GLUCOSE CLINICAL SIGNIFICANCE Glucose is the major carbohydrate

GLUCOSE, CLINICAL SIGNIFICANCE • Glucose is the major carbohydrate present in the peripheral blood. • Oxidation of glucose is the major source of cellular energy in the body. • Glucose derived from dietary sources is converted to glycogen for storage in the liver and muscle or to fatty acids for storage in adipose tissue. • Hyperglycemia (diabetes mellitus) occurs due to a relative deficiency or dysfunction of insulin. • A number of secondary factors also can contribute to elevated blood glucose levels. • These include pancreatitis, pituitary or thyroid dysfunction, renal failure and liver disease. • Hypoglycemia is less frequently observed. • A variety of conditions may cause hypoglycemia such as insulinemia, hypopituitarism, neoplasms or pharmacologic insulin induced hypoglycemia.

GLUCOSE Cond. • Glucose assay is the most commonly used test in the laboratory • Plasma glucose levels should be evaluated in relation to a patient’s meal i. e. , postprandial vs fasting. • Elevated glucose levels may also be indicative of diabetes mellitus Test Normal IFG or IGT Type 2 Diabetes Hemoglobin a 1 c <5. 7% 5. 7 to 6. 4% ≥ 6. 5% Fasting plasma glucose <100 mg/d. L 100 to 125 mg/d. L ≥ 126 mg/d. L OGTT after 2 hours <140 mg/d. L 140 to 199 mg/d. L ≥ 200 mg/d. L • Impaired glucose tolerance (IGT) or impaired fasting glucose (IFG) means that blood glucose is raised beyond normal levels (5. 6~6. 9 m. M/L), but not high enough to warrant a diabetes diagnosis. IGT indicates a much greater risk of developing diabetes and cardiovascular disease. • Glucose tolerance test (GT test) or Oral glucose tolerance test (OGTT) is the assay of serum glucose by feeding 75 g glucose solution and testing serum glucose at 1 -2 h interval.

METHODS FOR SERUM GLUCOSE ASSAY • • • Serum glucose is assayed enzymatically using glucose oxidase enzyme in the clinical laboratory. Today, enzymes, buffers and other color producing agents are prepared as a kit ready to load onto a auto-bioanalyzer. Biosensor is another technique/device that exploits this enzymatic method together with electron /proton measurement produced during oxidation of glucose. Glucometer is a device used at home for serum glucose assay that uses immobilized enzyme in a strip that is inserted in the device and a single drop of blood is put into the strip to be oxidised and the electron released is quantified by the device. Presence of glucose in urine is observed by using paper strips that gives a gross idea by change in color of the strip and the degree of urinary sugar excretion is denoted as +, ++, and +++ etc based on color deveoped on the strip within a few min of immersion in the urine.

BILIRUBIN, SIGNIFICANCE • • Bilirubin is a potentially toxic metabolite for the body to be excreted. Excessive levels of bilirubin in the bloodstream can lead to accumulation of bilirubin in the brain due to its ability to cross the blood–brain barrier, a condition known as kernicterus (meaning “yellow-stained nucleus”). The development of this condition impairs brain function by mechanisms that are not well-understood, but it can be fatal if left untreated. Bilirubin is also notable for its yellow coloration. Accumulation of this substance in the blood is the basis for jaundice, or a yellow discoloration of the skin and eyes which is a common symptom of liver diseases. Thus, measurement of bilirubin in the plasma can be a useful marker of such conditions. The total serum bilirubin level is the sum of the conjugated (direct) and unconjugated (indirect) bilirubin. – Normally the unconjugated bilirubin makes up 70 -85% of the total bilirubin Bilirubin metabolism begins with the breakdown of RBC in the reticuloendothelial system and it continues in the liver. – Elevation in total bilirubin may therefore be a reflection of any aberrations in bilirubin metabolism or increased levels of bilirubin production (such as hemolysis)

BILIRUBIN, Assay • In an older child or adult, normal values of direct bilirubin are from 0– 0. 4 mg/d. L. Normal values of total bilirubin are from 0. 3– 1. 0 mg/d. L. • For this test, at least 4 h fasting (except water) needed before collection of blood. • A small amount of your blood is needed to perform this test. The blood sample is obtained through venipuncture, a small amount of blood is collected in a test tube. • Cell Biolabs’ Bilirubin Assay Kit measures the total and direct bilirubin within serum, plasma, urine, cell lysates, or tissue lysate samples. • The assay is based on the Jendrassik-Grof method (Ref. 1) in which diazotized sulfanilic acid reacts with bilirubin to form azobilirubin, the latter of which can be detected at an OD of 540 nm (Figure 1). • Since unconjugated bilirubin and bilirubin bound to albumin react very slowly, an accelerant is added to the reaction to allow for measurement of total bilirubin. • In the absence of the accelerant, only the direct or conjugated bilirubin is measured. Diazotized Sulfanilic Acid + Direct (conjugated) Bilirubin → Azobilirubin (540 nm) Diazotized Sulfanilic Acid + Total Bilirubin + Accelerant → Azobilirubin (540 nm)

