Gastrointestinal Problems Ineterventions Presented by Joanna Shedd MS

Gastrointestinal Problems & Ineterventions Presented by Joanna Shedd, MS, CNS, RN
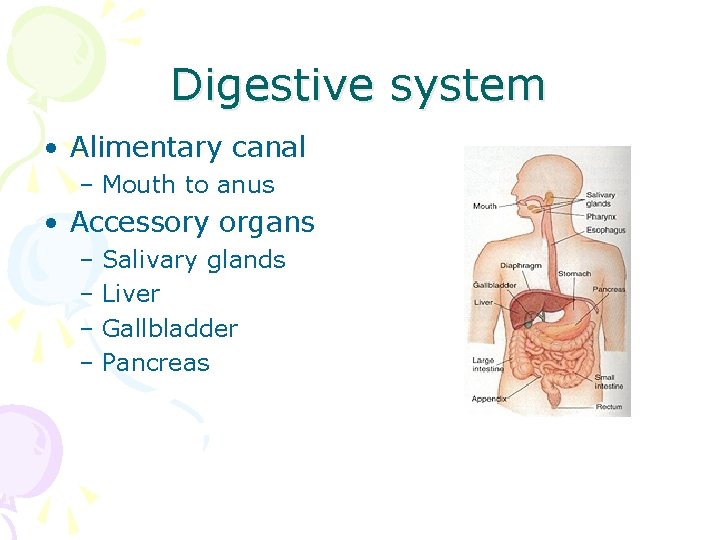
Digestive system • Alimentary canal – Mouth to anus • Accessory organs – Salivary glands – Liver – Gallbladder – Pancreas
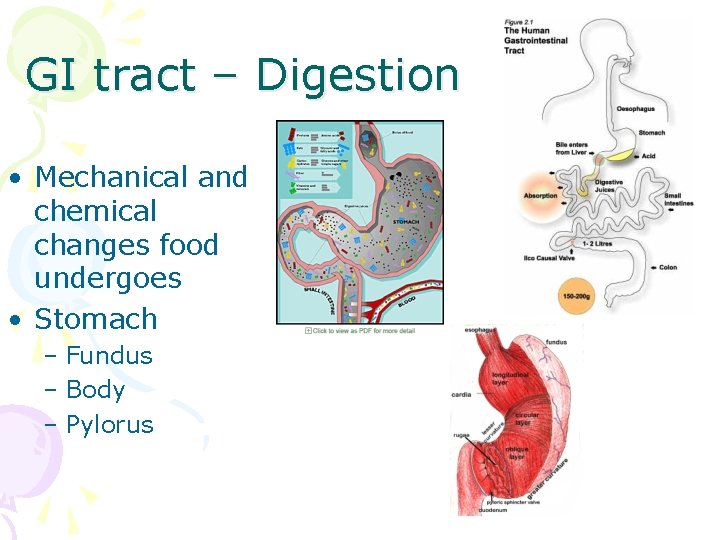
GI tract – Digestion • Mechanical and chemical changes food undergoes • Stomach – Fundus – Body – Pylorus

Mucosa Layer • Lines alimentary canal • Surface area for acids, bases, mucus, & enzymes • Mucosa is folded with grooves and pits

Peristalsis • Movement propelled along GI tract • Rhythmic layer of smooth muscle • Absorption of nutrients and water during peristalsis
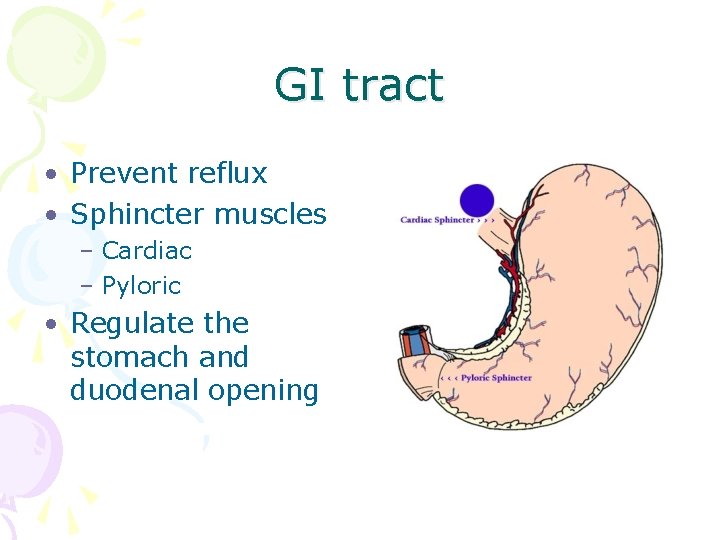
GI tract • Prevent reflux • Sphincter muscles – Cardiac – Pyloric • Regulate the stomach and duodenal opening
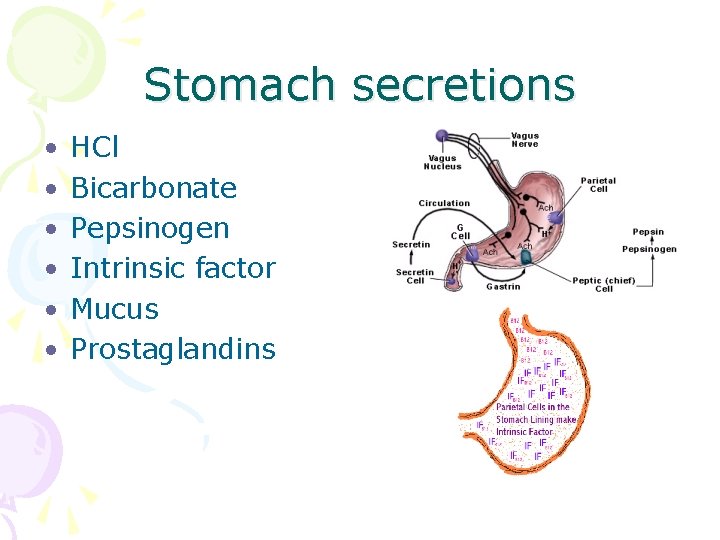
Stomach secretions • • • HCl Bicarbonate Pepsinogen Intrinsic factor Mucus Prostaglandins
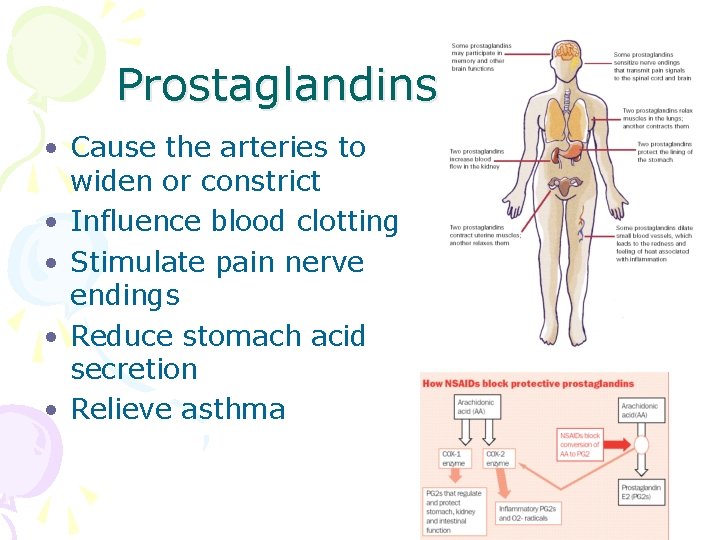
Prostaglandins • Cause the arteries to widen or constrict • Influence blood clotting • Stimulate pain nerve endings • Reduce stomach acid secretion • Relieve asthma
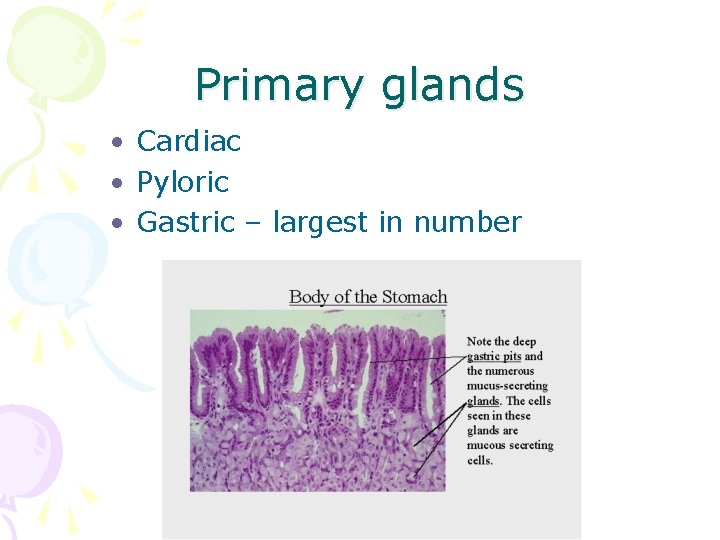
Primary glands • Cardiac • Pyloric • Gastric – largest in number

