Functional Design for Mobilisation and Ergonomics Agenda Arjo

Functional Design for Mobilisation and Ergonomics

Agenda Arjo. Huntleigh Philosophy Architect Guidebook • Preventable • Planning with the Guidebook • Positive Eight • By the bed • Mobility Gallery • In the toilet area • In the bath/in the shower • Care environment for the bariatric patient Work related injuries • The soiled utility room Safe Patient Handling & Mobility • Corridors, storage space and turning radii • Design for quality of care for now and in the future Falls in care facilities Page 2

Preventing Avoidable Pain & Costs by Safely Mobilising the Patient Page 3
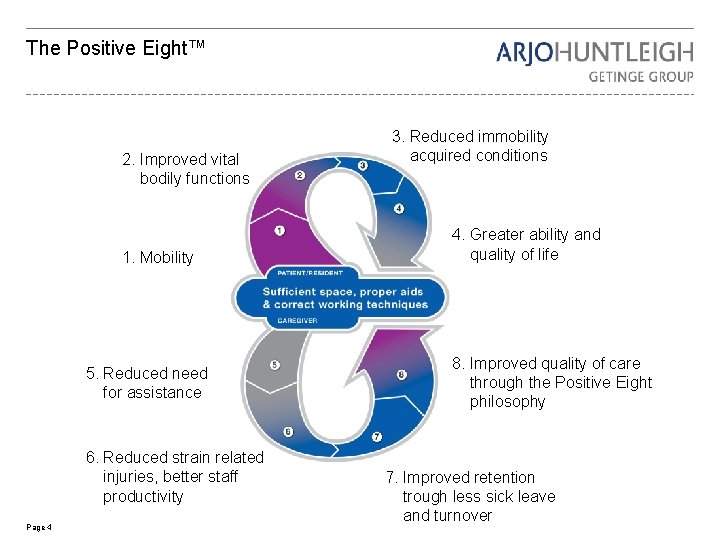
The Positive Eight™ 2. Improved vital bodily functions 1. Mobility 5. Reduced need for assistance 6. Reduced strain related injuries, better staff productivity Page 4 3. Reduced immobility acquired conditions 4. Greater ability and quality of life 8. Improved quality of care through the Positive Eight philosophy 7. Improved retention trough less sick leave and turnover

"We use the patient's abilities in order to stimulate their mobility" Page 5
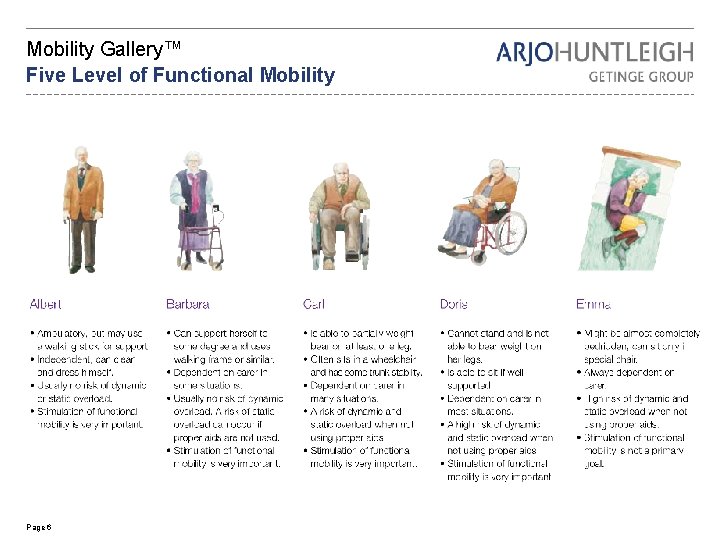

Mobility Gallery™ Five Level of Functional Mobility Page 6
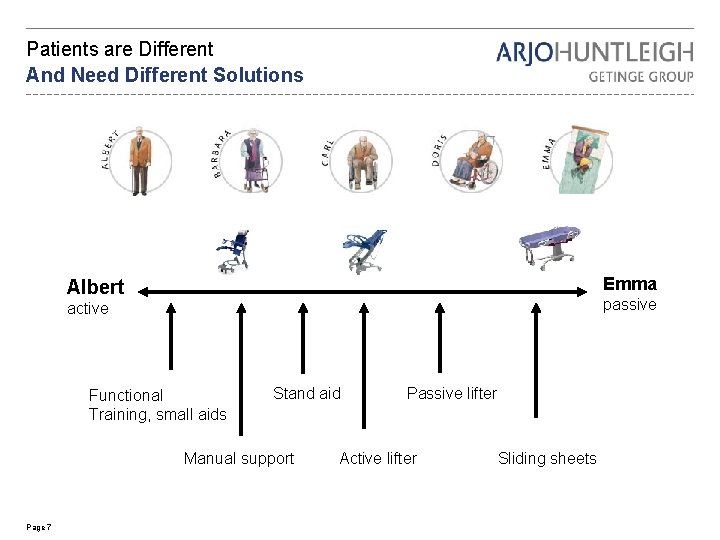
Patients are Different And Need Different Solutions Emma Albert passive active Functional Training, small aids Stand aid Manual support Page 7 Passive lifter Active lifter Sliding sheets

