GI bleeding l Never forget the general principle


GI bleeding l Never forget the general principle of internal medicine. – – l Airway, Breathing, Circulation Stabilize vital sign and aggressive resuscitation. Well explanation to the family. Acquire thorough history and past medical history. Differential diagnosis of GI bleeding – UGI & LGI l l l Make the diagnosis by yourself! Arrange adequate diagnostic procedure. Emperical treatment

消化道出血的間接症狀: dizziness , fainting, tachycardia, cold sweating, shock, abdominal fullness, poor appetite, cons. change l 一旦懷疑, 利用vital sign評估出血量最重耍 (occult bleeding or overt bleeding) l – Orthostatic hemodynamic change – 10 to 20% blood loss l Drop in systolic pressure > 10 mm. Hg, raise in pulse rate >15/min – Supine hypotension – greater than 20% blood loss 定位 UGI or LGI 同時評估 medical treatment or surgical treatment l GI bleeding vs Non-GI bleeding: 吐血 vs. 咳血 vs. internal bleeding l

Study in GI bleeding l l l l Digital exam for collect stool NG aspiration for DDx UGI and LGI PES: Panendoscopy or EGD( esophago-gastroduodenoscopy): should be perform early in the clinical course after vital sign stable or management. Colonoscopy/ rigid sigmoidscopy RBC scan: only in Taipei MMH: >0. 1 cc/min or 6 cc/hour Angiography: >0. 5 cc/min or 30 cc/hour Enteroscopy or capsule endoscopy Surgery

Why the GI bleeding patient need NPO l Not every GI bleeding patient should NPO l Prepare for emergency study or management l Avoid aspiration

GI bleeding 處理原則 Again and again : Check vital sign l Evaluate NPO or not l If NPO, IVF supply l Arrange laboratory study l – CBC, PTT, Blood group and cross match, liver and renal function. Blood product : Whole blood vs. pack RBC, FFP vs. FP, 代用血漿(ex. 6 HES) l Medication l How to arrange the study: NG irrigation, Blood sampling, PES, Angiography, Colonofiberscope, RBC scan l

Vital sign for GI bleeding Orthostatic hypotension: drop SBP over 10 mm. Hg, rise in pulse rate over 15 beat/min: blood loose 10 -20% l Supine hypotension: more than 20% l Shock index: SBP/HR<1 which hint blood loose over 25% l If the patient got Inderal using, the tachycardia may be disappear ( pacemaker also cover the risk sign) l

IVF supply in GI bleeding Large-bore IV line ( 14 -16 gauge catheter) is better than central line. Isotonic solution (NS), LR can be initiated plus plasma expander ( ex 5% hetastarch or 6 HES) l The IVF amount is dependent on: hemodynamic condition, other CV/renal condition, age l The IVF content is dependent on: underline disease ( DM, LC, Uremia, CHF…) l Some drug add in the IVF( KCL, HRI, st-B. . ) or the IVF is for therapy (PPI or H 2 RA for PUD; pitression/glypression, sandostadin in EV/GV) l

Blood product using in UGI bleeding l l l When transfusion is indicated: bleeding is massive, ongoing, or severe enough that colloid infusion alone is not adequate for tissue oxygenation. ( keep Ht over 25 -30%) The unit is different in Taiwan( 1 unit is about 250 cc but not 500 cc) Whole blood is better than pack RBC if the patient got no risk for fluid overload ( ex. CHF, uremia. . ) Keep platelet over 50000, and correct the PT with vit K, PTT with FFP(also for massive transfusion) Add Bena/Decadron in allergy patient and Lasix avoid fluid overload, Sincal after massive transfusion


UGI bleeding l Differential diagnosis of Variceal and Nonvariceal bleeding – History of liver cirrhosis with/without variceal bleeding – Massive hematemesis – Signs of liver cirrhosis – Spider nevi, Gynecomastia, Splenomegaly, Ascites, Jaundice – Lab data suggest liver cirrhosis – Hypoalbuminemia, PT prolonged, Mild impaired liver function (GOT>GPT) with hyperbilirubinemia, – History of alcohol abuse.

