Glutamine Objectives Discuss glutamine Discuss its role in
Glutamine

Objectives • Discuss glutamine • Discuss its role in metabolism and body composition • Discuss clinical uses of glutamine
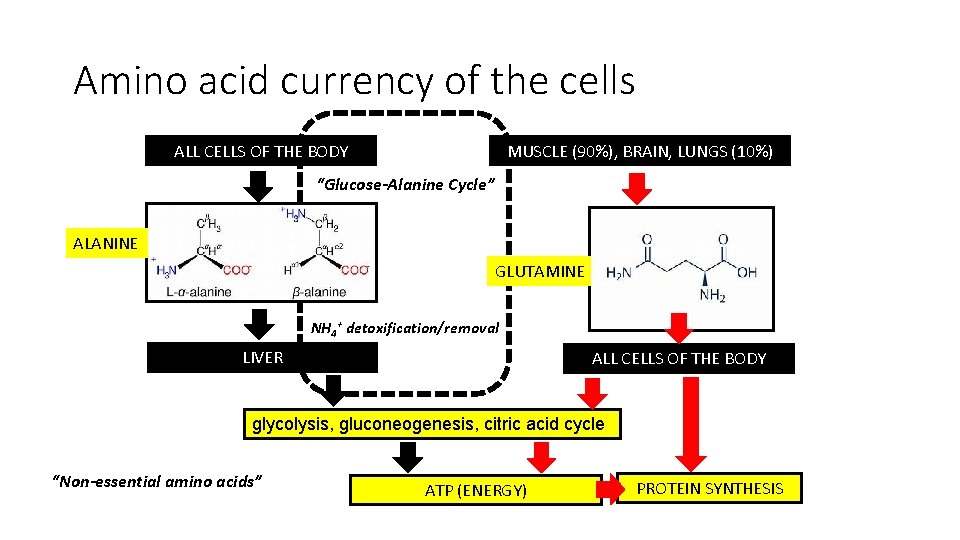
Amino acid currency of the cells ALL CELLS OF THE BODY MUSCLE (90%), BRAIN, LUNGS (10%) “Glucose-Alanine Cycle” ALANINE GLUTAMINE NH 4+ detoxification/removal LIVER ALL CELLS OF THE BODY glycolysis, gluconeogenesis, citric acid cycle “Non-essential amino acids” ATP (ENERGY) PROTEIN SYNTHESIS

Diet *Foods with High Glutamine Content: 1. Meat and poultry 2. Fish 3. Dairy products 4. Mushrooms (shitake) 5. Legumes (pea, beans, lentils) 6. Nuts and seeds 7. Vegetables *http: //www. diyhealthremedy. com/7 essential-food-sources-of-glutamine/ De Berardinis RK and Cheng T. Q's next: The diverse functions of glutamine in metabolism, cell biology and cancer. Oncogene. 2010 January 21; 29(3): 313– 324.

What is glutamine? • Non-essential amino acid • Synthesized by the body (muscle: 90%; brain and lungs: 10%) | can also be provided from the diet • Primary amino acid exchange between all metabolic processes • Provides carbon based source of energy (Kreb’s Cycle) • Provides amino acid backbone for protein synthesis De Berardinis RK and Cheng T. Q's next: The diverse functions of glutamine in metabolism, cell biology and cancer. Oncogene. 2010 January 21; 29(3): 313– 324.
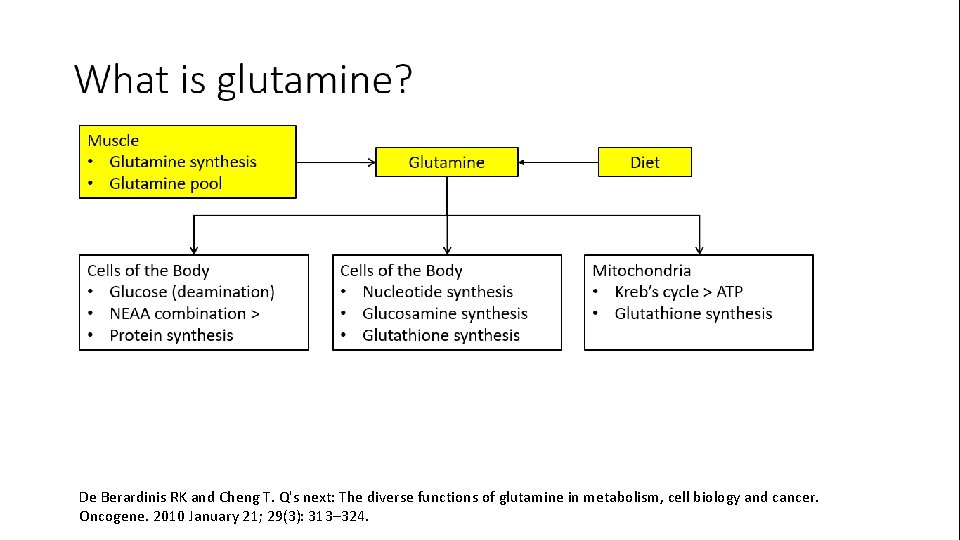
De Berardinis RK and Cheng T. Q's next: The diverse functions of glutamine in metabolism, cell biology and cancer. Oncogene. 2010 January 21; 29(3): 313– 324.

What is glutamine? • Non-essential amino acid • Synthesized by the body (muscle: 90%; brain and lungs: 10%) • Primary amino acid exchange between all metabolic processes • Provides carbon based source of energy (Kreb’s Cycle) • Provides amino acid backbone for protein synthesis • Primarily utilized by rapidly dividing cells: immune cell precursors, immune cells, WBC, mucosal cells, fibroblasts • Demand usually outstrips supply in high inflammation states, wound healing processes > thus it is considered a conditional essential amino acid in these conditions De Berardinis RK and Cheng T. Q's next: The diverse functions of glutamine in metabolism, cell biology and cancer. Oncogene. 2010 January 21; 29(3): 313– 324.
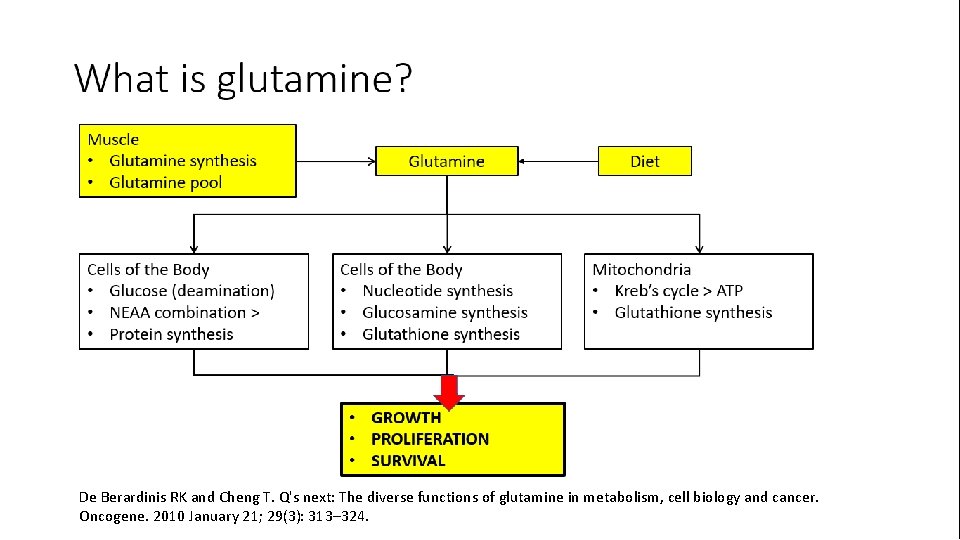
De Berardinis RK and Cheng T. Q's next: The diverse functions of glutamine in metabolism, cell biology and cancer. Oncogene. 2010 January 21; 29(3): 313– 324.

