George Eliot Hospital NHS Trust Draft Business Plan

George Eliot Hospital NHS Trust Draft Business Plan 2013/14 – 2015/16 Version 3. 3 27 th March 2013
Version control Version No. Date Author Change 1. 0 02/01/13 CB 1 st draft to share with Execs as basis for agreeing structure/content 1. 1 11/01/13 CB Draft including feedback from discussion at Board Development and Hospital Management Board; shared for final feedback 1. 2 16/01/13 CB Further updates included 1. 3 22/01/13 CB Further updates included, CIP amended, presented to Exec Team 1. 4 25/01/13 CB Final draft for 1 st cut submission 2. 0 26/02/13 CB Final draft for 2 nd cut submission 3. 1 10/03/13 CB Updated draft requiring input from Exec Team 3. 2 12/03/13 CB Updated draft for discussion at Board Development 13/03/13 3. 3 20/03/13 CB Updated draft for board approval
Glossary CIP Cost Improvement Programme: initiatives to secure cost savings or increased profitability from clinical services provided by the Trust to offset net reduction in tariffs CQUIN Clinical Quality & Innovation: quality improvements funded on achievement rather than through tariffs for healthcare activity DTOC Delayed transfers of care EOLC End of life care FRR Financial Risk Rating: used by Monitor to measure financial strength GRR Governance Risk Rating: used by Monitor to measure overall performance against key targets HSMR Hospital Standardised Mortality Rate: index produced monthly by Dr Foster comparing actual and expected deaths in hospital I&E Income and expenditure LOS Length of stay LUCC Leicester Urgent Care Centre (Primary care centre on Leicester Royal Infirmary site) OBC Outline Business Case PN Performance Notice QIPP Quality, Innovation, Productivity and Prevention: commissioner programme to increase overall efficiency and effectiveness from financial resource allocations SARC Sexual Assault Referral Centre SHMI Standardised Hospital Mortality Index: index published quarterly by DH, similar to HSMR but does not take palliative care into account and includes deaths up to 30 days after discharge from hospital SSF Securing a Sustainable Future: Trust’s project to procure a strategic partner Track & trigger Clinical information system prompting and recording information about patient care, observations etc

Contents • Overarching presentation • Attachments: – – – Improvement priorities (Annex A) Development priorities (Annex B) Performance and activity plan (Annex C) Workforce plan (Annex D) Finance schedules (Annex E) Planning checklist (Annex F)

Introduction • • • This plan has been prepared at a time of considerable change, not only for the Trust but also the NHS as a whole. In September 2011, we made the decision that it would not be possible to continue with the objective of becoming an independent Foundation Trust and that we would seek a strategic partner with which to achieve our ambitions to secure the widest range of clinically and financially sustainable services for the local community. We developed our proposed procurement process in May 2012 and this was approved by the SHA in December. It is disappointing that we have not been able to initiate that process while further consideration is given to it by the TDA and Treasury. The Trust is ready to start the process at any time. This may therefore be the last plan that we produce independently, since the next plan will reflect the proposals put forward by our preferred partner. But this plan is not a holding position. There is much that we need to do to maintain the momentum in improving services for our community. Not least, this plan is written with the recommendations of the Francis Report firmly in mind. We will shortly be publishing our formal response to that report and the key actions that we will take will be integrated with our existing Mortality Action Plan. This plan will also be updated to take account of any additional recommendations that may arise following the review of services to be conducted by Sir Bruce Keogh and his team. The board remains committed to finding the best possible future for the Trust measured against the needs of patients. We will implement this plan and conduct our search for a strategic partner in an open and transparent way to ensure the best possible outcome.

Our Vision is to EXCEL At Patient Care and we will continue to implement our core value pledges and strive to achieve our strategic objectives. These are: • Our Core Value Pledges: • • • Effective Open Communication EXcellence in All That We Do Challenge but Support Expect Respect and Dignity Local Healthcare that Inspires Confidence • Our Strategic Objectives: • • • 1. Constantly deliver high quality care in a safe environment 2. Enhance patient experience by providing local care tailored to the individual needs of the patient. 3. Develop partnership arrangements to promote and deliver a comprehensive range of Value for Money Integrated Services to protect and improve the health of the local community. 4. Empower, develop and support our staff to encourage positive leadership at every level. 5. Maintain financial stability, hit all agreed targets and satisfy our regulators

2012/13 has been a year of considerable achievement but we remain financially challenged. In summary, the main headlines are: • • Annual targets achieved: A&E 4 hours (but failed in Q 4), C Difficile, 18 weeks RTT, Cancer waiting times (except for the 62 day waiting time target) Mortality index: SHMI reduced from 1. 23 to 1. 12 Community services: Dental waiting times reduced; LUCC positive CQC visit; integration of Coventry and Warwickshire TB Service; exceeded Warwickshire Stop Smoking target. Performance improvement required: Cancer 62 day waiting time, cancelled operations, patient satisfaction (Friends & Family Test) Financial outturn: £ 5 m support funding; forecast break-even; CIP 6%; high medical agency/locum staffing ratio; FRR = 3 after financial support but 1 without support. Acute quality indicators: last Grade 4 pressure ulcer Aug 11, Grade 3 Nov 11; CQC visit November – no recommendations; Major projects progressed: Securing a Sustainable Future OBC approved, procurement ready to begin; new Paediatrics clinical model being implemented; awarded Lorenzo pilot site; SARC implemented

Planning context • • • The Trust Board is leading a process to identify a strategic partner that will result either in an acquisition by an NHS organisation or another organisational model. The business plan for 2013/14 aims to ensure that the Trust is attractive as possible so that we encourage a genuine competition that brings forward innovative solutions. The Trust has been an outlier in terms of mortality indicators, but over the past year significant reduction has been achieved. We have also received significant assurance about quality and patient safety from external inspections and peer reviews. The Trust has an improving foundation on which to rebuild its reputation. Nevertheless, the publication of the Francis Report has further increased the need to provide assurance about the quality and safety of services. The Trust continues to be financially challenged and will need continuing financial support until a new organisational model is implemented. However, it has opportunities both to make further efficiency improvements without compromising quality and patient safety, and also to regain market share lost over recent years. In particular, we have a lower proportion of elective activity than similar Trusts and this impacts on both our overall quality and financial position. The Trust is operating in a financially challenged local health economy. Historically, health services in northern Warwickshire have been under-funded and there has been no relative change in the allocation of resources for local commissioners for 2013/14. We must therefore work closely with commissioners and other providers to improve efficiency across the whole system within the financial constraints that exist. The financial gap reflected in this plan is partly a consequence of the Trust’s underlying position but also partly a reflection that commissioners are not able to offer sufficient funding to support the transformational change that we are jointly implementing.
