Gastroenterology Grand Rounds February 20 2014 Fellow David

Gastroenterology Grand Rounds February 20, 2014 Fellow: David Tang, M. D. Faculty: Marcelo Vela, M. D.

Case Presentation • 36 year old White man • Heartburn x 10 years • Intermittent dysphagia and chest pressure x 2 years • EGD in 2011 – Long segment Barrett’s Esophagus, Prague C 10 M 10, without dysplasia – Eosinophilic esophagitis • Symptoms resolved with twice daily Nexium
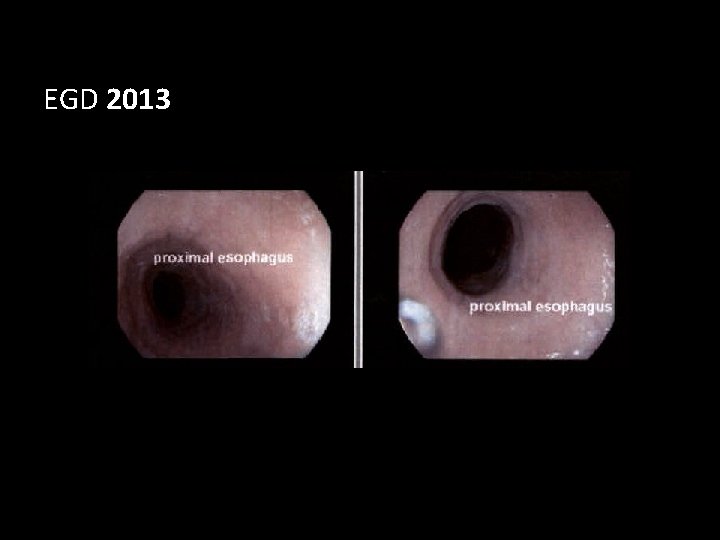
EGD 2013
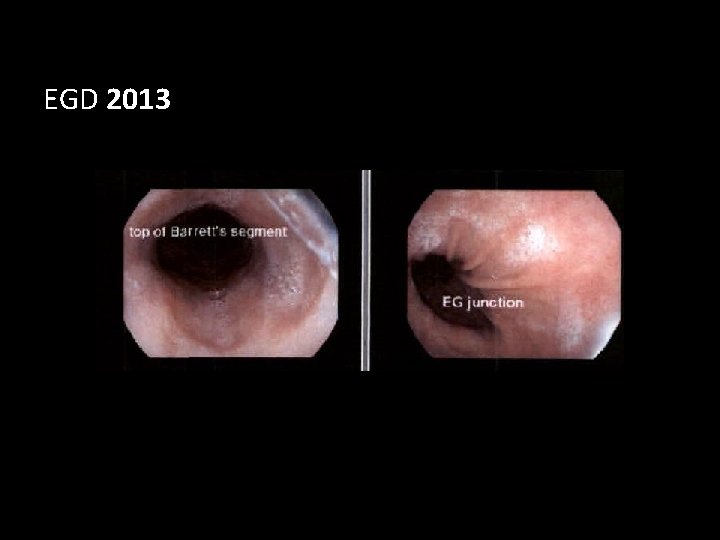
EGD 2013

Case Presentation • Histology – Esophagus at 34 cm to 28 cm Intestinal metaplasia with low grade dysplasia at multiple levels – Esophagus at 25 cm Squamous mucosa with > 40 intraepithelial eosinophils per high power field

Diagnosis Eosinophilic Esophagitis And Barrett’s Esophagus with Low Grade Dysplasia

Clinical Questions • What is the difference in recommendations for RFA in patients with LGD vs HGD? • What is the efficacy and durability of RFA for Barrett’s Esophagus with LGD? • Should RFA be performed for Barrett’s Esophagus with LGD? • What is the relationship between Barrett’s Esophagus and Eosinophilic Esophagitis? • How safe is RFA of dysplastic Barrett’s in Eosinophilic Esophagitis?
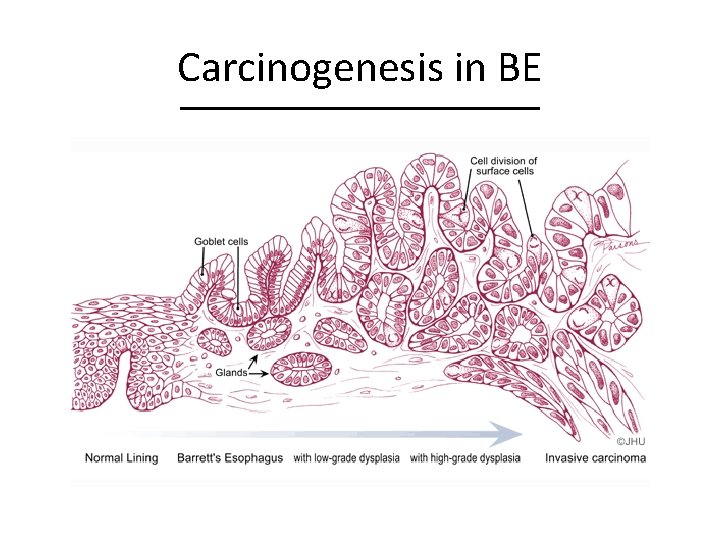
Carcinogenesis in BE

