Gastroschisis Development of an EvidenceBased Post Surgical Feeding

Gastroschisis: Development of an Evidence-Based Post. Surgical Feeding Guideline Noreen Beus Oeding, RN-BSN, NNP-Student Creighton University

Gastroschisis: Background CDC : 1, 871 infants with gastroschisis born annually in U. S. 4 -5 per 10, 000 live births with increasing occurrence in past two decades. Maternal risk factors: environmental exposure, young maternal age (<20 years), low BMI, low socioeconomic status, poor nutrition, smoking, illicit drug use, alcohol, analgesic medications, and GU infections.

Gastroschisis: Significance Concerns related to post-surgical repair Long-term TPN Delayed enteral feeding Long-term hospitalization Parenteral nutrition-associated liver disease Infection Cholestasis Hepatic failure Mortality

Clinical Problem Statement & Purpose There are many gaps in the knowledge about best management of enteral feeding in post-surgical gastroschisis infants. The purpose of this quality improvement project was to develop an evidence-based post-surgical feeding guideline for infants with gastroschisis, >34 weeks birth gestational age, or >1500 grams birthweight.

Review of Literature Associated Problems: infection, water loss, cow’s milk allergy, cholestasis, NEC Enteral Feedings: Timing of introduction of feeding indicates early feeding benefits: Reduction Start in NEC, sepsis, TPN, length of hospitalization. feeding Day 5 after primary/complete closure. Advancement: In conjunction with gastric decompression intervals, interval small breast milk feedings. Content: Breast milk is best. Immune support mediated by breast milk may prevent infection. Fortification: Improved growth with no associated adverse outcome per Cochrane Review. GER: Higher with associated complications, e. g. hiatal hernia. Feeding intolerance improved when GER treated. Nurses role in discharge preparation: Nurses can promote learning opportunities so parents can gain skill and confidence to take infant home. Parents should be educated re: possible complications e. g. strictures, bowel atresia, etc.

Methods: Project Development Quality Improvement Project ROL: Through review of literature, post-surgical feeding approaches that appear to be associated with improved patient outcomes were included in the development of an evidence-based feeding guideline. Medical Chart Review: A retrospective chart review was completed for 20 infants diagnosed with gastroschisis from two Level III-IV NICUs in the Mountain Region of the United States, to describe current practice and to better inform the development of the feeding guideline. Work with Stakeholders: The guideline was presented to relevant stakeholders for review and revision. An educational program and implementation plan was developed and presented.

