General Pediatrics Board Review Nephrology Fluids and Electrolytes

General Pediatrics Board Review Nephrology Fluids and Electrolytes Acid-Base UTI Hypertension Jeffrey M. Saland, M. D. Chief, Nephrology and Hypertension Department of Pediatrics Icahn School of Medicine at Mount Sinai

Why we Study….

Everybody Loves the Board Exam!
Composition of Body Fluids 4
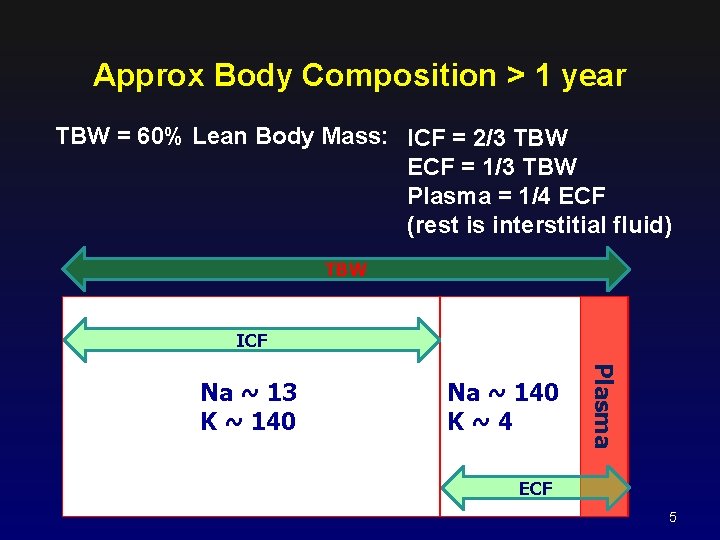
Approx Body Composition > 1 year TBW = 60% Lean Body Mass: ICF = 2/3 TBW ECF = 1/3 TBW Plasma = 1/4 ECF (rest is interstitial fluid) TBW ICF Na ~ 140 K~4 Plasma Na ~ 13 K ~ 140 ECF 5
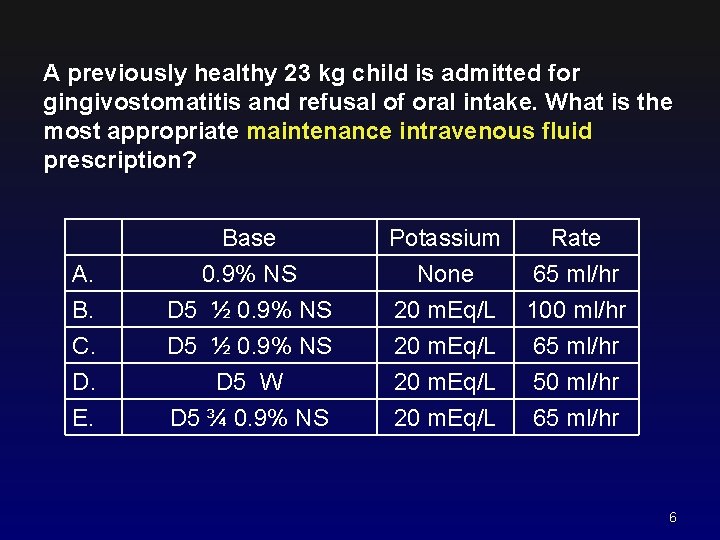

A previously healthy 23 kg child is admitted for gingivostomatitis and refusal of oral intake. What is the most appropriate maintenance intravenous fluid prescription? A. B. C. Base 0. 9% NS D 5 ½ 0. 9% NS Potassium None 20 m. Eq/L Rate 65 ml/hr 100 ml/hr 65 ml/hr D. E. D 5 W D 5 ¾ 0. 9% NS 20 m. Eq/L 50 ml/hr 65 ml/hr 6
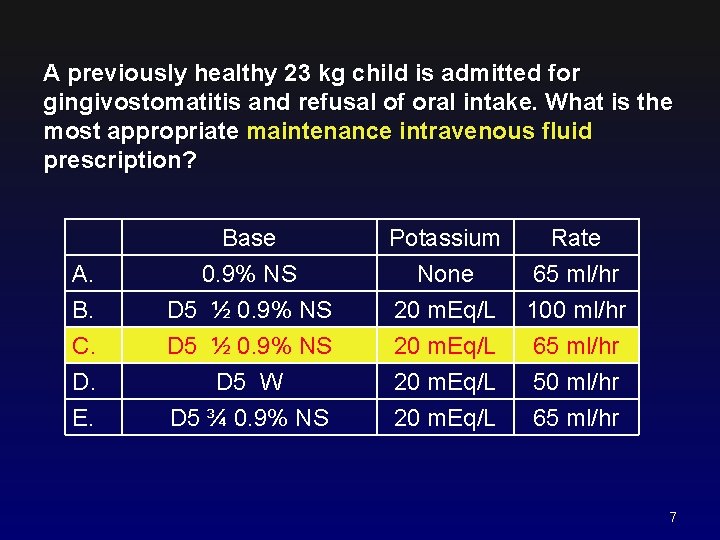
A previously healthy 23 kg child is admitted for gingivostomatitis and refusal of oral intake. What is the most appropriate maintenance intravenous fluid prescription? A. B. C. Base 0. 9% NS D 5 ½ 0. 9% NS Potassium None 20 m. Eq/L Rate 65 ml/hr 100 ml/hr 65 ml/hr D. E. D 5 W D 5 ¾ 0. 9% NS 20 m. Eq/L 50 ml/hr 65 ml/hr 7

What are maintenance fluids? The fluid and electrolytes necessary for a person to remain in net balance over the long term INTAKE ECF Plasma ICF OUTPUT 8

Sounds Easy! 9
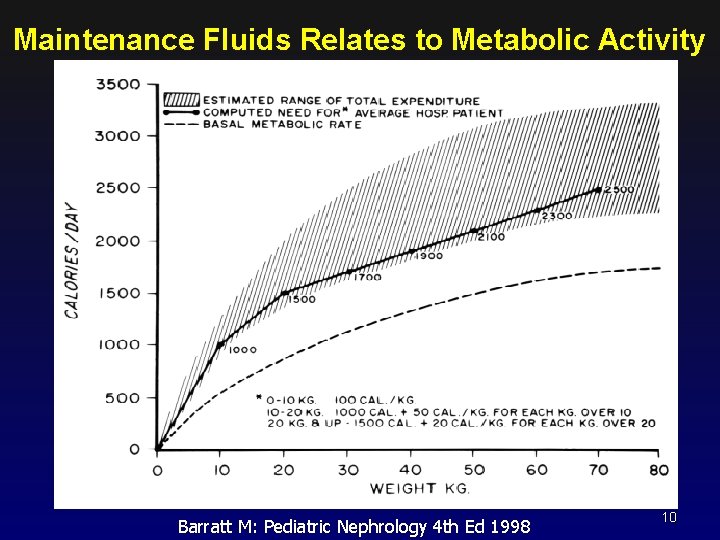
Maintenance Fluids Relates to Metabolic Activity Barratt M: Pediatric Nephrology 4 th Ed 1998 10

For the “average” patient, the use of 1 Cal corresponds to the use of 1 m. L of water Insensible losses: respiratory + evaporative not sweat 30 cc / 100 Cal 15 cc / 100 Cal 45 cc / 100 Cal Urine output losses Stool losses Growth “loss” 50 -75 cc / 100 Cal 5 -10 cc / 100 Cal 0 -15 cc / 100 Cal Water of oxidation (a gain) 10 -15 cc / 100 Cal TOTAL Approximately 100 cc / 100 Cal 11

Summary “maintenance fluids” Fluid needs are linked to the metabolic rate. Maintenance is approximately insensible plus urine losses. Maintenance fluids of the “average” patient are approximately: 1 st 10 kg: 2 nd 10 kg: the rest: 100 cc / kg / day or 4 ml/kg/hr 50 cc / kg / day or 2 ml/kg/hr 20 cc / kg / day or 1 ml/kg/hr 12

Changes in the metabolic rate or the environment change insensible fluid loss Increased INSENSIBLE Losses Fever (each deg > 38): Prematurity Radiant warmer Phototherapy Increased activity 12. 5% 100 -300% 50 -100% 25 -50% 5 -25% Decreased INSENSIBLE Losses Ventilation (humidified air) Sedation Decreased activity Hypothermia Enclosed Incubator 25 -40% 5 -25% 5 -15% 25 -50% 13

Maintenance Fluid DOES NOT Include Abnormal Losses Common / “Community” losses Gastrointestinal: diarrhea, vomiting Activity: sweating, increased ventilation, heat Burns: (even sunburn!) Uncommon / “Nosocomial” losses Drainage (eg chest tube, NG tube, et cetera) Bleeding Pathological renal losses (eg salt wasting, diabetes) These losses are universally hypo- or isotonic 14
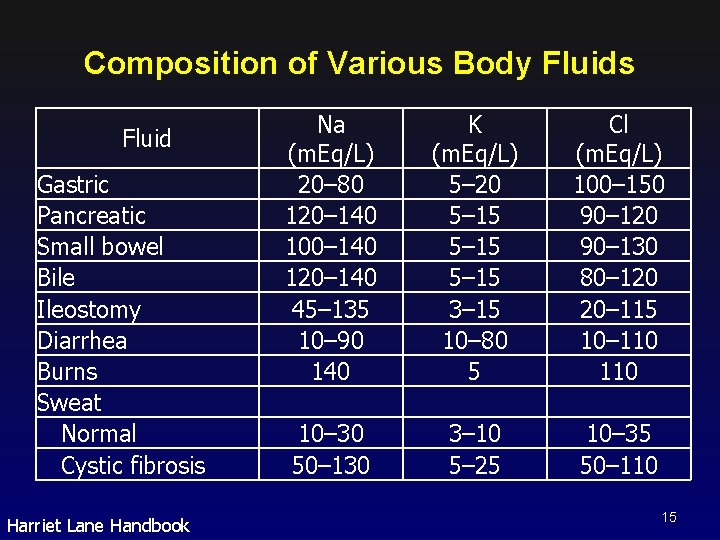
Composition of Various Body Fluids Fluid Gastric Pancreatic Small bowel Bile Ileostomy Diarrhea Burns Sweat Normal Cystic fibrosis Harriet Lane Handbook Na (m. Eq/L) 20– 80 120– 140 100– 140 120– 140 45– 135 10– 90 140 K (m. Eq/L) 5– 20 5– 15 3– 15 10– 80 5 Cl (m. Eq/L) 100– 150 90– 120 90– 130 80– 120 20– 115 10– 110 10– 30 50– 130 3– 10 5– 25 10– 35 50– 110 15