BLOOD UREA NITROGEN (BUN) • BUN measures the amount of urea nitrogen in the blood. • Urea is formed in the liver as the end product of protein metabolism and is transported to the kidneys for excretion. • A healthy kidneys remove BUN through urine, usually leaving a small amount of it in the blood. • A sick kidney has trouble removing BUN and leaves more of it in the blood. • Nearly all renal diseases can cause an inadequate excretion of urea, which causes the blood concentration to rise above normal. • The BUN is interpreted in conjunction with the creatinine test – these tests are referred to as “renal function studies”. • Additional causes of elevated BUN include: urinary tract obstruction, congestive heart failure or recent heart attack, gastrointestinal bleeding, dehydration resulting from drinking less fluids or for other reasons, shock, severe burns, certain antibiotics, and a high-protein diet.

BUN Assay v. For BUN test fasting is not necessary, even fasting does not alter the result. v Results of the BUN test are measured in mg/d. L in the United States and in mmol/L internationally. v. In general, around 7 to 20 mg/d. L (2. 5 to 7. 1 mmol/L) is considered normal. This range may vary, depending on the reference range used by the lab, and the age. v. There are two general methods for the BUN assay. v. The diacetyl, or Fearon, reaction develops a yellow chromogen with urea, and this is quantified by photometry. v. It has been modified for use in autoanalyzers and generally gives relatively accurate results. It still has limited specificity, however, as illustrated by spurious elevations with sulfonylurea compounds, and by colorimetric interference from hemoglobin when whole blood is used. v. In the more specific enzymatic methods, the enzyme urease converts urea to ammonia and carbonic acid. The products are proportional to the urea content in the sample. v. They are assayed in a variety of systems, some of which are automated. One system checks the decrease in absorbance at 340 mm when the ammonia reacts with alpha-ketoglutaric acid. v. The Astra system measures the rate of increase in conductivity of the solution in which urea is hydrolyzed. v. Even though the test is now performed mostly on serum, the term BUN is still retained by convention. The specimen should not be collected in tubes containing sodium fluoride because the fluoride inhibits urease. Also chloral hydrate and guanethidine have been observed to increase BUN values.

CREATININE • The creatinine test measures the amount of creatinine in the blood. • Creatinine is a catabolic product of creatine phosphate used in skeletal muscle contraction. • Creatinine, as with blood urea nitrogen, is excreted entirely by the kidneys and blood levels are therefore proportional to renal excretory function. • The normal serum creatinine (s. Cr) varies with the subject's body muscle mass and with the technique used to measure it. • For the adult male, the normal range is 0. 6 to 1. 2 mg/dl, or 53 to 106 μmol/L by the kinetic or enzymatic method, and 0. 8 to 1. 5 mg/dl, or 70 to 133 μmol/L by the older manual Jaffé reaction. • For the adult female, with her generally lower muscle mass, the normal range is 0. 5 to 1. 1 mg/dl, or 44 to 97 μmol/L by the enzymatic method.

METHODS FOR SERUM CREATININE ASSAY • Creatinine is assayed colorimetrically in clinical laboratories by using assay kits for faster and sensitive assay. • Here Bioanalyzer or Microplate reader is used for color measurement. • In the creatinine assay protocol, creatinine is converted to creatine by creatininase, • Creatine is converted to sarcosine, which is specifically oxidized to produce a product which reacts with a probe to generate red color (λmax = 570 nm). • Add samples and standards to wells, add reaction mix and incubate for 60 min at 37ºC, analyze with microplate reader.

