GASTROESOPGHEAL REFULX DISEASE IN CHILDREN Dr Shrish Bhatnagar

GASTROESOPGHEAL REFULX DISEASE IN CHILDREN Dr Shrish Bhatnagar

Dedication JNMC SGPGIMS Dr S K BHATNAGAR

DEFINATION • Gastroesophageal reflux or GER means Involuntary passage of gastric contents into the esophagus and is often Physiological but gastroesophageal reflux disease or GERD means symptoms or complications associated with pathological GER
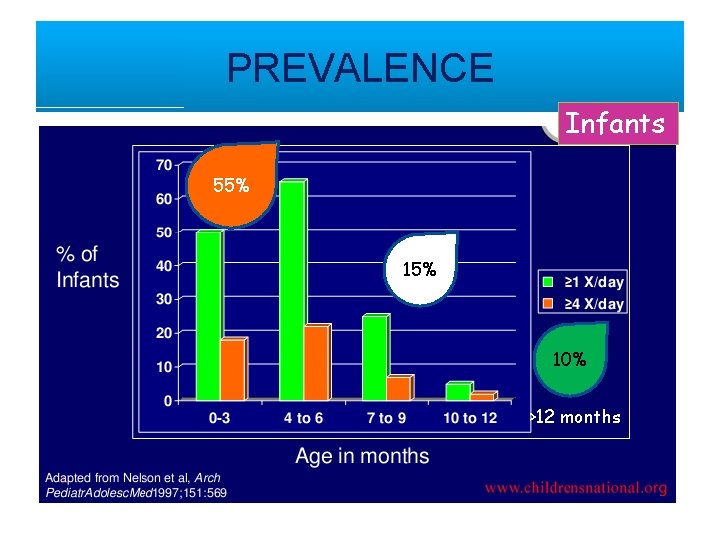
PREVALENCE Infants 55% 10% >12 months

Prevalence of GERD • GERD is defined to be present when reflux of gastric contents causes either troublesome symptoms or complications. • In a study from USA involving pyrosis or heartburn was reported in 1. 8% of the 3 -9 years age group and 3. 5% in the 10 to 17 years age group compared to 22% in adults (>18 years). • Hence, the prevalence of GERD slowly increases with age during childhood and becomes quite frequent among young adults.

Presenting symptoms

History

Case Snippet 1 • Newborn presents with bilious vomiting on day 3 • Clinically: dehydrated • Bilious vomiting usually suggests a small intestinal obstruction and we would normally expect a distended abdomen but • Abdomen: soft and sunken!
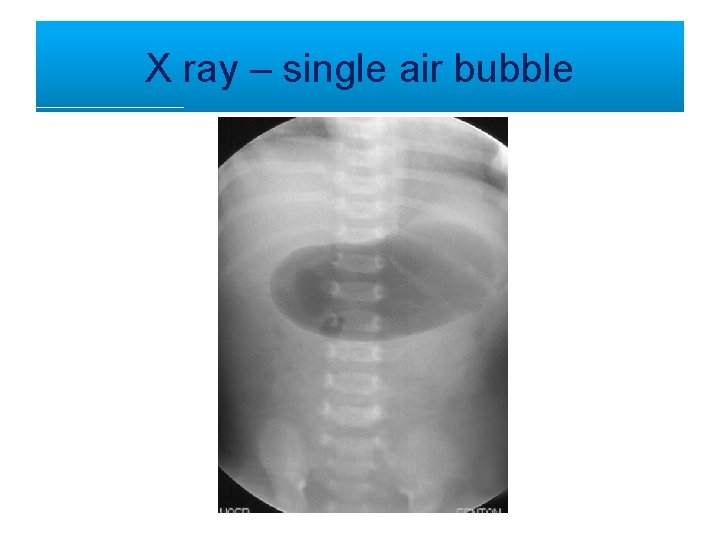
X ray – single air bubble
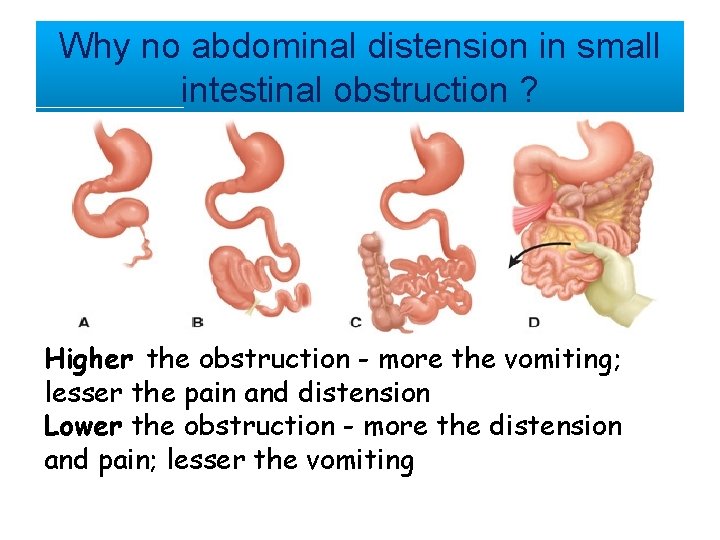
Why no abdominal distension in small intestinal obstruction ? Higher the obstruction - more the vomiting; lesser the pain and distension Lower the obstruction - more the distension and pain; lesser the vomiting

