Fractures and Dislocations about the Shoulder in the

Fractures and Dislocations about the Shoulder in the Pediatric Patient Christopher Bray, MD Original Author: Michael Wattenbarger, MD; March 2004 1 st Revision: Steven Frick, MD; August 2006 2 nd Revision: Joshua Klatt, MD; December 2009 3 rd Revision: Christopher Bray, MD; March 2014

Shoulder Trauma • • • Shoulder trauma is relatively uncommon Usually easy to diagnose and treat Rarely require reduction or open treatment Great remodeling potential Motion of shoulder joint compensates well Must differentiate the serious injury from mild! Bishop & Flatow: Pediatric Shoulder Trauma. CORR 432: 41 -8, 2005.

Shoulder Region Fractures. Indications for Open Reduction • • Open fractures Displaced intraarticular fractures Multiple trauma to facilitate rehabilitation Severe displacement with suspected soft tissue interposition
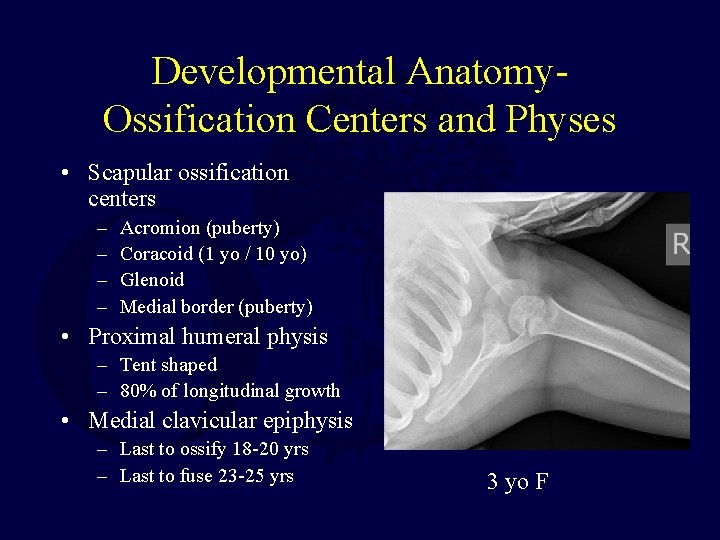
Developmental Anatomy. Ossification Centers and Physes • Scapular ossification centers – – Acromion (puberty) Coracoid (1 yo / 10 yo) Glenoid Medial border (puberty) • Proximal humeral physis – Tent shaped – 80% of longitudinal growth • Medial clavicular epiphysis – Last to ossify 18 -20 yrs – Last to fuse 23 -25 yrs 3 yo F
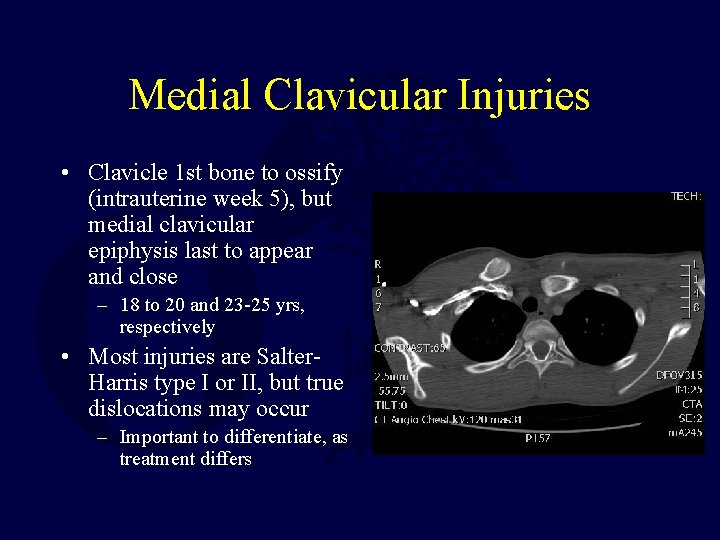
Medial Clavicular Injuries • Clavicle 1 st bone to ossify (intrauterine week 5), but medial clavicular epiphysis last to appear and close – 18 to 20 and 23 -25 yrs, respectively • Most injuries are Salter. Harris type I or II, but true dislocations may occur – Important to differentiate, as treatment differs
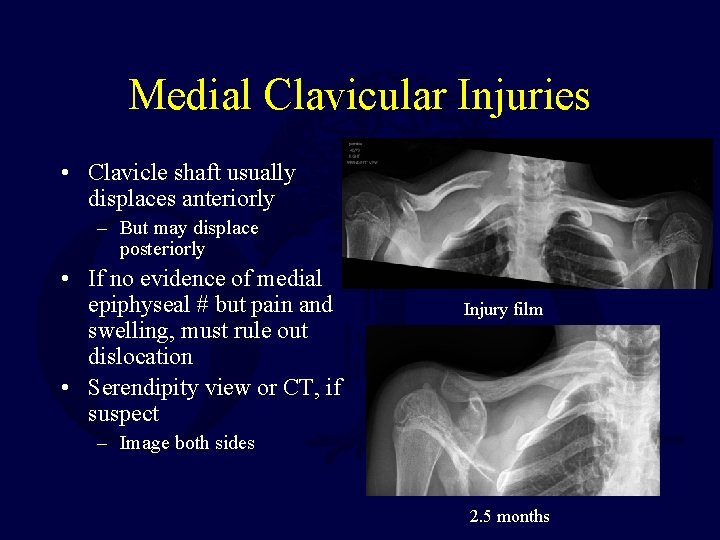
