GLANDULAR EPITHELIUM This type of epithelium is formed




- Slides: 14

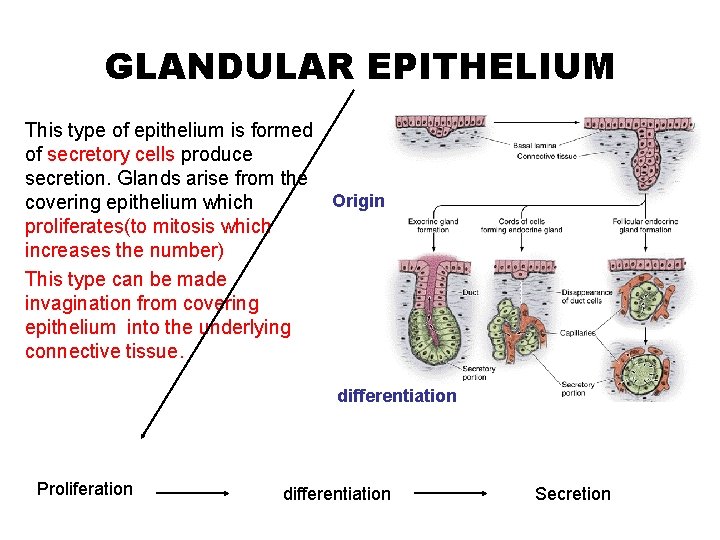
GLANDULAR EPITHELIUM This type of epithelium is formed of secretory cells produce secretion. Glands arise from the Origin covering epithelium which proliferates(to mitosis which increases the number) This type can be made invagination from covering epithelium into the underlying connective tissue. differentiation Proliferation differentiation Secretion

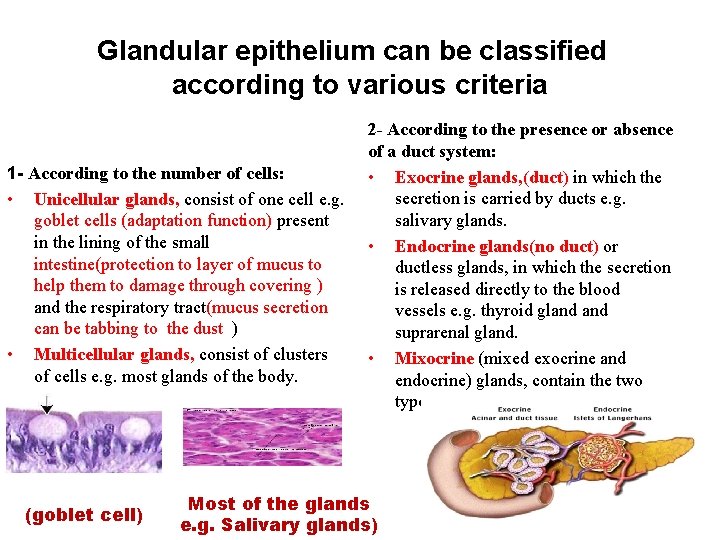
Glandular epithelium can be classified according to various criteria 1 - According to the number of cells: • Unicellular glands, consist of one cell e. g. goblet cells (adaptation function) present in the lining of the small intestine(protection to layer of mucus to help them to damage through covering ) and the respiratory tract(mucus secretion can be tabbing to the dust ) • Multicellular glands, consist of clusters of cells e. g. most glands of the body. (goblet cell) 2 - According to the presence or absence of a duct system: • Exocrine glands, (duct) in which the secretion is carried by ducts e. g. salivary glands. • Endocrine glands(no duct) or ductless glands, in which the secretion is released directly to the blood vessels e. g. thyroid gland suprarenal gland. • Mixocrine (mixed exocrine and endocrine) glands, contain the two types e. g. pancreas. Most of the glands e. g. Salivary glands)