Retrospective Chart Review Audit charts: gastroschisis infants > 34 weeks, between January 2014 to December 2016, at two Level III and IV NICU in the Mountain Region. Variables of interest: maternal/infant demographics, medications, surgical management (duration of gastric decompression suction and type of closure), type of feeding, method and timing of feeding, caloric supplementation, incidence of sepsis, pain management. Description of practice: gastroschisis post-surgical feeding guideline for infants of >34 weeks birth gestational age or >1500 grams birthweight.
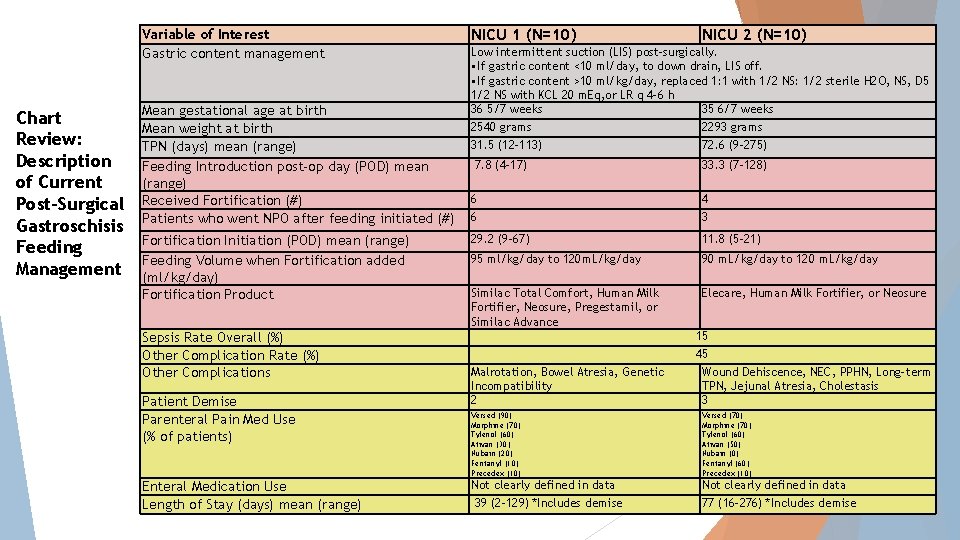
Variable of Interest Gastric content management Chart Review: Description of Current Post-Surgical Gastroschisis Feeding Management Mean gestational age at birth Mean weight at birth TPN (days) mean (range) Feeding Introduction post-op day (POD) mean (range) Received Fortification (#) Patients who went NPO after feeding initiated (#) Fortification Initiation (POD) mean (range) Feeding Volume when Fortification added (ml/kg/day) Fortification Product Sepsis Rate Overall (%) Other Complication Rate (%) Other Complications Patient Demise Parenteral Pain Med Use (% of patients) Enteral Medication Use Length of Stay (days) mean (range) NICU 1 (N=10) NICU 2 (N=10) Low intermittent suction (LIS) post-surgically. • If gastric content <10 ml/day, to down drain, LIS off. • If gastric content >10 ml/kg/day, replaced 1: 1 with 1/2 NS: 1/2 sterile H 2 O, NS, D 5 1/2 NS with KCL 20 m. Eq, or LR q 4 -6 h 36 5/7 weeks 35 6/7 weeks 2540 grams 2293 grams 31. 5 (12 -113) 72. 6 (9 -275) 7. 8 (4 -17) 33. 3 (7 -128) 6 6 4 3 29. 2 (9 -67) 11. 8 (5 -21) 95 ml/kg/day to 120 m. L/kg/day 90 m. L/kg/day to 120 m. L/kg/day Similac Total Comfort, Human Milk Fortifier, Neosure, Pregestamil, or Similac Advance Elecare, Human Milk Fortifier, or Neosure Malrotation, Bowel Atresia, Genetic Incompatibility 2 15 45 Wound Dehiscence, NEC, PPHN, Long-term TPN, Jejunal Atresia, Cholestasis 3 Versed (90) Morphine (70) Tylenol (60) Ativan (30) Nubain (20) Fentanyl (10) Precedex (10) Versed (70) Morphine (70) Tylenol (60) Ativan (50) Nubain (0) Fentanyl (60) Precedex (10) Not clearly defined in data 39 (2 -129) *Includes demise Not clearly defined in data 77 (16 -276) *Includes demise

Results: Feeding Guideline ROL: Post-surgical care feeding approaches in the literature that were associated with improved patient outcomes include Earlier introduction of enteral feedings with breast milk; including oral milk swabbing. Early timing of feeding in first 5 -10 days of life, depending upon bowel length and return of bowel function. Volume of feeding best increased by 10 ml/kg/day. Held at 10 ml/kg/day for intolerance. Fortification of feeding improved overall growth and nutrition. Less feeding intolerance with fewer interruptions, which supports use of feeding guideline. Chart review: differences in the rate of progression, in how infants were fortified, degree of illness, and complexity of infant status.


Implementation Target Audience and dissemination (3) 1) Neonatology providers 2) Surgical services 3) Dietary

Future Work/Research Others may adapt, implement, and test post-surgical feeding guidelines in their institutions. Feeding guidelines for post-surgical gastroschisis infants of decreased gestational age or weight. Possible use for gestational ages <34 weeks and/or <1500 grams. Future research questions: evidence-base post-surgical care guideline may: decrease time on TPN. decrease time to full feedings. decreased infection rates. decreased length of hospital stay. Improve care provider satisfaction.

Conclusion An evidence-based feeding guideline for gastroschisis post-surgical infants >34 weeks gestation or >1500 grams at birth, with educational and implementation plans, was developed and presented to stakeholders, and revised. Others may adapt, implement, and test this feeding guideline. This quality improvement project, through which an evidence-based feeding guideline for infants with gastroschisis was developed, may be a model for implementation to standardized care in NICUs.

