Funding policy based on DRGs Casemix Methodology of

Funding policy based on DRGs. Casemix. Methodology of DRG costing. RIC DRG Workshop Belgrade, 18 -22. November 2013.
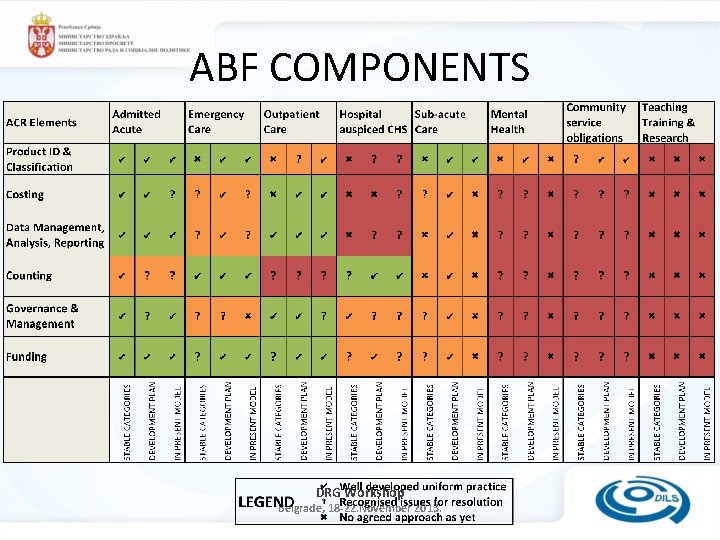
ABF COMPONENTS DRG Workshop Belgrade, 18 -22. November 2013.
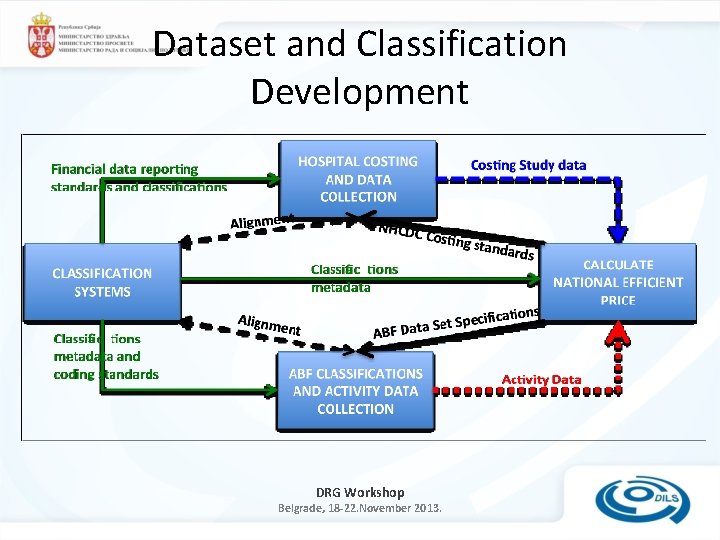
Dataset and Classification Development DRG Workshop Belgrade, 18 -22. November 2013.
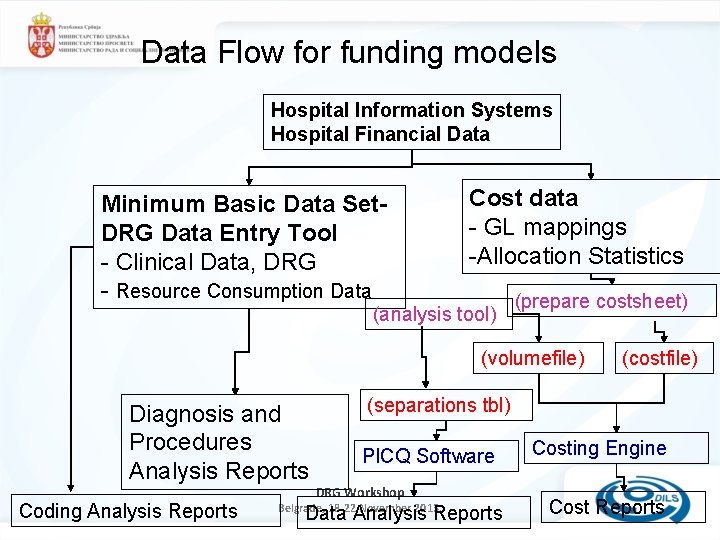
Data Flow for funding models Hospital Information Systems Hospital Financial Data Minimum Basic Data Set. DRG Data Entry Tool - Clinical Data, DRG - Resource Consumption Data Cost data - GL mappings -Allocation Statistics (analysis tool) (prepare costsheet) (volumefile) Diagnosis and Procedures Analysis Reports Coding Analysis Reports (costfile) (separations tbl) PICQ Software DRG Workshop Belgrade, 18 -22. November 2013. Data Analysis Reports Costing Engine Cost Reports