USG ABDOMEN 1. Pylorospasm 2. SMA SMV relationship axis on transverse images reversal sign should make us strongly suspect malrotation 3. The “whirlpool” sign - SMV wrapping around SMA is rare
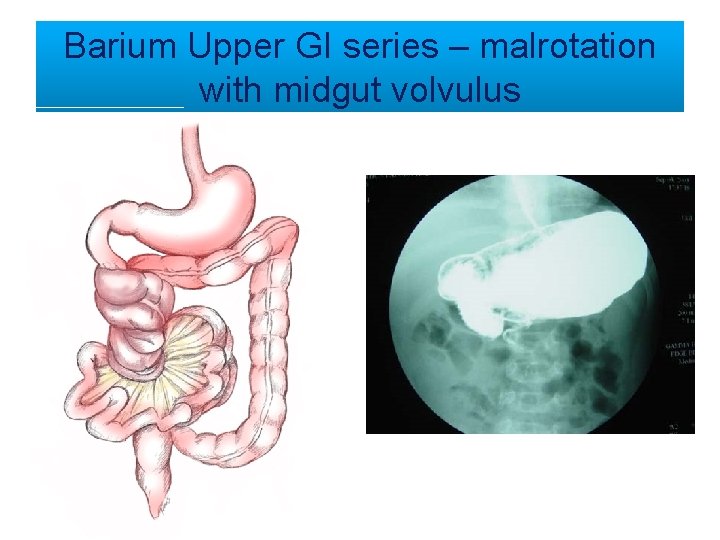
Barium Upper GI series – malrotation with midgut volvulus
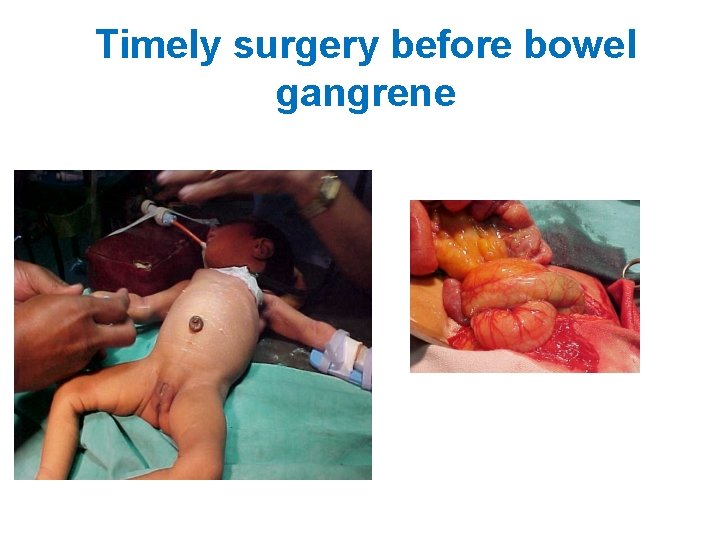
Timely surgery before bowel gangrene
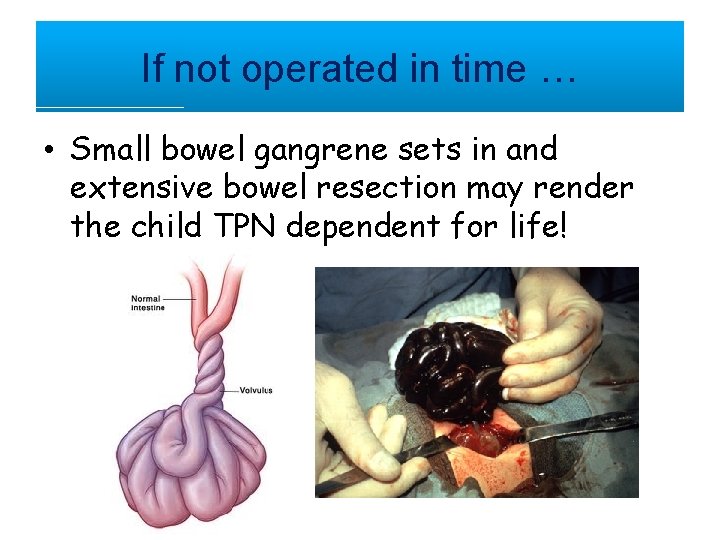
If not operated in time … • Small bowel gangrene sets in and extensive bowel resection may render the child TPN dependent for life!

