GI Grand Rounds Johanna Chan PGY5 Fellow Baylor

GI Grand Rounds Johanna Chan, PGY-5 Fellow Baylor College of Medicine 2/13/2014 Mentor: Dr. Waqar Qureshi With thanks to Dr. Rise Stribling and Dr. Norman Sussman

No conflicts of interest No financial disclosures

HPI • Reason for consult: abnormal liver function tests • 26 yo G 2 P 1001 healthy woman at 32 w 0 d gestation with quadriamniotic quadruplets • Conceived with clomifene • Uncomplicated pregnancy, routine prenatal care • Presented to obstetrics clinic at 32 wks GA with bilateral leg swelling, malaise, nausea, and poor oral intake x 4 -5 days • After labs, admitted directly from clinic to PFW

Allergies: NKDA – No known prior liver Soc. Hx disease PMHx – Gestational DM 2 (1 st pregnancy) – Uncomplicated SVD 2009 at 40 w 2 d Medications: MVI PSHx: Cerclage, 16 weeks Fam. Hx – Mother: DM 2 – Father: HTN – No liver disease or autoimmune disease – Never Et. OH – No prior IVDA, nasal cocaine, blood transfusions, tattoos – Never smoker – Stay-at-home mother – No recent travel, antibiotics, unusual food exposures

Physical Exam T 98. 6, BP 116/56, HR 112, RR 12, O 2 sat 98% RA Gen: NAD, AAOx 4, fatigued-appearing, jaundiced HEENT: +scleral icterus, PERRL, EOMI, MMM, OP clear CV: RRR no m/r/g Chest: CTAB no wheezes, slight crackles at bases Abd: soft, nontender, NABS, +gravid uterus Ext: WWP, no clubbing or cyanosis, +generalized swelling of BLE without pitting Neuro: oriented x 4, fatigued, conversational

Labs on admission 128 104 21 5. 4 14 2. 61 63 13. 3 7. 84 38. 5 79% PMNs Total prot 5. 8 Albumin 2. 6 Total bili 6. 3 Direct bili 5. 1 Alk phos 394 GGT 49 ALT 351 AST 504 7. 31/24/144 Lactate 5. 1 138 MCV 96 INR 2. 2 PTT 58. 4 D-dimer >20 Fibrinogen 60 LDH 1575 Haptoglobin 63

Additional labs Hepatitis A Ab (−) Hepatitis B s. Ab (+) Hepatitis B s. Ag (−) Hepatitis C Ab (−) HCV RNA (−) U/A: dark yellow, cloudy, 1+ bilirubin, trace blood, 2+ protein, neg nitrite, neg leuk Blood cultures (−) Urine culture (−)

Imaging • CXR normal • RUQ U/S on admission – Liver 13. 7 cm, normal in morphology and echotexture, no focal mass – Gallbladder contracted, 4 mm wall – CBD 6 mm – Portal vein diameter 14 mm – Ascites: none

Clinical course • Immediate C-section • No unusual degree of blood loss • GI evaluation immediately post-op: intubated/sedated on fentanyl but following commands, no bleeding
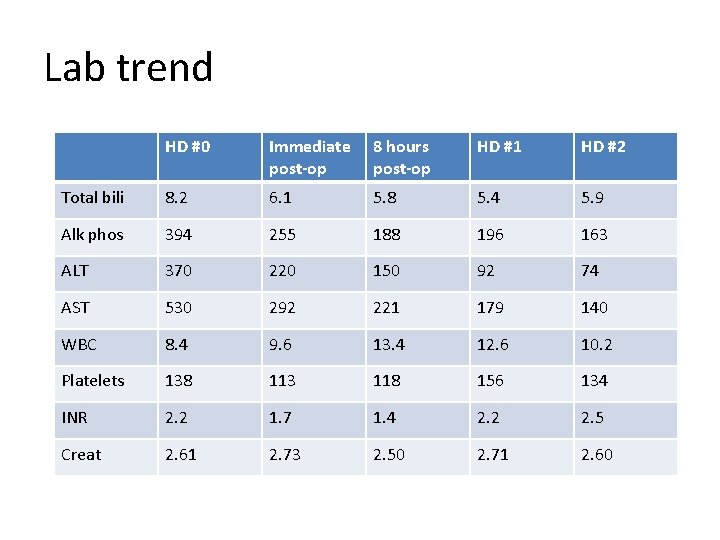
Lab trend HD #0 Immediate post-op 8 hours post-op HD #1 HD #2 Total bili 8. 2 6. 1 5. 8 5. 4 5. 9 Alk phos 394 255 188 196 163 ALT 370 220 150 92 74 AST 530 292 221 179 140 WBC 8. 4 9. 6 13. 4 12. 6 10. 2 Platelets 138 113 118 156 134 INR 2. 2 1. 7 1. 4 2. 2 2. 5 Creat 2. 61 2. 73 2. 50 2. 71 2. 60