Medial Clavicular Injuries • Clavicle shaft usually displaces anteriorly – But may displace posteriorly • If no evidence of medial epiphyseal # but pain and swelling, must rule out dislocation • Serendipity view or CT, if suspect Injury film – Image both sides 2. 5 months
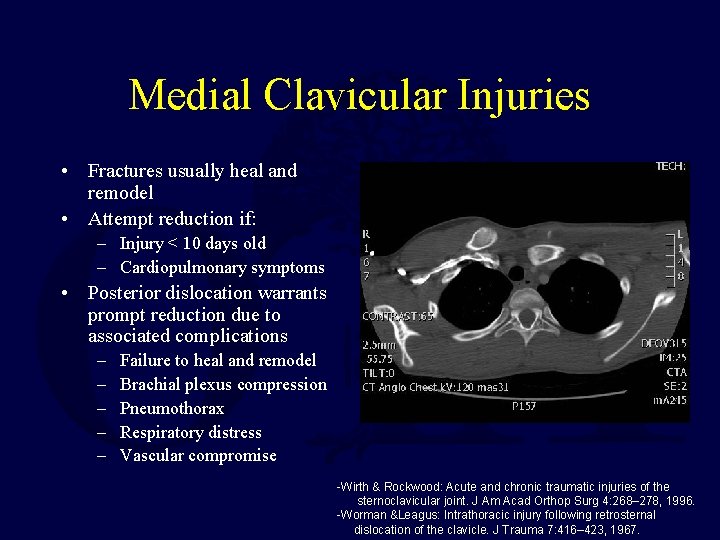
Medial Clavicular Injuries • Fractures usually heal and remodel • Attempt reduction if: – Injury < 10 days old – Cardiopulmonary symptoms • Posterior dislocation warrants prompt reduction due to associated complications – – – Failure to heal and remodel Brachial plexus compression Pneumothorax Respiratory distress Vascular compromise -Wirth & Rockwood: Acute and chronic traumatic injuries of the sternoclavicular joint. J Am Acad Orthop Surg 4: 268– 278, 1996. -Worman &Leagus: Intrathoracic injury following retrosternal dislocation of the clavicle. J Trauma 7: 416– 423, 1967.
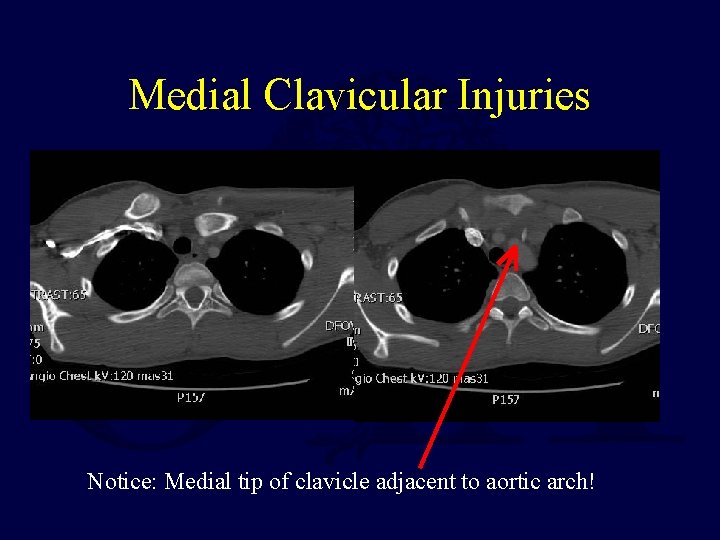
Medial Clavicular Injuries Notice: Medial tip of clavicle adjacent to aortic arch!
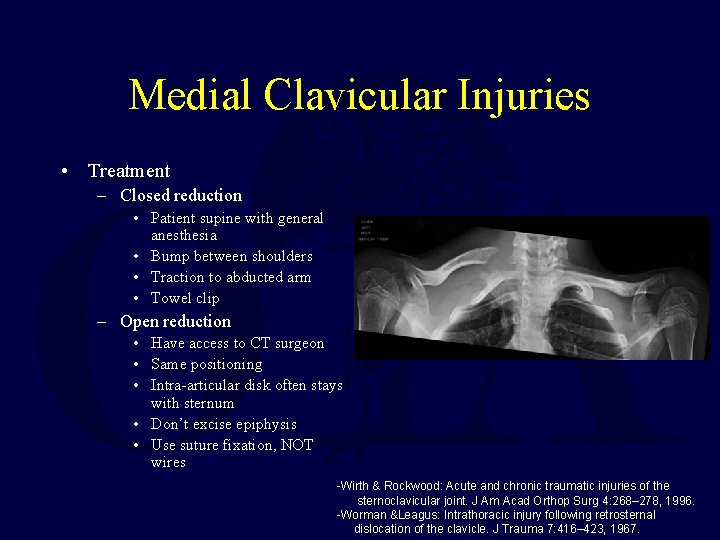
Medial Clavicular Injuries • Treatment – Closed reduction • Patient supine with general anesthesia • Bump between shoulders • Traction to abducted arm • Towel clip – Open reduction • Have access to CT surgeon • Same positioning • Intra-articular disk often stays with sternum • Don’t excise epiphysis • Use suture fixation, NOT wires -Wirth & Rockwood: Acute and chronic traumatic injuries of the sternoclavicular joint. J Am Acad Orthop Surg 4: 268– 278, 1996. -Worman &Leagus: Intrathoracic injury following retrosternal dislocation of the clavicle. J Trauma 7: 416– 423, 1967.

