Gait 3 types of gait to be examined

Gait

3 types of gait to be examined 1. Regular gait 2. Tandem gait (heel-to-toe walk) 3. Heel walk & Toe walk

Regular gait a. Instruct the patient to walk back and forth across the room b. Observe: (1) symmetry (2) (3) (4) (5) (6) balance distance between feet (width) length of stride arm swing heel strike c. Gait may be disturbed due to pain in the low back or lower extremity, deformity, or neurologic lesions

Classic gait abnormalities associated with neuromuscular disorders
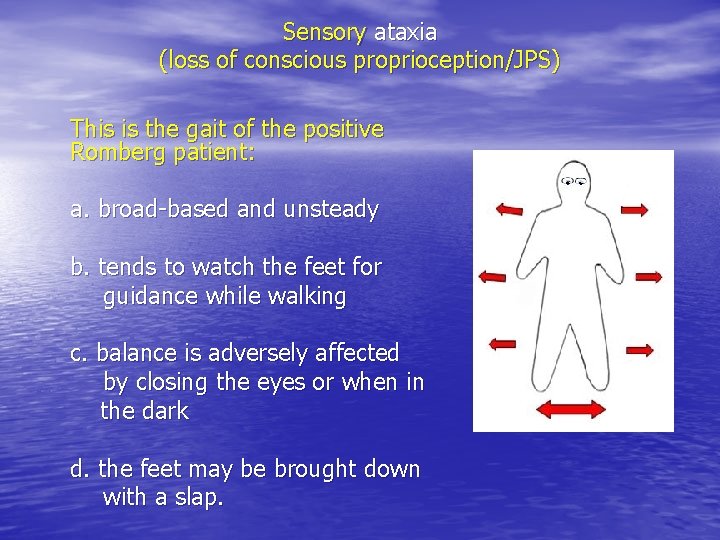
Sensory ataxia (loss of conscious proprioception/JPS) This is the gait of the positive Romberg patient: a. broad-based and unsteady b. tends to watch the feet for guidance while walking c. balance is adversely affected by closing the eyes or when in the dark d. the feet may be brought down with a slap.

Significance: loss of conscious proprioception (JPS) from the feet Causes of decreased conscious proprioception include: a. PNS: polyneuropathy (1) common causes: (a) diabetes (b) alcoholism (2) less common: (a) heavy metal poisoning b. CNS: dorsal column-medial lemniscus lesion (1) common causes: (a) multiple sclerosis (b) cervical spondylotic myelopathy (2) less common: (a) subacute combined systems disease (posterolateral sclerosis) (b) tabes dorsalis
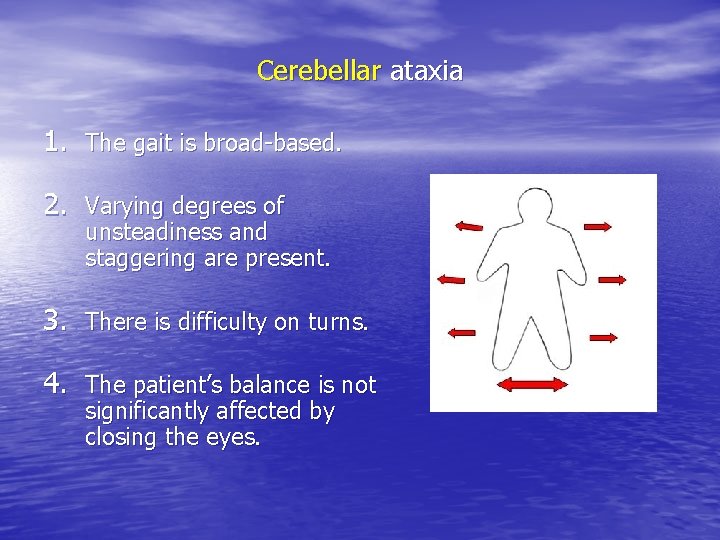
Cerebellar ataxia 1. The gait is broad-based. 2. Varying degrees of unsteadiness and staggering are present. 3. There is difficulty on turns. 4. The patient’s balance is not significantly affected by closing the eyes.

