Getting Inspired by High Frequency Jet Ventilation Clinical

Getting Inspired by High Frequency Jet Ventilation Clinical Applications and Optimization

Ventilation Facts • The least traumatic ventilation occurs in the mid-portion of the P/V curve. • Lungs are most vulnerable to injury during the recruitment phase. • A 5 cc/kg VT may not prevent overexpansion and lung injury • Apply L. O. V. E.

Goals of Assisted Ventilation • Achieve uniform lung inflation • Minimize over and under inflation • Minimize Fi. O 2 • Early appropriate extubation

How should HFV be used with newborn infants?

Potential HFV Applications 1. Prevent Lung Injury a. Must use early b. Must avoid hyperventilation c. Optimizing PEEP offers huge advantages 2. Treat Lung Injury (Rescue) a. Non-homogeneous Lung Disorders b. Air Leaks (PIE, PTX, etc. ) c. Whenever small VT and Low Paw helps
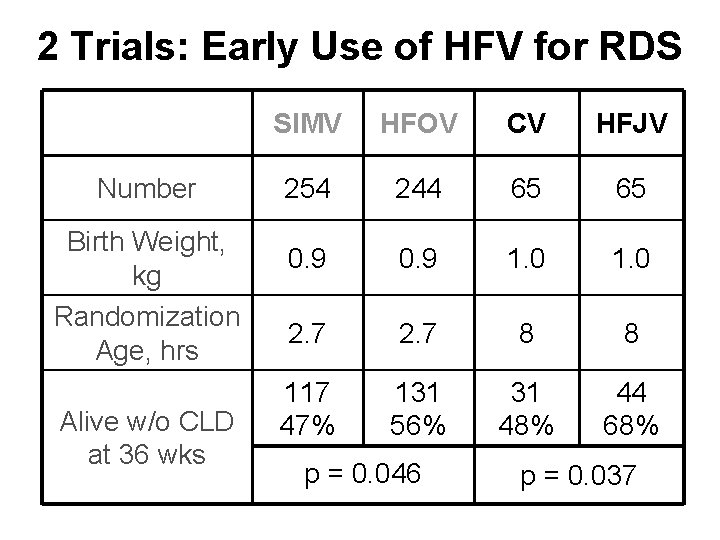
2 Trials: Early Use of HFV for RDS Number Birth Weight, kg Randomization Age, hrs Alive w/o CLD at 36 wks SIMV HFOV CV HFJV 254 244 65 65 0. 9 1. 0 2. 7 8 8 117 47% 131 56% 31 48% 44 68% p = 0. 046 p = 0. 037

HFJV vs. HFOV Similarities • Effective frequencies • Determinants of Pa. O 2 • Determinants of Pa. CO 2 • P drop down airways

Why does one need HFJV? Sick lungs aren’t always homogeneous.
We like to think that the lungs look like this… with lots of surface area for gas exchange.
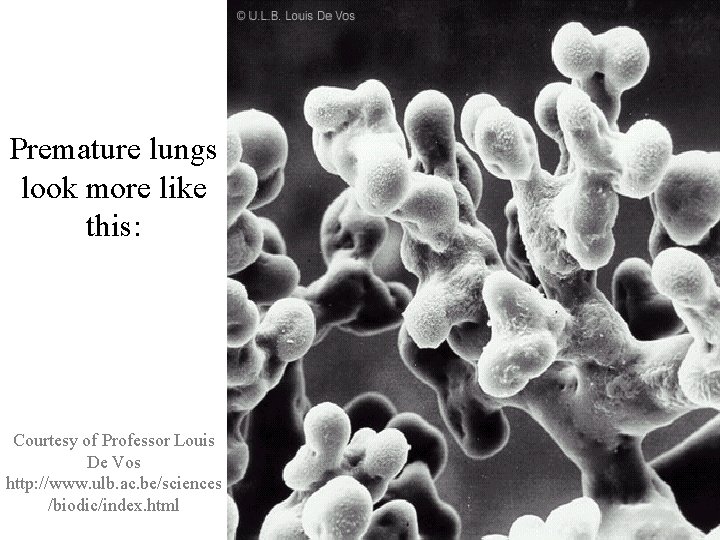
Premature lungs look more like this: Courtesy of Professor Louis De Vos http: //www. ulb. ac. be/sciences /biodic/index. html