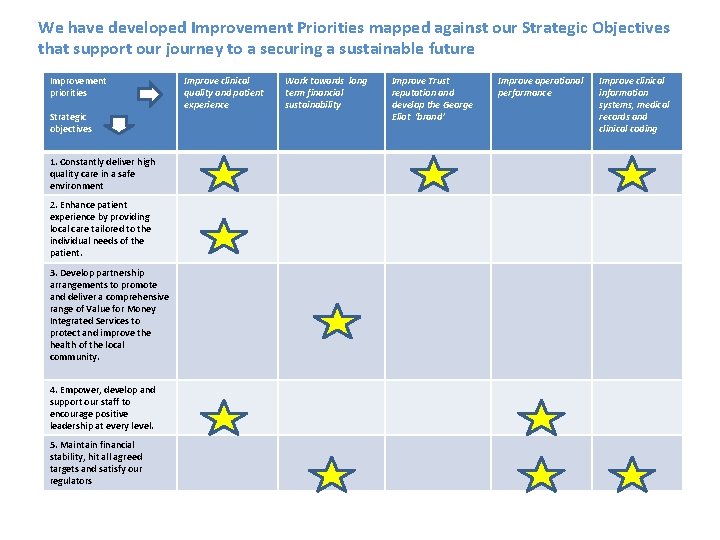
We have developed Improvement Priorities mapped against our Strategic Objectives that support our journey to a securing a sustainable future Improvement priorities Strategic objectives 1. Constantly deliver high quality care in a safe environment 2. Enhance patient experience by providing local care tailored to the individual needs of the patient. 3. Develop partnership arrangements to promote and deliver a comprehensive range of Value for Money Integrated Services to protect and improve the health of the local community. 4. Empower, develop and support our staff to encourage positive leadership at every level. 5. Maintain financial stability, hit all agreed targets and satisfy our regulators Improve clinical quality and patient experience Work towards long term financial sustainability Improve Trust reputation and develop the George Eliot ‘brand’ Improve operational performance Improve clinical information systems, medical records and clinical coding
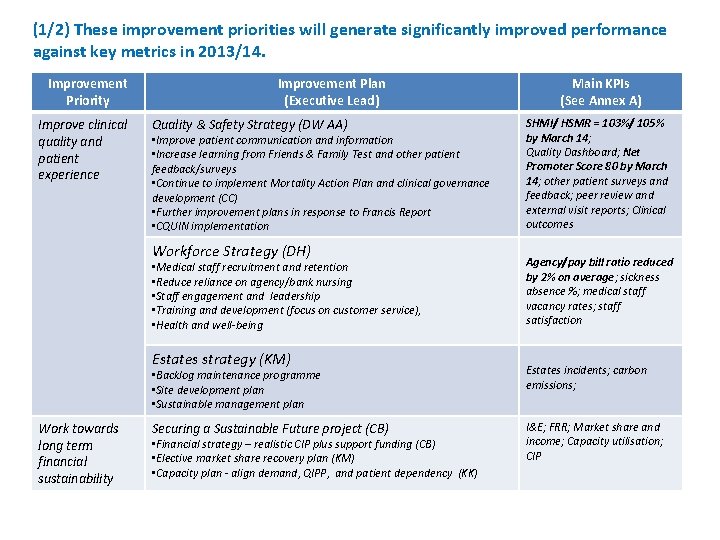
(1/2) These improvement priorities will generate significantly improved performance against key metrics in 2013/14. Improvement Priority Improve clinical quality and patient experience Improvement Plan (Executive Lead) Quality & Safety Strategy (DW AA) • Improve patient communication and information • Increase learning from Friends & Family Test and other patient feedback/surveys • Continue to implement Mortality Action Plan and clinical governance development (CC) • Further improvement plans in response to Francis Report • CQUIN implementation Workforce Strategy (DH) • Medical staff recruitment and retention • Reduce reliance on agency/bank nursing • Staff engagement and leadership • Training and development (focus on customer service), • Health and well-being Estates strategy (KM) Work towards long term financial sustainability Main KPIs (See Annex A) SHMI/ HSMR = 103%/ 105% by March 14; Quality Dashboard; Net Promoter Score 80 by March 14; other patient surveys and feedback; peer review and external visit reports; Clinical outcomes Agency/pay bill ratio reduced by 2% on average; sickness absence %; medical staff vacancy rates; staff satisfaction • Backlog maintenance programme • Site development plan • Sustainable management plan Estates incidents; carbon emissions; Securing a Sustainable Future project (CB) I&E; FRR; Market share and income; Capacity utilisation; CIP • Financial strategy – realistic CIP plus support funding (CB) • Elective market share recovery plan (KM) • Capacity plan - align demand, QIPP, and patient dependency (KK)
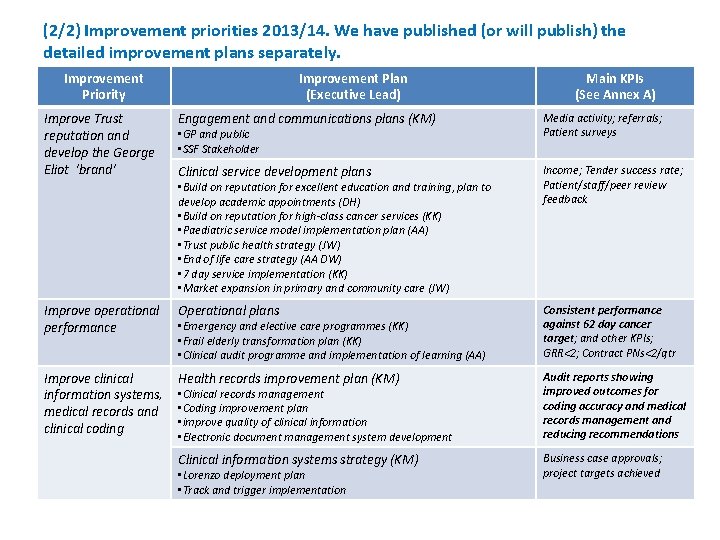
(2/2) Improvement priorities 2013/14. We have published (or will publish) the detailed improvement plans separately. Improvement Priority Improve Trust reputation and develop the George Eliot ‘brand’ Improvement Plan (Executive Lead) Main KPIs (See Annex A) Engagement and communications plans (KM) Media activity; referrals; Patient surveys Clinical service development plans Income; Tender success rate; Patient/staff/peer review feedback Improve operational performance Operational plans Consistent performance against 62 day cancer target; and other KPIs; GRR<2; Contract PNs<2/qtr Improve clinical information systems, medical records and clinical coding Health records improvement plan (KM) Audit reports showing improved outcomes for coding accuracy and medical records management and reducing recommendations Clinical information systems strategy (KM) Business case approvals; project targets achieved • GP and public • SSF Stakeholder • Build on reputation for excellent education and training, plan to develop academic appointments (DH) • Build on reputation for high-class cancer services (KK) • Paediatric service model implementation plan (AA) • Trust public health strategy (JW) • End of life care strategy (AA DW) • 7 day service implementation (KK) • Market expansion in primary and community care (JW) • Emergency and elective care programmes (KK) • Frail elderly transformation plan (KK) • Clinical audit programme and implementation of learning (AA) • Clinical records management • Coding improvement plan • improve quality of clinical information • Electronic document management system development • Lorenzo deployment plan • Track and trigger implementation
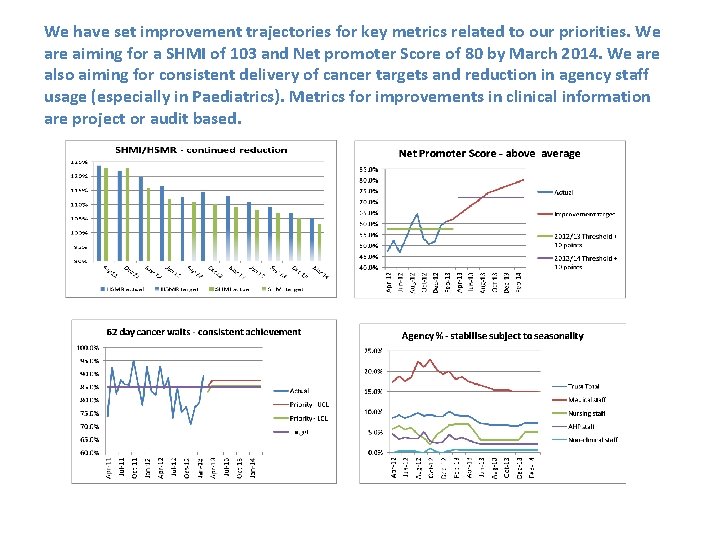
We have set improvement trajectories for key metrics related to our priorities. We are aiming for a SHMI of 103 and Net promoter Score of 80 by March 2014. We are also aiming for consistent delivery of cancer targets and reduction in agency staff usage (especially in Paediatrics). Metrics for improvements in clinical information are project or audit based.