FALLS IN CARE FACILITIES are preventable

Falls Prevention A Safety and Economic Priority Patient falls are the most common serious occurrences reported in hospitals and elderly care facilities* Patient Outcome • 35% of patients who fall in healthcare facilities suffer an injury** • Resulting in distress, pain, injury, loss of confidence, reduced mobility and loss of independence Healthcare Costs • Falls with serious injury increase the length of hospital stays by 6. 9 days and hospital charges by $13, 806 Page 9 * Haley et. al. Falls in English and Welsh hospitals, Qual Saf Health Care 2008; 17: **. Joint Commission, It’s a Long Way Down: Reducing the Risk of Patient Falls retrieved from on January 18, 2011 web

Resident/Patient Falls In the Bathroom • The bathroom area and a wet floor in the bathroom have shown to be important risk factors with regard to patient falls* ** • Approx. 235, 000 adults in the US visit emergency rooms every year because of fall injuries caused in the bathroom. *** • More than 30% of those injuries happen while bathing, showering or getting out of the bath or shower*** Page 10 • Vu MQ et al. , J Am Med Dir Assoc, 6(3 Suppl) (2005). • Cameron ID et al. . Cochrane Database Syst Rev(1): CD 005465: (2010). *** Centers for Disease Control and Prevention (CDC) US, 2008 Weekly June 10, 2011 / 60(22)
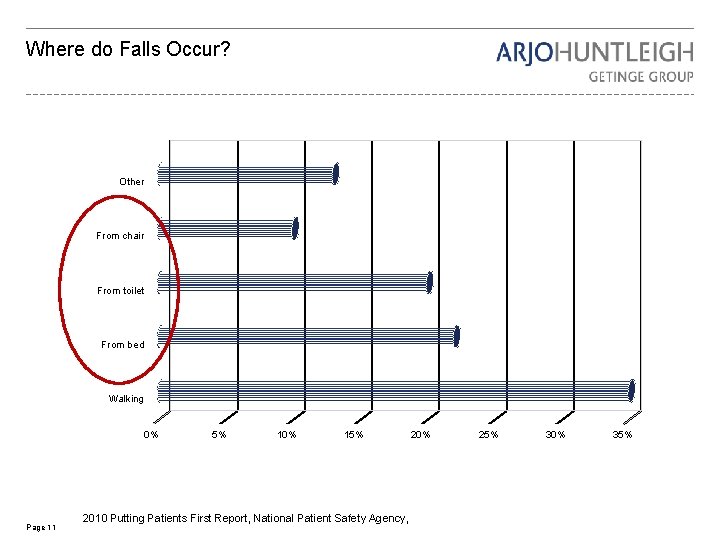
Where do Falls Occur? Other From chair From toilet From bed Walking 0% Page 11 5% 10% 15% 2010 Putting Patients First Report, National Patient Safety Agency, 20% 25% 30% 35%

Prevent Falls Assess Patient Mobility Level and Mental Status To decide on: • method of transferring the patient – what type of aid to use • continent status/toileting method • choice on personal hygiene method – showering/bathing or washing in bed • bed requirement and configuration • seating – what type of chair/wheelchair to use Page 12

Prevent Falls Environmental Factors Bathroom • grips and handles (availability and place) • transfer method available for toileting • toilet height • transfer method in/out bathtub • shower chair/seat • access to the bathroom & shower area Bed • side rails (function and use) • brakes • under bed light • the bed to be in low position when patients are unattended • ensure bed features are used to alert caregivers of unsafe conditions Page 13

Work related injuries are preventable

Health Care Workers Are at Great Risk Healthcare staff are subject to some of the greatest risk of musculoskeletal disorders (MSD) and injuries at work – causing: • • long term injuries absence from work staff turnover increased costs to healthcare providers • litigation and insurance claims Page 15 i. SO/TR 12296: 2012