Incidence of EAC in BE • Non dysplastic BE EAC – 0. 12% - 0. 50% per year • LGD EAC – 1. 7% per year • HGD EAC – 6. 6% per year Sikkema Am J Gastroenterol 2011 Hvid-jensen NEJM 2011 Wani Am J Gastroenterol 2009

Inter-observer Variability in LGD • 147 patients with a community diagnosis of LGD during BE surveillance – 15% with LGD confirmation by two other expert pathologists – 85 % down-staged to non dysplastic BE • Incidence rate of progression to HGD/EAC – 13. 4% in patients with confirmed LGD – 0. 49% in patients down-staged to NDBE Curvers Am J Gastroenterol 2010

2011 AGA Guidelines • “We recommend endoscopic eradication therapy with radiofrequency ablation (RFA) … rather than surveillance for treatment of patients with confirmed high-grade dysplasia”

2011 AGA Guidelines • “Endoscopic eradication therapy with RFA should also be a therapeutic option for treatment of patients with confirmed low-grade dysplasia in Barrett’s esophagus. ” • “In the absence of long-term studies showing efficacy, it is not clear that the potential benefit of ablation in reducing cancer risk for patients who have Barrett’s esophagus with low-grade dysplasia warrants the risks and substantial expense of the ablative procedures. ”