Clinical Scenarios of GER/GERD Case I : 5 month old who effortlessly spits-up 6 – 10 x/day, but seems comfortable and is growing well Case II : 4 month old who is losing weight is reported to vomit 2– 3 x/day, and seems increasingly fussy with feeds Case III : 15 year old who presents complaining of heartburn
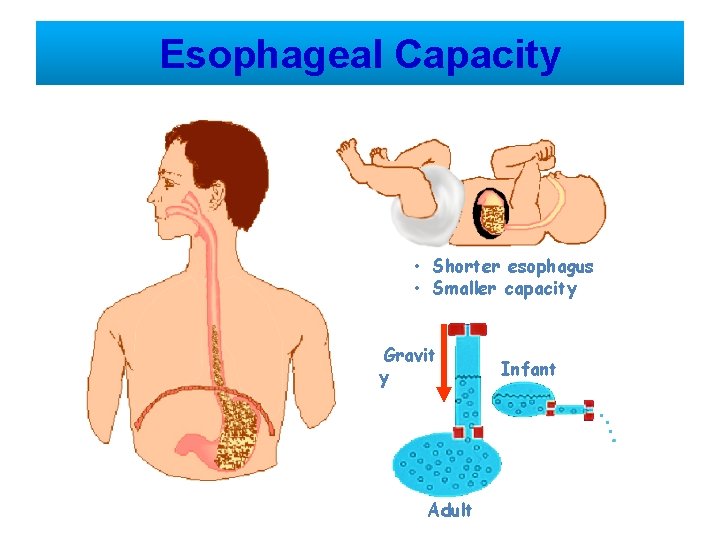
Esophageal Capacity • Shorter esophagus • Smaller capacity Gravit y Adult Infant
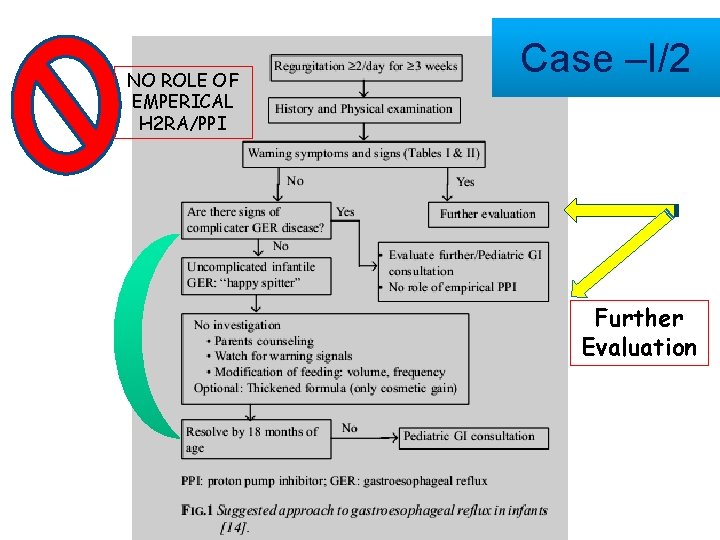
NO ROLE OF EMPERICAL H 2 RA/PPI Case –I/2 Further Evaluation
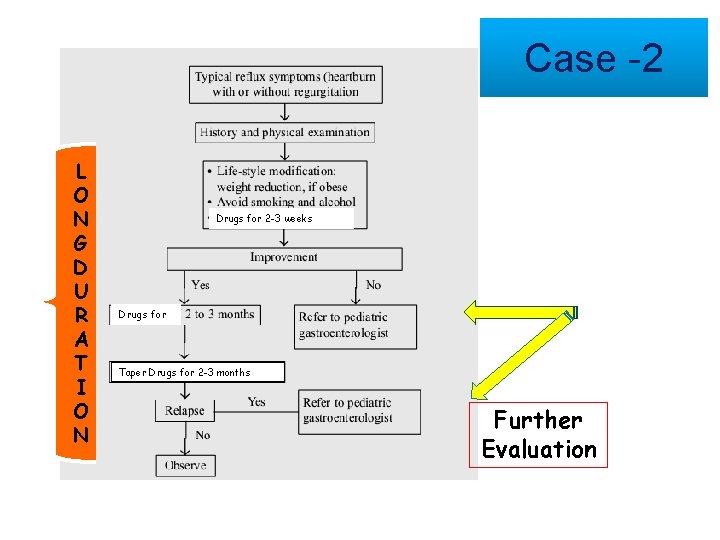
Case -2 L O N G D U R A T I O N Drugs for 2 -3 weeks Drugs for Taper Drugs for 2 -3 months Further Evaluation

