General Microbiology Laboratory Isolation and Identification of Gram

General Microbiology Laboratory Isolation and Identification of Gram Positive Cocci

Identified method for Staphylococci v. Gram-stain v Isolation and culture v Pure culture v Direct identification
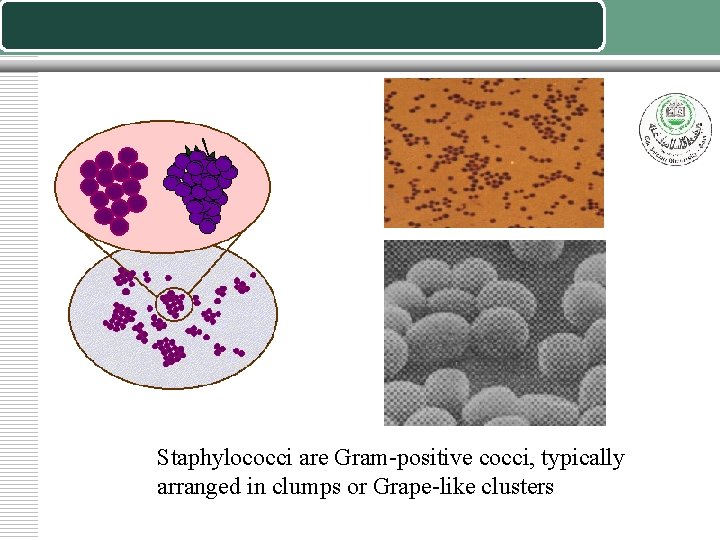
Staphylococci are Gram-positive cocci, typically arranged in clumps or Grape-like clusters


Direct identification v The mannitol fermentation test. v The Coagulase Test v The DNase Test v Novobiocin (NB) disc

The mannitol fermentation test. v. Inoculate the bacteria into a mannitol microtube, incubate at 370 C for 18 h. S. aureus will ferment mannitol to produce acid, which causes the medium to turn yellow.

Test Staphylococcus aureus Staphylococcus epidermidis Mannitol fermentation Positive Negative Staphylococcus saprophyticus Usually positive

The Coagulase Test v Coagulase is an enzyme converting fibrinogen into fibrin promoting blood clotting. v It might be a virulence factor with the coagulated blood around the bacteria protecting them from the immune system. v Coagulase-negative strains are often as pathogenic as coagulase-positive strains.