Treatment of variceal bleeding l The most important of all: – STABILIZED THE VITAL SIGN. – WELL EXPLAIN TO THE FAMILY – on critical, 1/3 mortality in each episode. l Pharmacological treatment: – Glypressin (Terlipressin) : 1 amp iv stat and q 6 h. – Sandostadin: 2 amp iv drip stat and 12 amp in 500 c. c. D 5 W run 24 hours – Pitressin: 20 amp in 480 c. c. D 5 W or NS (conc. 0. 8 IU/ml), run 12 cc/hr to 54 cc/hr (0. 2 IU/min to 0. 9 IU/min), side-effect: chest pain, peripheral cyanosis– combine nitrate--- Seldom used in recently years

Treatment of variceal bleeding l Endoscopic treatment – highly operator dependent, high failure rate in acute bleeding, once the procedure succeeded, the outcome is good. – Esophageal varices: band ligation – Gastric varices: Scleosing therapy l SB tube – trachea intubation first, the effect is not good.

l TIPS -- transjugular intrahepatic portosystemic shunt l Operation : Shunt surgery l Precipitating factors of variceal bleeding --treat the precipitating factor – SBP – Sepsis – Impending hepatic failure
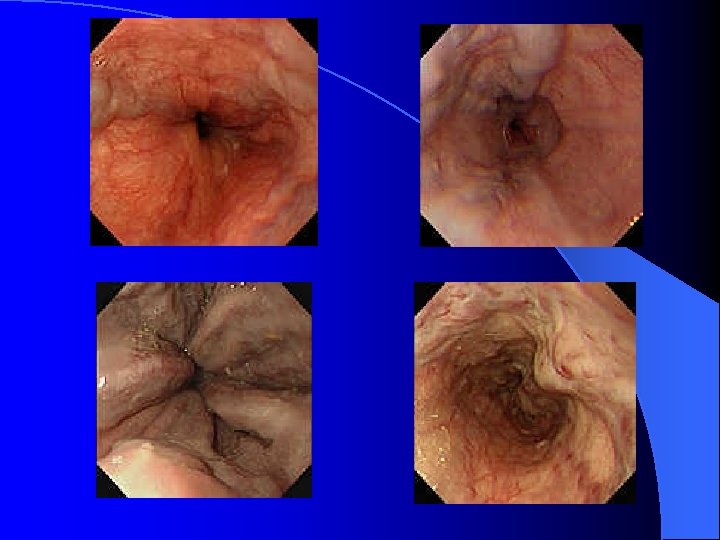
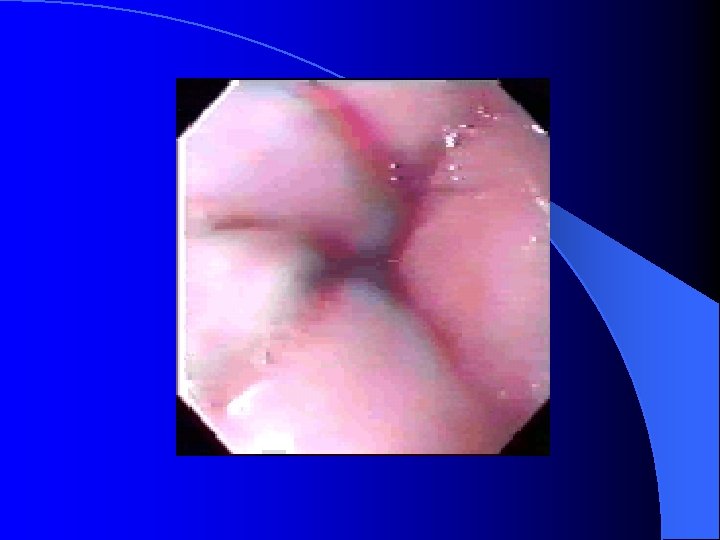
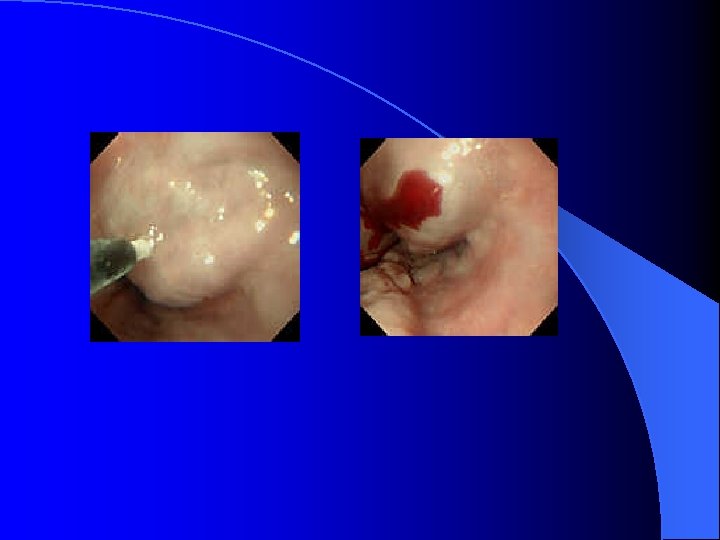
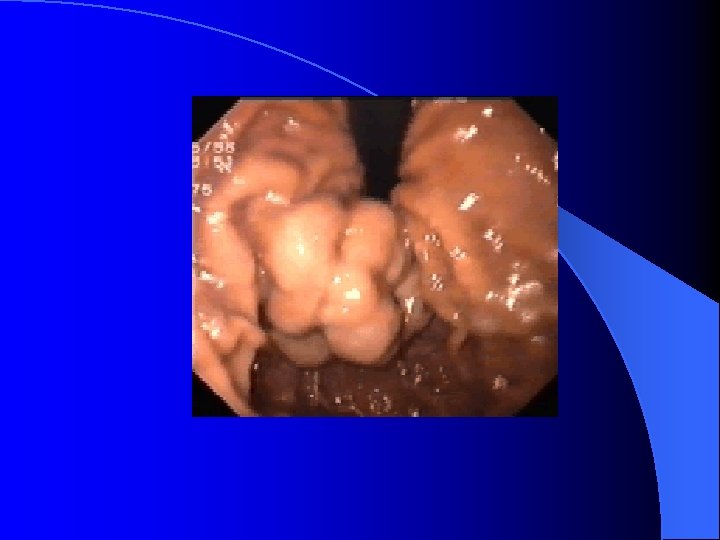