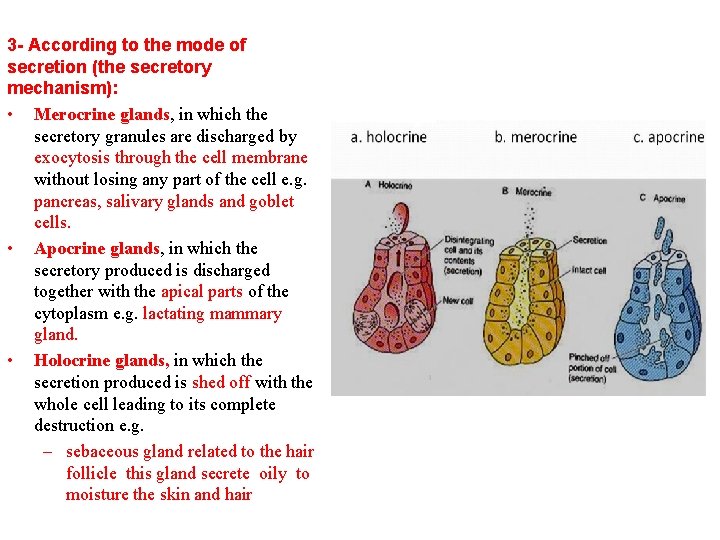
3 - According to the mode of secretion (the secretory mechanism): • Merocrine glands, in which the secretory granules are discharged by exocytosis through the cell membrane without losing any part of the cell e. g. pancreas, salivary glands and goblet cells. • Apocrine glands, in which the secretory produced is discharged together with the apical parts of the cytoplasm e. g. lactating mammary gland. • Holocrine glands, in which the secretion produced is shed off with the whole cell leading to its complete destruction e. g. – sebaceous gland related to the hair follicle this gland secrete oily to moisture the skin and hair

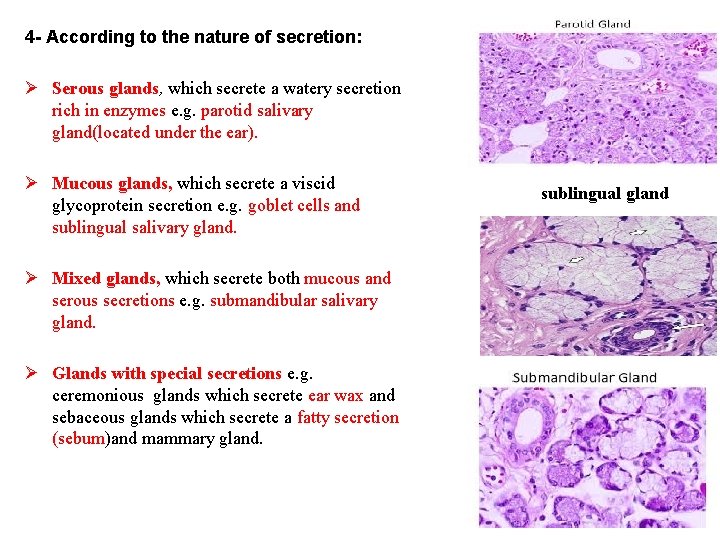
4 - According to the nature of secretion: Ø Serous glands, which secrete a watery secretion rich in enzymes e. g. parotid salivary gland(located under the ear). Ø Mucous glands, which secrete a viscid glycoprotein secretion e. g. goblet cells and sublingual salivary gland. Ø Mixed glands, which secrete both mucous and serous secretions e. g. submandibular salivary gland. Ø Glands with special secretions e. g. ceremonious glands which secrete ear wax and sebaceous glands which secrete a fatty secretion (sebum)and mammary gland. sublingual gland