Our SSF project will determine the long-term future of the organisation – either being acquired by another NHS organisation or continuing independently under another organisational model. The key drivers of success in this project will be: – Timely commencement of the procurement process – Stakeholder and staff engagement and communication. This will be integrated with the overall plan to enhance the reputation of the Trust and build the George Eliot ‘brand’. – Management of change and uncertainty. We will continue to invest in and develop services and infrastructure for the future where this does not conflict with proposals being put forward from potential partners. This will give assurance to staff and patients about the continuation of services. – Working closely with the TDA, DH and Treasury to ensure that the risk of delays in the approvals process is minimised. – Ensuring a tightly managed process guided by our professional advisers but involving stakeholders in the evaluation process that will inform the board’s decision on the preferred partner. – Meeting the targets in this plan so that potential partners are confident in the performance of the business for which they take responsibility. The indicative timescale for the project is summarised on the following slide. We are currently awaiting approval to begin the procurement process. Based on the current position, we have assumed that the new organisational form will now commence from January 2015.
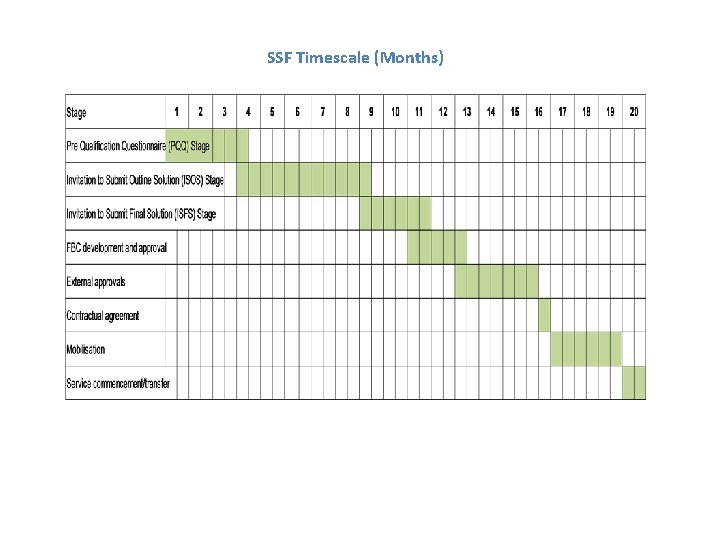
SSF Timescale (Months)
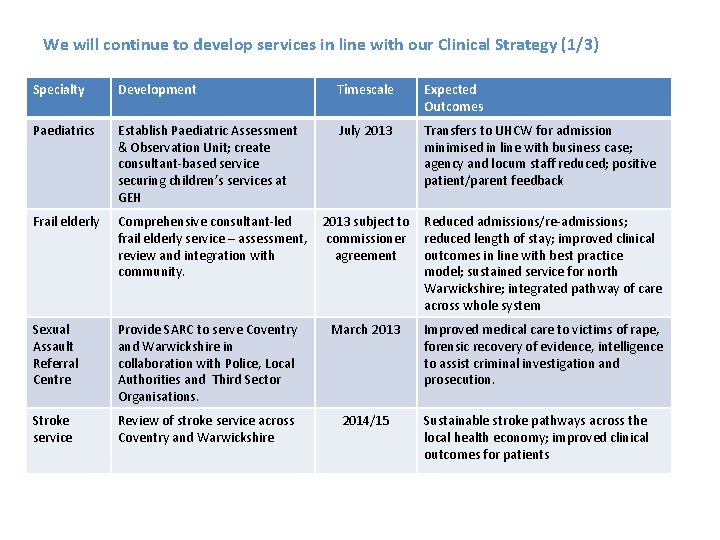
We will continue to develop services in line with our Clinical Strategy (1/3) Specialty Development Timescale Expected Outcomes Paediatrics Establish Paediatric Assessment & Observation Unit; create consultant-based service securing children’s services at GEH July 2013 Transfers to UHCW for admission minimised in line with business case; agency and locum staff reduced; positive patient/parent feedback Frail elderly Comprehensive consultant-led frail elderly service – assessment, review and integration with community. 2013 subject to commissioner agreement Reduced admissions/re-admissions; reduced length of stay; improved clinical outcomes in line with best practice model; sustained service for north Warwickshire; integrated pathway of care across whole system Sexual Assault Referral Centre Provide SARC to serve Coventry and Warwickshire in collaboration with Police, Local Authorities and Third Sector Organisations. March 2013 Improved medical care to victims of rape, forensic recovery of evidence, intelligence to assist criminal investigation and prosecution. Stroke service Review of stroke service across Coventry and Warwickshire 2014/15 Sustainable stroke pathways across the local health economy; improved clinical outcomes for patients
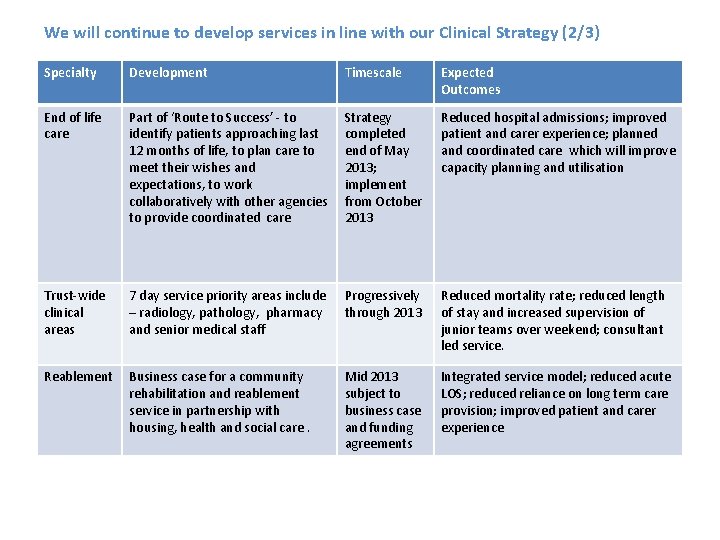
We will continue to develop services in line with our Clinical Strategy (2/3) Specialty Development Timescale Expected Outcomes End of life care Part of ‘Route to Success’ - to identify patients approaching last 12 months of life, to plan care to meet their wishes and expectations, to work collaboratively with other agencies to provide coordinated care Strategy completed end of May 2013; implement from October 2013 Reduced hospital admissions; improved patient and carer experience; planned and coordinated care which will improve capacity planning and utilisation Trust-wide clinical areas 7 day service priority areas include – radiology, pathology, pharmacy and senior medical staff Progressively through 2013 Reduced mortality rate; reduced length of stay and increased supervision of junior teams over weekend; consultant led service. Reablement Business case for a community rehabilitation and reablement service in partnership with housing, health and social care. Mid 2013 subject to business case and funding agreements Integrated service model; reduced acute LOS; reduced reliance on long term care provision; improved patient and carer experience
