Global Action Plan to combat antimicrobial resistance Antimicrobial

Global Action Plan to combat antimicrobial resistance | Antimicrobial Resistance Global Report on Surveillance 2014
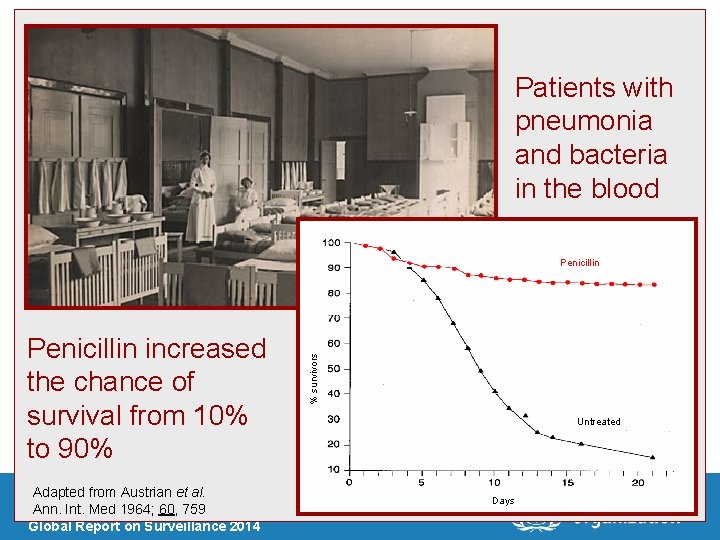
Patients with pneumonia and bacteria in the blood Penicillin increased the chance of survival from 10% to 90% Adapted from Austrian et al. | Ann. Int. Med 1964; 60, 759 Antimicrobial Resistance Global Report on Surveillance 2014 % survivors Penicillin Untreated Days
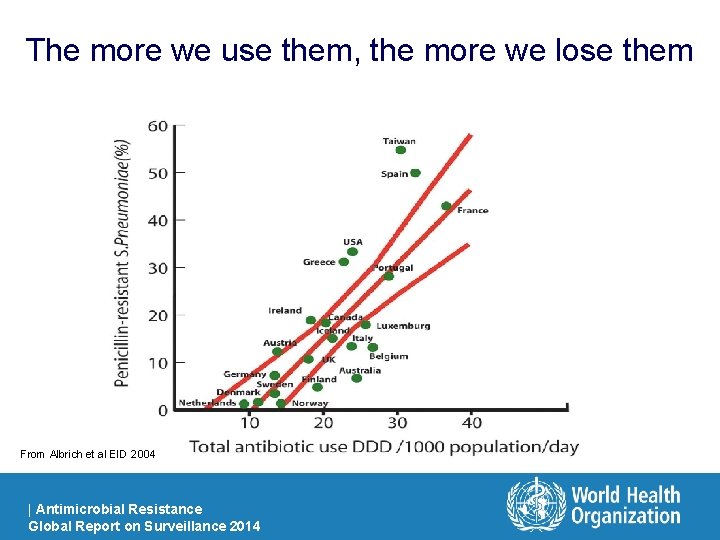
The more we use them, the more we lose them From Albrich et al EID 2004 | Antimicrobial Resistance Global Report on Surveillance 2014
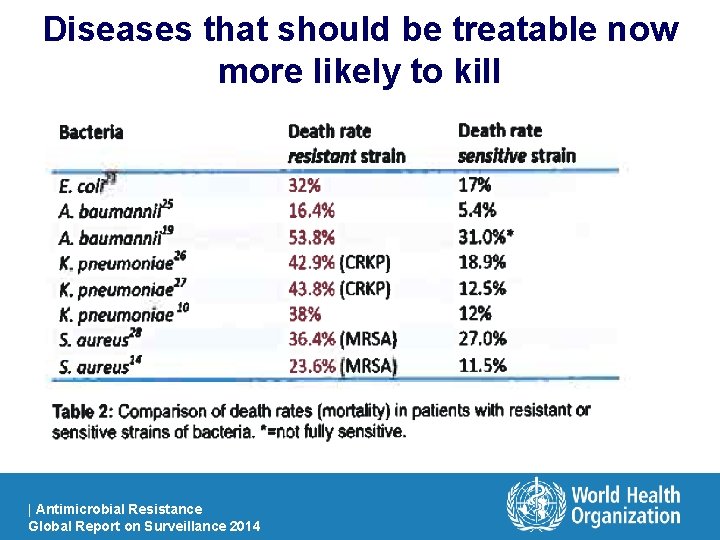
Diseases that should be treatable now more likely to kill | Antimicrobial Resistance Global Report on Surveillance 2014

