GESTATIONAL DIABETES MELLITUS A Comprehensive Look By Jeanne

GESTATIONAL DIABETES MELLITUS A Comprehensive Look By Jeanne Laird

GESTATIONAL DIABETES MELLITUS WHAT IS IT v. Gestational diabetes is a type of diabetes that develops during pregnancy v. With diabetes, the body cannot properly use sugars and starches (carbohydrates) for energy. v. At meals and snacks, the food we eat consists of proteins, carbohydrates and fats. Carbohydrates cannot be used for energy because they cannot get into the cell. v. During digestion, your body breaks down carbohydrates into glucose. The glucose cannot get into the cell and therefore accumulates in the blood stream causing high blood sugar.

WHICH FOODS CONTAIN CARBOHYDRATES Breads (including buns, muffins, bagels, biscuits, rolls, croissants, pizza crust, tortillas and taco shells) Cereals Pasta Rice Grains Potatoes Corn Peas Fruit Milk and yogurt Sweets such as: Jams and jellies Honey, syrups and table sugar Cakes, pies, cookies and pastries Donuts Candy Ice cream and other frozen desserts Certain condiments

WHO IS AT RISK? Risk factors that may increase your chances of experiencing gestational diabetes are: v. A family history of diabetes v. Previous delivery of a baby weighing more than 9 lbs. v. Previously having gestational diabetes mellitus v. Overweight at time of conception (a BMI > 30). v. Advanced maternal age (women over 40 have 6 X increased risk of developing GDM than younger women. ) v. Are Asian, African-American, Hispanic, Native American or Asian Pacific (these ethnicities have a higher risk of developing Diabetes and Gestational diabetes mellitus.

v. Hormones produced during pregnancy can interfere with a hormone called insulin. v. Insulin is the hormone that enables glucose from the food we eat to get into the cells so the cells can use it for fuel. v. Insulin “unlocks” the cell and allows glucose to enter. v. Just like a car needs fuel to run, our cells need glucose to grow, repair and do cellular work. v. The main fuel your body runs on is glucose; your brain needs a constant supply of glucose to carry out all of its functions and your muscles use glucose for movement and activity. v. These pregnancy hormones are at their highest level between 24 and 28 weeks of pregnancy. v. Pregnant woman are screened for gestational diabetes between 24 and 28 weeks of pregnancy. v WHAT CAUSES GESTATIONAL

COMPLICATIONS OF GDM DURING PREGNANCY Mothers with gestational diabetes may experience episodes of high blood sugar; And they also may experience episodes of low blood sugar. Both are serious and must be addressed immediately.
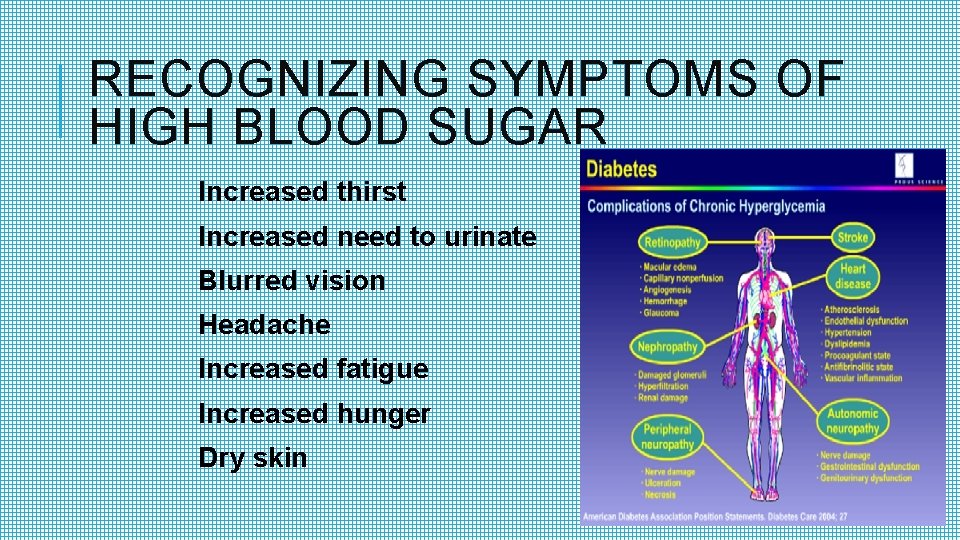
RECOGNIZING SYMPTOMS OF HIGH BLOOD SUGAR Increased thirst Increased need to urinate Blurred vision Headache Increased fatigue Increased hunger Dry skin