Glutamine in inflammation
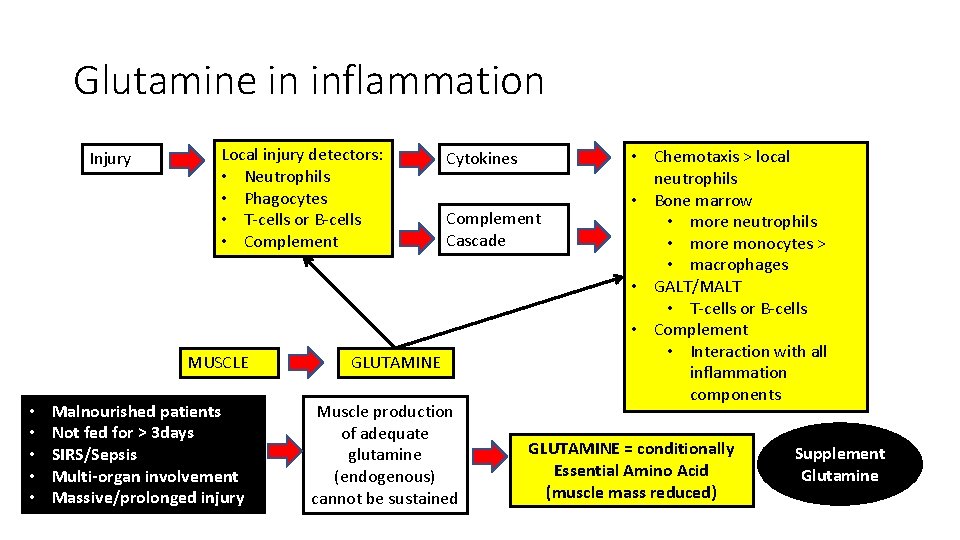
Glutamine in inflammation Injury Local injury detectors: • Neutrophils • Phagocytes • T-cells or B-cells • Complement MUSCLE • • • Malnourished patients Not fed for > 3 days SIRS/Sepsis Multi-organ involvement Massive/prolonged injury Cytokines Complement Cascade GLUTAMINE Muscle production of adequate glutamine (endogenous) cannot be sustained • Chemotaxis > local neutrophils • Bone marrow • more neutrophils • more monocytes > • macrophages • GALT/MALT • T-cells or B-cells • Complement • Interaction with all inflammation components GLUTAMINE = conditionally Essential Amino Acid (muscle mass reduced) Supplement Glutamine
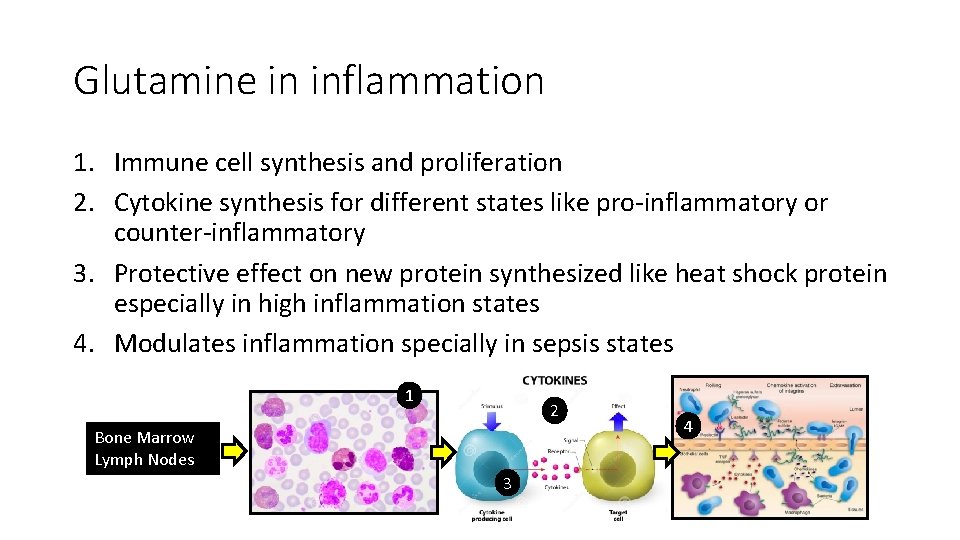
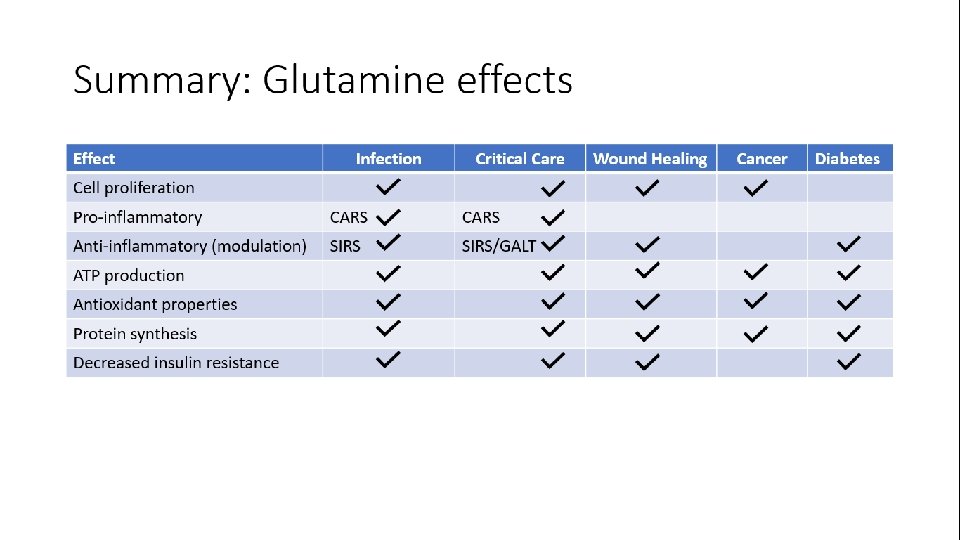
Glutamine in inflammation 1. Immune cell synthesis and proliferation 2. Cytokine synthesis for different states like pro-inflammatory or counter-inflammatory 3. Protective effect on new protein synthesized like heat shock protein especially in high inflammation states 4. Modulates inflammation specially in sepsis states 1 2 Bone Marrow Lymph Nodes 3 4
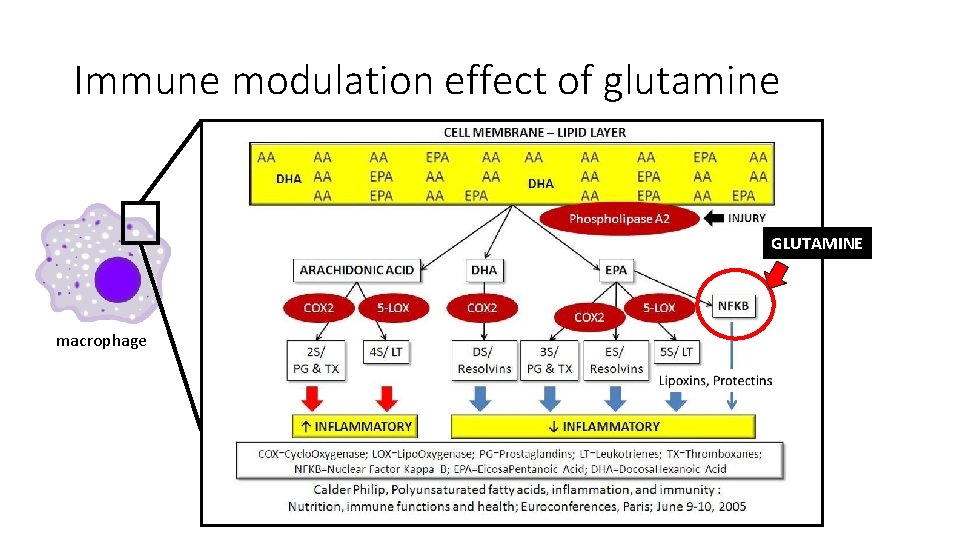
Immune modulation effect of glutamine GLUTAMINE macrophage
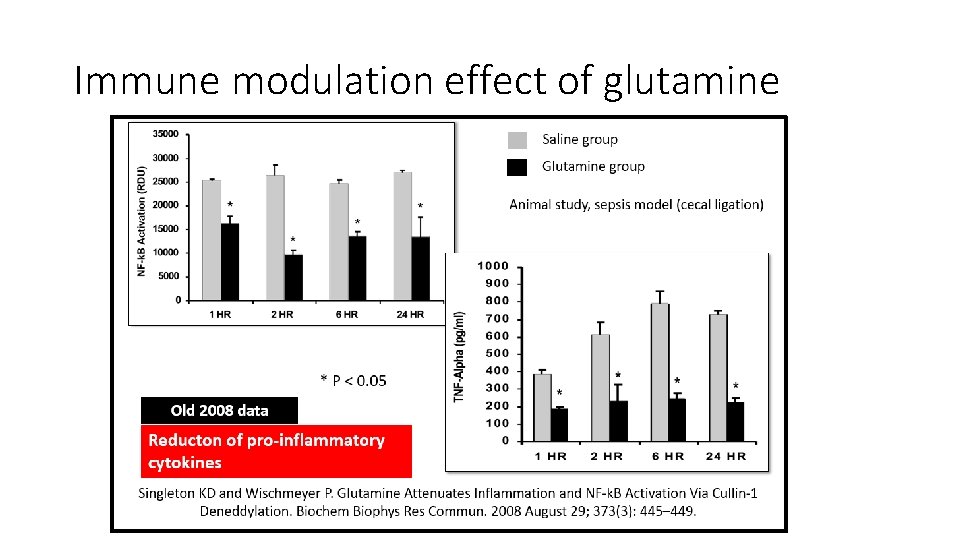
Immune modulation effect of glutamine
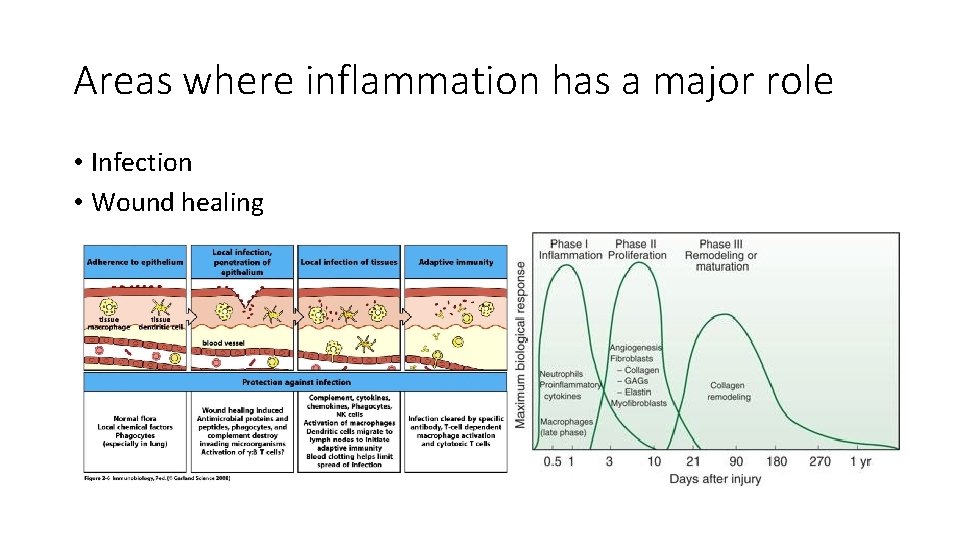
Areas where inflammation has a major role • Infection • Wound healing