Diaphyseal Clavicle Fxs • Most common fx of shoulder in children – 10 -15% of all fractures • 50% are in children <10 yrs • Almost always heal, usually clinically insignificant malunion – Possible role for operative management if significantly shortened or displaced • Excellent remodeling within 1 year • Complications very uncommon
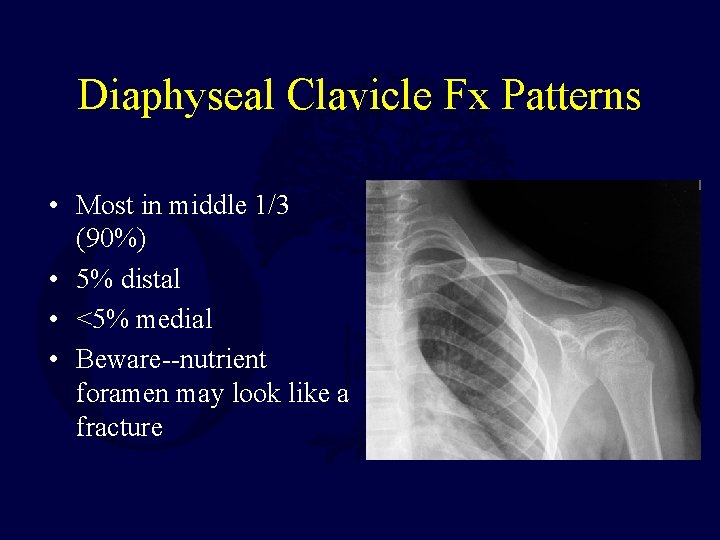
Diaphyseal Clavicle Fx Patterns • Most in middle 1/3 (90%) • 5% distal • <5% medial • Beware--nutrient foramen may look like a fracture
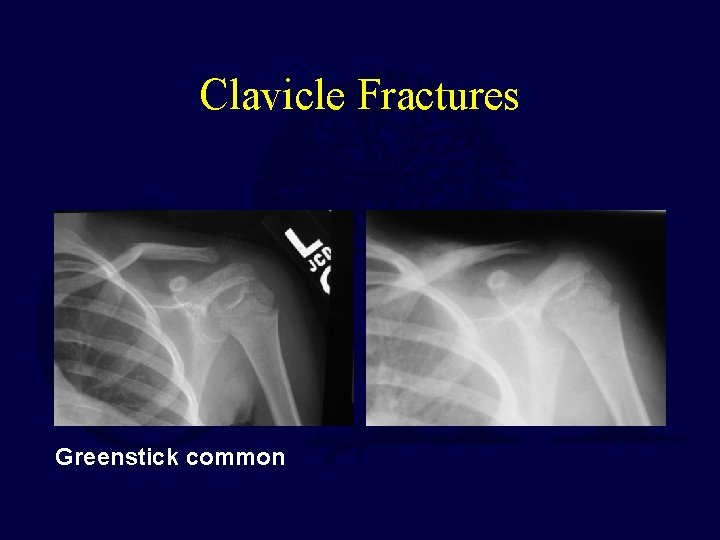
Clavicle Fractures Greenstick common
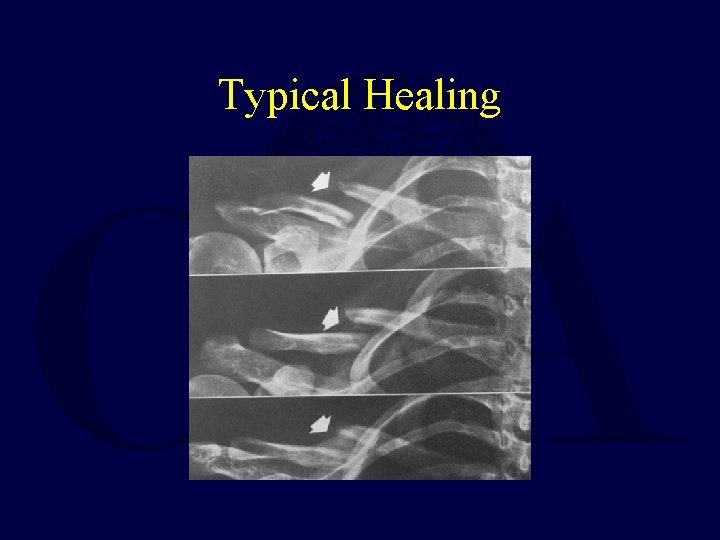
Typical Healing
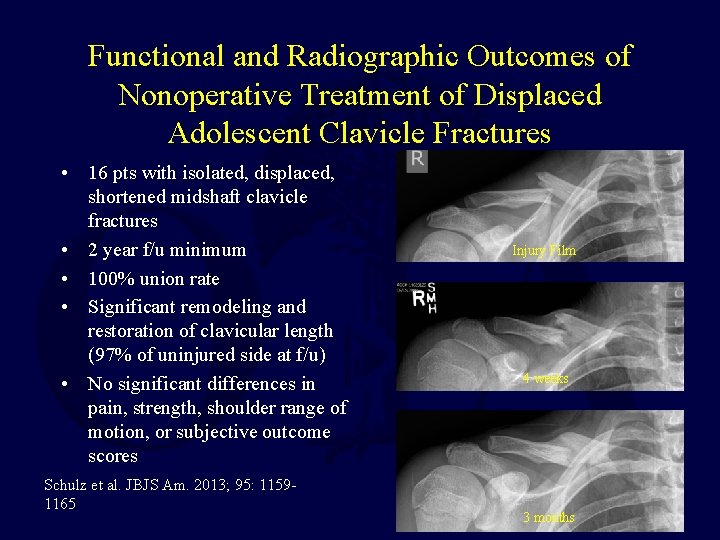
Functional and Radiographic Outcomes of Nonoperative Treatment of Displaced Adolescent Clavicle Fractures • 16 pts with isolated, displaced, shortened midshaft clavicle fractures • 2 year f/u minimum • 100% union rate • Significant remodeling and restoration of clavicular length (97% of uninjured side at f/u) • No significant differences in pain, strength, shoulder range of motion, or subjective outcome scores Schulz et al. JBJS Am. 2013; 95: 11591165 Injury Film 4 weeks 3 months

Adolescent Clavicle Fractures • ORIF may be indicated if widely displaced or shortened • Adult literature supports ORIF for completely displaced fractures • No consensus with pediatric patients yet Canadian Ortho Trauma Society. Nonop treatment compared with plate fixation of displaced midshaft clavicle fxs. JBJS-Am 89(1): 1 -10, 07. Vander Have et al. Op vs Nonop Tx of Midshaft Clav # in Adolescents POSNA 2009 Paper Presentation, Boston, MA
