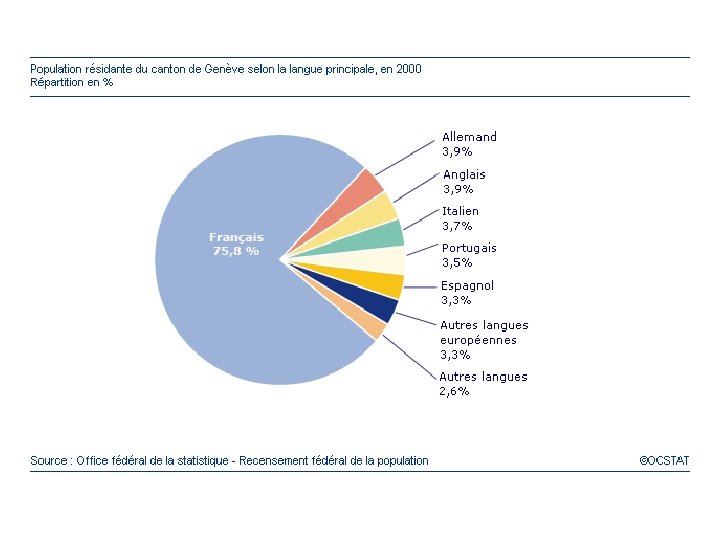
Geneva University Hospitals l l l 2167 beds
Geneva University Hospitals l l l 2'167 beds 1'285 doctors; 3'479 nurses; 1'477 paramedical Personnel: 51% non-Swiss; 88 countries Patients: 51% non-Swiss, 88 countries 2007 -09: major budget cutting exercise
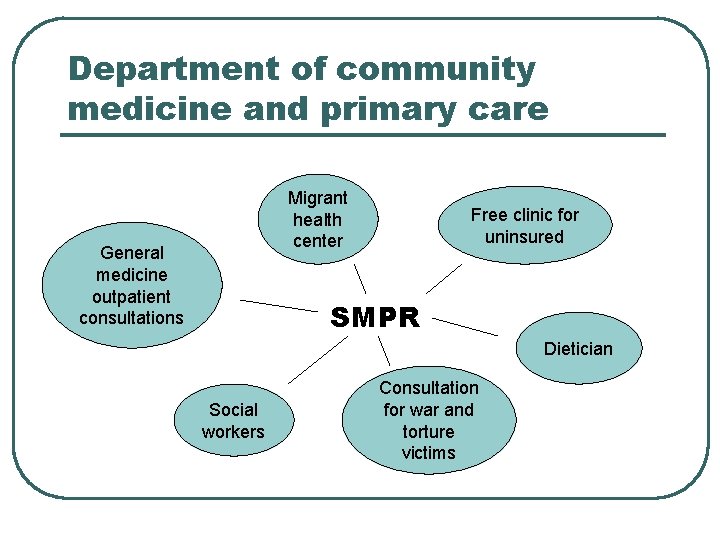
Department of community medicine and primary care Migrant health center General medicine outpatient consultations Free clinic for uninsured SMPR Dietician Social workers Consultation for war and torture victims

Context: Europe/Switzerland l European project: Migrant Friendly Hospitals • l l l www. mfh-eu. net/public/home. htm Swiss « Migration and Health Strategy 2002 -07” MFH named priority by Swiss Federal Public Health Office WHO and Swiss “Health promoting hospitals network” creates “Task Force on Migrant Friendly Hospitals» • www. healthhospitals. ch/franz/

Our working definition l Cultural competence: The capacity of the institution and clinicians to identify, understand respond effectively to the linguistic and cultural needs of patients

Strategies: HUG l l Cultural competence training for clinicians Interpreter services Cross-cultural consultation service Research/evaluation

