Gastrointestinal Blueprint PANCE Blueprint Esophagus Esophagitis Many causes
Gastrointestinal Blueprint PANCE Blueprint
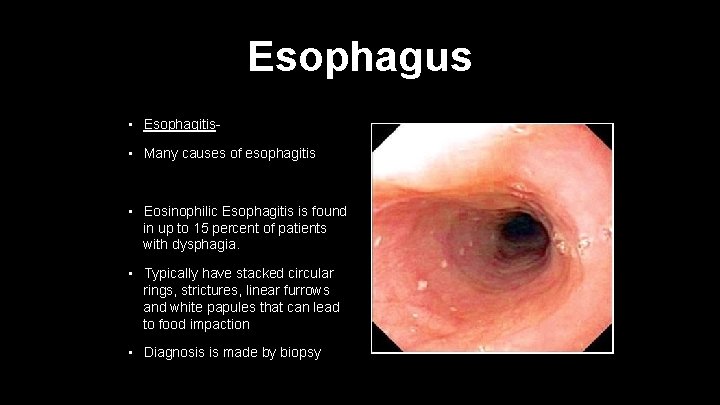
Esophagus • Esophagitis- • Many causes of esophagitis • Eosinophilic Esophagitis is found in up to 15 percent of patients with dysphagia. • Typically have stacked circular rings, strictures, linear furrows and white papules that can lead to food impaction • Diagnosis is made by biopsy

Esophagitis • Treated by elimination of dietary elements that cause allergic response. Start patient on proton pump inhibitor. • Topical steroids can be helpful in eosinophilic esophagitis • Esophageal dilation necessary for patients with symptomatic strictures • Radiation esophagitis may occur in patients being treated for head, neck, or thoracic cancers. • These patients have dysphagia and odynophagia
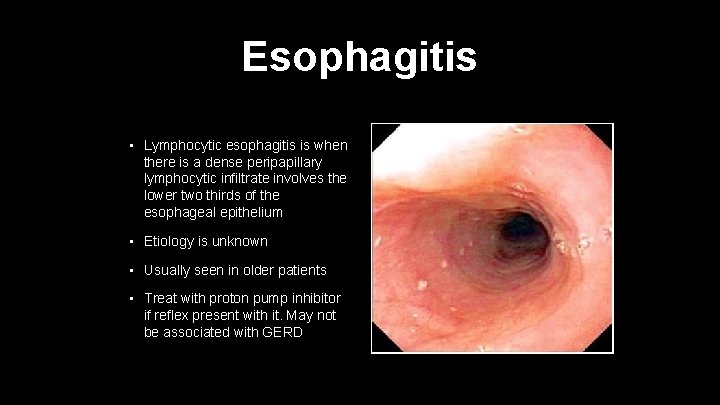
Esophagitis • Lymphocytic esophagitis is when there is a dense peripapillary lymphocytic infiltrate involves the lower two thirds of the esophageal epithelium • Etiology is unknown • Usually seen in older patients • Treat with proton pump inhibitor if reflex present with it. May not be associated with GERD

Esophagitis • Infectious Esophagitis due to many causes. Most common herpes simplex virus • Other causes of infectious causes such as cytomegalovirus (CMV), candidia, cryptococcosis, histoplasmosis, blastomycosis, and aspergilliosis • Immunosuppression should be suspected if present • Medication Induced Esophagitis caused by largely 3 groups of medications: antibiotics, NSAIDS< and others
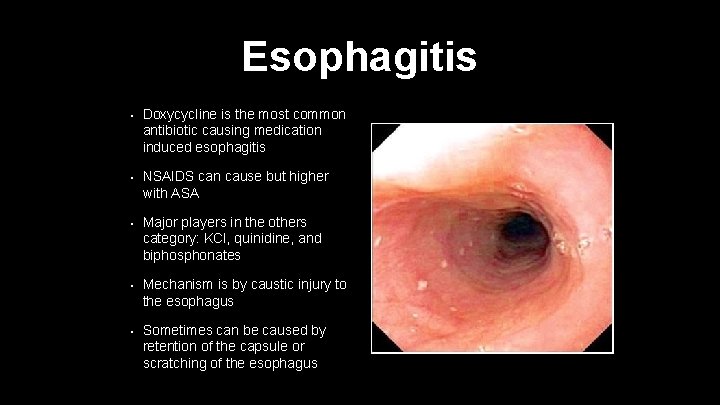
Esophagitis • Doxycycline is the most common antibiotic causing medication induced esophagitis • NSAIDS can cause but higher with ASA • Major players in the others category: KCl, quinidine, and biphosphonates • Mechanism is by caustic injury to the esophagus • Sometimes can be caused by retention of the capsule or scratching of the esophagus