Peptic ulcer disease l Etiology of peptic ulcer disease – Mucosal defensive factor Mucosal barrier to ion diffusion l Two component mucous barrier l Bicarbonate, Phospholipids l Local mucosal blood flow l Prostaglandins, EGF l Intrinsic mechanism that inhibit gastric secretion. l

Peptic ulcer disease l Etiology of peptic ulcer disease – Aggressive factors Gastric acid and pepsin l NSAIDs l H. Pylori l Free radical l


Diagnosis of PUD l Esophagogastroduodenalscopy (EGD) – Gastric ulcer and duodenal ulcer l Description of PUD in EGD – Stage : A 1, A 2, H 1, H 2, Scar – Size : the risk of recurrent bleeding increased if greater than 2 cm – Location : antrum, body, fundus, anterior wall, posterior wall, great curvature side, lesser curvatyre side – SRH (Stigmata of recent hemorrhage) – Gastritis and Erosion.
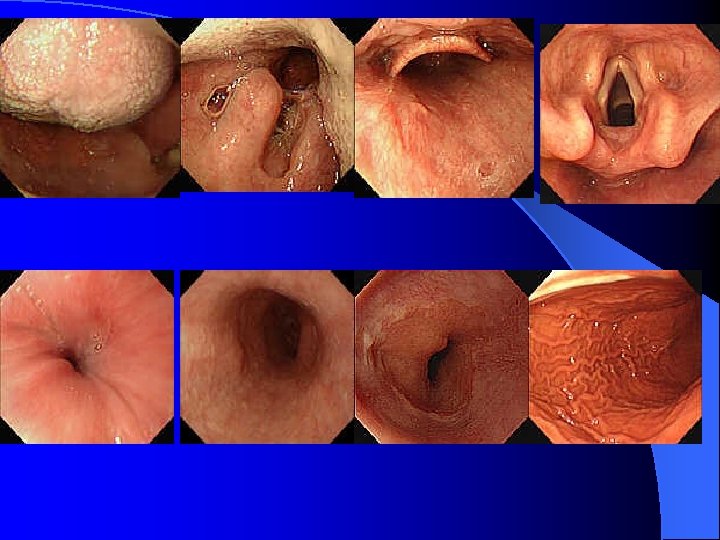
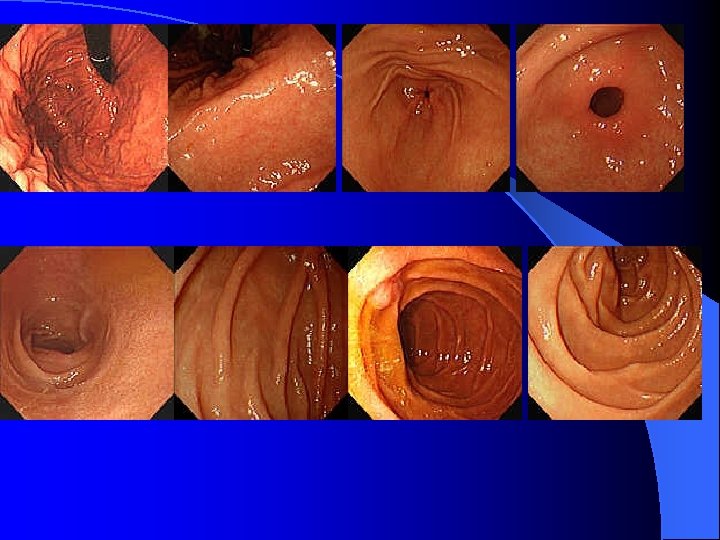
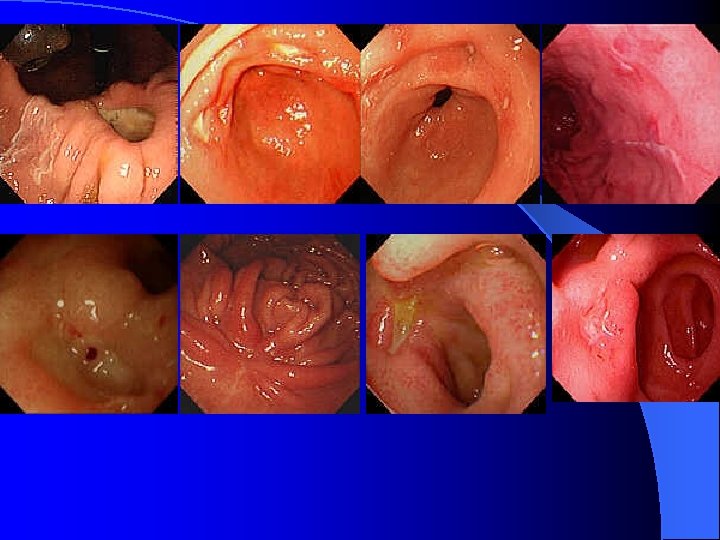

Risky sign in the PES description of UGI bleeding l Varix: RCS ( red color sign) which hint bleeding: red-whale marking, cherry-red spot, active bleeding; Cb>Cw, F 3>2>1 l Ulcer: A 1 -2(active), H 1 -2(healing) and S 12(scaring); active bleeding vs SRH (stigmata of recent bleeding) l Bleeding with unknown cause