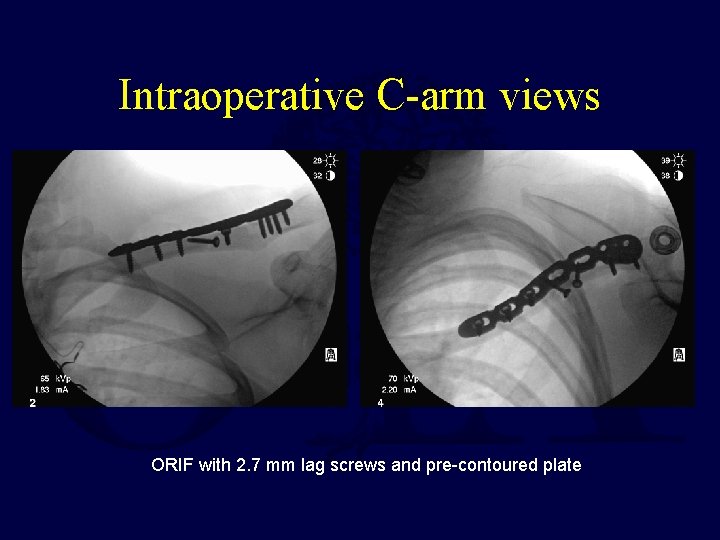
Intraoperative C-arm views ORIF with 2. 7 mm lag screws and pre-contoured plate

High energy displaced clavicle fractures in adolescents • Good results reported with ORIF – also report good results with ORIF of nonunion/malunion for those failing nonoperative care – Vanderhave POSNA 2009

Operative Versus Nonoperative Treatment of Midshaft Clavicle Fractures in Adolescents • 43 displaced clavicle • Differences – Return to activities fractures • 12 weeks operative • 25 nonoperative • 16 weeks • 18 operative nonoperative – Symptomatic hardware • All fractures united Vander Have et al. JPO 2010; 30: 307 -312. requiring removal (3/18) – Symptomatic malunion requiring corrective osteotomy (5/25)
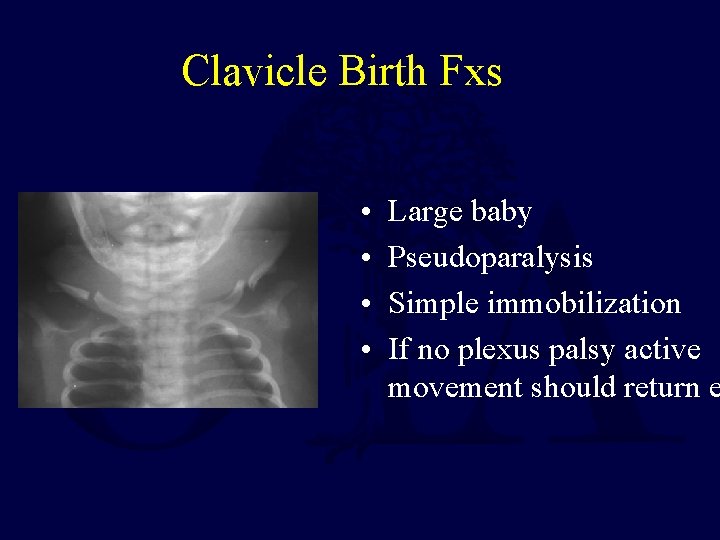
Clavicle Birth Fxs • • Large baby Pseudoparalysis Simple immobilization If no plexus palsy active movement should return e
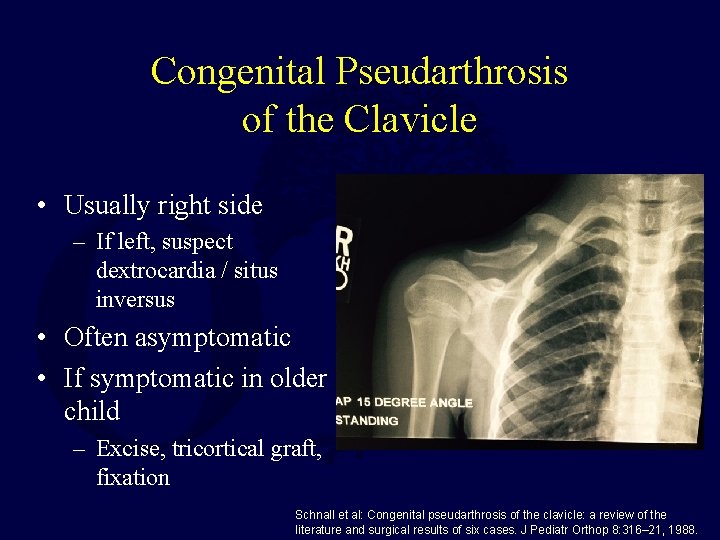
Congenital Pseudarthrosis of the Clavicle • Usually right side – If left, suspect dextrocardia / situs inversus • Often asymptomatic • If symptomatic in older child – Excise, tricortical graft, fixation Schnall et al: Congenital pseudarthrosis of the clavicle: a review of the literature and surgical results of six cases. J Pediatr Orthop 8: 316– 21, 1988.