The DNase Test v Inoculate DNase agar plates with a loop so that the growth is in plaques about 1 cm in diameter. I v ncubate at 370 C overnight. v Flood the plate with 1 N hydrochloric acid. Clearing around the colonies indicates DNase activity. v The hydrochloric acid reacts with unchanged deoxyribonucleic acid to give a cloudy precipitate. v A few other bacteria, e. g. Serratia, may give a positive reaction.
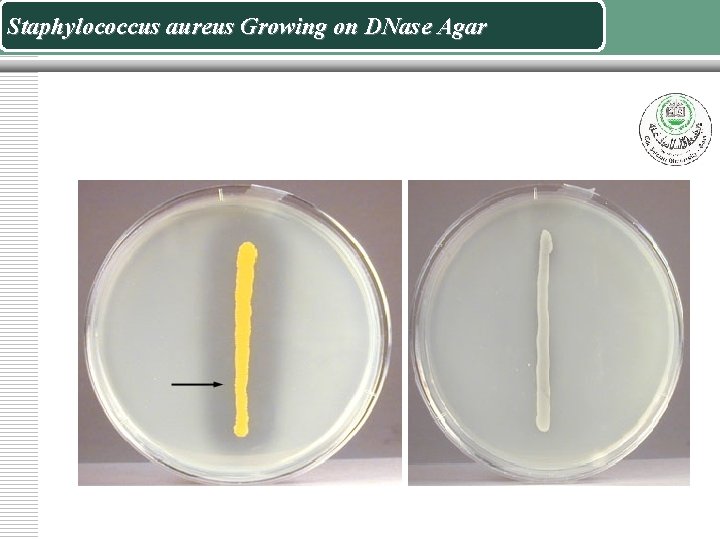
Staphylococcus aureus Growing on DNase Agar
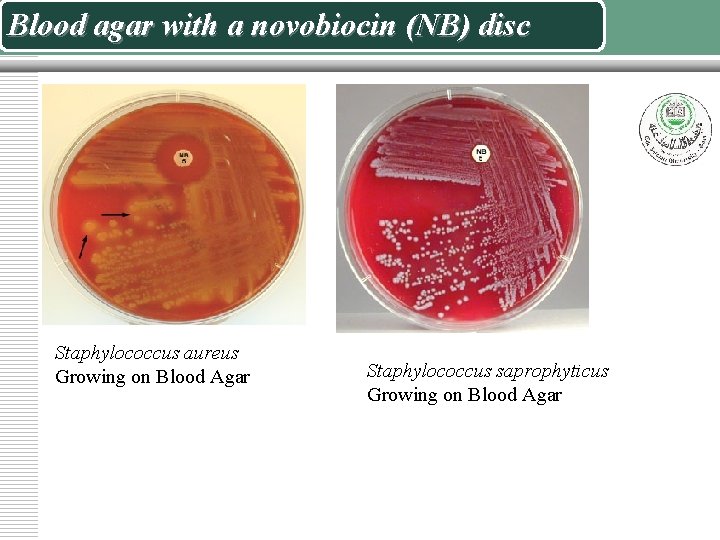
Blood agar with a novobiocin (NB) disc Staphylococcus aureus Growing on Blood Agar Staphylococcus saprophyticus Growing on Blood Agar
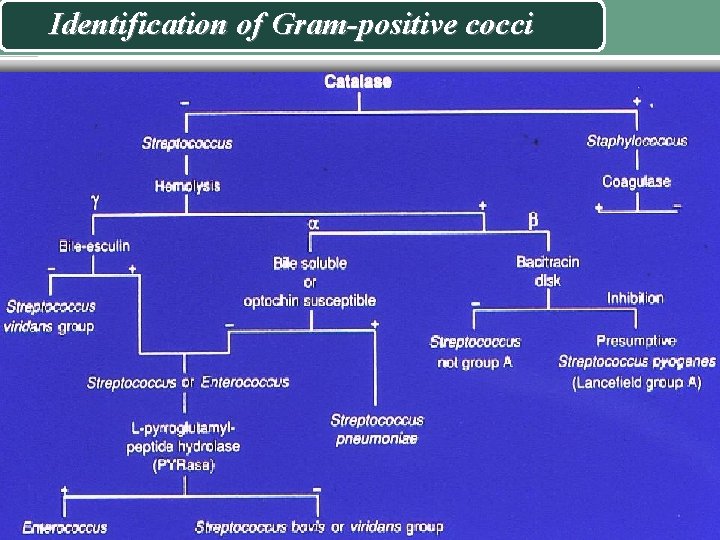
Identification of Gram-positive cocci

types Of Streptococcus

β haemolytic steps: Lancefield groups v Historically v A, B, C, F and G group specific antigens cell wall polysaccharide v group D and Enterococci lipoteichoic acid moiety Not always β haemolytic v Now: 18 different groups of strep: from A-H, and from K-T

(β) Haemolytic Streptococcus groups v S. pyogenes • Group A v S. agalactiae • Group B (occasionally α or none) v Streptococcus equismilis • Group C (occasionally α or none) v Streptococcus bovis • Group D (α or none, occasionally β) v Streptococcus anginosus • Group F & G
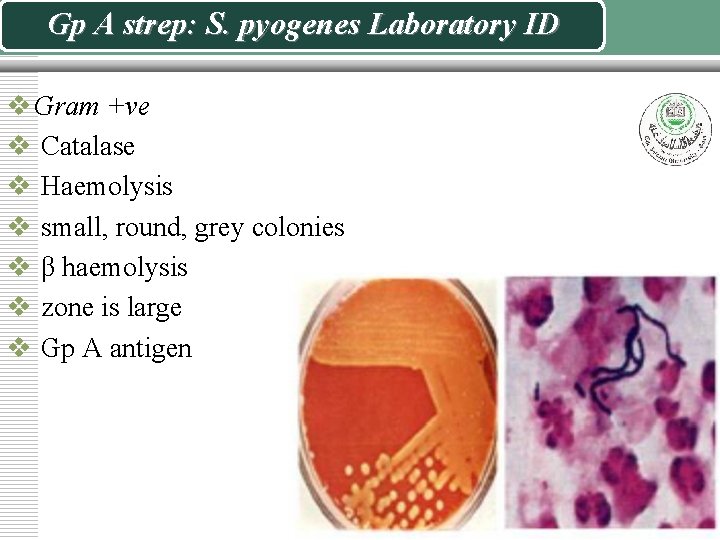
Gp A strep: S. pyogenes Laboratory ID v Gram +ve v Catalase v Haemolysis v small, round, grey colonies v β haemolysis v zone is large v Gp A antigen