AIM Dysplasia Trial • Multicenter RCT of RFA vs Sham procedure in dysplastic Barrett’s Esophagus • N = 127 – randomized in 2: 1 ratio • Primary outcomes – Complete eradication of LGD @ 12 mos – Complete eradication of HGD @ 12 mos – Complete eradication of IM @ 12 mos Shaheen NEJM 2009
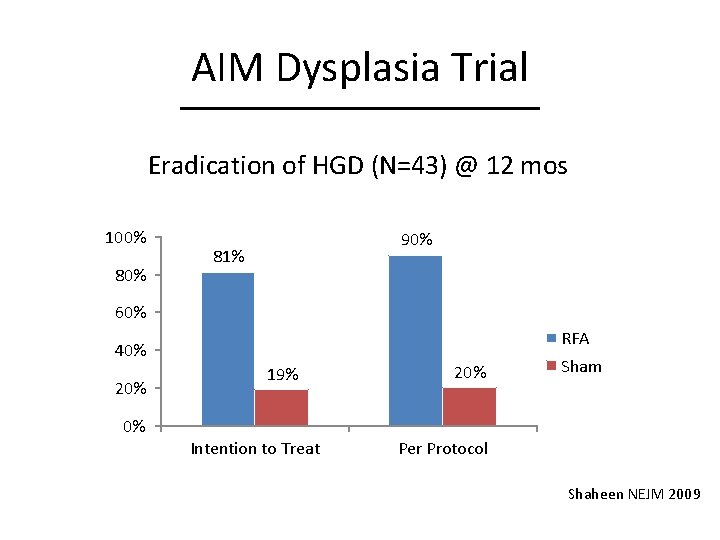
AIM Dysplasia Trial Eradication of HGD (N=43) @ 12 mos 100% 80% 90% 81% 60% RFA 40% 20% 0% 19% Intention to Treat 20% Sham Per Protocol Shaheen NEJM 2009
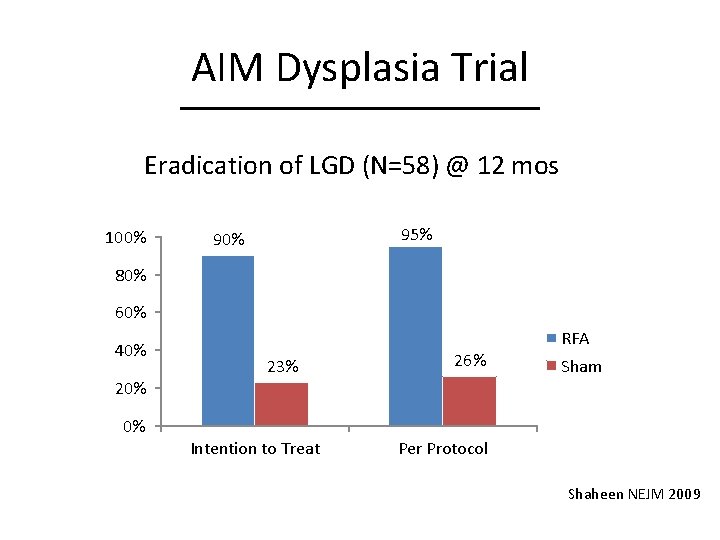
AIM Dysplasia Trial Eradication of LGD (N=58) @ 12 mos 100% 95% 90% 80% 60% 40% RFA 23% 26% Sham 20% 0% Intention to Treat Per Protocol Shaheen NEJM 2009
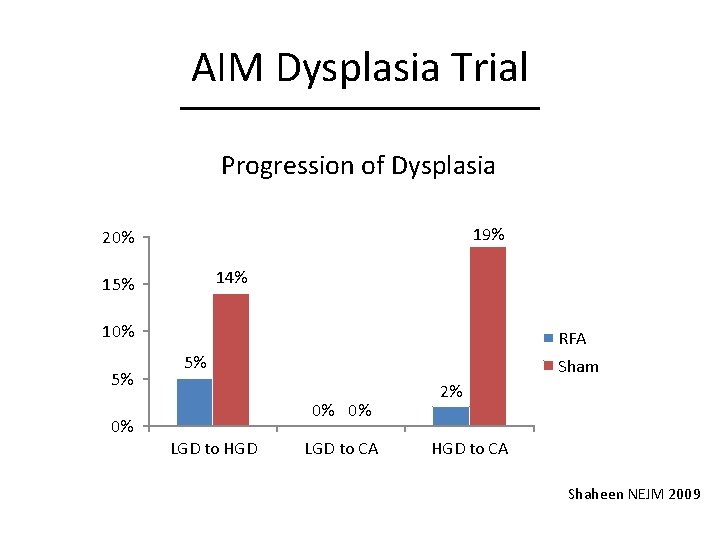
AIM Dysplasia Trial Progression of Dysplasia 19% 20% 14% 15% 10% 5% 0% RFA 5% Sham 0% 0% LGD to HGD LGD to CA 2% HGD to CA Shaheen NEJM 2009
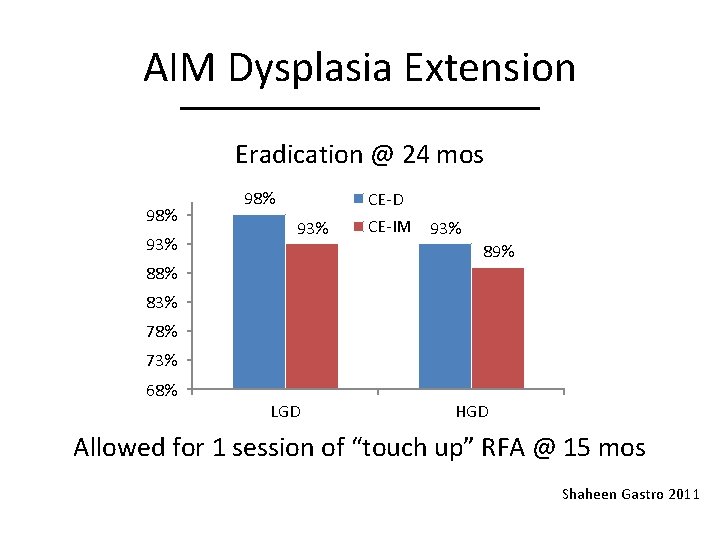
AIM Dysplasia Extension Eradication @ 24 mos 98% 93% 98% CE-D 93% CE-IM 93% 89% 88% 83% 78% 73% 68% LGD HGD Allowed for 1 session of “touch up” RFA @ 15 mos Shaheen Gastro 2011
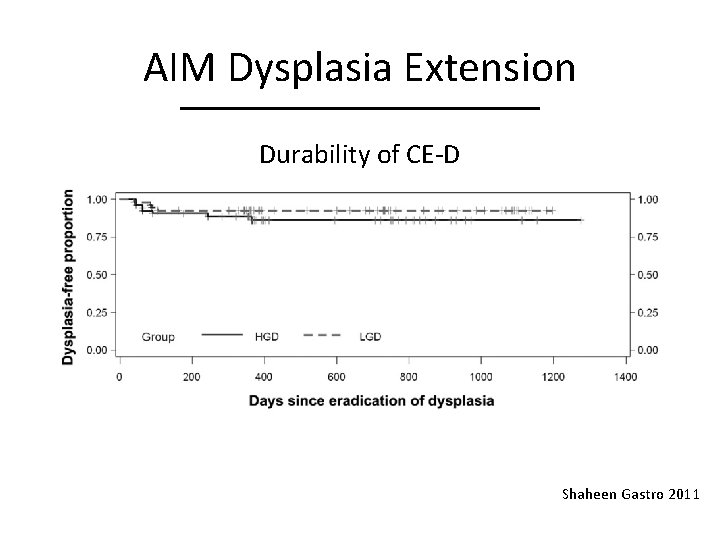
AIM Dysplasia Extension Durability of CE-D Shaheen Gastro 2011
![AIM Dysplasia Extension Incidence of Progression to EAC [per year] 6. 6% Post RFA AIM Dysplasia Extension Incidence of Progression to EAC [per year] 6. 6% Post RFA](http://slidetodoc.com/presentation_image/b1ca177d1bf283d2fdfaad44c2122fb9/image-19.jpg)
AIM Dysplasia Extension Incidence of Progression to EAC [per year] 6. 6% Post RFA Natural History 1. 7% 0. 51% LGD 0. 60% HGD Shaheen Gastro 2011 Wani Am J Gastroenterol 2009
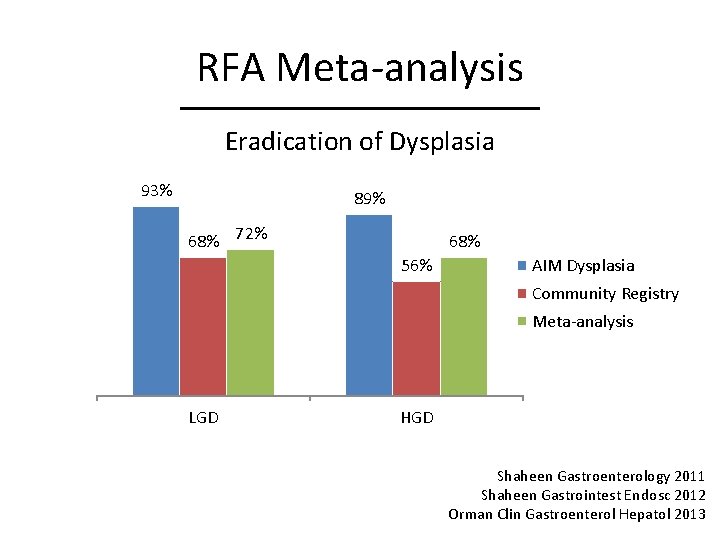
RFA Meta-analysis Eradication of Dysplasia 93% 89% 68% 72% 68% 56% AIM Dysplasia Community Registry Meta-analysis LGD HGD Shaheen Gastroenterology 2011 Shaheen Gastrointest Endosc 2012 Orman Clin Gastroenterol Hepatol 2013
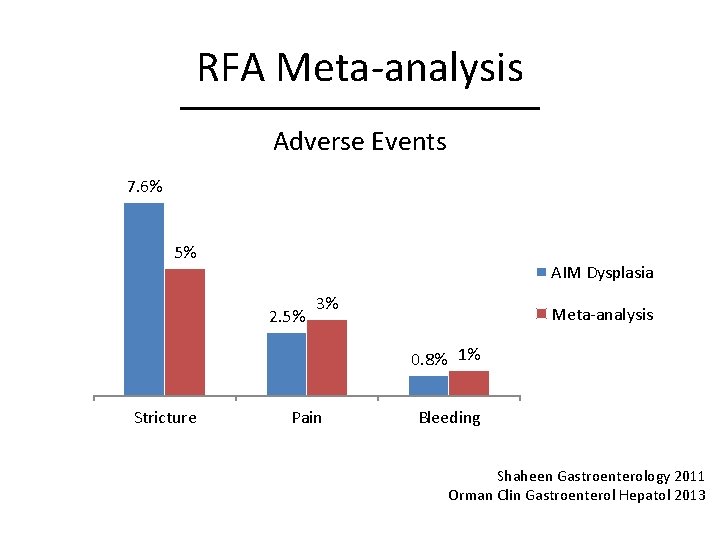
RFA Meta-analysis Adverse Events 7. 6% 5% AIM Dysplasia 2. 5% 3% Meta-analysis 0. 8% 1% Stricture Pain Bleeding Shaheen Gastroenterology 2011 Orman Clin Gastroenterol Hepatol 2013
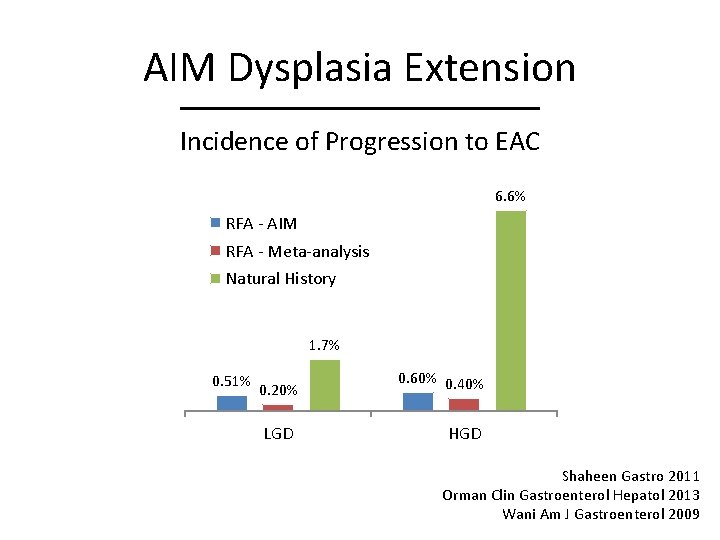
AIM Dysplasia Extension Incidence of Progression to EAC 6. 6% RFA - AIM RFA - Meta-analysis Natural History 1. 7% 0. 51% 0. 20% LGD 0. 60% 0. 40% HGD Shaheen Gastro 2011 Orman Clin Gastroenterol Hepatol 2013 Wani Am J Gastroenterol 2009

