Global Programme to Eliminate Lymphatic Filariasis GPELF Training

Global Programme to Eliminate Lymphatic Filariasis (GPELF) Training in monitoring and epidemiological assessment of mass drug administration for eliminating lymphatic filariasis TAS Module 1 Background

Learning objectives By the end of this module, you should be able to answer the questions: 1. What is lymphatic filariasis (LF)? 2. What is the Global Programme to Eliminate Lymphatic Filariasis (GPELF)? 3. What is a transmission assessment survey (TAS)? 4. How does the national programme report to the GPELF? Slide 2 Module 1 Background

Overview q What is LF? q The GPELF q Programme steps for interrupting transmission § Mapping § Mass drug administration (MDA) § Monitoring and evaluation during MDA § TAS § Post-MDA surveillance q Slide 3 Reporting to the GPELF Module 1 Background
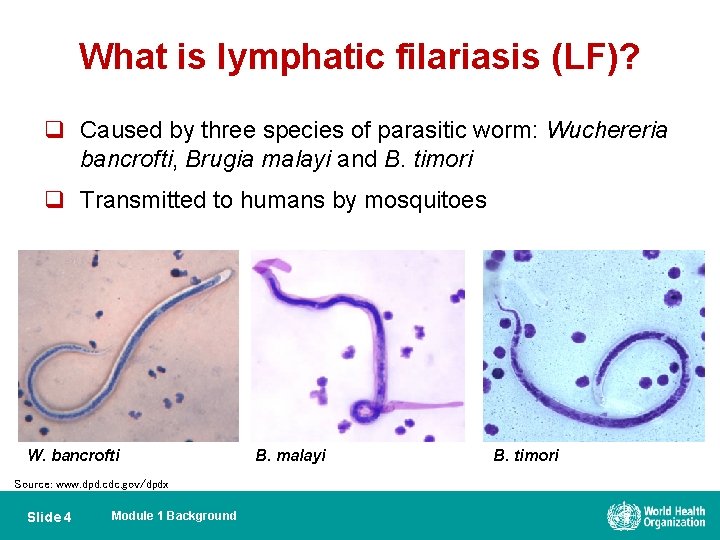
What is lymphatic filariasis (LF)? q Caused by three species of parasitic worm: Wuchereria bancrofti, Brugia malayi and B. timori q Transmitted to humans by mosquitoes W. bancrofti Source: www. dpd. cdc. gov/dpdx Slide 4 Module 1 Background B. malayi B. timori

What is lymphatic filariasis (LF)? q The commonest clinical manifestations are lymphoedema, which affects 15 million people, and scrotal hydrocoele, which affects 25 million men Lymphoedema Slide 5 Module 1 Background Hydrocoele
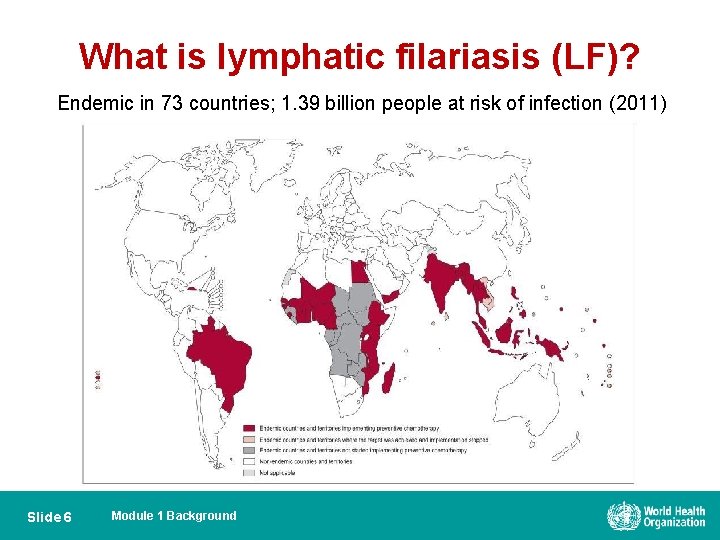
What is lymphatic filariasis (LF)? Endemic in 73 countries; 1. 39 billion people at risk of infection (2011) Slide 6 Module 1 Background