“Salt” Maintenance Requirements Na: K: 2 -5 m. Eq / kg /day 1 -2 m. Eq / kg /day There is a large variability in the intake of Na, and to a lesser extent K, by healthy people. Renal ability to conserve or excrete Na is very large. The ability to conserve or secrete K is also larger than the average variation in intake. 16

17

An 18 month old boy presents to the ER with a history of vomiting and diarrhea for several days. He is lethargic, has poor skin turgor, dry mucus membranes, and has tachycardia. He took 5 ml oral fluid but vomited almost immediately. The next most appropriate step is to: A Give 20 ml/kg of D 5 0. 45% NS intravenously over 20 -30 min Give 5 ml/kg of D 5 0. 9% NS B intravenously over 20 -30 min C Give 20 ml/kg of 0. 9% NS intravenously over 20 -30 min D Give 10 ml/kg of 3% NS intravenously over 20 -30 min E Await serum electrolytes before giving IV fluid TURNING POINT SLIDE: ANSWER IS C 18
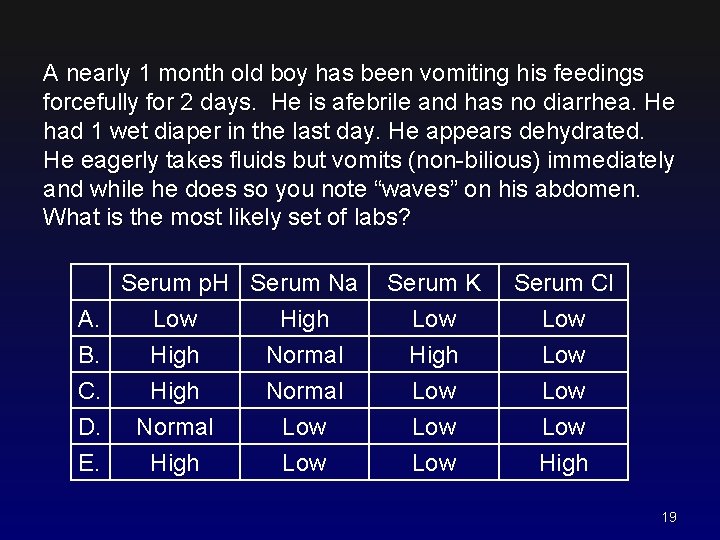
A nearly 1 month old boy has been vomiting his feedings forcefully for 2 days. He is afebrile and has no diarrhea. He had 1 wet diaper in the last day. He appears dehydrated. He eagerly takes fluids but vomits (non-bilious) immediately and while he does so you note “waves” on his abdomen. What is the most likely set of labs? Serum p. H Serum Na A. Low High B. High Normal C. High Normal D. E. Normal High Low Serum K Low High Low Serum Cl Low Low Low High 19

A nearly 1 month old boy has been vomiting his feedings forcefully for 2 days. He is afebrile and has no diarrhea. He had 1 wet diaper in the last day. He appears dehydrated. He eagerly takes fluids but vomits (non-bilious) immediately and while he does so you note “waves” on his abdomen. What is the most likely set of labs? Serum p. H Serum Na A. Low High B. High Normal C. High Normal D. E. Normal High Low Serum K Low High Low Serum Cl Low Low Low High 20

Signs & Symptoms of Dehydration I (fairly reliable) Mild Weight Loss Sensorium Severe 5% (infant) 10% (infant) 15% (infant) 2% (child/adult) 6% (child/adult) 9% (child/adult) Normal Urine Output Slight decrease hrs w/o UOP 2 -3 hours range 0. 5 -1. 5 cc/kg/hr Harriet Lane Handbook Moderate Fussy Lethargic Poor arousability Notable decrease 4 -6 hours <0. 5 cc/kg/hr Anuric 6 -12 hours None 21

Signs & Symptoms of Dehydration II (less reliable) Mild Skin turgor or 1+ decrease quality pale Moderate Severe 2+ decrease “gray” 3+ decrease mottled Drier “parched” Slightly increased Increased Very increased Fontanelle Normal Intermediate Sunken Eyes Normal Intermediate Sunken Blood Pressure Normal About normal Low Mucus Dry / “tacky” Membranes Pulse Harriet Lane Handbook 22

A 2 year-old presents with a 1 day history diarrhea and a 5% weight loss. Which of the following best represents the distribution of the fluid loss? A. B. C. Extracellular Intracellular 80% 20% 60% 40% 60% D. E. 20% 80% None of the above 23

A 2 year-old presents with a 1 day history diarrhea and a 5% weight loss. Which of the following best represents the distribution of the fluid loss? A. B. C. Extracellular Intracellular 80% 20% 60% 40% 60% D. E. 20% 80% None of the above 3 or more days: the correct answer would have been B. The ICF is relatively protected from volume loss. Harriet Lane Handbook 24

A nearly 13 month old girl has had diarrhea for 5 days. She has few wet diapers. Her BP is 86/40, pulse is 135. She weighs 9 kg and you estimate she is 10% dehydrated based on clinical parameters. Which of the following estimates of losses is best? (hint: disregard small Na loss from ICF) (Hint #2 you can get the answer without calculating Na loss at all) A. B. C. Total Deficit 900 m. L 1000 m. L ECF loss 540 ml 800 ml 400 ml ICF loss 360 ml 200 ml 600 ml Na Loss 75 m. Eq 110 m. Eq 55 m. Eq D. E. 1000 m. L 100 m. L 600 ml 80 m. L 400 ml 20 m. L 85 m. Eq 10 m. Eq 25
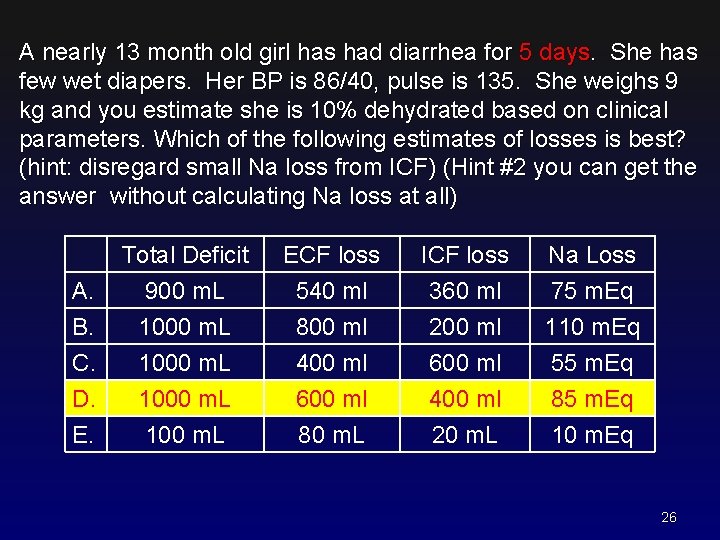
A nearly 13 month old girl has had diarrhea for 5 days. She has few wet diapers. Her BP is 86/40, pulse is 135. She weighs 9 kg and you estimate she is 10% dehydrated based on clinical parameters. Which of the following estimates of losses is best? (hint: disregard small Na loss from ICF) (Hint #2 you can get the answer without calculating Na loss at all) A. B. C. Total Deficit 900 m. L 1000 m. L ECF loss 540 ml 800 ml 400 ml ICF loss 360 ml 200 ml 600 ml Na Loss 75 m. Eq 110 m. Eq 55 m. Eq D. E. 1000 m. L 100 m. L 600 ml 80 m. L 400 ml 20 m. L 85 m. Eq 10 m. Eq 26

Calculating Percent Dehydration A 13 month old child was seen for a checkup and weighed 10 kg. 10 days later in the ER with gastroenteritis she weighs 9 kg. 10% Dehydration. A liter weighs 1 kg for our purposes. 27

A high school student and her friend have multiple episodes of vomiting and watery diarrhea after sharing lunch from a food cart at the park earlier in the day. Her bp is 95/45 and her pulse increases from 90 to 115 standing. She feels light-headed and has not urinated in the last 6 hours. Which is the most likely type of dehydration? A. B. C. D. Isotonic Hypertonic All are equally likely 28

A high school student and her friend have multiple episodes of vomiting and watery diarrhea after sharing lunch from a food cart at the park earlier in the day. Her bp is 95/45 and her pulse increases from 90 to 115 standing. She feels light-headed and has not urinated in the last 6 hours. Which is the most likely type of dehydration? A. B. C. D. Isotonic Hypertonic All are equally likely 29

A 17 year old girl is treated with a prolonged course of antibiotics for sinusitis. She develops profuse watery diarrhea that lasts several days. She had not been eating due to abdominal pain but had taken at least 2 liters of a yellow sports drink each day. In the ER, she still appears moderately dehydrated. You diagnose C. Dificile colitis. The most likely type of dehydration is: A. B. C. D. Isotonic Hypertonic All are equally likely 30