SURF Trial • European multicenter RCT of RFA vs Surveillance in LGD • N = 136 randomized in 1: 1 • Primary outcome – Neoplastic progression (HGD or EAC) at 3 years after randomization • Interim results at median 21 mos follow up presented at DDW 2013 Phoa Gastroenterology 2013
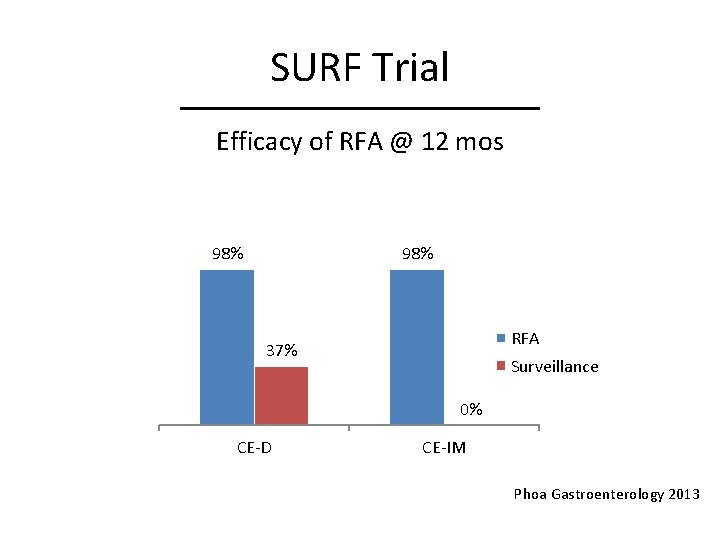
SURF Trial Efficacy of RFA @ 12 mos 98% RFA 37% Surveillance 0% CE-D CE-IM Phoa Gastroenterology 2013
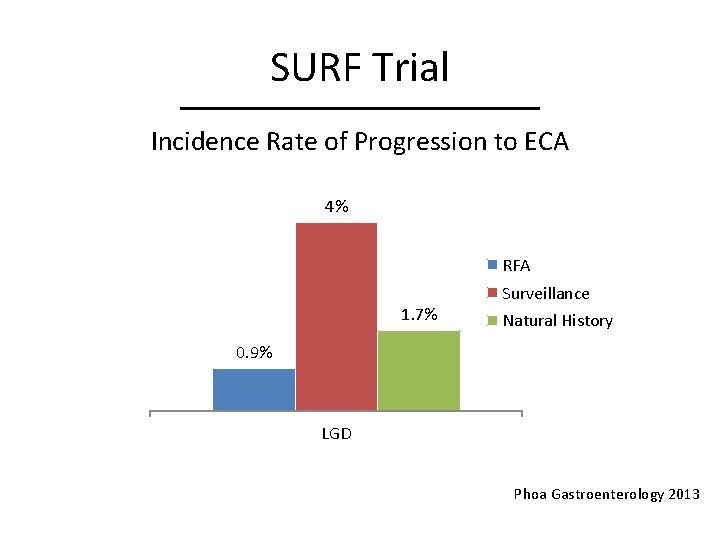
SURF Trial Incidence Rate of Progression to ECA 4% RFA 1. 7% Surveillance Natural History 0. 9% LGD Phoa Gastroenterology 2013

