Genus Bacillus Bacillus anthracis Causative agent of anthrax

Genus Bacillus

Bacillus anthracis �Causative agent of anthrax disease �Historical importance: �Was the 1 st pathogenic bacteria to be seen under microscope �Anthrax 1 st communicable disease to be transmitted by inoculation of infected blood � 1 st bacterium to be isolated in pure culture and shown to possess spores � 1 st bacterium used for the preparation of attenuated vaccine (Louis pasteur)

�Morphology: �Gram positive, spore forming bacillus �Spores are oval and central in position and are of the same width as the bacillary body, thus do not cause bulging of bacillus �Spores are formed in culture or soil but not in animal body �Sporulation occurs in unfavourable conditions for growth


�In culture, bacilli are arranged end-to-end in long chains, ends are truncated and have a swollen appearance, this gives a bamboo-stick appearance

�Antigens: �Capsular antigen: present in virulent strain �Cell wall antigen �Somatic antigen: induces antibody formation which is protective �Toxin: �Two virulence factors- capsular polypeptide, anthrax toxin �Capsular polypeptide inhibits phagocytosis

�Anthrax toxin has 3 components: �Edema factor (OF or factor I) �Protective antigen factor (PA or factor II) �Lethal factor (LF or factor III) �Individually non toxic, whole complex produces local edema, generalised shock

�Pathogenesis: �Anthrax is a zoonotic disease �Animals are infected by ingestion of the spores in soil �Infected animals shed large numbers of bacilli in the discharges from mouth, nose and rectum �Human anthrax is contracted from animals directly or indirectly �Cutaneous anthrax �Pulmonary anthrax �Intestinal anthrax

�Cutaneous anthrax: �Entry of infection through skin �Face, neck, hands, arms, back - usual sites �Lesion starts as papule, becomes vesicular containing fluid which may be clear or blood stained �Whole area is congested and edematous, several satellite lesions filled with serum or pus are arranged around a central necrotic lesion which is covered by a black eschar �The lesion is called a malignant pustule
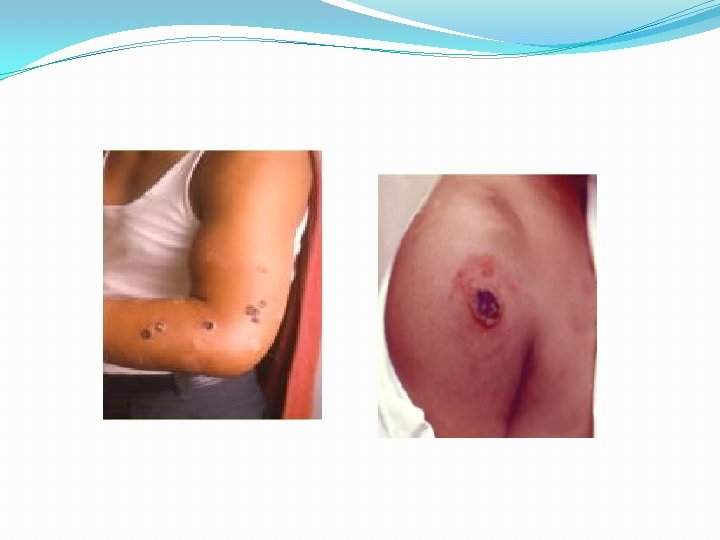

�Cutaneous anthrax is common in dock workers carrying loads of hides and skins on their bare back �This is called Hide porter’s disease �Pulmonary anthrax: �Common in wool factories, due to inhalation of dust of infected wool �Wool sorter’s disease �Hemorrhagic pneumonia with a high fatality rate �Hemorrhagic meningitis may be a complication �All 3 forms if not treated in time, lead to septicaemic anthrax and death

�Intestinal anthrax: �Rare, occurs mainly in primitive communities who eat carcass of animals dying of anthrax �Severe enteritis with bloody diarrhoea, death �Human anthrax may be industrial or non-industrial �Industries such as meat packing, wool factories �Non-industrial is occupations associated with animals like veterinarians, butchers, farmers �Can be seen in general population

� laboratory diagnosis: � 1. Specimen: swabs, fluid, pus from pustules (cutaneous anthrax), sputum and blood (pulmonary anthrax), faeces, peritoneal fluid (intestinal anthrax) � 2. Microscopy: �Large Gram positive bacilli �Capsule appears as clear halo around the bacterium in India-ink staining �Direct fluorescent antibody test for capsule specific staining and for polysaccharide ( cell wall) antigen

�Mc. Fadyean’s reaction: �When blood films containing anthrax bacilli are stained with polychrome methylene blue for 10 -12 seconds and examined under microscope, an amorphous purple material is noticed around the bacilli �This is due to the disintegrated capsular material �Characteristic of anthrax bacillus �Used for presumptive diagnosis of anthrax

� 3. Culture: �Aerobe and facultative anaerobe �a. Nutrient agar media: �Round colonies, raised and greyish white �Under low power of microscope, the edge of the colony is found to be composed of long, interlacing chains of bacilli, resembling locks of matted hair �This is called Medusa head appearance �b. Blood agar: �Non-hemolytic colonies, occasionally narrow zone of hemolysis