Clinical course • Hospital day #1 – Extubated – Fever 101. 5 – “Lethargic, but arousable” after holding sedation x 7 hours, follows commands but seems confused – No asterixis, but ammonia 76 • Hospital day #2: – Obvious further decline in mentation, no longer following commands, nonverbal – Transferred to Houston area hospital

Acute fatty liver of pregnancy (AFLP)

Clinical questions • What are clinical and pathophysiologic characteristics of AFLP? • How can we distinguish clinically from HELLP? • What are prognostic indicators and outcomes of AFLP?
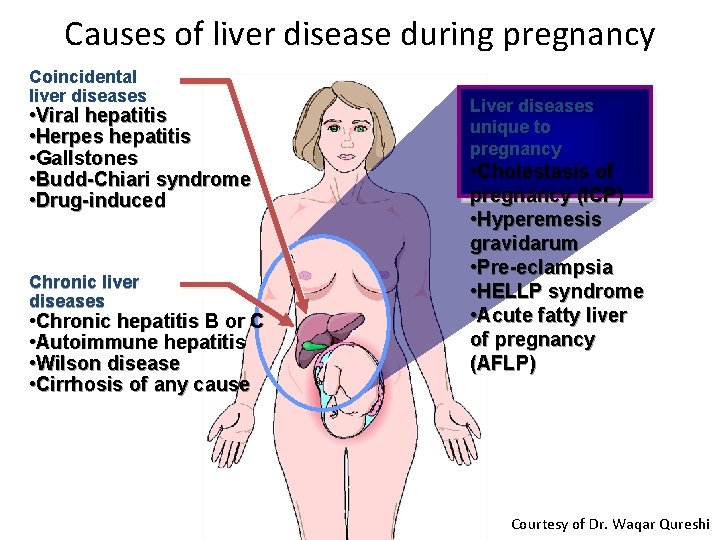
Causes of liver disease during pregnancy Coincidental liver diseases • Viral hepatitis • Herpes hepatitis • Gallstones • Budd-Chiari syndrome • Drug-induced Chronic liver diseases • Chronic hepatitis B or C • Autoimmune hepatitis • Wilson disease • Cirrhosis of any cause Liver diseases unique to pregnancy • Cholestasis of pregnancy (ICP) • Hyperemesis gravidarum • Pre-eclampsia • HELLP syndrome • Acute fatty liver of pregnancy (AFLP) Courtesy of Dr. Waqar Qureshi

Clinical questions • What are clinical and pathophysiologic characteristics of AFLP? • How can we distinguish clinically from HELLP? • What are prognostic indicators and outcomes of AFLP?

AFLP: Clinical presentation • 1 in 7, 000 to 1 in 16, 000 pregnancies (retrospective) • UK-based prospective study (UKOSS), 229 centers: 57 confirmed cases in 1, 132, 964 pregnancies • Third trimester • 40 -50% nulliparous • Increased incidence in twin pregnancies or multiple pregnancies Hay, J. Hepatology. 2008; 47(3): 1067 -76. Kaplan MM. N Engl J Med 1985; 313: 367 -70. Knight M et al. Gut 2008; 57: 951 -56. Steingrub JS. Crit Care Clin 2004; 20: 763 -776.

AFLP: Clinical presentation • 1934: Stander and Cadden, “acute yellow atrophy of the liver” • 1 -2 weeks: anorexia, N/V, RUQ pain • Ill-appearing: jaundice, edema, ascites, +/- encephalopathy • Liver dysfunction: hypofibrinogenemia, hypoalbuminemia, coagulopathy • Renal failure and hyperuricemia common • 50% have pre-eclampsia, and symptoms/labs may mimic HELLP Stander H, Cadden B. Am J Obstet Gynecol 1934; 28: 61 -69. Steingrub JS. Crit Care Clin 2004; 20: 763 -776.