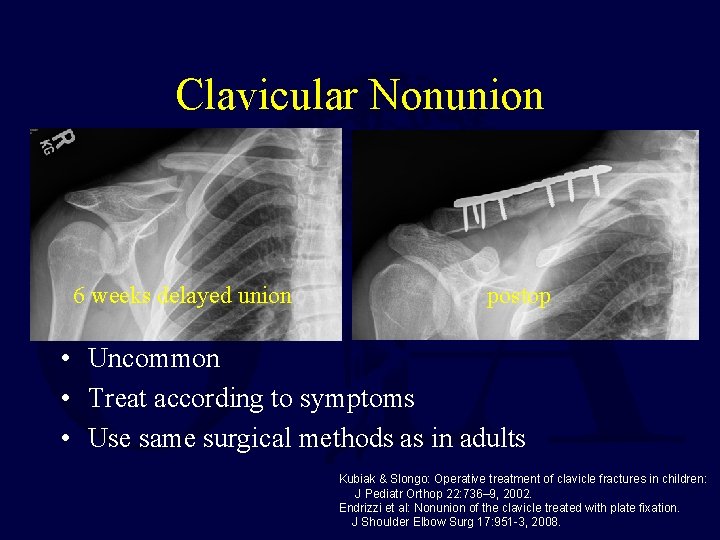
Clavicular Nonunion 6 weeks delayed union postop • Uncommon • Treat according to symptoms • Use same surgical methods as in adults Kubiak & Slongo: Operative treatment of clavicle fractures in children: J Pediatr Orthop 22: 736– 9, 2002. Endrizzi et al: Nonunion of the clavicle treated with plate fixation. J Shoulder Elbow Surg 17: 951 -3, 2008.
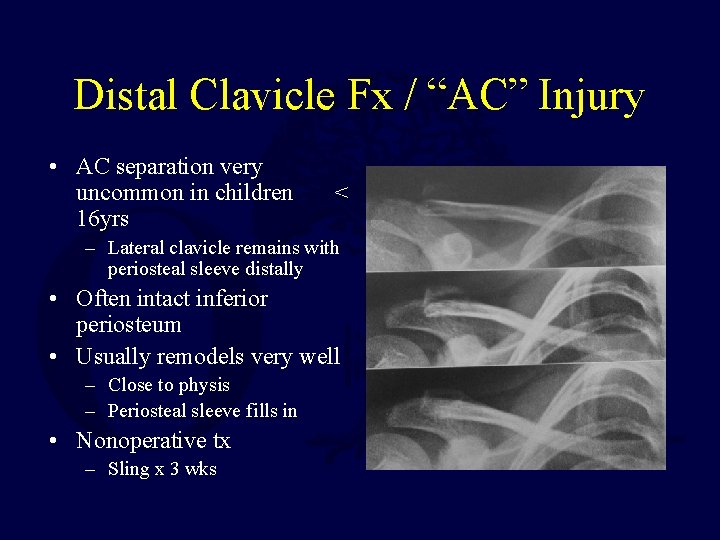
Distal Clavicle Fx / “AC” Injury • AC separation very uncommon in children 16 yrs < – Lateral clavicle remains with periosteal sleeve distally • Often intact inferior periosteum • Usually remodels very well – Close to physis – Periosteal sleeve fills in • Nonoperative tx – Sling x 3 wks
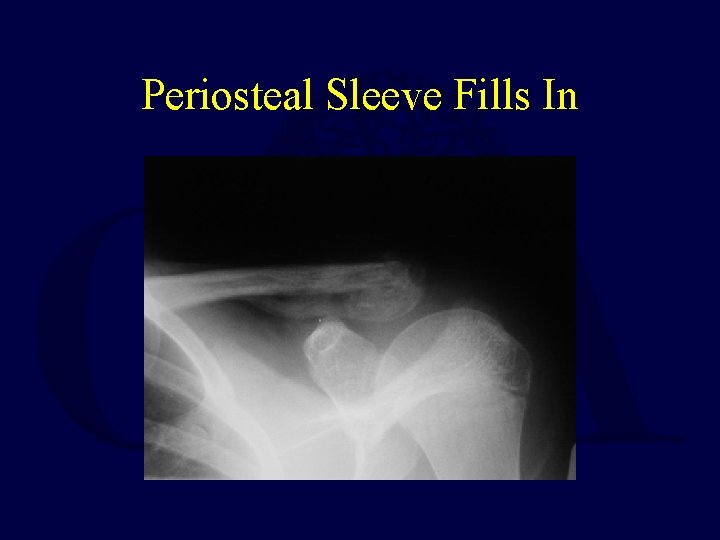
Periosteal Sleeve Fills In

Type IV AC Dislocation 11 yo female Ped vs car
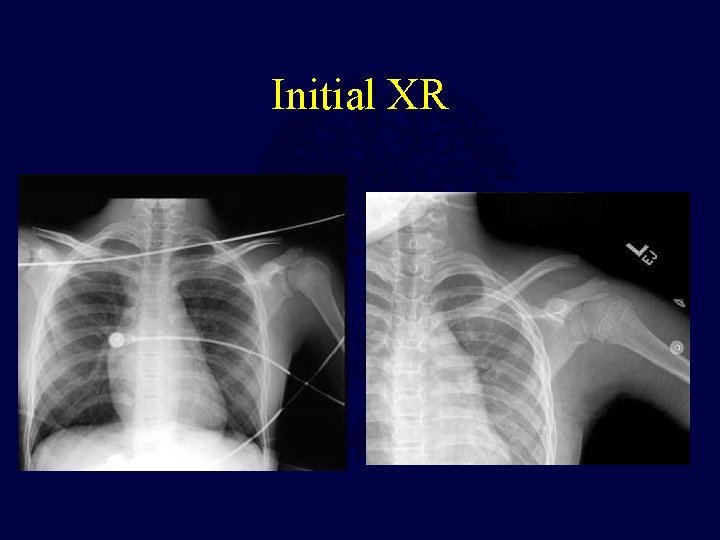
Initial XR
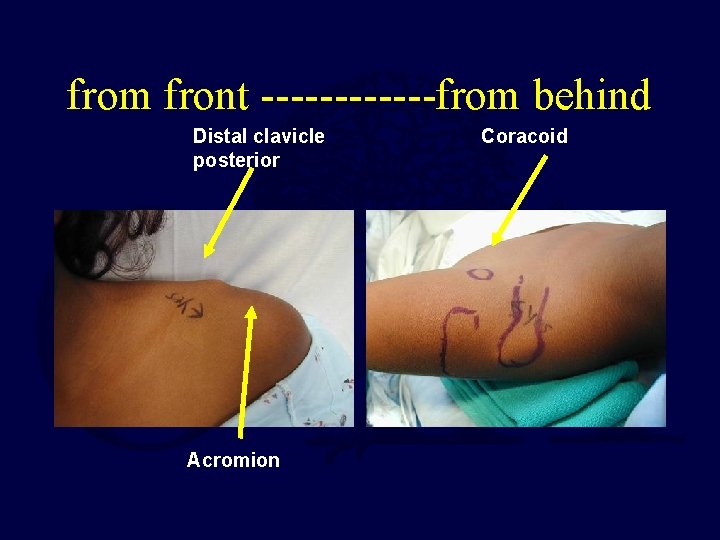
from front ------from behind Distal clavicle posterior Acromion Coracoid
