GESTATIONAL TROPHOBLASTIC DISEASE Jolanta Zegarska MD Ph D

GESTATIONAL TROPHOBLASTIC DISEASE Jolanta Zegarska MD, Ph. D Department of Obstetrics, Gynecology and Gynecological Oncology. Collegium Medicum in Bydgoszcz, Nicolaus Copernicus University in Torun

Definition • Gestational Trophoblastic Disease (GTD) • Represents a spectrum of diseases characterized by active abnormal proliferation of trophoblastic cells • Includes a unique spectrum of interrelated diseases: • Benign hydatiform mole • Invasive mole (Chorioadenoma destruens) • Choriocarcinoma • Placental site trophoblastictumor (very rare)

Epidemiology and Etiology • The incidence of molar pregnancy is about 1 in every 1500 to 2000 pregnancies (white woman) • Higher incidence among women in Asia (for example in Taiwan: 1 in every 125 to 200 pregnancies) • The cause of GTD is unknown • Most patients (80 -90%) follow a benign course • The risk for the development of a second molar pregnancy is 1 to 3 % (40 times greater than the risk for developing the first molar pregnancy) • GTD occur more frequently in women younger than 20 years and older than 40 years
Relationship Hydatidiform mole Invasive mole Abortion, delivery, ectopic pregnancy choriocarcinoma

HYDATIDIFORM MOLE

Hydatidiform mole/definition • the placental trophoblastic cells proliferate abnormally • It is a neoplastic proliferation of the trophoblast in which the terminal villi are transformed into vesicles filled with clear viscid material • there is stromal edema • forms vesicula which is like grape on its appearance

Hydatidiform mole/classification • Hydatidiform mole is divided into • Complete mole • Incomplete/partial mole • Based on clinical, patomorphological and genetic features

Complete mole • Most hydatidiform moles are complete • Have a 46 xx karyotype • Both of the x chromosomes are paternally derived • It results from the fertilization of an „empty egg” by haploid sperm 23 x which then duplicates to restore the diploid chromosomal complement • Only a small percentage are 46 XY • Complete molar pregnancy is only rarely associated with a fetus, and this may represent a form of twinning

Complete mole/Genetic

Complete mole • Histopathologic findings associated with a complete molar pregnancy • Hydropic villi • Absence of fetal blood vessels • Hyperplasia of trophoblastic tissue • Invasive mole differs from hydadtidiform mole only in its propensity to invade locally and to metastasize

Complete mole/symptoms • Bleeding in the first half of pregnancy • Irregular bleeding • Heavy vaginal bleeding • Lower abdominal pain • Excessive nausea/ hyperemesis gravidarum • Preeclampsia • Irritability • Dizziness • Photophobia • Hyperthyroidism • Nervousness • Anorexia • Tremors

Complete mole/signs • Tachycardia • Tachypnea • Hypertension • Absent fetal heart tones (and fetal parts) • Grape-like vesicles of the mole may be detected in the vagina • Enlarged uterus • 50% patients with molar pregnancies • 25% have size compatible and 25% have size smaller than gestational age • Ovarian enlargement by theca-lutein cyst • Occurs in about 1/3 of women with molar pregnancies
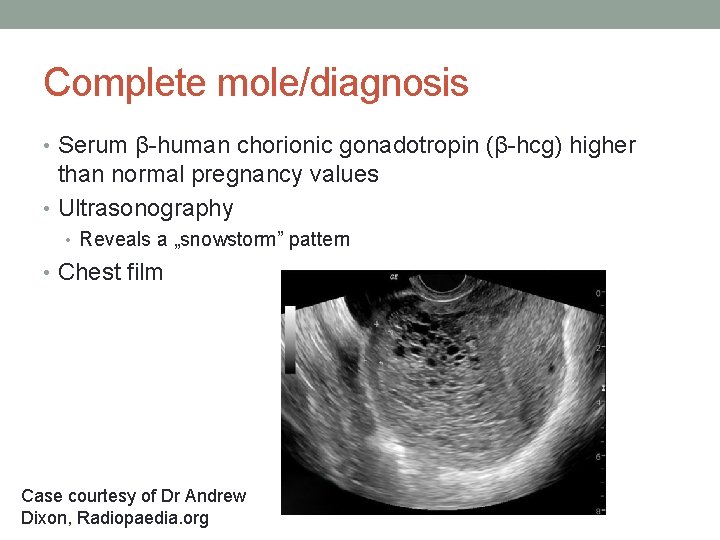
Complete mole/diagnosis • Serum β-human chorionic gonadotropin (β-hcg) higher than normal pregnancy values • Ultrasonography • Reveals a „snowstorm” pattern • Chest film Case courtesy of Dr Andrew Dixon, Radiopaedia. org