Data principles and privacy • The National Health Reform Agreement includes principles to underpin data collection to: – ensure patient privacy – minimise administrative burden – improve the evidence base of hospital funding • The Commonwealth and the States will enter into a National Health Information Agreement by that reflects the objectives of the National Health Reform Agreement DRG Workshop Belgrade, 18 -22. November 2013.
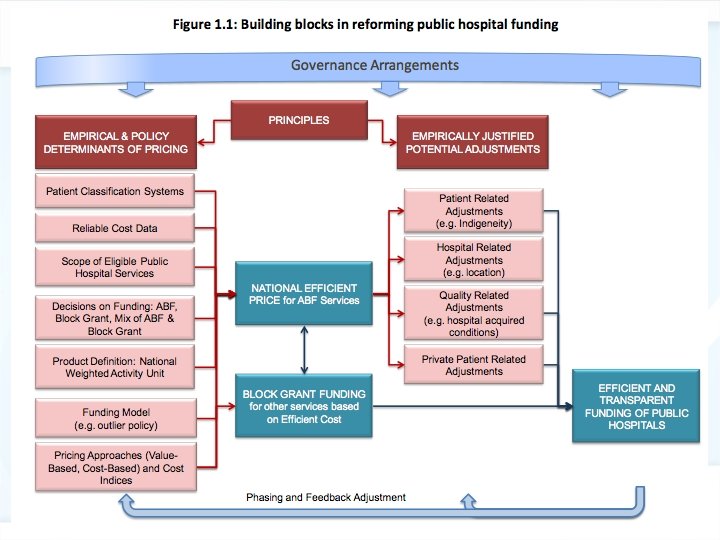
Towards a national pricing model for hospitals • What is a hospital? • Normative pricing >>> best practice pricing • Indexation rules • Private patients • http: //www. ihpa. gov. au/internet/ihpa/publishi ng. nsf/Content/EB 8 EFD 07 DF 85 BC 70 CA 2579830 0033 BE 1/$File/IHPA%20 Draft%20 Pricing%20 Fra mework_long%20 version. pdf DRG Workshop Belgrade, 18 -22. November 2013.

Health Policy Solutions (in association with Casemix Consulting and Aspex DRG Workshop Consulting) Page 58 Belgrade, 18 -22. November 2013.

Where does quality come in? • • • NHPA ACSQH Sentinel events loops Clinical pathways Complaints Pricing signals Epidemiology Clinical trials R&D new technology marketing DRG Workshop Belgrade, 18 -22. November 2013.
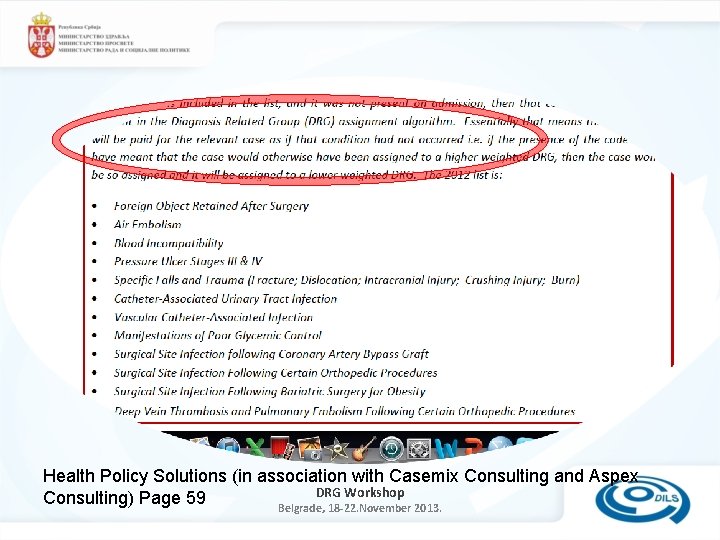
Health Policy Solutions (in association with Casemix Consulting and Aspex DRG Workshop Consulting) Page 59 Belgrade, 18 -22. November 2013.