Strategies: HUG l l Cultural competence training for clinicians Interpreter services Cross-cultural consultation service Research/evaluation
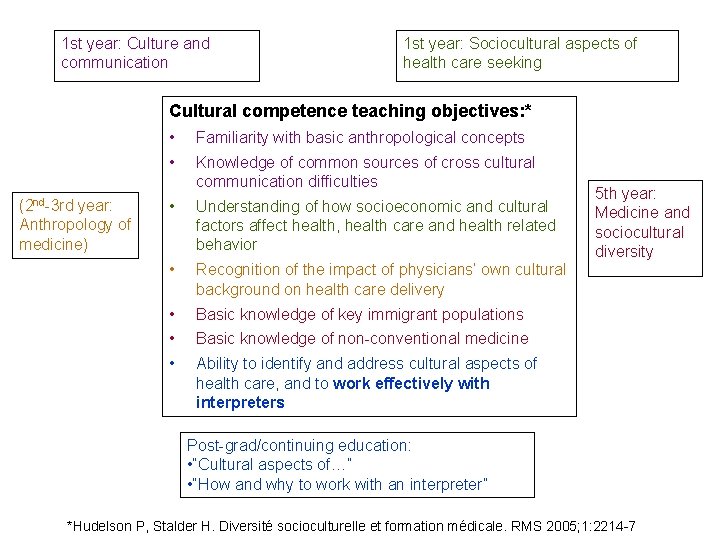
1 st year: Culture and communication 1 st year: Sociocultural aspects of health care seeking Cultural competence teaching objectives: * (2 nd-3 rd year: Anthropology of medicine) • Familiarity with basic anthropological concepts • Knowledge of common sources of cross cultural communication difficulties • Understanding of how socioeconomic and cultural factors affect health, health care and health related behavior • Recognition of the impact of physicians’ own cultural background on health care delivery • Basic knowledge of key immigrant populations • Basic knowledge of non-conventional medicine • Ability to identify and address cultural aspects of health care, and to work effectively with interpreters 5 th year: Medicine and sociocultural diversity Post-grad/continuing education: • “Cultural aspects of…” • “How and why to work with an interpreter” *Hudelson P, Stalder H. Diversité socioculturelle et formation médicale. RMS 2005; 1: 2214 -7
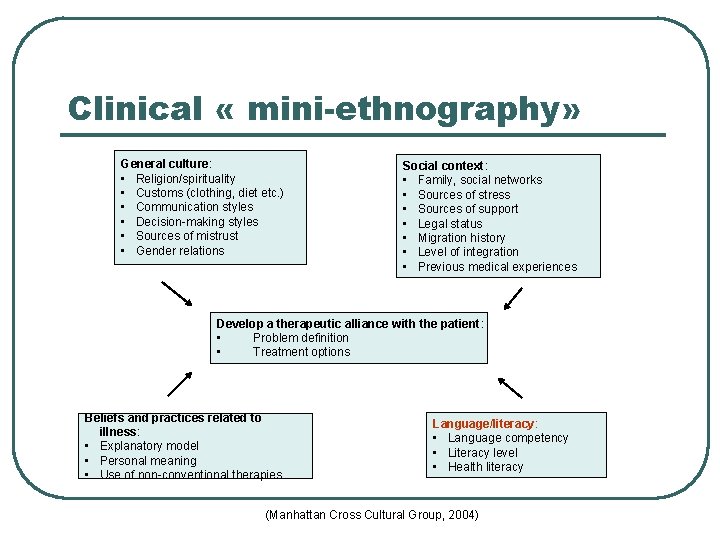
Clinical « mini-ethnography» General culture: • Religion/spirituality • Customs (clothing, diet etc. ) • Communication styles • Decision-making styles • Sources of mistrust • Gender relations Social context: • Family, social networks • Sources of stress • Sources of support • Legal status • Migration history • Level of integration • Previous medical experiences Develop a therapeutic alliance with the patient: • Problem definition • Treatment options Beliefs and practices related to illness: • Explanatory model • Personal meaning • Use of non-conventional therapies Language/literacy: • Language competency • Literacy level • Health literacy (Manhattan Cross Cultural Group, 2004)