References Adler, A. , 2014. Prediction of Feeding Difficulties In Post-Operative Neonates. Yale University Eli. Scholar – A Digital Platform for Scholarly Publishing at Yale, 1 -46. Burge, D. , Drewett, M. , & Hall, N. (2015). Do infants with gastroschisis have a high incidence of non-Ig. Emediated cow’s milk protein allergy? Pediatric Surgery International, 31(3), 271 -276. doi: 10. 1007/s 00383 -0153664 -5 Celegato, M. , & Gancia, P. (2011). Medical and nursing care in post-operative period to the newborn with surgical problems and intestinal ostomy. Early Human Development, 87. doi: 10. 1016/j. earlhumdev. 2011. 021 Chaudhury, P. , Haeri, S. , Horton, A. L. , Wolfe, H. M. , & Goodnight, W. H. (2010). Ultrasound prediction of birthweight and growth restriction in fetal gastroschisis. American Journal of Obstetrics and Gynecology, 203(4). doi: 10. 1016/j. ajog. 2010. 06. 030 Christison-Lagay, E. R. , Kelleher, C. M. , & Langer, J. C. (2011). Neonatal abdominal wall defects. Seminars in Fetal and Neonatal Medicine, 16(3), 164 -172. doi: 10. 1016/j. siny. 2011. 02. 003 Creasy, R. K. , & Resnik, R. (2014). Creasy and Resniks maternal fetal medicine: principles and practice (7 th ed. ). Philadelphia, PA: Elsevier Saunders. Data & Statistics Birth Defects: Gastroschisis. (2016). Retrieved November 17, 2016, from http: //www. cdc. gov/ncbddd/birthdefects/data. html Fallon, E. M. , Mitchell, P. D. , Potemkin, A. K. , Nehra, D. , Arsenault, D. A. , Robinson, E. M. , Puder, M. (2012). Cholestasis and growth in neonates with gastroschisis. Journal of Pediatric Surgery, 47(8), 1529 -1536. doi: 10. 1016/j. jpedsurg. 2011. 12. 028

References Fallon, E. M. , Mitchell, P. D. , Potemkin, A. K. , Nehra, D. , Arsenault, D. A. , Robinson, E. M. , Puder, M. (2012). Cholestasis and growth in neonates with gastroschisis. Journal of Pediatric Surgery, 47(8), 15291536. doi: 10. 1016/j. jpedsurg. 2011. 12. 028 Gillespie, B. M. , Chaboyer, W. , Allen, P. , Morely, N. , & Nieuwenhoven, P. (2013). Wound care practices: A survey of acute care nurses. Journal of Clinical Nursing, 23(17 -18), 2618 -2627. doi: 10. 1111/jocn. 12479 Gulack, B. C. , Laughon, M. M. , Clark, R. H. , Burgess, T. , Robinson, S. , Muhammad, A. , Zhang, A. , Davis, A. , Morton, R. , Chu, V. , Arnold, C. , Hornik, C. , Smith, B. (2016). Enteral Feeding with Human Milk Decreases Time to Discharge in Infants following Gastroschisis Repair. The Journal of Pediatrics, 170, 85 -89. doi: 10. 1016/j. jpeds. 2015. 11. 046 Jones, A. M. , Isenburg, J. , Salemi, J. L. , Arnold, K. E. , Mai, C. T. , Aggarwal, D. , Honein, M. A. (2016). Increasing Prevalence of Gastroschisis — 14 States, 1995– 2012. MMWR. Morbidity and Mortality Weekly Report, 65(2), 23 -26. doi: 10. 15585/mmwr. mm 6502 a 2 Khalil, B. A. , Baath, M. E. , Baillie, C. T. , Turnock, R. R. , Taylor, N. , Saene, H. F. , & Losty, P. D. (2008). Infections in gastroschisis: organisms and factors. Pediatric Surgery International, 24(9), 1031 -1035. doi: 10. 1007/s 00383 -008 -2210 -0 Kohler, J. A. , Perkins, A. M. , & Bass, W. T. (2013). Human milk versus formula after gastroschisis repair: Effects on time to full feeds and time to discharge. Journal of Perinatology, 33(8), 627 -630. doi: 10. 1038/jp. 2013. 27

