Gamma Ray and Beta Ray Probes Larry Mac

Gamma Ray and Beta Ray Probes Larry Mac. Donald Imaging Research Laboratory University of Washington Radiology http: //depts. washington. edu/nucmed/IRL/ 23 Oct. 2007 1

Gamma Ray and Beta Ray Probes “Probe” implies hand-held device provides positioning flexibility real-time response Most relevant arena for probes is the operating room OR compatible Expand the probe idea functionality (above points) to larger imaging systems Oct. 2007 2

Properties of Gamma Rays and Beta Rays Gamma Rays massless photons travel potentially long distances in body penetration is exponential: N=N 0 e- (mat. , E)*x typical ~ cm-m penetration, no maximum difficult to collimate mono-energetic (allows energy discrimination) Beta Rays (e- & e+) massive charged particles undergo many interactions in body penetration between exp. &linear typical ~ mm penetration, max. exists easy to collimate continuous distribution of energies up to a maximum (does not allow energy discrimination) Oct. 2007 3

Probe Application Requirements Procedure efficacy depends on measurement system consisting of Labeled compound extracted from blood into tumor/ROI high tumor-to-background remain in tumor for a time consistent with surgery and T 1/2 Radioisotope chemical properties for stable label appropriate half-life (T 1/2) emission compatible with the detector and patient safety Radiation detector efficient to radiation insensitive to background (or discrimination capability) good energy resolution (eliminate background and scatter) adequate collimation spatial resolution Oct. 2007 4

First Applications, Probes, Isotopes 1940’s First application: tumor localization pre- & intra-operative First probe: Geiger-Muller gas filled low sensitivity no energy resolution First isotope used with probe: 32 -P ( -) Emax = 1. 7 Me. V --> ~ 7 -8 mm range in tissue T 1/2=14 d --> dosimetry issues Oct. 2007 5

Available Tracers In principle any Nuc. Med. ( ) / PET ( +) agent + easy to collimate short range --> good localization confounding presence of 511 ke. V annihilation photons difficult to collimate Oct. 2007 6

Contemporary Applications, Probes, Isotopes Clinical Sentinel lymph nodes (SLN) replace complete axillary LN dissection with excision of selective SLN Scintillation and solid-state “pencil” detectors non-imaging small point detectors 99 m-Tc labeled colloids designed to flow through lymph systems - not biologically active Research Sentinel lymph nodes - add imaging capability, expand disease base Brain tumor margins - scint. /solidstate/combo imaging probes - +(PET) Arterial vulnerable plaque - “imaging” catheters - +(PET) Oct. 2007 7

SLN Procedure: Evaluate Spread of Cancer • Applied to melanoma, breast cancer. Other cancers being investigated. • Pathology of first downstream lymph nodes (Sentinel node(s)) is indicative of disease spread. • Removal of only Sentinel node(s) avoids complications of complete node basin dissection. • 99 m-Tc labeled colloid injected near primary tumor – drains through lymphatics. NO BACKGROUND, except injection site ~ 100 X node act. ---> HIGH CONTRAST at nodes; n. Ci sensitivity • Pre-operative imaging in Nuc. Med. with conventional camera is not universal. • Non-imaging gamma probes are used to find nodes during surgery. Oct. 2007 8

SLN Detection Technical Issues and Protocol Variations Probe - all quite similar Tracer - colloid particle size Injection site - subdermal / peritumorial / intratumorial / subcutaneous Number of injections Injection volume and activity Massage injection site? Injection - detection timing Detection mode: blue dye / gamma probe / preoperative imaging Dynamic imaging / early+late imaging Number of nodes to remove Pathology Requirements - H&E staining / IHC /Cytology Oct. 2007 9

