Frailty Craig Bowman Frailty Practitioner Vale of Leven

Frailty Craig Bowman Frailty Practitioner Vale of Leven Hospital August 2019

‘Frailty’ …? ¢ Is it inevitable?

‘Frailty’ …? ¢ ‘Frailty is a distinctive health state related to the ageing process in which multiple body systems gradually lose their in-built reserves’ (BGS, 2017) ¢ ‘Frailty is the inability to withstand illness without loss of function’ (Prof. G. Ellis)
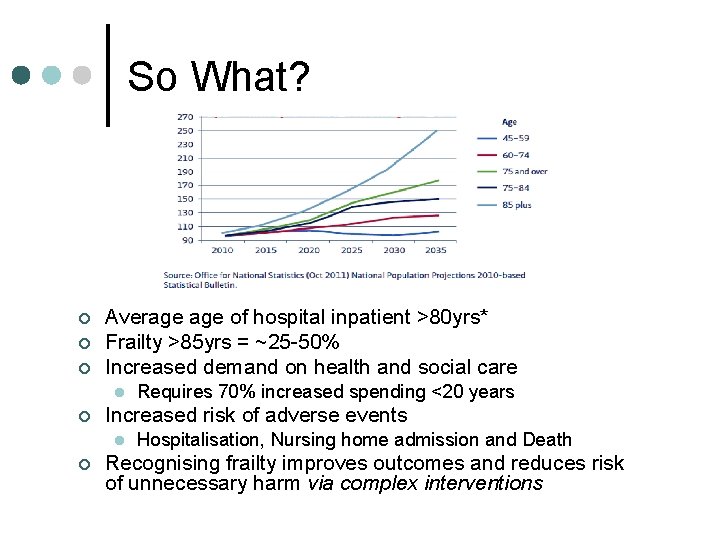
So What? ¢ ¢ ¢ Average of hospital inpatient >80 yrs* Frailty >85 yrs = ~25 -50% Increased demand on health and social care l ¢ Increased risk of adverse events l ¢ Requires 70% increased spending <20 years Hospitalisation, Nursing home admission and Death Recognising frailty improves outcomes and reduces risk of unnecessary harm via complex interventions

Scottish Government Priorities ¢ ¢ ¢ ¢ 2020 Vision l ‘Live longer healthier lives at home or in a homely setting’ l ‘focus upon prevention, anticipation and supported self-management’ l ‘Ensure people get back home as soon as appropriate, with minimal risk of readmission’ Quality Strategy l Shared decision-making about care l Personalised care plans for those people with the most complex care and support needs National Clinical Strategy l Focus upon early discharge planning l Facilitate access to Comprehensive Geriatric Assessment Scotland’s National Dementia Strategy l People can take part in their own care planning l People are enabled to live well and safely at home or in a homely setting l Input of family carers is encouraged and carers’ own needs are recognised 18% increase in emergency admissions of older people between 2011 - 2015 (6% higher than av. population) £ 820 m estimated cost to the NHS of older patients in hospital beds no longer requiring acute treatment (2. 7 million bed days lost) 54% hospital staff believe discharge planning is not started soon enough for older patients

Think Frailty ¢ Healthcare Improvement Scotland (2012); l ¢ Evidence/Service review; l l ¢ ‘improve acute care for older people by March 2014’ Identified areas for improvement Delirium often undetected = poorer outcomes Older People in Acute Care (OPAC); l l l Timely Comprehensive Geriatric Assessment (CGA) Input from a specialist team <24 hrs of admission Improve identification/management of delirium

Identifying Frailty ¢ ¢ Phenotype Model/Cumulative Deficit Model Frail patients commonly present with one or more ‘Frailty Syndromes’ (Geriatric Giants); Falls l Immobility l Delirium l Incontinence l Susceptibility to medication side effects BGS Fit for Frailty; l TUAG: >10 s to complete l Gait Speed: >5 s to walk 4 m +/- walking aid l PRISMA 7 Questionnaire: ‘yes’ 3 or more l ¢

Frailty Tool ¢ ¢ ¢ Frailty Screening Tool Developed by OPAC Trigger earlier interventions Currently ‘another bit of paper’ Plans; mandatory on Trak. Care ≥ 75 rys

Frailty Practitioner ¢ ¢ Established frailty teams in Glasgow; l Front door/Unscheduled care l Frailty Nurses l ECANs/ECONs l OAU New role at VOL; Nursing/AHPs Aims; l Identify frailty l Facilitate CGA l Improve hospital journey/quicker discharge Role development; improve autonomy of patient management

Comprehensive Geriatric Assessment (CGA) ¢ ¢ ¢ Recognised as the gold standard in management of frailty for older people Detailed process to identify an individuals health within a number of areas; l Physical l Socioeconomic/Environmental l Functional l Mobility/Balance l Psychological l Medication review Healthcare Improvement Scotland: https: //ihub. scot/media/2455/frailty-and-falls-assessment-andintervention-tool-poster. pdf

Rockwood CFS, Dalhousie University ¢ ¢ ¢ Measures frailty based on clinical assessment Ranges 1 - 9 based upon level of functional independence Agreed to be used in community teams across NHS GG&C, scores accessible within e. KIS

Living Well in the Communities Portfolio ¢ ¢ ¢ May 2019; Living and Dying Well with Frailty Collaborative Health and Social Care Partnership and GP Clusters Aims Oct 2020; l l l 10% reduction hospital bed days >65 yrs 10% reduction unscheduled GP home visits >65 yrs 20% increase of Anticipatory Care Plans (ACPs) for people living with frailty

Future of Frailty ¢ Local; l l ¢ Improve identification Local service improvement MIU/MAU signposting Rockwood Pictorial Self-Ax. National; l l Prevention/Anticipatory Care Phase 2 Frailty at the Front Door MFT e. FI

¢ ¢ ¢ ¢ ¢ Prof G Ellis, 2017, https: //ihub. scot/media/2661/20170825 -frailty-plenaryv 06. pdf BGS, 2014, https: //www. bgs. org. uk/sites/default/files/content/resources/files/201805 -23/fff_full. pdf NAO, 2016, https: //www. nao. org. uk/wpcontent/uploads/2015/12/Discharging-older-patientsfrom-hospital-Summary. pdf ONS, 2011, https: //www. ons. gov. uk/peoplepopulationandcommuni ty/populationandmigration/populationprojections/bullet ins/nationalpopulationprojections/2011 -10 -26 Staff. Net, http: //www. nhsggc. org. uk/media/223612/Medical%20 Treatments%20 and%20 AWIA. pdf Office of the Public Guardian, 2015, http: //www. publicguardian-scotland. gov. uk/ Scot Gov, 2011, https: //www. gov. scot/Topics/Health/Policy/2020 -Vision Scot Gov, 2012, https: //www. gov. scot/Topics/Health/Policy/Quality. Strategy Scot Gov, 2016, https: //www. gov. scot/Publications/2016/02/8699 Scot Gov, 2017, https: //www. gov. scot/Publications/2017/06/7735
- Slides: 14