Esophagitis • The most important therapy is to take the offending medication away • PPI's, antacids, and carafate can be prescribed but their value has not been significantly demonstrated. • Reflux esophagitis is due to hydrogen ion diffusion into the mucosa leading to cellular acidification and necrosis • Impaired esophageal emptying or decreased salivary function can contributed to increased exposure of the esophagus to the acid and induce this pathology
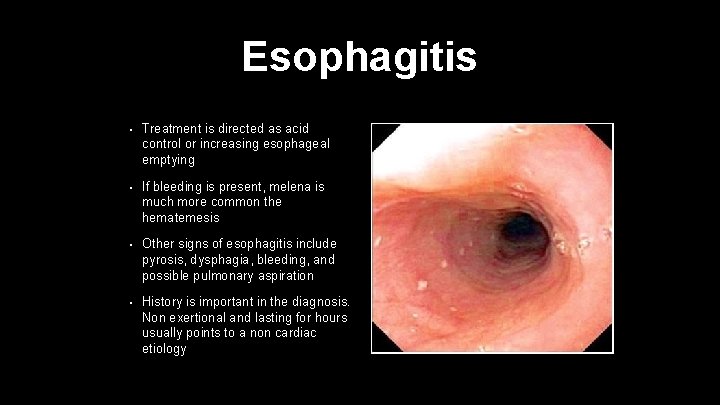
Esophagitis • Treatment is directed as acid control or increasing esophageal emptying • If bleeding is present, melena is much more common the hematemesis • Other signs of esophagitis include pyrosis, dysphagia, bleeding, and possible pulmonary aspiration • History is important in the diagnosis. Non exertional and lasting for hours usually points to a non cardiac etiology

Esophagitis • Other key elements include possibly awakens from sleep, worse after meals, and aggravated by lying down. • Usually improved with standing or sitting up. • Treatment can involve PPI, H 2 blockers, antacids, reglan (helps gastric emptying), and carafate • Non pharmacologic measures include weight loss, elevating head of the bed, and eliminating eating before bedtime or laying down.
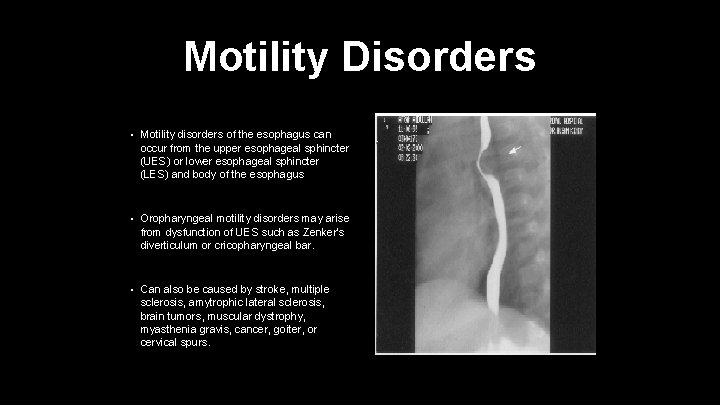
Motility Disorders • Motility disorders of the esophagus can occur from the upper esophageal sphincter (UES) or lower esophageal sphincter (LES) and body of the esophagus • Oropharyngeal motility disorders may arise from dysfunction of UES such as Zenker's diverticulum or cricopharyngeal bar. • Can also be caused by stroke, multiple sclerosis, amytrophic lateral sclerosis, brain tumors, muscular dystrophy, myasthenia gravis, cancer, goiter, or cervical spurs.

Motility Disorders • High incidence of aspiration with these disorders • Diagnosis with rapid sequence cine esophagography. Endoscopy plays a supportive role • Treatment is directed at reversing potential causes, aspiration precautions, and considering PEG tube if the underlying disorder is at high risk of aspiration • The body of the esophagus can have motility disorders that arise from the smooth muscle or the intrinsic nervous system