Medication/Management in UGI bleeding: PUD l l l PPI ( losec/nexium, takepron, pariet, ) : losec 1 Amp + NS 50 -100 cc drip over 10 min st and q 12 h; the 1# qd H 2 RA (zantac , tazac, famox): Zantac 3 Amp + 500 cc IVF run 20 cc/hr ; then 1# bid Sukit/gelfos 1 pk q 1 h x 4 -6 times Sucrate gel 1 Pk bid or ulsanic 1# qid (avoid using with antiacid, H 2 RA or PPI) Therapeutic endoscopy with bosmin injection, heat probe, hemoclip, laser. . Sometimes, surgical intervention still indicated
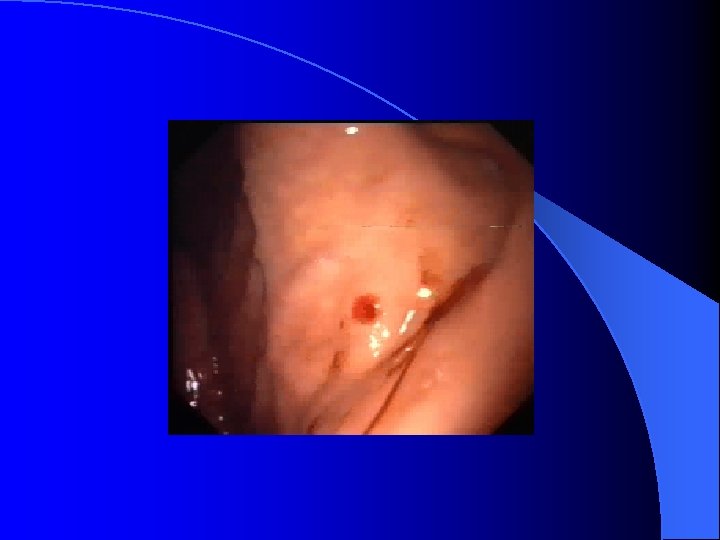

Medication/Management in UGI bleeding: Surgical intervention in PUD or other Dx Hypovolemic shock can not control by medical treatment l Massive transfusion over 4 -6 U/8 U(2000 cc) in 24 hours or over 10 U(2500 -5000 cc) overall l Recurrent or intractable bleeding after nonsurgical treatment l l Risk factor for OP: over 60 y/o, transfusion over 5 unit, shock, hematemesis with hypotension, coagulopathy, large ulcer over 2 cm, emergency Op, co morbid illness, rebleeding within 72 hours


Low GI bleeding l Hemorrhoid, anal fistula, angiodysplasia, radiation proctitis/colitis, aortoenteric fistula, tumor Urgent colonoscopy : difficult due to poor preparation l Consult Proctologist for the surgical intervention l Fortunately, most common LGI bleeding may stopped spontaneously. l
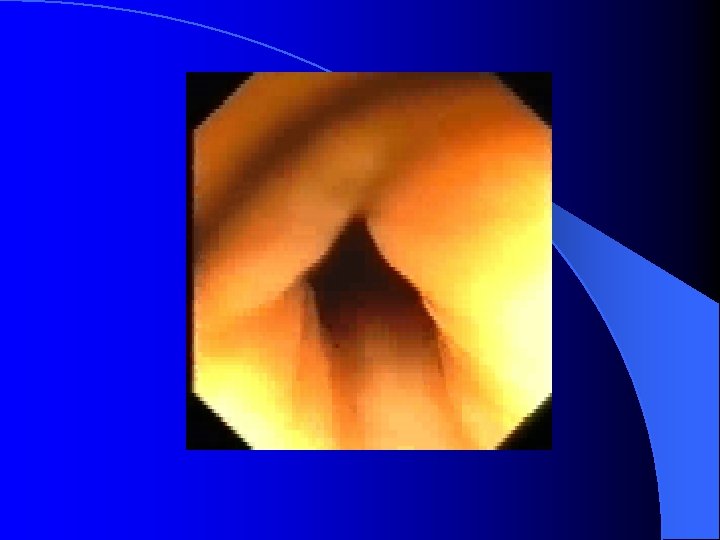