Glutamine in infection and critical care state

Glutamine in infection 1. Improves mucosal status of both gut and lungs by enhanced mucosal regeneration and maintenance of an effective mucosal barrier 2. Improves immune function especially WBC capabilities and antibody synthesis in the gastrointestinal and pulmonary systems – effect on the GALT and MALT
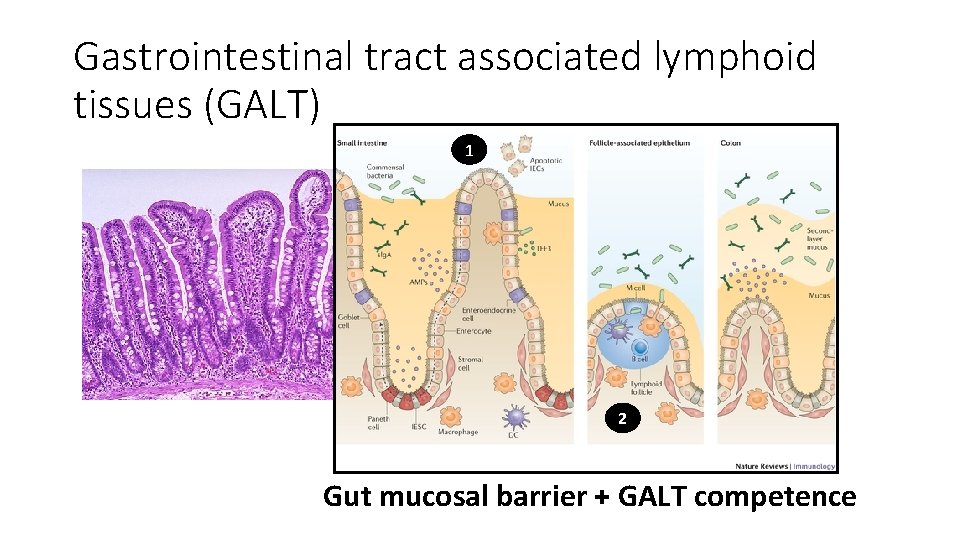
Gastrointestinal tract associated lymphoid tissues (GALT) 1 2 Gut mucosal barrier + GALT competence
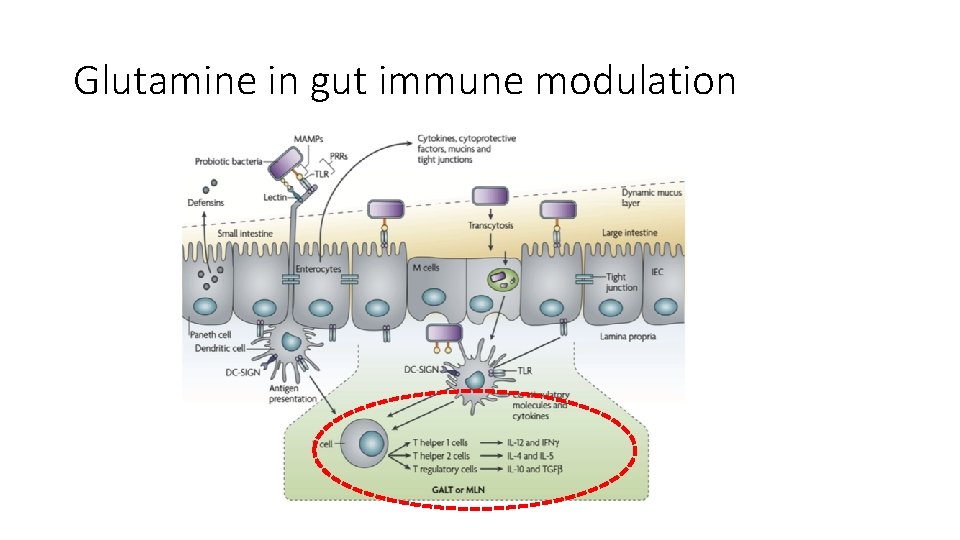
Glutamine in gut immune modulation
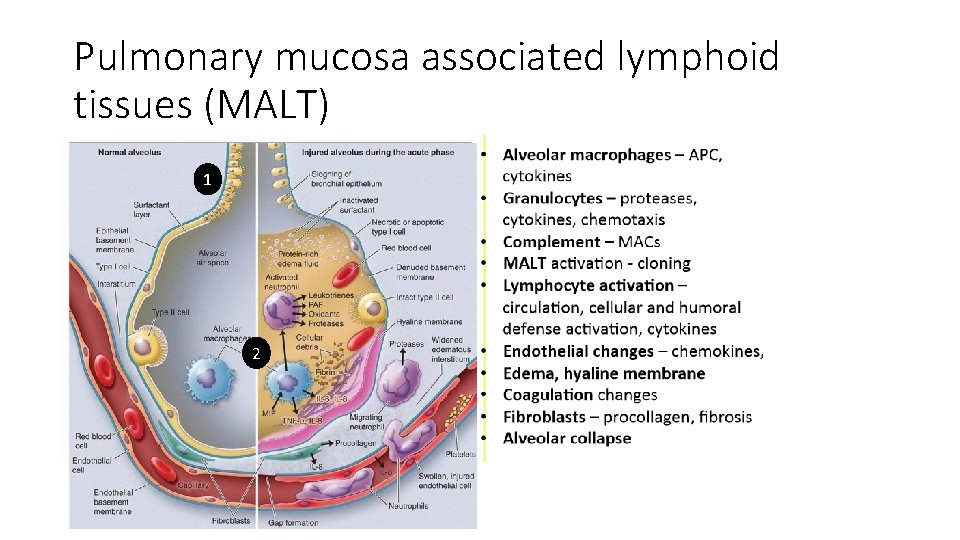
Pulmonary mucosa associated lymphoid tissues (MALT) 1 2
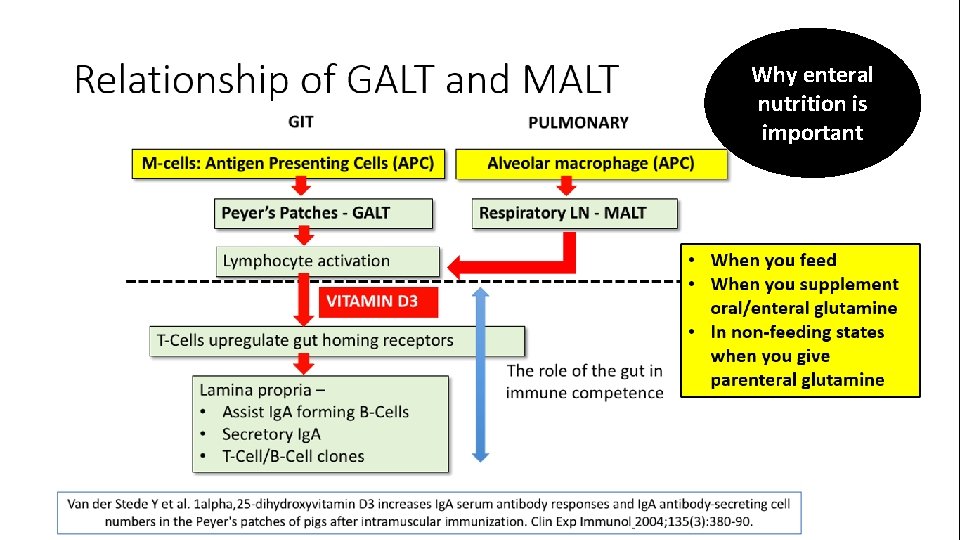
Why enteral nutrition is important
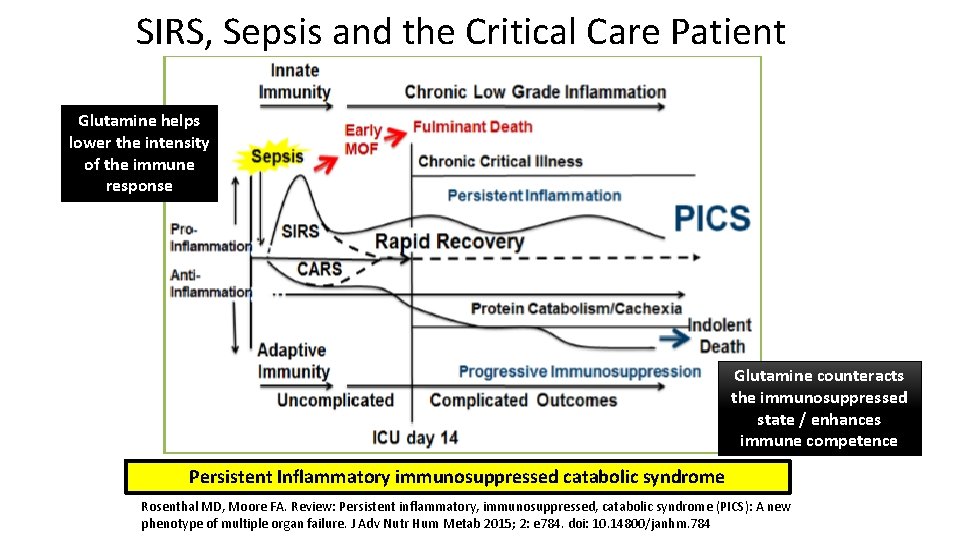
SIRS, Sepsis and the Critical Care Patient Glutamine helps lower the intensity of the immune response Glutamine counteracts the immunosuppressed state / enhances immune competence Persistent Inflammatory immunosuppressed catabolic syndrome Rosenthal MD, Moore FA. Review: Persistent inflammatory, immunosuppressed, catabolic syndrome (PICS): A new phenotype of multiple organ failure. J Adv Nutr Hum Metab 2015; 2: e 784. doi: 10. 14800/janhm. 784