Gastric gland • Chief cells • Secretes pepsinogen (inactive form of pepsin) • Activated at a p. H of 2 • Breaks down proteins in diet
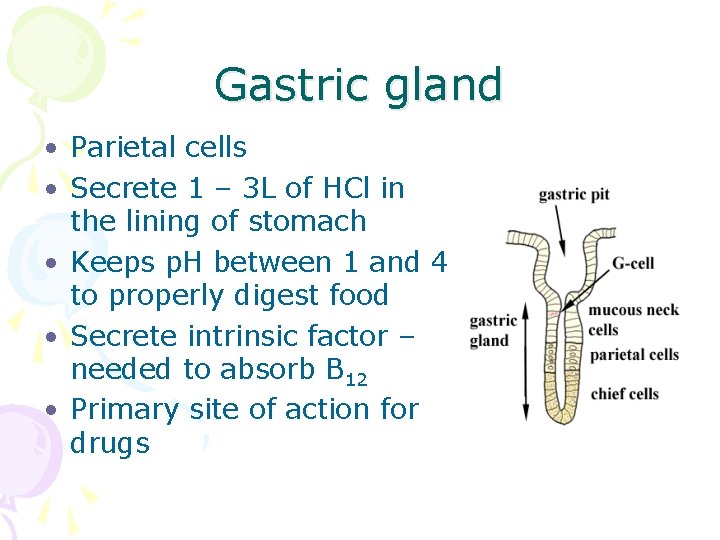
Gastric gland • Parietal cells • Secrete 1 – 3 L of HCl in the lining of stomach • Keeps p. H between 1 and 4 to properly digest food • Secrete intrinsic factor – needed to absorb B 12 • Primary site of action for drugs

Gastric Juice • Combined secretions from Chief cells and Parietal cells • Most acidic fluid in body • p. H 1. 5 -3. 5
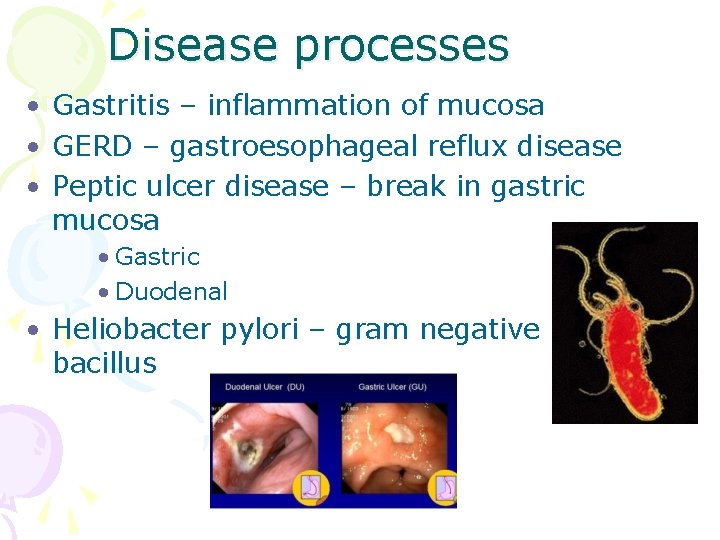
Disease processes • Gastritis – inflammation of mucosa • GERD – gastroesophageal reflux disease • Peptic ulcer disease – break in gastric mucosa • Gastric • Duodenal • Heliobacter pylori – gram negative bacillus
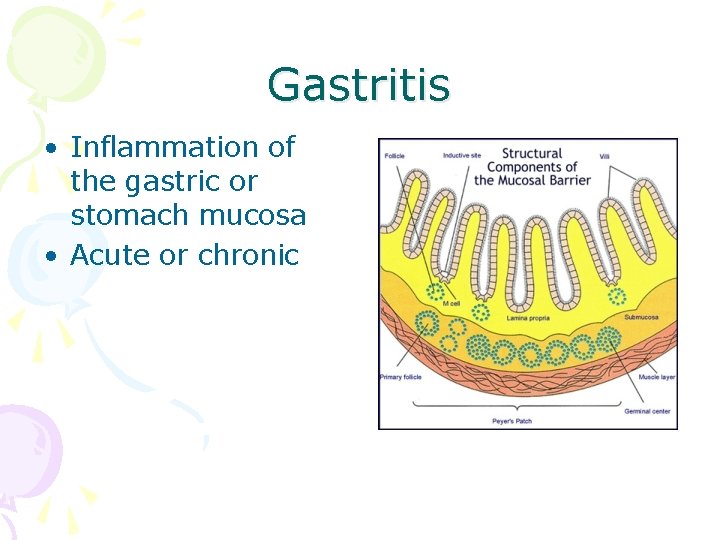
Gastritis • Inflammation of the gastric or stomach mucosa • Acute or chronic