SLN Theoretical Basis • Patients present with earlier stage of disease • Lymph flow is orderly and predictable • Tumor cells disseminate sequentially • The “sentinel” node is the first node encountered by tumor cells • Sentinel node status predicts distant basin status • Basin involvement is less frequent Oct. 2007 10
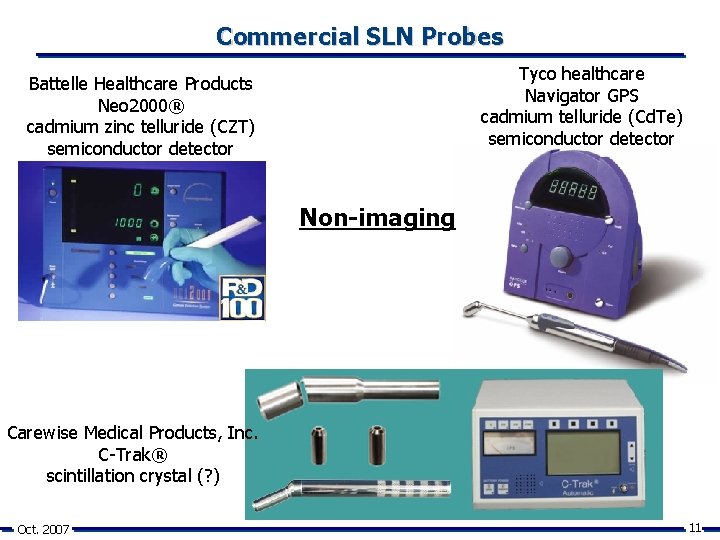
Commercial SLN Probes Tyco healthcare Navigator GPS cadmium telluride (Cd. Te) semiconductor detector Battelle Healthcare Products Neo 2000® cadmium zinc telluride (CZT) semiconductor detector Non-imaging Carewise Medical Products, Inc. C-Trak® scintillation crystal (? ) Oct. 2007 11

Important Operating Properties of Probes Sensitivity (counts/sec. /inj. activity) detector material detector size (depth) radiation type ( ) and energy Spatial resolution (resolving small nearby nodes) detector size (width / diameter) collimator opening Energy resolution (reject scatter) detector type (scintillation / semiconductor) detector material Oct. 2007 12
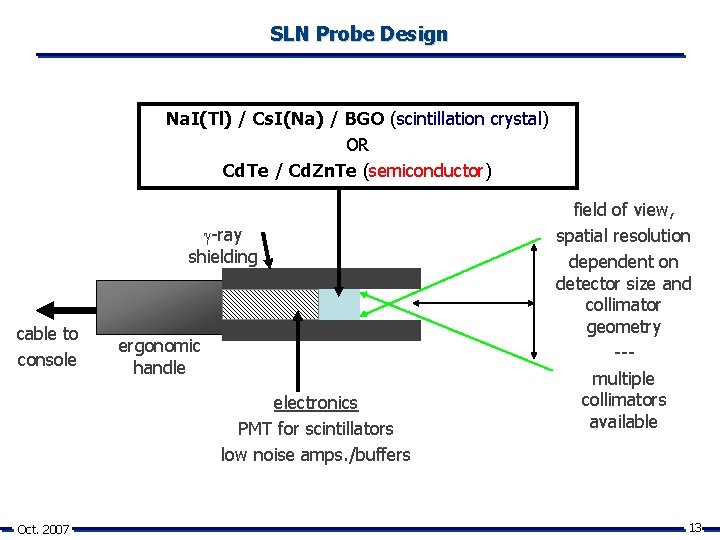
SLN Probe Design Na. I(Tl) / Cs. I(Na) / BGO (scintillation crystal) OR Cd. Te / Cd. Zn. Te (semiconductor) -ray shielding cable to console ergonomic handle electronics PMT for scintillators low noise amps. /buffers Oct. 2007 field of view, spatial resolution dependent on detector size and collimator geometry --multiple collimators available 13
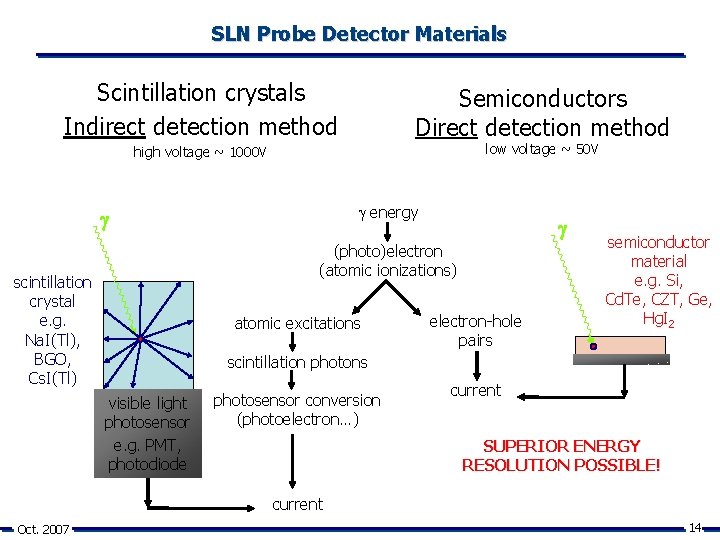
SLN Probe Detector Materials Scintillation crystals Indirect detection method Semiconductors Direct detection method low voltage ~ 50 V high voltage ~ 1000 V energy (photo)electron (atomic ionizations) scintillation crystal e. g. Na. I(Tl), BGO, Cs. I(Tl) atomic excitations electron-hole pairs semiconductor material e. g. Si, Cd. Te, CZT, Ge, Hg. I 2 scintillation photons visible light photosensor e. g. PMT, photodiode photosensor conversion (photoelectron…) current SUPERIOR ENERGY RESOLUTION POSSIBLE! current Oct. 2007 14