TREATING HIGH BLOOD SUGAR If you experience symptoms of high blood sugar First check your blood sugar If blood sugar is high, start drinking water. Continue drinking water to “dilute” the high blood sugar. Go for a walk (if not experiencing extreme fatigue or blurred vision). If you are on insulin, you may have to take an additional dose at this time to correct for the elevated blood sugar.
RECOGNIZING SYMPTOMS OF LOW BLOOD SUGAR Shakiness or tingling in the hands and feet Dizziness Increased hunger Weakness Confusion Irritability Headache Increased heartbeat Cold, clammy skin Breaking out in a sweat

TREATING LOW BLOOD SUGAR (RULE OF 15) Low blood sugar can be very dangerous and must be addressed immediately. If experiencing symptoms of low blood sugar: Immediately check your blood sugar if possible If blood sugar is below 60 Treat with 15 grams of a carbohydrate such as 4 oz. of juice or pop, 8 oz. of skim milk, a 15 gram glucose gel, 4 -5 glucose tablests, a tablespoon of honey, table sugar or agave nectar. • Wait 15 minutes and check blood sugar again. • If still below 60, have another 15 gram carbohydrate serving of one of the above mentioned options. • Wait another 15 minutes. Check blood sugar levels again. • If above 60, have a 15 gram carbohydrate snack with some protein to stabilize blood sugar. • If blood sugar still below 60, call 911.

GDM-WHAT ARE THE RISKS TO MOM AND BABY? For baby- Macrosomia and hypoglycemia v. Macrosomia is a baby of large birth weight. Birth weights of > 9 lbs Baby grows larger and faster. In macrosomia, a normal size baby may still be premature in development. In some cases, a larger birth weight baby may require a cesarean section delivery. v. Hypoglycemia- Low blood sugar After birth, babies exposed to high levels of glucose during gestation may experience low blood sugar, as their pancreas is still producing large levels of insulin to make up for the mother’s lack of insulin. This can cause glucose levels to suddenly drop in newborn babies. As a result, physicians normally check baby’s blood sugar at birth and several times thereafter.
WHEN MOM’S BLOOD SUGAR IS HIGH, SO IS BABY’S BLOOD SUGAR Excess blood sugar causes your baby to grow larger and faster than normal A large baby does not mean a fully developed and mature baby. GGG GG

GDM-WHAT ARE THE RISKS TO MOM AND BABY? v. In addition, larger babies delivered vaginally or more at risk of injury during delivery. v. With gestational diabetes, your baby is at increased risk of breathing problems and jaundice after birth. v. Babies born to mom’s with uncontrolled GDM are at higher risk of childhood obesity, developmental problems and developing diabetes themselves later in life.

GDM-WHAT ARE THE RISKS TO MOM AND BABY? o. The risks to mom include developing type 2 diabetes later in life o. Developing gestational diabetes mellitus with subsequent pregnancies o. High blood pressure during your pregnancy o. Caesarean section delivery o. Complications during delivery o. Pre eclampsia and eclampsia, life threatening conditions at time of delilvery

MANAGEMENT OF GESTATIONAL DIABETES MELLITUS: MONITORING Diabetes can be managed and controlled by following the five following steps: YOUR BLOOD SUGAR 1. Checking blood sugar first thing in the morning and two hours after breakfast, lunch and dinner. 2. Exercising 4 -5 times per week, 20 to 30 minutes per day. 3. Taking insulin or diabetes oral medication if recommended by your doctor 4. Following a special meal plan 5. Checking for ketones in your urine

CHECKING YOUR BLOOD GLUCOSE Checking your blood glucose (self blood glucose monitoring) is an essential part of managing your diabetes. There are several glucose monitors (glucometers) available for monitoring blood glucose levels. Check with your doctor, diabetes educator and your healthcare coverage to see which glucometer is right for you. It is a recommended that blood glucose levels be checked upon waking and two hours after each meal. Keep a log book: it is important to log all your blood glucose readings Keeping tract of glucose readings enables you and your healthcare team to identify trends throughout the day when blood sugar levels may run high or low.