Every day a caregiver is lifting 2 000 kg Page 16

Musculoskeletal Injuries Can be Prevented Greater risk of musculoskeletal injury is associated with: * ** - higher job strain - more frequent patient handling - lack of patient lifters The daily number of patient handling tasks provides the most direct measure for assessing the risk of back pain. 40% of staff injuries could have been prevented by using lifters*** Page 17 * Collins J et al. Rehabilitation Nursing, (2010): 35(6) ‘’ Thomas D, Thomas Y, Borner H et al (2009). Patient handling guidelines: literature review. Wellington ACC. *** Pompeii L. , et al. , American Journal of Industrial medicine; (2009) 52:

Safe Patient Handling The use of patient handling equipment, prevents staff injuries by decreasing work load. In additional the use of appropriate patient handling and mobility equipment: • Save time (direct and indirect)* • Save costs (costs for workers injuries and illness, pressure ulcers and patient falls)** • Increased patient mobility, the patient gets out of bed which increases health and reduces the risk for complications*** • Decrease the number of pressure ulcers (the more frequently the patient is moved, the less risk for pressure ulcers)*** Page 18 • Alamgir H, et al. Injury 40, no. 9 , 2009 ** Chhokar R et al. , Appl Ergon 36, no. 2, Mar 2005. *** Gucer PW et al, J Occup Environ Med. Jan; 55(1) 2013

Safe Patient Handling & Mobility • Is efficient – safe time • Reduce work related injuries • Increase patient quality of care (reduce pressure ulcers) • Increase patient mobility by reducing bed fastness • Is cost effective Page 19

Safe Patient Handling & Mobility To Achieve Success you Need to Assess • • Page 20 Patient – mobility level and mental status etc. Environment & space requirement Type and frequency of tasks Equipment availability - how they are used, installed and maintained

Architect Guidebook for Architect and Planners Functional Design for Mobilisation and Ergonomics Page 21

Architect Guidebook for Architect and Planners Functional Design for Mobilisation and Ergonomics • 4 th edition published June 2014 • Since first edition 1996, 30. 000 copies in 15 languages • Edited by experts, and reviewed by an international expert group of architects, ergonomists, nurses and patients • Strong links to CEN / ISO TR 12296 -2013 Ergonomics- Manual Handling of People in the Healthcare Sector • Applicable for all healthcare facilities with general care provided by 1 -2 caregivers, (excluding special wards) • Fresh new graphic design • Edited content and extensively re-written bariatrics (Plus-sized people) section • Extensive reference list Supported by web-tools – assessments and CAD drawings. Page 22

Architect Guidebook Table of Content Planning strategies Planning with the functional Guidebook The Positive Eight philosophy The patient/resident The caregivers Planning approaches for mobility support Applying concepts By the bed In the toilet area In the bath/in the shower Care environment for the bariatric patient The soiled utility room Corridors and elevators Storage space and turning radii Realising efficient care Summary & conclusion References Page 23

Planning with the Guidebook Functional Space for Safe Patient Handling and Mobilisation • Bird’s eye view images in combination with l plan drawings • Right-angled working areas • Smallest working areas • No ‘ideal’ room layout Turquoise area shows the minimum working area required from one side. Light turquoise area shows required extension of working area to facilitate activities from either side. Page 24
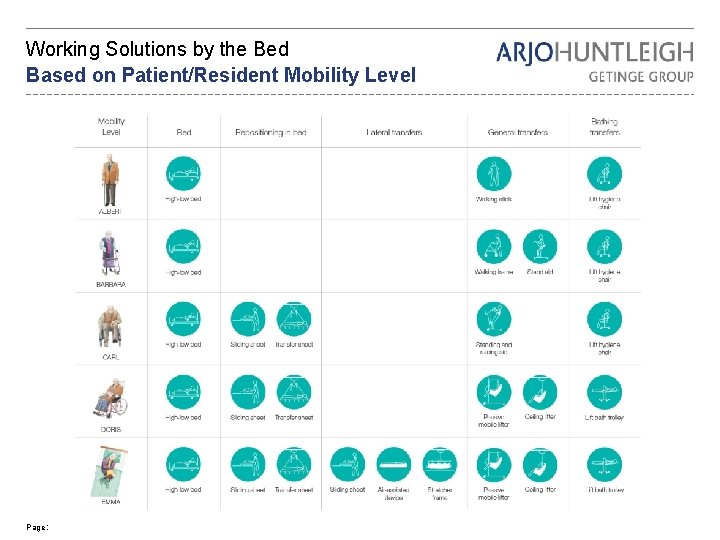
Working Solutions by the Bed Based on Patient/Resident Mobility Level Page 25