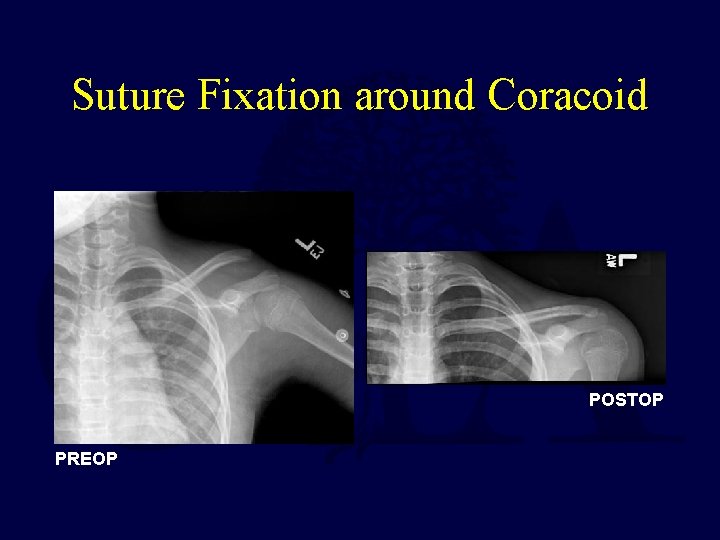
Suture Fixation around Coracoid POSTOP PREOP
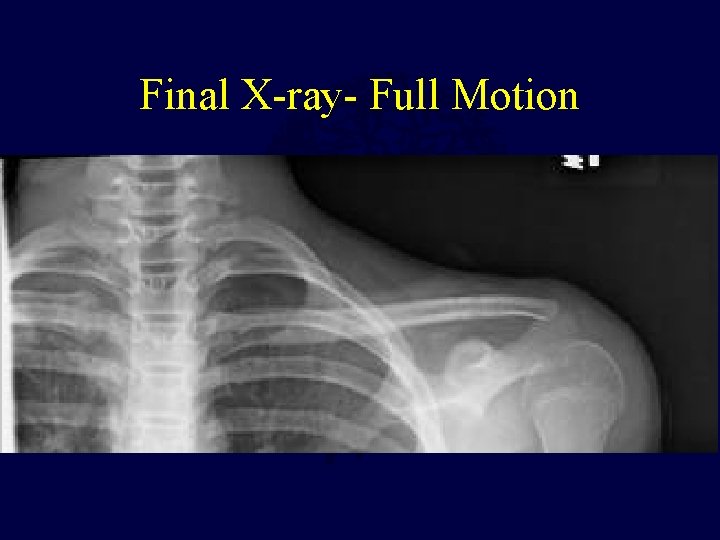
Final X-ray- Full Motion
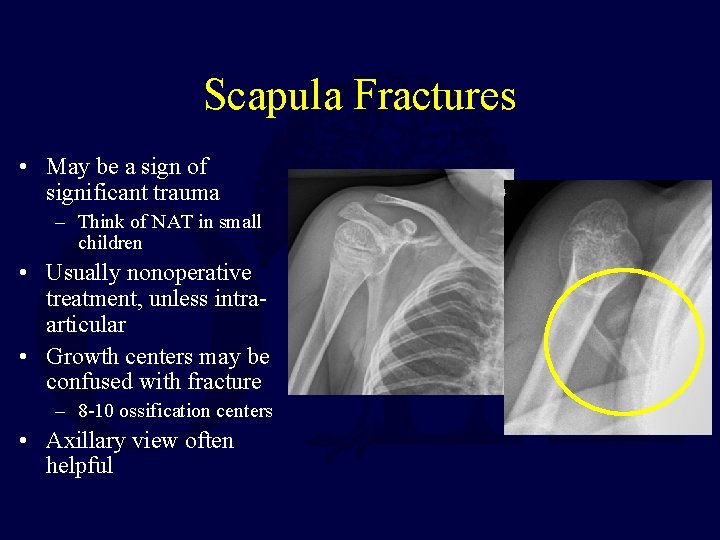
Scapula Fractures • May be a sign of significant trauma – Think of NAT in small children • Usually nonoperative treatment, unless intraarticular • Growth centers may be confused with fracture – 8 -10 ossification centers • Axillary view often helpful
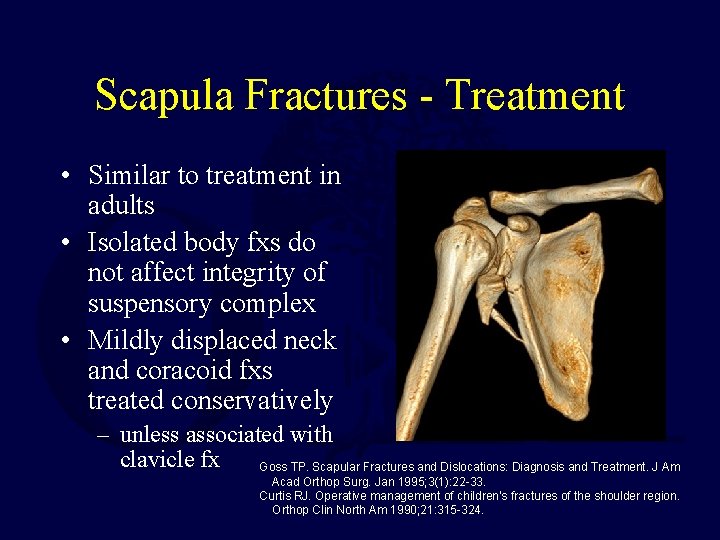
Scapula Fractures - Treatment • Similar to treatment in adults • Isolated body fxs do not affect integrity of suspensory complex • Mildly displaced neck and coracoid fxs treated conservatively – unless associated with clavicle fx Goss TP. Scapular Fractures and Dislocations: Diagnosis and Treatment. J Am Acad Orthop Surg. Jan 1995; 3(1): 22 -33. Curtis RJ. Operative management of children's fractures of the shoulder region. Orthop Clin North Am 1990; 21: 315 -324.
