Gestational Trophoblastic Disease GTD By Ahmed Refaat Abd

Gestational Trophoblastic Disease (GTD) By Ahmed Refaat Abd ELzaher Assistant Lecturer of Medical Oncology South Egypt Cancer Institute 2015

GTD Overview • Heterogeneous group of related lesions • Arise from abnormal proliferation of trophoblast of the placenta • Can follow any gestational event – abortion, miscarriage, ectopic, normal pregnancy • Unique because the maternal lesions arise from fetal (not maternal) tissue • Most GTD lesions produce (B-h. CG) • Can be cured even in the presence of widespread metastases

Overview Hydatidiform Mole: • Complete • Partial ** Benign Gestational Trophoblastic Neoplasia (GTN): • Persistent/Invasive Mole • Choriocarcinoma • Placental-Site Trophoblastic Tumor (PSTT) ** Malignant
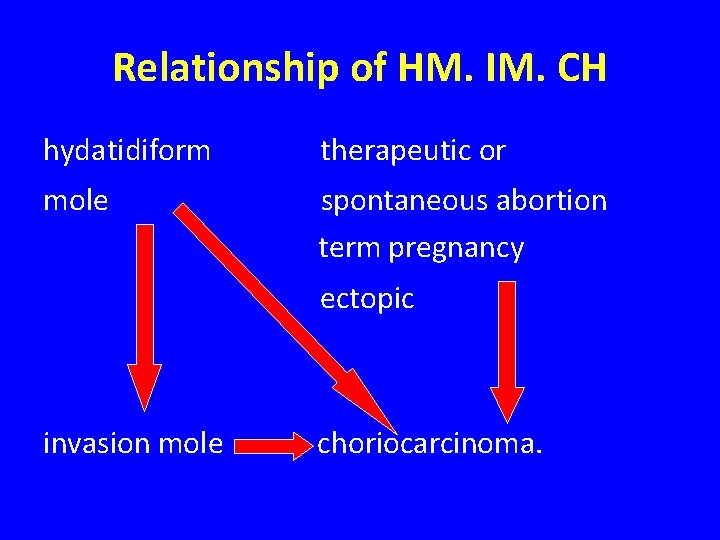
Relationship of HM. IM. CH hydatidiform therapeutic or mole spontaneous abortion term pregnancy ectopic invasion mole choriocarcinoma.

Hydatidiform mole

Hydatidiform Mole • North America: 0. 6 -1. 1 per 1000 pregnancies • Asia: 2 -10 per 1000 (3 x Western countries) • Difference possibly related low dietary intake of carotene (vitamin A deficiency) and animal fat • More common at reproductive extremes in age (>35 y or <20 y)

Hydatidiform Mole Risk Factors: • History of previous GTD – If one previous mole, 1% chance of recurrence (vs. 0. 1% in general population) – If 2 previous moles, risk of recurrence increases to 16 -28% • Smoking • Vitamin A deficiency • Blood type: – A or AB are at slightly higher risk than those with type B or O
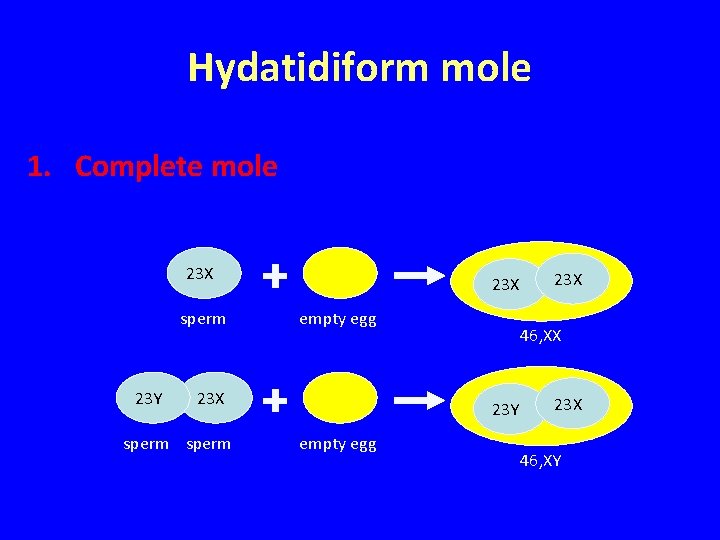
Hydatidiform mole 1. Complete mole 23 X sperm 23 Y 23 X empty egg 23 X sperm 46, XX 23 Y empty egg 23 X 46, XY

Hydatidiform mole 2. Partial mole 23 Y 23 X 23 X 23 Y sperm 23 X normal egg 69, XXY 23 X 23 X sperm 23 X Normal egg 69, XXX

