GLIOBLASTOMA MULTIFORME GBM Rachel A Multz MS 4

GLIOBLASTOMA MULTIFORME (GBM) Rachel A. Multz, MS 4 Bindu Setty, MD MRI

CASE HISTORY A 65 year old female with no relevant past medical history presents to an outside hospital with expressive aphasia, repetitive statements, and repeatedly writing the same word. She was sent to BMC for further workup of a mass seen on CT.
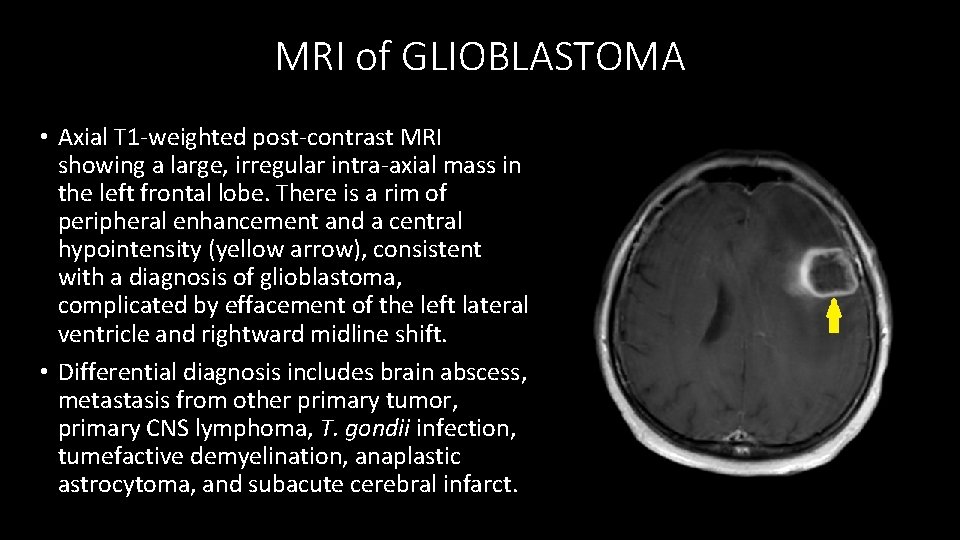
MRI of GLIOBLASTOMA • Axial T 1 -weighted post-contrast MRI showing a large, irregular intra-axial mass in the left frontal lobe. There is a rim of peripheral enhancement and a central hypointensity (yellow arrow), consistent with a diagnosis of glioblastoma, complicated by effacement of the left lateral ventricle and rightward midline shift. • Differential diagnosis includes brain abscess, metastasis from other primary tumor, primary CNS lymphoma, T. gondii infection, tumefactive demyelination, anaplastic astrocytoma, and subacute cerebral infarct.

MRI of GLIOBLASTOMA • Axial FLAIR MRI showing a large, irregular intra-axial mass in the left frontal lobe (yellow arrow), consistent with a diagnosis of glioblastoma, complicated by a large area of surrounding vasogenic edema (red arrow), effacement of the left lateral ventricle, and rightward midline shift. • Differential diagnosis includes brain abscess, metastasis from other primary tumor, primary CNS lymphoma, T. gondii infection, tumefactive demyelination, anaplastic astrocytoma, and subacute cerebral infarct.

CLINICAL FOLLOW UP The following day, the patient underwent craniotomy with resection of the tumor. Pathology showed the mass to be glioblastoma, IDH-wildtype, WHO Grade IV with partial methylation of the MGMT promoter region. She subsequently underwent treatment with radiation and temozolomide, complicated by severe neutropenia and thrombocytopenia.