Space Requirements by the Bed Page 26
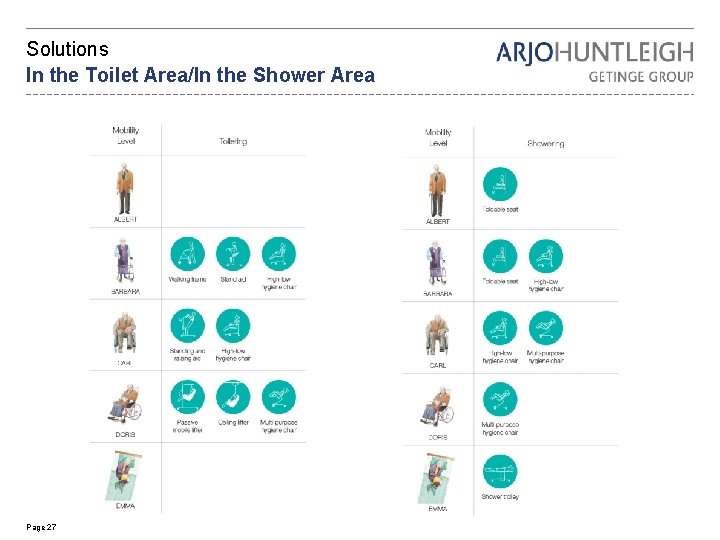
Solutions In the Toilet Area/In the Shower Area Page 27
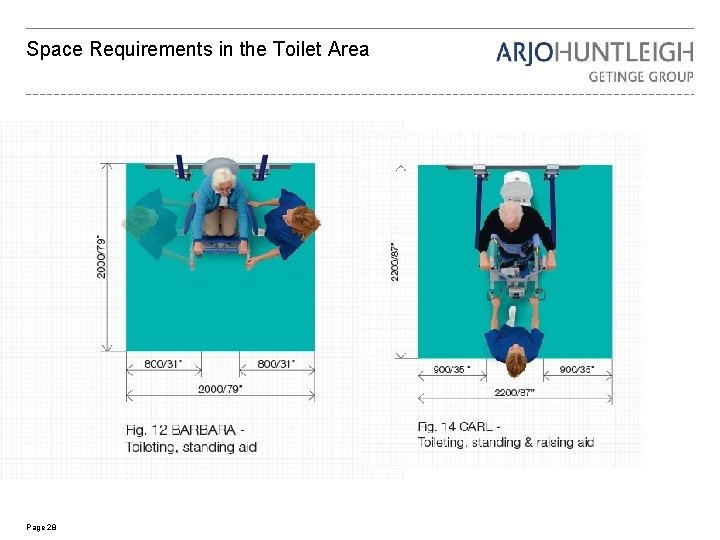
Space Requirements in the Toilet Area Page 28

Space Requirements in the Shower Area Page 29

Bathing Solutions Page 30
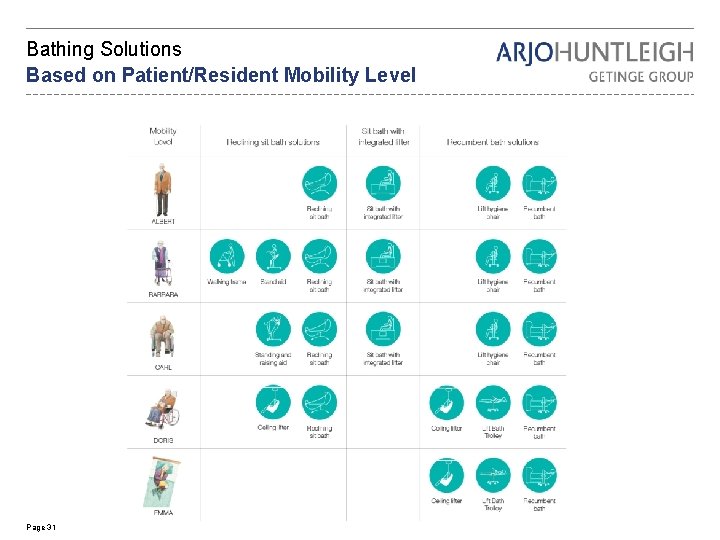
Bathing Solutions Based on Patient/Resident Mobility Level Page 31

Care Environment for the Bariatric Patient Increasing number of bariatric patients • BMI over 40 • Overweight > 45 kg (100 lbs) • Weight is greater than 136 kg (300 lbs) • The patient’s size or shape is not compatible with standard equipment In the Guidebook • Evidence based principles for space and environmental planning • Algorithms for the number of caregivers per mobility/activity/ chosen equipment • Solution grid per mobility level • Practical design tips Page 32