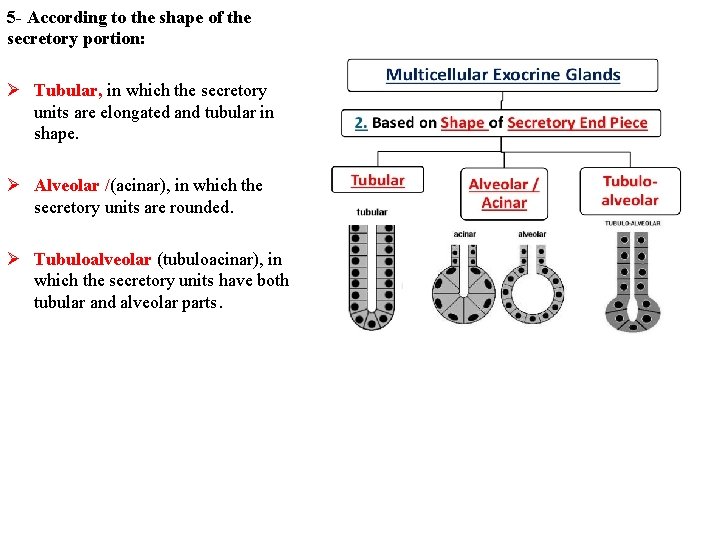
5 - According to the shape of the secretory portion: Ø Tubular, in which the secretory units are elongated and tubular in shape. Ø Alveolar /(acinar), in which the secretory units are rounded. Ø Tubuloalveolar (tubuloacinar), in which the secretory units have both tubular and alveolar parts.

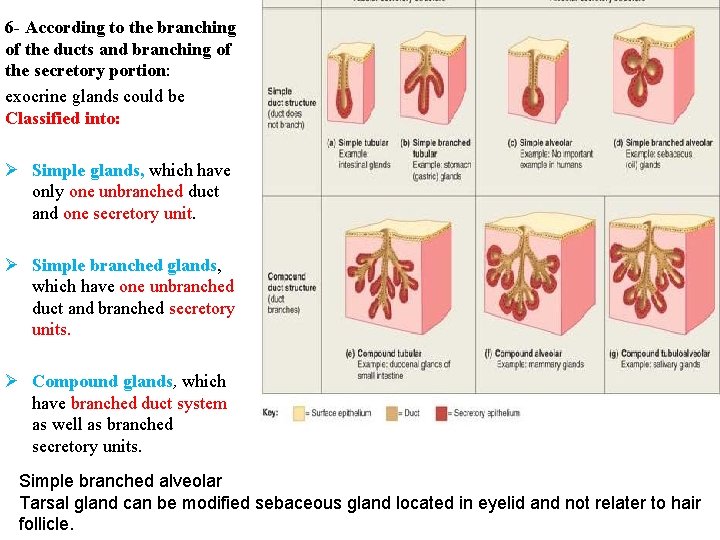
6 - According to the branching of the ducts and branching of the secretory portion: exocrine glands could be Classified into: Ø Simple glands, which have only one unbranched duct and one secretory unit. Ø Simple branched glands, which have one unbranched duct and branched secretory units. Ø Compound glands, which have branched duct system as well as branched secretory units. Simple branched alveolar Tarsal gland can be modified sebaceous gland located in eyelid and not relater to hair follicle.

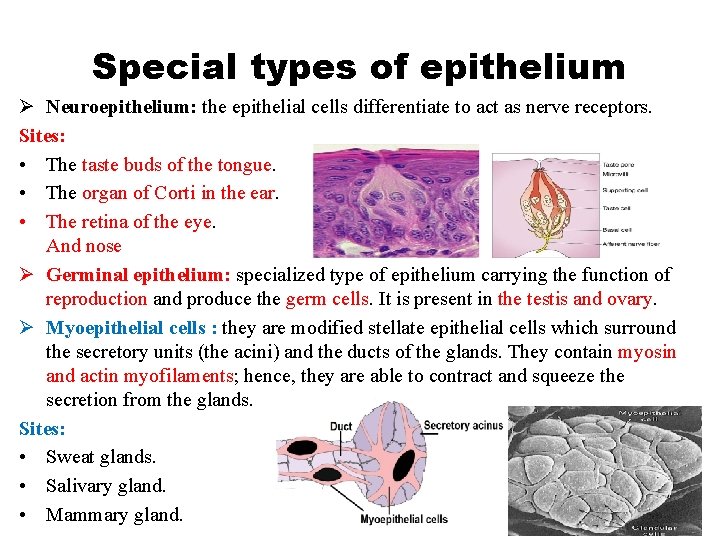
Special types of epithelium Ø Neuroepithelium: the epithelial cells differentiate to act as nerve receptors. Sites: • The taste buds of the tongue. • The organ of Corti in the ear. • The retina of the eye. And nose Ø Germinal epithelium: specialized type of epithelium carrying the function of reproduction and produce the germ cells. It is present in the testis and ovary. Ø Myoepithelial cells : they are modified stellate epithelial cells which surround the secretory units (the acini) and the ducts of the glands. They contain myosin and actin myofilaments; hence, they are able to contract and squeeze the secretion from the glands. Sites: • Sweat glands. • Salivary gland. • Mammary gland.

