Glomerulonephritis Yonas G BPharm Msc Glomerulonephritis Glomerulus capillary
Glomerulonephritis Yonas G. (BPharm, Msc. )

Glomerulonephritis Glomerulus – capillary loop with basement membrane which allows passage of specific molecules into the nephron Glomerulonephritis – inflammation/damage of the glomerular basement membrane resulting in altered function. Can present as nephrotic and/or nephritic syndrome. 2

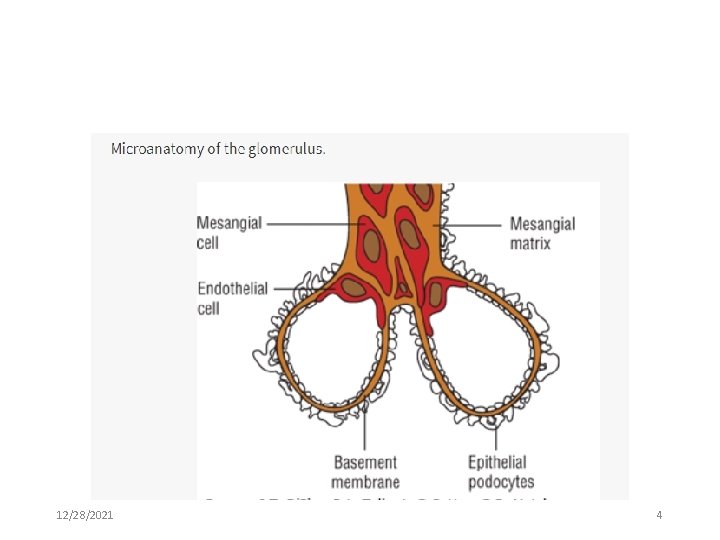
NORMAL GLOMERULAR ANATOMY AND FUNCTION • The glomerulus, which is enclosed within the Bowman’s capsule, consists of two important components: ØThe capillary wall: primary filtration barrier, ØThe mesangium: provides support for the glomerular capillaries and also modulates blood flow through the capillaries. • CW: allows small nonprotein plasma constituents up to the size of inulin(5. 2 KDa) to pass freely while excluding macromolecules equal to or larger than albumin (69 KDa). • Passage through the glomerular membrane (GM) is impacted by both the size and charge (-vely charged restricted) of the solute. 12/28/2021 3
12/28/2021 4

EPIDEMIOLOGY AND ETIOLOGY • In the US, glomerulonephritis was the third most common cause of ESRD, • accounting for approximately 16% of all the living ESRD patients. • Humoral and cellular immunologic mechanisms participate in the pathogenesis of most glomerulonephritis. 12/28/2021 5

PATHOPHYSIOLOGY • The glomerular lesion characterized/appeared as; • diffuse (involving all glomeruli), • focal (involving some but not all glomeruli), or • segmental, also known as local (involving part of the individual glomerulus). • The pathologic manifestations may also be described as proliferative (overgrowth of epithelium, endothelium, or mesangium), membranous (thickening of GBM), and/or sclerotic. 12/28/2021 6

• The glomerular capillary wall is particularly susceptible to immune-mediated injury. • Antigens and antibodies tend to localize in the glomerulus, • because of its high blood flow and capillary hydrostatic pressure. • Parenchymal damage can be induced as a result of humoral- and cell-mediated immune reactions. • Antibodies and sensitized T lymphocytes are the primary mediators 12/28/2021 7

• This days an increasing body of evidence show that infections initiate most forms of GN through activation of innate immune response. • Production of antibodies to endogenous or exogenous antigens that are recognized as foreign by the host is the first step in humoral immunologic damage to the glomerulus. 12/28/2021 8

Clinical manifestation 12/28/2021 9

Nephrotic Syndrome • NS is characterized by proteinuria greater than 3. 5 g/day/1. 73 m 2, hypoproteinemia, edema, and hyperlipidemia. • A hypercoagulable state may also be present in some patients. • Normal urinary protein excretion is between 40 and 80 mg/day, with a maximum of 150 mg. • Fewer than 20 mg of the excreted proteins are albumin. 12/28/2021 10

Nephritic Syndrome • Glomerular bleeding resulting in hematuria is typical in nephritic syndrome. • Dysmorphic red cells, especially acanthocytes, are a sensitive and specific marker of glomerular bleeding. • The presence of pus and cellular and granular casts in the urine is common. 12/28/2021 11

DIAGNOSTIC CONSIDERATIONS • History to identify potential systemic causes. • Medication, environmental, and occupational histories may also help identify exposure to potentially nephrotoxic agents. • A comprehensive physical examination and laboratory evaluation may reveal the presence of systemic diseases that may contribute to the development of glomerular disease. • Urinalysis to differentiate the nephrotic from nephritic disease. • The GFR may be used to determine the extent of glomerular damage. • In the early stages of the disease, the GFR may remain normal. • Biopsy: for specific Dx. 12/28/2021 12

Treatment General approach • In secondary glomerular diseases, such as PSGN, after the initiating factor is removed, the prognosis of the renal disease is often good. • In contrast, the rates of renal function deterioration among the primary glomerulonephritis vary markedly. • The majority of patients with minimal-change disease, Ig. A nephropathy, and membranous nephropathy have a good prognosis. 12/28/2021 13

Non-pharmacologic Therapy For patients with nephrotic syndrome, dietary measures involve; • restriction of sodium intake to 50 to 100 m. Eq/day (mmol/day), • protein intake of < 0. 8 to 1 g/day and • a low-fat diet of less than 200 mg cholesterol per day. • Total fat should account for less than 30% of daily total calories. • Stop smoking 12/28/2021 14