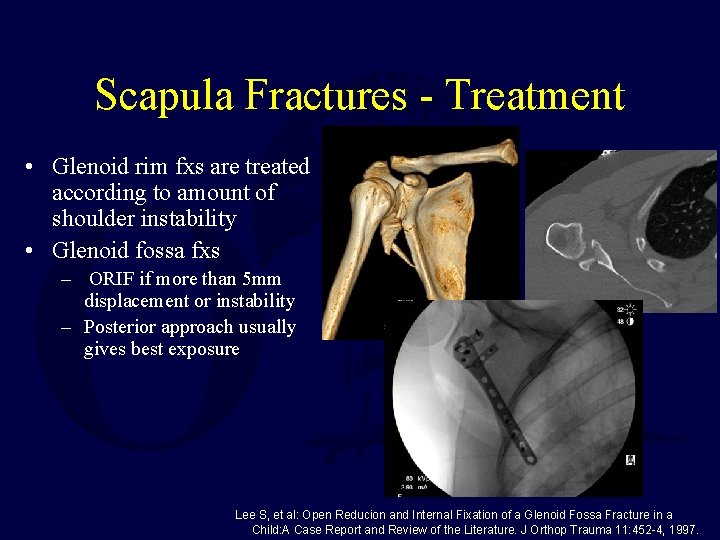
Scapula Fractures - Treatment • Glenoid rim fxs are treated according to amount of shoulder instability • Glenoid fossa fxs – ORIF if more than 5 mm displacement or instability – Posterior approach usually gives best exposure Lee S, et al: Open Reducion and Internal Fixation of a Glenoid Fossa Fracture in a Child: A Case Report and Review of the Literature. J Orthop Trauma 11: 452 -4, 1997.

Glenohumeral Dislocations • Rare in young children – < 2% of all dislocations are in children < 10 yrs – 20% are in children 10 -20 yrs • Most are anterior, as in adults – Frequently associated Hill-Sachs lesion • High rate of recurrent instability in childhood or adolescence (70 -100%)

Traumatic Shoulder Dislocation • Gentle reduction – Pre-post neuro exam • Immobilization for approx 3 weeks • Shoulder rehabilitation • Surgical stabilization /reconstruction reserved for recurrent instability – Wait until skeletally mature, if possible
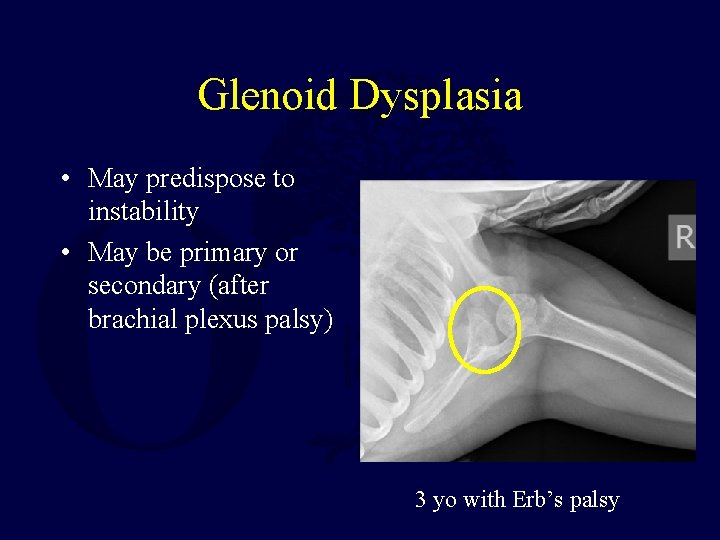
Glenoid Dysplasia • May predispose to instability • May be primary or secondary (after brachial plexus palsy) 3 yo with Erb’s palsy

