Gastroparesis Internal Medicine Noon Conference September 16 th

Gastroparesis Internal Medicine Noon Conference September 16 th, 2019 Charles Mc. Mahon, MD

Gastroparesis �Lecture overview: • • Definitions Normal gastric function Pathophysiology Epidemiology Signs/Symptoms Testing/Diagnosis Treatment

Gastroparesis Definition �Delayed emptying of the stomach in the absence of mechanical outlet obstruction �ACG guideline definition – “combination of the symptoms of gastroparesis, absence of gastric outlet obstruction or ulceration, and delay in gastric emptying. ”

Normal Stomach Mechanical Physiology �Stomach is very small when relaxed and empty and increases 10 x w/ intake �Liquids empty from the stomach first, followed by solids, which are initially stored in the fundus (fundic accommodation – lag phase) �Food is then moved from the fundus to the antrum and ground into chyme
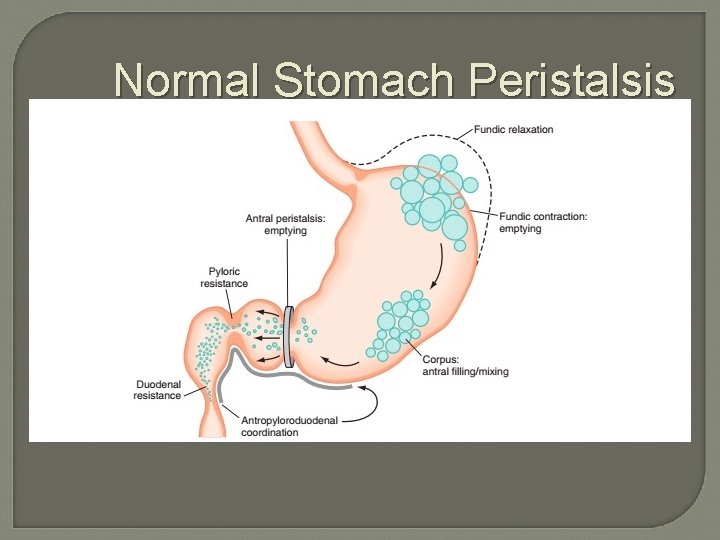
Normal Stomach Peristalsis
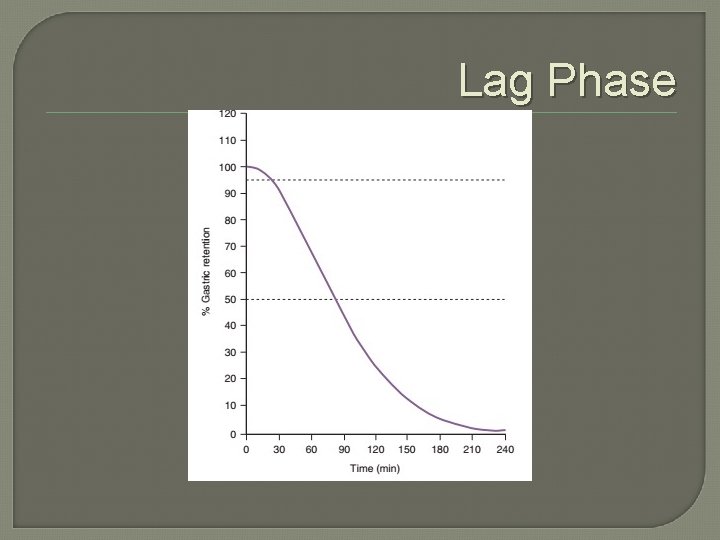
Lag Phase