A 17 year old girl is treated with a prolonged course of antibiotics for sinusitis. She develops profuse watery diarrhea that lasts several days. She had not been eating due to abdominal pain but had taken at least 2 liters of a yellow sports drink each day. In the ER, she still appears moderately dehydrated. You diagnose C. Dificile colitis. The most likely type of dehydration is: A. B. C. D. Isotonic Hypertonic All are equally likely 31
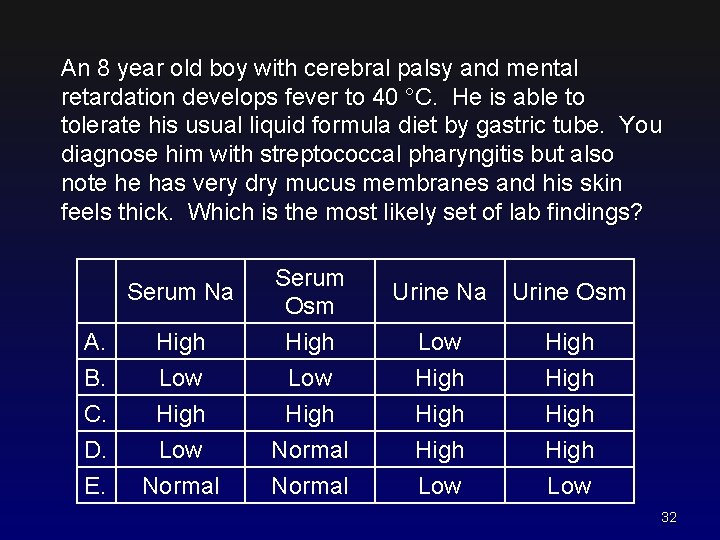
An 8 year old boy with cerebral palsy and mental retardation develops fever to 40 °C. He is able to tolerate his usual liquid formula diet by gastric tube. You diagnose him with streptococcal pharyngitis but also note he has very dry mucus membranes and his skin feels thick. Which is the most likely set of lab findings? A. B. C. D. E. Serum Na Serum Osm Urine Na Urine Osm High Low Normal High Low High Normal Low High High Low 32
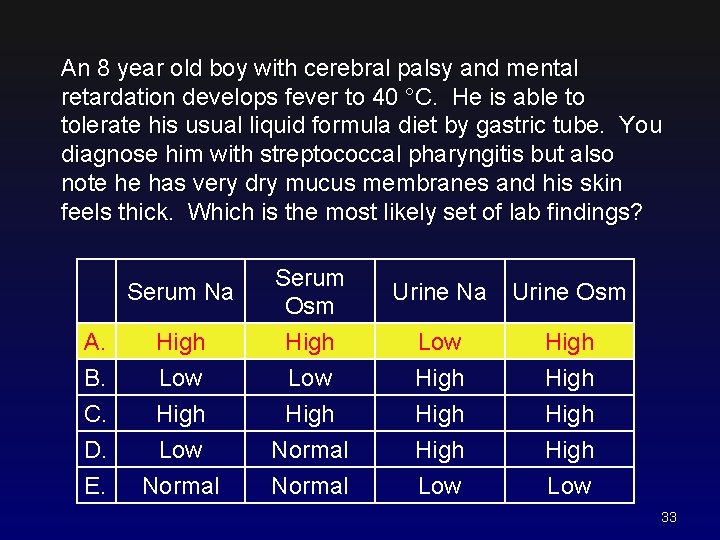
An 8 year old boy with cerebral palsy and mental retardation develops fever to 40 °C. He is able to tolerate his usual liquid formula diet by gastric tube. You diagnose him with streptococcal pharyngitis but also note he has very dry mucus membranes and his skin feels thick. Which is the most likely set of lab findings? A. B. C. D. E. Serum Na Serum Osm Urine Na Urine Osm High Low Normal High Low High Normal Low High High Low 33
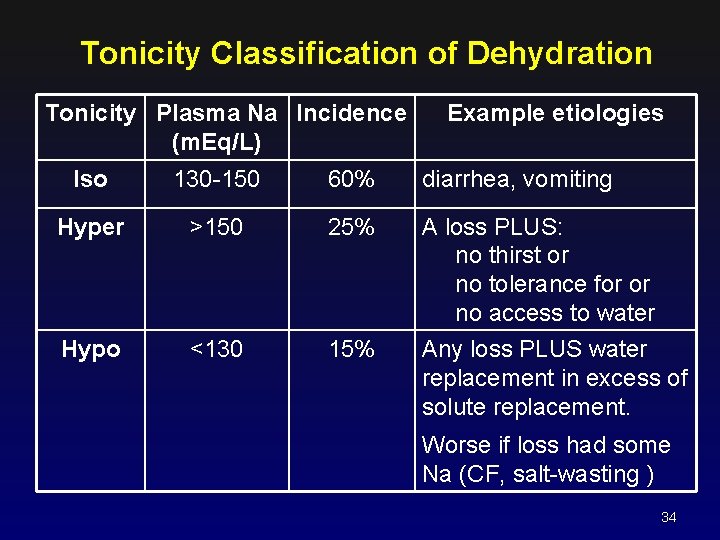
Tonicity Classification of Dehydration Tonicity Plasma Na Incidence (m. Eq/L) Example etiologies Iso 130 -150 60% diarrhea, vomiting Hyper >150 25% Hypo <130 15% A loss PLUS: no thirst or no tolerance for or no access to water Any loss PLUS water replacement in excess of solute replacement. Worse if loss had some Na (CF, salt-wasting ) 34

35

A 10 year old boy has high fever and dehydration due to seasonal influenza. He has not urinated in over 24 hours. His serum creatinine is elevated from 0. 7 to 1. 6. Urine is taken to calculate fractional excretion of Na. Two days later he is rehydrated and has normal urine output and his creatinine is baseline. What best describes his diagnosis and most likely FENa on presentation? Diagnosis Acute Kidney A Injury Acute Kidney B Injury C D Pre-Renal Azotemia FENa 3% TURNING POINT SLIDE: ANSWER IS D 0. 3% 3% 0. 3% 36

Example: How to calculate the FENa SERUM: Na 124, K 4, Cl 94, Total CO 2 12 Creat 0. 8 mg/d. L, BUN 40, Glucose 70 URINE: specific gravity 1. 030, trace protein, no blood or glucose, small ketones; urine Na 15, creat 40 37

FENa is a useful test when: • The urine output is low. • No current use of diuretics. < 1% (0. 01): pre-renal azotemia (“acute renal success”) > 2% (0. 02): acute kidney injury (“acute renal failure”) Exceptions: acute GN has low FENa, obstruction can vary 38
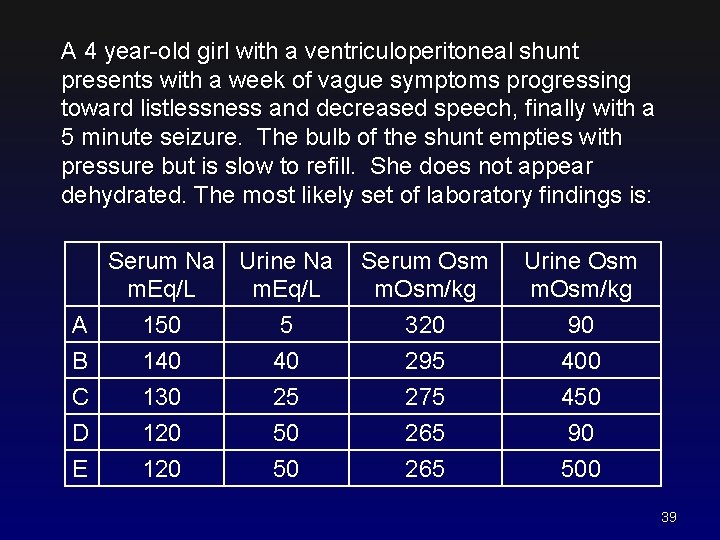
A 4 year-old girl with a ventriculoperitoneal shunt presents with a week of vague symptoms progressing toward listlessness and decreased speech, finally with a 5 minute seizure. The bulb of the shunt empties with pressure but is slow to refill. She does not appear dehydrated. The most likely set of laboratory findings is: Serum Na Urine Na m. Eq/L A B C D E 150 140 130 120 5 40 25 50 50 Serum Osm m. Osm/kg Urine Osm m. Osm/kg 320 295 275 265 90 400 450 90 500 39
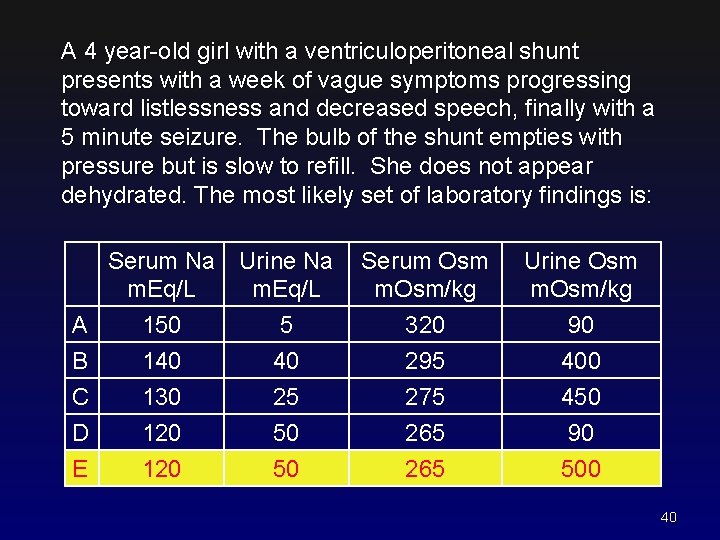
A 4 year-old girl with a ventriculoperitoneal shunt presents with a week of vague symptoms progressing toward listlessness and decreased speech, finally with a 5 minute seizure. The bulb of the shunt empties with pressure but is slow to refill. She does not appear dehydrated. The most likely set of laboratory findings is: Serum Na Urine Na m. Eq/L A B C D E 150 140 130 120 5 40 25 50 50 Serum Osm m. Osm/kg Urine Osm m. Osm/kg 320 295 275 265 90 400 450 90 500 40

SIADH: Too Much ADH Etiologies: • CNS disease (hydrocephalus, meningitis, etc) • Lung (pneumonia, RSV, etc) • Nausea or Pain • Cancer or Stem Cell transplantation • Drugs (SSRI’s) Should exclude: • Thyroid, adrenal, cardiac, or renal disease • Volume deficits / dehydration Hyponatremia, inappropriately high urine Osm (>100) Urine Na can be variable– usually “highish” 41
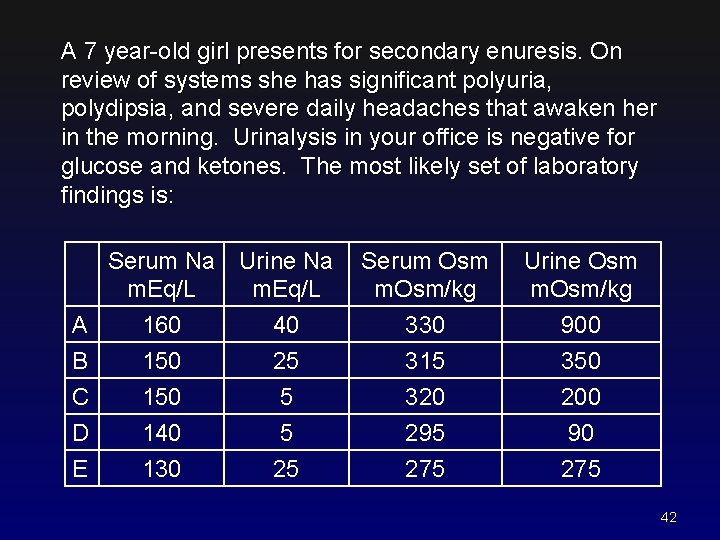

A 7 year-old girl presents for secondary enuresis. On review of systems she has significant polyuria, polydipsia, and severe daily headaches that awaken her in the morning. Urinalysis in your office is negative for glucose and ketones. The most likely set of laboratory findings is: Serum Na Urine Na m. Eq/L A B C D E 160 150 140 130 40 25 5 5 25 Serum Osm m. Osm/kg Urine Osm m. Osm/kg 330 315 320 295 275 900 350 200 90 275 42
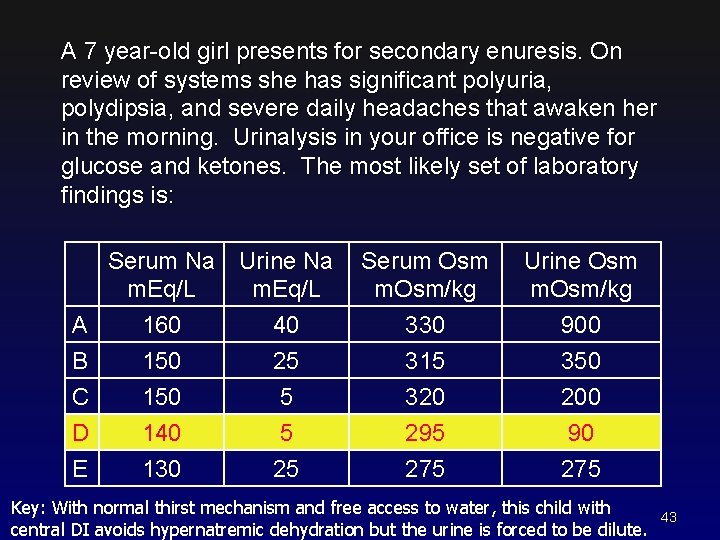