How to measure quality • • Process indicators Protocol compliance Outcome indicators Effort Inputs Failures and risks Value for money DRG Workshop Belgrade, 18 -22. November 2013.

THE FIRST IDEA OF A NATIONAL EFFICIENT PRICE • COMPLETE DATA • ACCURATE DATA • CONSISTENT COUNTING – Activity ~ Financial • NORMATIVE PRICING • STANDARD PRICING • REFERENCE PRICING • THE MARKET DRG Workshop Belgrade, 18 -22. November 2013.

THE SECOND IDEA OF A NATIONAL EFFICIENT PRICE • Whose costs? Whose quality? • Who pays for what? ? NHIF Mo. H INSURERS PATIENT HEALTH SYSTEM OPERATORS, REGIONS, HMOs EMPLOYED PRACTITIONERS Drug, MD SUPPLIERS SUPPORT SERVICES MANUFACTURERS HOSPITALS, HEALTH CLINCS, PRACTITIONERS DRG Workshop Belgrade, 18 -22. November 2013.
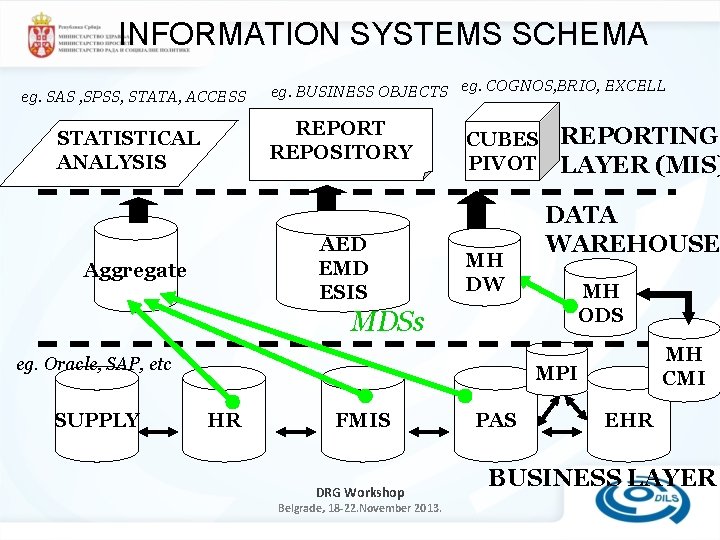
INFORMATION SYSTEMS SCHEMA eg. SAS , SPSS, STATA, ACCESS eg. BUSINESS OBJECTS eg. COGNOS, BRIO, EXCELL REPORT REPOSITORY STATISTICAL ANALYSIS AED EMD ESIS Aggregate CUBES PIVOT MH DW MDSs eg. Oracle, SAP, etc SUPPLY REPORTING LAYER (MIS) DATA WAREHOUSE MH ODS MH CMI MPI HR FMIS DRG Workshop Belgrade, 18 -22. November 2013. PAS EHR BUSINESS LAYER