TESTING FOR KETONES Ketones are particles that are produced when the body cannot use glucose for fuel and therefore begins to breakdown fat for fuel. When large amounts of fat are broken down and used for fuel, ketones form and can accumulate in the blood. Ketones are acidic and can cause your blood to become acidic. Ketones can spill into the urine when: Your blood glucose is out of control You are not eating enough carbohydrates You skipped a meal You are not taking in enough calories A 10 hour span between meals has occurred (ex. bedtime and breakfast)

MONITORING KETONES When ketones accumulate in the blood they can cause a condition called ketosis, which can be harmful to your baby. Ketones should be checked First thing in the morning When you are sick When you have not eaten enough carbohydrates or calories When your blood glucose reading is high Your healthcare team may recommend checking for ketones every morning upon waking. There should be no ketones in your urine. Any presence of ketones should be reported to your doctor.

EXERCISE: THE INVISIBLE INSULIN Exercise is an essential component of managing your diabetes. Exercise can help keep glucose levels within a healthy range. Exercise, like insulin, helps get glucose out of the blood stream and into the cells. (Which is why it is nicknamed “invisible insulin. ”) The best time to exercise is right after a meal when blood sugar levels are the highest. In order to reap the benefits of the insulin-like effect of exercise, it is recommended to exercise at least 4 -5 times per week for at least 20 -30 minutes. Exercise does not need to be done all at one time, 2 -15 minute walks or 310 minute walks will still produce benefits.

MEAL PLAN Healthy food choices Small, frequent meals throughout the day Portion control (plate method, carb counting) Meal/snack timing ◦ Avoid skipping meals ◦ Eat a bedtime snack

MEAL PLAN Carb intake affects blood sugar ◦ Limit excess sugars ◦ May need less carbs at breakfast ◦ Low Glycemic Index (GI) foods reduce after meal hyperglycemia and rate of LGA babies ◦ If on insulin, carb quantity and distribution dependent on insulin requirements of pregnancy Keep food records Teach label reading

CONSTANT CARBS Breakfast Lunch and Dinner Snacks ◦ 30 grams carbs ◦ Discourage juice ◦ Encourage lean protein and whole grains ◦ 45 to 60 grams carbs ◦ Based on clients schedule ◦ 15 - 20 grams carbs ◦ Recommend HS (before bed) snack for all

Goals for Managing Gestational Diabetes Mellitus Medical nutrition therapy for pregnancy Maintain normal blood glucose levels Adequate weight gain (not too much, not too little) Adequate calories and nutrition for maternal and fetal well-being. Iron: 30 mg/day Calcium: 1200 mg/day Folate: 400 ug/day Caffeine: < 300 mg/day Alcohol: avoid
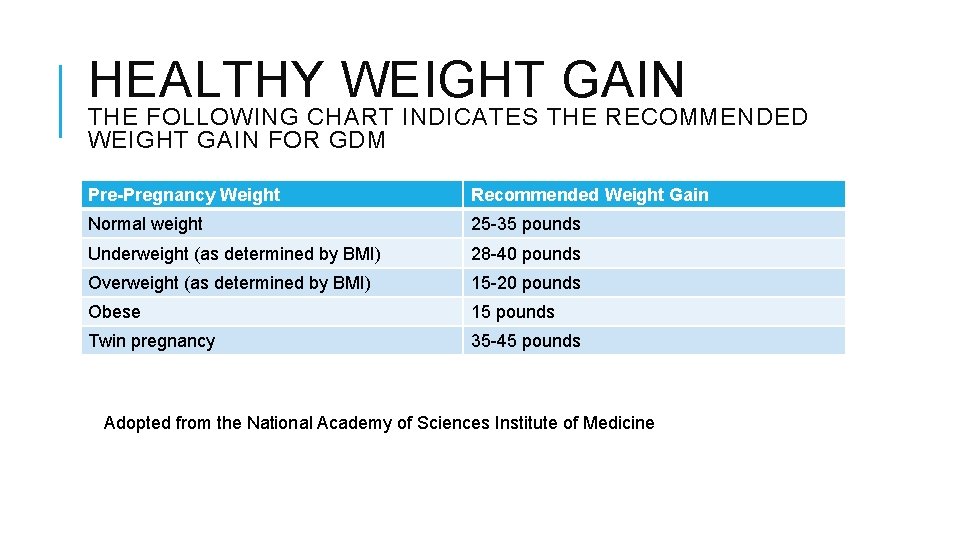
HEALTHY WEIGHT GAIN THE FOLLOWING CHART INDICATES THE RECOMMENDED WEIGHT GAIN FOR GDM Pre-Pregnancy Weight Recommended Weight Gain Normal weight 25 -35 pounds Underweight (as determined by BMI) 28 -40 pounds Overweight (as determined by BMI) 15 -20 pounds Obese 15 pounds Twin pregnancy 35 -45 pounds Adopted from the National Academy of Sciences Institute of Medicine