Clinical uses of glutamine in infection • Hastens recovery in respiratory infections 1 • Reduces duration of mechanical ventilation • Shortens ICU stay • Reduces mortality • Sustains mucosal function in gut during periods of non-intake 2 • Reduces incidence of bacterial translocation • Maintains GALT competence • Modulates inflammatory response in SIRS or Sepsis 3 1. 2. 3. Stehle P et al. Clin Nutr ESPEN. 2017 Feb; 17: 75 -85. Santos RG et al. Br J Nutr. 2014 Jan 14; 111(1): 93 -100 Cetinbas F et al. . J Crit Care. 2010 Dec; 25(4): 661. e 1 -6.
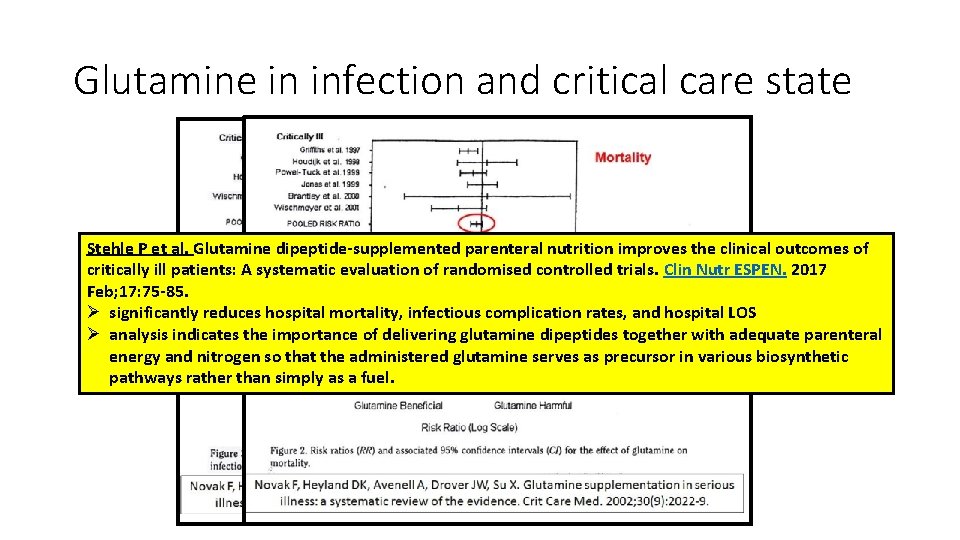

Glutamine in infection and critical care state Stehle P et al. Glutamine dipeptide-supplemented parenteral nutrition improves the clinical outcomes of critically ill patients: A systematic evaluation of randomised controlled trials. Clin Nutr ESPEN. 2017 Feb; 17: 75 -85. Ø significantly reduces hospital mortality, infectious complication rates, and hospital LOS Ø analysis indicates the importance of delivering glutamine dipeptides together with adequate parenteral energy and nitrogen so that the administered glutamine serves as precursor in various biosynthetic pathways rather than simply as a fuel.