The basic components • Patient costing fundamentals • Costing standards and methods • The Idea of Patient Level Information and Costing • Allocating expenditure from accounts to activity Workshop • Key uses of patient. DRGcost data Belgrade, 18 -22. November 2013.
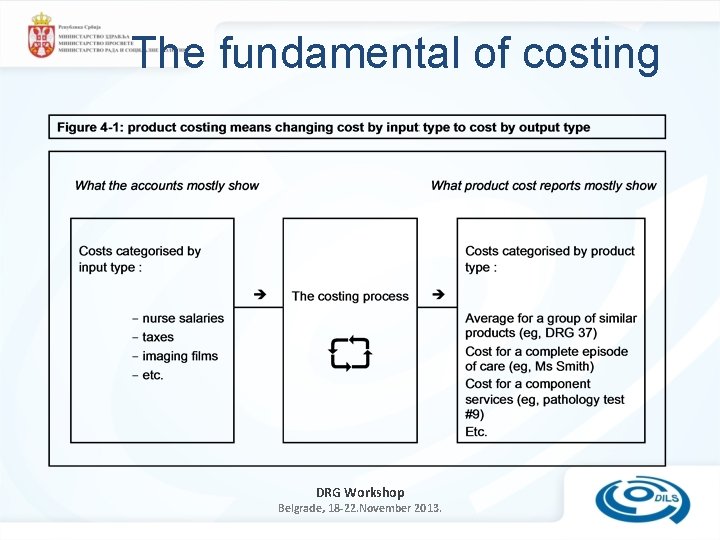
The fundamental of costing DRG Workshop Belgrade, 18 -22. November 2013.
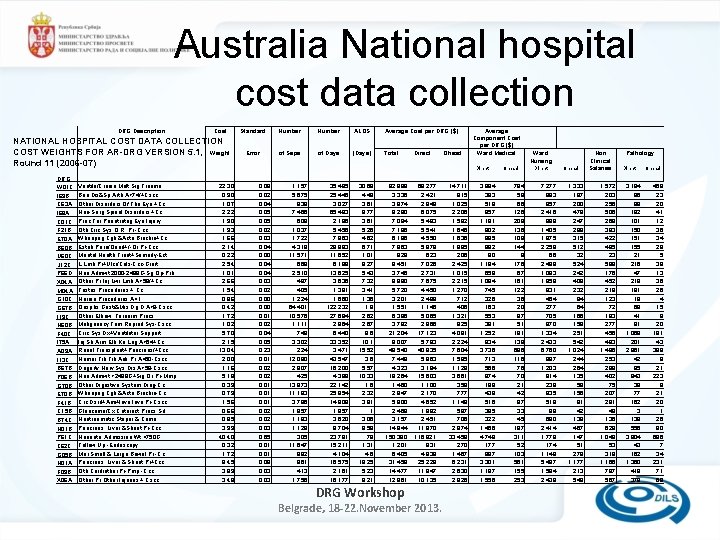
Australia National hospital cost data collection DRG Description Cost NATIONAL HOSPITAL COST DATA COLLECTION COST WEIGHTS FOR AR-DRG VERSION 5. 1, Weight Round 11 (2006 -07) DRG W 01 Z I 69 B C 63 A I 68 A C 01 Z F 21 B E 70 A B 60 B U 60 Z J 12 C P 66 D X 04 A M 04 A G 10 Z G 67 B I 19 Z N 60 B F 40 Z I 75 A A 09 A I 13 C B 67 B P 06 B G 70 B E 70 B F 41 B C 15 B B 74 Z H 01 B P 61 Z Z 62 Z G 05 B H 01 A F 09 B X 06 A Standard Number ALOS Average Cost per DRG ($) Error of Seps of Days (Days) Total Direct Ohead Average Component Cost per DRG ($) Ward Medical Direct Ohead Non Clinical Salaries Ward Nursing Direct Pathology Direct Ohead Ventiln/Cranio Mult Sig Trauma Bne Dis&Sp Arth A>74/+Cscc Other Disorders Of The Eye +Cc Non-Surg Spinal Disorders +Cc Proc For Penetratng Eye Injury Oth Circ Sys O. R. Pr -Ccc Whoopng Cgh &Acte Brnchio+Cc Estab Para/Quad+/-Or Pr-Ccc Mental Health Treat+Samedy-Ect L Lmb Pr+Ulcr/Cels-Ccc-Graft Neo, Admwt 2000 -2499 G-Sg Op-Prb Other Pr Inj Lwr Lmb A>59/+Cc Testes Procedures + Cc Hernia Procedures A<1 Oesphs, Gastr&Mis Dg D A>9 -Cscc Other Elbow, Forearm Procs Malignancy Fem Reprod Sys-Cscc Circ Sys Dx+Ventilator Support Inj Sh, Arm, Elb, Kn, Leg A>64+Cc Renal Transplant+Pancreas/+Ccc Humer, Tib, Fib, Ank Pr A<60 -Cscc Degnrtv Nerv Sys Dis A>59 -Cscc Neo, Admwt >2499 G+Sig Or Pr-Mmp Other Digestive System Diag-Cc Whoopng Cgh &Acte Brnchio-Cc Crc Dsrd+Ami+Inva Inve Pr-Cscc Glaucoma/Cx Cataract Procs, Sd Nontraumatic Stupor & Coma Pancreas, Liver &Shunt Pr-Ccc Neonate, Admission Wt <750 G Follow Up -Endoscopy Mnr Small & Large Bowel Pr -Cc Pancreas, Liver & Shunt Pr+Ccc Oth Cardiothor Pr-Pmp -Ccc Other Pr Other Injuries + Cscc 22. 30 0. 90 1. 07 2. 22 1. 90 1. 93 1. 66 2. 14 0. 22 2. 54 1. 01 2. 66 1. 54 0. 86 0. 42 1. 72 1. 02 5. 70 2. 15 13. 04 2. 00 1. 16 5. 18 0. 39 0. 79 1. 56 0. 66 0. 85 3. 99 40. 40 0. 32 1. 72 8. 45 3. 89 3. 48 0. 02 0. 04 0. 05 0. 02 0. 03 0. 04 0. 00 0. 04 0. 03 0. 02 0. 00 0. 01 0. 02 0. 04 0. 05 0. 23 0. 01 0. 02 0. 03 0. 65 0. 01 0. 08 0. 