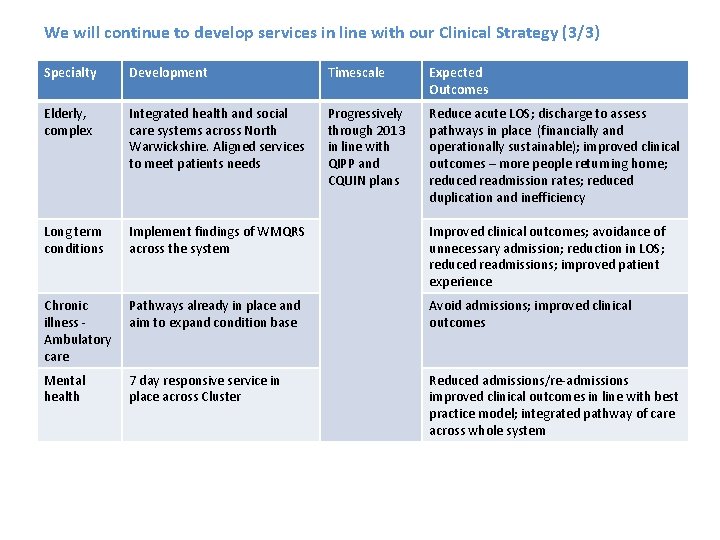
We will continue to develop services in line with our Clinical Strategy (3/3) Specialty Development Timescale Expected Outcomes Elderly, complex Integrated health and social care systems across North Warwickshire. Aligned services to meet patients needs Progressively through 2013 in line with QIPP and CQUIN plans Reduce acute LOS; discharge to assess pathways in place (financially and operationally sustainable); improved clinical outcomes – more people returning home; reduced readmission rates; reduced duplication and inefficiency Long term conditions Implement findings of WMQRS across the system Improved clinical outcomes; avoidance of unnecessary admission; reduction in LOS; reduced readmissions; improved patient experience Chronic illness Ambulatory care Pathways already in place and aim to expand condition base Avoid admissions; improved clinical outcomes Mental health 7 day responsive service in place across Cluster Reduced admissions/re-admissions improved clinical outcomes in line with best practice model; integrated pathway of care across whole system
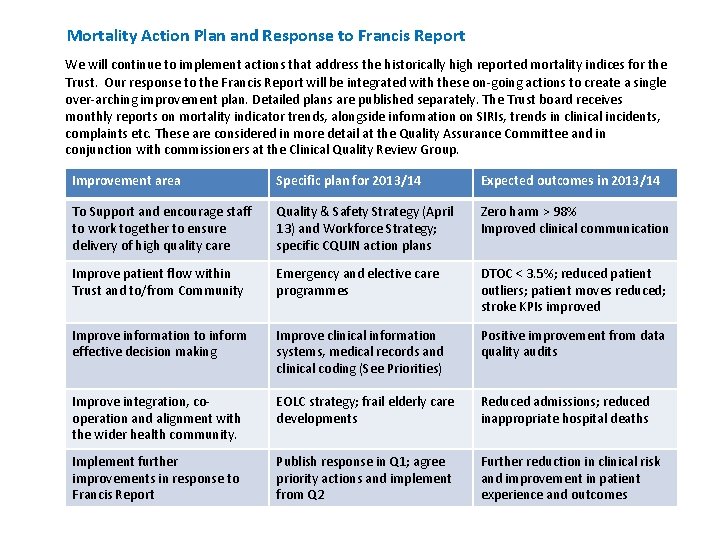
Mortality Action Plan and Response to Francis Report We will continue to implement actions that address the historically high reported mortality indices for the Trust. Our response to the Francis Report will be integrated with these on-going actions to create a single over-arching improvement plan. Detailed plans are published separately. The Trust board receives monthly reports on mortality indicator trends, alongside information on SIRIs, trends in clinical incidents, complaints etc. These are considered in more detail at the Quality Assurance Committee and in conjunction with commissioners at the Clinical Quality Review Group. Improvement area Specific plan for 2013/14 Expected outcomes in 2013/14 To Support and encourage staff to work together to ensure delivery of high quality care Quality & Safety Strategy (April 13) and Workforce Strategy; specific CQUIN action plans Zero harm > 98% Improved clinical communication Improve patient flow within Trust and to/from Community Emergency and elective care programmes DTOC < 3. 5%; reduced patient outliers; patient moves reduced; stroke KPIs improved Improve information to inform effective decision making Improve clinical information systems, medical records and clinical coding (See Priorities) Positive improvement from data quality audits Improve integration, cooperation and alignment with the wider health community. EOLC strategy; frail elderly care developments Reduced admissions; reduced inappropriate hospital deaths Implement further improvements in response to Francis Report Publish response in Q 1; agree priority actions and implement from Q 2 Further reduction in clinical risk and improvement in patient experience and outcomes
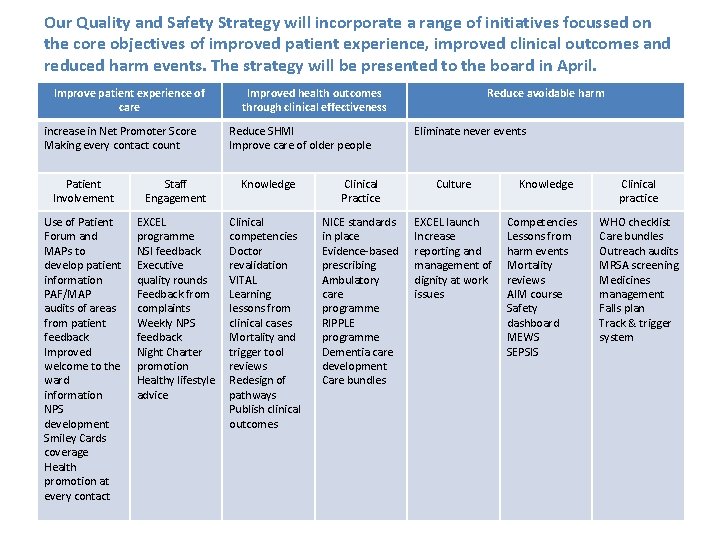
Our Quality and Safety Strategy will incorporate a range of initiatives focussed on the core objectives of improved patient experience, improved clinical outcomes and reduced harm events. The strategy will be presented to the board in April. Improve patient experience of care increase in Net Promoter Score Making every contact count Improved health outcomes through clinical effectiveness Reduce SHMI Improve care of older people Reduce avoidable harm Eliminate never events Patient Involvement Staff Engagement Knowledge Clinical Practice Culture Use of Patient Forum and MAPs to develop patient information PAF/MAP audits of areas from patient feedback Improved welcome to the ward information NPS development Smiley Cards coverage Health promotion