A 7 year-old girl presents for secondary enuresis. On review of systems she has significant polyuria, polydipsia, and severe daily headaches that awaken her in the morning. Urinalysis in your office is negative for glucose and ketones. The most likely set of laboratory findings is: Serum Na Urine Na m. Eq/L A B C D E 160 150 140 130 40 25 5 5 25 Serum Osm m. Osm/kg Urine Osm m. Osm/kg 330 315 320 295 275 900 350 200 90 275 Key: With normal thirst mechanism and free access to water, this child with central DI avoids hypernatremic dehydration but the urine is forced to be dilute. 43

Diabetes Insipidus: Not Enough ADH Or ADH not Effective Etiologies: • CNS disease (pituitary infiltration, damage) • Drugs (lithium) • Nephrogenic (V 2 receptor or aquaporin defect) • Others more rare With access to water, just polyuria, polydipsia Without access to water, hypernatremia, polyuria, polydipsia Hypernatremic dehydration • Inappropriately dilute urine • Water deprivation test diagnostic but dangerous • Response to DDAVP diagnostic of central DI • Genetic testing for nephrogenic DI 44

An overweight 15 year old girl is admitted with polyuria and severe dehydration. Severe hyperglycemia of 800 mg/dl without ketoacidosis is discovered. Serum electrolytes are significant for Na of 140, K of 4. 3, Cl of 98, CO 2 of 19, BUN is 53, Creatinine is 1. 6. Which of the following is NOT true? A Excessive 0. 9% NS may exacerbate the situation B Serum K can be expected to fall with rehydration. TURNING POINT SLIDE: ANSWER IS D C Serum Na can be expected to rise with rehydration D Hyperglycemia causes the lab equipment to malfunction and produce falsely low Na values E Dehydration is the result of osmotic diuresis 45

Acid / Base Mr. Osborne, may I be excused? My brain is full. 46

Calculating the Serum Anion Gap Formula: Measured Cations minus Measured Anions Na plus (K) minus Cl minus CO 2 (K is often excluded) Fact: The ACTUAL cations = the ACTUAL anions Fact: Many organic anions / acids are not measured USUALLY: the anion gap is < 16 (with K) or <12 (without K) HIGH gap implies more than usual “unmeasured” anions LOW gap generally results from low albumin Low Gap Acidosis = CO 2 loss Basically: RTA or diarrhea 47

A 6 month old girl born at term and with no apparent illnesses presents with failure to thrive. She is mildly tachypneic at rest. Lab evaluation is remarkable for serum Na 140, K 2. 5, Chloride of 115, bicarbonate of 11 and creatinine of 0. 3 mg/d. L. Which of the following is most consistent with distal (type I) renal tubular acidosis (RTA)? A B C D E Urine p. H Urine Ca Citrate K 6. 5 < 5. 5 >7 >7 High Low Low Low High High Low Urine Anion Gap (Na+ + K+) - Cl> 0 (positive) < 0 (negative) 48
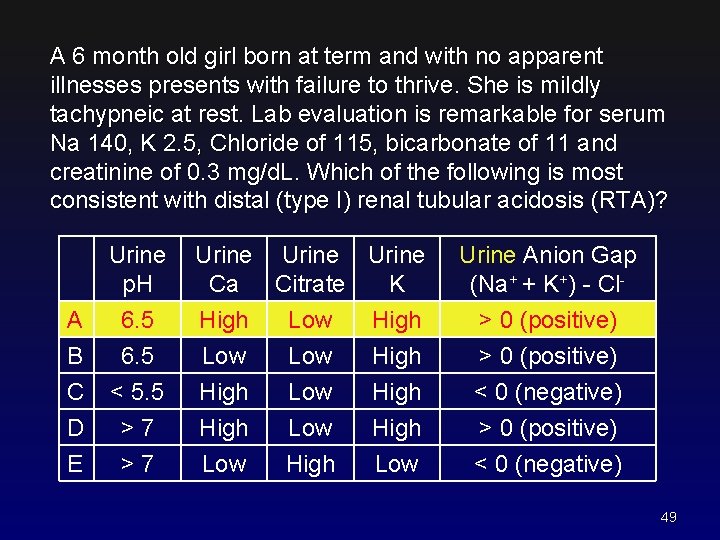
A 6 month old girl born at term and with no apparent illnesses presents with failure to thrive. She is mildly tachypneic at rest. Lab evaluation is remarkable for serum Na 140, K 2. 5, Chloride of 115, bicarbonate of 11 and creatinine of 0. 3 mg/d. L. Which of the following is most consistent with distal (type I) renal tubular acidosis (RTA)? A B C D E Urine p. H Urine Ca Citrate K 6. 5 < 5. 5 >7 >7 High Low Low Low High High Low Urine Anion Gap (Na+ + K+) - Cl> 0 (positive) < 0 (negative) 49

Renal Tubular Acidosis Associated with growth failure Low serum anion gap metabolic acidosis May be compensated by pulmonary hyperventilation Urine anion gap should be positive: (Na+ + K+) > Cl. Clinical pearls: • Confirm metabolic acidosis with a VBG • Distal RTA (type I) is most common • Types I and II have hypokalemia • Type IV has hyperkalemia (aldosterone defect) • Can be treated with bicitra with varying success 50
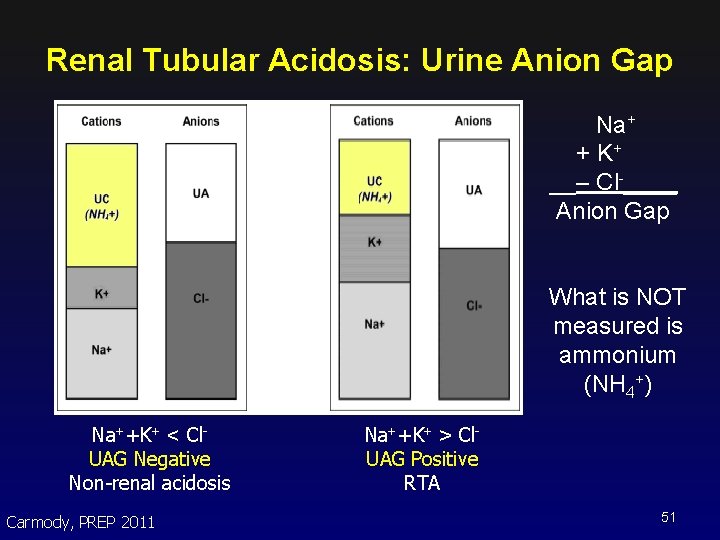
Renal Tubular Acidosis: Urine Anion Gap Na+ + K+ __– Cl-____ Anion Gap What is NOT measured is ammonium (NH 4+) Na++K+ < Cl. UAG Negative Non-renal acidosis Carmody, PREP 2011 Na++K+ > Cl. UAG Positive RTA 51

Renal Tubular Acidosis: Distal vs Proximal Distal (type 1) • Commonly associated with hypercalc. URIA, stone risk • Late nephron defect, urine p. H “always” > 5. 5 • Low urine citrate • Distal RTA (type I) can associate with deafness Proximal (type 2) • More rare • Often associated with Renal Fanconi Syndrome • Lower threshold of bicarbonate reabsorption • Urine p. H depends on plasma bicarbonate, may be < 5. 5 52
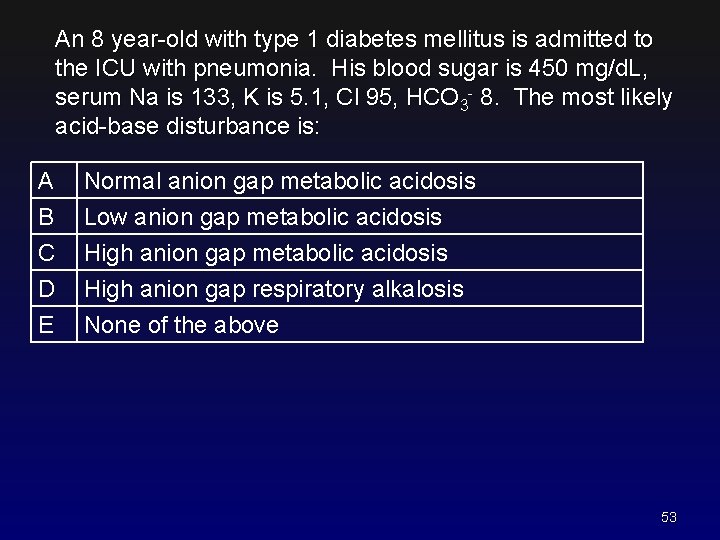

An 8 year-old with type 1 diabetes mellitus is admitted to the ICU with pneumonia. His blood sugar is 450 mg/d. L, serum Na is 133, K is 5. 1, Cl 95, HCO 3 - 8. The most likely acid-base disturbance is: A B C D E Normal anion gap metabolic acidosis Low anion gap metabolic acidosis High anion gap respiratory alkalosis None of the above 53

An 8 year-old with type 1 diabetes mellitus is admitted to the ICU with pneumonia. His blood sugar is 450 mg/d. L, serum Na is 133, K is 5. 1, Cl 95, HCO 3 - 8. The most likely acid-base disturbance is: A B C D E Normal anion gap metabolic acidosis Low anion gap metabolic acidosis High anion gap respiratory alkalosis None of the above Don’t forget– we ASSUMED the p. H was low because metabolic acidosis is so likely. We really need a blood gas to know for sure! 54