Impact on mutliple sectors of health care Infectious disease Medical Procedures l Pneumonia l Neonatal care l Gonorrhea l Transplantation l Enteric infections l Cancer treatment l Blood infections l Surgery l etc. | Antimicrobial Resistance Global Report on Surveillance 2014

Why now? Increasingly serious global public health threat – New evidence and information – Desperation over "dry pipeline" Economic impact – World Economic Forum 2013 Global Risk Report Growing awareness and commitment – Political, professional, public | Antimicrobial Resistance Global Report on Surveillance 2014
| Antimicrobial Resistance Global Report on Surveillance 2014

Antimicrobial Resistance Global Report on Surveillance 2014 (I) • Focuses on antibacterial resistance (ABR) • Information gathered include: Surveillance of ABR according to WHO regions National and published data on 7 bacteria | Antimicrobial Resistance Global Report on Surveillance 2014 Systematic reviews of evidence of health and economic burden in 5 bacteria/ resistance combinations Identification of gaps

Selected Bacteria/Resistance Combinations Bacterium Resistance/ decreased susceptibility to: Escherichia coli 3 rd generation cephalosporins, fluoroquinolones Klebsiella pneumoniae 3 rd generation cephalosporins, carbapenems Staphylococcus aureus Methicillin (beta-lactam antibiotics) i. e. MRSA Streptococcus pneumoniae Penicillin Nontyphoidal Salmonella (NTS) Fluoroquinolones Shigella species Fluoroquinolones Neisseria gonorrhoeae 3 rd generation cephalosporins | Antimicrobial Resistance Global Report on Surveillance 2014
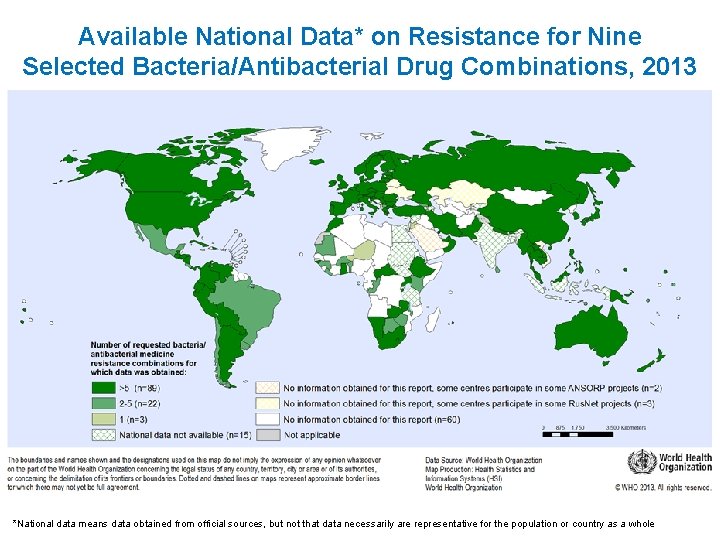
Available National Data* on Resistance for Nine Selected Bacteria/Antibacterial Drug Combinations, 2013 *National data means data obtained from official sources, but not that data necessarily are representative for the population or country as a whole
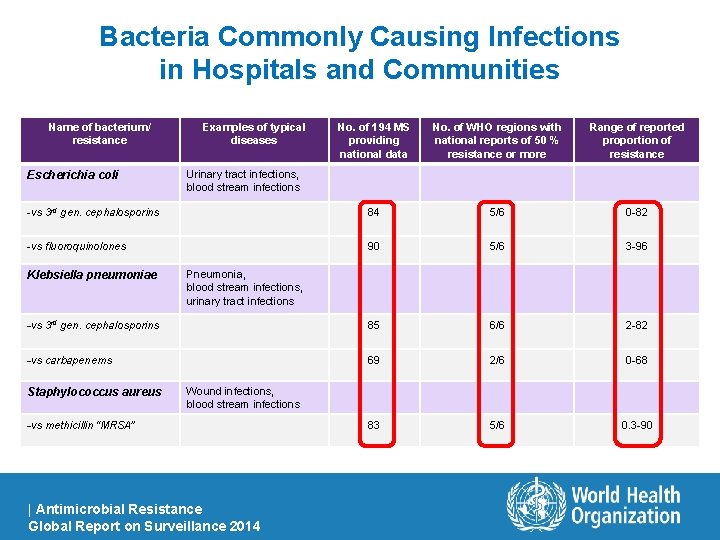