The Premature Lung • Alveoli have yet to be fully formed • Surfactant is not yet being adequately produced • Terminal bronchioles make up the most compliant area of the lungs
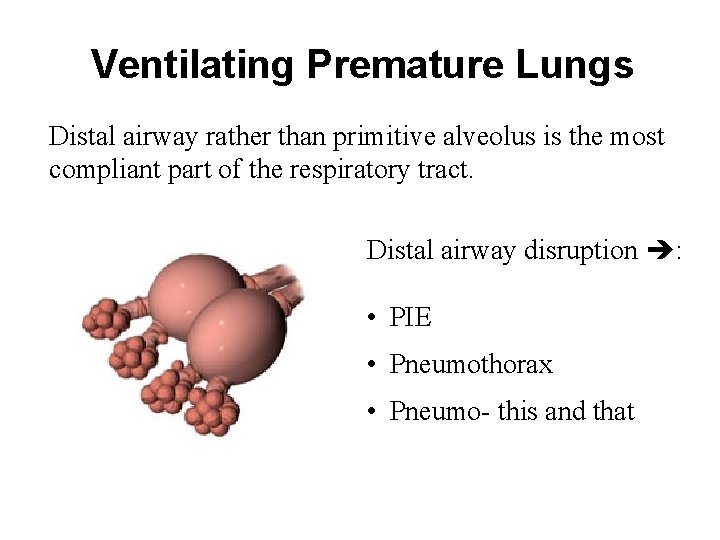
Ventilating Premature Lungs Distal airway rather than primitive alveolus is the most compliant part of the respiratory tract. Distal airway disruption : • PIE • Pneumothorax • Pneumo- this and that
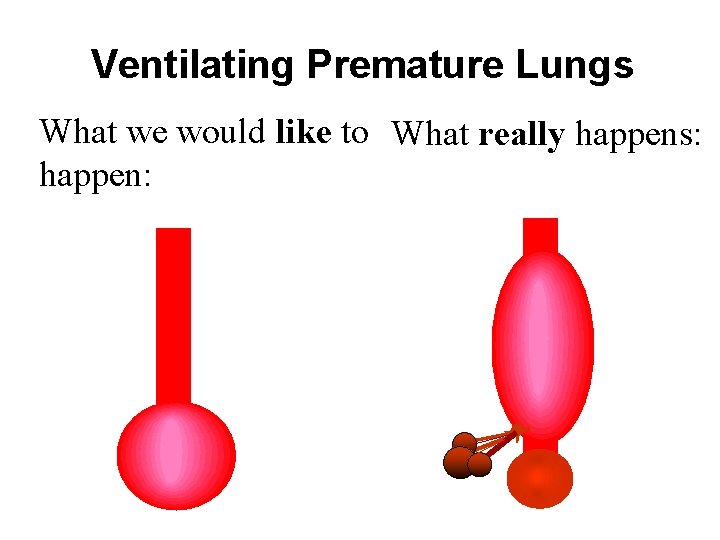
Ventilating Premature Lungs What we would like to What really happens: happen:

Airleaks Originate in Terminal Airways Thar she blows!!

Positive pressure ventilation damages premature lungs • Inflammation • Inhibited alveolar development • PIE and other airleaks • Smooth muscle growth in small airways and alveoli

Using small tidal volumes to treat lung injuries is critically important! How those small tidal volumes are delivered is also critically important!

The Jet squirts gas into the lungs faster than any other ventilator. So what?
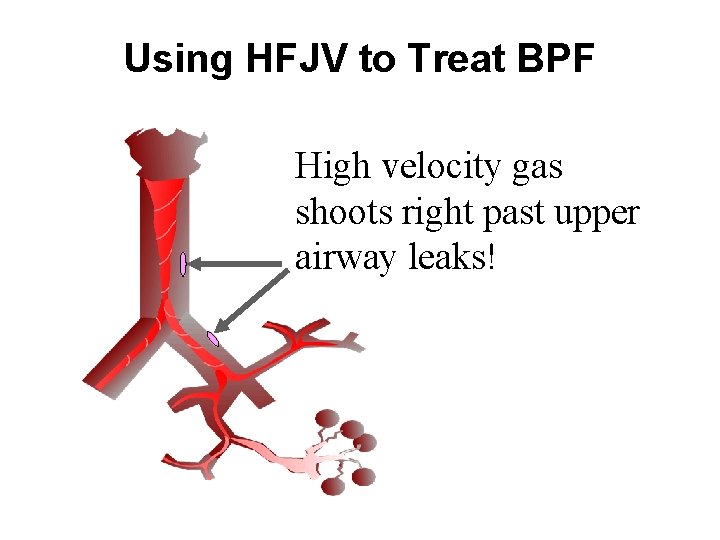
Using HFJV to Treat BPF High velocity gas shoots right past upper airway leaks!

Squirting gas into lungs very rapidly enables the Jet to ventilate Non-Homogenous lung disorders.
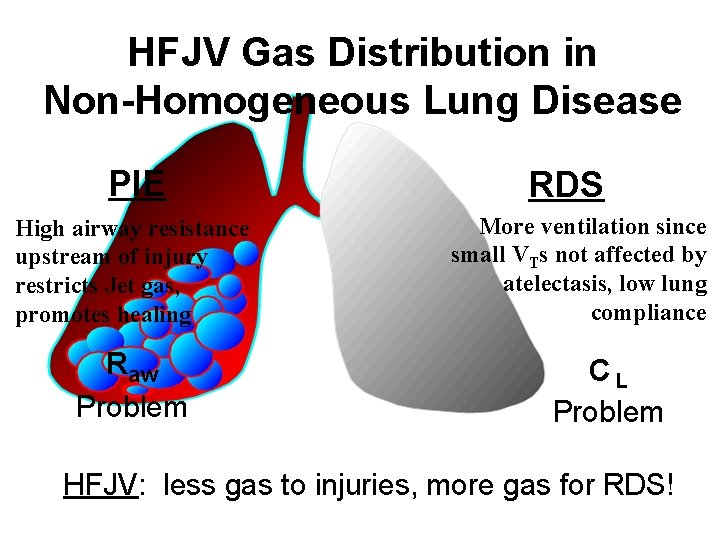
HFJV Gas Distribution in Non-Homogeneous Lung Disease PIE High airway resistance upstream of injury restricts Jet gas, promotes healing Raw Problem RDS More ventilation since small VTs not affected by atelectasis, low lung compliance CL Problem HFJV: less gas to injuries, more gas for RDS!
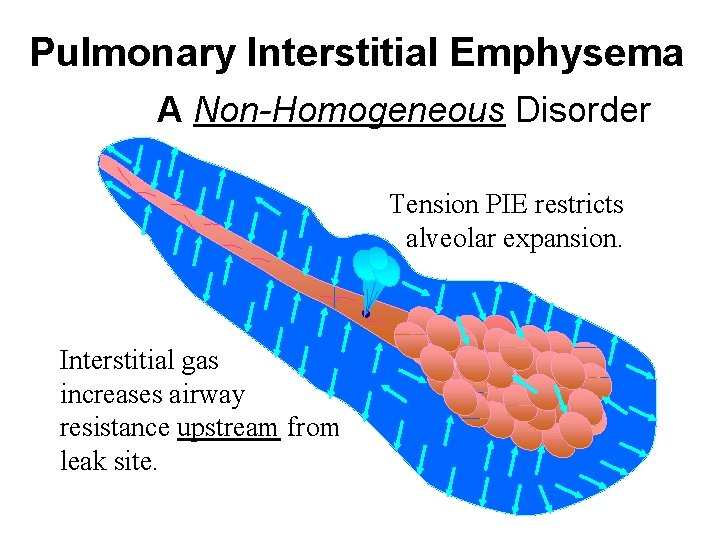
Pulmonary Interstitial Emphysema A Non-Homogeneous Disorder Tension PIE restricts alveolar expansion. Interstitial gas increases airway resistance upstream from leak site.

