Gallbladder and pancreas Underlying Cause of Cholecystitis Cholecystitis
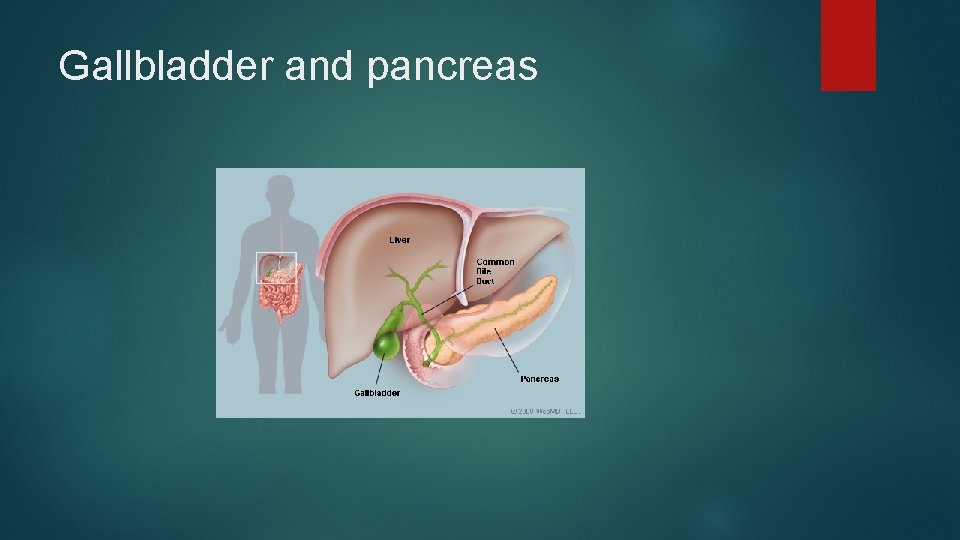
Gallbladder and pancreas

Underlying Cause of Cholecystitis?

Cholecystitis Inflammation of gallbladder that can be acute or chronic process Acute Calculous cholecystitis- Inflammation from stone. Bile is unable to get out contributing to the irritation of gallbladder. Associated impaired circulation, edema, and distention can lead to ischemia and infection. Peritonitis may be complication of perforated gallbladder. Acalculous cholecystitis- inflammation w/o stones, biliary stasis Chronic Results from inefficient bile emptying, fibrotic and contracted gallbladder. What assessment findings can you anticipate? Diagnostics? Meds?

Cholecystitis Severe, steady pain in the upper right part of abdomen Pain that radiates from abdomen to right shoulder or back Tenderness over abdomen when it's touched Sweating Nausea, vomiting, signs of dehydration Fever, chills Abdominal bloating Tachycardia Usually occur after a meal, particularly a large meal or a meal high in fat.

Cholecystitis Jaundice- what is this? Dark orange and foamy urine-from excess circulating bilirubin in chronic cases. Steatorrhea and clay-colored feces (absence of urobilinogen to color stool from chronic) Pruritius- from what? Murphy’s sign- cannot take deep breath when examiners fingers are passed below hepatic margin due to pain
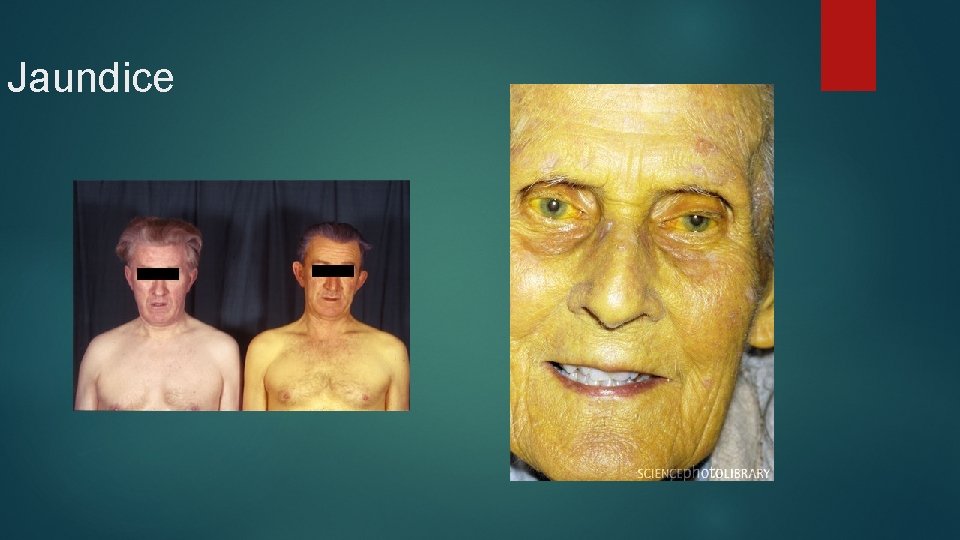
Jaundice