Causes of cerebellar ataxia a. Multiple sclerosis b. Chronic alcohol abuse (anterior lobe syndrome) c. Cerebrovascular disease (posterior circulation) d. Tumors (1) children: 10 tumors (2) adults: metastatic
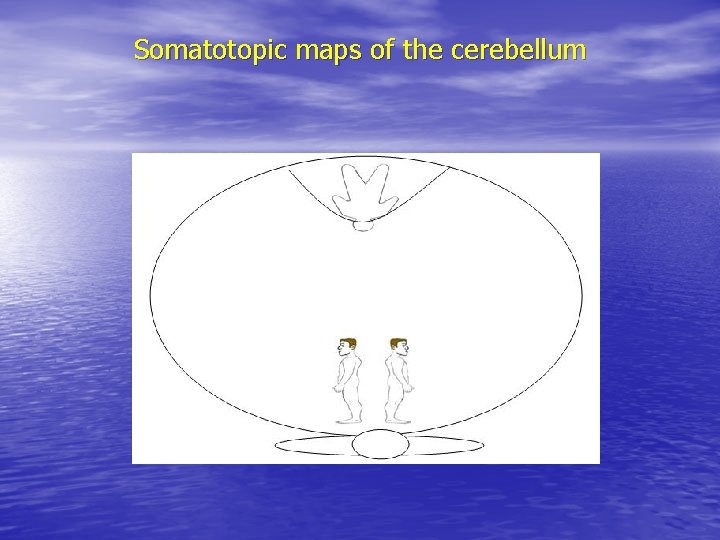
Somatotopic maps of the cerebellum

Follow-up for suspected cerebellar lesions Follow-up suspected cerebellar lesion with point-to-point and rapid alternating movement tests of limb coordination, looking for dysmetria and dysdiadochokinesis, respectively.
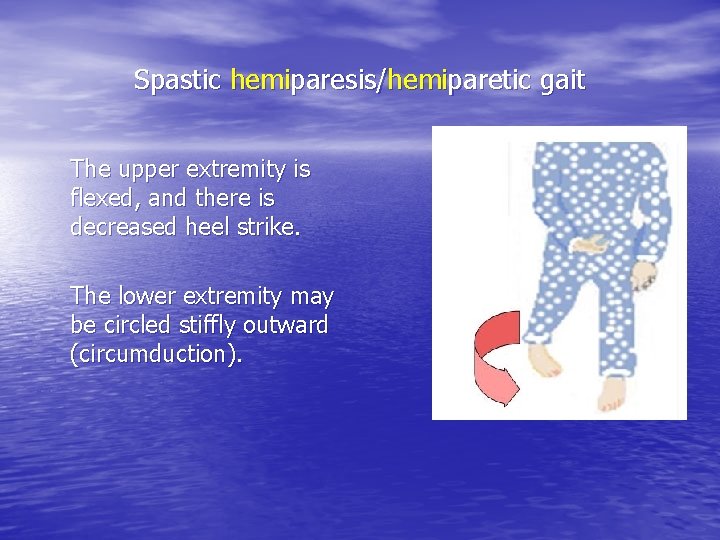
Spastic hemiparesis/hemiparetic gait The upper extremity is flexed, and there is decreased heel strike. The lower extremity may be circled stiffly outward (circumduction).

Spastic hemiparesis gait Significance: UMN lesion a. C 1 -4 spinal cord lesion, ipsilateral (above C 5 origin of the brachial plexus) b. cerebrovascular disease, contralateral (internal capsule)