Bacteria Commonly Causing Infections in Hospitals and Communities Name of bacterium/ resistance No. of 194 MS providing national data No. of WHO regions with national reports of 50 % resistance or more Range of reported proportion of resistance -vs 3 rd gen. cephalosporins 84 5/6 0 -82 -vs fluoroquinolones 90 5/6 3 -96 -vs 3 rd gen. cephalosporins 85 6/6 2 -82 -vs carbapenems 69 2/6 0 -68 83 5/6 0. 3 -90 Escherichia coli Klebsiella pneumoniae Staphylococcus aureus Examples of typical diseases Urinary tract infections, blood stream infections Pneumonia, blood stream infections, urinary tract infections Wound infections, blood stream infections -vs methicillin “MRSA” | Antimicrobial Resistance Global Report on Surveillance 2014
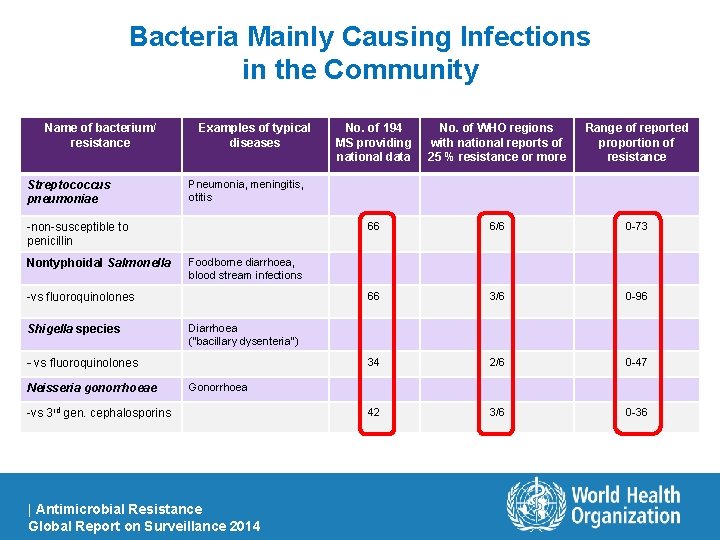

Bacteria Mainly Causing Infections in the Community Name of bacterium/ resistance Streptococcus pneumoniae Examples of typical diseases 66 6/6 0 -73 66 3/6 0 -96 34 2/6 0 -47 42 3/6 0 -36 Diarrhoea (“bacillary dysenteria”) - vs fluoroquinolones Neisseria gonorrhoeae Range of reported proportion of resistance Foodborne diarrhoea, blood stream infections -vs fluoroquinolones Shigella species No. of WHO regions with national reports of 25 % resistance or more Pneumonia, meningitis, otitis -non-susceptible to penicillin Nontyphoidal Salmonella No. of 194 MS providing national data Gonorrhoea -vs 3 rd gen. cephalosporins | Antimicrobial Resistance Global Report on Surveillance 2014