Diagnostics Labs- WBC, AST, LDH, direct and indirect bili, amylase and lipase (if from pancreatic involvement). CT Scan or abdominal US can create pics of your gallbladder A hepatobiliary iminodiacetic acid (HIDA) scan tracks the production and flow of bile from your liver to your small intestine and shows if bile is blocked at any point along the way. Involves injecting a radioactive chemical into your body. The chemical binds to the bile-producing cells, so it can be clearly seen as it travels with the bile through the bile ducts.

Medications Antibiotics Pain medication

Risk Factors Gallstones Being female-Women have a greater risk of gallstones than men do. This makes women more likely to develop cholecystitis. Increasing age- As you get older, your risk of gallstones increases, as does your risk of cholecystitis. What are your nursing priorities? What nursing interventions will you initiate?

Interventions NPO with N/V NG decompression for severe vomiting, antiemetic as ordered Pharmacological Small Therapy low fat meals and avoid gassy foods Prepare for possible surgery
Nonsurgical ESWL- shockwaves break down stones smaller Percutaneous transhepatic biliary catheter to open ducts

Surgical interventions Cholecystectomy Choledocholithotomy- incision to common bile duct to remove stone. May be performed laparoscopy, usually not open anymore Once your gallbladder is removed, bile flows directly from your liver into your small intestine, rather than being stored in your gallbladder. You don't need your gallbladder to live, does not affect your ability to digest food, although it can cause diarrhea that is usually temporary.
Post-op interventions What are you watching when your patient comes back after surgery?

Post-op Monitor CDB, resp complications r/t pain splint abd Ambulate- this helps prevent what complications? Analgesics for incisional pain Diet as prescribed Any drains such as JP What teaching will you initiate for prevention of gallstones?

Prevention Lose weight slowly- Rapid weight loss can increase the risk of gallstones. Maintain a healthy weight. Obesity and being overweight increase the risk of gallstones. Choose a healthy diet. Diets high in fat and low in fiber may increase the risk of gallstones. Choose a diet that's full of fruits, vegetables and whole grains.

Pancreatitis During normal digestion, the inactivated pancreatic enzymes move through ducts in your pancreas and travel to the small intestine, where the enzymes become activated and help with digestion. In pancreatitis, the enzymes become activated while still in the pancreas. This causes the enzymes to irritate the cells of your pancreas, causing inflammation and the signs and symptoms associated with pancreatitis. So basically the pancreas starts to digest itself.

Pancreatitis Acute pancreatitis is an acute inflammatory process of the pancreas. The primary etiologic factors are biliary tract disease (most common cause in women) and alcoholism (most common cause in men). Abdominal pain usually located in the left upper quadrant is the predominant symptom of acute pancreatitis. Other manifestations include nausea, vomiting, hypotension, tachycardia, and jaundice.
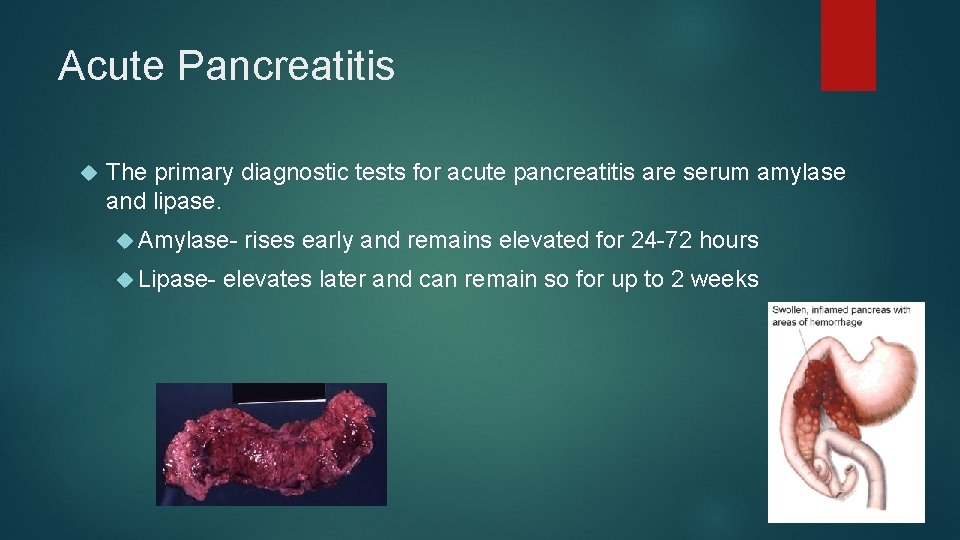
Acute Pancreatitis The primary diagnostic tests for acute pancreatitis are serum amylase and lipase. Amylase Lipase- rises early and remains elevated for 24 -72 hours elevates later and can remain so for up to 2 weeks