UMN lesion characteristics Distribution of weakness and spasticity: a. Upper extremity: (1) spasticity is relatively greater in the anterior flexor muscles (2) weakness is relatively greater in the posterior extensor muscles. b. Lower extremity: (1) spasticity is relatively greater in the plantar flexors (2) weakness is relatively greater in the dorsiflexors. Facial weakness: UMN (corticobulbar) facial weakness involves the contralateral lower quadrant of the face.
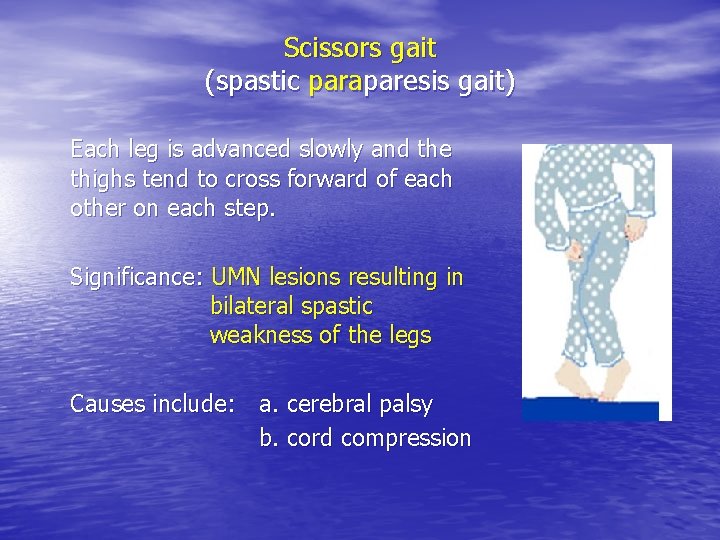
Scissors gait (spastic paraparesis gait) Each leg is advanced slowly and the thighs tend to cross forward of each other on each step. Significance: UMN lesions resulting in bilateral spastic weakness of the legs Causes include: a. cerebral palsy b. cord compression
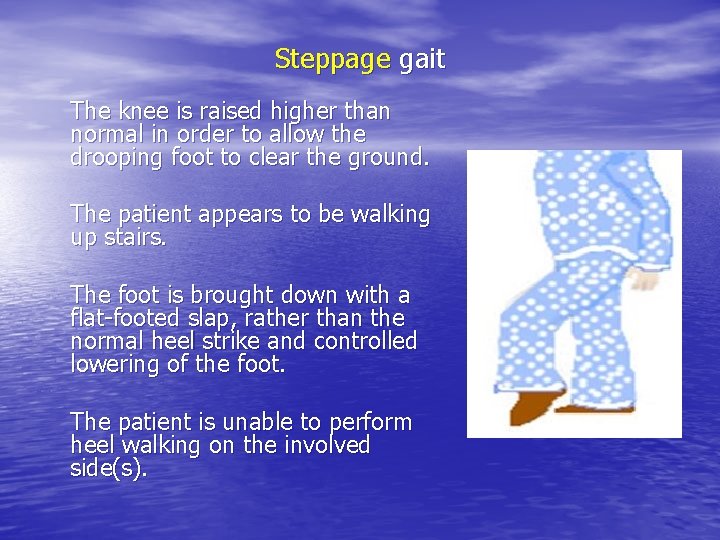
Steppage gait The knee is raised higher than normal in order to allow the drooping foot to clear the ground. The patient appears to be walking up stairs. The foot is brought down with a flat-footed slap, rather than the normal heel strike and controlled lowering of the foot. The patient is unable to perform heel walking on the involved side(s).

Steppage gait Significance: foot drop/paresis of the dorsiflexors Etiology: a. L 5 lesion (radiculopathy, polio) b. Common peroneal nerve lesion
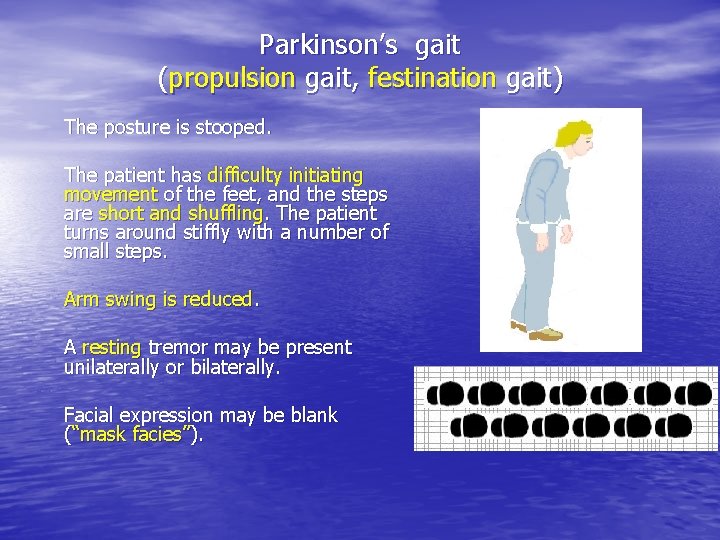
Parkinson’s gait (propulsion gait, festination gait) The posture is stooped. The patient has difficulty initiating movement of the feet, and the steps are short and shuffling. The patient turns around stiffly with a number of small steps. Arm swing is reduced. A resting tremor may be present unilaterally or bilaterally. Facial expression may be blank (“mask facies”).
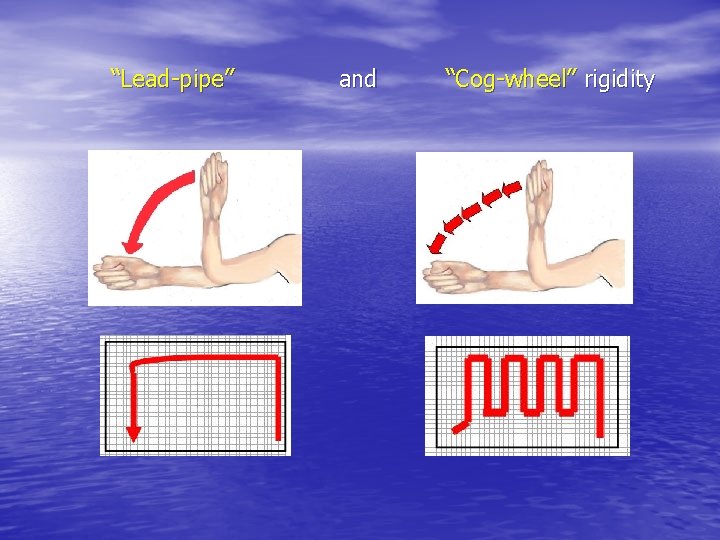
“Lead-pipe” and “Cog-wheel” rigidity