Strategies: HUG l l Cultural competence training for clinicians Interpreter services Cross-cultural consultation service Research

Interpreter services in Geneva l l l Network of 90+ interpreters (50+ languages), coordinated by the Geneva Red Cross Interpreters: immigrants, refugees, a few asylum seekers Interpreters work for a wide range of institutions HUG/CRG convention HUG intranet site where interpreter list can be accessed; hospital services contact interpreters directly Services paid by departmental budgets

Use of interpreter services l Total # hours in 2006: 9504 • 0% Geriatrics • 0% Long-term care facility • 5% Ob-Gyn • 6% Internal Medicine • 6% Neurosciences (includes dermatology) • 7% Pediatrics • 20% Psychiatry • 54% Community Medicine

Challenges l l Underutilization in many departments? Use of internal, ad hoc interpreters Agency: • • • Sees interpreting as “secondary activity” Provides little/no training for interpreters Does not yet require certification for hiring Has no quality control procedures Has lengthy process for identifying/hiring of new interpreters Currently no other interpreter services available

Certification in Switzerland l l Granted by the “Association suisse pour l'interprétariat communautaire et la médiation culturelle” http: //inter-pret. ch/ Requirements: • Completion of 2 training modules • Attestation: language competency • Attestation: 50 hours minimum interpreting experience l Cost: 2500 CHF ($2200) plus transport

Example of training content l l Module 1: Intro to community interpreting • • • 96 hours of class time 8 hours small-group supervisions 65 hours individual work (reading, learning-process journal, written case presentation) Module 2: Overview of specific domains • • • 63 hours of class time 8 hours small-group work (visits, tutoring) 45 hours individual work (reading, research, preparation of personal materials)

HUG: Activities (since Oct ’ 06) l l l l l Qualitative situation analysis Creation of « Quality group » for interpreting Information/training sessions for interpreters Development of explicit HUG requirements Establishment of “incident reporting” system Improved intranet site Grand rounds presentation on language barriers Presentations in hospital newspaper and hospital television program HUG list of approved interpreters (planned) User satisfaction survey (planned)

User satisfaction survey l l l Frequency of contact with non-francophone patients Use of and preferences regarding various strategies for communicating with nonfrancophone patients Familiarity with Red Cross interpreter service Satisfaction with the Red Cross interpreter service Opinions regarding priority activities for improving communication with nonfrancophone patients

How do you evaluate the quality of services provided by CRG interpreters: (Always, often, sometimes, rarely, never) l l l l l CRG interpreters are available when needed CRG interpreters arrive on time CRG interpreters introduce themselves and explain their role CRG interpreters have adequate language competency You have confidence in the accuracy of medical information communicated by CRG interpreters If necessary, CRG interpreters ask for clarification during the encounter before interpreting CRG interpreters ensure that you understand what the patient is trying to communicate to you When necessary, CRG interpreters clarify cultural beliefs or practices mentioned by the patient CRG interpreters maintain neutrality during the consultation

Future priorities l l Systematic collection of patient language data to improve planning of interpreter services and monitor use Require/offer training for hospital interpreters Offer information session for all new staff on when and how to use interpreters Develop methods to evaluate quality of interpreting

Strategies: HUG l l Cultural competence training for clinicians Interpreter services Cross-cultural consultation service Research

Cultural consultation service l Aim is to help clinicians identify and address cultural/linguistic barriers to care l CCS multi-disciplinary team: doctors, nurses, psychiatrists, anthropologist, cultural informants/interpreters l Services provided: in-depth evaluation, sociocultural information, referral to community resources, recommendations for culturally appropriate care/communication, etc.