KIDNEY FAILURE • • • Kidney failure is the inability of the kidneys to adequately filter metabolic waste products from the blood. Kidney failure has many possible causes. Some lead to a rapid decline in kidney function (acute kidney injury, also called acute renal failure). Others lead to a gradual decline in kidney function (chronic kidney disease, also called chronic renal failure). In addition to the kidneys being unable to filter metabolic waste products (such as creatinine and urea nitrogen) from the blood, the kidneys are less able to control the amount and distribution of water in the body (fluid balance) and the levels of electrolytes (sodium, potassium, calcium, phosphate) and acid in the blood. When kidney failure has lasted for some time, blood pressure often rises. The kidneys lose their ability to produce sufficient amounts of a hormone ( erythropoietin) that stimulates the formation of new red blood cells, resulting in a low red blood cell count (anemia). The kidneys also lose their ability to produce sufficient calcitriol (the active form of vitamin D), which is vital to bone health. In children, kidney failure affects the growth of bones. In both children and adults, kidney failure can lead to weaker, abnormal bones.
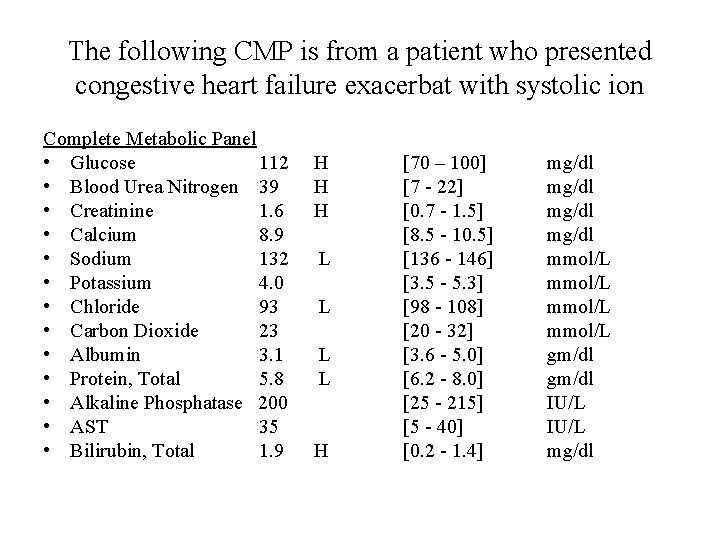
The following CMP is from a patient who presented congestive heart failure exacerbat with systolic ion Complete Metabolic Panel • Glucose 112 • Blood Urea Nitrogen 39 • Creatinine 1. 6 • Calcium 8. 9 • Sodium 132 • Potassium 4. 0 • Chloride 93 • Carbon Dioxide 23 • Albumin 3. 1 • Protein, Total 5. 8 • Alkaline Phosphatase 200 • AST 35 • Bilirubin, Total 1. 9 H H H L L H [70 – 100] [7 - 22] [0. 7 - 1. 5] [8. 5 - 10. 5] [136 - 146] [3. 5 - 5. 3] [98 - 108] [20 - 32] [3. 6 - 5. 0] [6. 2 - 8. 0] [25 - 215] [5 - 40] [0. 2 - 1. 4] mg/dl mmol/L gm/dl IU/L mg/dl

Interpretion? (Do not fret, you will begin learning this skill as MHD progresses and into your clerkships. This is only an example of how laboratory data will complement your understanding of pathophysiology!) • BUN and creatinine are elevated with a BUN: Creat ratio greater than 20: 1 consistent with pre-renal azotemia, the result of inadequate renal perfusion and resulting reduced urea clearance. • Hepatic congestion leads to hypoxia and altered function of the liver cells. Bilirubin, especially the indirect fraction, and enzymes, like alkaline phosphatase, may be elevated. Total protein may decline at the expense of the decreased albumin produced in the liver. • The electrolyte changes, especially hyponatremia, reflect a dilutional effect with water retention and decreased glomerular filtration rate (poor perfusion) • Hyperglycemia is present but it is not known whether this was a fasting or random sample

One final BMP pearl • Clinicians have a short-hand way to report BMP values: NA K Cl BUN C 02 Cr If we look at the last BMP… 142 107 10 3. 9 27 0. 8 100 Glu

LIPID PROFILE • A lipid profile means the complete picture of lipids present in blood. Lipid profile affects the health of the circulatory system. • It is a panel of blood tests that serves as an initial screening tool for abnormalities in lipids. • It includes: assay of total cholesterol, Triacyl Glycerol, Low Density Lipoprotein, High Density Lipoprotein, Very Low Density Lipoprotein, cholesterol: HDL ratio. • Abnormal lipid profile causes diseases of the circulatory system including atherosclerosis, heart diseases and certain forms of pancreatitis. • Lipid profile is ordered along with other parameters such as CBC and BMP. • Traditionally, most laboratories have required patients to fast for 9– 12 hours before screening. • However, recent studies have questioned the utility of fasting before lipid panels, and some diagnostic labs now routinely accept non-fasting samples.
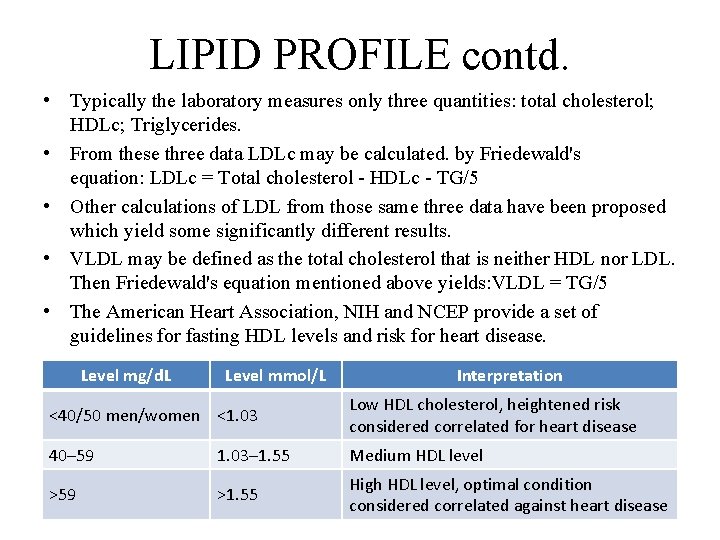