AFLP: Swansea diagnostic criteria (Six or more in the absence of other explanation) • Vomiting • Abdominal pain • Polydipsia/polyuria • Encephalopathy • High bilirubin > 15 micromol/L • Hypoglycemia < 4 mmol/L • High uric acid > 340 micromol/L • Leukocytosis > 11 x 106/L • Ascites or bright liver on ultrasound • High AST/ALT > 42 micromol/L • High ammonia > 47 micromol/L • Renal impairment with creatinine > 150 micromol/L • Coagulopathy PT > 14 sec • Microvesicular steatosis on liver biopsy Ch’ng CL et al. Gut 2002; 51(6): 876 -80. Goel A et al. Gut 2011; 60(1): 138 -9.

AFLP: Clinical complications • Early complications of AFLP – Acute renal failure – Acute pancreatitis – Hypoglycemia – Infection – Hepatic encephalopathy • Late complications – Cerebral edema, seizures – Coagulopathy, GI hemorrhage – Hepatic failure

AFLP: Pathophysiology • Fetal long-chain 3 -hydroxyacyl coenzyme A dehydrogenase (LCHAD) deficiency • LCFA accumulate in mother incorporate in TGs within hepatocytes • Microvesicular fat deposition, zone 3 • Histologically and clinically similar to Reye’s syndrome and Jamaican Vomiting Sickness (both diseases of microvesicular fatty infiltration) Hay, J. Hepatology. 2008; 47(3): 1067 -76. Joshi D et al. Lancet. 2010; 375(9714): 594 -605. Steingrub JS. Crit Care Clin 2004; 20: 763 -776.
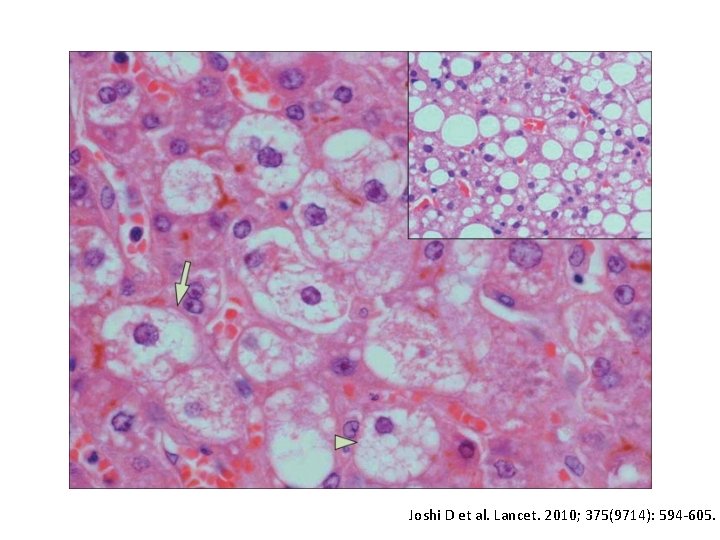
Joshi D et al. Lancet. 2010; 375(9714): 594 -605.

Clinical questions • What are clinical and pathophysiologic characteristics of AFLP? • How can we distinguish clinically from HELLP? • What are prognostic indicators and outcomes of AFLP?

HELLP • First described in 1982 by Weinstein • 1 in 1, 000 to 6 in 1, 000 pregnancies • Second or third trimester, postpartum possible • Risk factors: advanced maternal age, multiparity, and white ethnicity • “Pro-inflammatory and pro-coagulant” state: alterations in platelet and cytokine activation, segmental vasospasm, vascular endothelial damage Hepburn IS. Dig Dis Sci. 2008; 53: 2334 -2358. Than NN and Neuberger J. Best Pract Res Clin Gastroenterol. 2013; 27(4): 565 -75. Weinstein L. Am J Obstet Gynecol 1983; 142: 159 -67.