Conditions predisposing to Severe GERD

Testing for Reflux Disorders • No one test can be used to diagnose reflux, and instead must be matched to a clinical question • Reflux tests are useful – To document the presence of GER(D) – To detect complications – To establish a causal relationship between GER and symptoms – To evaluate therapy – To exclude other conditions BARIUM STUDIES OBSOLETE
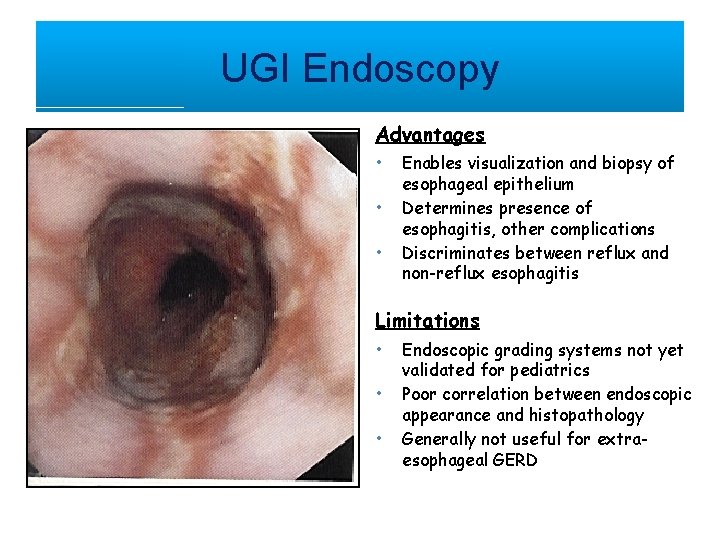
UGI Endoscopy Advantages • • • Enables visualization and biopsy of esophageal epithelium Determines presence of esophagitis, other complications Discriminates between reflux and non-reflux esophagitis Limitations • • • Endoscopic grading systems not yet validated for pediatrics Poor correlation between endoscopic appearance and histopathology Generally not useful for extraesophageal GERD

Case snippet 2 • 8 month old with non bilious vomiting since 3 months of age. • Vomits both liquids as well as solids • Thought to have GERD • Advised more solids, domperidone and PPI • No response! • USG abdomen: normal • Barium swallow: showed evidence of gastroesophageal reflux disease but no hiatus hernia