�c. Gelatin stab culture: �Gelatin is liquefied at the top of the tube due to aerobic conditions �Gives a characteristic inverted fir tree appearance �d. Selective media: �PLET medium containing heart infusion agar with polymyxin, lysozyme, EDTA (ethylene diamine tetracetic acid) and thallous acetate

�e. Solid medium with penicillin: �B. anthracis grown on this medium become large, spherical and occurs in chains on the surface of the agar, resembling a string of pearls �This is useful to differentiate B. anthracis from B. cereus

�Biochemical reactions: �Catalase positive �Glucose, maltose, sucrose fermented with acid only �Nitrates reduced to nitrites �Resistance: �Vegetative form is killed at 600 C in 30 mins �Spores are destroyed by: � 4% potassium permanganate solution in 15 mins �Autoclaving at 1210 C for 15 minutes �Spores in animal product is destroyed by duckering: 2% formaldehyde is used at 30 -400 C for 20 mins for disinfection of wool, 0. 25% at 600 C for animal hair

� 4. Serology � 5. PCR �Presumptive identification of anthrax: � 1. Large Gram positive bacilli with morphology of anthrax bacillus and non-motile � 2. Non-hemolytic on blood agar, cultural characteristics � 3. Catalase positive

�Treatment: �Doxycycline, ciprofloxacin �Prophylaxis; �Improvement of factory hygiene, proper sterilization of animal products like wool �Carcasses of infected animals are buried deep in lime �Immunisation of animals �For humans for those who are occupationally exposed, alum precipitated toxoid given intramuscularly, 3 doses at intervals of 6 weeks and 6 months, booster dose after an year

�Anthracoid bacilli: �Aerobic spore bearing bacilli resembling B. anthracis are called anthracoid bacilli or pseudoanthrax bacilli �Of them the most important is B. cereus recognised to cause foodborne gastroenteritis �B. subtilis can be an opportunistic pathogen causing eye infections and septicemia �B. licheniformis can cause food poisoning

�spores are used to test the efficiency of sterilisation by autoclaves �Differentiation of B. anthracis and anthracoid bacilli is important �Few differentiating features:
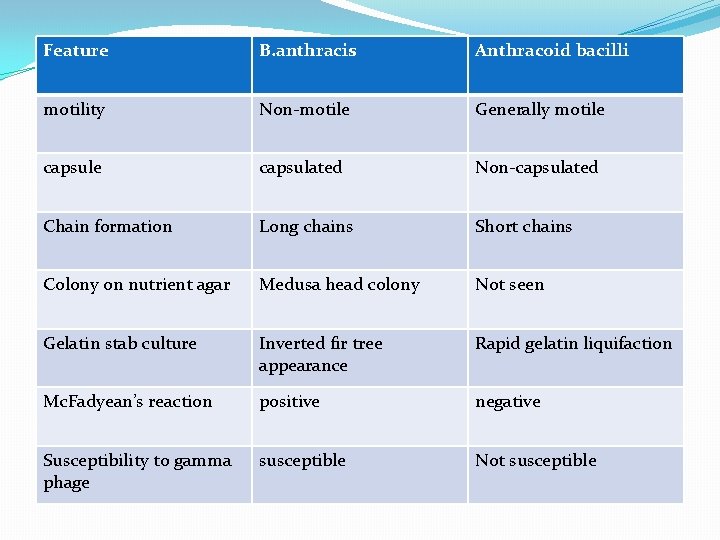
Feature B. anthracis Anthracoid bacilli motility Non-motile Generally motile capsulated Non-capsulated Chain formation Long chains Short chains Colony on nutrient agar Medusa head colony Not seen Gelatin stab culture Inverted fir tree appearance Rapid gelatin liquifaction Mc. Fadyean’s reaction positive negative Susceptibility to gamma phage susceptible Not susceptible

Bacillus cereus �Causes food poisoning �Widely distributed in nature in soil, vegetables, milk, cereals, spices, meat, poultry �Few spores survive during cooking and germinate into vegetative bacilli thus causing food poisoning

�Types of food poisoning: � 1. Short incubation period type (1 -5 hours) �Emetic type �Characterised by acute nausea, vomiting within 1 -5 hours after a meal �Diarrhoea is uncommon �Source of food: usually consumption of cooked rice, fried rice of chinese restaurants �Caused by serotypes 1, 3, 5 �Produce a toxin which resembles staphylococcal enterotoxin �Stool – large numbers of bacilli seen

� 2. Long incubation period type (8 -16 hours): �Diarrhoeal type �Abdominal pain and diarrhoea, 8 -16 hours after ingestion of contaminated food �Vomiting is rare �Caused by serotypes 2, 6, 8, 9 , 10 �Produce an enterotoxin which resembles heat labile enterotoxin of Escherichia coli �Stool – small number of bacilli seen

�Laboratory diagnosis: �Specimen: Suspected food, faeces, vomitus �Culture on ordinary media or special media like mannitol-eggyolk-phenol red-polymyxin agar �Spore bearing Gram positive bacilli seen on smears prepared from colonies �Motile, non-capsulated, not susceptible to gamma phage and does not react with fluorescent antibody conjugate (differentiating features from B. anthracis)

�Treatment: �Self limiting disease, requires no specific treatment �Control: �Hygienic practices with food handling �Adequate cooking and proper storing
- Slides: 29