elimination caused by competition with the elevated concentrations of lactate, which should be excreted. Test: Give IV GLUCAGON INJECTION

CLINICAL PRESENTATION OF GSD TYPE I Poor growth. Hypoglycemia. Hepatomegaly. May result in early death. Altered neutrophil functions predisposing to bacterial infections (type Ib).

GSD TYPE II, ACID MALTASE DEFICIENCY POMPE'S DISEASE Defect: Deficiency of a lysosomal enzyme, alpha-1, 4 glucosidase and alpha – 1, 6 glucosidase (Acid Maltase) Effect: Accumulation of normally structured glycogen in lysosomes of most tissues (heart, liver and muscles).

CLINICAL PRESENTATION OF GSD TYPE II Its clinical presentation is more generalized. Two forms of the disease exist: 1. Infantile 2. Adult. In the classic infantile form main clinical signs are: Cardiomegaly and Muscular hypotonia. Death from heart failure by age 2 In the juvenile and adult forms: Involvement of skeletal muscles (muscle dystrophy) dominates.

GSD TYPE III (LIMIT DEXTRINOSIS) FORBE'S OR CORI'S DISEASE Defect: Deficiency of debranching enzyme. Effect: Accumulation of characteristic branched (abnormal) polysaccharide (limit dextrin). (Dextrin is linear glycogen and Limit Dextrin is one with branching) Clinical Presentation: Mild Fasting hypoglycemia Hepatomegaly Muscle weakness

GSD IV (AMYLOPECTINOSIS) ANDERSON'S DISEASE Defect: Deficiency of Branching enzyme. Effect: Accumulation of polysaccharide with few branch points (abnormal). Clinical Presentation: Hepatosplenomegaly Cirrhosis Death from heart or liver failure at early age.

GSD V (MCARDLE’S SYNDROME) Defect: Deficiency of Muscle Phosphorylase Effect: Accumulation of normal glycogen in muscles only. Ø Clinical Fetaures: Muscle breakdown (Rhabdomyolysis eventually resulting in myoglobinuria in severe cases). Increase Creatine Kinase Muscle variant Muscle cramps Poor exercise tolerance Blood lactate very low after exercise.

GSD VI (HER’S SYNDROME) Defect: Deficiency of Liver Phosphorylase Effect: Accumulation of normal glycogen in liver Clinical Presentation: Mild Fasting hypoglycemia (gluconeogenis) Hepatomegaly Mild Hyperlipidemia and hyperketosis if present

TREATMENT OF GLYCOGEN STORAGE DISEASE Treatment depends on the type of GSD. For the types of GSD that can be treated, patients must carefully follow a special diet. Frequent high carbohydrate meals during the day help prevent blood sugar levels from dropping. Corn starch every four to six hours – including during overnight hours – also can help keep blood sugar levels from getting low.

Continuous night time feeding in order to maintain the blood glucose level. Special feeding tube can be placed into the child’s stomach. Treatment for uric acid build up in the body. In some types of this disease, children must limit their amount of exercise to reduce muscle cramps.

Patients with treatable GSD do very well if the blood glucose level is maintained. In the more severe cases of GSD, infection and other complications are likely to occur. These include liver, heart and respiratory failure. If liver failure occurs, receiving a liver transplant is the only option. Transplants have been effective in reversing the symptoms of GSD.
- Slides: 30