Case progress • • Vomiting continued! Mild FTT Serum Ig. A t. TG negative Pediatric Gastroenterological consult
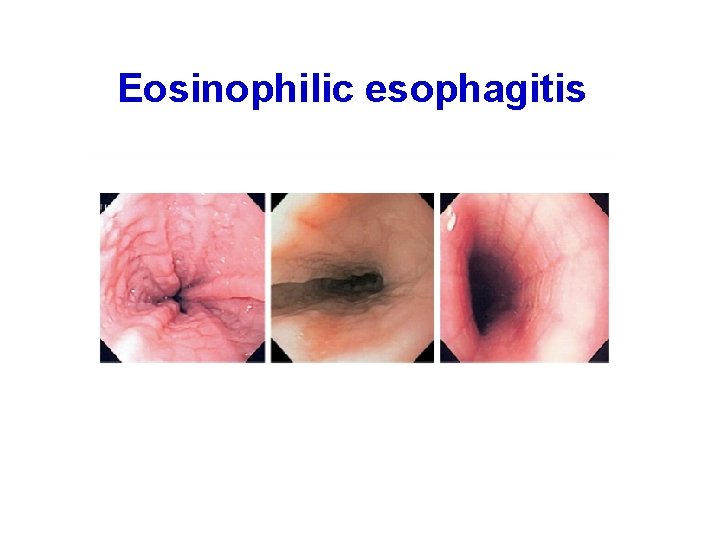
Eosinophilic esophagitis

Management • Eosinophilic esophagitis is a difficult disease to treat - often needing a trained pediatric gastroenterologist and allergy specialist • In small children – complete elimination of M ilk E gg W heat S oy • Older children - steroid sprays to be swallowed
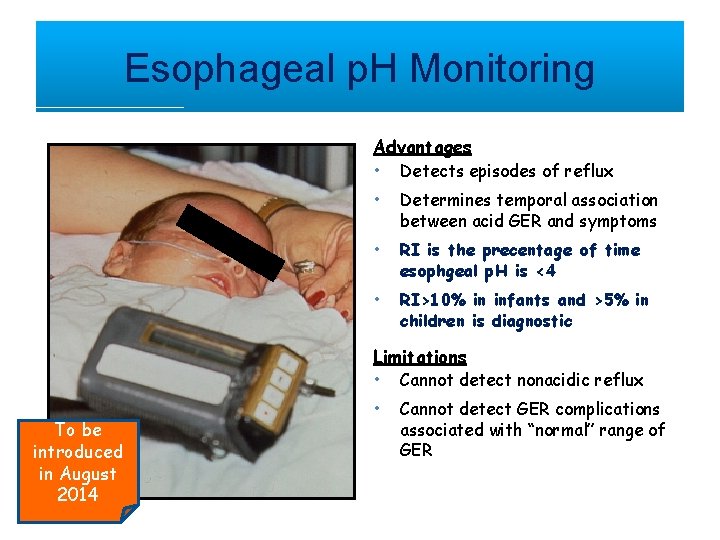
Esophageal p. H Monitoring Advantages • Detects episodes of reflux • Determines temporal association between acid GER and symptoms • RI is the precentage of time esophgeal p. H is <4 • RI>10% in infants and >5% in children is diagnostic Limitations • Cannot detect nonacidic reflux To be introduced in August 2014 • Cannot detect GER complications associated with “normal” range of GER
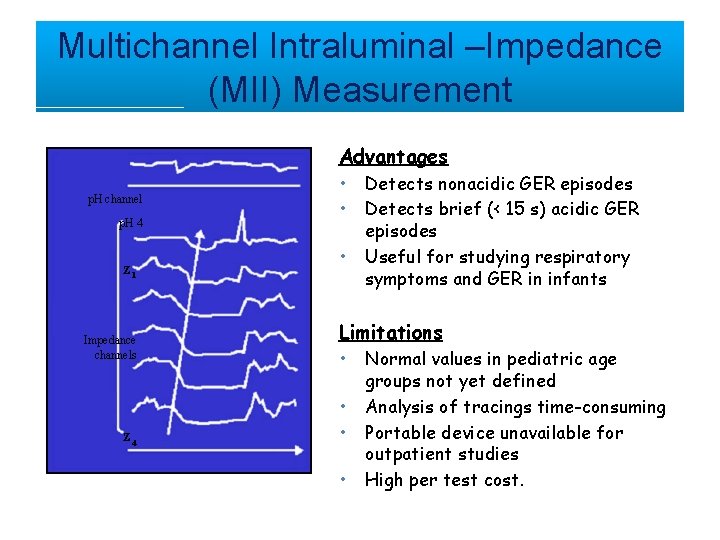
Multichannel Intraluminal –Impedance (MII) Measurement Advantages p. H channel p. H 4 Z 1 Impedance channels Z 4 • • • Detects nonacidic GER episodes Detects brief (< 15 s) acidic GER episodes Useful for studying respiratory symptoms and GER in infants Limitations • • Normal values in pediatric age groups not yet defined Analysis of tracings time-consuming Portable device unavailable for outpatient studies High per test cost.