SLN Probe Uses Current common clinical applications Melanoma Breast cancer Active research application areas (oncology) Colon Head and neck Cervical / Reproductive Lung Oct. 2007 15

Intra-Operative Imaging of Sentinel Lymph Nodes Oct. 2007 16

Introduce a compact high-resolution gamma camera into the operating room Goals: • Reduce time of surgical procedures/node search. • Increase confidence that all implicated nodes are removed. • Identify nodes near injection site. • Find additional hot nodes hidden by attenuation. Advantages: • • • Oct. 2007 Display isotope distribution live-time in O. R. Rapidly assay secondary node basins. Faster learning curve. Reduce surgical incision size & morbidity due to node removal. Quantifiable measure of activity in nodes. 17

Intra-Operative SLN Imaging: Hand-Held Gamma Camera The Hand-Held Camera can be used pre-operatively and intra-operatively • Simultaneous image and audible count rate indicator • 1 mm intrinsic spatial resolution • 2 cm square intrinsic FOV • Multiple collimators dictate a range of imaging parameters. • Smart algorithms identify activity concentrations in low statistics distributions Oct. 2007 18

Intra-Operative SLN Imaging: Luma. GEM™ in the Operating Room Articulating arm Image acq. / processing PC Luma. GEM™ • Protocols vary widely • Degree of pre-OR imaging varies None Passive NM participation Active