High Anion Gap Metabolic Acidosis: M: U: D: P: I: L: E: S: methanol (and metabolic diseases) uremia diabetes (ketoacids), d-lactic acidosis (paraldehyde); propylene glycol Isoniazid, Iron Lactate Ethanol, Ethylene glycol Salicylates 55
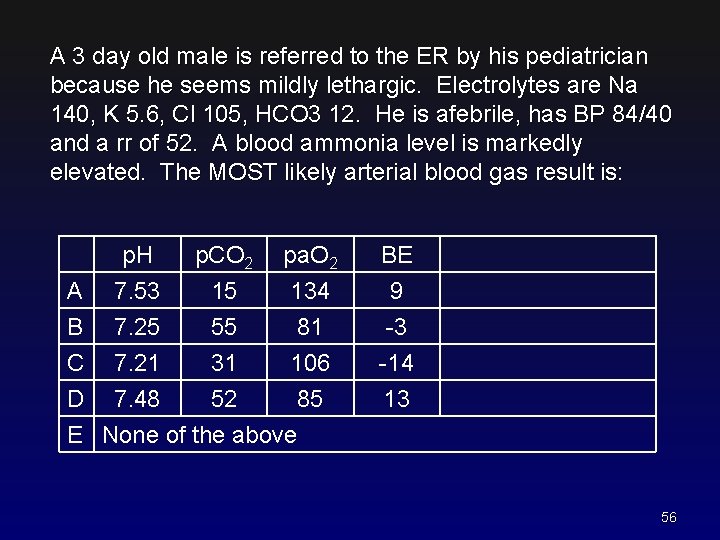

A 3 day old male is referred to the ER by his pediatrician because he seems mildly lethargic. Electrolytes are Na 140, K 5. 6, Cl 105, HCO 3 12. He is afebrile, has BP 84/40 and a rr of 52. A blood ammonia level is markedly elevated. The MOST likely arterial blood gas result is: A B C p. H 7. 53 7. 25 7. 21 p. CO 2 15 55 31 pa. O 2 134 81 106 D 7. 48 52 85 E None of the above BE 9 -3 -14 13 56
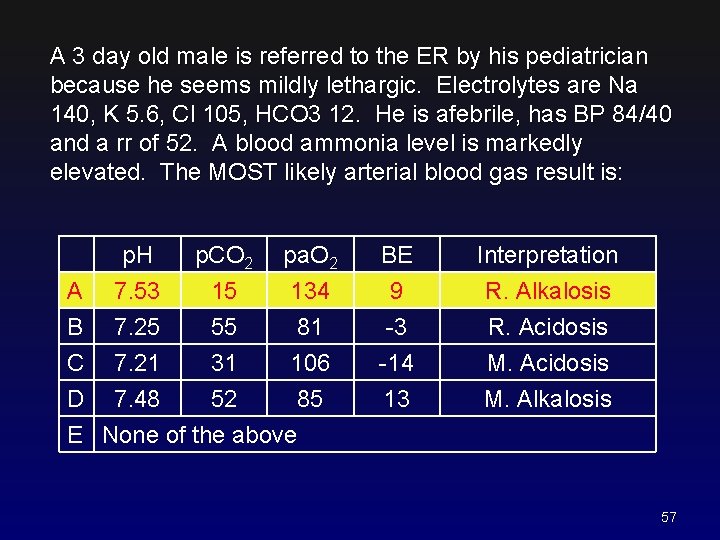
A 3 day old male is referred to the ER by his pediatrician because he seems mildly lethargic. Electrolytes are Na 140, K 5. 6, Cl 105, HCO 3 12. He is afebrile, has BP 84/40 and a rr of 52. A blood ammonia level is markedly elevated. The MOST likely arterial blood gas result is: A B C p. H 7. 53 7. 25 7. 21 p. CO 2 15 55 31 pa. O 2 134 81 106 D 7. 48 52 85 E None of the above BE 9 -3 -14 Interpretation R. Alkalosis R. Acidosis M. Acidosis 13 M. Alkalosis 57
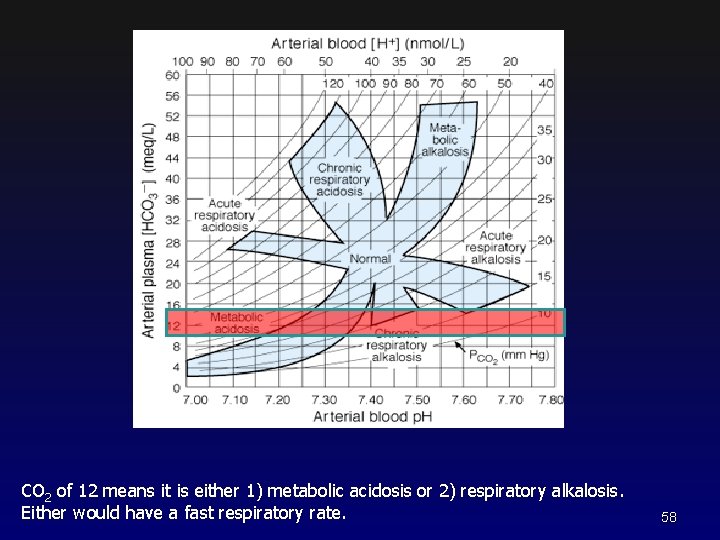
CO 2 of 12 means it is either 1) metabolic acidosis or 2) respiratory alkalosis. Either would have a fast respiratory rate. 58
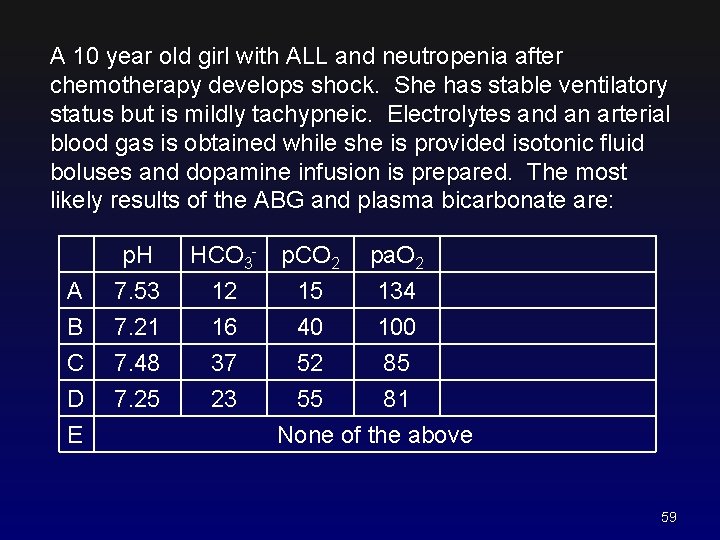
A 10 year old girl with ALL and neutropenia after chemotherapy develops shock. She has stable ventilatory status but is mildly tachypneic. Electrolytes and an arterial blood gas is obtained while she is provided isotonic fluid boluses and dopamine infusion is prepared. The most likely results of the ABG and plasma bicarbonate are: A B C D E p. H 7. 53 7. 21 7. 48 7. 25 HCO 3 - p. CO 2 12 15 16 40 37 52 23 pa. O 2 134 100 85 55 81 None of the above 59
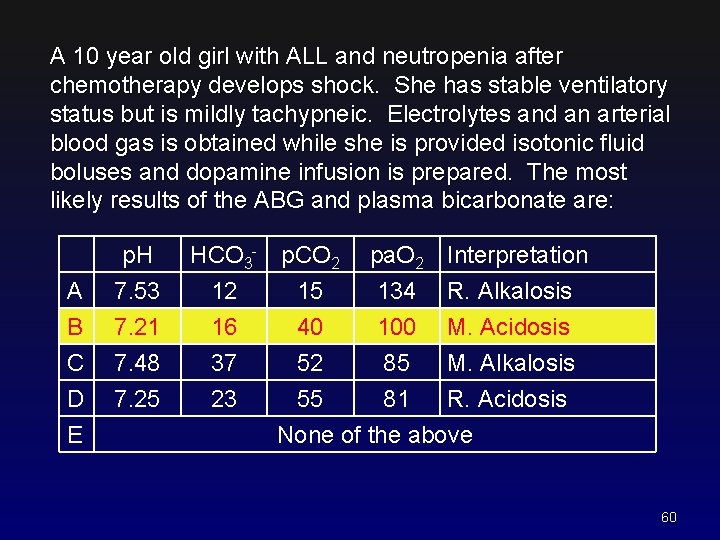
A 10 year old girl with ALL and neutropenia after chemotherapy develops shock. She has stable ventilatory status but is mildly tachypneic. Electrolytes and an arterial blood gas is obtained while she is provided isotonic fluid boluses and dopamine infusion is prepared. The most likely results of the ABG and plasma bicarbonate are: A B C D E p. H 7. 53 7. 21 7. 48 7. 25 HCO 3 - p. CO 2 12 15 16 40 37 52 23 pa. O 2 134 100 85 Interpretation R. Alkalosis M. Acidosis M. Alkalosis 55 81 R. Acidosis None of the above 60
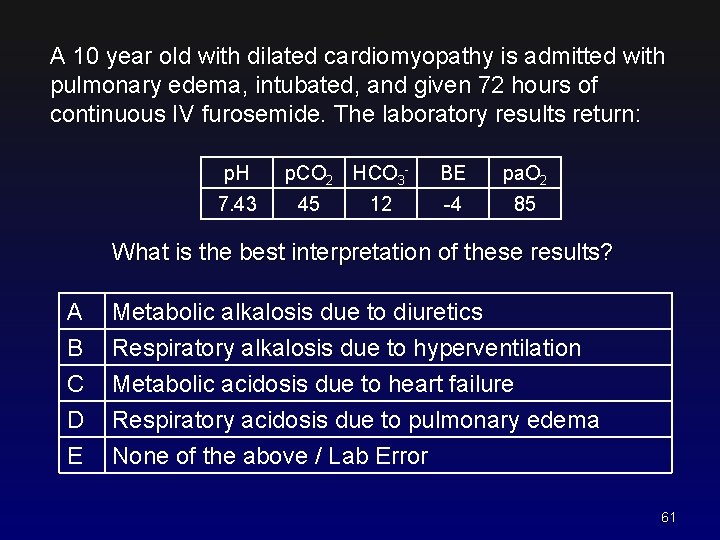
A 10 year old with dilated cardiomyopathy is admitted with pulmonary edema, intubated, and given 72 hours of continuous IV furosemide. The laboratory results return: p. H 7. 43 p. CO 2 HCO 345 12 BE pa. O 2 -4 85 What is the best interpretation of these results? A B C D Metabolic alkalosis due to diuretics Respiratory alkalosis due to hyperventilation Metabolic acidosis due to heart failure Respiratory acidosis due to pulmonary edema E None of the above / Lab Error 61
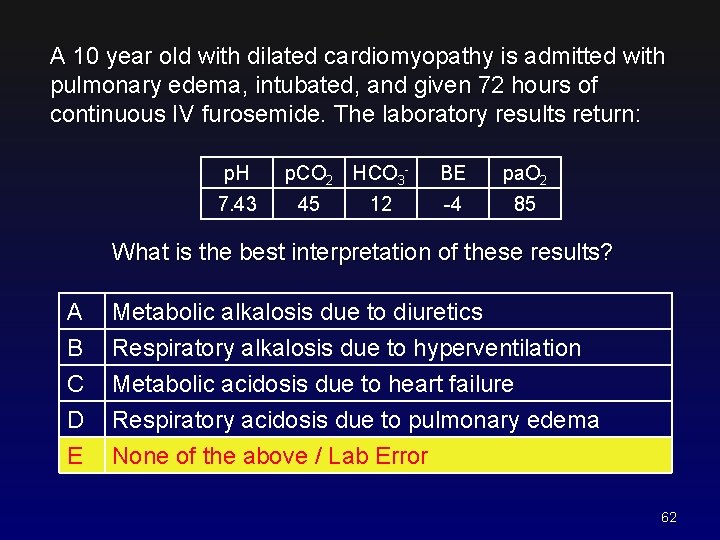
A 10 year old with dilated cardiomyopathy is admitted with pulmonary edema, intubated, and given 72 hours of continuous IV furosemide. The laboratory results return: p. H 7. 43 p. CO 2 HCO 345 12 BE pa. O 2 -4 85 What is the best interpretation of these results? A B C D Metabolic alkalosis due to diuretics Respiratory alkalosis due to hyperventilation Metabolic acidosis due to heart failure Respiratory acidosis due to pulmonary edema E None of the above / Lab Error 62