03 1, 157 5, 675 839 7, 466 609 1, 037 1, 722 4, 319 11, 571 668 2, 510 497 405 1, 224 64, 401 10, 576 1, 111 749 3, 302 224 12, 090 2, 907 425 13, 873 11, 193 3, 786 1, 957 1, 183 1, 129 305 11, 647 892 861 413 1, 756 35, 485 25, 445 3, 027 65, 483 2, 196 5, 456 7, 963 28, 993 11, 652 6, 189 13, 625 3, 636 1, 381 1, 660 122, 232 27, 694 2, 964 6, 440 33, 352 3, 471 43, 547 16, 200 4, 388 22, 142 25, 954 14, 809 1, 957 3, 620 9, 704 23, 781 15, 211 4, 104 16, 575 2, 161 16, 177 30. 68 4. 48 3. 61 8. 77 3. 61 5. 26 4. 62 6. 71 1. 01 9. 27 5. 43 7. 32 3. 41 1. 36 1. 9 2. 62 2. 67 8. 6 10. 1 15. 52 3. 6 5. 57 10. 33 1. 6 2. 32 3. 91 1 3. 06 8. 59 78 1. 31 4. 6 19. 25 5. 23 9. 21 82, 988 3, 336 3, 974 8, 280 7, 084 7, 186 6, 186 7, 963 829 9, 451 3, 746 9, 890 5, 720 3, 201 1, 551 6, 386 3, 792 21, 204 8, 007 48, 540 7, 448 4, 323 19, 264 1, 460 2, 947 5, 800 2, 469 3, 157 14, 844 150, 380 1, 201 6, 405 31, 458 14, 477 12, 961 DRG Workshop 68, 277 2, 421 2, 949 6, 075 5, 493 5, 541 4, 550 5, 979 623 7, 026 2, 731 7, 675 4, 450 2, 489 1, 146 5, 065 2, 866 17, 123 5, 783 40, 935 5, 863 3, 194 15, 603 1, 100 2, 170 4, 652 1, 882 2, 451 11, 870 116, 921 931 4, 938 25, 228 11, 847 10, 135 Belgrade, 18 -22. November 2013. 14, 711 915 1, 025 2, 206 1, 592 1, 645 1, 636 1, 985 206 2, 425 1, 015 2, 215 1, 270 712 406 1, 321 925 4, 081 2, 224 7, 604 1, 585 1, 129 3, 661 359 777 1, 148 587 706 2, 974 33, 459 270 1, 467 6, 231 2, 630 2, 826 3, 984 393 519 957 1, 181 802 895 892 80 1, 184 658 1, 084 745 326 163 553 381 1, 252 834 3, 736 713 566 974 199 438 516 395 322 1, 466 4, 748 177 887 3, 301 1, 187 1, 556 784 59 66 126 208 136 109 144 8 176 67 161 122 36 20 87 51 191 139 696 116 76 70 21 42 87 33 45 187 311 52 103 561 155 253 7, 277 883 957 2, 416 999 1, 405 1, 975 2, 258 66 2, 498 1, 093 1, 958 931 454 277 705 870 1, 334 2, 433 6, 760 997 1, 203 914 238 935 519 98 690 2, 414 1, 779 174 1, 148 5, 497 1, 584 2, 439 1, 333 197 200 479 247 288 315 512 32 524 242 409 232 94 64 166 159 251 542 1, 024 244 264 135 58 156 91 42 138 467 147 51 278 1, 177 213 549 1, 572 203 256 506 269 383 422 485 23 599 176 452 218 123 72 193 277 456 493 1, 496 253 288 402 75 207 291 48 136 629 1, 049 53 318 1, 166 797 567 3, 194 96 99 182 101 150 151 155 21 216 47 218 191 18 68 41 81 1, 069 201 2, 961 42 95 843 38 77 162 3 138 556 3, 904 43 162 1, 360 418 378 468 23 20 41 12 36 34 29 5 38 13 36 26 4 15 8 20 181 43 398 8 21 223 8 21 20 1 26 90 686 7 34 231 71 69