Normal Stomach Electrical Physiology �Mediated by the myenteric plexus �Myenteric plexus is regulated via vagal efferents from the dorsal motor vagal complex in the brainstem �Myenteric plexus motor neurons: • Excitatory: Acetylcholine • Inhibitory: NO �Gastric pacemaker – Interstitial Cells of Cajal (ICC), contractile rhythm 3 cpm
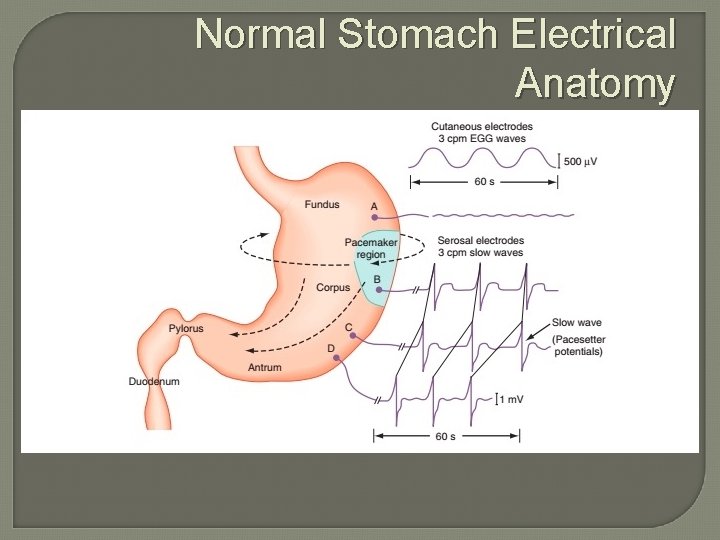
Normal Stomach Electrical Anatomy

Gastroparesis Epidemiology Often undiagnosed, true prevalence may be >1. 5% More common in women (approx 4: 1 prevalence) More common in diabetes (30 x Type 1, 8 x Type II) Population based studies 5. 2%, 1%, and 0. 2% of I, II, and nondiabetics develop gastroparesis

Gastroparesis Epidemiology Mean onset age 33 Impacts QOL, costs, and associated with M&M

Gastroparesis Pathophysiology Unknown to a significant degree Full thickness gastric biopsies have shown multiple abnormalities: ICC dropout (seems to correlate best with delays in gastric emptying) Decreased density of nerve fibers Smooth muscle fibrosis Changes in neurotransmitters Myenteric immune infiltrate in the muscle layer

Gastroparesis Pathophysiology DM – abnormalities on multiple levels – motor dysfunction, intrinsic nervous system damage Postsurgical Medication induced (anticholinergic, opiate, GLP-1 analogs) Postviral Gastroparesis - viral prodrome

Gastroparesis Signs/Symptoms Clinical suspicion: • • Nausea Vomiting Bloating Early satiety/post-prandial fullness Abdominal pain Difficult to control/refractory GERD H/o diabetes, recent viral illness, recent negative EGD and/or upper GI imaging

Gastroparesis Signs/Symptoms Gastroparesis Cardinal Symptom Index (GCSI)

Gastroparesis Testing/Diagnosis Concern for gastroparesis: • EGD (r/o ulcer, stricture, other cause of narrowing, H. • • Pylori, malignancy) Medication review Imaging Pill testing, via p. H or direct visualization/Breath testing – not validated currently Gastric Scintigraphy, Gastric Emptying Study, GES
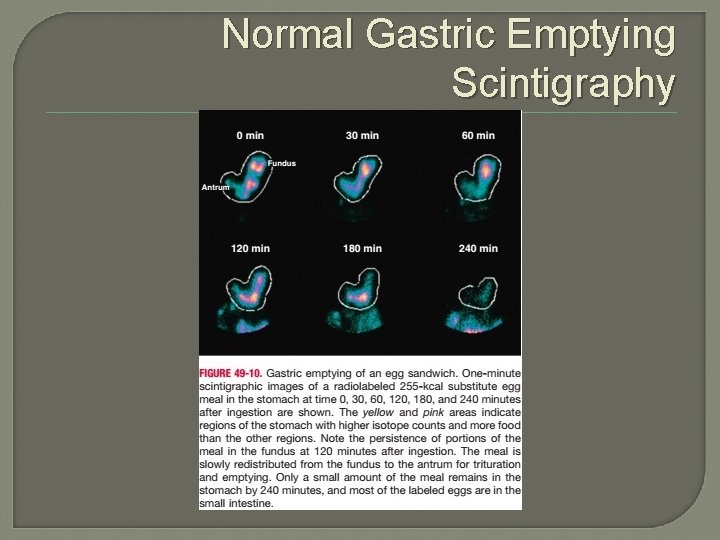
Normal Gastric Emptying Scintigraphy