Solutions for the Bariatric Patients Page 33
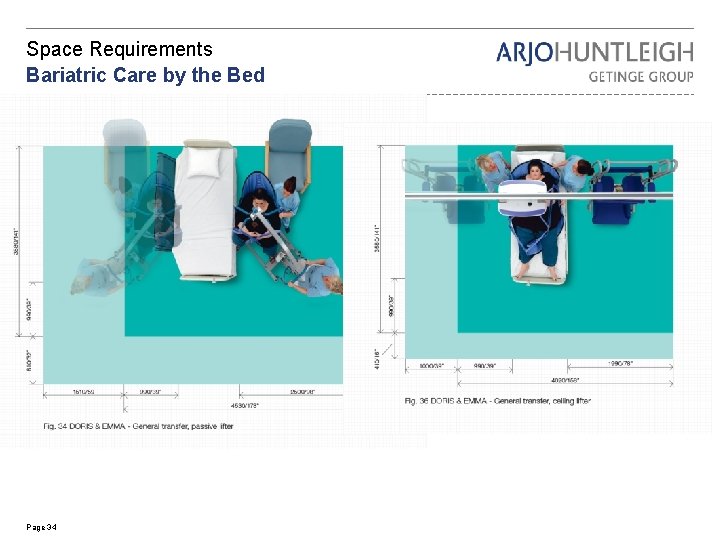
Space Requirements Bariatric Care by the Bed Page 34

Space Requirements Bariatric Care in the Toilet and Shower Area Page 35

Facility Planning for the Bariatric Patient Check List • Doorways with • Elevator capacity • weight of a bariatric patient, equipment, and two to three caregivers • Hazardous pathways? • If the usual pathway is restricted • alternative route • • Flooring capacity Size/weight limits to been identified for all equipment, furniture and fixtures? Ceiling structure needs to meet the specifications 10% of the seating provided in clinical and visitor areas should meet bariatric specifications • Suitable bariatric bathroom facilities Is an effective communication system or process in place to share the information? Page 36

The Soiled Utility Room – Four Cornerstones 1. 2. 3. 4. Page 37 Collection point for soiled goods Hand washbasin Flusher disinfector Storage space for clean goods
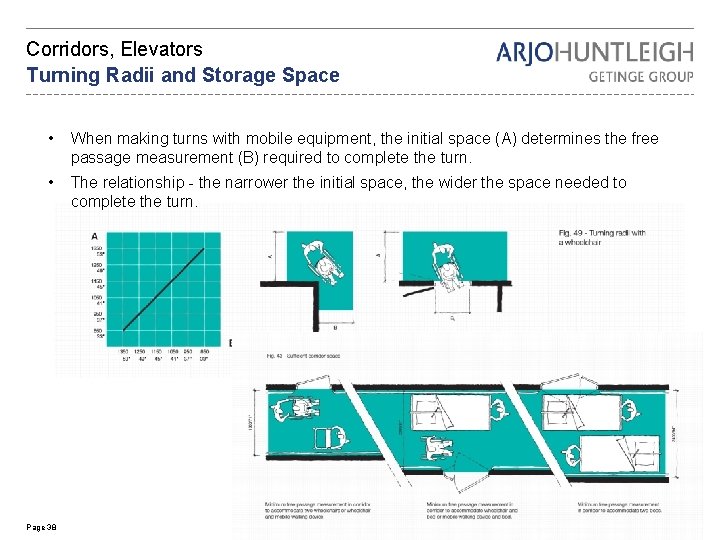
Corridors, Elevators Turning Radii and Storage Space • When making turns with mobile equipment, the initial space (A) determines the free passage measurement (B) required to complete the turn. • The relationship - the narrower the initial space, the wider the space needed to complete the turn. Page 38

Design for Quality of Care for Now and in the Future • Appoint a strong multi-disciplinary project team • Get a good picture of the patient today and plan for “tomorrow” • Working towards a new work environment • A cultural change • Visualisation of the effect of change over time • Measuring financial impact Page 39

‘Anyone involved in planning of the care process of patient handling can benefit from this Guidebook…’ ‘As an architect who has become increasingly interested in the relationship between human factors and ergonomics and design, this book is an invaluable resource for designing healthcare environments. Being able to understand the interaction of the space with the intended function, for both caregivers and patients with differing abilities and needs, is paramount for architects and designers to provide the best solutions. The graphic nature of the diagrams make the recommendations easy to understand implement. This is a must have on any reference shelf. ’ Ellen Taylor, AIA MBA EDAC, United States Page 40

Questions? Thank you! Page 41
- Slides: 41