NHCDC Reporting Standards http: //www. health. gov. au /internet/main/publishing. nsf/Content/0 FABA 9 D 6 D B 24 D 7 E 8 CA 257712000 C 5 D 3 C/$File/Hospital. Pat ient. Costing. Standards_v 2 _Final_June%202011. pd f DRG Workshop Belgrade, 18 -22. November 2013.

Why do we need clinical costing? • Accurately value products – eg DRG’s for funding – Costweights for funding and payment – Activity analysis in weighted activity terms • Benchmark our hospital against others and over time – Properly manage performance – care profiles – Set achievement targets – ‘match the above average performers over the next two years’ DRG Workshop Belgrade, 18 -22. November 2013.

Clinical Costing Standards Association DRG Workshop Belgrade, 18 -22. November 2013.

The importance of hospitals being able to analyse their costs of production • Clinicians are the control locus of expenditure • “Every clinical decision is an expenditure decision” • Hospitals must be able to provide feedback to clinicians on comparative use of resource (cost) with benchmarks • Both normative (peer hospitals) and best practice standards (clinical pathways) DRG Workshop Belgrade, 18 -22. November 2013.

The idea of fully absorbed costing • • Starts with total expenditure of hospital. Broken into overhead and direct. INPATIENT FRACTION IS APPLIED *either here Overhead costs are attributed to treatment units. Then become part of direct costs of treating patients. *or here • Unit costs are attributed to patients according to their service utilisation and/OR • Direct patient costs allocated according to utilisation (activity) statistics. DRG Workshop Belgrade, 18 -22. November 2013.

Inpatient expenditure fractions • Cost centres in general ledger and/or • Inpatient ratio of staff utilisation • Inpatient ratio of floor space, utilty access points, service times, • Inpatient ratio of diagnostics orders • Weighted units of service provided (eg beddays, consultations, DRG Workshop Belgrade, 18 -22. November 2013.

Direct costs and overhead costs • Almost anything can be a direct cost if individual patient utilisation is recorded. • Many cost centres provide services to other cost centres. • It is important to have a standard sequence of distributing the costs of overhead cost centres to other cost centres. DRG Workshop Belgrade, 18 -22. November 2013.

The Yale cost model • A standard method of cost disaggregation from total hospital expenditure to patient episode or DRG. • Follows a set sequence of disaggregation from overhead cost centres to ‘intermediate product’ cost centres. • Allocates from intermediate products to patients according to utilisation or service weights. DRG Workshop Belgrade, 18 -22. November 2013.

Intermediate products of interest to hospital managers – examples • Cost per meal per patient per day for ward x compared to hospital average • Cost of Xray A compared to other providers • Cost per hour of nursing service in ICU (b) • Surgeon cost for operation x compared to other surgeons DRG Workshop Belgrade, 18 -22. November 2013.