Gastroparesis Testing/Diagnosis Gastric Emptying Study: • Nuclear Medicine Test • Scintigraphy at 0, 1, 2, 4 hours w/ radiolabeled food (eggs, generally) • Shorter tests/liquid tests less sensitive • Need to be off meds that accelerate or delay gastric emptying for 48 -72 h prior to testing and have euglycemia • Positive - >60% label remaining at 2 hours and > 10% at 4 hours

Gastroparesis Testing/Diagnosis Other, less often used/still somewhat experimental tests: Wireless capsule motility testing 13 C breath testing

Gastroparesis Testing/Diagnosis Seems to be poor correlation between symptoms and degree of emptying seen on GES Screen patients with gastroparesis for DM, thyroid disease – if unknown. Consider autoimmune/neurologic screening

Gastroparesis Testing/Diagnosis Accelerated/rapid gastric emptying and functional dyspepsia can present with symptoms similar to gastroparesis, so GES is recommended prior to initiating medical or surgical therapies Differential diagnosis of symptoms can also include rumination syndrome, cyclic vomiting syndrome, and cannabinoid hyperemesis syndrome
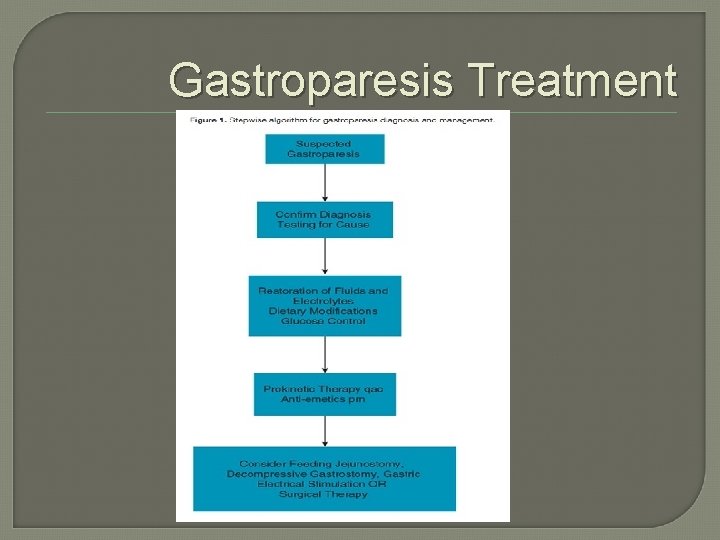
Gastroparesis Treatment

Gastroparesis Treatment � Resuscitation/near and long term plan for nutritional support (other enteral feeding options and/or TPN) � Enteral (and postpyloric) feeding preferred � Consultation w/ a dietician • Frequent small volume/fiber/fat meals • Liquids only, if all that is tolerated � Jejunal feeding may be indicated if repeated hospitalizations or 10% BW loss in 3 -6 months

Gastroparesis Treatment �Medical: • Prokinetics: Metoclopramide (D 2 antagonist) �Try as low dose, short course as possible and document discussion of risks/benefits (TD <1%) • Domperidone (D 2 antagonist, not in U. S. w/o investigatory drug form) �Need monitoring of baseline and repeat ECGs �Withhold if QTc >470 ms in males and >450 ms in females