Pharmacologic Therapy Immunosuppressive Agents • Immunosuppressive agents, alone or in combination, are commonly used to alter the immune processes. • Corticosteroids, as a result of their immunosuppressive and anti-inflammatory activities reduce the production and/or release of many substances that mediate the inflammatory process, • such as prostaglandins, leukotrienes, platelet-activating factors, tumor necrosis factors, and interleukin-1 (IL-1). • Cytotoxic agents, such as cyclophosphamide, chlorambucil, or azathioprine, are commonly used to treat glomerular diseases. 12/28/2021 15

• Cyclosporine can reduce lymphokine production by activated T lymphocytes, and it may decrease proteinuria by improving the permeability of the GBM. • Several new agents, such as monoclonal antibodies (rituximab), imidazole nucleoside (mizoribine), are now being evaluated for their usefulness 12/28/2021 16

Diuretics • Management of nephrotic edema involves salt restriction, bed rest, and use of support stockings and diuretics. • Large doses of the loop diuretic, such as 160 to 480 mg of furosemide, may be needed for patients with moderate edema. • availability at luminal receptor sites ↓ • In some instances, a thiazide diuretic or metolazone may be added to enhance natriuresis. 12/28/2021 17

• For patients with morbid edema, albumin infusion may be used. • To expand plasma volume and increase diuretic delivery to the renal tubules, thus enhancing diuretic effect. • May precipitate congestive heart failure. • For patients with significant edema, the goal of treatment should be a daily loss of 1 to 2 lb (0. 45 -0. 9 kg) of fluid until the patient’s desired weight has been obtained. 12/28/2021 18

Antihypertensive Agents • ACEIs/ARBs delay the loss of renal function for patients with diabetic and nondiabetic (primarily glomerulonephritis) renal diseases. • ACEIs/ARBs can reduce proteinuria through different mechanisms and combined use has been shown to be more effective than monotherapy. • NDHP CCB (diltiazem and verapamil) reduce proteinuria and preserve renal function and could be used as an additional agent. • In contrast, the DHP CCB (nifedipine, amlodipine) are effective in lowering blood pressure, but without the benefit of proteinuria reduction. 12/28/2021 19

NSAIDS • Probably reduce proteinuria through PGE 2 inhibition, resulting in a reduction of intraglomerular pressure, • Indomethacin and meclofenamate, the two most evaluated NSAIDs • similar efficacy to ACEIs, and combined treatment with an ACEI. • However, adherence to a low-sodium diet or concurrent use of a diuretic is needed to maximize the antiproteinuric effect. • Because of their potential for nephrotoxicity, especially for patients with preexisting CKD, long-term use of an NSAID for renoprotection is not commonly prescribed. 12/28/2021 20

Adrenocorticotropin • A synthetic ACTH analog has been used in Europe for proteinuria reduction associated with nephrotic syndrome. • It was reported to have effects similar to alternating months of steroids and cyclophosphamide. • Instead of the synthetic analog, a natural, purified ACTH gel is available in the US and is approved by the FDA 12/28/2021 21

Statins • It is important to treat patients with persistent nephrotic syndrome, especially those with high VLDL and LDL cholesterol levels. • Therapy is especially needed for those with concurrent atherosclerotic cardiovascular disease, or with additional risk factors for atherosclerosis, • such as smoking and hypertension. • HMG-Co. A reductase inhibitors, also known as “statins” such as simvastatin, atorvastatin are considered the treatment of choice 12/28/2021 22

• They reduce total plasma cholesterol concentration, LDL cholesterol, and total plasma triglyceride concentrations • Aside from the lipid-lowering effects, statins can reduce cardiovascular risk independent of serum lipid concentrations. • Renoprotection: through the reduction of cell proliferation and mesangial matrix accumulation and their antiinflammatory and immunomodulatory effects. • Limited studies revealed the effect on renal function preservation is not clear. 12/28/2021 23

Anticoagulants • Renal vein thrombosis, PE, or other thromboembolic events are serious and common complications of nephrotic syndrome, • Documented thromboembolic episodes should be anticoagulated with warfarin until remission of nephrotic syndrome • The use of prophylactic anticoagulation is controversial 12/28/2021 24

Selective prophylactic use recommended in the following circumstances: • Severe nephrotic syndrome & serum albumin concentration less than 2 -2. 5 g/d. L • Those who require prolonged bed rest, • Those receiving high-dose IV steroid therapy, • Individuals who are dehydrated • Postsurgical patients 12/28/2021 25

Conclusions 26 n Nephrotic syndrome results from increased GBM permeability and is associated with proteinuria, hypoalbuminemia, edema and hyperlipidemia � n Minimal Change Disease is the most common cause of Nephrotic Syndrome in Children and respondes well to steroids Nephritic Syndrome results from Immune Complex mediated inflammation of the glomerular capillaries, which generally results in Hematuria � Acute Post Strep Glomerulonephritis is the most common cause of GN and has a good prognosis, requiring mostly supportive care

Nephritic vs Nephrotic Clinical Patterns of Glomerular Disease n. Nephrotic: • Proteinuria >3. 5 g/day • Edema • Hyperlipidemia • Red cell casts usually absent n. Nephritic (Immune complex Glomerular Inflammation): • Red cells +/- casts • Usually <3. 5 g/day proteinuria • Hypertension • Acute Renal Failure • Edema 27

Evaluation of Therapeutic Outcomes 12/28/2021 28
Thank you 12/28/2021 29
- Slides: 29