Chronic Pancreatitis Chronic pancreatitis is a continuous, prolonged, inflammatory, and fibrosing process of the pancreas. The pancreas becomes progressively destroyed as it is replaced with fibrotic tissue. Strictures and calcifications may also occur in the pancreas. Clinical manifestations of chronic pancreatitis include abdominal pain, symptoms of pancreatic insufficiency, including malabsorption with weight loss, constipation, jaundice with dark urine, steatorrhea, and diabetes mellitus. What complications should you monitor for?

Complications Diabetes. Damage to insulin-producing cells in your pancreas from chronic pancreatitis can lead to diabetes. Acute pancreatitis can make your pancreas vulnerable to bacteria and infection. Pancreatic infections are serious and require intensive treatment, such as surgery to remove the infected tissue. Malnutrition. Both acute and chronic pancreatitis can cause your pancreas to produce fewer of the enzymes that are needed to break down and process nutrients from the food you eat. This can lead to malnutrition, diarrhea and weight loss, even though you may be eating the same foods or the same amount of food. Pancreatic cancer. Long-standing inflammation in your pancreas caused by chronic pancreatitis is a risk factor for developing pancreatic cancer.

complications Pseudocyst. Acute pancreatitis can cause fluid and debris to collect in cystlike pockets in your pancreas. A large pseudocyst that ruptures can cause complications such as internal bleeding and infection. Turner’s sign- grayish-blue discoloration to flanks from pancreatic enzyme leakage into peritoneal cavity. Can go into shock, what measures should be in place? Cullen’s sign- discoloration of abdomen and periumbilical area. Diagnostics?

Diagnostics Blood tests to look for elevated levels of pancreatic enzymes- amylase and lipase Stool tests in chronic pancreatitis to measure levels of fat that could suggest your digestive system isn't absorbing nutrients adequately Computerized tomography (CT) scan to look for gallstones and assess the extent of pancreas inflammation Abdominal ultrasound to look for pancreas inflammation

Collaborative Care Relief of pain; prevention or alleviation of shock; reduction of pancreatic secretions; control of fluid and electrolyte imbalances; prevention or treatment of infections; and removal of the precipitating cause. Because hypocalcemia can also occur usually early on from release of fatty acids combining with calcium, the nurse must observe for symptoms of tetany, such as jerking, irritability, and muscular twitching. Also watch for positive Trousseau's sign which is carpal spasm of the patient's hand Chvostek’s sign which is facial twitching when tapping face just below and in front of ear. Normal Calcium- 8. 6 -10 mg/d. L

Collaborative Care Diet-NPO gives your pancreas a chance to recover by decreasing GI activity and enzyme production. This is your best intervention to control pain!! Pain medications- Pancreatitis can cause severe pain. IVF Pancreatic enzyme supplements can help your body breakdown and process the nutrients in the foods you eat. Enzymes are taken with meals and snacks. Diet- low fat meals with high nutrients. Chronic may need huge amount of calories for healing so collaborate with dietician. When under control treat underlying problem….

Collaborative care Pancreatitis caused by a narrowed or blocked bile duct may require procedures to open or widen the bile duct Gallbladder surgery- If gallstones remove your gallbladder (cholecystectomy). Pancreas surgery-Surgery may be necessary to drain fluid from your pancreas or to remove diseased tissue. Treatment for alcohol dependence. Drinking several drinks a day over many years can cause pancreatitis- refer to therapy. Weekend binge drinking can also cause an acute pancreatitis.