NM participation • Nuclear medicine in the OR requires logistical coordination between NM & Surgery Monitor on back of gamma cam. (not shown) displays images in View-Thru format. ~ 1 m 2 footprint wheel base Oct. 2007 19
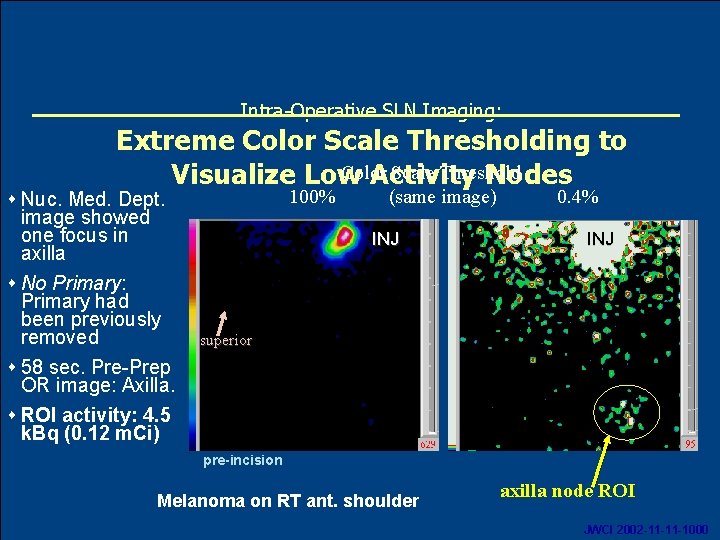
Intra-Operative SLN Imaging: Extreme Color Scale Thresholding to Color Scale Threshold Visualize Low Activity Nodes s Nuc. Med. Dept. image showed one focus in axilla s No Primary: Primary had been previously removed s 58 sec. Pre-Prep OR image: Axilla. s ROI activity: 4. 5 k. Bq (0. 12 m. Ci) 100% (same image) INJ 0. 4% INJ superior pre-incision Melanoma on RT ant. shoulder Oct. 2007 axilla node ROI 20 JWCI 2002 -11 -11 -1000
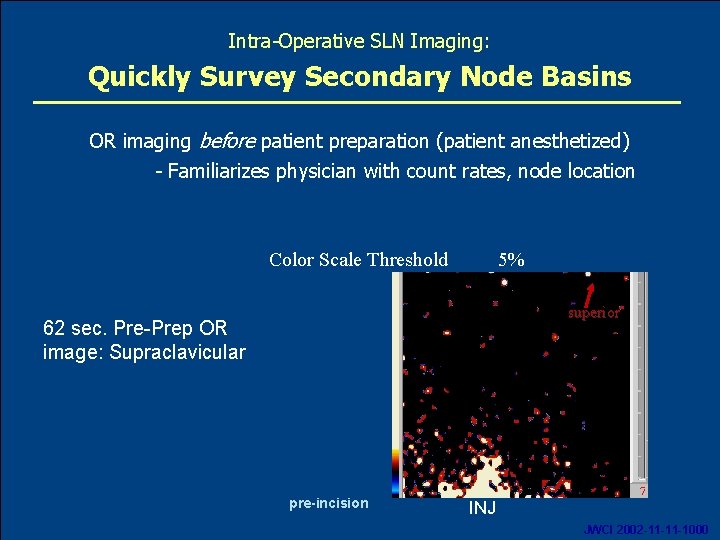
Intra-Operative SLN Imaging: Quickly Survey Secondary Node Basins OR imaging before patient preparation (patient anesthetized) - Familiarizes physician with count rates, node location Color Scale Threshold 5% superior 62 sec. Pre-Prep OR image: Supraclavicular pre-incision Oct. 2007 INJ 21 JWCI 2002 -11 -11 -1000
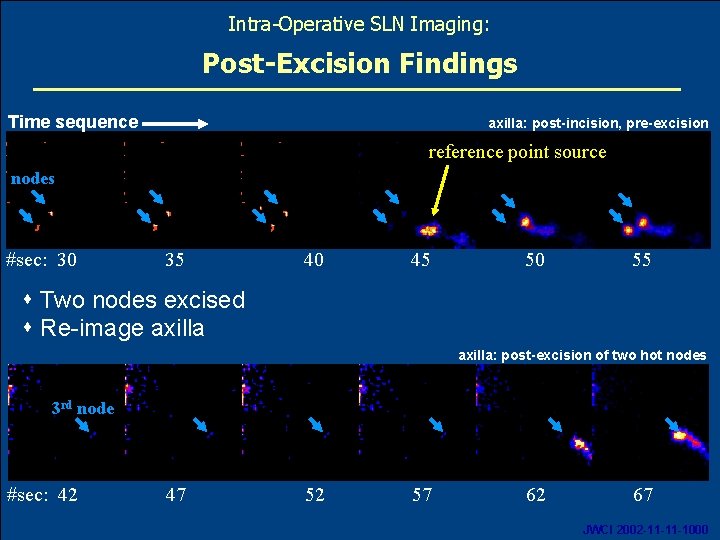
Intra-Operative SLN Imaging: Post-Excision Findings Time sequence axilla: post-incision, pre-excision reference point source nodes #sec: 30 35 40 45 50 55 s Two nodes excised s Re-image axilla: post-excision of two hot nodes 3 rd node #sec: 42 Oct. 2007 47 52 57 62 67 22 JWCI 2002 -11 -11 -1000