Pathophysiology • Gastric mucous membrane becomes edematous • Hyperemia occurs • Mucosa undergoes superficial erosion • Potential for hemorrage
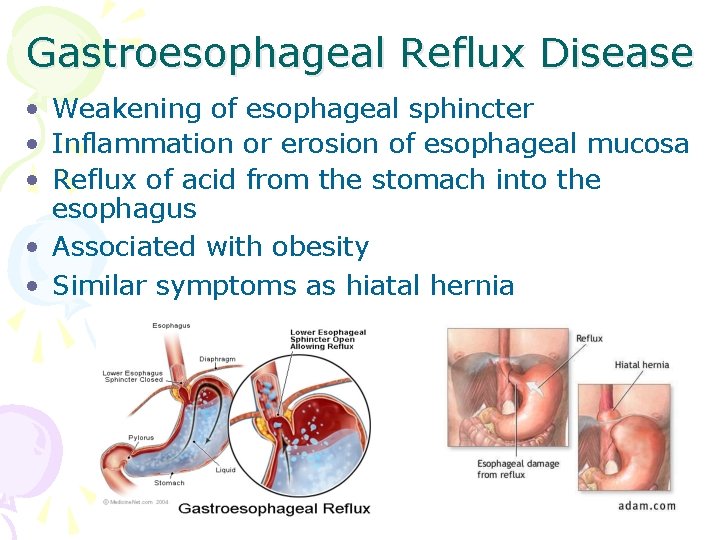
Gastroesophageal Reflux Disease • Weakening of esophageal sphincter • Inflammation or erosion of esophageal mucosa • Reflux of acid from the stomach into the esophagus • Associated with obesity • Similar symptoms as hiatal hernia

Symptoms of GERD • • • Heartburn with belching Heartburn after fatty or acidic foods Increased burning if laying down after eating Can lead to esophagitis or ulcers or strictures Pts frequently self treat with OTC meds

Risk factors for Peptic Ulcer (PUD) • • • Family hx of PUD Blood type O Smoking Caffeine Drugs: glucocorticoids, ASA, NSAIDs • Excessive psychological stress • Infection with H. pylori

Symptoms of Duodenal Ulcer • Gnawing or burning upper abd pain • Pain disappears with food intake • Nighttime abd pain • Nausea/ vomiting • Hemataemesis • Black, tarry stools

Symptoms of Gastric Ulcer • Pain may continue even after a meal • Anorexia • Weight loss • Vomiting • Less common than duodenal mass ulcer

Non-pharmacologic Tx of PUD • Lifestyle changes • Stop smoking, alcohol use • Reduce stress • Herbal: Ginger

Pharmacologic Treatment (Tx) • Goals: immediate relief from symptoms • Healing of the ulcer • Prevent future recurrence • Medication will depend on: – Disease – Severity of symptoms – Over-the-counter (OTC) vs. prescription (Rx)
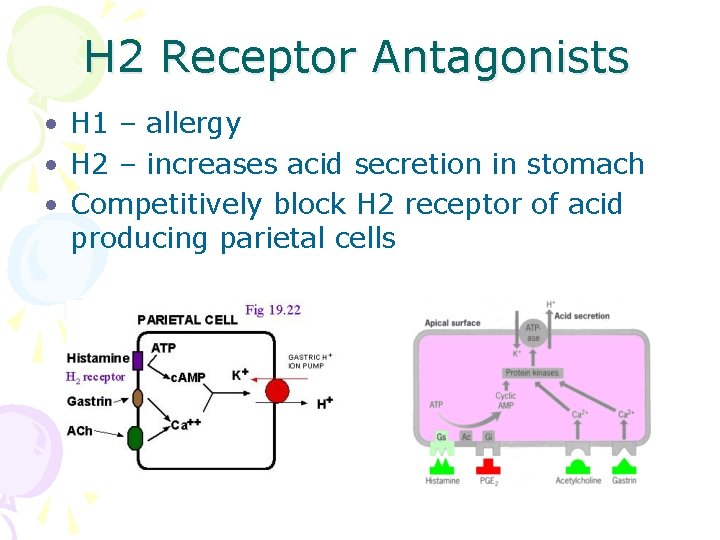
H 2 Receptor Antagonists • H 1 – allergy • H 2 – increases acid secretion in stomach • Competitively block H 2 receptor of acid producing parietal cells

H 2 Receptor Antagonists • Increase gastric p. H • Reduces the volume of gastric acid secretion • Reduce the concentration of the secretions

H 2 Antagonists – Uses • Hypersecretion of stomach acids • Gastro-esophageal reflux • Treatment and prophylaxis of duodenal ulcers • Prevention of upper GI bleed in critically ill patients • Adjunctive therapy for NSAID use

H 2 Antagonists – Nursing • Decrease absorption of drugs that require an acidic GI environment • Decrease absorption of H 2 Antagonist with antacids • Assess GI discomfort • Periodic evaluation of blood counts, gastric acid tests, renal/ hepatic tests

H 2 Antagonists – Nursing • Elderly – CNS effects of drowsiness, dizziness, confusion, headache • Liver and kidney function – may need smaller doses with impaired function • Decrease absorption of vitamin B 12 with prolonged use – increase in diet • Iron supplements

H 2 Antagonists – Education • Take last dose at bedtime - better suppression of nocturnal acid • Raise HOB for GERD clients to decrease reflux • Safety / fall precautions • No meal intake 2 hours prior to sleep