• General Characteristics IN A NUTSHELL • Mass with thick, irregular ring enhancing border with central necrosis • Mass effect (ventricular effacement, cistern effacement) with surrounding vasogenic edema • Typically found in frontal, temporal, or parietal lobe (supratentorial) • Other Associated Findings • Crosses corpus callosum (“butterfly glioma”) • Hemorrhagic component due to high vascularity of tumor • Potential Complications • • Midline shift Increased intracranial pressure Herniation (uncal, subfalcine, tonsillar) Rarely, can invade meninges or be multifocal • Remember • Tumor cells infiltrate far beyond the abnormalities visible on imaging • MR more sensitive than CT

VOICE RAD: MRI OF GLIOBLASTOMA BY DR. SETTY (2020)
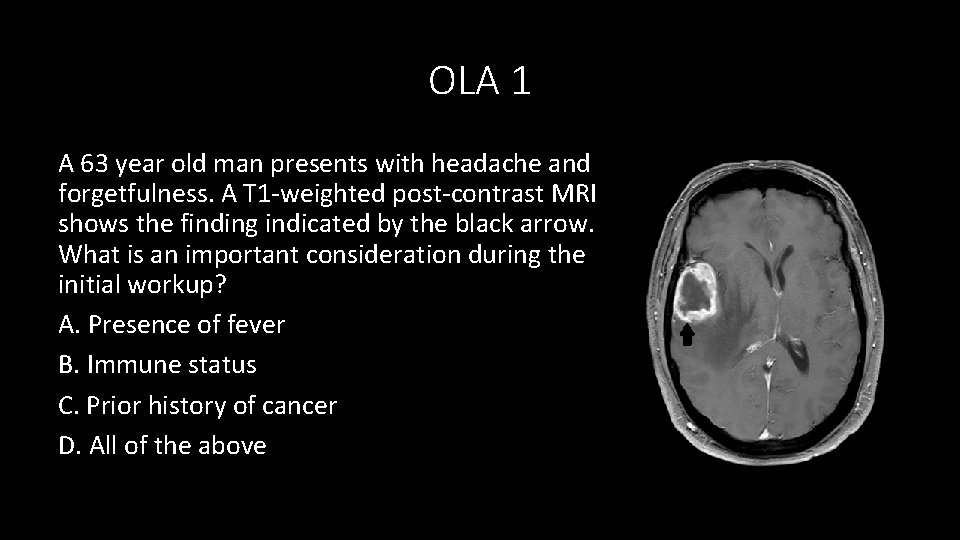
OLA 1 A 63 year old man presents with headache and forgetfulness. A T 1 -weighted post-contrast MRI shows the finding indicated by the black arrow. What is an important consideration during the initial workup? A. Presence of fever B. Immune status C. Prior history of cancer D. All of the above

IMAGING SPECTRUM of GLIOBLASTOMA “Butterfly Glioma” • Image: Axial T 1 -weighted post-contrast image of a 52 year old female showing a large, irregular mass in the left frontal lobe that crosses the midline involving the genu of the corpus callosum (yellow arrow). There is a rim of peripheral enhancement and a central hypointensity, consistent with a diagnosis of glioblastoma, complicated by ventricular effacement and midline shift.
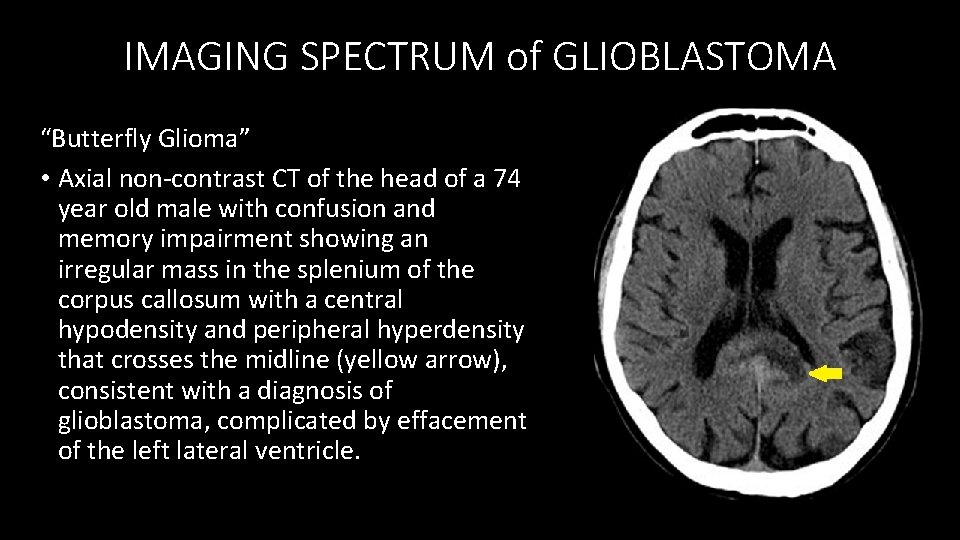
IMAGING SPECTRUM of GLIOBLASTOMA “Butterfly Glioma” • Axial non-contrast CT of the head of a 74 year old male with confusion and memory impairment showing an irregular mass in the splenium of the corpus callosum with a central hypodensity and peripheral hyperdensity that crosses the midline (yellow arrow), consistent with a diagnosis of glioblastoma, complicated by effacement of the left lateral ventricle.