HELLP: Clinical presentation • Hemolysis (microangiopathic hemolytic anemia), Elevated Liver enzymes, and Low Platelets • RUQ pain, N/V, malaise, and peripheral edema • Hemolysis unconjugated bilirubin and LDH elevations • Intravascular fibrin deposition, vasoconstriction of hepatic vascular bed, and increased sinusoidal pressure mild-moderate ALT/AST increase, mild bilirubin elevation Hepburn IS. Dig Dis Sci. 2008; 53: 2334 -2358. Than NN and Neuberger J. Best Pract Res Clin Gastroenterol. 2013; 27(4): 565 -75. Steingrub JS. Crit Care Clin 2004; 20: 763 -776.

HELLP: Clinical presentation • 5 -15% of pre-eclampsia cases develop HELLP • 70 -80% of HELLP cases co-exist with preeclampsia • Most frequent complication is DIC (30%) • Other complications: – abruptio placentae (16%) – acute renal failure (7%) – eclampsia – pulmonary edema/ARDS, severe ascites – hepatic infarction, subcapsular hematoma or hepatic Hay, J. Hepatology. 2008; 47(3): 1067 -76. rupture Hepburn IS. Dig Dis Sci. 2008; 53: 2334 -2358. Joshi D et al. Lancet. 2010; 375(9714): 594 -605. Steingrub JS. Crit Care Clin 2004; 20: 763 -776.
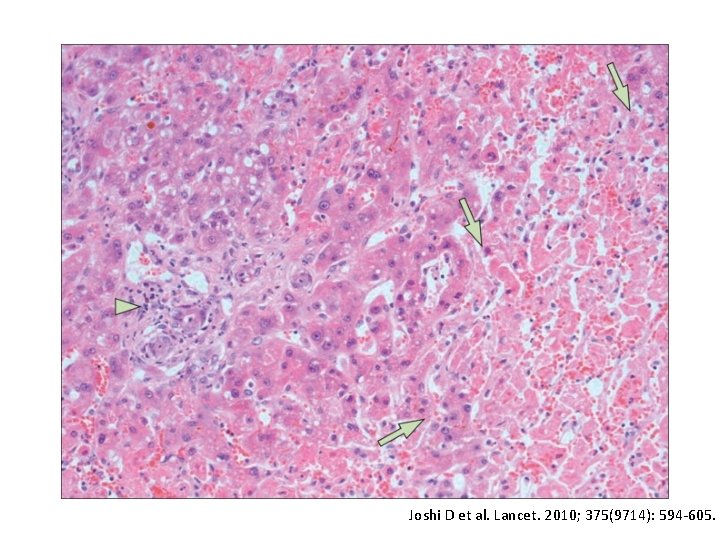
Joshi D et al. Lancet. 2010; 375(9714): 594 -605.

AFLP vs. HELLP
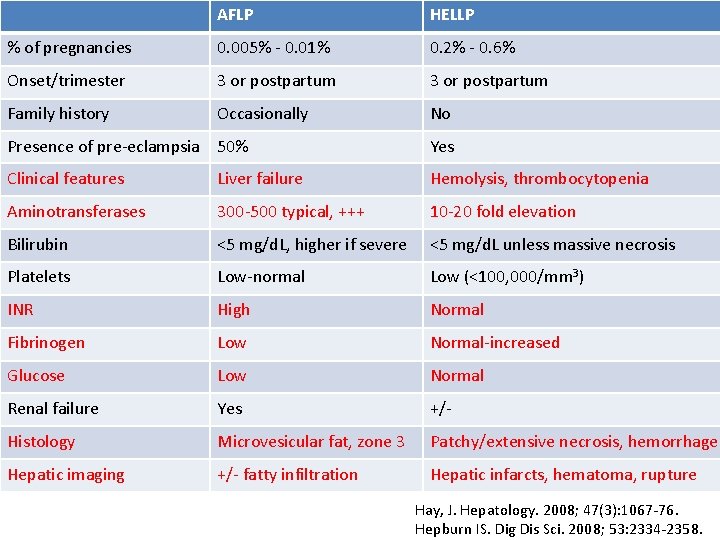
AFLP HELLP % of pregnancies 0. 005% - 0. 01% 0. 2% - 0. 6% Onset/trimester 3 or postpartum Family history Occasionally No Presence of pre-eclampsia 50% Yes Clinical features Liver failure Hemolysis, thrombocytopenia Aminotransferases 300 -500 typical, +++ 10 -20 fold elevation Bilirubin <5 mg/d. L, higher if severe <5 mg/d. L unless massive necrosis Platelets Low-normal Low (<100, 000/mm 3) INR High Normal Fibrinogen Low Normal-increased Glucose Low Normal Renal failure Yes +/- Histology Microvesicular fat, zone 3 Patchy/extensive necrosis, hemorrhage Hepatic imaging +/- fatty infiltration Hepatic infarcts, hematoma, rupture Hay, J. Hepatology. 2008; 47(3): 1067 -76. Hepburn IS. Dig Dis Sci. 2008; 53: 2334 -2358.