LIPID PROFILE contd. • Typically the laboratory measures only three quantities: total cholesterol; HDLc; Triglycerides. • From these three data LDLc may be calculated. by Friedewald's equation: LDLc = Total cholesterol - HDLc - TG/5 • Other calculations of LDL from those same three data have been proposed which yield some significantly different results. • VLDL may be defined as the total cholesterol that is neither HDL nor LDL. Then Friedewald's equation mentioned above yields: VLDL = TG/5 • The American Heart Association, NIH and NCEP provide a set of guidelines for fasting HDL levels and risk for heart disease. Level mg/d. L Level mmol/L Interpretation <40/50 men/women <1. 03 Low HDL cholesterol, heightened risk considered correlated for heart disease 40– 59 1. 03– 1. 55 Medium HDL level >59 >1. 55 High HDL level, optimal condition considered correlated against heart disease

METHODS FOR LIPID PROFILE ØTotal Cholesterol is measured enzymatically in serum or plasma in a series of coupled reactions that hydrolyze cholesteryl esters and oxidize the 3 -OH group of cholesterol. Ø One of the reaction byproducts, H 2 O 2 is measured quantitatively in a peroxidase catalyzed reaction that produces a color. ØAbsorbance is measured at 500 nm. The color intensity is proportional to cholesterol concentration. The reaction sequence is as follows: ØCholesteryl ester + H 2 O ----cholesteryl ester hydrolase ----->cholesterol + fatty acid ØCholesterol + O 2 -----Cholesterol Oxidase-------> cholest-4 -en-3 -one + H 2 O 2 Ø 2 H 2 O 2 + 4 -aminophenazone + phenol ----Peroxidase------> 4 -(p-benzoquinone monoimino)-phenazone + 4 H 2 O. ØTriglycerides are measured enzymatically in serum or plasma using a series of coupled reactions in which triglycerides are hydrolyzed to produce glycerol. Glycerol is then oxidized using glycerol oxidase, and H 2 O 2, one of the reaction products, is measured as described above for cholesterol. Absorbance is measured at 500 nm. The reaction sequence is as follows: ØTriglycerides + 3 H 2 O ---Lipase----> glycerol + fatty acids ØGlycerol + ATP ----Glycerokinase-------> glycerol-3 -phosphate + ADP

Contd. ØGlycerol-3 -phosphate + O 2 ---Glycerophosphate oxidase----> dihydroxyacetone phosphate + H 2 O 2 ØH 2 O 2 + 4 -aminophenazone + 4 -chlorophenol ---Peroxidase--> 4 -(p-benzoquinonemonoimino)- phenazone + 2 H 2 O + HCl. ØDirect HDL method. HDL is measured directly in serum. The basic principle of the method is as follows. ØThe apo. B containing lipoproteins in the specimen are reacted with a blocking reagent that renders them non-reactive with the enzymatic cholesterol reagent under conditions of the assay. ØThe apo. B containing lipoproteins are thus effectively excluded from the assay and only HDL-chol is detected under the assay conditions. ØThe method uses sulfated alpha-cyclodextrin in the presence of Mg+2, which forms complexes with apo. B containing lipoproteins, and polyethylene glycol-coupled cholesteryl esterase and cholesterol oxidase for the HDL-cholesterol measurement. The reactions are as follows: ØApo. B containing lipoproteins + α-cyclodextrin + Mg+2 + dextran SO 4 ---> soluble nonreactive complexes with apo. B-containing lipoproteins

Contd. ØHDL-cholesteryl esters ……PEG-cholesteryl esterase > HDL-unesterified cholesterol + fatty acid. ØUnesterified chol + O 2 …. . PEG-cholesterol oxidase > cholestenone + H 2 O 2 ØH 2 O 2 + 5 -aminophenazone + N-ethyl-N-(3 -methylphenyl)-N’_succinyl ethylene diamine + H 2 O + H+ peroxidase > qunoneimine dye + H 2 O ØAbsorbance is measured at 600 nm.
- Slides: 18