Cost Effectiveness of RFA • Computer model RFA and surveillance strategies of 50 year old “patients” followed until age 80 or death. • Possible causes of death – Age related all cause mortality – RFA complications – Surgical esophagectomy mortality – Esophageal adenocarcinoma Hur Gastroenterology 2012

Cost Effectiveness of RFA • LGD cohort – Confirmed assume no initial diagnostic error – Stable LGD found on more than one EGD at least 6 months apart • Management – Endoscopic surveillance q 6 months x 1 year, then yearly – RFA at 0, 2, 4, 9 mos, then “touch up” RFA as needed Hur Gastroenterology 2012

Cost Effectiveness of RFA • RFA Outcomes – Residual dysplasia – CE-D – CE-IM – Recurrence of IM – Sub squamous intestinal metaplasia • Incremental cost effective ratio (ICER) • Willingness to pay (WTP) set at $100, 000/QALY Hur Gastroenterology 2012
Cost Effectiveness of RFA RFA Surgery Hur Gastroenterology 2012
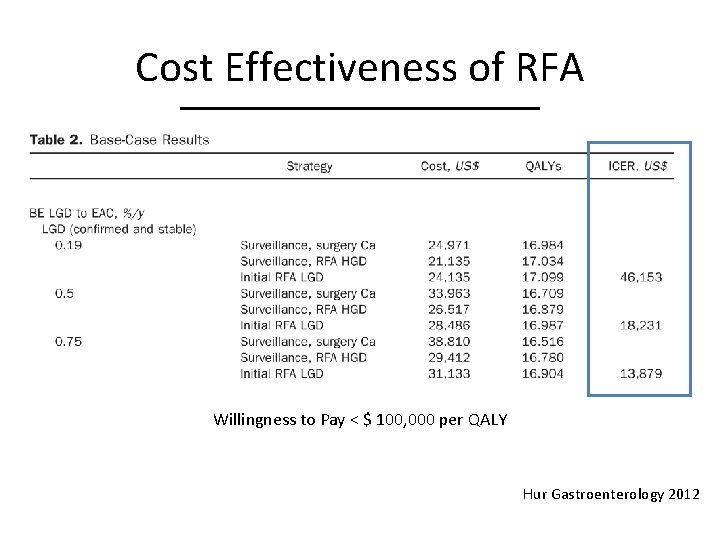