at every contact EXCEL programme NSI feedback Executive quality rounds Feedback from complaints Weekly NPS feedback Night Charter promotion Healthy lifestyle advice Clinical competencies Doctor revalidation VITAL Learning lessons from clinical cases Mortality and trigger tool reviews Redesign of pathways Publish clinical outcomes NICE standards in place Evidence-based prescribing Ambulatory care programme RIPPLE programme Dementia care development Care bundles EXCEL launch Increase reporting and management of dignity at work issues Knowledge Competencies Lessons from harm events Mortality reviews AIM course Safety dashboard MEWS SEPSIS Clinical practice WHO checklist Care bundles Outreach audits MRSA screening Medicines management Falls plan Track & trigger system
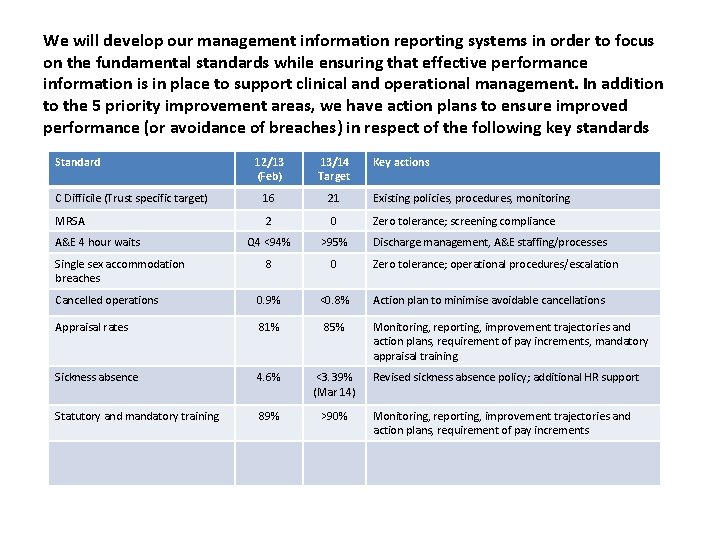
We will develop our management information reporting systems in order to focus on the fundamental standards while ensuring that effective performance information is in place to support clinical and operational management. In addition to the 5 priority improvement areas, we have action plans to ensure improved performance (or avoidance of breaches) in respect of the following key standards Standard 12/13 (Feb) 13/14 Target C Difficile (Trust specific target) 16 21 Existing policies, procedures, monitoring MRSA 2 0 Zero tolerance; screening compliance Q 4 <94% >95% 8 0 Cancelled operations 0. 9% <0. 8% Appraisal rates 81% 85% Sickness absence 4. 6% <3. 39% (Mar 14) Statutory and mandatory training 89% >90% A&E 4 hour waits Single sex accommodation breaches Key actions Discharge management, A&E staffing/processes Zero tolerance; operational procedures/escalation Action plan to minimise avoidable cancellations Monitoring, reporting, improvement trajectories and action plans, requirement of pay increments, mandatory appraisal training Revised sickness absence policy; additional HR support Monitoring, reporting, improvement trajectories and action plans, requirement of pay increments
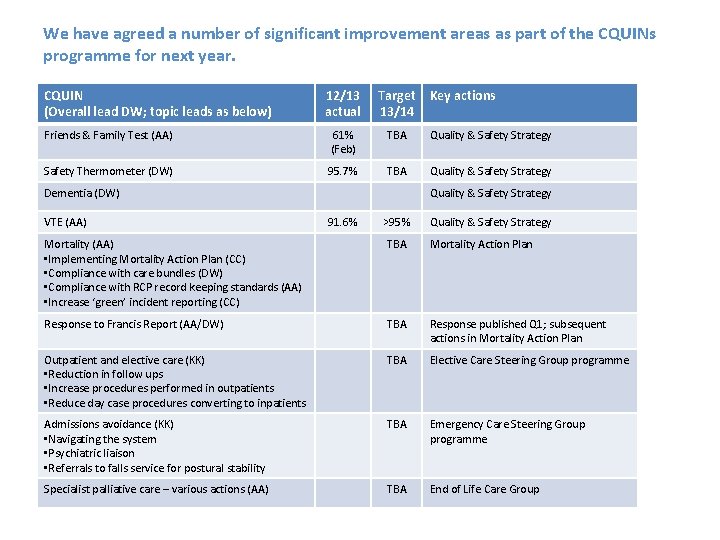
We have agreed a number of significant improvement areas as part of the CQUINs programme for next year. CQUIN (Overall lead DW; topic leads as below) 12/13 actual Target 13/14 Friends & Family Test (AA) 61% (Feb) TBA Quality & Safety Strategy Safety Thermometer (DW) 95. 7% TBA Quality & Safety Strategy Dementia (DW) VTE (AA) Key actions Quality & Safety Strategy 91. 6% >95% Quality & Safety Strategy Mortality (AA) • Implementing Mortality Action Plan (CC) • Compliance with care bundles (DW) • Compliance with RCP record keeping standards (AA) • Increase ‘green’ incident reporting (CC) TBA Mortality Action Plan Response to Francis Report (AA/DW) TBA Response published Q 1; subsequent actions in Mortality Action Plan Outpatient and elective care (KK) • Reduction in follow ups • Increase procedures performed in outpatients • Reduce day case procedures converting to inpatients TBA Elective Care Steering Group programme Admissions avoidance (KK) • Navigating the system • Psychiatric liaison • Referrals to falls service for postural stability TBA Emergency Care Steering Group programme Specialist palliative care – various actions (AA) TBA End of Life Care Group

Using the new NHS Quality Dashboard We will monitor all the relevant indicators in the new NHS Quality Dashboard, using this both as an indictor of where performance deviates significantly from other Trusts and where significant variations in performance trends occur. At the present time, we do not intend to set improvement targets against all the indicators in the dashboard. Where these are significant, they are already included elsewhere in the plan. In 2013/14, we will report on variations in key indicators and those where our performance varies from that of other Trusts as part of the Integrated Performance Report.