Reference Kuschel, C. , & Harding, J. (1999). Multicomponent fortified human milk for promoting growth in preterm infants. The Cochrane Database of Systematic Reviews. doi: 10. 1002/14651858. cd 000343 Ledbetter, D. J. (2006). Abdominal Wall Defects: omphalocele and Gastroschisis. Surgical Clinics of North America, (86), 249 -260. doi: 10. 1016/j. suc. 2005. 12. 003 Lemoine, J. B. , Smith, R. R. , & White, D. (2015). Got Milk? Effects of Early Enteral Feedings in Patients With Gastroschisis. Advances in Neonatal Care, 15(3), 166 -175. doi: 10. 1097/anc. 0000000171 Peterson, S. J. , & Bredow, T. S. (2013). Middle range theories: Application to nursing research and practice (3 rd ed. ). Shuler Nurse Practitioner Practice Model. New York, NY: Wolter Luwer Health - Lippincott Williams & Wilkins. Rodriguez, N. A. , Meier, P. P. , Groer, M. W. , Zeller, J. M. , Engstrom, J. L. , & Fogg, L. (2010). A Pilot Study to Determine the Safety and Feasibility of Oropharyngeal Administration of Own Mother's Colostrum to Extremely Low-Birth-Weight Infants. Advances in Neonatal Care, 10(4), 206 -212. doi: 10. 1097/anc. 0 b 013 e 3181 e 94133 Sankalecha, S. , Koshire, A. , Anand, M. , & Gondse, B. (2014). Omphalocele: A Case Report. MVP Journal of Medical Science, 1(1), 42 -43. doi: 10. 15306/mvpjms/2014/v 1 i 1/46890 Savoie, K. B. , Bachier-Rodrigueqz, M. , Jones, T. L. , Jeffreys, K. , Papraniku, D. , Sevilla, W. M. , …Huang, E. Y. (2016). Standardization of Feeding Advancement After Neonatal Gastrointestinal Surgery. Nutrition in Clinical Practice, 31(6), 810 -818. Doi: 10. 1177/0884533616658766

References Segal, I. , Kang, C. , Albersheim, S. G. , Skarsgard, E. D. , & Lavoie, P. M. (2014). Surgical site infections in infants admitted to the neonatal intensive care unit. Journal of Pediatric Surgery, 49(3), 381 -384. doi: 10. 1016/j. jpedsurg. 2013. 08. 001 Stanger, J. , Zwicker, K. , Albersheim, S. , & Murphy, J. J. (2014). Human milk fortifier: An occult cause of bowel obstruction in extremely premature neonates. Journal of Pediatric Surgery, 49(5), 724 -726. doi: 10. 1016/j. jpedsurg. 2014. 02. 054 Tsai, J. , Blinman, T. A. , Collins, J. L. , Laje, P. , Hedrick, H. L. , Adzick, N. S. , & Flake, A. W. (2014). The contribution of hiatal hernia to severe gastroesophageal reflux disease in patients with gastroschisis. Journal of Pediatric Surgery, 49(3), 395 -398. doi: 10. 1016/j. jpedsurg. 2013. 09. 005 Walter-Nicolet, E. , Rousseau, V. , Kieffer, F. , Fusaro, F. , Bourdaud, N. , Oucherif, S. , . . . Mitanchez, D. (2009). Neonatal Outcome of Gastroschisis Is Mainly Influenced by Nutritional Management. Journal of Pediatric Gastroenterology and Nutrition, 48(5), 612 -617. doi: 10. 1097/mpg. 0 b 013 e 31818 c 5281 Williams, T. , Butler, R. , & Sundem, T. (2003). Management of the Infant with Gastroschisis: A Comprehensive Review of the Literature. Newborn and Infant Nursing Reviews, 3(2), 55 -63. doi: 10. 1053/nbin. 2003. 36106

Thank You! Noreen Beus, RN-BSN, NNP-Student, Creighton University: Neonatal Doctorate Nurse Practitioner Program nnbeus@gmail. com 801 -673 -5673

Questions?
- Slides: 19