Glutamine in wound healing

Glutamine in wound healing • Optimizes the wound healing environment by its role in the inflammatory response especially in removal of infectious agents • Provides the amino acids for protein synthesis e. g. ground substance, collagen by the fibroblasts • Provides optimized cell function by increasing synthesis of antioxidant products like glutathione and its derivatives • Enhances wound healing
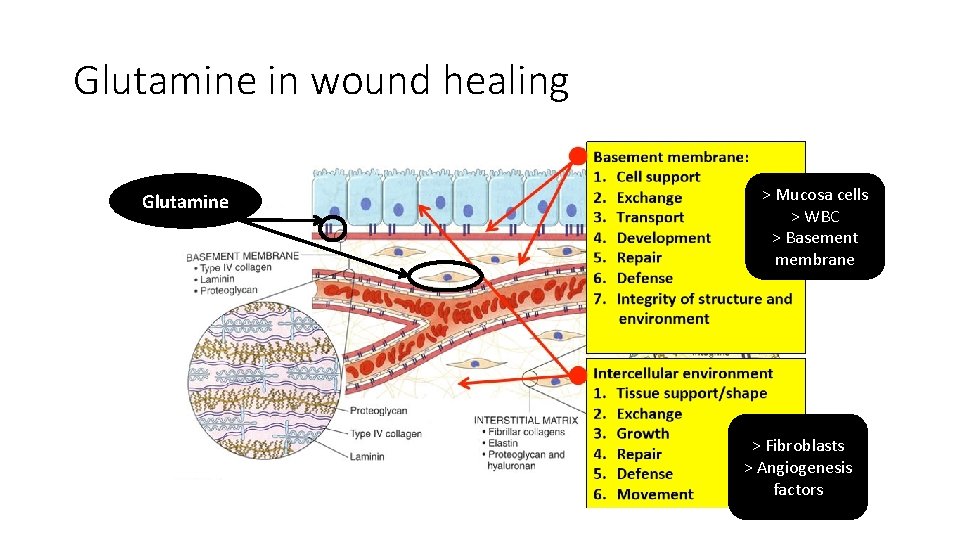
Glutamine in wound healing Glutamine > Mucosa cells > WBC > Basement membrane > Fibroblasts > Angiogenesis factors
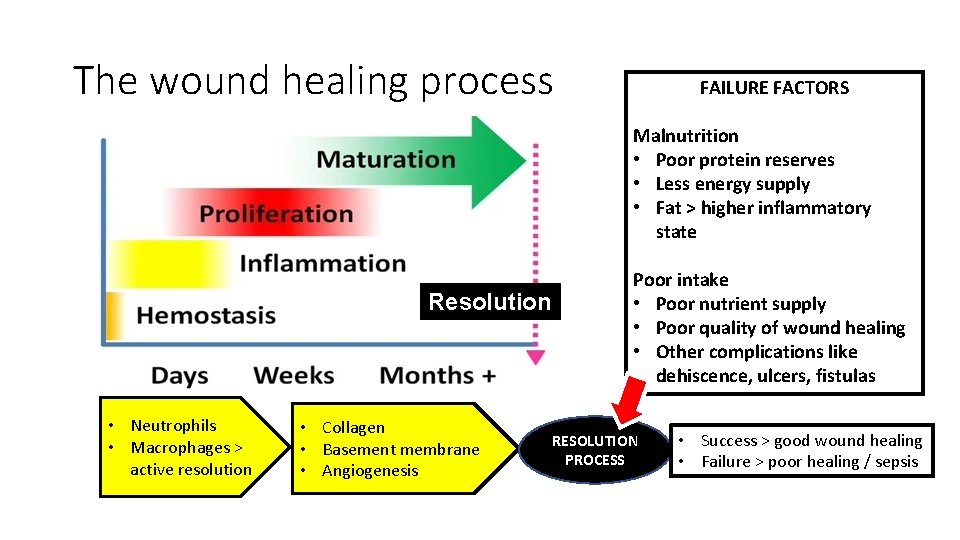
The wound healing process FAILURE FACTORS Malnutrition • Poor protein reserves • Less energy supply • Fat > higher inflammatory state Resolution • Neutrophils • Macrophages > active resolution • Collagen • Basement membrane • Angiogenesis Poor intake • Poor nutrient supply • Poor quality of wound healing • Other complications like dehiscence, ulcers, fistulas RESOLUTION PROCESS • Success > good wound healing • Failure > poor healing / sepsis
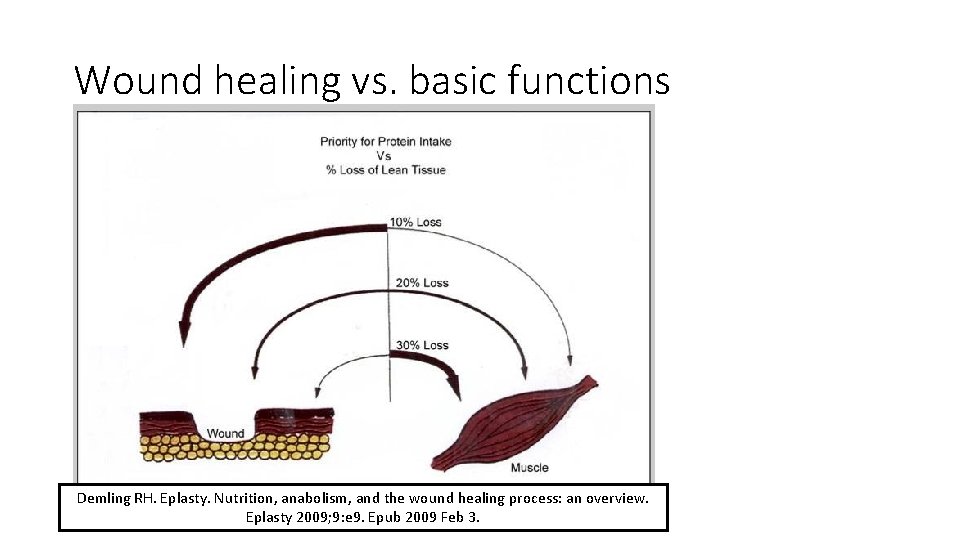
Wound healing vs. basic functions Demling RH. Eplasty. Nutrition, anabolism, and the wound healing process: an overview. Eplasty 2009; 9: e 9. Epub 2009 Feb 3.
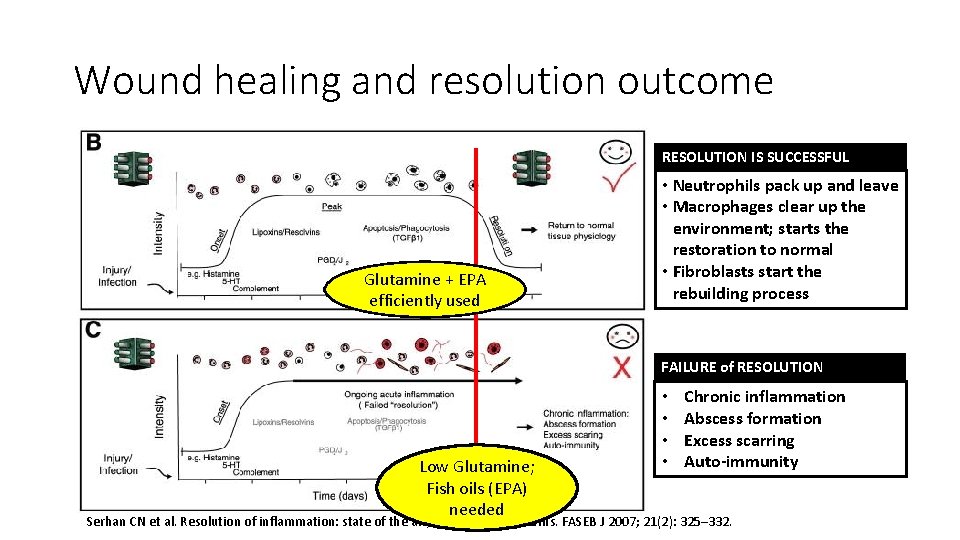
Wound healing and resolution outcome RESOLUTION IS SUCCESSFUL Glutamine + EPA efficiently used • Neutrophils pack up and leave • Macrophages clear up the environment; starts the restoration to normal • Fibroblasts start the rebuilding process FAILURE of RESOLUTION Low Glutamine; Fish oils (EPA) needed • • Chronic inflammation Abscess formation Excess scarring Auto-immunity Serhan CN et al. Resolution of inflammation: state of the art, definitions and terms. FASEB J 2007; 21(2): 325– 332.

Resolution is an active process • The pro-inflammatory mechanisms probably are counterbalanced by endogenous anti-inflammatory signals • Mainly mediated by families of local-activity mediators that are biosynthesized from essential fatty acids eicosapentaenoic acid and Omegaven docosahexaenoic acid. Fish oil tablets 100 ml iv • These mediators are termed resolvins and protectins. 2 -3 g/day • Inflammation resolution is also mediated by lipoxins, trihydroxystearin containing eicosanoids that are generated within the vascular lumen through platelet-leukocyte interactions. https: //www. ucm. es/data/cont/docs/420 -2014 -02 -07 -WOUND-HEALING-3 Nov-2013. pdf