Hydatidiform Mole Clinical Manifestations: • Vaginal bleeding (97%) /anemia • Enlarged uterus (size > dates) • Pelvic pain • Theca lutein cysts • Hyperemesis gravidarum • Hyperthyroidism • Preeclampsia <20 weeks gestation • Vaginal passage of hydropic vesicles • Partial mole usually presented as incomplete or missed abortion

Diagnosis • Complete : U/S usually very sensitive – generalized swelling (snow-storm ) • partial mole U/S may detect focal cystic spaces of varying diameter Diagnosis on histology of curettings
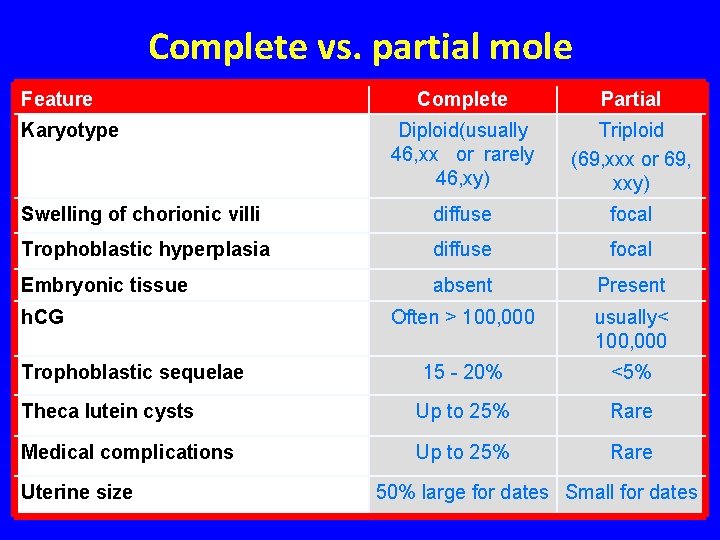

Complete vs. partial mole Feature Complete Partial Diploid(usually 46, xx or rarely 46, xy) Triploid (69, xxx or 69, xxy) Swelling of chorionic villi diffuse focal Trophoblastic hyperplasia diffuse focal Embryonic tissue absent Present Often > 100, 000 usually< 100, 000 15 - 20% <5% Theca lutein cysts Up to 25% Rare Medical complications Up to 25% Rare Karyotype h. CG Trophoblastic sequelae Uterine size 50% large for dates Small for dates

Hydatidiform Mole Treatment • Evaluate for coexisting conditions: - History and physical - CBC, coagulation profile, serum chemistry - thyroid function - blood type and cross match - chest radiography - pelvic ultrasonography • Evacuation of mole - Suction curettage - Hysterectomy if completed childbearing • If Rh negative, give rhogham

Hydatidiform Mole Treatment chemotherapy HM don’t need usually chemotherapy because HM is benign disease.

Follow-Up Care – Molar Pregnancy • 80% of patients cured by evacuation • Follow B-h. CG levels every two weeks until 3 consecutive tests negative • Then monthly B-h. CG every month for 6 -12 months • More than half of patients will have complete regression of h. CG to normal within 2 months of evacuation. • Avoid pregnancy for at least 6 months after first normal B-h. CG (oral contraceptive pills is preferable) • Subsequent Pregnancies: – Send placenta for pathology – Check B- h. CG 6 weeks postpartum

Prognosis • Complete mole has the latent risk of local invasion or telemetastasis • The high-risk factors includes – β-HCG>100000 IU/L – uterine size is > 20 weeks size. – the luteinizing cyst is >6 cm – If >40 years old, the risk of invasion and metastasis may be 37%, If >50 years old, the risk of invasion and metastasis may be 56%. – repeated mole: the morbidity of invasion and metastasis increase 3~4 times

Gestational Trophoblastic Neoplasia (GTN) • Persistent/Invasive Mole • Choriocarcinoma • Placental-Site Trophoblastic Tumor (PSTT) ** Malignant

Risk Factors for GTN After Mole • Preevacuation uterine size greater than gestationl age or larger than 20 weeks gestation • Theca-lutein cysts larger than 6 cm • Age > 40 years • Serum h. CG levels > 100, 000 m. IU/m. L • Previous hydatidiform mole

Invasive Mole • • Myometrial invasion by hydatidiform mole Formerly known as chorioadenoma destruens 1 in 15, 000 pregnancies 10 -17% of hydatidiform moles will progress to invasive moles