Management- Life style Changes For Infants • Normalize feeding volume and frequency • Consider thickened formula • Consider non-prone positioning during sleep • Consider trial of hypoallergenic formula For Older Children • Avoid large meals • Do not lie down immediately after eating • Lose weight, if obese • Avoid caffeine, chocolate, and spicy foods that provoke symptoms • Eliminate exposure to tobacco smoke
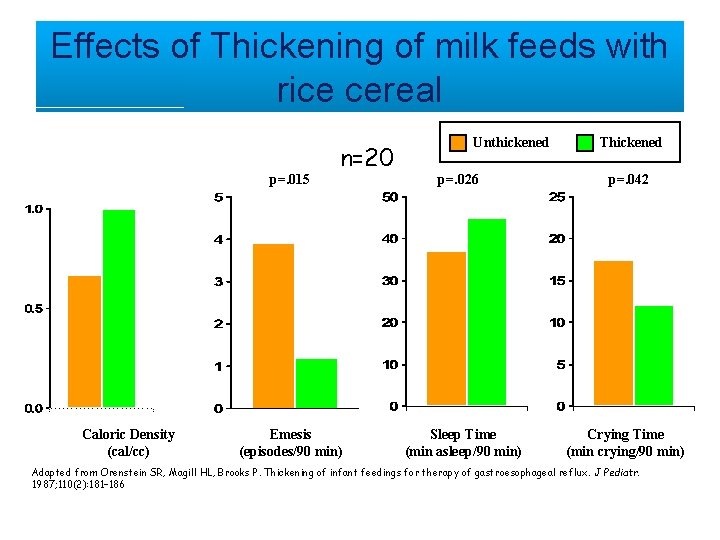
Effects of Thickening of milk feeds with rice cereal p=. 015 Caloric Density (cal/cc) n=20 Emesis (episodes/90 min) Unthickened p=. 026 Sleep Time (min asleep/90 min) Thickened p=. 042 Crying Time (min crying/90 min) Adapted from Orenstein SR, Magill HL, Brooks P. Thickening of infant feedings for therapy of gastroesophageal reflux. J Pediatr. 1987; 110(2): 181– 186
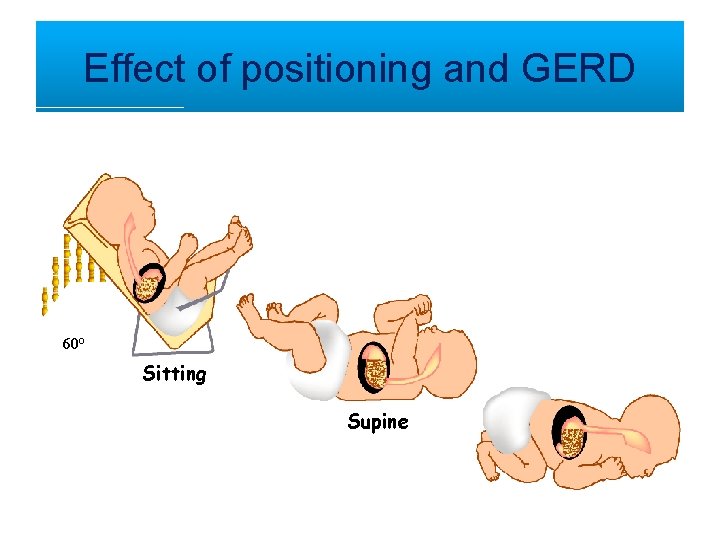
Effect of positioning and GERD 60° Sitting Supine

Case snippet 3 • 1. 5 yr old toddler brought by mum for complaints of non bilious vomiting last 2 -3 months • Vomiting usually occurs during and soon after feeds • What is your diagnosis?