AFLP vs. HELLP • In comparison with HELLP… • AFLP patients more likely to have liver failure – coagulopathy, hypoglycemia, encephalopathy, DIC, and renal failure • DIC present in >75% of AFLP cases and only 20 -40% of HELLP cases • AFLP patients less likely to have thrombocytopenia Steingrub JS. Crit Care Clin 2004; 20: 763 -776.

AFLP vs. HELLP • DDx AFLP – HELLP – fulminant hepatic failure 2/2 acute viral hepatitis – drug toxicity • DDx HELLP – AFLP – acute viral hepatitis – gastroenteritis – appendicitis – cholecystitis – ITP – SLE – TTP/HUS

Clinical questions • What are clinical and pathophysiologic characteristics of AFLP? • How can we distinguish clinically from HELLP? • What are prognostic indicators and outcomes of AFLP?

AFLP Prognosis and Management • Hypoglycemia and PSE: poor prognostic sign • Estimated maternal mortality of around 10 -20% and a perinatal mortality of 20 -30% • Prompt delivery of fetus and supportive care • Limited case report/series data for plasmapheresis • Liver transplantation for ALF • Spontaneous survivors have no long-term sequelae; liver function normalizes 1 -4 weeks after delivery Hay, J. Hepatology. 2008; 47(3): 1067 -76. Jin F et al. Discovery Medicine. 2012(13): 369– 373, 2012. Steingrub JS. Crit Care Clin 2004; 20: 763 -776. Seyyed Majidi MR et al. Case Rep Obstet Gynecol. 2013; 615975.
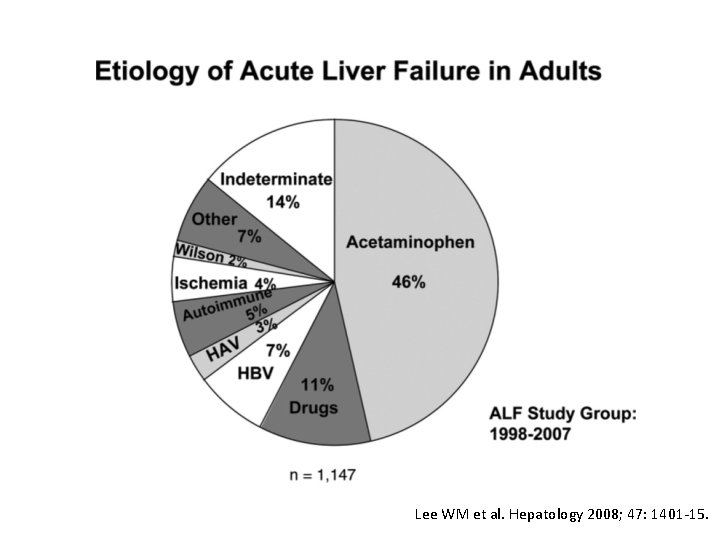
Lee WM et al. Hepatology 2008; 47: 1401 -15.
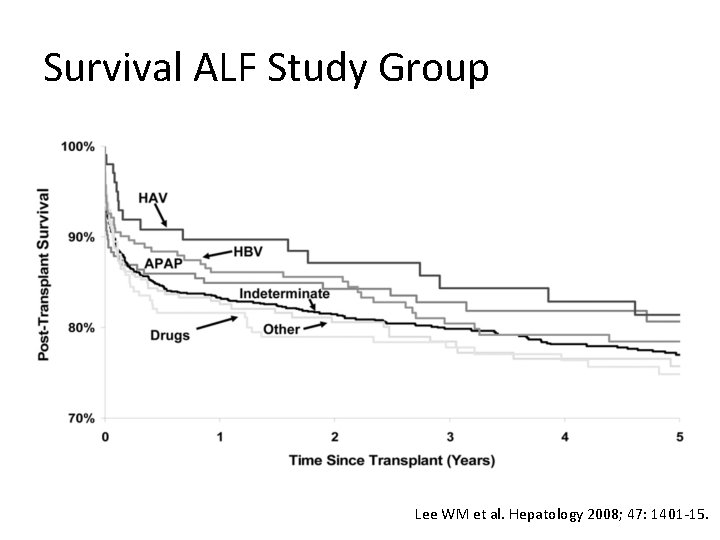
Survival ALF Study Group Lee WM et al. Hepatology 2008; 47: 1401 -15.