Cost Effectiveness of RFA Willingness to Pay < $ 100, 000 per QALY Hur Gastroenterology 2012

Barrett’s Esophagus and Eo. E • Cross sectional study of 200 patients with BE • 14 of 200 patients with BE (7%) found to have > 15 eosinophils/hpf on squamous biopsy Ravi Am J Gastroenterol 2011

Post RFA Esophageal Eosinophilia • Retrospective review of 148 patients with pre and post RFA esophageal biopsies • 4 of 148 patients (2. 7%) developed esophageal eosinophilia at 12 months – All four had LGD – None had clinical or endoscopic findings suggestive of Eo. E – No pre RFA biopsies of squamous epithelium – Adverse events not reported Villa Dis Esophagus 2013

Safety of Esophageal Dilation in Eo. E • Retrospective single center study • N = 293 dilations in 161 patients – 9. 2% mucosal tear – 0. 3% major bleeding – 1% immediate perforation • All treated without surgery • Prior study of 36 patients with complication rate of 31% and perforation rate of 8% Jung GIE 2011 Cohen Clin Gastroenterol Hepatol 2007

Thank you Dr. Marcelo Vela Dr. Nicolas Villa

References Prasad G, Talley N, Romero Y, et al. Prevalence and predictive factors of eosinophilic esophagitis in patients presenting with dysphagia: a prospective study. The American journal of gastroenterology 2007; 102: 2627 -2632. Wolfsen H, Hemminger L, Achem S. Eosinophilic esophagitis and Barrett's esophagus with dysplasia. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association 2007; 5. Rodrigo S, Abboud G, Oh D, et al. High intraepithelial eosinophil counts in esophageal squamous epithelium are not specific for eosinophilic esophagitis in adults. The American journal of gastroenterology 2008; 103: 435 -442. Shaheen N, Sharma P, Overholt B, et al. Radiofrequency ablation in Barrett's esophagus with dysplasia. The New England journal of medicine 2009; 360: 2277 -2288. Wani S, Puli S, Shaheen N, et al. Esophageal adenocarcinoma in Barrett's esophagus after endoscopic ablative therapy: a meta-analysis and systematic review. The American journal of gastroenterology 2009; 104: 502 -513. Jacobs J, Spechler S. A systematic review of the risk of perforation during esophageal dilation for patients with eosinophilic esophagitis. Digestive diseases and sciences 2010; 55: 1512 -1515. American Gastroenterological A, Spechler S, Sharma P, et al. American Gastroenterological Association medical position statement on the management of Barrett's esophagus. Gastroenterology 2011; 140: 1084 -1091. Hvid-Jensen F, Pedersen L, Drewes A, et al. Incidence of adenocarcinoma among patients with Barrett's esophagus. The New England journal of medicine 2011; 365: 1375 -1383. Ravi K, Katzka D, Smyrk T, et al. Prevalence of esophageal eosinophils in patients with Barrett's esophagus. The American journal of gastroenterology 2011; 106: 851 -857.