Is this GERD or forced feeding? • GERD symptoms usually peak around 3 - 6 months of age or even earlier. More with liquids > solids Vomiting - more of a passive regurgitation Irritability - suggests esophagitis/ CMPA Extraesophageal symptoms - nocturnal cough, Sandifer syndrome - more common in devp delay • Picky eating starts after 1 yr of age. Food refusal. Picky eaters. Sensory oral aversions. Delve deeper into the history - meal times are warzone between mum and kid • But sometimes they co exist!

Treatment of GERD in Older Children • A left sided sleeping position with elevation of the head of the bed may decrease symptoms and GER • In adults, obesity and late night eating are associated with increased reflux – To date, no evidence to support specific dietary restrictions to decrease symptoms of GER in pediatric populations • Appropriate to trial acid suppression

Pharmacological Therapy • Children with GERD need potent acid suppression therapy for at least 12 weeks. • Antacids can be used for symptomatic relief for a brief period but prolonged therapy is contraindicated in children due to side effects • Aluminum toxicity (osteopenia, rickets, microcytic anemia, and neurotoxicity) in aluminum containing antacids and sucralfate • Risk of milk alkali syndrome (hypercalcemia, alkalosis, and renal failure with calcium containing antacids.

Histamine-2 Receptor Antagonists in Pediatric with GERD (H 2 -RAs) • Ranitidine, and Famotidine are safe and effective. Ranitidine comes in 75 mg/5 ml syrup, dose 410 mg/kg/day, divided BID-TID. Famotidine - dose 1 -1. 2 mg/kg/day, divided BID -TID

Histamine-2 Receptor Antagonists in Pediatric with GERD (H 2 -RAs) �Oral dose for peptic ulcer: 2 mg/kg to 4 mg/kg, twice daily to a maximum of 300 mg per day. ; �Maintenance of Healing of Duodenal and Gastric Ulcers: 2 -4 mg/kg once daily to a maximum of 150 mg. day. �Treatment of GERD and Erosive Esophagitis : 510 mg/kg/day usually given as 2 divided doses.

Proton Pump Inhibitors • They are also called Na-K-ATPase inhibitors as they inhibit acid secretion • PPIs should be taken 30 minutes before breakfast • Once daily dosing is adequate and children – 2 -2. 5 mg/ kg/day for omeprazole and – 1. 4 mg/kg/day for lansoprazole • The advantages of PPIs are – more effective in relieving symptoms and healing esophagitis – prolonged action (requires once daily dose), – no tachyphylaxis on prolonged use, and – relatively safe drug on long term use.

Duration of Medical Therapy • GERD needs profound acid suppression for a longer duration of time. • Drug therapy is recommended for at least 12 weeks and then to taper over 2 to 3 months as rebound hyperacidity is known after sudden stoppage of drugs • In a diagnosed case of GERD, if there is no symptomatic improvement in 4 weeks then the dose of drugs needs to be increased. • In erosive esophagitis, repeat endoscopy to document healing is indicated at the end of 12 weeks course • In a long term follow-up study in children, it has been shown that prolonged drugs therapy (median 3 years and up to 12 years) is safe

Bronchial asthma and GERD • The clinical association of bronchial asthma and GERD is very strong but causal relationship has not yet been established. • It is not yet clear” Is it asthma that causes GERD or is it GERD that causes asthma? ” • Persistent asthma with symptomatic GERD: can be treated with PPI with a clear explanation given to the patient that symptoms might improve • Intermittent asthma : there is no clinical relation with GERD • Difficult to control asthma : (chronic symptoms, continued requirement of steriods) : may derive some benefit from medical therapy. However It is recommended to perform p. H study before considering a trial of long-term PPI therapy

GERD in neurologically impaired children • Prevalence of GERD in neurologically impaired children is much higher and the prevalence is almost 50%. • Severity and complications of GERD is also much more in this subset of patients. • It has been shown that the prevalence of erosive esophagitis is 30% to 70% compared to just 5% in normal children. • This group of children needs prolonged medication and more often surgery

Conclusions • GER is common in infants but GERD is not so common in early childhood. • Most infants have physiological reflux and resolve by 18 months of age. • There is no gold standard diagnostic test. • Empirical H 2 RA/ PPI therapy for 4 weeks is justified in older children and adolescents with classical symptoms. • Medical therapy with H 2 RA/ PPI is very effective and safe and should be continued for long duration • Surgical therapy carries significant morbidity and often fails in those who need it most

THANK YOU
- Slides: 42