Ileus l Very dangerous diagnosis when new patient arrive with this diagnosis l Paralytic vs Mechanical l NPO in most cases l IVF supply l Overlapping with acute abdomen l Series F/U the same kind x ray film
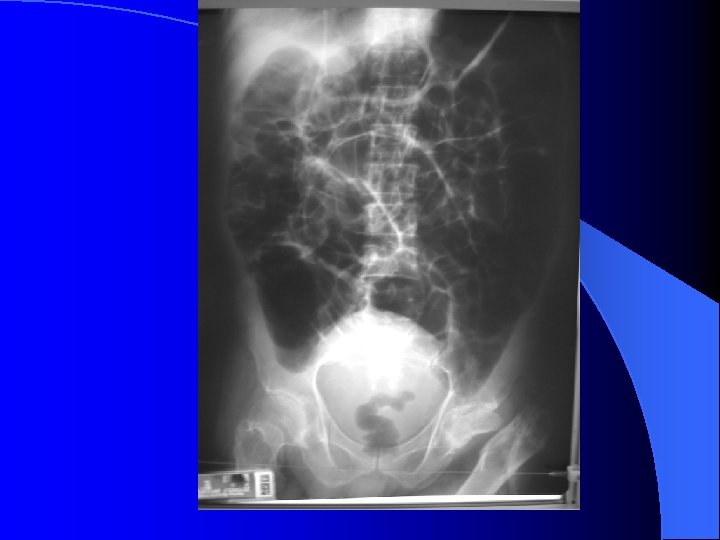
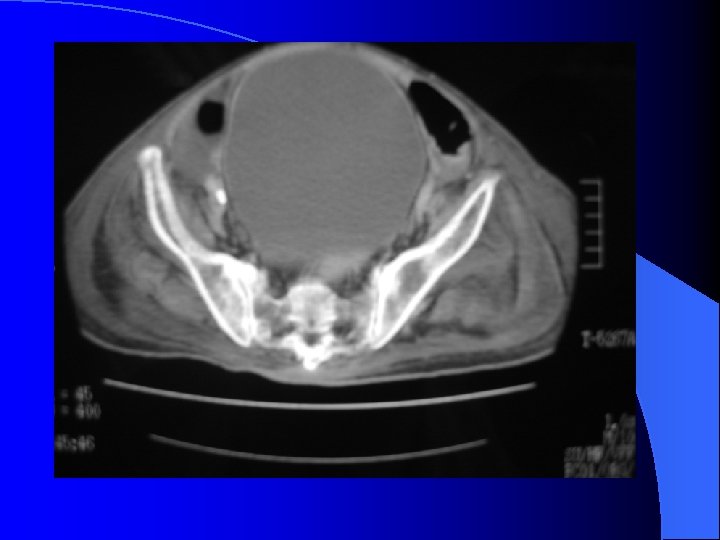
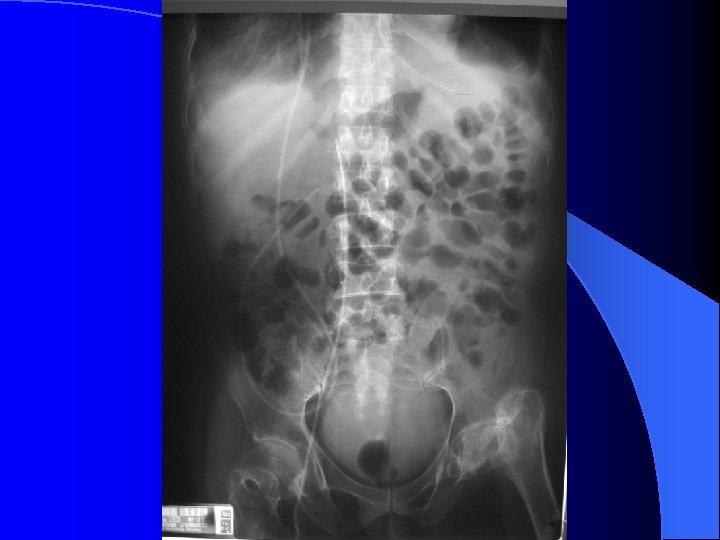