The principal manifestations of injury in premature lungs are airway narrowing and alveolar disruption.

If we can reduce mechanical ventilation of injured areas of premature lungs, they can heal and grow new lung parenchyma.

HFJV decreases ventilation where airway resistance is increased, so injured alveoli can heal and multiply.

Passive Exhalation • The Jet relies on the lungs for passive exhalation. • Passive exhalation helps the patient in two ways.
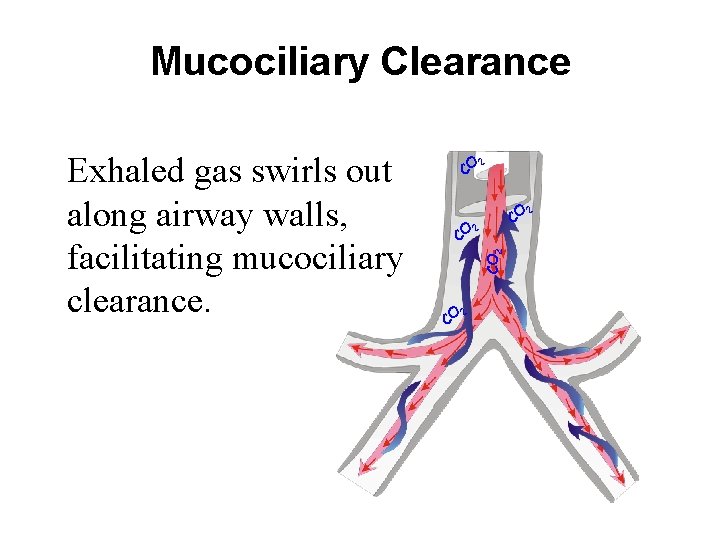
Mucociliary Clearance CO 2 Exhaled gas swirls out along airway walls, facilitating mucociliary clearance. CO CO 2 2