The « cultural formulation » outline l l l Cultural identity (including language & literacy) Cultural explanations of the illness Cultural factors related to the psychosocial environment and levels of functioning Cultural elements of the clinician-patient relationship (including language issues) Overall impact of culture on diagnosis and care Lewis-Fernandez & Diaz (2002). The cultural formulation: a method for assessing cultural factors affecting the clinical encounter. Psychiatry Quarterly 73(4): 271 -95.

CCS example l l l 25 year old Cameroonian man, former asylum seeker, now undocumented. Does not speak French well; consultations conducted in English. Followed regularly for hypertension; asks for a “test to know whether his future children will be healthy. ” Young female resident does not understand patient’s request; feels patient is asking for inappropriate exams. Patient becomes aggressive and dissatisfied, accuses resident of knowing nothing about medicine.

Linguistic and cultural barriers “Well, I don’t speak very good English. I have to admit that, you know. And, well, neither does he. So often I have to ask him to repeat what he just said because I didn’t understand. And I think that made him angry…We had such a level of incomprehension and such a gap between what he expected from me and what I was offering him, that he became aggressive. ”

Strategies: HUG l l Cultural competence training for clinicians Interpreter services Cross-cultural consultation service Research

Research activities: examples l Improving communication between physicians and patients who speak a foreign language l Perceptions and experiences of residents regarding the care of culturally and linguistically diverse patients l Perceptions and experiences of medical interpreters regarding cross cultural communication difficulties l Cultural competence: development of tools to measure clinicians' core knowledge, attitudes and skills l Interpreter service user satisfaction survey

Improving communication l l l Intervention: Four 2 -hour workshops for general medicine residents Self-administered questionnaire to doctors and patients pre and post intervention 6 items on perceptions of the quality of patient-doctor communication Bischoff et al. Improving communication between physicians and patients who speak a foreign language. Br J Gen Pract. 2003; 53(492): 541 -6.

Results l l 1016 consultations: 40% allophone patients Languages: Albanian, Serbo-Croatian, Somali, Spanish, Arabic, Portuguese, Farsi Physicians: • • • Higher satisfaction with French-speaking patients, both before and after intervention Higher satisfaction with trained vs ad hoc interpreters Use of trained vs ad hoc interpreters increased • Satisfaction of allophone patients greater postintervention Patients: Bischoff et al. Improving communication between physicians and patients who speak a foreign language. Br J Gen Pract. 2003; 53(492): 541 -6.

Interpreters’ recommendations l l l Be aware of potential sources of misunderstanding Have basic knowledge about patient’s country of origin Be sensitive to translation difficulties Adapt to patient’s communication style Discuss communication issues with interpreters Hudelson P. Improving patient-provider communication: insights from interpreters Fam Pract. 2005 Jun; 22(3): 311 -6.
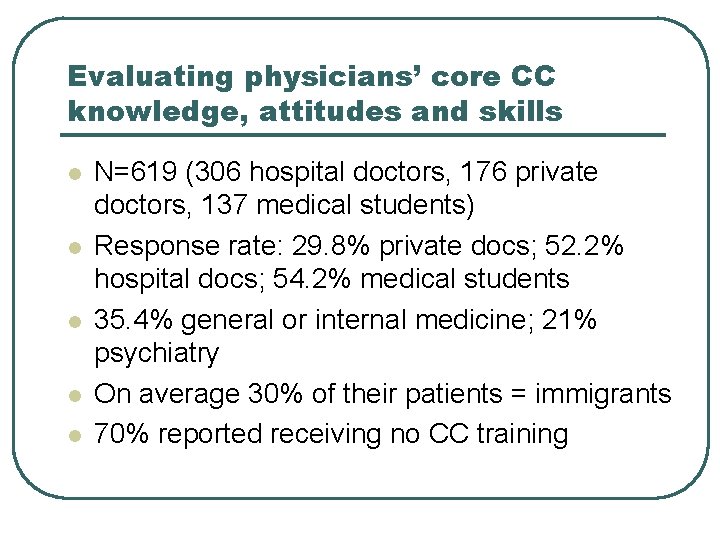
Evaluating physicians’ core CC knowledge, attitudes and skills l l l N=619 (306 hospital doctors, 176 private doctors, 137 medical students) Response rate: 29. 8% private docs; 52. 2% hospital docs; 54. 2% medical students 35. 4% general or internal medicine; 21% psychiatry On average 30% of their patients = immigrants 70% reported receiving no CC training