General Electrolytes 63

A 6 month old boy develops diarrhea for 4 days. He appears dehydrated and is given a bolus of 0. 9% NS and promptly produces a generous wet diaper. Electrolytes are obtained with difficulty during the blood draw and return the following values: Na 143, K 7. 3, Cl 109, CO 2 14, Ca is 10. 1 mg/dl. The next step in management is A B C D Repeat the laboratory tests in 24 hours Administer intravenous Calcium gluconate Administer intravenous sodium bicarbonate Begin intravenous D 5 ½ 0. 9% NS with 20 m. Eq KCl per liter at 1. 5 times maintenance rate E None of the above 64

A 6 month old boy develops diarrhea for 4 days. He appears dehydrated and is given a bolus of 0. 9% NS and promptly produces a generous wet diaper. Electrolytes are obtained with difficulty during the blood draw and return the following values: Na 143, K 7. 3, Cl 109, CO 2 14, Ca is 10. 1 mg/dl. The next step in management is A B C D Repeat the laboratory tests in 24 hours Administer intravenous Calcium gluconate Administer intravenous sodium bicarbonate Begin intravenous D 5 ½ 0. 9% NS with 20 m. Eq KCl per liter at 1. 5 times maintenance rate E None of the above 65

A 9 year old boy is chronically treated with oral furosemide for vascular congestion related to dilated cardiomyopathy. All of the following electrolyte disturbances are likely EXCEPT: A B C D Hypokalemia Hypophosphatemia Hypocalcemia Hyponatremia E Hypomagnesemia 66

A 9 year old boy is chronically treated with oral furosemide for vascular congestion related to dilated cardiomyopathy. All of the following electrolyte disturbances are likely EXCEPT: A B C D Hypokalemia Hypophosphatemia Hypocalcemia Hyponatremia E Hypomagnesemia 67

Hyperkalemia can be induced by all of the following medications EXCEPT: A B C D Intravenous terbutaline Epinephrine Angiotensin converting enzyme inhibitor Hydrochlorthiazide (HCTZ) E Spironolactone 68

Hyperkalemia can be induced by all of the following medications EXCEPT: A B C D Intravenous terbutaline Epinephrine Angiotensin converting enzyme inhibitor Hydrochlorthiazide (HCTZ) E Spironolactone 69

UTI’s and So on… 70

An otherwise healthy, well-grown 4 year-old girl has had 3 febrile UTIs, the first at age 3 years. She has been taking TMP/SMX since the 2 nd UTI. Review of systems reveals constipation. She has occasional enuresis but no frequency or dysuria. Renal sonography and voiding cystourethrogram (VCUG) are normal. Which of the following is likely to be helpful in her evaluation and treatment? A B C D Renal scintigraphy Evaluation for immunodeficiency Increase daily fluid intake to 2 – 2. 5 liters/day Prescribe stool softener & a regular bowel routine E Switch prophylaxis to nitrofurantoin 71

An otherwise healthy, well-grown 4 year-old girl has had 3 febrile UTIs, the first at age 3 years. She has been taking TMP/SMX since the 2 nd UTI. Review of systems reveals constipation. She has occasional enuresis but no frequency or dysuria. Renal sonography and voiding cystourethrogram (VCUG) are normal. Which of the following is likely to be helpful in her evaluation and treatment? A B C D Renal scintigraphy Evaluation for immunodeficiency Increase daily fluid intake to 2 – 2. 5 liters/day Prescribe stool softener & a regular bowel routine E Switch prophylaxis to nitrofurantoin 72

A 3 month old male has a febrile UTI with E. Coli. His renal ultrasound is negative. The best to evaluate for vesicoureteral reflux (VUR) is: A B C D 99 Tc DTPA renal scintigraphy 99 Tc DMSA renal scintigraphy Voiding cystourethrogram Urodynamics study E Magnetic resonance (MR) urogram 73

A 3 month old male has a febrile UTI with E. Coli. His renal ultrasound is negative. The best to evaluate for vesicoureteral reflux (VUR) is: A B C D 99 Tc DTPA renal scintigraphy 99 Tc DMSA renal scintigraphy Voiding cystourethrogram Urodynamics study E Magnetic resonance (MR) urogram 74

All of the following statements about UTI are correct EXCEPT: A Under the age of 1 year, the risk of UTI in females is greater than in males B Circumcision of boys does not affect the risk of UTI C The prevalence of UTI in febrile infants under 3 months of age and without an obvious source on clinical examination is 5 -10% D The incidence of UTI in patients with abnormal urinary tract anatomy is greater than in those with normal urinary tract anatomy E There is controversy whether a 1 st UTI requires evaluation if a prenatal sonogram was normal. 75

All of the following statements about UTI are correct EXCEPT: A Under the age of 1 year, the risk of UTI in females is greater than in males * B Circumcision of boys does not affect the risk of UTI C The prevalence of UTI in febrile infants under 3 months of age and without an obvious source on clinical examination is 5 -10% D The incidence of UTI in patients with abnormal urinary tract anatomy is greater than in those with normal urinary tract anatomy E There is controversy whether a 1 st UTI requires evaluation if a prenatal sonogram was normal. * 0 -3 months male>>female, then it reverses 76

An 8 month old male is found to have grade II VUR on the right and grade IV VUR on the left with mild hydronephrosis. Which of the following actions is most correct? A Commence daily antibiotic prophylaxis B Commence antibiotic prophylaxis and repeat VCUG in 6 months C Watchful waiting, antibiotic prophylaxis for VUR is unnecessary. D Antibiotic prophylaxis and left ureteral reimplant E Reassure the family their son’s VUR is likely to fully resolve without intervention 77

An 8 month old male is found to have grade II VUR on the right and grade IV VUR on the left with mild hydronephrosis. Which of the following actions is most correct? A Commence daily antibiotic prophylaxis B Commence antibiotic prophylaxis and repeat VCUG in 6 months C Watchful waiting, antibiotic prophylaxis for VUR is unnecessary. D Antibiotic prophylaxis and left ureteral reimplant E Reassure the family their son’s VUR is likely to fully resolve without intervention 78

Besides fever, signs and symptoms of UTI in infants include: A B C D E Irritability Diarrhea Difficulty feeding Jaundice Any of the above 79

Besides fever, signs and symptoms of UTI in infants include: A B C D E Irritability Diarrhea Difficulty feeding Jaundice Any of the above 80

An 8 year old boy in the 3 rd grade develops secondary nocturnal enuresis. On review of systems he has constipation. When he was a newborn you had ordered a spinal ultrasound and x-ray after noting a sacral dimple, and both were normal. Urinalysis is negative for leukocyte esterase and nitrates. The next most appropriate steps are: A B C D Renal and bladder ultrasound Spine MRI and referral to pediatric neurosurgery Prescribe stool softener & a regular bowel routine Referral to pediatric urology E Reduce evening fluids & use a bedtime wetting alarm 81

An 8 year old boy in the 3 rd grade develops secondary nocturnal enuresis. On review of systems he has constipation. When he was a newborn you had ordered a spinal ultrasound and x-ray after noting a sacral dimple, and both were normal. Urinalysis is negative for leukocyte esterase and nitrates. The next most appropriate steps are: A B C D Renal and bladder ultrasound Spine MRI and referral to pediatric neurosurgery Prescribe stool softener & a regular bowel routine Referral to pediatric urology E Reduce evening fluids & use a bedtime wetting alarm 82
Nephrology 83
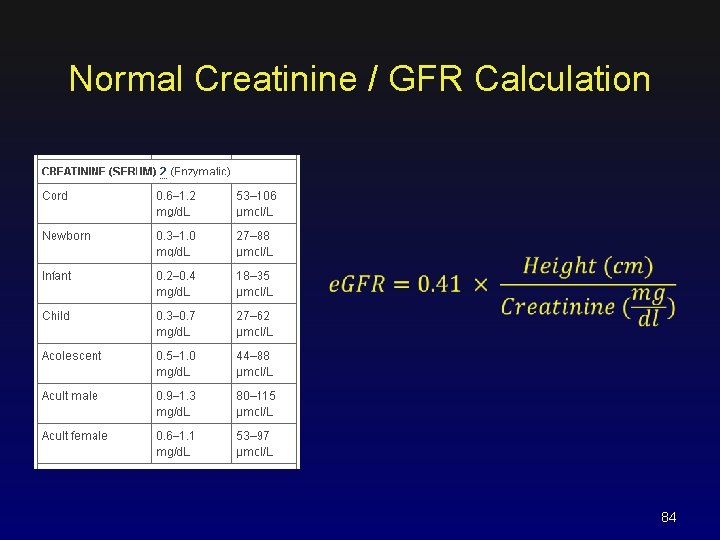
Normal Creatinine / GFR Calculation 84

A 3 year-old boy is referred to pediatric nephrology for sudden onset of edema and 4+ proteinuria. True statements about the nephrotic syndrome in this child include: A The majority of children will respond to corticosteroid treatment within 1 week B IV infusion of 25% albumin and furosemide will decrease recovery time C Progression to renal failure is likely D Steroid response is predictive of renal histology E A family history of nephrotic syndrome is common 85

A 3 year-old boy is referred to pediatric nephrology for sudden onset of edema and 4+ proteinuria. True statements about the nephrotic syndrome in this child include: A The majority of children will respond to corticosteroid treatment within 1 week B IV infusion of 25% albumin and furosemide will decrease recovery time C Progression to renal failure is likely D Steroid response is predictive of renal histology E A family history of nephrotic syndrome is common 86

A 14 year-old overweight girl has proteinuria 100 mg/d. L on two separate occasions, first noted during a screening examination for summer camp. The remainder of the urinalysis is normal and the blood pressure is normal. The most appropriate next step in management is: A B C D Request a hemoglobin A 1 C Renal and bladder ultrasonography Request a urine culture Request a first morning urine protein and creatinine E Request a 24 hour urine collection for protein 87