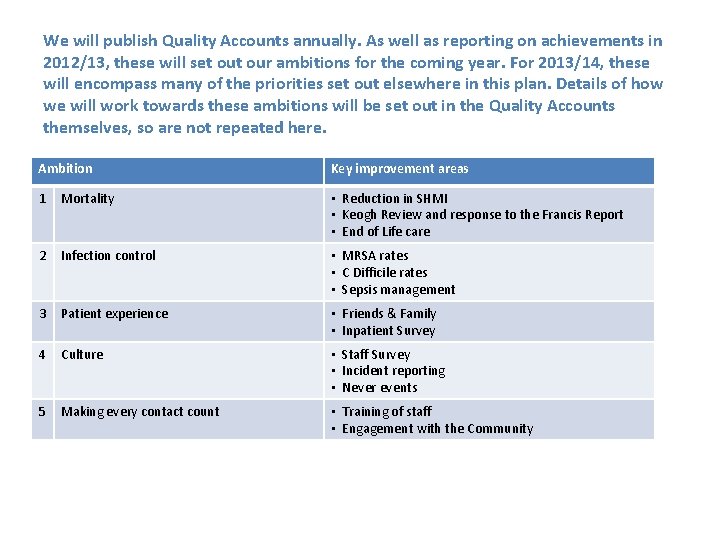
We will publish Quality Accounts annually. As well as reporting on achievements in 2012/13, these will set our ambitions for the coming year. For 2013/14, these will encompass many of the priorities set out elsewhere in this plan. Details of how we will work towards these ambitions will be set out in the Quality Accounts themselves, so are not repeated here. Ambition Key improvement areas 1 Mortality • Reduction in SHMI • Keogh Review and response to the Francis Report • End of Life care 2 Infection control • MRSA rates • C Difficile rates • Sepsis management 3 Patient experience • Friends & Family • Inpatient Survey 4 Culture • Staff Survey • Incident reporting • Never events 5 Making every contact count • Training of staff • Engagement with the Community

Our long term financial model is based on identifying a strategic partner that will either acquire the Trust or create an alternative organisational structure to achieve long term clinical and financial sustainability. We have modelled each scenario although the real test of these will not come until potential partners actually submit bids through our procurement process. These scenarios are compared against a pessimistic base case which assumes that no significant action is taken restructure services in order to address the underlying deficit. The LTFMs for each scenario are summarised below:
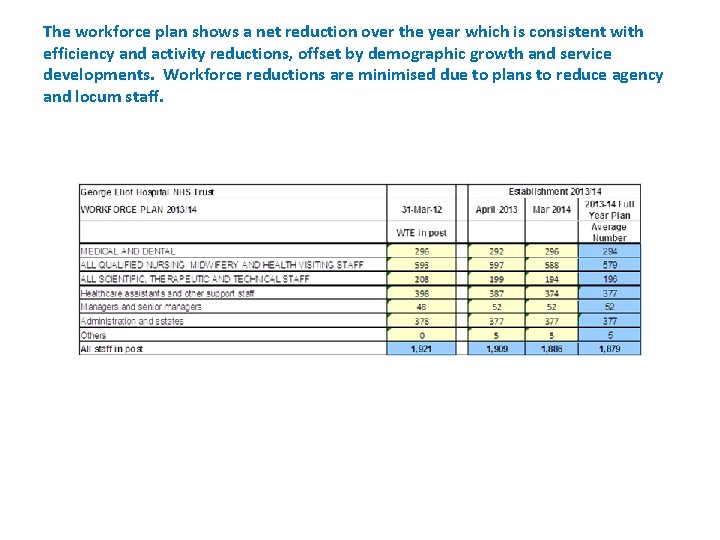
The workforce plan shows a net reduction over the year which is consistent with efficiency and activity reductions, offset by demographic growth and service developments. Workforce reductions are minimised due to plans to reduce agency and locum staff.

Staff satisfaction, performance management and organisational development • • Staff satisfaction survey (2012) – key findings – 20 improved – 5 diminished – 3 stayed the same – Overall engagement significantly improved over 3 year period Summary results – Communication between senior managers and staff improved (31% reporting good communication compared with 23% in 2011 and 19% 2010) – Increased number of staff reporting happy for friend and family to be treated at GEH 55% (compared with 48% in 2010) – Increased number of staff recommending GEH as place to work (54% compared with 46% in 2011) – Confidence in raising concerns 90% of staff confident to raise concerns of fraud (90% compared with 86% in the average Trust and 87% for this Trust in 2010) – Best performing 20% of Trusts in respect of job relevant learning or development in last 12 months and in receiving health and safety training • Organisation development – Development and signoff of Vision and Values Pledges (EXCEL) – Communicate through internal team meetings and external forums including patient and other stakeholder events – Integration of values pledges into appraisal process – Talent management and succession planning process developed aligned to leadership academy framework – Revised Education and Training Structure to further enable inter professional E&T and widening participation – Expansion of work experience to include local workless – Implementation and expansion of apprenticeship programmes – Workforce Planning Process – successful service redesign programme delivered – integrated workforce planning process and enhanced capacity and capability. – Development of competence based recruitment
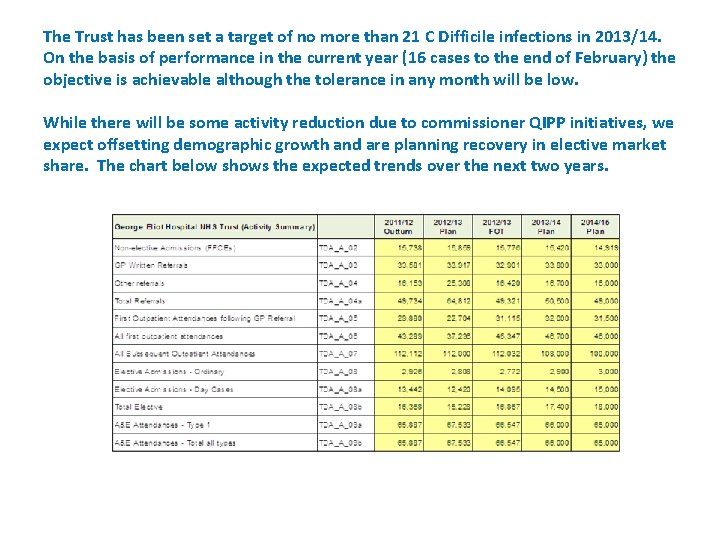
The Trust has been set a target of no more than 21 C Difficile infections in 2013/14. On the basis of performance in the current year (16 cases to the end of February) the objective is achievable although the tolerance in any month will be low. While there will be some activity reduction due to commissioner QIPP initiatives, we expect offsetting demographic growth and are planning recovery in elective market share. The chart below shows the expected trends over the next two years.