References Shaheen N, Overholt B, Sampliner R, et al. Durability of radiofrequency ablation in Barrett's esophagus with dysplasia. Gastroenterology 2011; 141: 460 -468. Spechler S, Sharma P, Souza R, et al. American Gastroenterological Association technical review on the management of Barrett's esophagus. Gastroenterology 2011; 140. Hur C, Choi S, Rubenstein J, et al. The cost effectiveness of radiofrequency ablation for Barrett's esophagus. Gastroenterology 2012; 143: 567 -575. Dellon E, Gonsalves N, Hirano I, et al. ACG clinical guideline: Evidenced based approach to the diagnosis and management of esophageal eosinophilia and eosinophilic esophagitis (Eo. E). The American journal of gastroenterology 2013; 108: 679. Orman E, Li N, Shaheen N. Efficacy and durability of radiofrequency ablation for Barrett's Esophagus: systematic review and meta-analysis. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association 2013; 11: 1245 -1255. Villa N, El-Serag H, Younes M, et al. Esophageal eosinophilia after radiofrequency ablation for Barrett's esophagus. Diseases of the esophagus : official journal of the International Society for Diseases of the Esophagus / I. S. D. E 2013; 26: 674 -677. Falk G. Update on ablation for Barrett's esophagus. Current gastroenterology reports 2014; 16: 368. Fitzgerald R, di Pietro M, Ragunath K, et al. British Society of Gastroenterology guidelines on the diagnosis and management of Barrett's oesophagus. Gut 2014; 63: 7 -42.
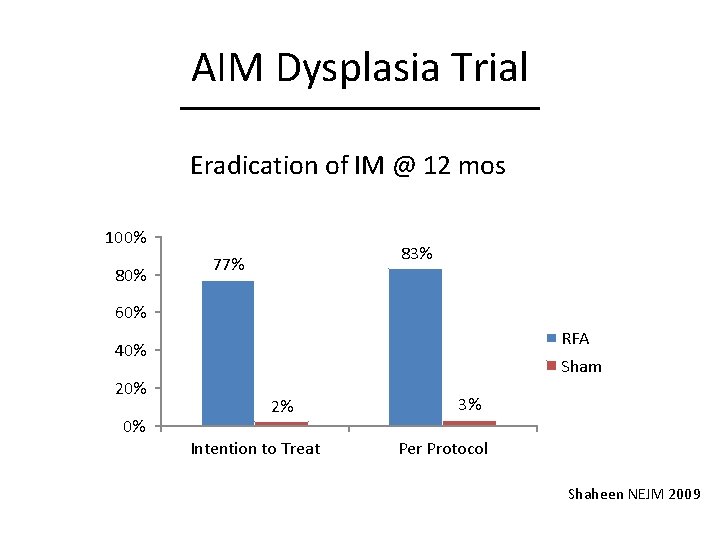
AIM Dysplasia Trial Eradication of IM @ 12 mos 100% 83% 77% 60% RFA 40% 20% 0% Sham 2% Intention to Treat 3% Per Protocol Shaheen NEJM 2009

AIM Dysplasia Extension • 2 year extension of AIM Dysplasia • Original control arm offered cross over to RFA • N = 119 – 106 patients completed 2 nd year of follow up • 100 eligible for extension through year 5 – 56 completed 3 rd year of follow up at time of publication • Durability of eradication of both dysplasia and metaplasia assessed at 2 nd and 3 rd year Shaheen Gastro 2011
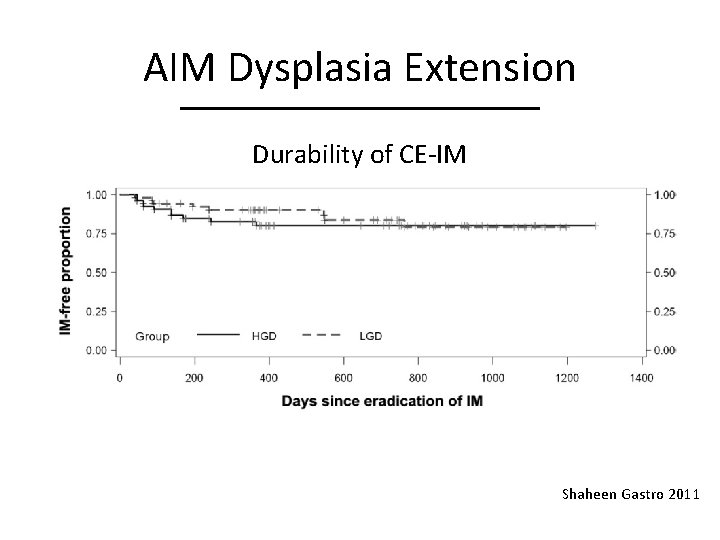
AIM Dysplasia Extension Durability of CE-IM Shaheen Gastro 2011

AIM Dysplasia Extension Progression of Dysplasia • 5 of 119 (4. 3%) with progression of any type • 3 LGD HGD – 2 with eventual CE-IM – 1 with EMR of focal HGD and withdrew from study • 1 LGD to EAC – Initially randomized to Sham arm x 12 mos – RFA x 3 after crossing over – Eventual EMR of focal EAC • 1 HGD to EAC – EMR of focal EAC – Eventual CE-IM at 3 years Shaheen Gastro 2011

RFA Meta-analysis • Efficacy of RFA – 3802 patients • 2135 patients in RFA registry from 148 community and academic practices • Durability of RFA – 540 patients Orman Clin Gastroenterol Hepatol 2013
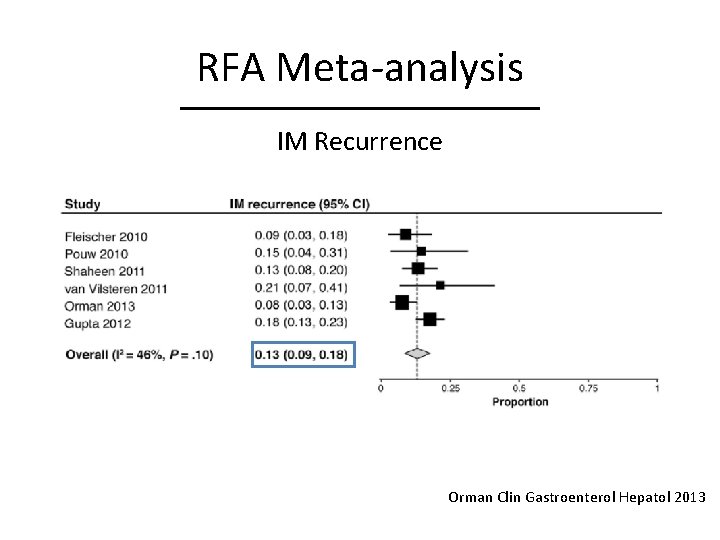
RFA Meta-analysis IM Recurrence Orman Clin Gastroenterol Hepatol 2013