A 14 year-old overweight girl has proteinuria 100 mg/d. L on two separate occasions, first noted during a screening examination for summer camp. The remainder of the urinalysis is normal and the blood pressure is normal. The most appropriate next step in management is: A B C D Request a hemoglobin A 1 C Renal and bladder ultrasonography Request a urine culture Request a first morning urine protein and creatinine E Request a 24 hour urine collection for protein Orthostatic (postural) proteinuria is evaluated by a first morning urine 88

A 16 year old boy has microscopic hematuria on a urinalysis done for a school form. Family history is significant for his mother having microscopic hematuria since childhood. A maternal uncle required dialysis. Which of the following is true of this boy’s condition? A B C D It is associated with conductive hearing loss It is associated with retinal abnormalities Immunoglobulin A levels are elevated in 50% of cases Female carriers are at risk of kidney failure E Skin biopsy may reveal leukocytoclastic vasculitis 89

A 16 year old boy has microscopic hematuria on a urinalysis done for a school form. Family history is significant for his mother having microscopic hematuria since childhood. A maternal uncle required dialysis. Which of the following is true of this boy’s condition? A B C D It is associated with conductive hearing loss It is associated with retinal abnormalities Immunoglobulin A levels are elevated in 50% of cases Female carriers are at risk of kidney failure E Skin biopsy may reveal leukocytoclastic vasculitis Alport Disease = Hereditary nephritis 90

A 13 year old boy has microscopic hematuria on a urinalysis done for a school form. Family history is significant for his father and a paternal grandparent having long-standing microscopic hematuria. There is no family history of kidney failure. There is no proteinuria. Blood pressure, urine calcium, and renal/bladder sonography is normal. Which of the following is true? A There is an elevated risk of kidney stones B Renal biopsy is indicated C The glomerular basement membrane often appears thick by electron microscopic examination. D Female carriers are at risk of kidney failure E None of the above 91

A 13 year old boy has microscopic hematuria on a urinalysis done for a school form. Family history is significant for his father and a paternal grandparent having long-standing microscopic hematuria. There is no family history of kidney failure. There is no proteinuria. Blood pressure, urine calcium, and renal/bladder sonography is normal. Which of the following is true? A There is an elevated risk of kidney stones B Renal biopsy is indicated C The glomerular basement membrane often appears thick by electron microscopic examination. D Female carriers are at risk of kidney failure E None of the above Benign familial hematuria = thin basement membranes -- benign 92

A 3 day old male infant has been is brought to the ER for blood in the diaper, which the family produces. The diaper has multiple brick-red discolorations in the front. There is no significant perinatal history. Exam finds a vigorous infant in no distress with normal blood pressure. Bagged urinalysis is negative for blood by dipstick and by microscopy. The most likely cause of these findings is: A B C D Hemoglobinuria Sickle cell trait Calcium oxalate crystals Uric acid crystals E Porphyria 93

A 3 day old male infant has been is brought to the ER for blood in the diaper, which the family produces. The diaper has multiple brick-red discolorations in the front. There is no significant perinatal history. Exam finds a vigorous infant in no distress with normal blood pressure. Bagged urinalysis is negative for blood by dipstick and by microscopy. The most likely cause of these findings is: A B C D Hemoglobinuria Sickle cell trait Calcium oxalate crystals Uric acid crystals E Porphyria 94

Hematuria Red Urine Hematuria See Harriet Lane list– favorites for the boards! (eg beets, blackberries, urates, rifampin) In reality, red urine that is not blood is not commonly encountered in practice, except maybe red diaper urates. Important uncommon causes: hemoglobinuria myoglobinuria 95

A 16 year old boy develops sharp flank pain and gross hematuria. Sonography shows multiple large “soap bubble” cysts in each kidney. The mother reports that her mother, who lived in a developing country, suffered from episodes of painful blood in the urine and died with a kidney disease in her 40’s. Which of the following is true? A The disease is associated with hearing loss B The disease is associated with intracranial aneurysms C An older brother, age 20, has a normal sonogram and therefore does not carry the gene D Both parents are carriers of the gene E This disease is found in about 1 in 5000 people 96

A 16 year old boy develops sharp flank pain and gross hematuria. Sonography shows multiple large “soap bubble” cysts in each kidney. The mother reports that her mother, who lived in a developing country, suffered from episodes of painful blood in the urine and died with a kidney disease in her 40’s. Which of the following is true? A The disease is associated with hearing loss B The disease is associated with intracranial aneurysms C An older brother, age 20, has a normal sonogram and therefore does not carry the gene D Both parents are carriers of the gene E This disease is found in about 1 in 5000 people 97

Polycystic Kidney Disease Autosomal Dominant PKD (ADPKD) • More commonly affects adults • Larger cysts, liver cysts • Intracranial aneurysms • Mitral valve prolapse, aortic root dilitation • Common: affects about 1: 1000 Autosomal Recessive PKD (ARPKD) • More commonly affects infants • Smaller cysts, liver fibrosis (ductal plate malformation) • May need liver and/or kidney transplant • Rare: affects about 1 in 20, 000 -40, 000 people 98

A 12 year old boy develops sharp flank pain and gross hematuria. His father has had several kidney stones and has required surgery for them once. Sonography shows mild unilateral hydronephrosis but no kidney stone. All of the following are true EXCEPT? A Increasing fluid intake is therapeutic B The sonogram does NOT rule out the presence of a kidney stone. C The risk of kidney stones increases with higher calcium intake D A 24 hour urine analysis can help determine risk factors for stone formation E Crohn’s disease increases the risk of kidney stones 99

A 12 year old boy develops sharp flank pain and gross hematuria. His father has had several kidney stones and has required surgery for them once. Sonography shows mild unilateral hydronephrosis but no kidney stone. All of the following are true EXCEPT? A Increasing fluid intake is therapeutic B The sonogram does NOT rule out the presence of a kidney stone. C The risk of kidney stones increases with higher calcium intake D A 24 hour urine analysis can help determine risk factors for stone formation E Crohn’s disease increases the risk of kidney stones 100

2 days following a fall trip to a farm and apple cider press in the country, a 3 year old boy develops bloody diarrhea which his parents manage at home with fluids. The next week, the is brought to the ER lethargic and pale. He has not urinated in over 8 hours. Lab testing finds WBC of 26, 000, hemoglobin of 9. 8 g/d. L, platelets 65, 000, serum creatinine of 1 mg/d. L, BUN 54 mg/d. L. All of the following statements about this condition are true EXCEPT: A It is precipitated by infection with enteric bacteria producing shiga toxin such as E. Coli O 157: H 7 B C D E It is preventable by early treatment with antibiotics End stage renal failure is uncommon Recurrence is atypical Hypertension is common and may be severe 101

2 days following a fall trip to a farm and apple cider press in the country, a 3 year old boy develops bloody diarrhea which his parents manage at home with fluids. The next week, the is brought to the ER lethargic and pale. He has not urinated in over 8 hours. Lab testing finds WBC of 26, 000, hemoglobin of 9. 8 g/d. L, platelets 65, 000, serum creatinine of 1 mg/d. L, BUN 54 mg/d. L. All of the following statements about this condition are true EXCEPT: A It is precipitated by infection with enteric bacteria producing shiga toxin such as E. Coli O 157: H 7 B C D E It is preventable by early treatment with antibiotics End stage renal failure is uncommon Recurrence is atypical Hypertension is common and may be severe 102

A 4 month old girl is brought to the ER lethargic and pale. She has not urinated in over 8 hours. Lab testing finds WBC of 26, 000, hemoglobin of 8. 8 g/d. L, platelets 56, 000, serum creatinine of 1 mg/d. L, BUN 54 mg/d. L. The blood smear shows schistocytes and helmet cells. True statements about this case include all of the following EXCEPT: A B C D Defective complement system regulation is likely Hypertension is common and may be severe End stage renal failure is common Recurrence is common E Treatment is symptomatic 103

A 4 month old girl is brought to the ER lethargic and pale. She has not urinated in over 8 hours. Lab testing finds WBC of 26, 000, hemoglobin of 8. 8 g/d. L, platelets 56, 000, serum creatinine of 1 mg/d. L, BUN 54 mg/d. L. The blood smear shows schistocytes and helmet cells. True statements about this case include all of the following EXCEPT: A B C D Defective complement system regulation is likely Hypertension is common and may be severe End stage renal failure is common Recurrence is common E Treatment is symptomatic 104

A 6 year-old girl develops tea-colored urine. Urine dip finds 4+ blood and 3+ protein. There is mild edema present and the blood pressure is 114/74. Review of systems is negative. Her twin brother currently has fever and a sore throat. Which of the following statements is CORRECT? A Complement C 3 & C 4 may remain low for 4 -6 weeks The brother can be protected B from the same condition by prompt antibiotic treatment C TURNING POINT SLIDE ANSWER IS D There is high risk of rheumatic heart disease also Rapid progression and need D for dialysis is uncommon and requires renal biopsy E Hypertension is uncommon and requires renal biopsy 105
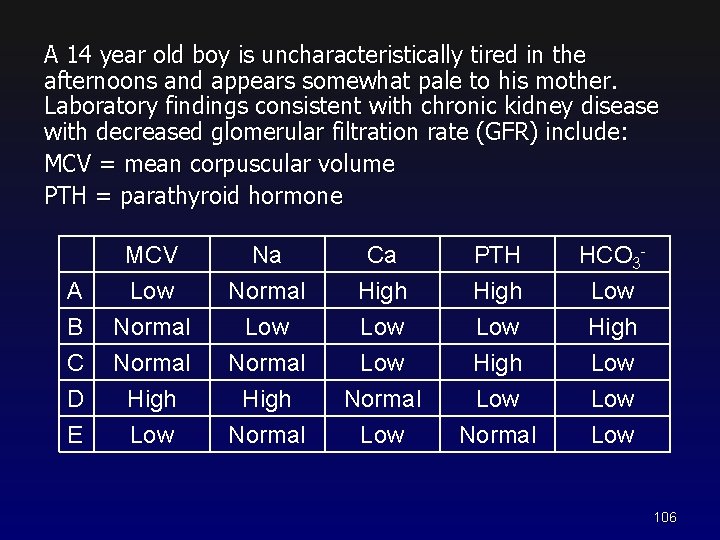
A 14 year old boy is uncharacteristically tired in the afternoons and appears somewhat pale to his mother. Laboratory findings consistent with chronic kidney disease with decreased glomerular filtration rate (GFR) include: MCV = mean corpuscular volume PTH = parathyroid hormone A B C MCV Low Normal Na Normal Low Normal Ca High Low PTH High Low High HCO 3 Low High Low D E High Low High Normal Low 106
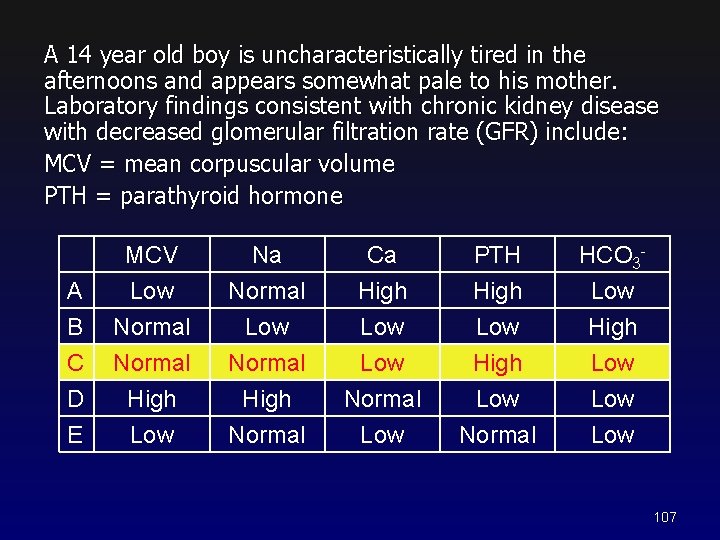
A 14 year old boy is uncharacteristically tired in the afternoons and appears somewhat pale to his mother. Laboratory findings consistent with chronic kidney disease with decreased glomerular filtration rate (GFR) include: MCV = mean corpuscular volume PTH = parathyroid hormone A B C MCV Low Normal Na Normal Low Normal Ca High Low PTH High Low High HCO 3 Low High Low D E High Low High Normal Low 107