H 2 Antagonists – Education • No caffeine, alcohol, harsh spices, chocolate, or peppermint in diet • No smoking • No ASA • Call MD for bloody stools or increased abdominal pain
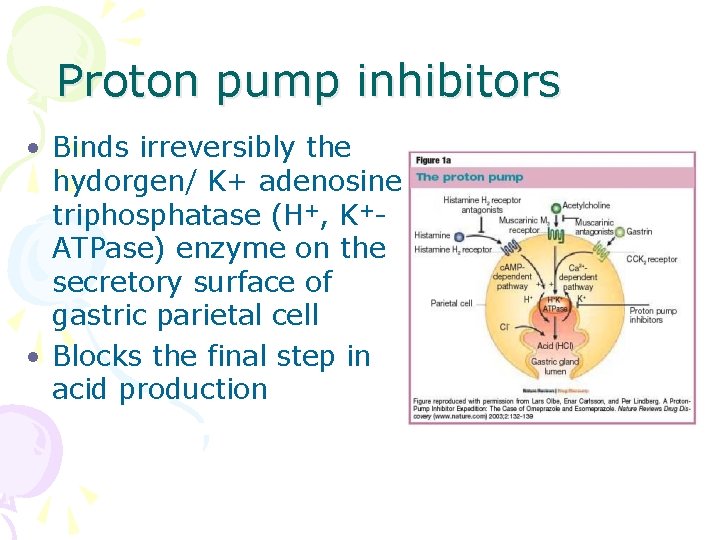
Proton pump inhibitors • Binds irreversibly the hydorgen/ K+ adenosine triphosphatase (H+, K+ATPase) enzyme on the secretory surface of gastric parietal cell • Blocks the final step in acid production
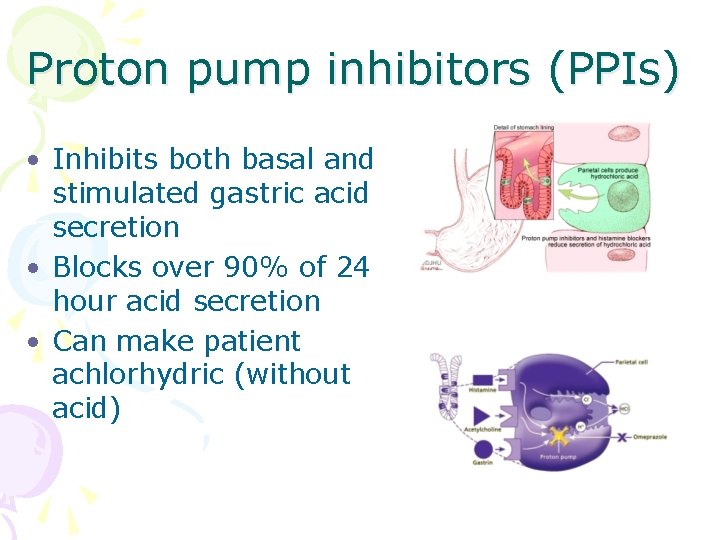
Proton pump inhibitors (PPIs) • Inhibits both basal and stimulated gastric acid secretion • Blocks over 90% of 24 hour acid secretion • Can make patient achlorhydric (without acid)

PPIs – Uses • GERD maintenance therapy • Long term treatment of active duodenal ulcer (Prilosec) • Active benign gastric ulcers • Treatment for H. Pylori (Prilosec/ Prevacid) • Hypersecretory condition – Zollinger-Ellison syndrome

PPIs – Nursing • Monitor for GI symptoms or headache • Effect of med – decreased GI reflux or heartburn • Frequency, consistency, and color of stools • Report GI bleeding, abd. pain & heartburn

PPIs – Education • Take meds prior to meals • Do not crush or chew • Difficulty swallowing, open capsules sprinkle on food • Can give with antacids • If given NG, flush with lots of water
PPIs – Education • No smoking, alcohol use, foods that cause gastric discomfort • Beneficial bacteria – yogurt or acidophilus • Sleep with HOB elevated – 30 degrees
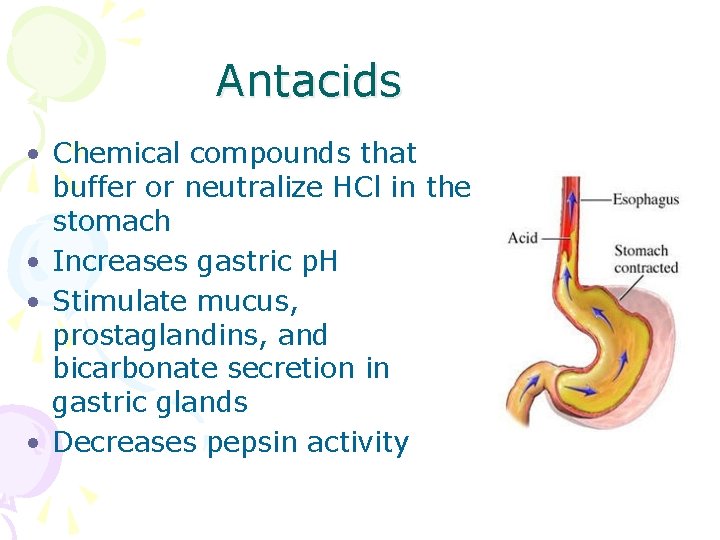
Antacids • Chemical compounds that buffer or neutralize HCl in the stomach • Increases gastric p. H • Stimulate mucus, prostaglandins, and bicarbonate secretion in gastric glands • Decreases pepsin activity

Antacids – Uses • • Hyperacidity related to PUD GERD Heartburn Replacement of minerals – Calcium • Usually has rapid onset of action and lasts 20 -40 min if patient is fasting

Antacids – Adverse • Systemic alkalosis – rare, will take a lot of meds • Sodium overload • Rebound acid production after discontinuance • Renal calculi • Decrease, bind or inactivate many drugs

Antacids – Nursing • Baseline assessment of patient’s pain/ nutritional status • Sensitivity to medications containing metals • Document response to medication • Document frequency and consistency of stools

Antacids – Nursing • Monitor urinary p. H, Ca, lytes, PO 4 • Renal failure – avoid Mag based meds • Heart failure and HTN – avoid Na based meds • NSAIDs – common adjunctive therapy

Antacids – Education • Liquid antacids > than tablets to neutralize acid • Liquid antacids diminish appetite • Shake liquid preps thoroughly • Full glass of water after taking meds • If giving through NG, flush with lots of water