Intra-Operative SLN Imaging: Summary Discussion • Locate more hot nodes in less time • Increases confidence • Degree of pre-OR imaging varies None Passive NM participation Active NM participation • Expanding beyond melanoma/breast • Cost/Benefit Ratio Oct. 2007 23

Research Beta Ray Probes Oct. 2007 24
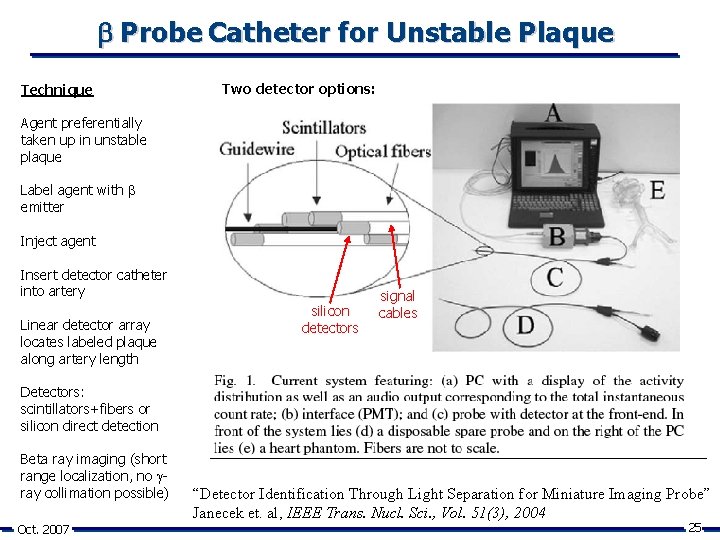
Probe Catheter for Unstable Plaque Technique Two detector options: Agent preferentially taken up in unstable plaque Label agent with emitter Inject agent Insert detector catheter into artery Linear detector array locates labeled plaque along artery length silicon detectors signal cables Detectors: scintillators+fibers or silicon direct detection Beta ray imaging (short range localization, no ray collimation possible) Oct. 2007 “Detector Identification Through Light Separation for Miniature Imaging Probe” Janecek et. al, IEEE Trans. Nucl. Sci. , Vol. 51(3), 2004 25
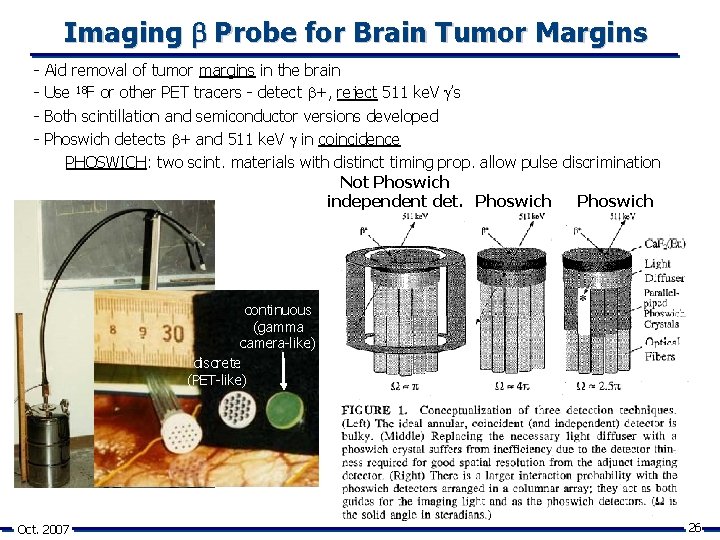
Imaging Probe for Brain Tumor Margins - Aid removal of tumor margins in the brain Use 18 F or other PET tracers - detect +, reject 511 ke. V ’s Both scintillation and semiconductor versions developed Phoswich detects + and 511 ke. V in coincidence PHOSWICH: two scint. materials with distinct timing prop. allow pulse discrimination Not Phoswich independent det. Phoswich continuous (gamma camera-like) discrete (PET-like) Oct. 2007 26
- Slides: 26