Persistent Mole Definition of persistent molar disease and need for chemotherapy (at least one of the following): – B-h. CG plateau for ≥ 4 values for ≥ 3 weeks – B-h. CG increase of ≥ 10% for ≥ 3 values for ≥ 2 weeks – B-h. CG persistence 6 months after molar evacuation – Histopathologic diagnosis of choriocarcinoma – Presence of metastatic disease

Choriocarcinoma • • • Most aggressive type of GTN Abnormal trophoblastic hyperplasia Absence of chorionic villi Direct invasion of myometrium Most often develops from a complete hydatidiform mole • Vascular spread to distant sites: – Lungs – Brain – Liver – Pelvis and vagina – Spleen, intestines, and kidney

Choriocarcinoma • May come from any type of pregnancy - 25% follow abortion or tubal pregnancy - 25% with term gestation - 50% from hydatidiform moles • 2 -3% of moles progress to choriocarcinoma • Incidence 1 in 40, 000 pregnancies – Rarely, choriocarcinomas can develop in other parts of the body in both men and women. These are not related to pregnancy as ovaries and testicles • Nongestational choriocarcinoma tends to be less responsive to chemotherapy and has a less favorable prognosis than the gestational variant

Placental-Site Trophoblastic Tumor (PSTT) • Originate from intermediate cytotrophoblast cells • Secrete human placental lactogen (h. PL) • B-h. CG often normal • Less vascular invasion, necrosis and hemorrhage than choriocarcinoma • Lymphatic spread • Arise months to years after term pregnancy but can occur after spontaneous abortion or molar pregnancy

Placental-Site Trophoblastic Tumor (PSTT) • Most common symptom is vaginal bleeding • Tend to: - Remain in uterus - Disseminate late - Produce low levels of B-h. CG compared to other GTN - Be resistant to chemotherapy (treat with surgery)

Signs & Symptoms GTN • Continued uterine bleeding, uterine perforation, enlarged irregular uterus, persistent bilateral ovarian enlargement • From metastatic lesions: abdominal pain, hemoptysis, melena, increased intracranial pressure (headaches, seizures, hemiplegia), dyspnea, cough, chest pain

Diagnosis of GTN • Increase or plateau in B-h. CG after molar pregnancy • Pathologic diagnosis by D&C or biopsy of metastatic lesions • WARNING: biopsy of metastatic lesions can result in massive hemorrhage • Metastatic workup: CXR (or CT chest), CT abdomen/pelvis +/- CT/MR of brain

Classification & Staging of GTD • FIGO Staging – Describes anatomic distribution of disease • World Health Organization (WHO) Scoring Index – Describes prognosis
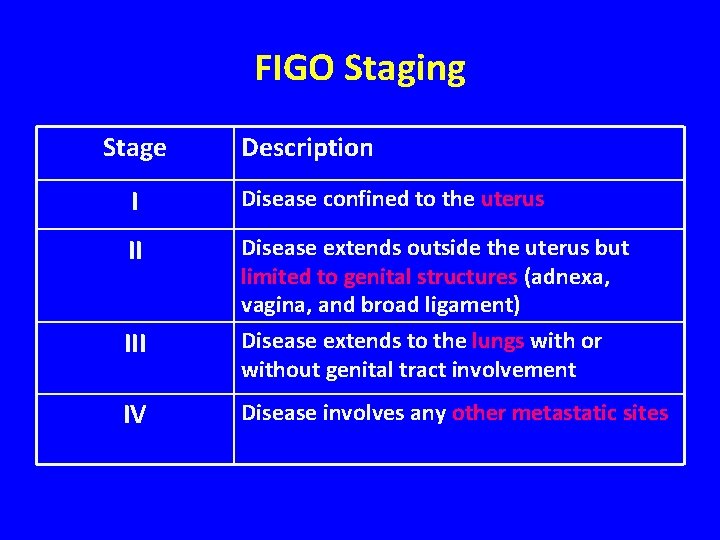
FIGO Staging Stage Description I Disease confined to the uterus II Disease extends outside the uterus but limited to genital structures (adnexa, vagina, and broad ligament) III Disease extends to the lungs with or without genital tract involvement IV Disease involves any other metastatic sites
The World Health Organization (WHO) scoring system for GTD
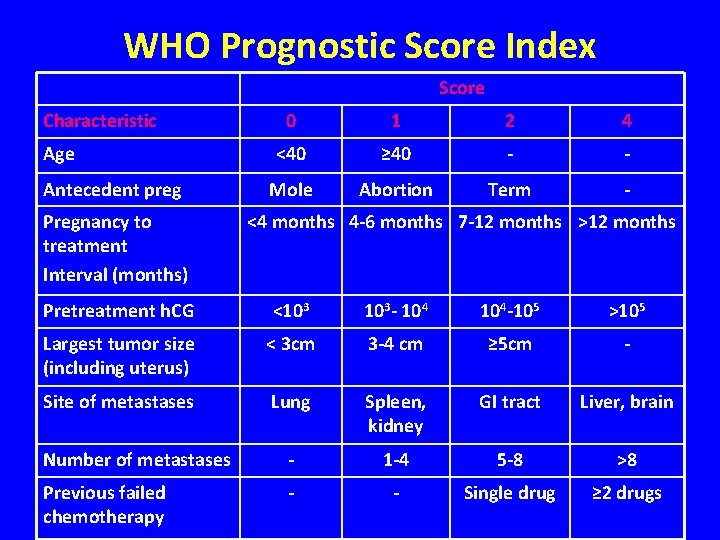
WHO Prognostic Score Index Score Characteristic Age Antecedent preg Pregnancy to treatment Interval (months) 0 1 2 4 <40 ≥ 40 - - Mole Abortion Term - <4 months 4 -6 months 7 -12 months >12 months Pretreatment h. CG <103 103 - 104 -105 >105 Largest tumor size (including uterus) < 3 cm 3 -4 cm ≥ 5 cm - Site of metastases Lung Spleen, kidney GI tract Liver, brain Number of metastases - 1 -4 5 -8 >8 Previous failed chemotherapy - - Single drug ≥ 2 drugs