Antacids – Education • Adhere to therapy schedule • Dosing schedule important: 2 hours after other meds, 1 hour prior • Stools may appear white • Check expiration of antacid • Identify source of gastric discomfort and educate to prevent recurrence
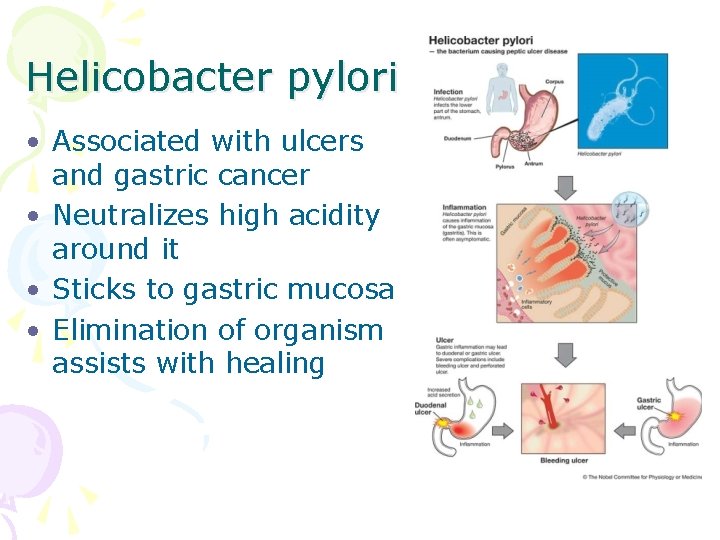
Helicobacter pylori • Associated with ulcers and gastric cancer • Neutralizes high acidity around it • Sticks to gastric mucosa • Elimination of organism assists with healing

Treatment of H. pylori • Antibiotics – Biaxin, Amoxicillin, Flagyl, Tetracycline • Bismuth – Pepto Bismol or Tritec • H 2 antagonist – Zantac OR PPI – Protonix • Treatment time 7 -14 days
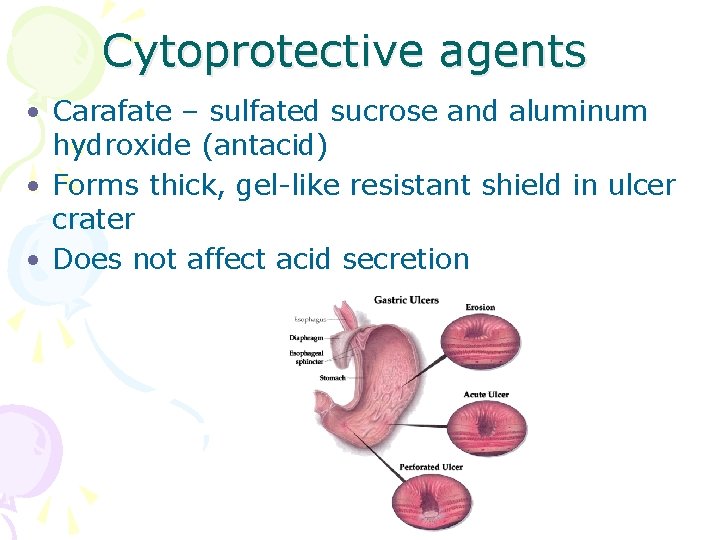
Cytoprotective agents • Carafate – sulfated sucrose and aluminum hydroxide (antacid) • Forms thick, gel-like resistant shield in ulcer crater • Does not affect acid secretion

Carafate – Nursing • Assess abdominal pain • Fluid and electrolyte balances • Gastric p. H (>5 desired) • Altered absorption with antacids • Risk of aluminum toxicity
Carafate – Education • Give on empty stomach • Antacids 30 minutes before or after Carafate • Up to 2 hours between carafate and other meds • 4 -8 weeks for optimal ulcer healing

Cytoprotective Agents – Cytotec • Synthetic prostaglandin • Decreases gastric acid secretion • Increase gastric cytoprotective mucus • Increase bicarbonate

Cytotec – Uses • Prevents gastric ulcers associated with NSAID use • Used in combination with methotrexate for surgically induced abortions

Cytotec – Nursing • Assess GI pain/ discomfort • Assess frequency, consistency, and color of stools • Start the same time as NSAID therapy starts

Cytotec – Nursing • Can be given with antacids • Use with magnesium antacids can cause diarrhea • Call for diarrhea episodes >1 week • Therapy – 4 weeks unless healing documented by endoscopic exam
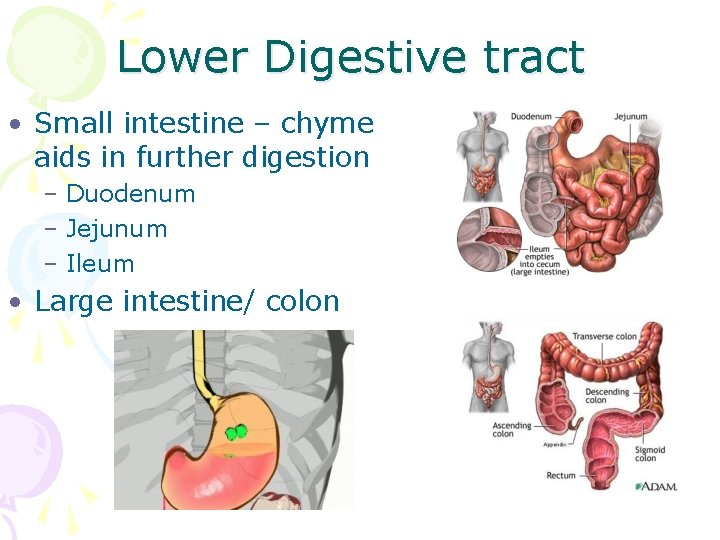
Lower Digestive tract • Small intestine – chyme aids in further digestion – Duodenum – Jejunum – Ileum • Large intestine/ colon

Lower digestive tract • Activation of parasympathetic increase peristalsis • Colon receives chyme in fluid state • Reabsorption of water • Excrete waste material • Host flora – bacteria & fungi
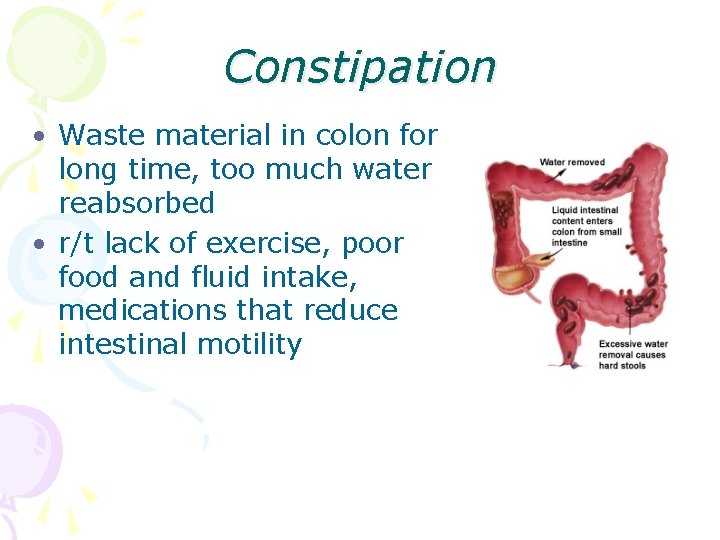
Constipation • Waste material in colon for long time, too much water reabsorbed • r/t lack of exercise, poor food and fluid intake, medications that reduce intestinal motility
Constipation • Common post-op complication • Seen more frequently in elderly • seek treatment with painful BM with severe straining • Can lead to complete bowel obstruction