Cost Effectiveness of RFA • Assumptions – NDBE EAC 0. 12%, 0. 33%, 0. 50% – LGD EAC 0. 19%, 0. 5%, 0. 75% Hur Gastroenterology 2012

Eosinophilic Esophagitis • Symptoms – Dysphagia, Food impaction – Reflux – Dyspepsia • Associated with atopy • Requires > 15 eos per HPF on biopsy
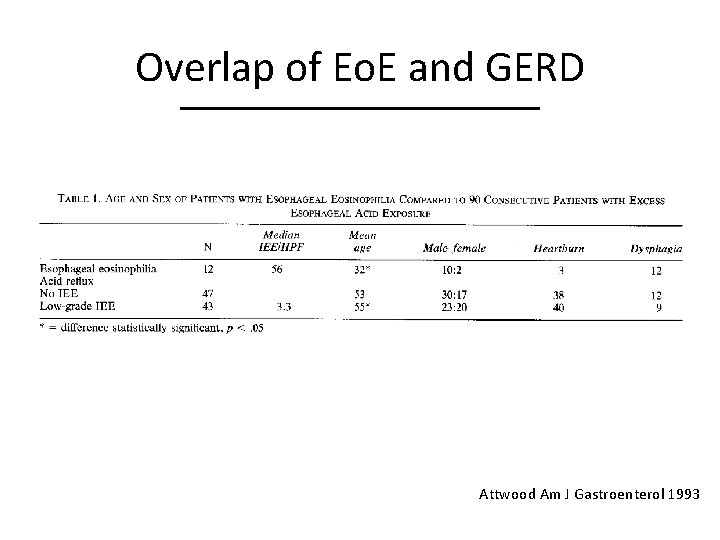
Overlap of Eo. E and GERD Attwood Am J Gastroenterol 1993
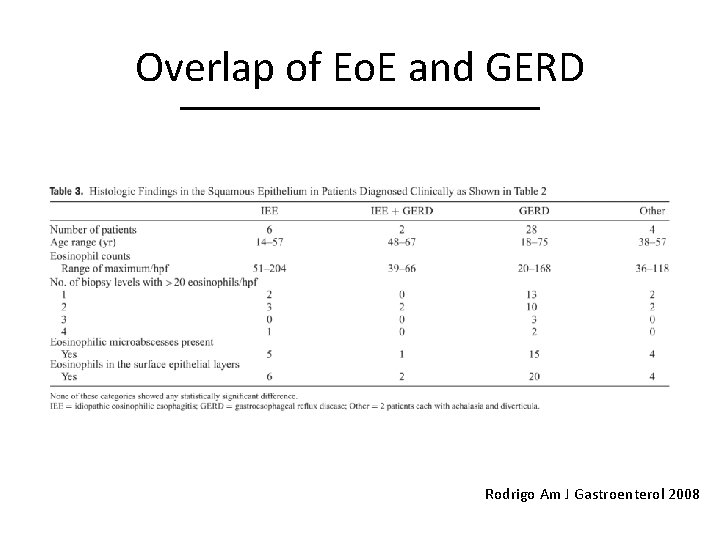
Overlap of Eo. E and GERD Rodrigo Am J Gastroenterol 2008
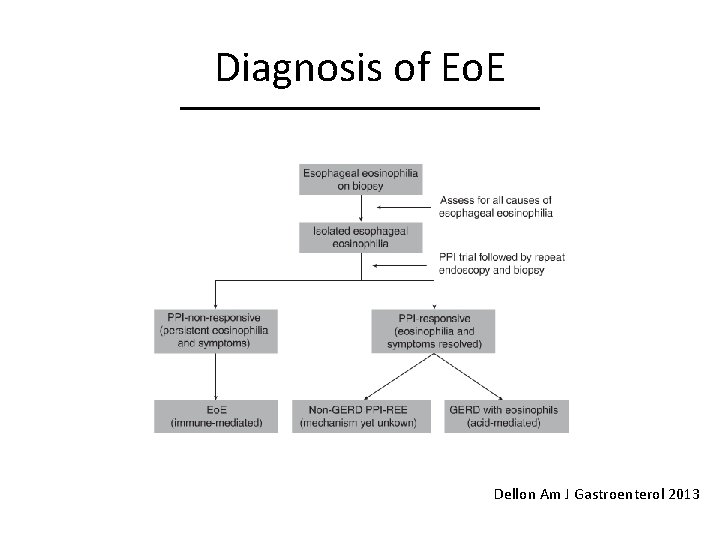
Diagnosis of Eo. E Dellon Am J Gastroenterol 2013
- Slides: 47