The financial plan for 2013/14 shows a deficit of £ 7. 9 m resulting from the underlying deficit for which support was provided in 2012/13, commissioner QIPP schemes which are not fully offset by cost avoidance and the expected costs of the SSF project. There are more downside risks than upside risks.
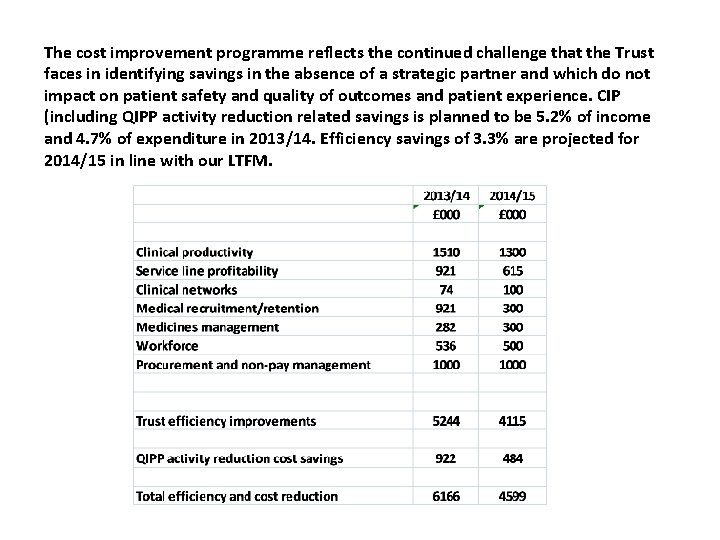
The cost improvement programme reflects the continued challenge that the Trust faces in identifying savings in the absence of a strategic partner and which do not impact on patient safety and quality of outcomes and patient experience. CIP (including QIPP activity reduction related savings is planned to be 5. 2% of income and 4. 7% of expenditure in 2013/14. Efficiency savings of 3. 3% are projected for 2014/15 in line with our LTFM.

Implementing the cost improvement programme • • • Overall management of the CIP is directed by the Director of Finance, but implementation is the responsibility of operational divisions and departments Development and implementation of initiatives is supported by a Programme Management Office staffed by experienced external facilitators All initiatives are developed and owned by the appropriate clinical director, clinical lead or departmental manager and a Project Initiation Document is produced Some crossorganisational themes are managed by the PMO. All initiatives are reviewed by the Medical and Nursing Directors before implementation. Periodical reviews take place to confirm that initiatives, once implemented, are not adversely affecting quality of patient care. Finance maintains a master schedule of CIP initiatives, budget deductions, actual achievement and forecast performance. CIP performance is monitored monthly by the Finance Committee and reported at summary level to the board as part of the Integrated Performance Report.
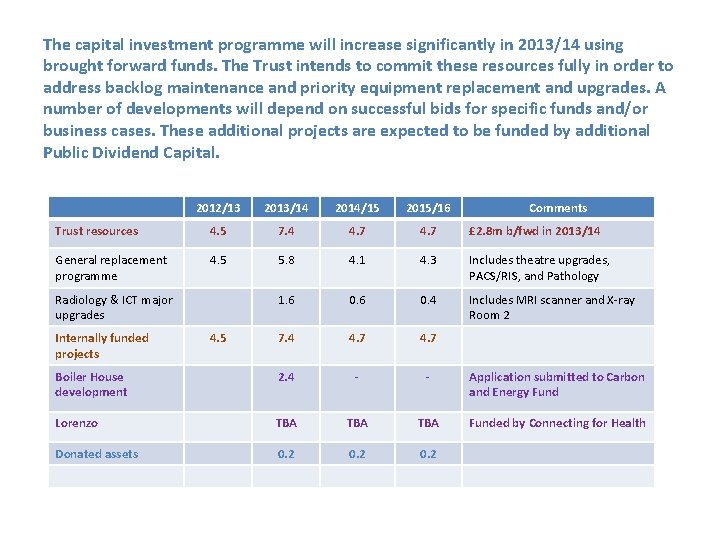
The capital investment programme will increase significantly in 2013/14 using brought forward funds. The Trust intends to commit these resources fully in order to address backlog maintenance and priority equipment replacement and upgrades. A number of developments will depend on successful bids for specific funds and/or business cases. These additional projects are expected to be funded by additional Public Dividend Capital. 2012/13 2013/14 2014/15 2015/16 Trust resources 4. 5 7. 4 4. 7 £ 2. 8 m b/fwd in 2013/14 General replacement programme 4. 5 5. 8 4. 1 4. 3 Includes theatre upgrades, PACS/RIS, and Pathology 1. 6 0. 4 Includes MRI scanner and X-ray Room 2 7. 4 4. 7 Boiler House development 2. 4 - - Application submitted to Carbon and Energy Fund Lorenzo TBA TBA Funded by Connecting for Health Donated assets 0. 2 Radiology & ICT major upgrades Internally funded projects 4. 5 Comments
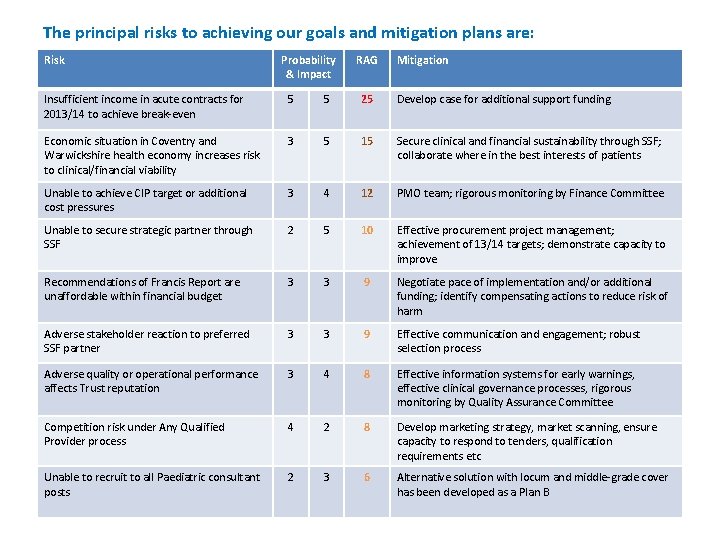
The principal risks to achieving our goals and mitigation plans are: Risk Probability & Impact RAG Mitigation Insufficient income in acute contracts for 2013/14 to achieve break-even 5 5 25 Develop case for additional support funding Economic situation in Coventry and Warwickshire health economy increases risk to clinical/financial viability 3 5 15 Secure clinical and financial sustainability through SSF; collaborate where in the best interests of patients Unable to achieve CIP target or additional cost pressures 3 4 12 PMO team; rigorous monitoring by Finance Committee Unable to secure strategic partner through SSF 2 5 10 Effective procurement project management; achievement of 13/14 targets; demonstrate capacity to improve Recommendations of Francis Report are unaffordable within financial budget 3 3 9 Negotiate pace of implementation and/or additional funding; identify compensating actions to reduce risk of harm Adverse stakeholder reaction to preferred SSF partner 3 3 9 Effective communication and engagement; robust selection process Adverse quality or operational performance affects Trust reputation 3 4 8 Effective information systems for early warnings, effective clinical governance processes, rigorous monitoring by Quality Assurance Committee Competition risk under Any Qualified Provider process 4 2 8 Develop marketing strategy, market scanning, ensure capacity to respond to tenders, qualification requirements etc Unable to recruit to all Paediatric consultant posts 2 3 6 Alternative solution with locum and middle-grade cover has been developed as a Plan B