Complete mole / prognosis • Complete mole has the latent risk of local invasion or telemetastasis • The high-risk factors includes • β-HCG > 100000 IU/L • Uterine size is obviously larger than that with the same gestational time. • The luteinizing cyst is > 6 cm • If > 40 years old, the risk of invasion and metastasis may be 37%, If > 50 years old, the risk of invasion and metastasis may be 56%. • Repeated mole: the morbidity of invasion and metastasis increase 3~4 times

Incomplete mole • 10% of moles are incomplete • Is not associated with age • Karyotype is usually a triploid • Often 69 XXY (80%) • These lesions often present with a coexistent fetus • The fetus usually has a triploid karyotype and is defective • A partial mole has some hydropic villi, whereas other villi are essentially normal • Fetal vessels are seen in a partial mole • The trophoblastic tissue exhibits less striking hyperplasia

Incomplete mole • Patients display most of the pathologic and clinical features of patients with complete mole, although usually in less severe form • Partial moles are usually diagnosed later than are complete moles • Partial moles generally present as spontaneous or missed abortion • Usually is not detected before the spontaneous termination of pregnancy • No luteinizing cyst
Incomplete mole • Ultrasonography performed for other indications may indicate possible molar degeneration of the placenta associated with the developing fetus • An amniocentesis should be performed to determine whether karyotype of the coexisting fetus is normal • Uterine size is usually normal or small for dates • Preeclampsia usually occurs between 17 and 22 weeks (about 1 month later than with complete mole) • Partial moles rarely metastasize, and only rarely is there a need for chemotherapy

Pathologic features Complete mole Embryotic or fetal tissue - incomplete mole + Villus stromal edema diffuseed localized Trophoblastic hyperplasia diffuseed localized Villus outline regular irregular Villus stromal blood vessel Karyotype diploid + triploid or tetraploid

Hydatidiform mole / treatment • Evacuation • Suction evacuation followed by sharp curettage of the uterine cavity • Regardless of the duration of pregnancy • Intravenous oxytocin • To help stimulate uterine contractions and reduce blood loss • Most patient have an uncomplicated course in the postoperative period • Some require blood, fresh frozen plasma or platelet transfusion • Rarely a patient can experience acute respiratory distress from trophoblastic embolization or fluid overload

Hydatidiform mole / follow up • Weekly serum analysis of β-hcg • The levels should steadily decline to undetectable levels • Usually within 12 – 16 weeks Chemotherapy • Prophylactic chemotherapy is not indicated, because 90% have spontaneus remissions. • If the β-hcg levels plateau or rise at any time, chemotherapy should be initiated

INVASIVE MOLE

Invasive mole • Usually a locally invasive tumor • It constitutes about 5 – 10 % of all molar pregnancies • Most of those with persistent β-hcg levels after molar evacuation • The lesion may: • Penetrate the entire myometrium • Rupture through the uterus • Result in hemorrhage into the broad ligament or peritoneal cavity • Rarely is associated with metastases • Vagina, lungs • Brain (rarely)

Invasive mole / Clinical manifestation • irregular vaginal bleeding • uterine subinvolution • theca lutein cyst does not disappear after emptying uterus • abdominal pain • metastatic focus manifestation

Invasive mole / Diagnosis • history and clinical manifestation • successive measurement of HCG • ultrasound examination • X-ray and CT • histologic diagnosis

Invasive mole • Histologic confirmation of invasive mole is almost always made at the time of hysterectomy • Hysterectomy is usually performed • in patients with persistent β-hcg levels following evacuation of molar pregnancy • In patients with persistent titers of β-hcg despite chemotherapy who have no evidence of metastatic disease • Hysterectomy is usually curative

CHORIOCARCINOMA

Choriocarcinoma • The frankly malignant form of gestational trophoblastic disease • Genetic analysis of choriocarcinomas usually reveals aneuploidy or polyploidy • Typical for anaplastic carcinomas • Appears grossly as a vascular-appearing, irregular and „beefy” tumor • Often growing through the uterine wall • Metastatic lesions appear hemorrhagic and have consistency of currant jelly • Histological consist of sheets of malignant cytotrophoblast and syncytiotrophoblast with no identifiable villi

Choriocarcinoma • 50%gestational choriocarcinoma result from hydatidiform mole • Trophoblastic disease following a normal pregnancy is always choriocarcinoma • The tumor has a tendency to disseminate hematogenously, particularly to the lungs, vagina, brain, liver, kidneys and gastrointestinal tract • FIGO staging of gestational trophoblastic neoplasia