Passive exhalation also enables the Jet to work at lower Paw.
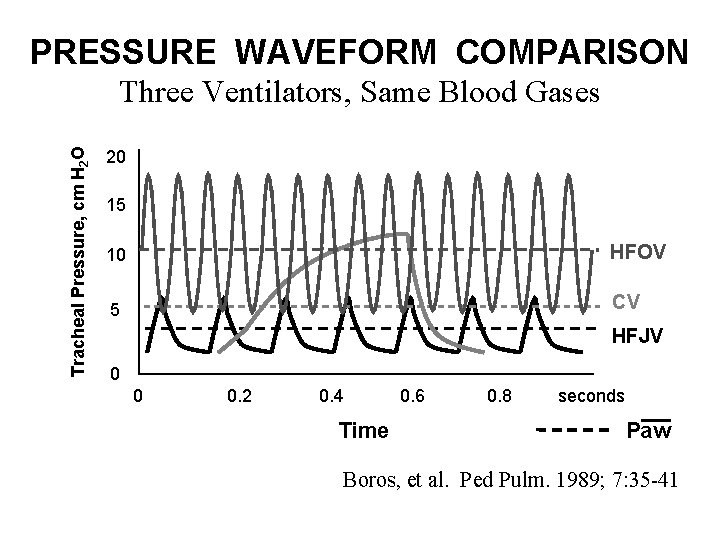
PRESSURE WAVEFORM COMPARISON Tracheal Pressure, cm H 2 O Three Ventilators, Same Blood Gases 20 15 10 HFOV 5 CV HFJV 0 0 0. 2 0. 4 Time 0. 6 0. 8 seconds Paw Boros, et al. Ped Pulm. 1989; 7: 35 -41
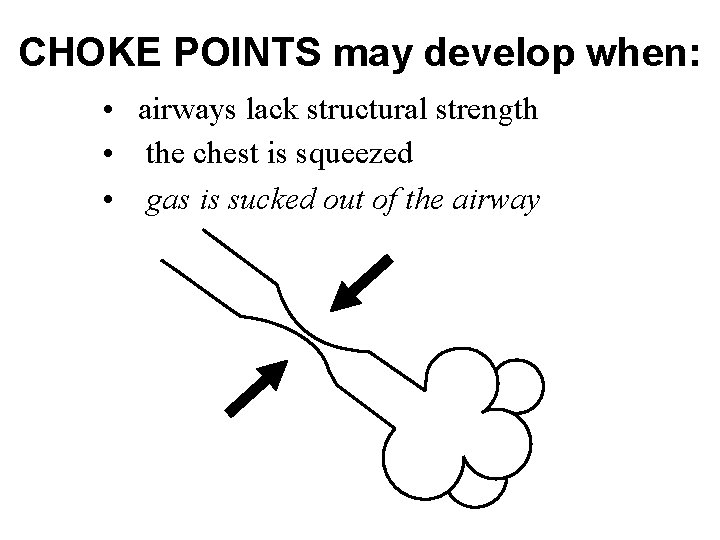
CHOKE POINTS may develop when: • airways lack structural strength • the chest is squeezed • gas is sucked out of the airway
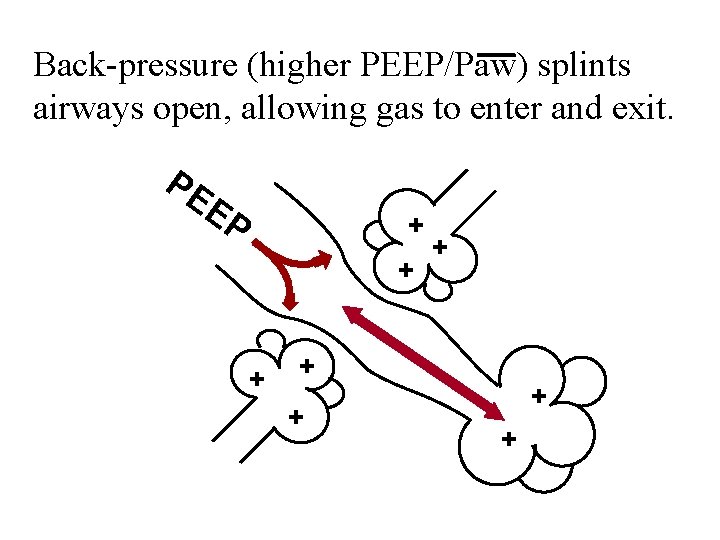
Back-pressure (higher PEEP/Paw) splints airways open, allowing gas to enter and exit. PE EP + + + +

Consequences of Active Exhalation 1. A limit to how much Paw can be reduced. 2. Possible interference with venous return, cardiac output.

HFJV vs. HFOV When is the Jet the HFV of choice? • Air Leak Syndromes (particularly PIE, Ptx) • Excessive Secretions (e. g. , some pneumonias, MAS) • Hemodynamic Compromise (e. g. , PPHN, cardiac anomalies)

Other Conditions When Jet is the HFV of choice: • Non-Homogeneous Lung Disorders (e. g. , when HFOV fails) • Difficult to Wean Patients (e. g. , BPD, Chronic Lung Disease)
The “Jet” Operating instructions: www. bunl. com
“Patient Box”
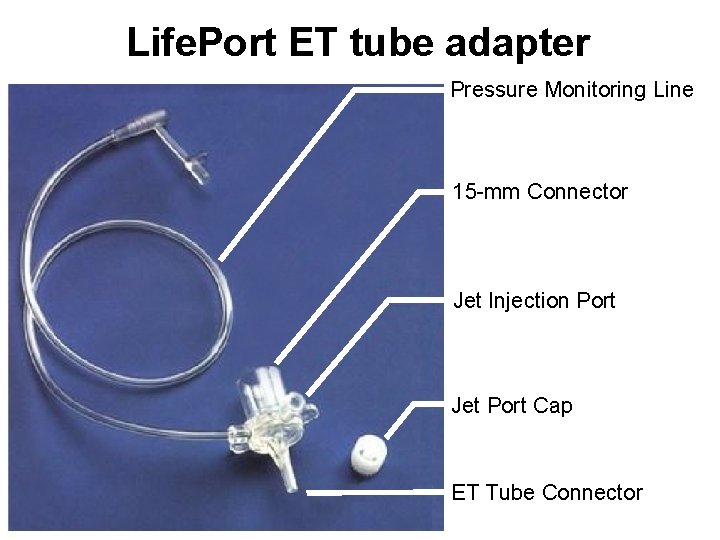
Life. Port ET tube adapter Pressure Monitoring Line 15 -mm Connector Jet Injection Port Jet Port Cap ET Tube Connector
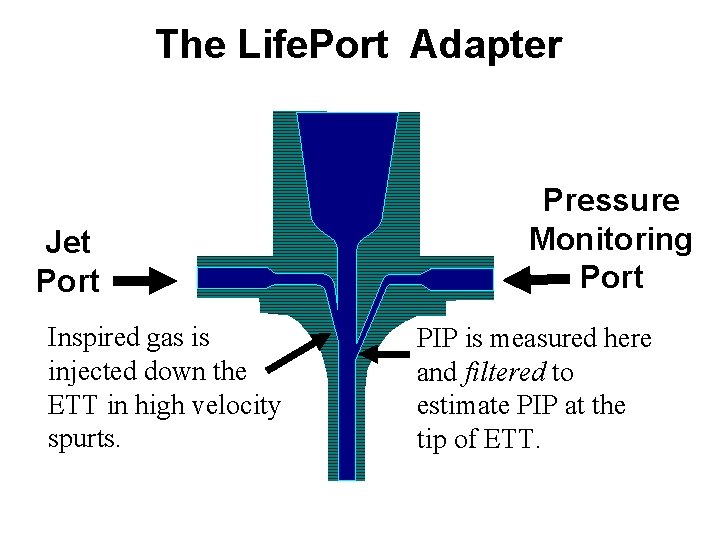
The Life. Port Adapter Jet Port Inspired gas is injected down the ETT in high velocity spurts. Pressure Monitoring Port PIP is measured here and filtered to estimate PIP at the tip of ETT.