Isolation and Identification of group A beta hemolytic (Streptococcus pyogenes) 1. on Blood agar. Streptococcus pyogenes produces a zone of beta hemolysis around 2 -3 mm in diameter surrounding each colony 2. Sensitivity to the antibiotic bacitracin 3. Group A Strep is senstive, other b haemolytic streps are resistant.
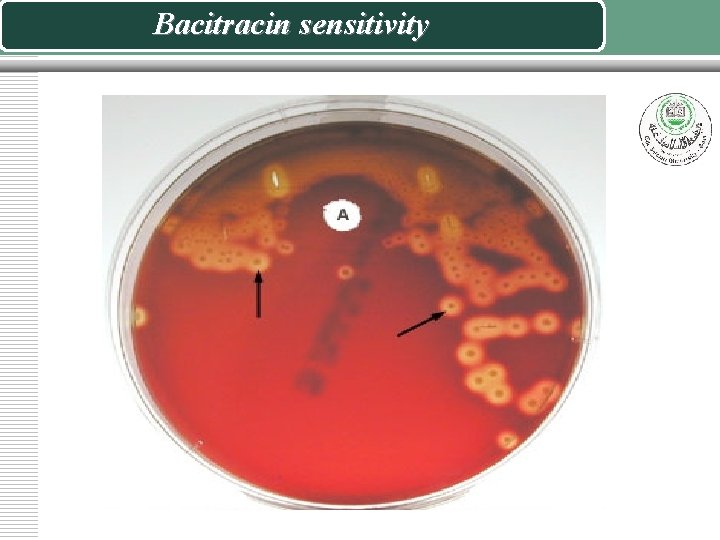
Bacitracin sensitivity
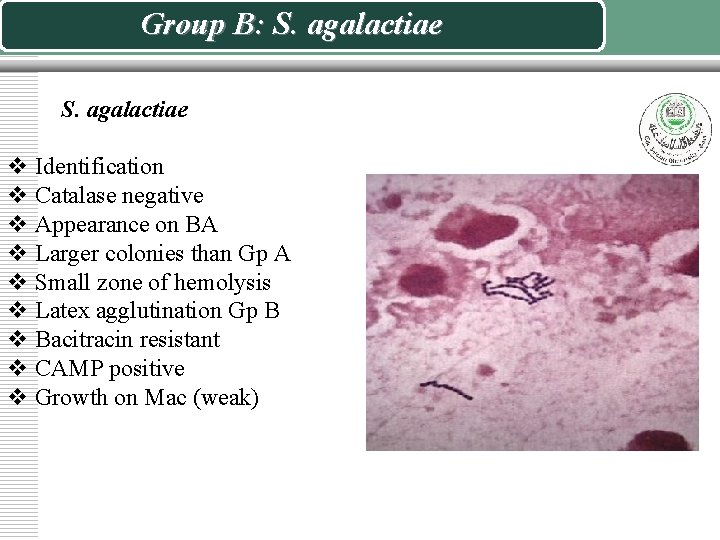
Group B: S. agalactiae v Identification v Catalase negative v Appearance on BA v Larger colonies than Gp A v Small zone of hemolysis v Latex agglutination Gp B v Bacitracin resistant v CAMP positive v Growth on Mac (weak)

Presumptive ID Tests - CAMP v The “CAMP” test (acronym for developers) is used to differentiate S. agalactiae (GBS), which is positive, from other beta hemolytic strep, all of which are negative v “CAMP factor” is a soluble hemolysin produced by GBS that combines in a synergistic way with a similar hemolysin of S. aureus to form an arrowhead zone of clearing. See image v The staph is streaked perpendicularly to the unknown strep. After appropriate incubation time an “arrowhead-shaped” clear zone of hemolysis will appear.