A 7 year-old boy with a history of posterior urethral valves and stage 3 CKD has short stature. All of the following factors commonly contribute to short stature in children with CKD EXCEPT: IGF: insulin-like growth factor A Growth hormone deficiency B Resistance to growth hormone C Decreased bioavailability of IGF-1 due to increased IGF binding proteins D Vitamin D deficiency and renal osteodystrophy E Nutritional disturbances 108

A 7 year-old boy with a history of posterior urethral valves and stage 3 CKD has short stature. All of the following factors commonly contribute to short stature in children with CKD EXCEPT: IGF: insulin-like growth factor A Growth hormone deficiency B Resistance to growth hormone C Decreased bioavailability of IGF-1 due to increased IGF binding proteins D Vitamin D deficiency and renal osteodystrophy E Nutritional disturbances 109

A newborn has a sonogram due to an abnormal prenatal sonogram. The left kidney is bit large but otherwise normal. The right kidney has multiple cystic areas and abnormal cortex. The right side shows no uptake on nuclear renal scan. All of the following statements are correct EXCEPT: A B C D Vesicoureteral reflux is a common finding Genetic testing is not likely to be useful The left kidney will eventually develop cysts and fail There is an increased risk of hypertension E ALL of the above are correct 110

A newborn has a sonogram due to an abnormal prenatal sonogram. The left kidney is bit large but otherwise normal. The right kidney has multiple cystic areas and abnormal cortex. The right side shows no uptake on nuclear renal scan. All of the following statements are correct EXCEPT: A B C D Vesicoureteral reflux is a common finding Genetic testing is not likely to be useful The left kidney will eventually develop cysts and fail There is an increased risk of hypertension E ALL of the above are correct Multicystic Dysplastic Kidney is a birth defect and not progressive 111

The parents of a 15 year-old followed in the renal clinic for advancing kidney disease ask your advice about what will happen as his kidneys fail. All of the following are true about End Stage Renal Disease (ESRD) EXCEPT: A A kidney from a live donor is usually better than from a deceased donor. B Hemodialysis does not replace all of the function of the kidneys C Peritoneal dialysis is usually done at home D Nutritional restrictions frequently include potassium, phosphorus, and sodium. E All of the above are true 112

The parents of a 15 year-old followed in the renal clinic for advancing kidney disease ask your advice about what will happen as his kidneys fail. All of the following are true about End Stage Renal Disease (ESRD) EXCEPT: A A kidney from a live donor is usually better than from a deceased donor. B Hemodialysis does not replace all of the function of the kidneys C Peritoneal dialysis is usually done at home D Nutritional restrictions frequently include potassium, phosphorus, and sodium. E All of the above are true 113

Blood Pressure and Hypertension 114

A 9 year-old girl with no symptoms has BP 145 -165 / 90 -100 discovered on a routine physical and confirmed several times. The remainder of her examination is normal. True statements about this case include: A Two additional measurements of BP are required to make the diagnosis of hypertension B The most likely diagnosis is essential hypertension C Best initial treatment is intravenous nicardipine infusion to lower the BP to normal D Normal renal ultrasonography can rule out renal and renovascular causes of hypertension. E The elevated blood pressure is likely long-standing 115

A 9 year-old girl with no symptoms has BP 145 -165 / 90 -100 discovered on a routine physical and confirmed several times. The remainder of her examination is normal. True statements about this case include: A Two additional measurements of BP are required to make the diagnosis of hypertension B The most likely diagnosis is essential hypertension C Best initial treatment is intravenous nicardipine infusion to lower the BP to normal D Normal renal ultrasonography can rule out renal and renovascular causes of hypertension. E The elevated blood pressure is likely long-standing 116

All of the following statements about normal blood pressure in children are true EXCEPT: A B C D Normal BP increases with age during childhood Boys normally have higher BP than girls Normal BP is higher in taller children Normal BP is higher in overweight and obese children E ALL of the above are true statements 117

All of the following statements about normal blood pressure in children are true EXCEPT: A B C D Normal BP increases with age during childhood Boys normally have higher BP than girls Normal BP is higher in taller children Normal BP is higher in overweight and obese children E ALL of the above are true statements Increased BP with height is physiologic and normal. Increased BP with obesity is pathophysiological and abnormal. 118

Blood Pressure Tables 119
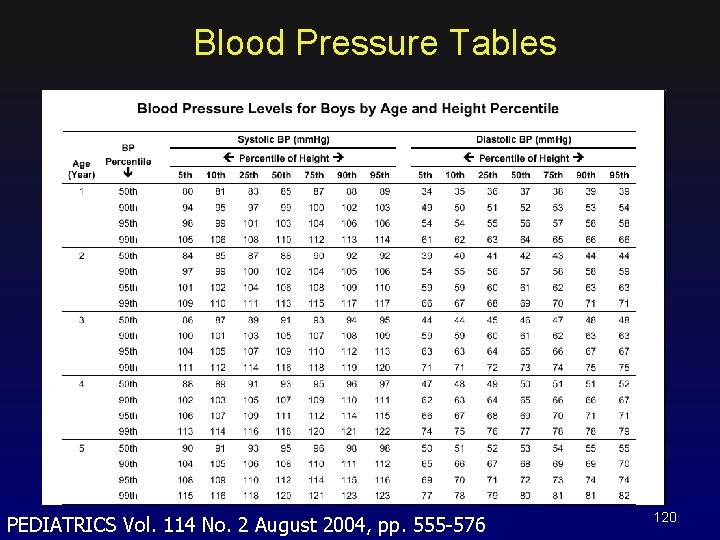
Blood Pressure Tables PEDIATRICS Vol. 114 No. 2 August 2004, pp. 555 -576 120
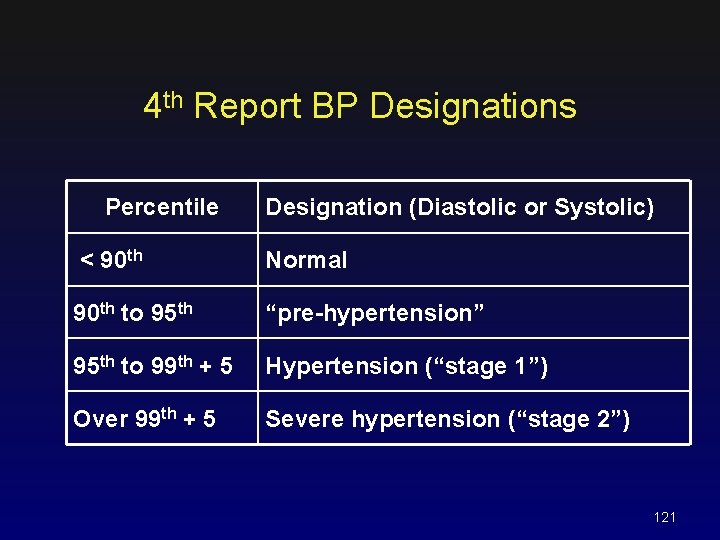
4 th Report BP Designations Percentile Designation (Diastolic or Systolic) < 90 th Normal 90 th to 95 th “pre-hypertension” 95 th to 99 th + 5 Hypertension (“stage 1”) Over 99 th + 5 Severe hypertension (“stage 2”) 121

A 9 year-old girl with asymptomatic stage 2 HTN is evaluated first by renal sonography then by magnetic resonance arteriography. A long right-sided renal arterial narrowing with high velocities is suspicious for renal artery stenosis. She was not in the NICU after birth and never had central venous nor arterial access. The MOST likely etiology of this disease is: A B C D Tuberous sclerosis Neurofibromatosis Williams Syndrome Bartter Syndrome E Fibromuscular dysplasia 122

A 9 year-old girl with asymptomatic stage 2 HTN is evaluated first by renal sonography then by magnetic resonance arteriography. A long right-sided renal arterial narrowing with high velocities is suspicious for renal artery stenosis. She was not in the NICU after birth and never had central venous nor arterial access. The MOST likely etiology of this disease is: A B C D Tuberous sclerosis Neurofibromatosis Williams Syndrome Bartter Syndrome E Fibromuscular dysplasia 123

A 13 year old girl with a BMI in the 96 th percentile is referred for stage 1 HTN. Initial management should include all of the following EXCEPT: A B C D Therapeutic lifestyle changes Evaluation of lipid levels Urinalysis Thorough review of possible diet supplements, overthe-counter medications, caffeine intake, and illicit drug use E Renal angiography 124

A 13 year old girl with a BMI in the 96 th percentile is referred for stage 1 HTN. Initial management should include all of the following EXCEPT: A B C D Therapeutic lifestyle changes Evaluation of lipid levels Urinalysis Thorough review of possible diet supplements, overthe-counter medications, caffeine intake, and illicit drug use E Renal angiography Just making a point here– obesity-related HTN is common and frequently responds to diet and exercise (TLC). Don’t forget these other items– all are fair game for questions. 125

ONLY 125 Slides? It’s a BIG topic Read the Topic Outline 126

Interested in Nephrology? We Don’t Bite (Too Much) Contact Me! Apply! 127

Keep Studying and Good Luck! 128
- Slides: 128