IMAGING SPECTRUM of GLIOBLASTOMA “Butterfly Glioma” • Image: Sagittal T 1 -weighted post-contrast image of a 74 year old male with confusion and memory impairment showing an irregular mass in the splenium of the corpus callosum with peripheral hyperintensity (yellow arrow) consistent with a diagnosis of glioblastoma.

IMAGING SPECTRUM of GLIOBLASTOMA “Butterfly Glioma” • Image: Axial FLAIR image of a 74 year old male with confusion and memory impairment showing an irregular hyperintense mass in the splenium of the corpus callosum that crosses the midline (yellow arrow), consistent with a diagnosis of glioblastoma, complicated by effacement of the left lateral ventricle.
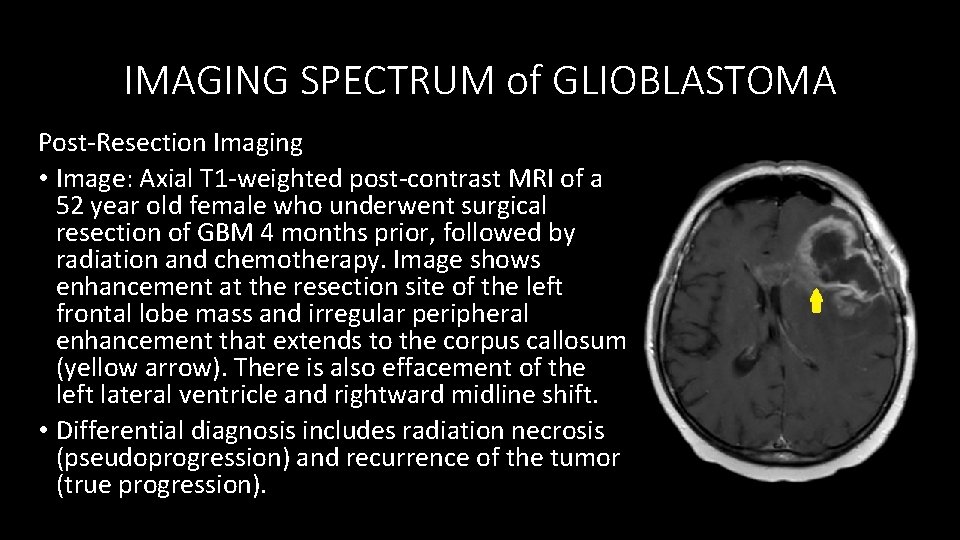
IMAGING SPECTRUM of GLIOBLASTOMA Post-Resection Imaging • Image: Axial T 1 -weighted post-contrast MRI of a 52 year old female who underwent surgical resection of GBM 4 months prior, followed by radiation and chemotherapy. Image shows enhancement at the resection site of the left frontal lobe mass and irregular peripheral enhancement that extends to the corpus callosum (yellow arrow). There is also