S. agalactiae §Synergistic haemolysis observed between betahemolytic Staphylococcus aureus and group B streptococci. �� Positive reaction: arrowhead haemolysis pattern

α – Haemolytic streps: Viridans streps v. Not groupable by Lancefield groups v No group specific CHO v Streptococcus pneumoniae v Primary human pathogen v. S. sanguis v S. mitis v S. mutans v S. salivarius


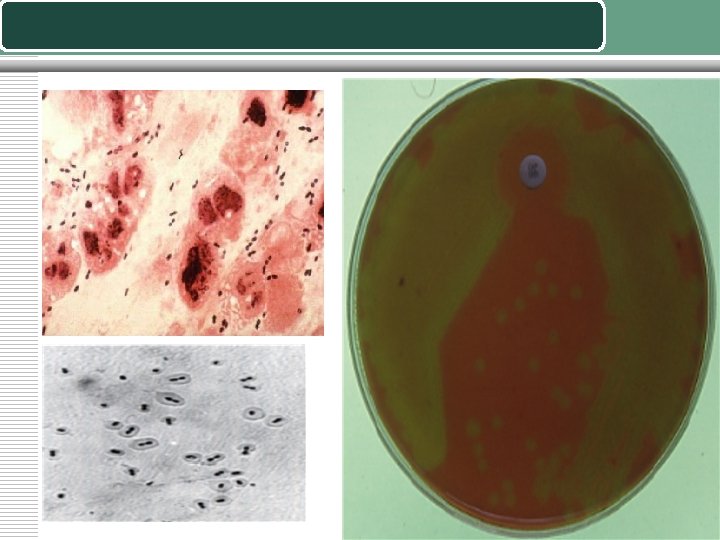
The Pneumococcus (Streptococcus pneumoniae) 1: Isolation on Blood agar • Pneumococci frequently require enriched media and increased CO 2 tension for initial isolation. • They are usually isolated on Blood agar and incubated in a candle jar (a closed container in which a lit candle is placed to remove O 2 and increase CO 2 ) at 37 C. On Blood agar, colonies appear small, shiny, and translucent. • They are surrounded by a zone of alpha hemolysis 2: Optochin sensitivity • Pneumococci are the only streptococci that are sensitive to the drug optochin(ethylhydrocupreine hydrochloride). 3: Gram stain: gram-positive, diplococci

The Genus Enterococcus v Enterococci are gram-positive streptococci, typically occurring in pairs and short chains, that are normal flora of the intestinal tract. Enterococci responsible for a variety of opportunistic infections in humans, and serologically belong to Lancefield group D streptococci. v On Bile Esculin agar v Unlike most bacteria, the enterococci will grow in the presence of the bile salts in the medium. v They hydrolyze the esculin, producing esculetin which reacts with the iron salts in the medium turning the agar black

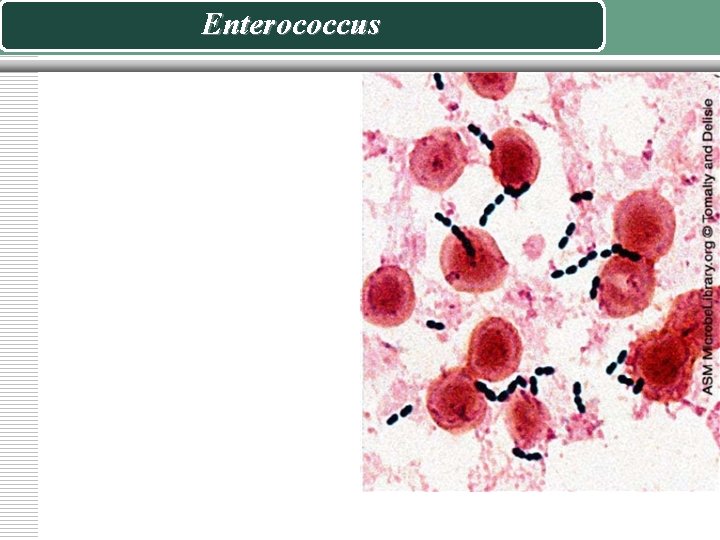
Enterococcus

Laboratory ID: Enterococcus vwhite colonies v alpha and no haemolysis (rarely beta) v Also grow on Mac. Conkey v Resembles S. pneumoniae in Gram stains v Bile esculin positive v Grows on Mac

End of lecture
- Slides: 30