Global Programme to Eliminate Lymphatic Filariasis (GPELF) q In 1997, the World Health Assembly resolved to eliminate lymphatic filariasis as a public health problem (WHA resolution 50. 29). q In 2000, the GPELF was launched by WHO Goal: Global elimination by 2020 Aim 1. Stop the spread of infection: interrupt transmission by MDA Aim 2. Reduce the suffering caused by the disease: morbidity management and disability prevention Slide 7 Module 1 Background

Global Programme to Eliminate Lymphatic Filariasis (GPELF) GPELF works in partnership with: § the ministries of health of countries endemic for LF, which are responsible for national programmes § donors § pharmeceutical and diagnostics companies § academic and research institutions § nongovernmental organizations § WHO Slide 8 Module 1 Background
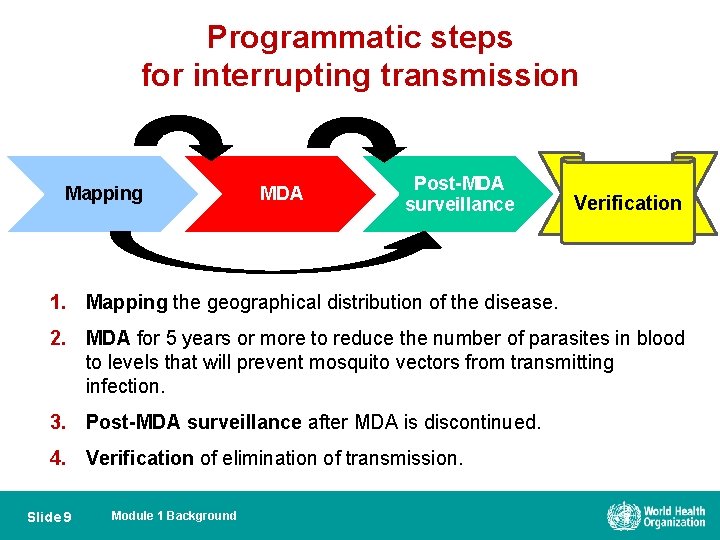
Programmatic steps for interrupting transmission Mapping MDA Post-MDA surveillance Verification 1. Mapping the geographical distribution of the disease. 2. MDA for 5 years or more to reduce the number of parasites in blood to levels that will prevent mosquito vectors from transmitting infection. 3. Post-MDA surveillance after MDA is discontinued. 4. Verification of elimination of transmission. Slide 9 Module 1 Background

Mapping: to determine whether active transmission is occurring and whether MDA is necessary. 1. Define the implementation unit (IU) for MDA. 2. Conduct mapping by: § reviewing existing information § conducting mapping surveys ü Measure antigenaemia by immunochromatographic tests (ICT) or measure microfilaria in blood films from older school-aged or adult populations. If the prevalence in this population is ≥ 1%, classify the IU as endemic. Slide 10 Module 1 Background

MDA GPELF recommends mass administration: q of a combination of medicines: § diethylcarbamazine (DEC) + albendazole (in countries not co-endemic for onchocerciasis) § ivermectin + albendazole (in countries co-endemic for onchocerciasis) q of single-dose treatment for at least 5 years q to all eligible individuals in the entire endemic area The objective is to achieve: • a reduction in the density of microfilariae circulating in the blood of infected individuals and • a reduction in the prevalence of infection in the entire community to levels at which it is assumed that microfilariae can no longer be transmitted by mosquito vectors to new human hosts. Slide 11 Module 1 Background
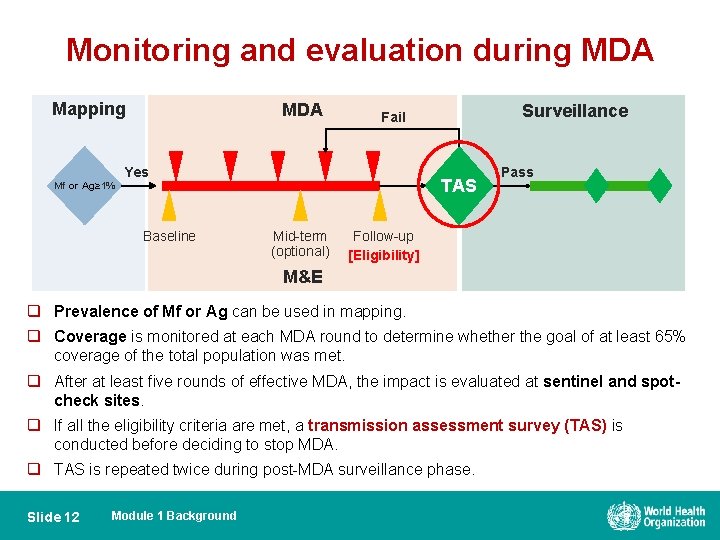
Monitoring and evaluation during MDA Mapping MDA Yes TAS Mf or Ag≥ 1% Baseline Surveillance Fail Mid-term (optional) Pass Follow-up [Eligibility] M&E q Prevalence of Mf or Ag can be used in mapping. q Coverage is monitored at each MDA round to determine whether the goal of at least 65% coverage of the total population was met. q After at least five rounds of effective MDA, the impact is evaluated at sentinel and spotcheck sites. q If all the eligibility criteria are met, a transmission assessment survey (TAS) is conducted before deciding to stop MDA. q TAS is repeated twice during post-MDA surveillance phase. Slide 12 Module 1 Background