Nausea and vomiting(1) l Bowel obstruction or pregnancy must exclude first. Besides, extra-abdominal problem ( IICP, metabolic problem. . )also need exclude. l The vomitus also help for identified the obstruction level by color l NG decompression amount is another key for evaluate the degree for obstruction

Nausea and vomiting (2) Novamin( proclorperazine): ADR- drowsiness, acute dystonic reaction, EPS, postural hypotension. . l Dopamine antagonist - primperan (metoclopramide- EPS is notorious ADR) and motilium (domperidone). Cisparide is not approve in FDA now l Ondansteron (zofran) and Granisetron ( kytril) are 5 HT 3 (serotonin) receptor inhibitor for C/T l

Diarrhea(1) The definition of diarrhea include the BM increase over 3 times per day and the amount increase l Acute diarrhea vs chronic diarrhea : 2 week l NPO is the first step in DDx the secretary and osmotic diarrhea (but IVF supply also indicated after NPO especially in DM patient) l Stool study : stool OB, pus cell and culture when infectious diarrhea is suspected esp. in bacterial infection). PMC need special agar for culture. Ameba and parasite ova in chronic diarrhea also need considered. l

Diarrhea (2) l l l Drug may be the most common cause of diarrhea in hospital( senokot, Mg. O, antacids, digitalis, quinidine, colchicine, antibiotic. . ) PMC( pseudomembranous colitis)must be carefully monitor when antibiotic using Parasite still need consider esp. in MMH Taitung branch. Most AGE is caused by virus and self-limiting. Diarrhea in cancer patients post radiotherapy is dangerous.

Diarrhea (3) l l l l Review the drug sheet Evaluate the risky sign: BM over 6 times, bloody stool or tenesmus, fever, severe abd pain, dehydration Hydration by enteral feeding if possible Symptomatic treatment with : Kaopetin 15 -20 cc/ Tannalbin for loose stool, Anti-muscarinics ( buscopan-scopolamine, trancolonmepenzolate, bentyl-dicyclomine, esperan-oxapium), Smooth muscle relaxant ( Spasmonal-alverine, Cospanon-Flopropione, Duspatalin. Mebeverine) Imodium 2# st Codeine and Morphine Antibiotic in Infectious diarrhea after stool culture and study: FQ and sulfa drug

PMC or AAC l l l Pseudomenbranous colitis or antibiotic-associated colitis C. difficle is not the only cause Cleocin is most notorious drug. PCN and Cepha got most patient! Dx: scope , toxin, culture( in anaerobic condition) Tx: stop antibiotic, symptomatic control, oral antibiotic ( metronidazole, vancomycine), IV antibiotic may be the last choice. Inferon Berna enema…

Constipation(1) l Medication also the main cause of constipation ( Calcium channel blocker, opiates, anticholinergic, iron, barium sulfate) l Besides, old age and several disease (DM, hypothyroidism, scleroderma, myotonic dystrophy. . ) patient also got constipation tendency l Intestinal obstruction must exclude first

Constipation (2) l Fiber supplementation: Konsyl or Normacol l Emollient laxative: Mineral oil l Stimulant cathartics: Castor oil, Anthraquinones ( senokot 1 -2# qhs), Bisacodyl ( dulcolax 1 -2# qhs or supp) l Osmotic cathartic: Mg citrate, lactulose. . l Fleet enema

TPN l l l l Indication: 不能吃, 不想吃, 吃不下 Time: not over 7 days NPO How to order: gradually increase the dose and concentration How to calculate the water amount How to calculate the calori demand How to calculate the protein demand How to calculate the fat supply How to supply the trace element, Vit…

TPN(2) Complication of TPN 1. Mechanical problem: caused by CVP insertion 2. Chemical problem: BS, electrolyte balance. . 3. Infection problem 4. Other problem: GB stasis and stone, LFT impairment, drug interaction