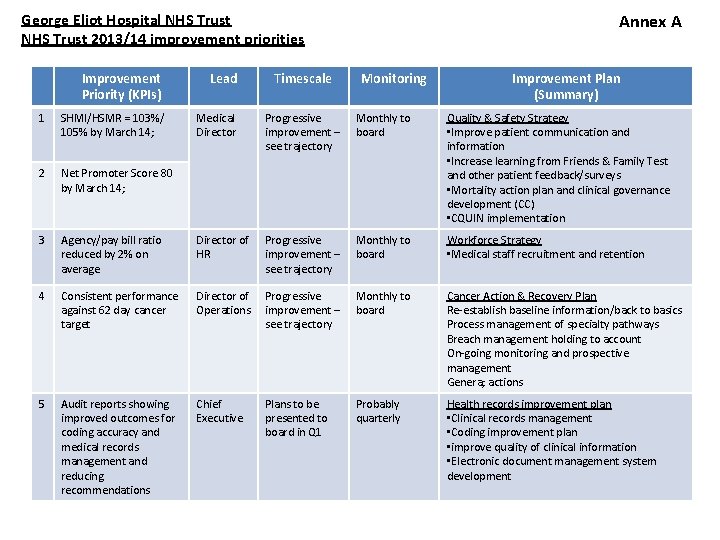
Annex A George Eliot Hospital NHS Trust 2013/14 improvement priorities Improvement Priority (KPIs) Lead Timescale Monitoring Improvement Plan (Summary) 1 SHMI/HSMR = 103%/ 105% by March 14; Medical Director Progressive improvement – see trajectory Monthly to board 2 Net Promoter Score 80 by March 14; Quality & Safety Strategy • Improve patient communication and information • Increase learning from Friends & Family Test and other patient feedback/surveys • Mortality action plan and clinical governance development (CC) • CQUIN implementation 3 Agency/pay bill ratio reduced by 2% on average Director of HR Progressive improvement – see trajectory Monthly to board Workforce Strategy • Medical staff recruitment and retention 4 Consistent performance against 62 day cancer target Director of Operations Progressive improvement – see trajectory Monthly to board Cancer Action & Recovery Plan Re-establish baseline information/back to basics Process management of specialty pathways Breach management holding to account On-going monitoring and prospective management Genera; actions 5 Audit reports showing improved outcomes for coding accuracy and medical records management and reducing recommendations Chief Executive Plans to be presented to board in Q 1 Probably quarterly Health records improvement plan • Clinical records management • Coding improvement plan • improve quality of clinical information • Electronic document management system development
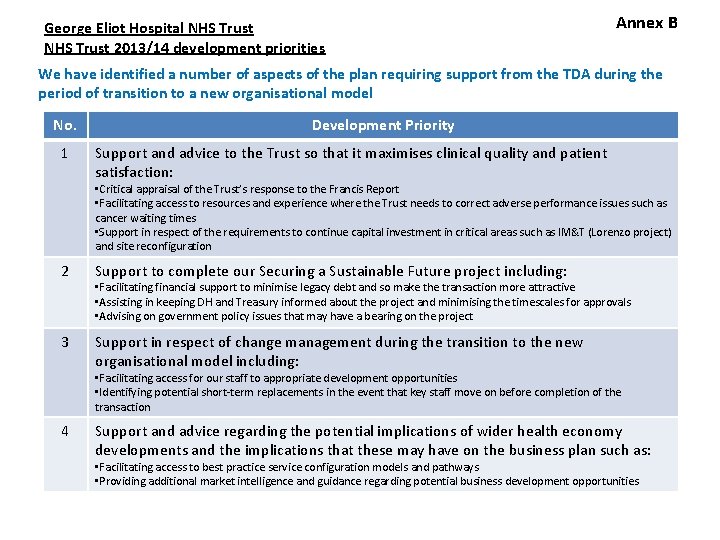

George Eliot Hospital NHS Trust 2013/14 development priorities Annex B We have identified a number of aspects of the plan requiring support from the TDA during the period of transition to a new organisational model No. 1 Development Priority Support and advice to the Trust so that it maximises clinical quality and patient satisfaction: • Critical appraisal of the Trust’s response to the Francis Report • Facilitating access to resources and experience where the Trust needs to correct adverse performance issues such as cancer waiting times • Support in respect of the requirements to continue capital investment in critical areas such as IM&T (Lorenzo project) and site reconfiguration 2 Support to complete our Securing a Sustainable Future project including: 3 Support in respect of change management during the transition to the new organisational model including: • Facilitating financial support to minimise legacy debt and so make the transaction more attractive • Assisting in keeping DH and Treasury informed about the project and minimising the timescales for approvals • Advising on government policy issues that may have a bearing on the project • Facilitating access for our staff to appropriate development opportunities • Identifying potential short-term replacements in the event that key staff move on before completion of the transaction 4 Support and advice regarding the potential implications of wider health economy developments and the implications that these may have on the business plan such as: • Facilitating access to best practice service configuration models and pathways • Providing additional market intelligence and guidance regarding potential business development opportunities
- Slides: 34