Types of Costing 1/2 • Clinical Costing – bottom up costing approach – each patient episode is a product – requires data of all goods and services consumed in the treatment of individual patients – Data are then converted into cost estimates for each patient by reference to measures of the relative costs of providing these services – Allows analysis of resource use by individual patient episode DRG Workshop Belgrade, 18 -22. November 2013.
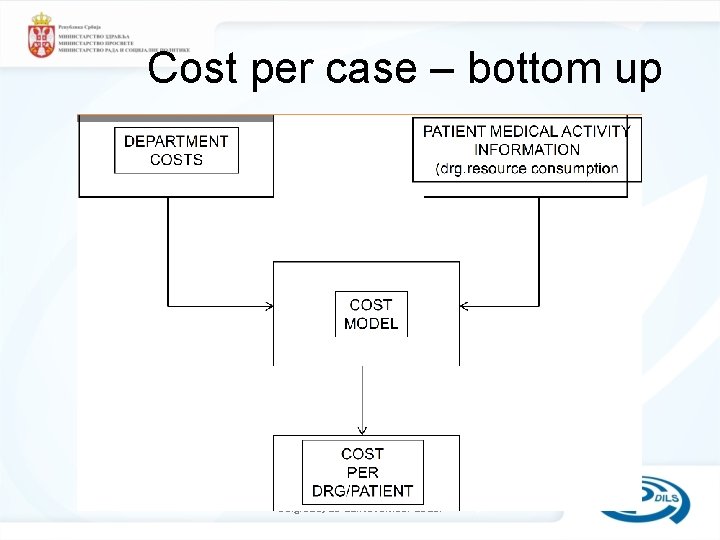
Cost per case – bottom up DRG Workshop Belgrade, 18 -22. November 2013.

Types of Costing 2/2 • Cost Modelling – top down approach – Expenditure is allocated to groups of patients in each DRG based on measures of average consumption for the patients in each DRG – Relies on the use of service weights • and/or other generalised utilisation statistics. DRG Workshop Belgrade, 18 -22. November 2013.
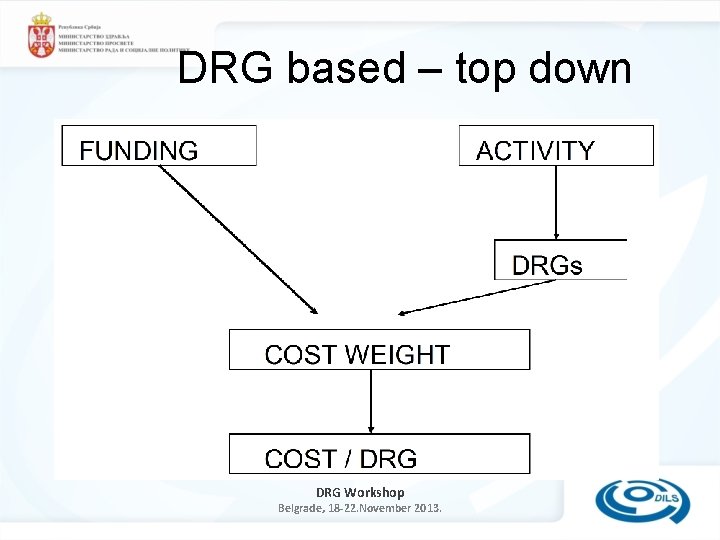
DRG based – top down DRG Workshop Belgrade, 18 -22. November 2013.

Why Patient Costing? • Patient costing provides detail at the individual patient episode – Easier to apply patient costing to other patient types • Patient costing systems are a good data repository – Choice between the methodologies is dependent on information capture DRG Workshop Belgrade, 18 -22. November 2013.

Available costing systems • Most systems, available currently use both methods of costing • More precision is obtained by increasing clinical costing elements • Pure patient costing is not (always) feasible – Feeders can be expensive – Skills are not always available • A hybrid of clinical costing (preferred) and cost modelling (default) is usually the answer. DRG Workshop Belgrade, 18 -22. November 2013.