Therapy for GTN • Single agent therapy for nonmetastatic (stage I) or low-risk metastatic (stage II and III) with score <7 survival rates ~ 100% • Combination chemotherapy +/- radiation and/or surgery for high-risk metastatic disease with score ≥ 7

Therapy: Nonmetastatic GTN • Single-agent with either methotrexate or dactinomycin • Chemotherapy continued until h. CG values normal and then 2 -3 cycles beyond • Change to alternative single-agent for h. CG plateaus above normal or toxicities • If significant elevation of h. CG or new metastases, switch to multiagent • 85 -90% cured with initial regimen, <5% will require hysterectomy for cure

Therapy: Low-risk Metastatic GTN • Low-risk metastatic disease can be treated with single-agent therapy with 5 -day regimens • Cure rates ~100% but 30 -50% will be develop resistance to first agent • If resistance to sequential single-agent chemotherapy (5 -10% of patients), switch to multiagent chemotherapy

Therapy: High-risk Metastatic GTN • Stage IV • Stage II/III with score > 7 • Disease refractory to single-agent chemotherapy Combination Chemotherapy: • EMACO: – Day 1: Etoposide, Methotrexate and Dactinomycin – Day 8: Cyclophosphamide and Vincristine (Oncovorin) – Repeat q 2 weeks until remission – Continue for at least 2 -3 cycles beyond first normal h. CG • MAC (Methotrexate, Dactinomycin, Cyclophosphamide) • EMA/EP – EMA + Etoposide and Cisplatin

Metastatic Gestational Trophoblastic Tumors • Surgery – It is indicated for tumor resistant to chemotherapy and single metastases persisting despite chemotherapy. • RT – RT, in combination with chemotherapy, is clearly indicated for the primary management of patients with brain metastases.

PSTT Therapy • Hysterectomy • Chemotherapy for metastatic disease or nonmetastatic disease with poor prognosis: - Interval from index pregnancy > 2 years - Deep myometrial invasion - Tumor necrosis - Mitotic count > 6 per 10 high-power fields • Survival rates: – ~100% for nonmetastatic disease – 50 -60% for metastatic disease

Follow-up Care • After completion of chemotherapy, follow serial h. CG every 2 weeks for three months, then monthly for one year • Physical examinations every 6 -12 months and imaging as indicated

Reproductive Performance • Most women resume normal ovarian function • Women who undergo chemotherapy are advised not to conceive for one year after completion of treatment • No increase risk of stillbirths, abortions, congenital anomalies, prematurity, or major obstetric complications

False Positive Serum h. CG • Phantom h. CG syndrome/ phantom choriocarcinoma • 3 -4% of healthy individuals have human-antimouse antibodies that can mimic h. CG immunoreactivity • To verify: – Urine h. CG should be negative – Should not show parallel decrease with serial dilutions – Test at national B-h. CG reference lab

Summary • Hydatidiform mole is a benign condition, 80% cured with suction D&C • Malignant GTN: – Persistent or invasive mole – Choriocarcinoma – PSTT • WHO score > 7 represents high-risk disease • GTN very sensitive to chemotherapy

Thank You For Your Time
- Slides: 41