Clinical update • Quadruplets were born healthy and are doing well at TCH • Babies should be screened for LCHAD deficiency • Mother at Hermann reportedly has severe pancreatitis, persistent eclampsia with seizures, liver function guarded but stable • She is undergoing plasmapheresis

Take home points • Early recognition of both HELLP and AFLP are critical • Management is prompt delivery of fetus (as well as placenta for HELLP) and supportive care • Clinical distinction between HELLP and AFLP may be subtle – Close postpartum monitoring – Maintain high level of suspicion for AFLP and liver failure

References • • • Ch’ng CL et al. Prospective study of liver dysfunction in pregnancy in South Wales. Gut 2002; 51(6): 876 -80). Ch’ng CL et al. Acute fatty liver of pregnancy in South Wales. Gastroenterology 2002; 123(Supple 1): 53. Goel A et al. How accurate are the Swansea criteria to diagnose acute fatty liver of pregnancy in diagnosing microvesicular steatotis? Gut 2011; 60(1): 138 -9. Hay, J. Liver disease in pregnancy. Hepatology. 2008 Mar; 47(3): 1067 -76. Hepburn IS. Pregnancy-associated liver disorders. Dig Dis Sci. 2008 53: 2334 -2358. Ibdah JA et al. A fetal fatty-acid oxidation disorder as a cause of liver disease in pregnant women. N Engl J Med 1999; 340: 1723 -31. Jin F et al. Therapeutic effects of plasma exchange for the treatment of 39 patients with acute fatty liver of pregnancy. Discovery Medicine, vol. 13, no. 72, pp. 369– 373, 2012. Joshi D et al. Liver disease in pregnancy. Lancet. 2010 Feb 13; 375(9714): 594 -605. Kaplan MM. Acute fatty liver of pregnancy. N Engl J Med 1085; 313: 367 -70. Knight M et al. A prospective national study of acute fatty liver of pregnancy in the UK. Gut 2008; 57: 951 -56. Lee WM et al. Acute liver failure: summary of a workshop. Hepatology 2008; 47: 140115.

References (continued) • • • Lee WM, Stravitz RT, Larson AM. Introduction to the revised American Association for the Study of Liver Diseases Position Paper on acute liver failure 2011. Hepatology. 2012; 55: 965 -967. Seyyed Majidi MR et al. Plasmapheresis in acute fatty liver of pregnancy: an effective treatment. Case Rep Obstet Gynecol. 2013; 615975. Reyes H. Acute fatty liver of pregnancy. Clin Liver Dis 1999; 3: 69 -81. Reyes H et al. Acute fatty liver of pregnancy: a clinical study of 12 episodes in 11 patients. Gut 1994; 35: 101 -106. Stander H, Cadden B. Acute yellow atrophy of the liver in pregnancy. Am J Obstet Gynecol 1934; 28: 61 -69. Steingrub JS. Pregnancy-associated severe liver dysfunction. Crit Care Clin 2004; 20: 763 -776. Than NN and Neuberger J. Liver abnormalities in pregnancy. Best Pract Res Clin Gastroenterol. 2013 Aug; 27(4): 565 -75. Vigil de Gracia P. Acute fatty liver and HELLP syndrome: two distinct pregnancy disorders. Int J Gynaecol Obstet. 2001 Jun; 73(3): 215 -20. Weinstein L. Syndrome of hemolysis, elevated liver enzymes, and low platelet count: a severe consequence of hypertension in pregnancy. Am J Obstet Gynecol 1983; 142: 159 -67.

Questions or comments?
- Slides: 39