Findings l l Patients’ lack of French rated #1 source of difficulty with migrant patients 83% consider professional interpreters very important for ensuring quality care 41% strongly agreed that hospitals should always provide professional interpreters 58. 6% rated highly their ability to work effectively with a professional interpreter

Findings l l Patients’ lack of French rated #1 source of difficulty with migrant patients 83% consider professional interpreters very important for ensuring quality care 41% strongly agreed that hospitals should always provide professional interpreters 58. 6% rated highly their ability to work effectively with a professional interpreter

Exercise: a clinical vignette An orthopedic surgeon is to see a patient that was referred to him by a general medicine physician. The patient only speaks Swahili. The surgeon has planned for a longer consultation than usual, and has scheduled a professional interpreter. The patient and the interpreter, who do not know each other, arrive simultaneously for the consultation. The doctor greets them, invites them to sit down, and then turns to the interpreter and says: “Ask Mr. Z what brings him here today. ” Indicate everything that the doctor forgot to do or could have done better.

Answers we were looking for: l l l Speak directly to the patient Introduce the interpreter to the patient Explain confidentiality Ask patient if he accepts the interpreter Meet with the interpreter beforehand to discuss objectives of the consultation

What we got: l l l 22% gave no correct answers 39% gave 1 correct answer 30% gave 2 correct answers 8% gave 3 correct answers 1% gave 4 correct answers 0 gave all 5 answers

Conclusion: challenges l l Raise awareness of language barriers as a quality/safety issue Encourage use of professional interpreters in the face of budget cuts Train clinicians to work with interpreters Monitor interpreter needs and degree to which needs are being met
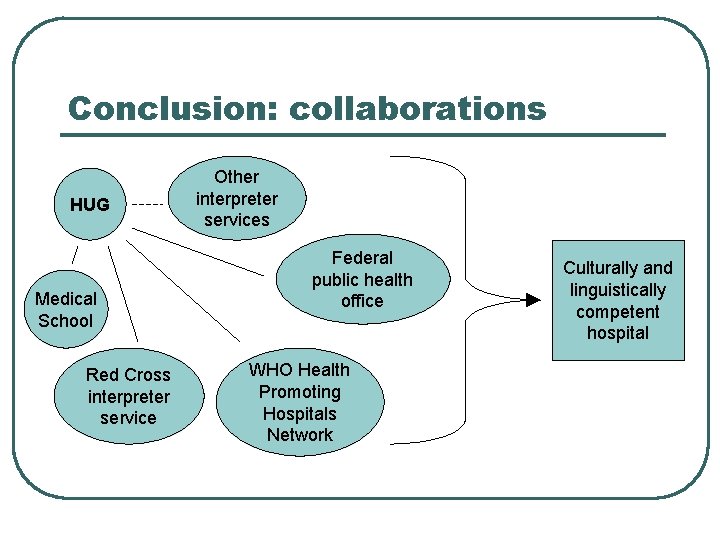
Conclusion: collaborations HUG Medical School Red Cross interpreter service Other interpreter services Federal public health office WHO Health Promoting Hospitals Network Culturally and linguistically competent hospital

And finally… What are your ideas for strengthening professionalism and quality among agency interpreters?

Thank you for your attention! Patricia Hudelson, Ph. D Medical Anthropologist Department of Community Medicine & Primary Care Geneva University Hospitals Patricia. Hudelson@hcuge. ch
- Slides: 39