Functions of epithelium: • The most important function of covering epithelial membranes is the protection(stratified (keratinized)is special type of protection) against injuries, bacteria, chemicals and water. • Secretion by glandular epithelium. • Absorption by epithelial lining of the small intestine and renal tubules. • Filtration by epithelial lining of certain parts in kidney to facilitate urine formation and in lung for gas diffusion. • Reproduction by germinal epithelium of testis and ovary that are specialized in producing sperms and ova respectively. • Contraction by the myoepithelial cells. • Receptor function by the neuroepithelium specialized in perception of special senses stimuli.

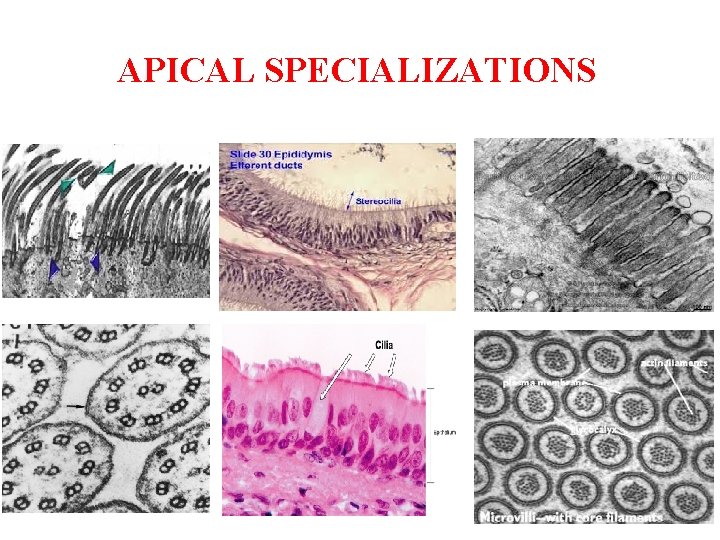
EPITHELIAL POLARITY(modification of adopt function) (CELL SURFACE SPECIALIZATION) The epithelial cell has an apical, basal and lateral surfaces; meaning that cell regions near each surface exhibit special structural modifications to carry out specific functions. APICAL SPECIALIZATIONS The apical surface of the epithelial cell is the upper free surface exposed to the body exterior or the cavity of an internal organ. The structural modifications in the apical domain include Microvilli(short/nonmotile /numerous of number) : these are non-motile cytoplasmic projections which arise from the apical surface of most of epithelial cells as finger-like evaginations; they contain a core of actin filaments. Ø Function: they increase the surface area for fluid absorption. They are present mainly in the absorptive columnar cells of the intestine and kidney tubules. Ø Cilia(long/motile) are generally-motile cytoplasmic projections that extend from the cell surface. Cilia are hair-like processes that are longer than microvilli. Ø Stereocilia(long/nonmotile) are long, branching microvilli found mainly in the non ciliated pseudostartified columnar epithelium of the male genital ducts e. g. the epididymis. They increase the surface area for fluid absorption. Ø Note*the responsible to make the cilia is centriole because it have micro tubules.

APICAL SPECIALIZATIONS

Clinical hint: Abnormal proteins of cilia or flagella resulting from mutation are responsible for the immotile cilia syndrome(genetic defect in protein and flagella ). The symptoms are: Male infertility due to immotile spermatozoa. Chronic respiratory infection caused by lack of cleaning action of cilia in the ciliated pseudostratified columnar epithelium of respiratory tract. BASAL SPECIALIZATIONS The structural modifications in the basal domain include v flagella: Flagella resemble cilia in structure but they are much longer and are single per cell e. g. flagellum of the spermatozoon. v basal infoldings v the basement membrane v cell-to-matrix junction. Ø Basal infoldings: the basal cell membrane is thrown into folds. This aims to increase the surface area where ions transport occurs as in kidney tubules