ADDITIONAL QUESTIONS YOU MAY HAVE

CAFFEINE AND PREGNANCY v. Here are the facts: Caffeine is a stimulant that increases heartrate and blood pressure, not only in you, but also in your baby. v. Caffeine is a diuretic which can cause losses in body fluids and lead to dehydration. v. Caffeine crosses the placenta where it is difficult for an unborn baby to metabolize. This can lead to abnormal sleep patterns and movement. v. Better to play it safe during pregnancy and limit caffeine consumption to no more than 150 mg or less per day.

Check out the caffeine content: Dunkin’ Donuts Coffee with Turbo Shot (20 oz) 436 mg Starbucks Coffee Venti (20 oz) 415 mg Starbucks House Blend Coffee (16 oz) 259 mg Dunkin’ Donuts Regular Coffee (14 oz) 178 mg 7 Eleven Big Gulp Coca-Cola (32 oz) 92 mg Red Bull (8. 4 oz) 80 mg Ben & Jerry’s Coffee Buzz Ice Cream(8 oz) 72 mg Black tea (8 oz) 30 -80 mg] Green tea (8 oz) 35 -60 mg Mountain Dew (12 oz) 54 mg Dr. Pepper (12 oz) 37 mg Coca Cola (12 oz) 35 mg Baker’s chocolate (1 oz) 26 mg Excedrin (per capsule) 65 mg http: //www. cspinet. org/new/cafchart. htm

SWEETENERS The following sweeteners have been approved by the FDA for use during pregnancy: Stevia Sucralose (Splenda) Acesulfame K (Sunnett) Aspartame (Equal and Nutrasweet) Stevia and Sucralose are your best bet, as Acesulfame K and Aspartame, as well as Saccharin (not recommended) cross the placenta. Sugar alcohols are also safe, but used in large quantity may cause gas, bloating and diarrhea in some individuals.

FOOD SAFETY DURING PREGNANCY q. Egg yolks must be cooked thoroughly, no soft yolks q. Limit seafood, especially canned tuna and crustaceans q. Avoid large predator fish such as swordfish, king mackerel, ahi tuna, orange roughie and shark. These fish all contain high levels of mercury q. Avoid lunchmeats and soft unpasteurized cheeses q. Only consume dairy products that are pasteurized

AFTER DELIVERY After delivery, your physician will check your babies blood sugar to detect low blood sugar and treat it accordingly. Six weeks after delivery you also should have your blood sugar checked to ensure it has returned to normal. Most often the blood sugar returns to normal after delivery of those woman who have experienced GDM. Due to the fact that you are at a higher risk of becoming a diabetic, it is advised you have a glucose tolerance test yearly.

• Follow up BG testing 6 – 12 weeks using a test other than an A 1 C Normal Pre-diabetes Diabetes Fasting < 100 - 125 > 126 2 hrs pp (75 g OGTT) < 140 – 199 > 200 Follow-up Every 1 -3 yrs Annually Immediately

DIABETES MELLITUS PREVENTION PROGRAM The Riverside Diabetes Wellness Clinic would like to invite you to attend our Diabetes Prevention program. After delivery, consider taking proactive steps to decrease the likelihood of developing diabetes mellitus later in life. The Diabetes Prevention Program takes place in a small group setting and provides support, suggestions and an interactive curriculum. If interested, please contact RDWC for more information.

SOURCES Diabetes and Pregnancy: Gestational Diabetes. U. S. Department of Health and Human Services Centers for Disease Control and Prevention BD Getting Started: Gestational Diabetes. Beckson, Dickinson and Company Gestational Diabetes. Cornerstones 4 Care a trademark of Novo Nordisk
- Slides: 33