HFJV Monitoring and Alarms • Sensitive to changes in patient’s condition • Help you maintain optimal lung volume without xrays

Monitoring HFJV with High – Low Alarms • Servo Pressure • Mean Airway Pressure
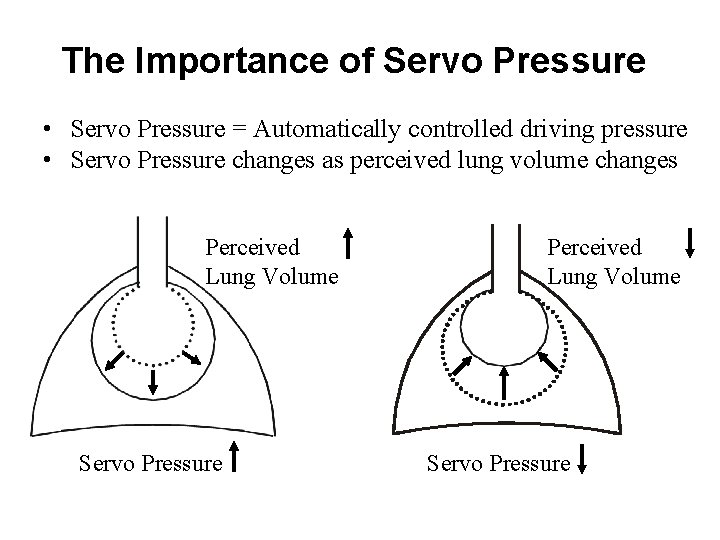
The Importance of Servo Pressure • Servo Pressure = Automatically controlled driving pressure • Servo Pressure changes as perceived lung volume changes Perceived Lung Volume Servo Pressure

Observing Servo Pressure can facilitate patient management Servo Increases Servo Decreases • Improved compliance and/or resistance • Worsened compliance and/or resistance • Airleak • Obstruction of ET Tube • Disconnected Tubing • Tension pneumothorax • Extubation • Patient needs suctioning

Servo Pressure • High Alarm (usually good news): o o improved lung mechanics (compliance or resistance) tubing leaks, etc.

Servo Pressure • Low Alarm (always bad news): o degradation of lung mechanics o atelectasis o accumulation of secretions o tension pneumothorax o right mainstem intubation o etc.

Mean Airway Pressure • High Alarm: inadvertent PEEP, gas trapping. • Low Alarm: tubing leaks or disconnects, inadvertent changes in CV settings, etc.
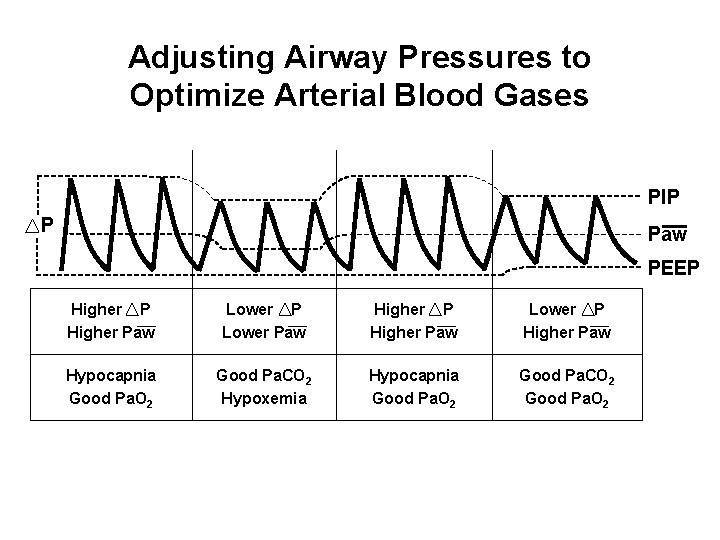
Adjusting Airway Pressures to Optimize Arterial Blood Gases PIP P Paw PEEP Higher Paw Lower Paw Higher Paw Lower P Higher Paw Hypocapnia Good Pa. O 2 Good Pa. CO 2 Hypoxemia Hypocapnia Good Pa. O 2 Good Pa. CO 2 Good Pa. O 2