Clinical uses of glutamine in wound healing • Improves wound healing in: • Acute wounds as in surgery, surgery site infections, burns especially when large or in malnourished patients 1 • Chronic ulcers like decubitus ulcers, chronic infection (when combined with arginine and hydroxy-methyl-butyrate (HMB) 2 • Reduces complication rates 3 • Surgical site infection 4 • Dehiscence 1. 2. 3. 4. Lorenz KJ et al. GMS Interdiscip Plast Reconstr Surg DGPW. 2015 Dec 15; 4: Doc 15 Armstrong DG et al. Diabet Med. 2014 Sep; 31(9): 1069 -77. Yue C et al. Am Surg. 2013 May; 79(5): 506 -13 Anderson DJ et al. Infect Control Hosp Epidemiol. 2007 Sep; 28(9): 1047 -53
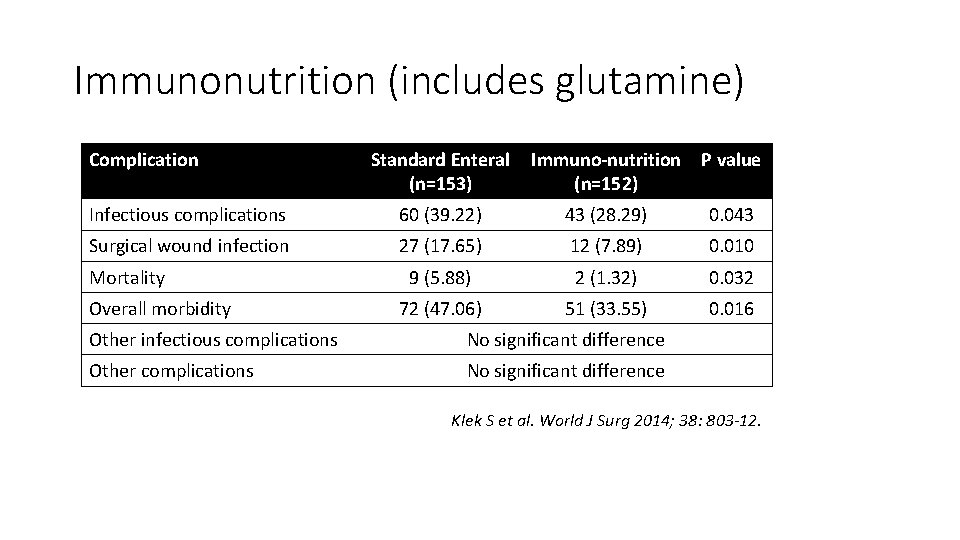
Immunonutrition (includes glutamine) Complication Standard Enteral (n=153) Immuno-nutrition (n=152) P value Infectious complications 60 (39. 22) 43 (28. 29) 0. 043 Surgical wound infection 27 (17. 65) 12 (7. 89) 0. 010 9 (5. 88) 2 (1. 32) 0. 032 72 (47. 06) 51 (33. 55) 0. 016 Mortality Overall morbidity Other infectious complications No significant difference Other complications No significant difference Klek S et al. World J Surg 2014; 38: 803 -12.

Glutamine in cancer
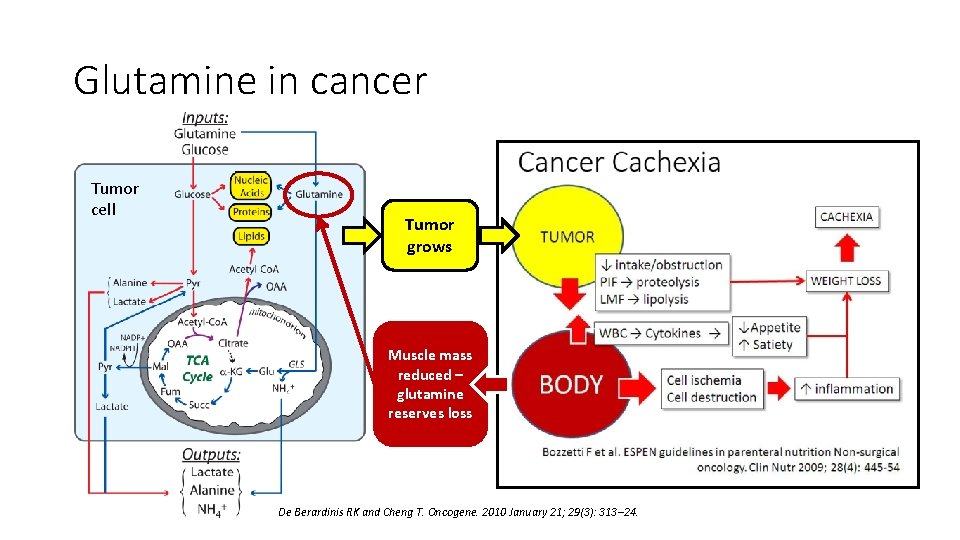
Glutamine in cancer Tumor cell Tumor grows Muscle mass reduced – glutamine reserves loss De Berardinis RK and Cheng T. Oncogene. 2010 January 21; 29(3): 313– 24.
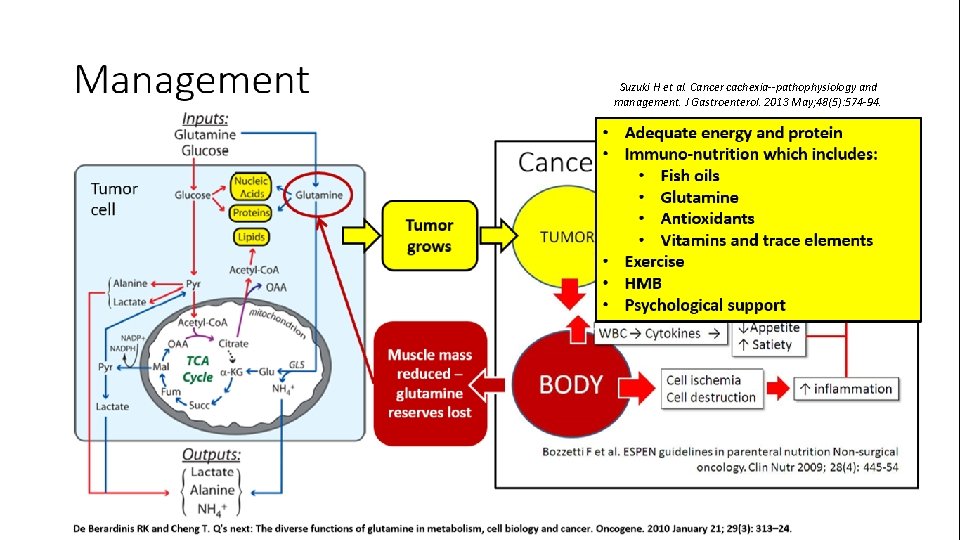
Suzuki H et al. Cancer cachexia--pathophysiology and management. J Gastroenterol. 2013 May; 48(5): 574 -94.