Motility Disorders • Scleroderma affects the smooth muscle of the esophagus and achalasia and Chagas disease are affected by disorders of the intrinsic nervous system • Other disorders can cause diffuse esophageal spasm • Cine esophagography and esophageal manometry confirms the diagnosis • Achalasia usually responds to brisk dilation of the LES or surgical myotomy
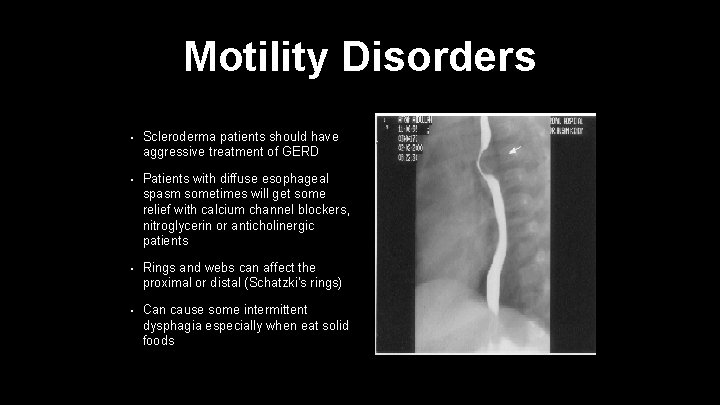
Motility Disorders • Scleroderma patients should have aggressive treatment of GERD • Patients with diffuse esophageal spasm sometimes will get some relief with calcium channel blockers, nitroglycerin or anticholinergic patients • Rings and webs can affect the proximal or distal (Schatzki's rings) • Can cause some intermittent dysphagia especially when eat solid foods
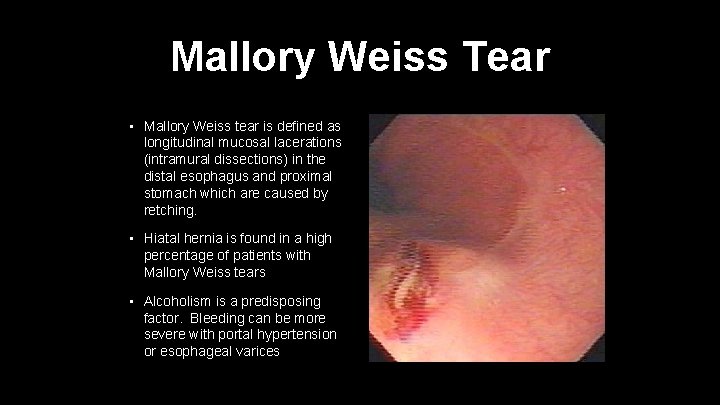
Mallory Weiss Tear • Mallory Weiss tear is defined as longitudinal mucosal lacerations (intramural dissections) in the distal esophagus and proximal stomach which are caused by retching. • Hiatal hernia is found in a high percentage of patients with Mallory Weiss tears • Alcoholism is a predisposing factor. Bleeding can be more severe with portal hypertension or esophageal varices

Mallory Weiss Tear • Presenting symptoms are acute GI bleeding, epigastric abdominal pain or back pain • Bleeding occurs because of a tear that involves the esophageal venous or arterial plexus • Patients usually have non bloody vomitus before the bleeding starts • High percentage of patient need a blood transfusion but bleeding is self limited
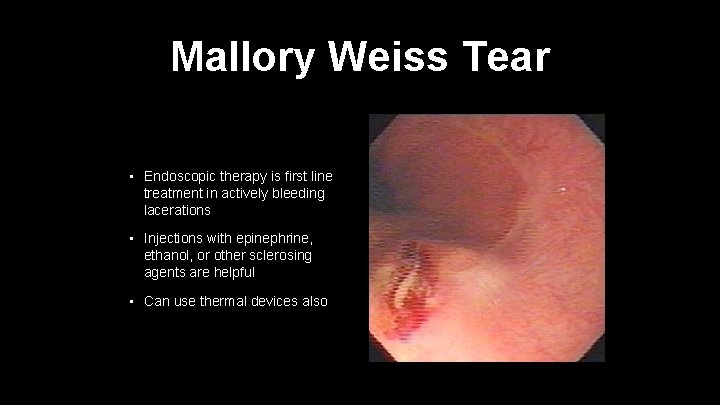
Mallory Weiss Tear • Endoscopic therapy is first line treatment in actively bleeding lacerations • Injections with epinephrine, ethanol, or other sclerosing agents are helpful • Can use thermal devices also
Esophageal Neoplasms • Most esophageal cancers are squamous cell or adenocarcinomas • Barrett's esophagus can give rise to adenocarcinoma • Small cell carcinoma and sarcoma can arise out of the distal esophagus • Family aggregation has been described with a high incidence of squamous cell carcinoma in China. • Family history is a good indicator for Barrett's esophagus

Esophageal Neoplasms • The presence of underlying esophageal disease such as achalasia and caustic strictures increases the risk of esophageal cancer • Prior gastrectomy increases the risk for squamous cell carcinoma • Atrophic gastritis, human papilloma virus, tylosis, biphosphonates, and poor oral hygiene have been shown to increase the risk of esophageal cancer • Most all of adenocarcinomas arise from a region of Barrett's esophagus which is due to GERD

Esophageal Neoplasms • Smoking increases the risk form adenocarcinoma of the esophagus • Alcohol consumption does not increase the risk for esophageal adenocarcinoma • Obesity has been liked to esophageal adenocarcinoma and adenocarcinoma of the gastric cardia • Zollinger Ellison Syndrome may be at increased risk for adenocarcinoma
Esophageal Neoplasms • Use of drugs that decreased lower esophageal sphincter pressure may increases the risk of adenocarcinoma • Cholecystectomy and nitrosative stress have been associated with carcinogenesis • NSAIDS may have a protective effects • Patients with locally advanced cancer can cause some solid food dysphagia