Foods causing constipation • Alcohol • Foods with high content of white flour • Dairy • Chocolate

Laxatives • Treatment of constipation • Abnormal, infrequent, and difficult passage of feces through the lower GI tract • Used as prep for medical procedures • Used to facilitating removal of unwanted substances from the body
![Laxatives – promote bowel by: • [Constipation is a symptom, not a disease] • Laxatives – promote bowel by: • [Constipation is a symptom, not a disease] •](http://slidetodoc.com/presentation_image/67ce606194d7c2162adec3d7671b2dc0/image-58.jpg)
Laxatives – promote bowel by: • [Constipation is a symptom, not a disease] • Affecting fecal consistency • Increasing fecal movement through colon • Removing stool from the rectum • Cathartic – stronger, more complete emptying

Bulk-forming laxatives • • • Act like fiber naturally in diet Absorb water into intestine Increases bulk, distends bowel Initiates reflex bowel activity Used to prevent constipation

Bulk-Forming – Nursing • Give with at least 2 glasses of water/ fluid • Give right away, do not wait • Make sure patient can swallow to reduce risk of blockage • Take at different time than meds to ensure proper absorption
Stool softener • Docusate salts – Colace, Dialose, Surfak • Helps avoid straining for medical or surgical situations • Softening of fecal impacts • Facilitates bowel of anorectal conditions

Stimulant • Stimulate nerves that innervate intestine • Irritate bowel • Increased peristalsis • Increases fluid in the colon • Increases bulk, softens stool

Stimulant • Acute constipation • Diagnostic preps • Surgical preps
Stimulant – Nursing • Rapid and potent effects • Safety precautions – need for BRP assist • Combo therapy with osmotics and enemas for preps • Assess for dehydration – IV fluids • Changes in vital signs

Laxatives – Nursing • Document frequency, consistency, and color of stools • Vital signs • Patient comfort during defecation • Review medical history for causative factors

Laxatives – Nursing • Bowel status by careful assessment • Suppositories – go past anal sphincter • Enemas – lay on left side, ask patient to hold as long as possible • Avoid habitual use of laxatives
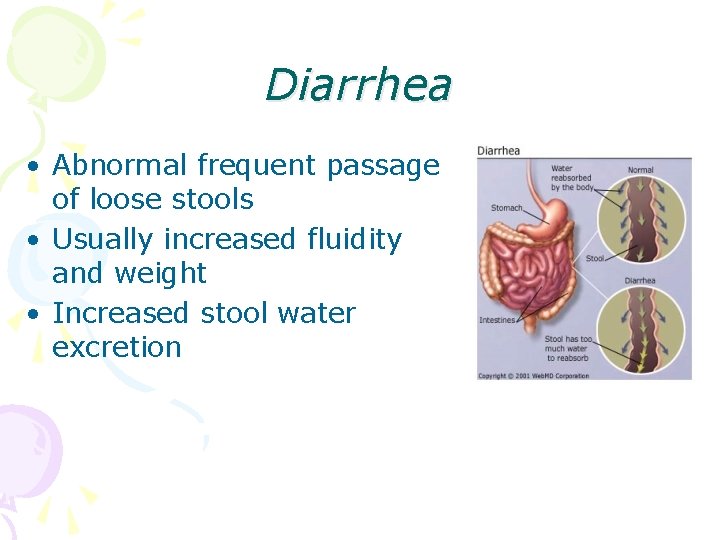
Diarrhea • Abnormal frequent passage of loose stools • Usually increased fluidity and weight • Increased stool water excretion
Diarrhea • May be caused by medications • Infections of the bowel • Prolonged use of antibiotics – kills flora • Overgrowth of opportunistic organisms
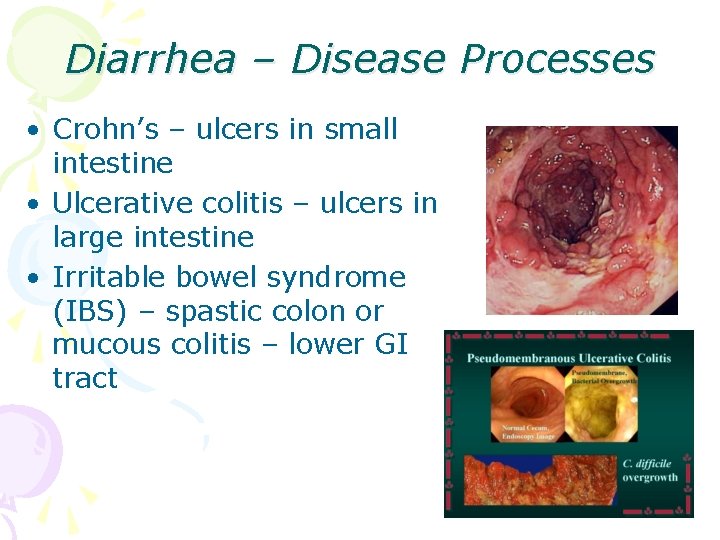
Diarrhea – Disease Processes • Crohn’s – ulcers in small intestine • Ulcerative colitis – ulcers in large intestine • Irritable bowel syndrome (IBS) – spastic colon or mucous colitis – lower GI tract

Drug therapy for Diarrhea • • • Dependent on causative agent Antibiotic/ anti-parasitic Anti-inflammatory Stop offending drug Lower offending drug Substitute offending drug

Opioids • Most effective treatment • Decreases bowel motility • Slow peristalsis increase fluid/ electrolyte reabsorption in intestines • Reduce pain associated with diarrhea and rectal spasms • Reduces stool frequency and volume

Opioids – Nursing • Safety for BRP • Abdominal assessment – effectiveness of drugs • Stop meds once diarrhea resolved • Call if bloody stools Motofen