effacement of the left lateral ventricle and rightward midline shift. • Differential diagnosis includes radiation necrosis (pseudoprogression) and recurrence of the tumor (true progression).
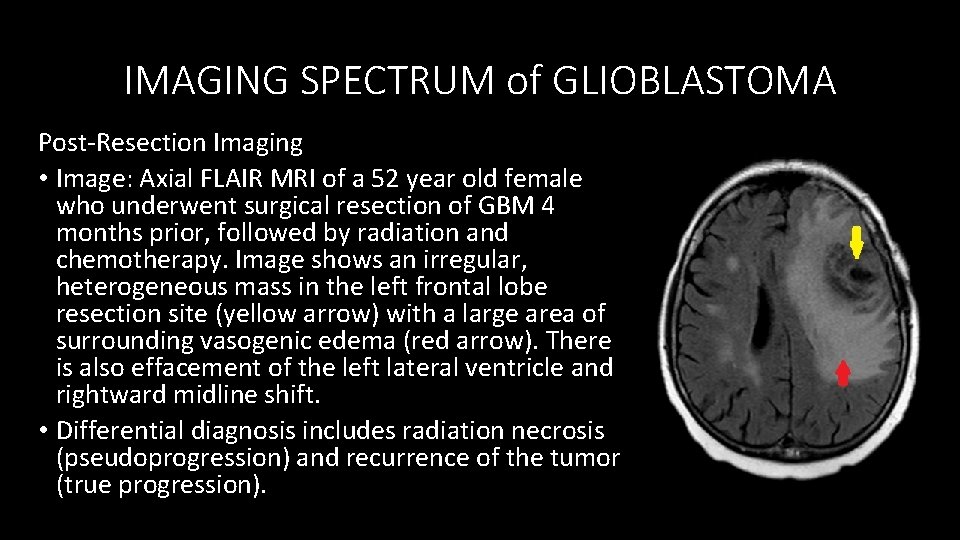
IMAGING SPECTRUM of GLIOBLASTOMA Post-Resection Imaging • Image: Axial FLAIR MRI of a 52 year old female who underwent surgical resection of GBM 4 months prior, followed by radiation and chemotherapy. Image shows an irregular, heterogeneous mass in the left frontal lobe resection site (yellow arrow) with a large area of surrounding vasogenic edema (red arrow). There is also effacement of the left lateral ventricle and rightward midline shift. • Differential diagnosis includes radiation necrosis (pseudoprogression) and recurrence of the tumor (true progression).
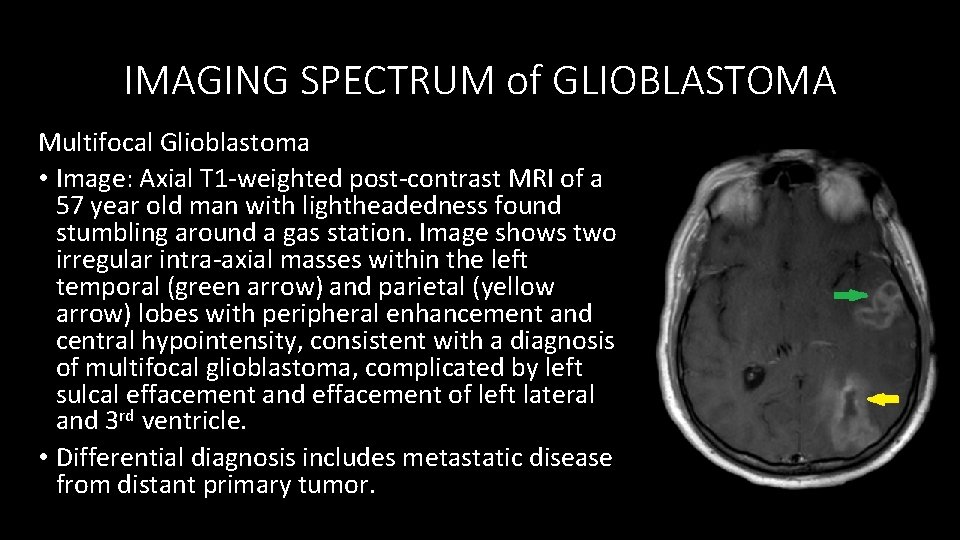
IMAGING SPECTRUM of GLIOBLASTOMA Multifocal Glioblastoma • Image: Axial T 1 -weighted post-contrast MRI of a 57 year old man with lightheadedness found stumbling around a gas station. Image shows two irregular intra-axial masses within the left temporal (green arrow) and parietal (yellow arrow) lobes with peripheral enhancement and central hypointensity, consistent with a diagnosis of multifocal glioblastoma, complicated by left sulcal effacement and effacement of left lateral and 3 rd ventricle. • Differential diagnosis includes metastatic disease from distant primary tumor.
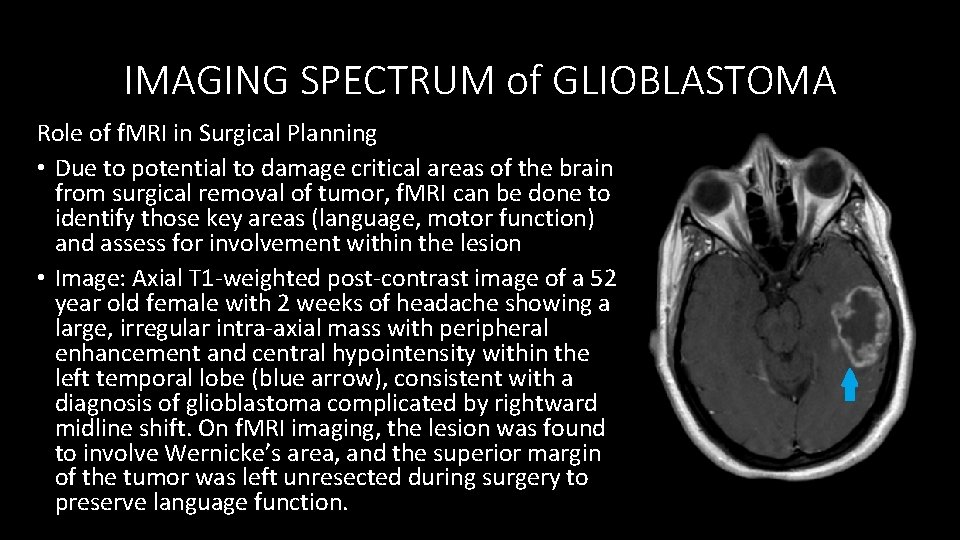
IMAGING SPECTRUM of GLIOBLASTOMA Role of f. MRI in Surgical Planning • Due to potential to damage critical areas of the brain from surgical removal of tumor, f. MRI can be done to identify those key areas (language, motor function) and assess for involvement within the lesion • Image: Axial T 1 -weighted post-contrast image of a 52 year old female with 2 weeks of headache showing a large, irregular intra-axial mass with peripheral enhancement and central hypointensity within the left temporal lobe (blue arrow), consistent with a diagnosis of glioblastoma complicated by rightward midline shift. On f. MRI imaging, the lesion was found to involve Wernicke’s area, and the superior margin of the tumor was left unresected during surgery to preserve language function.