How much PEEP should one use with HFJV?
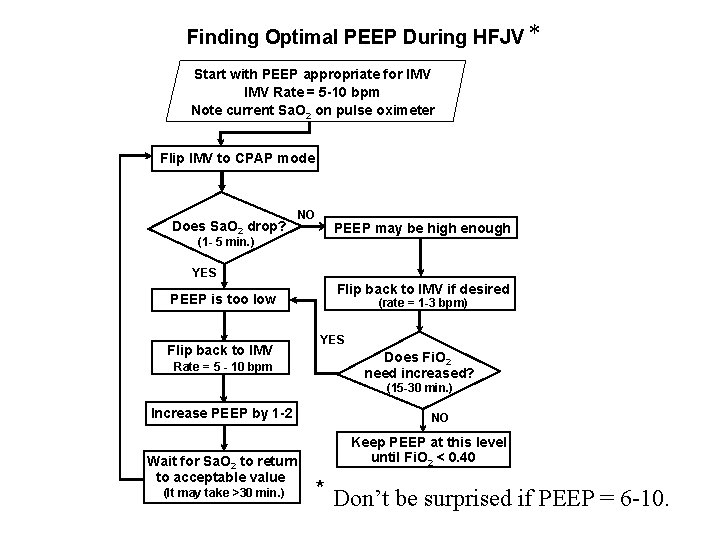
Finding Optimal PEEP During HFJV * Start with PEEP appropriate for IMV Rate = 5 -10 bpm Note current Sa. O 2 on pulse oximeter Flip IMV to CPAP mode Does Sa. O 2 drop? NO (1 - 5 min. ) PEEP may be high enough YES PEEP is too low Flip back to IMV Rate = 5 - 10 bpm Flip back to IMV if desired (rate = 1 -3 bpm) YES Does Fi. O 2 need increased? (15 -30 min. ) Increase PEEP by 1 -2 Wait for Sa. O 2 to return to acceptable value (It may take >30 min. ) NO Keep PEEP at this level until Fi. O 2 < 0. 40 * Don’t be surprised if PEEP = 6 -10.
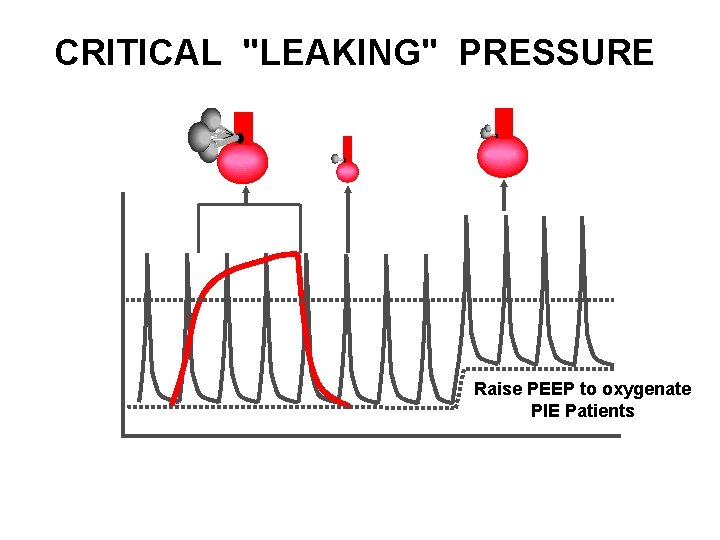
CRITICAL "LEAKING" PRESSURE cm H 2 O 30 20 15 10 Raise PEEP to oxygenate PIE Patients 5 0. 0 0. 5 1. 0 seconds 1. 5 2. 0

Other Patient Management Strategies for HFJV
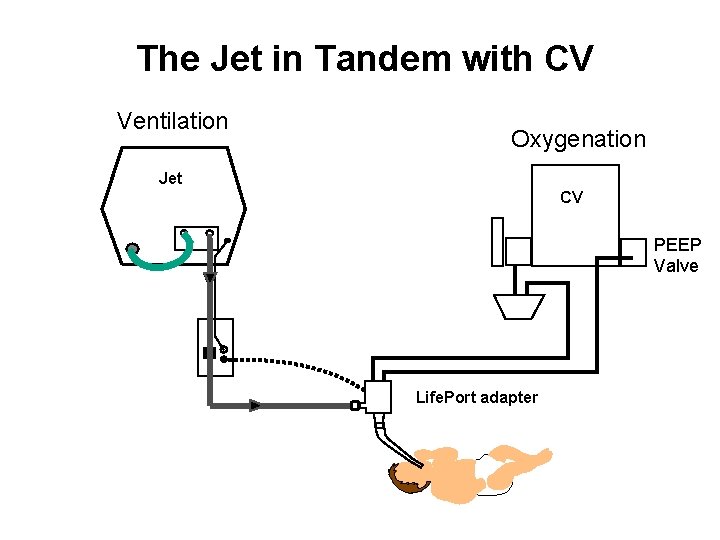
The Jet in Tandem with CV Ventilation Oxygenation Jet CV PEEP Valve Life. Port adapter

HFV ∆P is key to controlling Pa. CO 2 VCO 2 f x VT 2 Drazen JM, et al. Physiol. Rev. 64: 505, 1984. Fredberg, JJ. Acta Anaesthesiol. Scand. 33: 170, 1989.