Anti-diarrheals – Nursing • Determine cause of diarrhea • Monitor stools for frequency and consistency • Bowel sounds
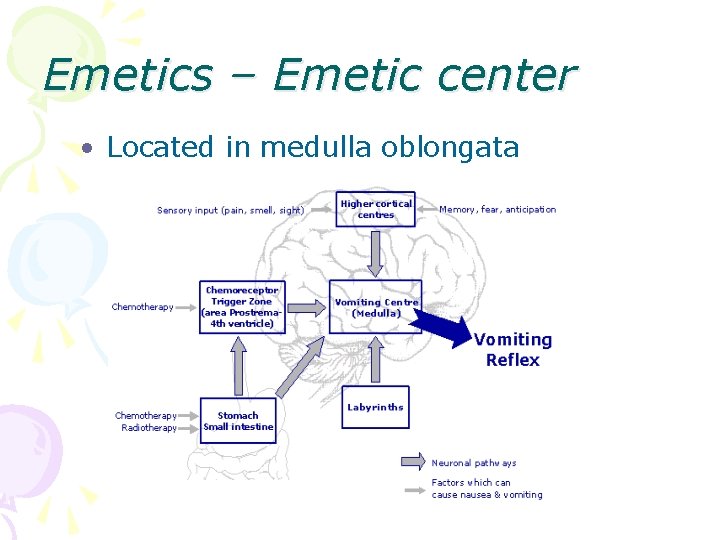
Emetics – Emetic center • Located in medulla oblongata
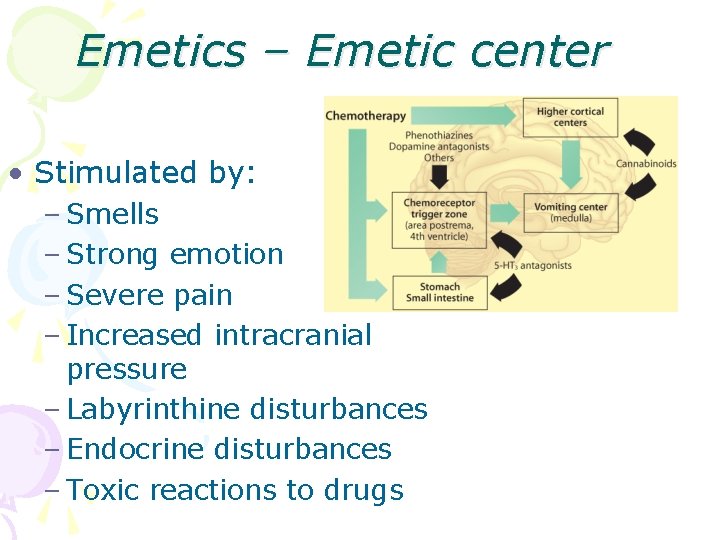
Emetics – Emetic center • Stimulated by: – Smells – Strong emotion – Severe pain – Increased intracranial pressure – Labyrinthine disturbances – Endocrine disturbances – Toxic reactions to drugs
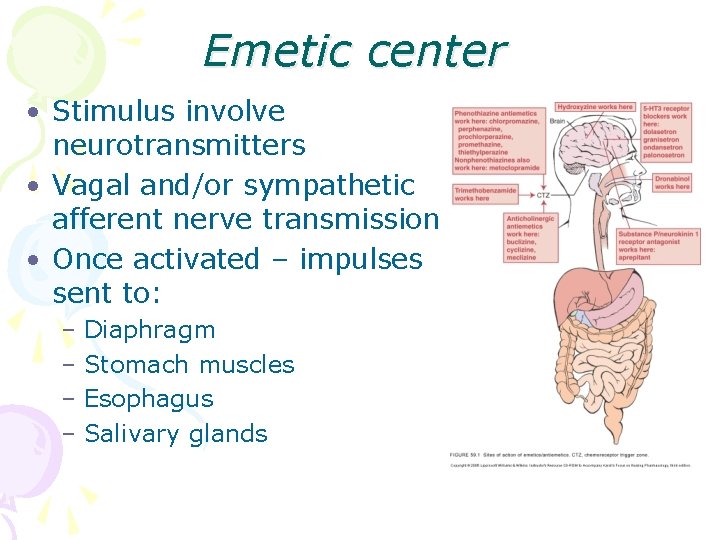
Emetic center • Stimulus involve neurotransmitters • Vagal and/or sympathetic afferent nerve transmission • Once activated – impulses sent to: – Diaphragm – Stomach muscles – Esophagus – Salivary glands

Antihistamines • Promethazine (Phenergan) • Meclizine (Antivert, Dramamine) • Diphenhydramine (Benadryl)

Antihistamines – Uses • • • Motion sickness Non-productive cough Sedation Rhinitis Allergy symptoms Nausea/ vomiting

Antihistamines – Nursing • If to prevent nausea, give 30 minutes prior to noxious stimulus • If for sleep, safety precautions • Document effectiveness • Phenergan not compatible with LR IV solution

Cannabinoids • Inhibitory effects in reticular formation, thalamus, and cerebral cortex • Synthetic derivative of tetrahydrocannabinol Marijuana • Dronabinol (Marinol) • Nabilone (Cesamet)

Cannabinoids – Uses • Nausea/ vomiting associated with chemo • Anorexia/ weight loss in AIDS patients (stimulate appetite) • Glaucoma

Cannabinoids – Adverse • • • Drowsiness Confusion Euphoria Visual disturbances Speech difficulty

Cannabinoids – Nursing • Vital signs – increase HR, decrease temp • Decreases REM sleep • Risk of drug abuse high

Cannabinoids – Nursing • Can have withdrawal symptoms if stopped abruptly: irritability, insomnia, restlessness, diaphoresis • Drug-induced mood or behavior changes

Uses • Commonly used for prevention of nausea vomiting in cancer therapy • Decadron – push slowly, can give “crotch itch” • Emend – newest class of drugs used after chemo

Anti-emetics – Nursing • Find cause of vomiting • NG tube if patient unconscious and vomiting • Safety precautions for drowsiness • Amount, color, consistency of emesis
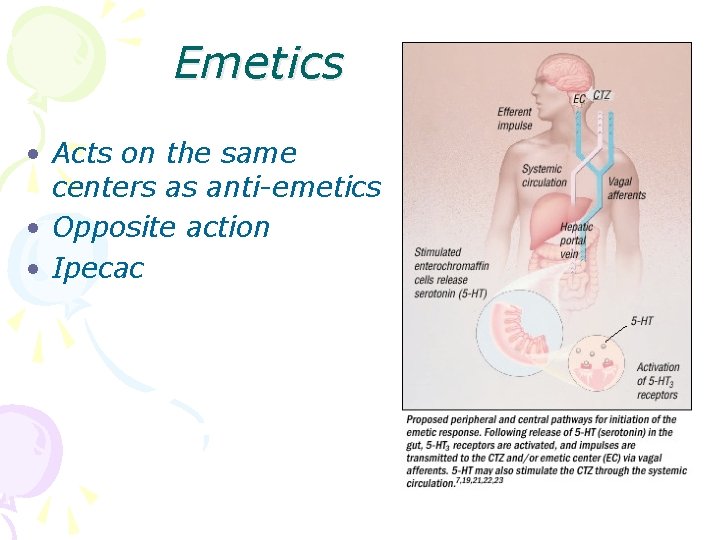
Emetics • Acts on the same centers as anti-emetics • Opposite action • Ipecac