PLICS UK 2010 hospital survey • • • Over 95 acute organisations have either implemented a PLICS system, or are in the process of implementing a PLICS system. Almost a further 20 acute organisations are planning to implement PLICS in the next few years. Of the 51 organisations who have implemented PLICS, 45 report that they have used PLICS data to inform their 2009/10 reference cost return Nearly 90% of those organisations who have implemented a PLICS system, or are in the process of implementing a PLICS system report that they are using the Acute Clinical Costing Standards. Of those planning not to implement PLICS, 31 are acute providers, with the remainder being PCT, Community, Ambulance and other Take up or planned take of PLICS in the non-acute sector is primarily by Mental Health organisations DRG Workshop Belgrade, 18 -22. November 2013.

Cost allocation process Overhead Allocation Statistics Recurrent Expenditure Allocation Overhead Costs to Patient Care Cost Centres GL costs, FTEs, Floor space Program Fractions Remove non-Inpatient Costs Patient Data DRG Workshop Allocate Final Costs to products Belgrade, 18 -22. November 2013. Inpatient Fractions Outpatients, Teaching and Research Weights/Utilisation

Recurrent Expenditure • General Ledger information • Expenses eg – nursing salaries – medical/surgical supplies – cleaning – drugs • Group these into overhead and patient care cost centres DRG Workshop Belgrade, 18 -22. November 2013.

Overhead Allocation Statistics • Measures or estimates the cost of the services provided by one cost centre to the others • Cleaning costs are often distributed by cleaning staff rosters or floor space • Human Resources – staff headcount DRG Workshop Belgrade, 18 -22. November 2013.

Reciprocal Allocation Method Cleaning Finance Administration Cardiology DRG Workshop Belgrade, 18 -22. November 2013.

Program Fractions / Inpatient Fractions • Remove cost data that doesn’t have patient information eg – Non-inpatient costs – Teaching and research DRG Workshop Belgrade, 18 -22. November 2013.

Allocate Final Costs • Use service weights or utilisation data – Measure of the relative resource utilisation by DRG for patient services where data on actual resource use is not known – Estimated or actual cost and utilisation of service DRG Workshop Belgrade, 18 -22. November 2013.

Results • • Average cost by DRG Estimated cost by patient Detailed service utilisation data by patient Reports give average utilisation of major service type – Average nurse costs – Average medical costs – Average theatre costs – Average drug/imaging/pathology costs DRG Workshop Belgrade, 18 -22. November 2013.

COSTING SOFTWARE • VISASYS – COMBO PRODUCTS – http: //www. visasys. com. au/products. htm • POWER HEALTH SOLUTIONS – PCM – http: //www. powerhealthsolutions. com/products/PPM/Cost. Manager/ • TRENDSTAR – http: //www. yardleyconsulting. com/hospital-cost-accounting/90 -hosptialactivity-based-coting-abc • ECLYPSYS – SUNRISE PRODUCTS – www. eclipsys. com/cb 6 d 5 ab 4 -2 a 9 b-4117 -86 f 8. . . /download. htm • HOME MADE SOLUTIONS – eg SAS based DRG Workshop Belgrade, 18 -22. November 2013.

Let’s look at a costweight report NHCDC PUBLIC COSTWEIGHTS TABLE R 13 Pub. CWest 60. xls http: //www. health. gov. au/internet/main/publishing. nsf/Content/Round_13 -costreports DRG Workshop Belgrade, 18 -22. November 2013.

KEY USES OF PATIENT COST DATA • PRICING AND CASE WEIGHTING • MANAGING EFFICIENCY AND QUALITY OF HOSPITAL SERVICES – BY COMPLETE OUTPUT UNITS – BY INTERMEDIATE PRODUCTS • CLAIMS OPTIMISATION DRG Workshop Belgrade, 18 -22. November 2013.

The relationship between costs and price • Cost is ONE input into price considerations • Average cost, median cost, marginal cost can all be considered. • Variable, fixed and variable or full economic cost may be relevant for different purposes. • BASIC PRICE IS – BUDGET/ACTIVITY – for public hospitals – MARKET QUOTE – for private sector DRG Workshop Belgrade, 18 -22. November 2013. providers purchasers

THANKS QUESTIONS? DRG Workshop Belgrade, 18 -22. November 2013.
- Slides: 44