Gastroparesis Treatment � Medical: • Erythromycin: Macrolide antibiotic (mimics motilin) �Good for acute/hospital treatment �Tachyphylaxis (2 weeks) �Can also prolong QT and interfere w/ drug metabolism • Symptom control w/ Ondansetron (5 -HT 3 antagonists), Prochlorperazine, Promethazine, Diphenhydramine, Benzos, Tricyclics (more for visceral hypersensitivity) to act on different serotonin, histamine, dopamine, muscarinic, GABA receptors
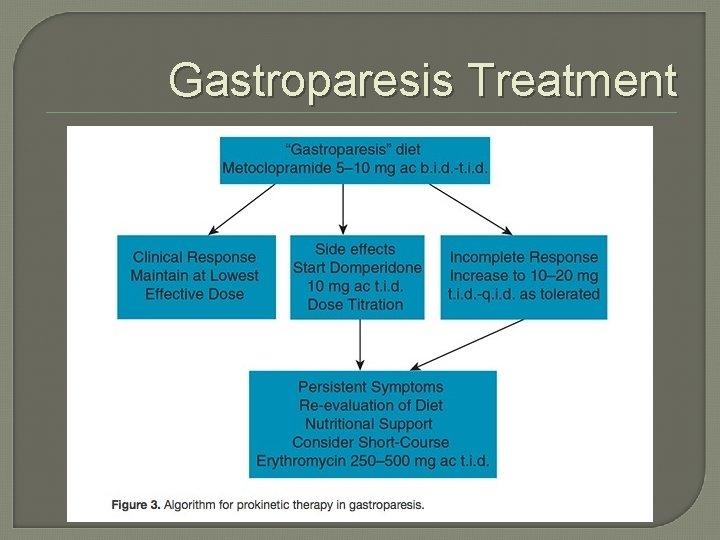
Gastroparesis Treatment

Gastroparesis Treatment �Avoid/minimize opioids, motility slowing medications �Avoid alcohol, tobacco �Glycemic control (BG <200) �Diet: low fiber/fat/red meat, small and frequent meals �Postviral gastroparesis may improve with time (can be > 1 year)
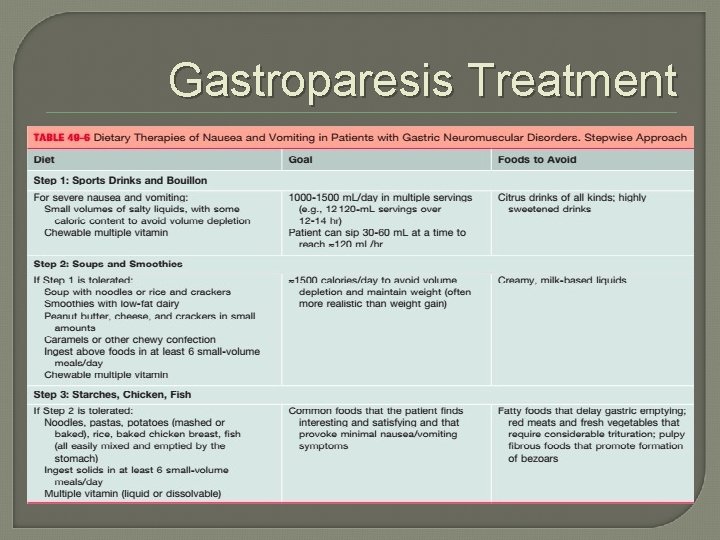
Gastroparesis Treatment

Gastroparesis Treatment �Non-Medical: • ? Botox injection into pyloric area? �Conflicting study data, not currently recommended • G-POEM • Self Expanding Metal Pyloric Stents �Unclear long term risks and significant complication risk as well as lack of data

Gastroparesis Treatment �Non-Medical: • Gastric Electric Stimulators “gastric pacemakers” (surgical implant, GES) �Compassionate use �Equivocal results – mostly surgical studies �Costs/risks of surgery �Need for careful patient selection (better in DM? ) • Sometimes other surgeries – venting gastrostomy, gasctrectomy, pyloroplasty, gastrojejunostomy • Acupuncture


References 1. 2. 3. 4. Dhalla S, Pasricha, J. Gastroparesis. In: Rao SSC, Parkman HP, Mc. Callum RW. Handbook of gastrointestinal motility and functional disorders. Thorofare, NJ: SLACK Incorporated; 2015 107 -114). Camilleri M, et al. ACG Guidelines. Management of gastroparesis. Am J Gastroenterol 2013; 108: 18– 37; doi: 10. 1038/ajg. 2012. 373; published online 13 November 2012. Accessed March 18, 2017. Koch, K. (2015). Gastric Neuromuscular Function and Neuromuscular Disorders (9 th ed. , pp. 811 -838). Philadelphia, Pennsylvania: Elsevier Saunders. Camilleri M. Treatment of gastroparesis. In: Up. To. Date, Grover S (Ed), Up. To. Date, Waltham, MA. (Accessed on March 20, 2017. )
- Slides: 31