Parkinson’s disease results from degeneration of the substantia nigra portion of the basal ganglia resulting in decrease of the neurotransmitter dopamine. The major characteristics of Parkinson’s disease are: 1. resting tremor 2. rigidity 3. slow movement (“bradykinesia”) and difficulty initiating movement - loss of movement (“akinesia”)

Waddling gait When the foot is lifted off the ground, the pelvis on that side drops down. The patient may throw the trunk to the opposite side prior to lifting the leg in an attempt to compensate. Significance: weakness of the proximal muscles of the lower extremity (pelvic girdle) Causes: a. muscle disease (myopathy) (1) muscular dystrophy (genetic) (2) polymyositis (autoimmune/inflam) b. polio

Also, observe the patient as they sit and rise from a chair. With proximal muscle weakness, the patient may use their hands to walk up the thighs as they attempt to rise from the chair (Gower’s sign). The Trendelenburg test should be performed as a followup. Stand behind the patient and ask the patient to raise one leg off the ground at a time. Observe the gluteal folds. Dropping of the pelvis in the coronal plane on the unsupported side is a positive finding, suggestive of weakness of the contralateral gluteus medius.

Tandem gait (heel-to-toe walk) Standing nearby, ready to support the patient in case they become unstable, ask the patient to walk as if on a tightrope, placing the heel of one foot directly in front of the other foot.
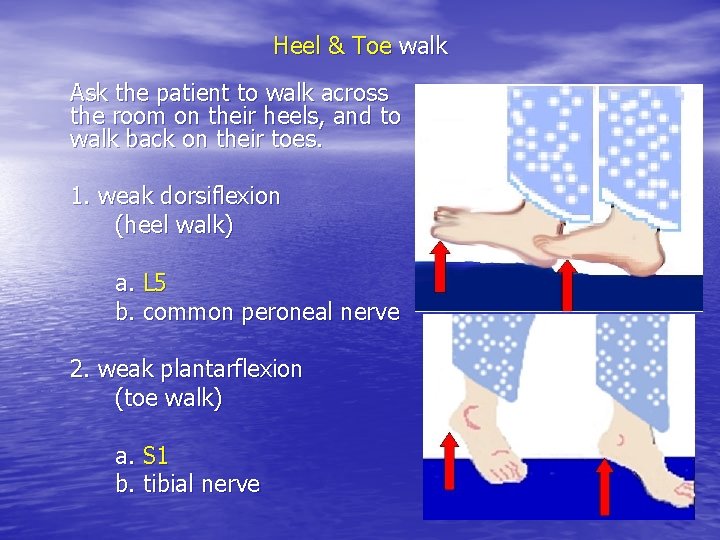
Heel & Toe walk Ask the patient to walk across the room on their heels, and to walk back on their toes. 1. weak dorsiflexion (heel walk) a. L 5 b. common peroneal nerve 2. weak plantarflexion (toe walk) a. S 1 b. tibial nerve
- Slides: 23