Emetics – Uses • Treatment of oral drug overdose • Treatment of oral poisoning

Emetics – Nursing • Assess vitals and LOC • Call poison control before giving Ipecac • Vomiting is never induced in an unconscious patient • Watch for aspiration of emesis • Used for strychnine poisoning may precipitate seizures

Emetics – Nursing • Document amount, color, character of emesis • Monitor VS before and after administration • Monitor drug levels for toxicity

Emetics – Nursing • Follow syrup with water • Maintain fluid/ electrolyte balance • Do not give with charcoal as charcoal will absorb emetic component of ipecac

Emetics – Education • If kept at home, read directions • Poison control center number by phone • Keep out of reach of small children • Never give to unconscious person

Charcoal • • Used for tx of upset stomach Used for tx of flatulence Lower cholesterol levels Treat cholestasis Used for tx of poisonings Absorbs content Can be put directly on wounds for healing
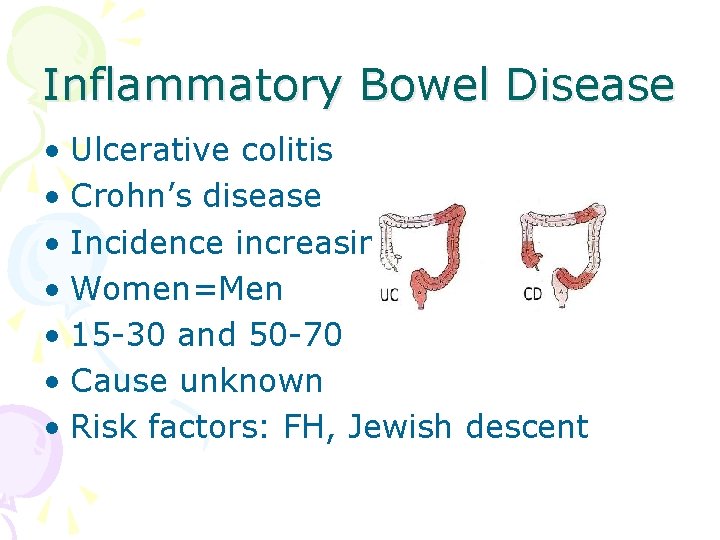
Inflammatory Bowel Disease • Ulcerative colitis • Crohn’s disease • Incidence increasing • Women=Men • 15 -30 and 50 -70 • Cause unknown • Risk factors: FH, Jewish descent

Crohn’s Disease • Inflammation of GI tract extending through all layers • Distal ileum and ascending colon • Remissions and exacerbations • Fissure, fistulas, abscess

Signs & Symptoms: Crohn’s Disease • RLQ pain-unrelieved with defecation • Diarrhea • Crampy abdominal pain • Occurs after meals • Weight loss • Malnutrition • anemia

Signs & Symptoms Crohn’s Disease • Stools less frequent and are semisolid • Usually no blood in stool • Steatorrhea if small bowel is affected • RLQ cramping my mimic appendicitis, pain is diffuse

Diagnostics: Crohn’s Disease • Sigmoidoscopy • UGI with barium-”string sign” in terminal ileum • Biopsy
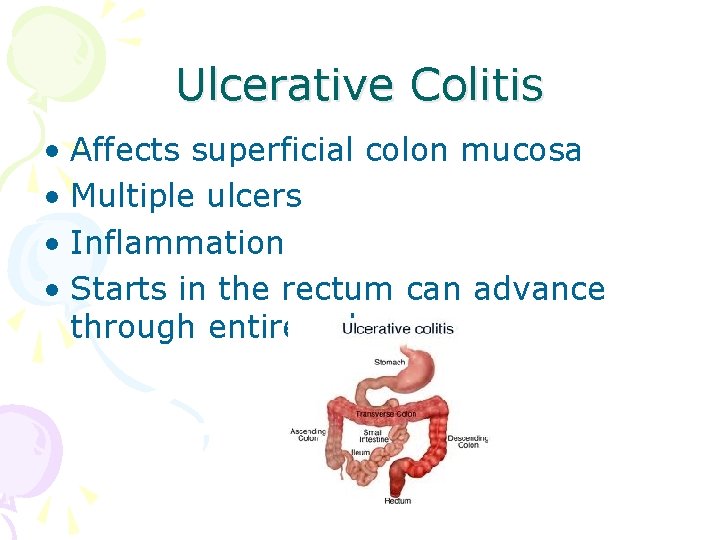
Ulcerative Colitis • Affects superficial colon mucosa • Multiple ulcers • Inflammation • Starts in the rectum can advance through entire colon

Signs & Symptoms: Ulcerative Colitis • Exacerbations and remissions of inflammation • Weight loss • Bleeding mild to severe • Anemia • Fatigue • LLQ pain, tenesmus • Extra-intestinal manifestations: skin, eye, joint, liver

Signs & Symptoms: Ulcerative Colitis • Frequent diarrhea • Stool contains mucous, blood and pus • Abdominal cramping prior to bowel movement • Fluid and electrolyte loss • Potential precursor to colon cancer

Diagnostics: Ulcerative Colitis • CBC-anemia • OB tests + • Leukocytosis • Decreased albumin • Electrolyte imbalance • Sigmoidoscopy • biopsy

Meds for IBD • Initially may have TPN • Antibiotics (esp with Crohn’s) – Flagyl • Immunomodulation – Methotrexate

Meds for IBD • Acute stages: – Anti-diarrheals – Sedatives (prior to procedures – Anti-perastaltics • diphenoxylate

Pharmacologic Management • Aminosalicylates (anti. Inflammatories – Sulfasalazine/ Azulfadine – Olsalazine/ Dipentum – Mesalamine/ Asacol or Pentasa – Balsalazide/ Colazal
Meds for IBD • Corticosteroids – Prednisone • Monoclonal antibodies – Infliximab/Remicade – Natalizumab/ Tysabri

Meds for IBD • Immunosuppressives (Immune modifiers) – Azothioprine/ Imuran – Mercaptopurine/ Purinethol – Cyclosporine/ Sandimmune

Nursing Interventions: IBD • Promote rest • Support groups/coping • Self management • Pain relief: anticholenergic 30” before meals. Dicyclomine. • Nutrition • Decrease anxiety • Follow up care

Management of IBD • Decrease inflammation • Suppress immune response • Bowel rest • Minimize complications • Nutritional support • Medications • Surgery: total colectomy, ileostomy
- Slides: 109