Transmission assessment Survey (TAS) A TAS is the basis for a decision to move from MDA to post-MDA surveillance. Technical aspect Guidance Geographical area Evaluation Unit (EU) When survey should be conducted • • Target population Children aged 6– 7 years Diagnostic tests W. bancrofti areas: ICT Brugia spp. areas: Brugia Rapid™ Survey design Cluster sampling or systematic sampling in schools or the community, or a census When all the eligibility criteria are met At least 6 months after the last round of MDA A TAS is a simplified version of the ‘stopping-MDA survey’ protocol. Slide 13 Module 1 Background

Limitations of previous guideline Mapping MDA Fail Yes Stopping MDA survey Mf or Ag≥ 1% Baseline < 1% Mf < 0. 1% ICT LQAS 3000 children Mid-term (optional) Difficult to implement; extremely conservative threshold. Surveillance Pass Follow-up [Eligibility] M&E q An additional 5– 10 sentinel or spot-check tests were required per IU. q Antigenaemia surveys of 2– 4 -year-old children were not informative in most countries. q Lot quality assurance sampling surveys were difficult to implement (e. g. too many schools to visit per IU to test 3000 children). q The 1 in 3000 threshold was too conservative. Slide 14 Module 1 Background

Post-MDA surveillance p A TAS is not only an important decision-making step for stopping MDA but is also one of the methods of post-MDA surveillance recommended for detecting whether recrudescence of transmission has occurred. p A survey should be repeated at least twice after MDA is stopped, at an interval of 2– 3 years, to ensure that recrudescence has not occurred and therefore transmission can be considered interrupted. Mapping MDA Yes TAS Mf or Ag≥ 1% Baseline Mid-term (optional) M&E Slide 15 Module 1 Background Surveillance Fail Follow-up [Eligibility] Pass
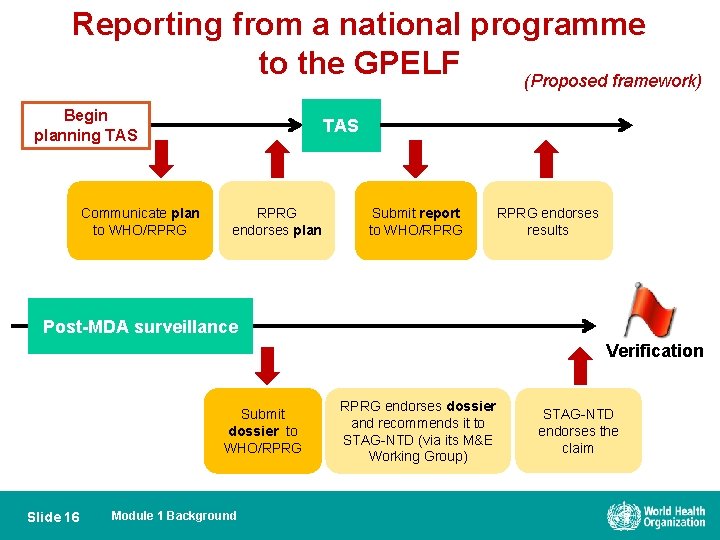
Reporting from a national programme to the GPELF (Proposed framework) Begin planning TAS Communicate plan to WHO/RPRG TAS RPRG endorses plan Submit report to WHO/RPRG endorses results Post-MDA surveillance Verification Submit dossier to WHO/RPRG Slide 16 Module 1 Background RPRG endorses dossier and recommends it to STAG-NTD (via its M&E Working Group) STAG-NTD endorses the claim
- Slides: 16