Systemic Reviews: Evidence of the Burden of Antibacterial Resistance Is there any difference in outcome from infections caused by resistant vs sensitive bacteria? | Antimicrobial Resistance Global Report on Surveillance 2014
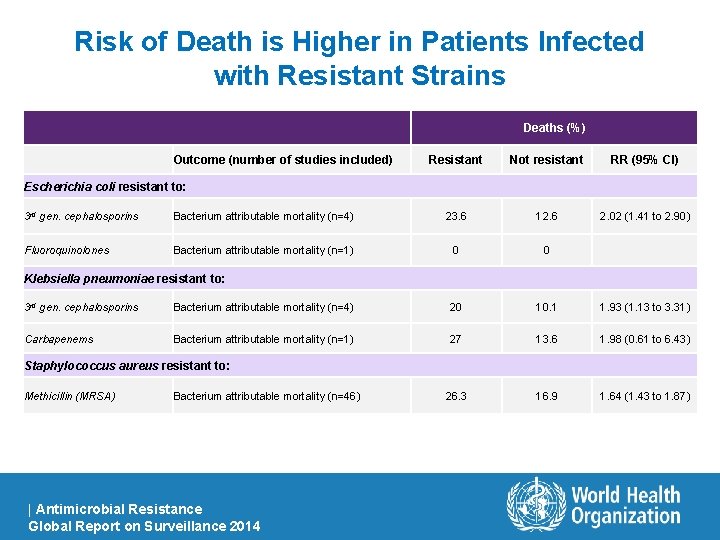
Risk of Death is Higher in Patients Infected with Resistant Strains Deaths (%) Outcome (number of studies included) Resistant Not resistant RR (95% CI) 2. 02 (1. 41 to 2. 90) Escherichia coli resistant to: 3 rd gen. cephalosporins Bacterium attributable mortality (n=4) 23. 6 12. 6 Fluoroquinolones Bacterium attributable mortality (n=1) 0 0 Klebsiella pneumoniae resistant to: 3 rd gen. cephalosporins Bacterium attributable mortality (n=4) 20 10. 1 1. 93 (1. 13 to 3. 31) Carbapenems Bacterium attributable mortality (n=1) 27 13. 6 1. 98 (0. 61 to 6. 43) 26. 3 16. 9 1. 64 (1. 43 to 1. 87) Staphylococcus aureus resistant to: Methicillin (MRSA) Bacterium attributable mortality (n=46) | Antimicrobial Resistance Global Report on Surveillance 2014

Estimates of Burden of Antibacterial Resistance European Union Thailand United States population 500 m population 70 m population 300 m 25, 000 deaths per year >38, 000 deaths >23, 000 deaths 2. 5 m extra hospital days >3. 2 m hospital days >2. 0 m illnesses Overall societal costs (€ 900 million, hosp. days) Approx. € 1. 5 billion per year Overall societal costs US$ 84. 6– 202. 8 mill. direct >US$1. 3 billion indirect Overall societal costs Up to $20 billion direct Up to $35 billion indirect Source: ECDC 2007 Source: Pumart et al 2012 Source: US CDC 2013 Global information is insufficient to show complete disease burden impact and costs | Antimicrobial Resistance Global Report on Surveillance 2014

Summary: Antibacterial Resistance 1. High proportions of resistance were reported in all regions to common treatments for bacteria causing infections in both healthcare settings and in the community 2. Antibacterial resistance has a negative effect on patient outcomes and health expenditures 3. Treatment options for common infections are running out 4. Despite limitations, the report demonstrates worldwide magnitude of ABR and surveillance gaps | Antimicrobial Resistance Global Report on Surveillance 2014

