Gestational trophoblastic tumours Dr Mohammad AbdelRahman Lecturer Ob

Gestational trophoblastic tumours Dr: Mohammad Abdel-Rahman Lecturer Ob. Gyn 2020

Management • Evacuation • Surgical evacuation is the usual treatment of molar pregnancy using suction curettage • Medical induction using prostaglandins is not used (except in partial mole with large fetus) due to risk of severe haemorrhage and risk of embolization of the tumour cells • The uterus is soft and there is possibility of perforation of the uterus so surgical evacuation with ring and sharp curettage is not favoured and use of negative suction is sufficient for evacuation. Evacuation is usually done under ultrasound control to minimize the risk of perforation.

Management • Evacuation • Bleeding can be significant so blood must be ready at the time of surgery plus the use of oxytocin at the time of evacuation. Oxytocin also might decrease the risk of perforation by making the uterus harder. • Biopsy is sent for histopathology to (1) prove the diagnosis of mole and (2) exclude the possibility of Choriocarcinoma. • N. B. 1 Currently hysterotomy is not done • NB 2 Theca lutein cysts resolute spontaneously (never touch)

Follow up • Vesicular mole is a premalignant condition that can transform into malignancy. The risk of p. GTD is 10 % in complete mole and 0. 5 % in partial mole. • Β-h. CG is the tumour marker that is used to follow up the resolution of the tumour after evacuation. It should be repeated every weekly at first month then every two weeks until 6 months. • During the whole period of follow up the woman should take contraception. • COCs or IUD should not be used until βh. CG become normal (Barrier methods can be used) • If the Β-h. CG level does not fall (plateau) or if it increases this diagnoses the condition called Persistent gestational trophoblastic tumour (p-GTD)

Follow up Indications of chemotherapy: 1. Persistent gestational trophoblastic tumour (p-GTD). 2. If histopathology shows Choriocarcinoma • Chemotherapy is either single agent or combination chemotherapy according to risk scoring (see below)

Invasive mole • It is a complete or partial mole (histolopathologically shows villi) but shows invasion of the myometrium. • It is almost always follows molar pregnancy. Management is by chemotherapy not re-evacuation. • Most of cases of p. GTD are invasive mole

Choriocarcinoma • Pathology: • It is a metastatic malignant trophoblastic tumour characterized by the presence of sheets of trophoblastic cells. There are no villi. • About 50 % follows molar pregnancy, 25 % follows miscarriage, and 25 % follows normal term pregnancy.

Choriocarcinoma • Clinical picture: • Vaginal bleeding: the most common presentation • Genital metastasis: vulva, vagina • Distant metastasis: • Lung: most common. Present as cough, dyspnea, hemoptysis, acute respiratory failure • Other areas: liver (jaundice, hypochondrial pain), brain (seizures), . .

Choriocarcinoma Staging of Gestational Trophoblastic Neoplasia Stage I Disease confined to uterus Stage II GTN extending outside uterus but limited to genital structures (adnexa, vagina, broad ligament) Stage III GTN extending to lungs Stage IV All other metastatic sites

Choriocarcinoma • Investigation: • β-h. CG : important in follow up • Ultrasound: Intracavitary mass with high blood flow on Doppler • Metastatic workup: Chest x-ray, abdominal, and pelvic ultrasound. CT chest, abdomen, pelvis, and brain • Treatment: is by Chemotherapy either single agent or combination chemotherapy according to risk scoring
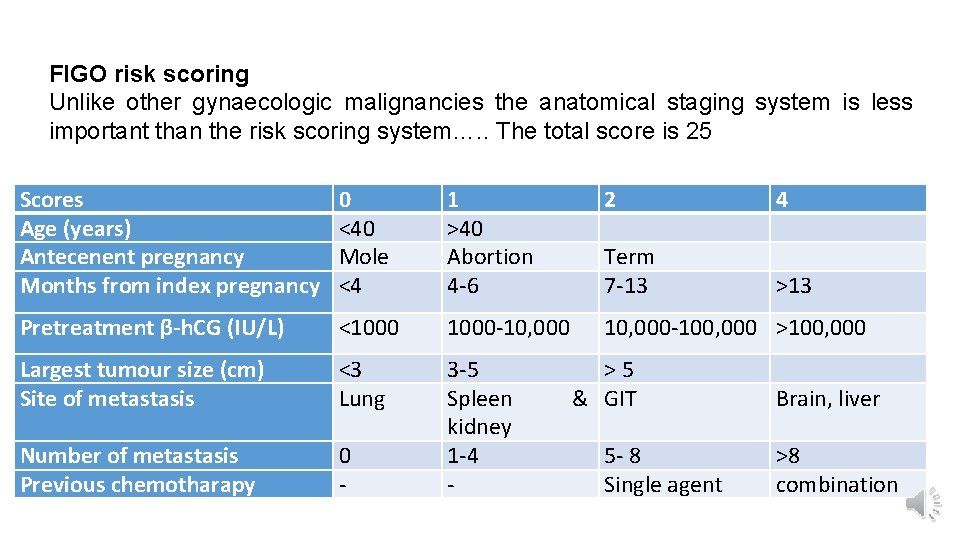
FIGO risk scoring Unlike other gynaecologic malignancies the anatomical staging system is less important than the risk scoring system…. . The total score is 25 Scores Age (years) Antecenent pregnancy Months from index pregnancy 0 <40 Mole <4 1 >40 Abortion 4 -6 2 Term 7 -13 Pretreatment β-h. CG (IU/L) <1000 -10, 000 -100, 000 >100, 000 Largest tumour size (cm) Site of metastasis <3 Lung Number of metastasis Previous chemotharapy 0 - 3 -5 Spleen kidney 1 -4 - > 5 & GIT 5 - 8 Single agent 4 >13 Brain, liver >8 combination

Choriocarcinoma • Management of low risk (if score ≤ 6) • Single agent methotrexate is given alternatively with folinic acid. • If β-h. CG do not fall (plateauing) or if it increases during the treatment: give combination chemotherapy (EMA-CO) • Cure rate is 100 % • Management of high risk (if score ≥ 7) • Combination chemotherapy (EMA-CO) is given. • [Etoposide, Methotrexate, Adriamycin…. . Cyclophosphamide, Vincristine (Oncovin)] • If β-h. CG do not fall (plateauing) or if it increases during the treatment: hysterectomy is indicated • Cure rate is 95 %

Choriocarcinoma Follow up • There is a risk of recurrence and long term follow up (may be for life) is required. • Contraception is used for 1 year
- Slides: 13