Choriocarcinoma / symptoms • Symptoms of metastatic disease • Vaginal bleeding • Uterine choriocarcinoma • Vaginal metastasis • Hemoptysis, cough, dyspnea • Result of lung metastasis • Headache, dizzy spells • Central nervous system metastases • Rectal bleeding, dark stools • Metastasis to gastrointestinal tract

Choriocarcinoma / signs • Uterine enlargement • Blood seen on examination with a speculum • Mass in vagina (metastatic tumor) • Acute abdomen • Rupture of uterus • Abdominal pain • Theca-lutein cyst • Neurologic signs • Partial weakness, paralysis, aphasia etc

Choriocarcinoma / diagnosis • Great imitator of the other diseases !!!! • May not be suspected • Unless it follows molar pregnancy • Screen for choriocarcinoma: β-hcg • Computer tomography (CT) • Pelvis • Abdomen • head • Cerebrospinal fluid β-hcg level • Ratio of serum to cerebrospinal fluid hcg levels of less than 40: 1 suggest central nervous system involvement • β subunit does not cross the blood-brain barrier readily

Clinical features / poor prognosis • Urinary β-hcg level > 100 000 IU/24 hr • Serum β-hcg level > 40 000 IU • Disease presents more than 4 months from the antecedent pregnancy • Metastasis to the brain or liver • Regardless of β-hcg titer or duration of disease • Prior failure to respond to single-agent chemotherapy • Choriocarcinoma after a full-term delivery

Choriocarcinoma / treatment • Chemotherapy • Methotrexate • Actinomycin D • Cyclophosphamide • Modified Bagshave regimen (EMA-CO) • Surgery • Hysterectomy • Pulmonary resection • Radiotherapy (in conjunction with chemotherapy) • Brain • liver

Choriocarcinoma / prognosis • 95 -100% of patients with GTN with good prognosis are cured • 50 – 70 % patients with poor diagnosis are cured • Most patient who die have brain or liver metastases • Causes of death: • Vaginal bleeding. • Haemoptysis. • Intraperitoneal hemorrhage. • Peritonitis. • Metastasis to the vital organs e. g, brain. • Pulmonary complications
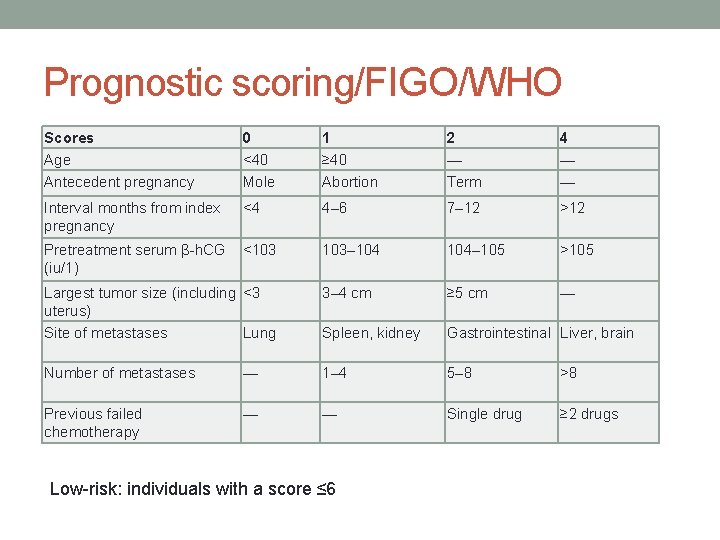
Prognostic scoring/FIGO/WHO Scores Age Antecedent pregnancy 0 <40 Mole 1 ≥ 40 Abortion 2 — Term 4 — — Interval months from index pregnancy <4 4– 6 7– 12 >12 Pretreatment serum β-h. CG (iu/1) <103 103– 104– 105 >105 Largest tumor size (including <3 uterus) Site of metastases Lung 3– 4 cm ≥ 5 cm — Spleen, kidney Gastrointestinal Liver, brain Number of metastases — 1– 4 5– 8 >8 Previous failed chemotherapy — — Single drug ≥ 2 drugs Low-risk: individuals with a score ≤ 6

Choriocarcinoma / follow up • serum hcg levels should be measured • once per week until 4 normal values are obtained. • once per month for 1 year. • Patients with poor prognosis should be checked monthly for 2 years after 3 -4 consecutive weekly normal serum hcg levels. • Levels should be checked every 3 months until 5 years • Patients should use a reliable method of contraception. • Advise not to be pregnant within 12 months after molar evacuation
- Slides: 37