Esophageal Neoplasms • Weight loss may happen from dysphagia • Aspiration pneumonia can happen but infrequent • Chronic GI blood loss is common with esophageal cancer with melena • Tracheobronchial fistulas are a late complication of esophageal cancer because of the direct invasion through the esophageal wall to the main stem bronchus • Esphogectomy is the treatment of choice for superficial esophageal cancers

Esophageal Neoplasms • The cancer has to be staged as well as the depth determined • Evaluation for distant metastasis can be done with CT or PET scanning • Criteria for unresectable disease includes: distant metastasis to peritoneal, lung, bone, adrenal, brain, or liver mets, thoracic or abdominal esophagus near great vessels, heart or trachea, cervical esophageal tumors • Palliative surgical resection is usually not indicated • External beam radiation therapy (EBRT) is indicated for unresectable cancer • Chemotherapy and radiation therapy is the standard nonoperative management for unresectable therapy
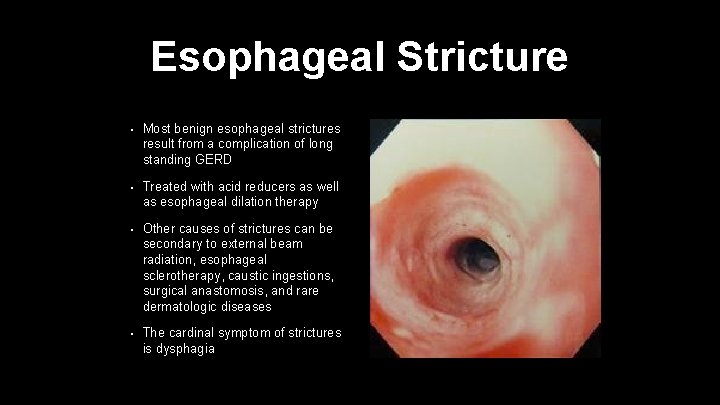
Esophageal Stricture • Most benign esophageal strictures result from a complication of long standing GERD • Treated with acid reducers as well as esophageal dilation therapy • Other causes of strictures can be secondary to external beam radiation, esophageal sclerotherapy, caustic ingestions, surgical anastomosis, and rare dermatologic diseases • The cardinal symptom of strictures is dysphagia

Esophageal Stricture • Contraindications to esophageal dilation include: incomplete healed perforation, potentially malignant stricture, pharyngeal or cervical deformity, caution with eosinophilic esophagitis, large thoracic aneurysm, and impacted food bolus • Can be dilated with balloon dilators or mechanical dilators • Simple strictures are related to reflux esophagitis • Complex strictures are long, narrow, tortuous, or strictures associated with hiatal hernias and esophageal diverticulae.
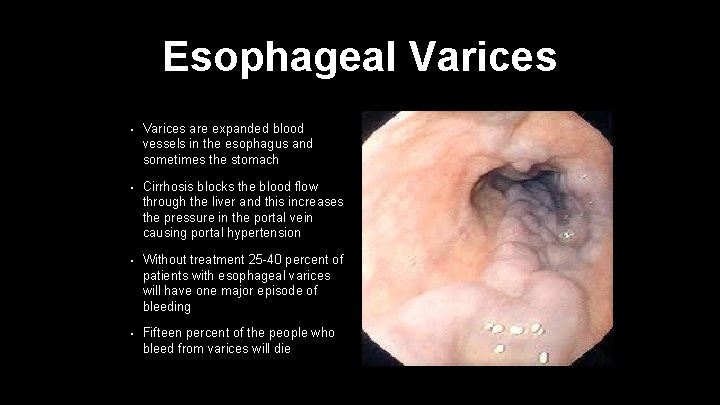
Esophageal Varices • Varices are expanded blood vessels in the esophagus and sometimes the stomach • Cirrhosis blocks the blood flow through the liver and this increases the pressure in the portal vein causing portal hypertension • Without treatment 25 -40 percent of patients with esophageal varices will have one major episode of bleeding • Fifteen percent of the people who bleed from varices will die

Esophageal Varices • Varices do not cause symptoms until the bleed or ruptures • Treatment involves beta blockers for those that have refractory ascites • patients need to avoid alcohol and lose weight • Variceal band ligation can be placed around the varices to prevent them from bleeding • PPI's help speed the healing of erosions and ulcers that develop when the band falls off the varices. • If they rupture will need massive blood transfusion, volume replacement, and emergent endoscopy
- Slides: 26