Glutamine in diabetes
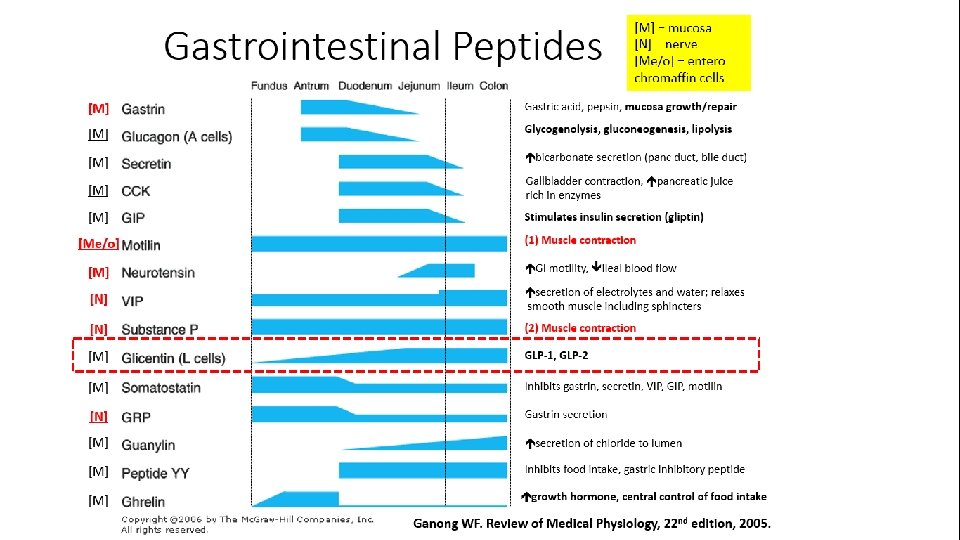
Gastrointestinal Peptides
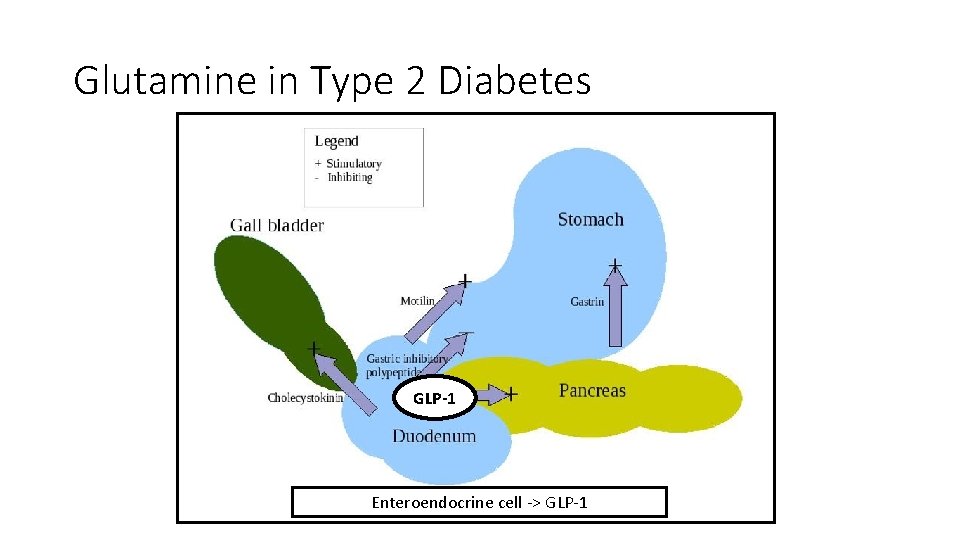
Glutamine in Type 2 Diabetes GLP-1 Enteroendocrine cell -> GLP-1
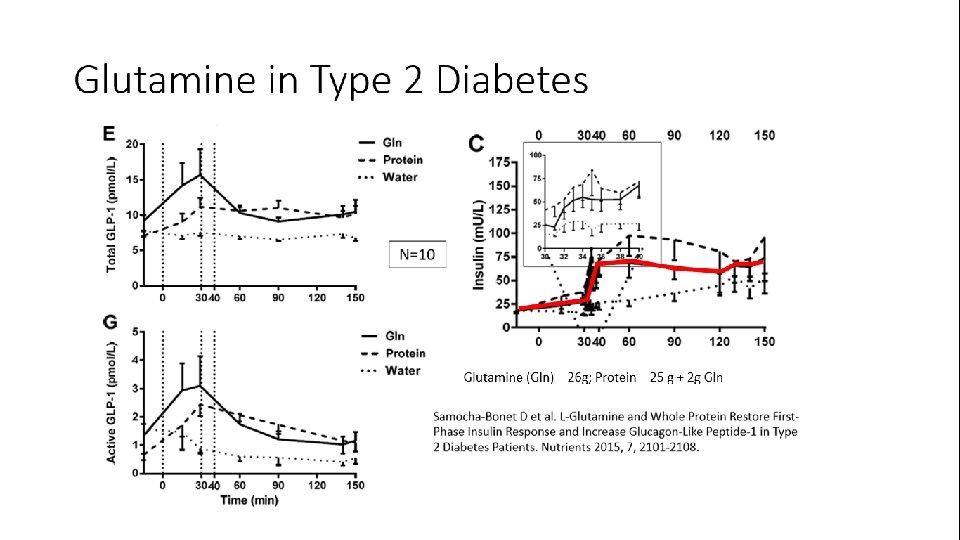
Glutamine in Type 2 Diabetes
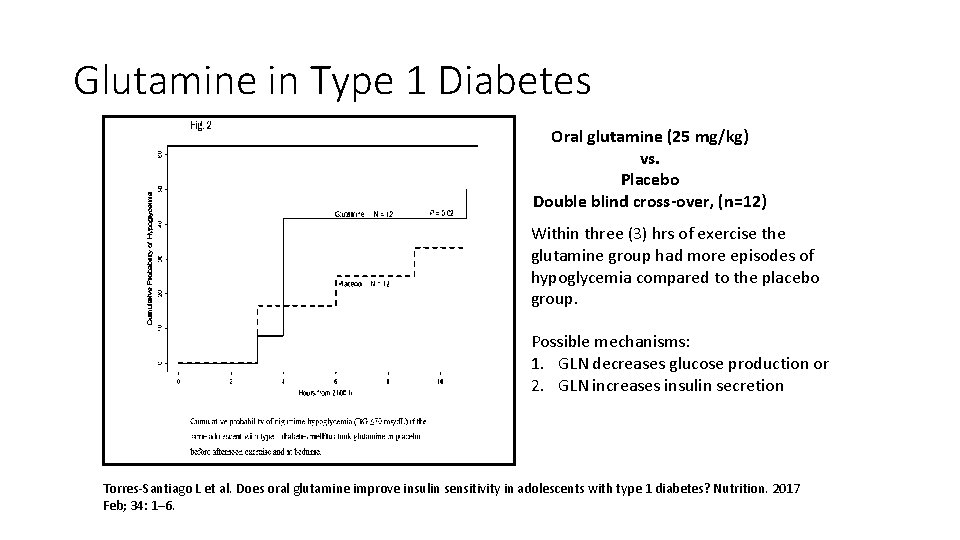
Glutamine in Type 1 Diabetes Oral glutamine (25 mg/kg) vs. Placebo Double blind cross-over, (n=12) Within three (3) hrs of exercise the glutamine group had more episodes of hypoglycemia compared to the placebo group. Possible mechanisms: 1. GLN decreases glucose production or 2. GLN increases insulin secretion Torres-Santiago L et al. Does oral glutamine improve insulin sensitivity in adolescents with type 1 diabetes? Nutrition. 2017 Feb; 34: 1– 6.
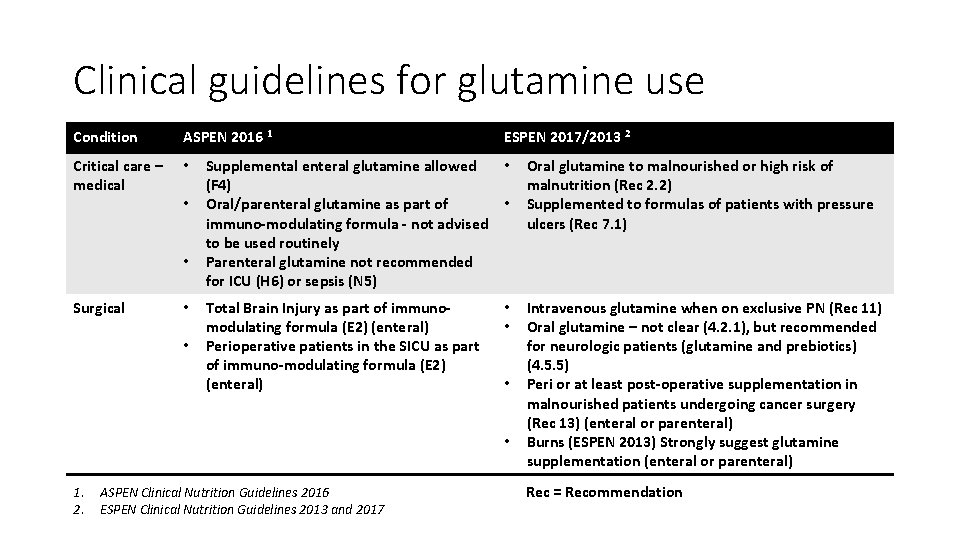