Oxygenation: 2 -Step Process Step One • Stabilize alveoli with adequate PEEP. Step Two • Recruit collapsed alveoli with IMV when atelectasis is present.
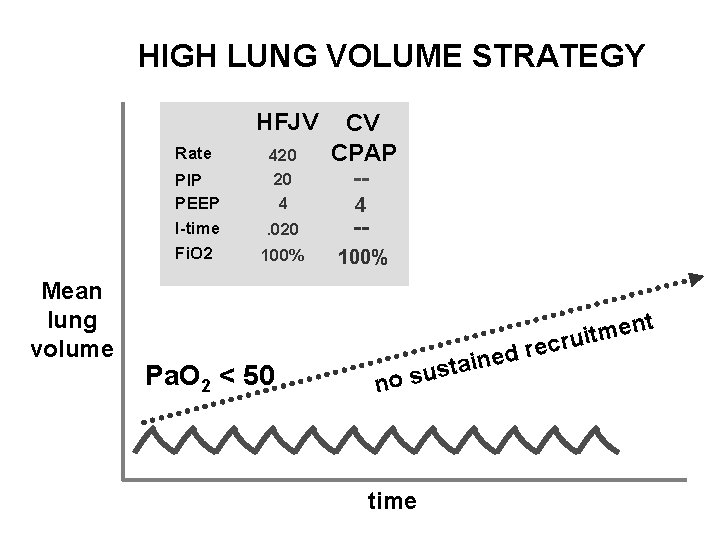
HIGH LUNG VOLUME STRATEGY HFJV Rate PIP PEEP I-time Fi. O 2 Mean lung volume 420 20 4. 020 100% CV CPAP -4 -100% t en m t i u cr Pa. O 2 < 50 e r d e n ustai no s time
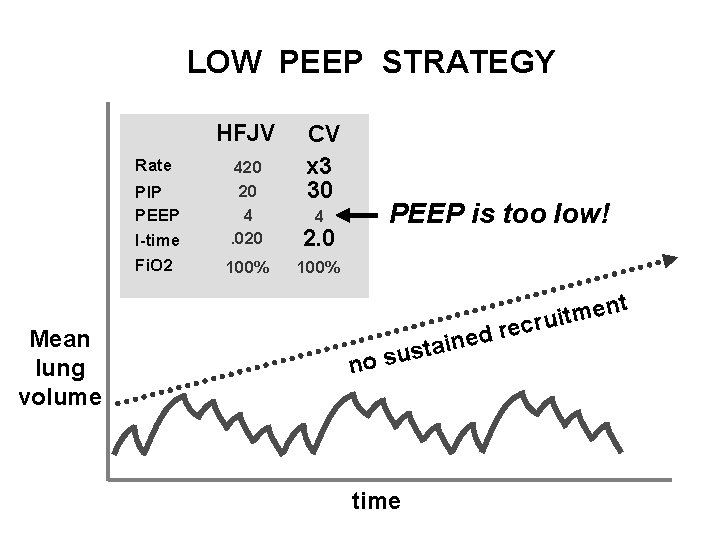
LOW PEEP STRATEGY HFJV Rate PIP PEEP I-time Fi. O 2 Mean lung volume CV x 3 30 420 20 4. 020 2. 0 100% 4 PEEP is too low! ned i a t s u no s time re t n e m cruit
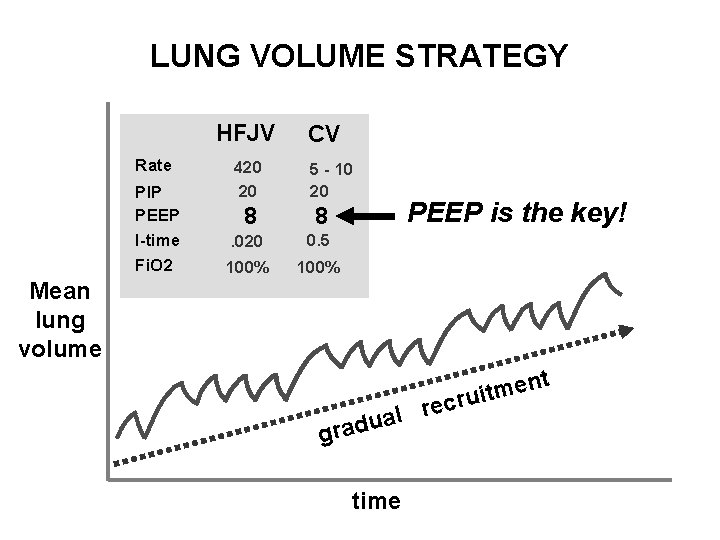
LUNG VOLUME STRATEGY HFJV Rate PIP PEEP I-time Fi. O 2 420 20 CV 5 - 10 20 8 8 . 020 0. 5 100% PEEP is the key! Mean lung volume t n e m cruit re l a adu gr time
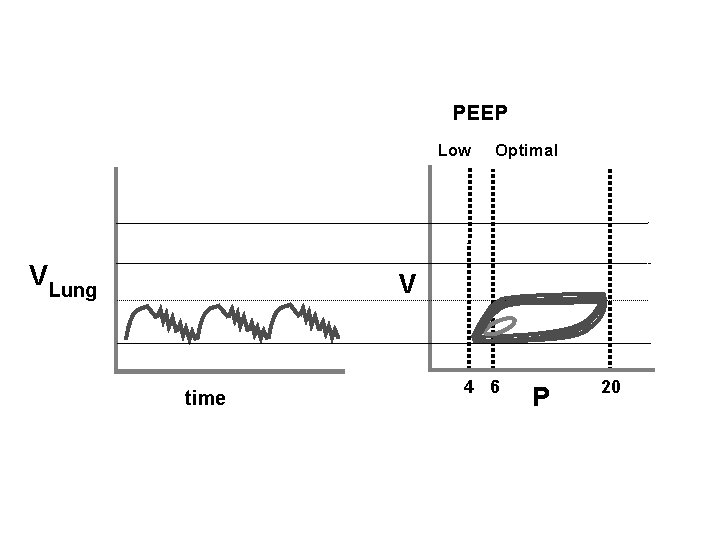
PEEP Low V Lung Optimal V time 4 6 P 20
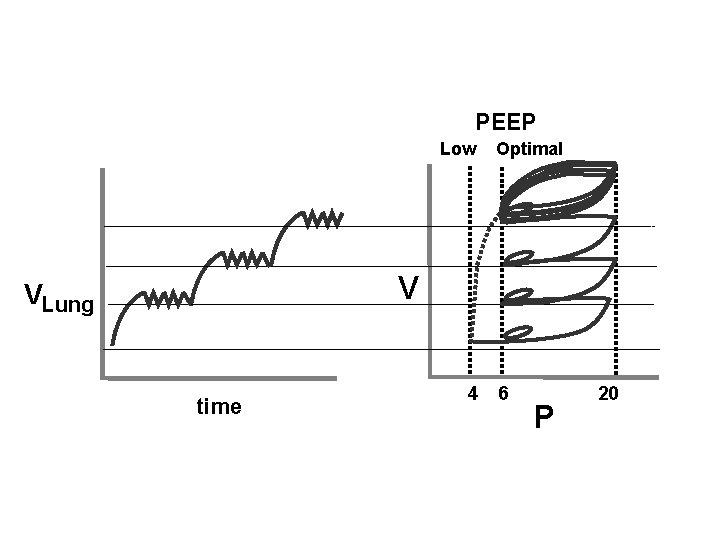
PEEP Low Optimal V VLung time 4 6 P 20
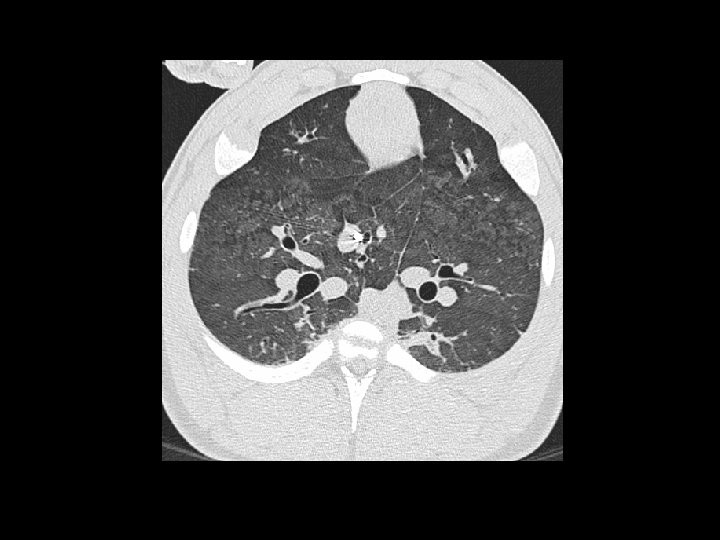