Complication of hepatic insufficiency l l l l Fulminant hepatic failure Hepatic encephalopathy Hepato-pulmonary syndrome Hepato-renal syndrome Portal hypertension Ascites SBP Coagulopathy

Hepatic failure l l l l How to identified the hepatic failure? PT is more important than AST/ALT Bilirubin also very important parameter Hypoglycemia and hypocholesterol also risky sign Cons. Level must evaluate carefully and closely The NH 3 level is not parallel to cons. Level Very high mortality if no chance for liver transplant The Child-Turcott-Pugh score ( A: 2. 8 -3. 5, A: slightly, Bil: 2 -3, Encephalopathy 1 -2, PT 4 -6) – A: 5, 6 ; B: 7 -9 ; C: 10 -15

Hepatic encephalopaghy ( HE) Correct the precipitating factor: azotemia, tranquilizer, opioid, sedative-hyponotic, GI bleeding, hypokalemia, alkalosis, constipation, infection, diarrhea, porto-systemic shunt l Medication : lactulose po and enema; Neomycine po and enema, Metronidazole po, BCAA chain supply (aminopoly-H) l The possibility of intra-cranial lesion must exclude ( ex. ICH, SDH, brain tumor) l

Hepato-pulmonary sndrome l Intra-pulmonary shunt increase l Hypoxia l Prove by angiography or contrast heart echo.

Hepato-renal syndrome l Similar to pre-renal azotemia l Difficult in DDx l Check Urine Na l Also caused by peripherial arteriol dilatation l Acute vs. Chronic l The kidney is normal !!

Portal HTN l PE: caput medusa, hemorrhoid… l Normal portal presssure: 7 mm. Hg ( about 10 cm H 2 O) l Portal HTN: over 10 mm. Hg ( got S/S if over 12 -15 mm. Hg) l EV or GV bleeding (dependent on which collateral circulation)

Ascites and SBP l l l Aldactone is the first choice for diuretic in LC related ascites Any LC patient with fever, abdominal pain need screen the SBP Neutrophile over 250/ul E coli, KP and Strep pneumoniae Empiric antibiotic: 3 rd cephalosporine or 1 st + aminoglycoside ( risk for renal toxicity) Norfloxcin 400 mg qd can reduce the recurrence for SBP

Coagulopathy l PT prolong l Thrombocytopenia l PTT prolong if the condition worsen or complication

Pancreatitis l l l Lab data can not complete exclude or include all cases CT is most sensitive diagnosis tool in severe pancreatitis Hydration is the key point for treatment Biliary pancreatitis is more common in Taiwan and female patient. Alc related pancreatitis is most common cause in USA and increase in Taiwan Hypertriglycemia vs. DM vs. pancreatitis

Pancreatitis (2) l Biliary pancreatitis need drainage ASAP l Ranson criteria and APACHE II: if Ranson over 3 point or APACHE over 5, the patient got severe pancreatitis l Identified the severe vs mild pancreatitis: clinical course (CV, chest, GI, nephro complication), scoring system, CT staging

Ranson criteria On admission: Alcoholic (Non-alcoholic) WBC: >16000 (18000) Blood sugar: >200 (220) LDH: >350 (400) AST: >250 (440) Age: >55 (70) During the first 48 hours of admission Fall in hematocrit: >10% (10%) Serum calcium: <8 mg/dl (8 mg/dl) Base deficit: >4 m. Eq/L (5 m. Eg/L) Increase in BUN: >5 mg/dl (2 mg/dl) Fluid sequestration: >6 L (6 L) Arterial PO 2: <60 mm. Hg (60 mm. Hg)

Pancreatitis (3) Nature course: l Acute renal failure and M. acidosis l Lung complication (ARDS. . ) l Ileus and GI bleeding l 2 nd infection of necrotic tissue (2 week) l Pseudocyst (6 weeek)

Acute cholangitis vs cholecystitis Comparison of the triade: RUQ pain+ fever+ leucocytosis RUQ pain + fever+ jaundice (Charcot triade) +shock+ cons change (Raynold pentade)

Thank You for Your Attention!
- Slides: 64