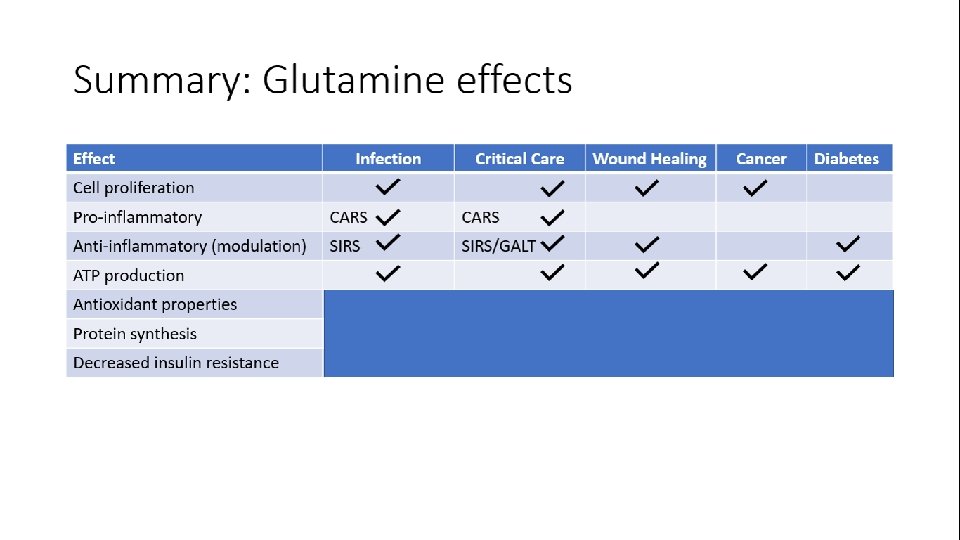
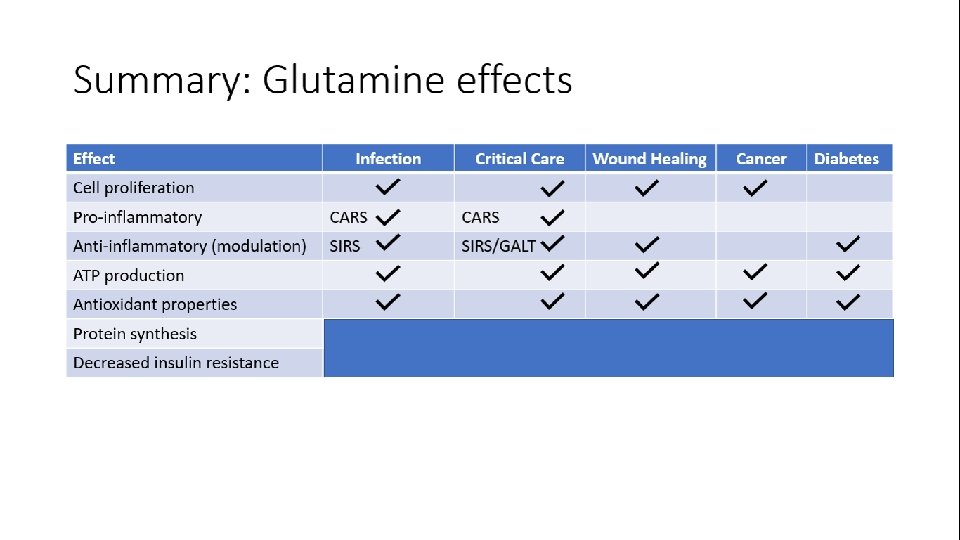
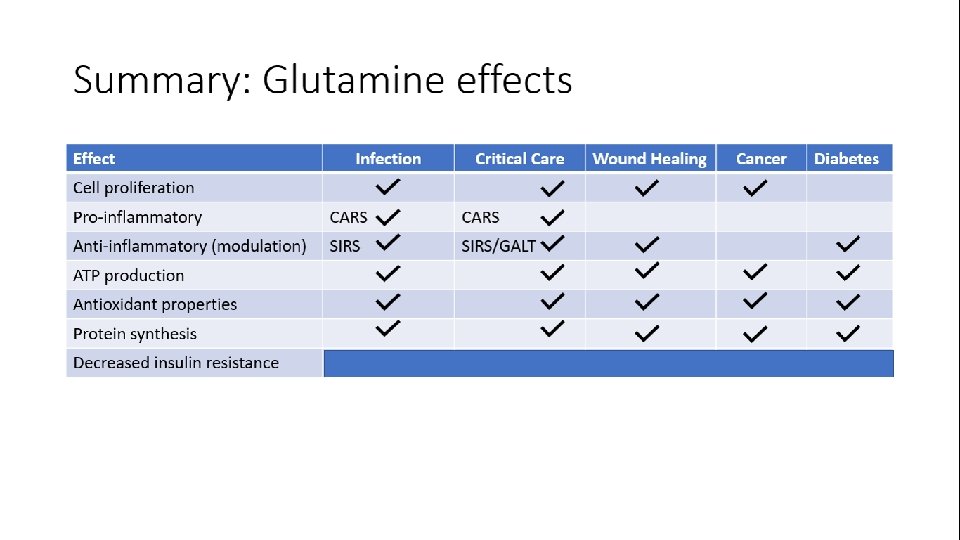

Clinical guidelines for glutamine use Condition ASPEN 2016 1 Critical care – medical • • • Surgical • • ESPEN 2017/2013 2 Supplemental enteral glutamine allowed • (F 4) Oral/parenteral glutamine as part of • immuno-modulating formula - not advised to be used routinely Parenteral glutamine not recommended for ICU (H 6) or sepsis (N 5) Oral glutamine to malnourished or high risk of malnutrition (Rec 2. 2) Supplemented to formulas of patients with pressure ulcers (Rec 7. 1) Total Brain Injury as part of immunomodulating formula (E 2) (enteral) Perioperative patients in the SICU as part of immuno-modulating formula (E 2) (enteral) Intravenous glutamine when on exclusive PN (Rec 11) Oral glutamine – not clear (4. 2. 1), but recommended for neurologic patients (glutamine and prebiotics) (4. 5. 5) Peri or at least post-operative supplementation in malnourished patients undergoing cancer surgery (Rec 13) (enteral or parenteral) Burns (ESPEN 2013) Strongly suggest glutamine supplementation (enteral or parenteral) • • 1. 2. ASPEN Clinical Nutrition Guidelines 2016 ESPEN Clinical Nutrition Guidelines 2013 and 2017 Rec = Recommendation
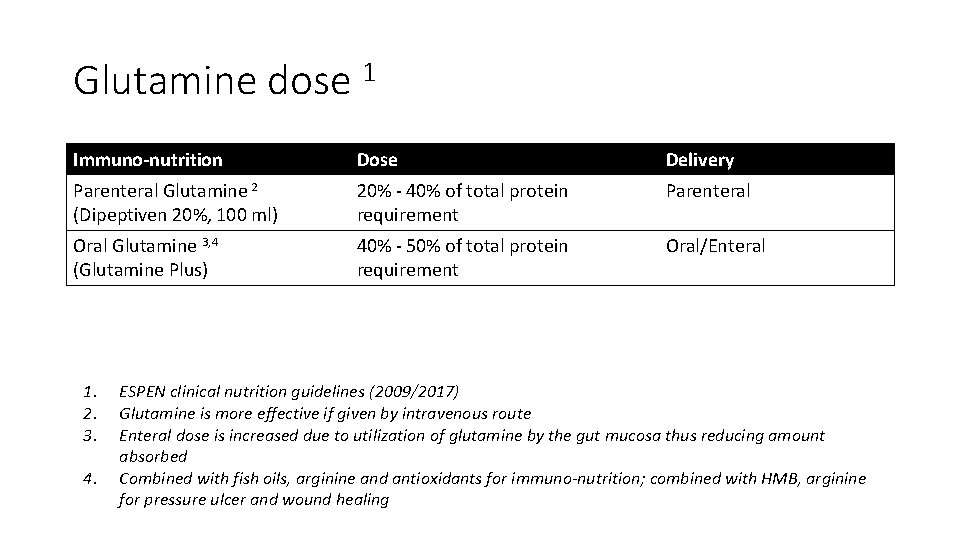
Glutamine dose 1 Immuno-nutrition Dose Delivery Parenteral Glutamine 2 (Dipeptiven 20%, 100 ml) 20% - 40% of total protein requirement Parenteral Oral Glutamine 3, 4 (Glutamine Plus) 40% - 50% of total protein requirement Oral/Enteral 1. 2. 3. 4. ESPEN clinical nutrition guidelines (2009/2017) Glutamine is more effective if given by intravenous route Enteral dose is increased due to utilization of glutamine by the gut mucosa thus reducing amount absorbed Combined with fish oils, arginine and antioxidants for immuno-nutrition; combined with HMB, arginine for pressure ulcer and wound healing

When to give glutamine • In surgery: • Preoperative build up: oral, tube feed or parenteral • Malnourished patient • Cancer patient • Post-operative: oral, tube feed or parenteral • All surgeries especially when malnourished or high risk • With complications • Burns: oral, enteral or parenteral • Surgical intensive care: oral, tube feed or parenteral • In medical/critical care: 1. Detect malnutrition 2. Determine nutrient requirements 3. Determine your glutamine dose 4. Determine route 5. Make sure prescribed diet is taken (70%-75%) 6. That means count intake daily/regularly • Malnourished or high risk of malnutrition: oral, tube feed or parenteral • Pressure ulcers: oral or enteral • Total brain injury: oral, enteral or parenteral

Thank You
- Slides: 52