Resolution on AMR World health Assembly May 2014. . . To develop a draft global action plan to combat AMR. . . to ensure that all countries. . . have the capacity to combat AMR. – Takes into account existing action plans and all available evidence and best practice – To apply a multisectoral approach by consulting. . . Submit to 2015 Health Assembly through the Executive Board January 2015 – November 2014 | Antimicrobial Resistance Global Report on Surveillance 2014

Consultation on draft GAP (1) Online consultation held between 4 July and 1 September 2014 – Open to Member States, organizations – 130 contributions received from all relevant sectors • Member States, Government agencies and organizations: 54 • NGOs and civil society: 40 • Private sector: 16 • Academia: 16 • Other (International organizations): 4 | Antimicrobial Resistance Global Report on Surveillance 2014

Consultation on draft GAP (2) Strengthen tripartite collaboration – FAO, OIE, WHO – Worked together on development of global action plan • Shared actions for the collaboration 16 October consultation with Member States – http: //www. who. int/drugresistance/memberstatemeeting/en/ 17 October 3 rd meeting of WHO Advisory Group Additional Member State consultations scheduled – Optimizing use of medicines (Oslo, November) – Global surveillance (Stockholm, December) | Antimicrobial Resistance Global Report on Surveillance 2014

Draft global action plan will be based on… 5 Guiding principles – Whole of society engagement – Prevention first – Access, not excess – Sustainability – Incremental targets for implementation | Antimicrobial Resistance Global Report on Surveillance 2014

Five strategic objectives: Improve awareness and understanding Strengthen the knowledge and evidence base Reduce the incidence of infection Optimize the use of antimicrobial medicines Develop the economic case for sustainable investment Commitments to report progress | Antimicrobial Resistance Global Report on Surveillance 2014

Communication, Awareness, Training ØPublic communication programmes ØProfessional education, training, certification ØSchools curricula ØPublic information and media ØRole for all stakeholders in promoting public understanding of infection prevention and use of antimicrobial medicines | Antimicrobial Resistance Global Report on Surveillance 2014

Strengthen the knowledge and evidence base ØCapacity to collect, analyse and report data Ø Global surveillance based on national capacity ØIntegration of data between human and animal sectors ØDevelop global public health research agenda Ø Implement (research funders to support) ØRepository of information Ø Global health R&D observatory | Antimicrobial Resistance Global Report on Surveillance 2014

Reduce the incidence of infection ØHygiene, infection prevention and control Ø Healthcare settings (hospitals) ØSanitation, water and food safety ØControl of STI, vector borne diseases Ø HIV, gonorrhoea, malaria ØRole of vaccines and immunization Ø Expand use of existing vaccines (e. g. pneumococcal) Ø Reduce prevalence of infection inappropriately treated with antibiotics (e. g. influenza, rotavirus) Ø New priority vaccines to prevent difficult-to-treat or untreatable infections ØAnimal husbandry Ø High density livestock (terrestrial and aquatic) | Antimicrobial Resistance Global Report on Surveillance 2014

Optimize use ØRegulatory mechanisms for new antibiotics ØEffective low-cost tools for diagnosis and susceptibility testing ØAccess to medicines accompanied by measures to protect continued efficacy ØCode of practice | Antimicrobial Resistance Global Report on Surveillance 2014

Sustainable investment ØEconomic case for investment ØRealizing the global investment needs Ø Developing countries ØCoordinating initiatives aimed at renewing investment in new antibiotics, diagnostics & other tools | Antimicrobial Resistance Global Report on Surveillance 2014

Implementing, monitoring and evaluation ØCountries should develop and implement national action plans Ø “building blocks” Ø National priorities, circumstances ØWHO will develop a framework for monitoring and evaluation Ø WHO to report every 2 years ØOthers to develop own action plans and report within normal reporting cycle | Antimicrobial Resistance Global Report on Surveillance 2014

Thank you | Antimicrobial Resistance Global Report on Surveillance 2014
- Slides: 28