Overall therapy…. Stop drinking alcohol Stop smoking Choose a low-fat diet Drink more (water) As with any disease process……

Q A client has been admitted to the hospital with a diagnosis of acute pancreatitis and the nurse is assessing the client's pain. What type of pain is consistent with this diagnosis? A. Burning and aching, located in the left lower quadrant and radiating to the hip B. Severe and unrelenting, located in the epigastric area and radiating to the back C. Burning and aching, located in the epigastric area and radiating to the umbilicus D. Severe and unrelenting, located in the left lower quadrant and radiating to the groin

A B. Severe and unrelenting, located in the epigastric area and radiating to the back The pain associated with acute pancreatitis is often severe and unrelenting, is located in the epigastric region, and radiates to the back. The other options are incorrect.

Q The nurse is assessing a client who is experiencing an acute episode of cholecystitis. Where should the nurse anticipate the location of the pain? A. Right lower quadrant, radiating to the back B. Right lower quadrant, radiating to the umbilicus C. Right upper quadrant, radiating to the left scapula and shoulder D. Right upper quadrant, radiating to the right scapula and shoulder

A D. Right upper quadrant, radiating to the right scapula and shoulder During an acute episode of cholecystitis, the client may complain of severe right upper quadrant pain that radiates to the right scapula and shoulder. This is determined by the pattern of dermatomes in the body. The other options are incorrect.

Q The nurse is caring for a client with acute pancreatitis and is monitoring the client for paralytic ileus. Which assessment data should alert the nurse to this occurrence? A. Inability to pass flatus B. Loss of anal sphincter control C. Severe, constant pain with rapid onset D. Firm, nontender mass palpable at the lower right costal margin

A A. Inability to pass flatus An inflammatory reaction such as acute pancreatitis can cause paralytic ileus, the most common form of nonmechanical obstruction. Inability to pass flatus is a clinical manifestation of paralytic ileus. Loss of sphincter control is not a sign of paralytic ileus. Pain is associated with paralytic ileus, but the pain usually manifests as a more constant generalized discomfort. Option 4 is the description of the physical finding of liver enlargement. The liver may be enlarged in cases of cirrhosis or hepatitis. Although this client may have an enlarged liver, an enlarged liver is not a sign of paralytic ileus or intestinal obstruction.

Q The nurse provides dietary instructions to a client with a diagnosis of cholecystitis. Which food item identified by the client indicates an understanding of foods to avoid? A. Fresh fruit B. Brown gravy C. Fresh vegetables D. Poultry w/o skin

A B, brown gravy The client with cholecystitis should decrease overall intake of dietary fat. Foods that should be avoided include sausage, gravies, fatty meats, fried foods, products made with cream, and desserts. Appropriate food choices include fruits and vegetables, fish, and poultry without skin.

Q The nurse is performing an assessment on a client with a suspected diagnosis of acute pancreatitis. The nurse will direct the assessment to look for which as a hallmark sign of this disorder? A. Hypothermia B. Epigastric pain radiating to the neck area C. Severe abdominal pain relieved by vomiting D. Severe abdominal pain that is unrelieved by vomiting

A D. Severe abdominal pain that is unrelieved by vomiting Nausea and vomiting are common presenting manifestations of acute pancreatitis. A hallmark symptom is severe abdominal pain that is not relieved by vomiting. The vomitus characteristically consists of gastric and duodenal contents. Fever also is a common sign but usually is mild, with temperatures less than 39° C. Epigastric pain radiating to the neck area is not a characteristic symptom.

Q A hospitalized client is diagnosed with pancreatitis. The nurse plans care, knowing that production of which substance will be elevated in blood studies for this client? A. Pepsin B. Lactase C. Lipase D. Enterokinase

A C. Lipase

Q A. B. The nurse is obtaining a health history for a client with chronic pancreatitis. The health history is most likely to include which as a common causative factor in this client's disorder? Weight gain Use of alcohol C. Exposure to occupational chemicals D. Abdominal pain relieved with food or antacids

A B. use of alcohol Chronic pancreatitis occurs most often in alcoholics. Abstinence from alcohol is important to prevent the client from developing chronic pancreatitis. Clients usually experience malabsorption with weight loss. Chemical exposure is associated with cancer of the pancreas. Pain will not be relieved with food or antacids.

Pancreatitis Case Study
- Slides: 41