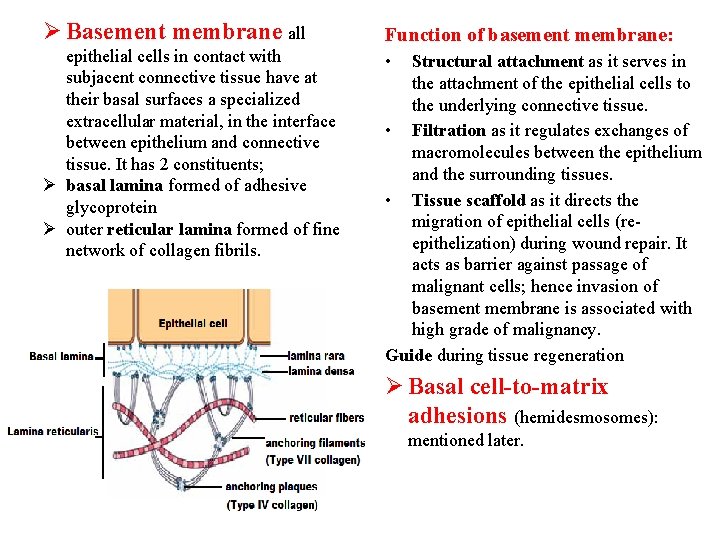
Ø Basement membrane all Function of basement membrane: epithelial cells in contact with subjacent connective tissue have at their basal surfaces a specialized extracellular material, in the interface between epithelium and connective tissue. It has 2 constituents; Ø basal lamina formed of adhesive glycoprotein Ø outer reticular lamina formed of fine network of collagen fibrils. • Structural attachment as it serves in the attachment of the epithelial cells to the underlying connective tissue. • Filtration as it regulates exchanges of macromolecules between the epithelium and the surrounding tissues. • Tissue scaffold as it directs the migration of epithelial cells (reepithelization) during wound repair. It acts as barrier against passage of malignant cells; hence invasion of basement membrane is associated with high grade of malignancy. Guide during tissue regeneration Ø Basal cell-to-matrix adhesions (hemidesmosomes): mentioned later.

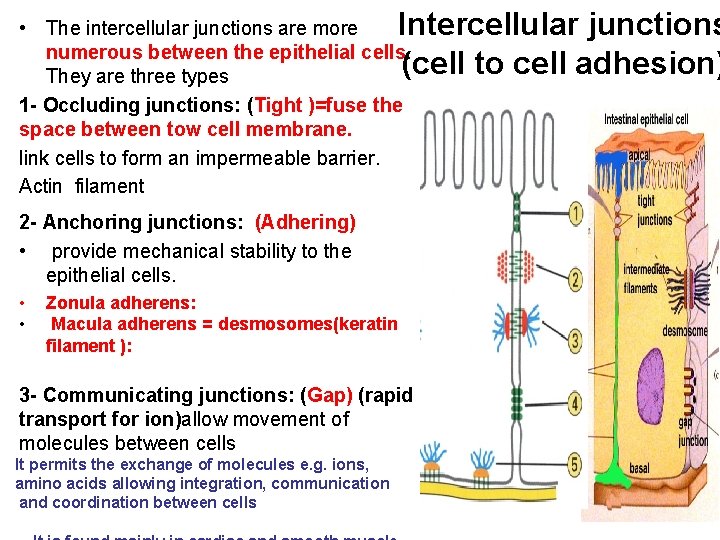
• The intercellular junctions are more Intercellular junctions numerous between the epithelial cells. (cell to cell adhesion) They are three types 1 - Occluding junctions: (Tight )=fuse the space between tow cell membrane. link cells to form an impermeable barrier. Actin filament 2 - Anchoring junctions: (Adhering) • provide mechanical stability to the epithelial cells. • • Zonula adherens: Macula adherens = desmosomes(keratin filament ): 3 - Communicating junctions: (Gap) (rapid transport for ion)allow movement of molecules between cells It permits the exchange of molecules e. g. ions, amino acids allowing integration, communication and coordination between cells