Using IMV to recruit collapsed alveoli is a temporary maneuver. Do not continue to use high CV rate with high PEEP once oxygenation improves!

Combining CV & HFJV doesn’t have to be Complicated • Only Jet PIP requires adjustment, to control PCO 2. • CV PEEP is the main determinant of Paw and PO 2.

HFJV + CV = Versatility CV breaths can: • Recruit collapsed alveoli. • Dilate or open collapsed airways. • And, you can add them with or without HFJV breaths.

HFJV + CV: Keep It Simple • CV settings are usually minimized, except for PEEP • IMV Rate: 10 bpm zero (CPAP) • PIP and I-time settings should be set in proportion to Rate.

Summary…

Why HFJV? 1. Very Gentle (prevent CLD? ) • Small Tidal Volumes • Low Airway Pressures 2. Easy to Use, Like Conventional Ventilation • Same principles of gas exchange • Same setting changes produce same blood gas changes 3. Combined HFJV / CV = Great Versatility 4. Works great with non-homogeneous lung disorders.

When is the Jet the HFV of choice? • Air Leak Syndromes • Non-Homogeneous Lung Disorders • Excessive Secretions • Hemodynamic Compromise • Difficult to Wean (BPD, CLD) Patients

Are you Inspired? • Read the handout • Website: www. bunl. com • Call the Hotline: 1 -800 -HFJV
INO via HFJV
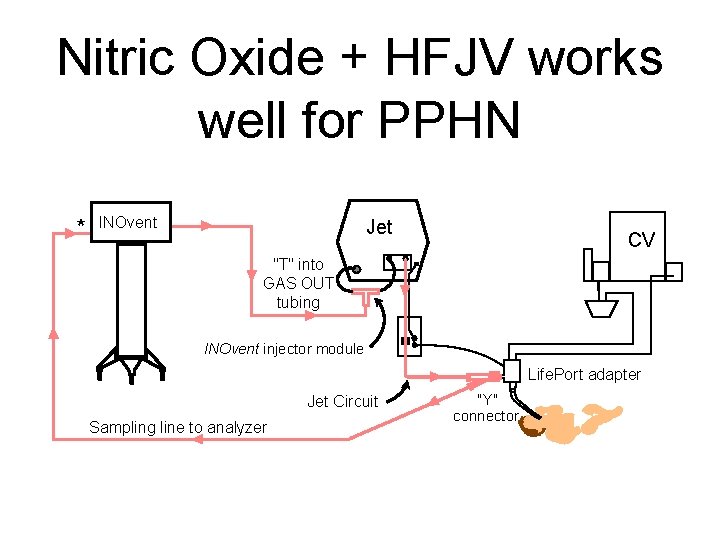
Nitric Oxide + HFJV works well for PPHN * INOvent Jet CV "T" into GAS OUT tubing INOvent injector module Life. Port adapter Jet Circuit Sampling line to analyzer "Y" connector
- Slides: 68