DISCUSSION • Most common adult primary brain tumor, derived from astrocytes • Typically diagnosed after 40, though peaks between 65 and 75 • Slight male predominance (3: 2 M: F) • No “typical” presentation, varies with size and location of tumor • Most commonly seizures, focal neurologic deficit • Can see symptoms of increase intracranial pressure (papilledema, headache that is worse in the morning or worsens with valsalva/bending over, nausea/vomiting) • Highly aggressive tumor (WHO Grade IV) • Median survival typically ~1 year • Even with surgical debulking, recurrence almost inevitable due to diffuse infiltration and microinvasion of tumor cells • Debulking can be followed by radiation and/or chemotherapy (temozolomide)

DISCUSSION Classification of Glioblastoma • Glioblastomas are broadly classified into IDH-1 wildtype (R 132 H-) or IDH-1 mutant (R 132 H+) • Primary (de novo) GBM are typically IDH-wildtype, arise in older individuals, and carry a worse prognosis. ~90% of cases. • Secondary GBM typically are IDH-mutant, arise in younger individuals from a lower grade astrocytoma, and carry a better prognosis. ~10% of cases. • Another important molecular marker in GBM is MGMT methylation, whose presence has shown to be an independent favorable prognostic factor in patients with GBM. There has been demonstrated survival benefit in GBM patients with MGMT methylation who are treated with radiation and temozolomide.
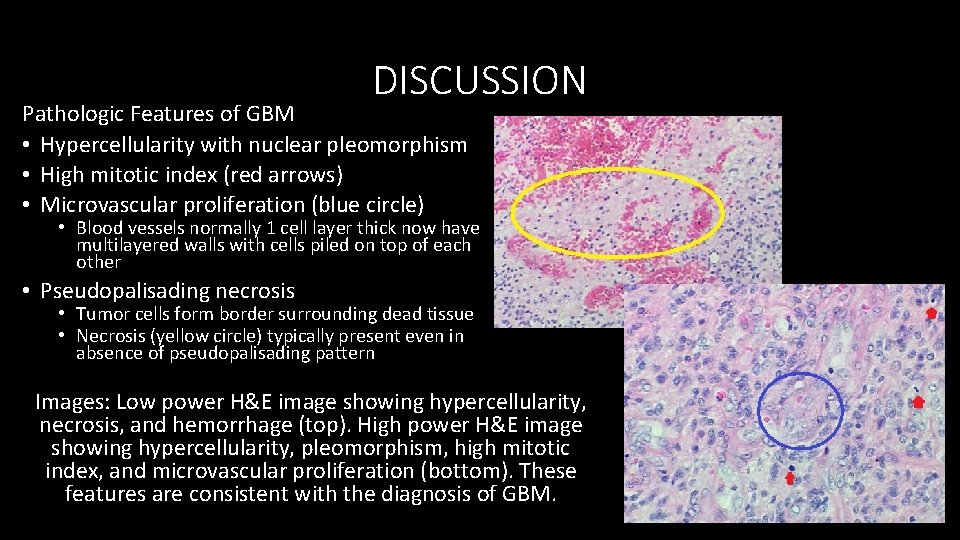
DISCUSSION Pathologic Features of GBM • Hypercellularity with nuclear pleomorphism • High mitotic index (red arrows) • Microvascular proliferation (blue circle) • Blood vessels normally 1 cell layer thick now have multilayered walls with cells piled on top of each other • Pseudopalisading necrosis • Tumor cells form border surrounding dead tissue • Necrosis (yellow circle) typically present even in absence of pseudopalisading pattern Images: Low power H&E image showing hypercellularity, necrosis, and hemorrhage (top). High power H&E image showing hypercellularity, pleomorphism, high mitotic index, and microvascular proliferation (bottom). These features are consistent with the diagnosis of GBM.

LINKS AND REFERENCES • Consistent References: • https: //radiopaedia. org/articles/glioblastoma? lang=us • https: //brain. thecommonvein. net/glioblastoma/ • https: //braintumor. org/wp-content/assets/WHO-Central-Nervous-System. Tumor-Classification. pdf • Other Journals and Texts • Osborn AG. Handbook of Neuroradiology. Mosby Inc. (1991) ISBN: 0815165781. • Osborn AG et al. Diagnostic Imaging: Brain. Amirsys Inc. (2004) ISBN: 0721629059. • OLAS
- Slides: 20