Atraumatic Instability • Often multiple joint ligamentous laxity • Multidirectional instability usually present • May be voluntary (discourage) • Treat with rotator cuff strengthening
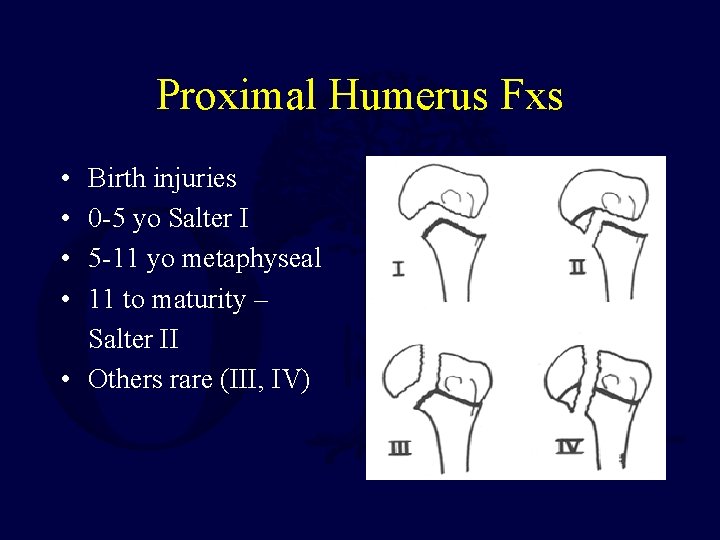
Proximal Humerus Fxs • • Birth injuries 0 -5 yo Salter I 5 -11 yo metaphyseal 11 to maturity – Salter II • Others rare (III, IV)
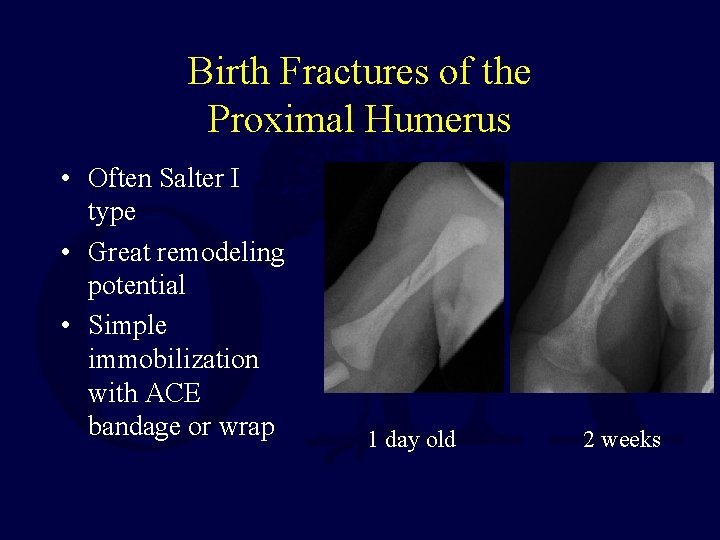
Birth Fractures of the Proximal Humerus • Often Salter I type • Great remodeling potential • Simple immobilization with ACE bandage or wrap 1 day old 2 weeks
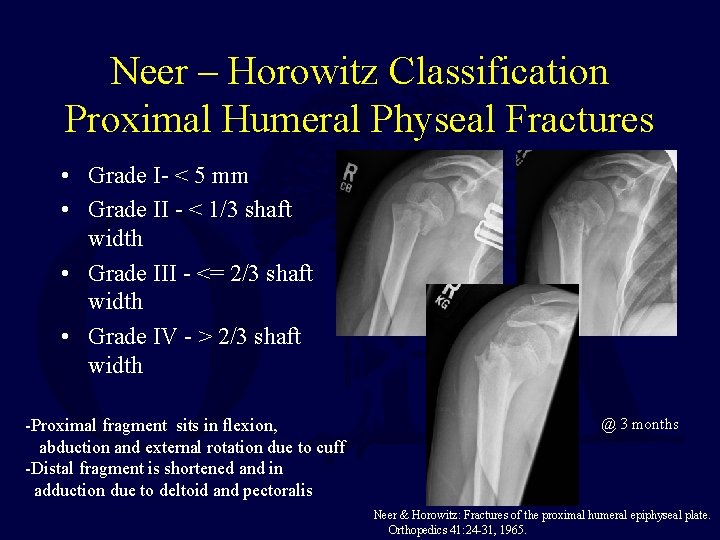
Neer – Horowitz Classification Proximal Humeral Physeal Fractures • Grade I- < 5 mm • Grade II - < 1/3 shaft width • Grade III - <= 2/3 shaft width • Grade IV - > 2/3 shaft width -Proximal fragment sits in flexion, abduction and external rotation due to cuff -Distal fragment is shortened and in adduction due to deltoid and pectoralis @ 3 months Neer & Horowitz: Fractures of the proximal humeral epiphyseal plate. Orthopedics 41: 24 -31, 1965.
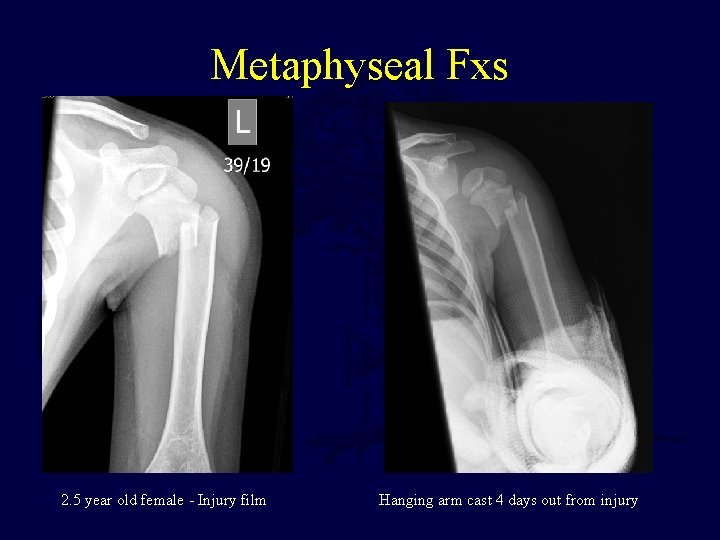
Metaphyseal Fxs 2. 5 year old female - Injury film Hanging arm cast 4 days out from injury
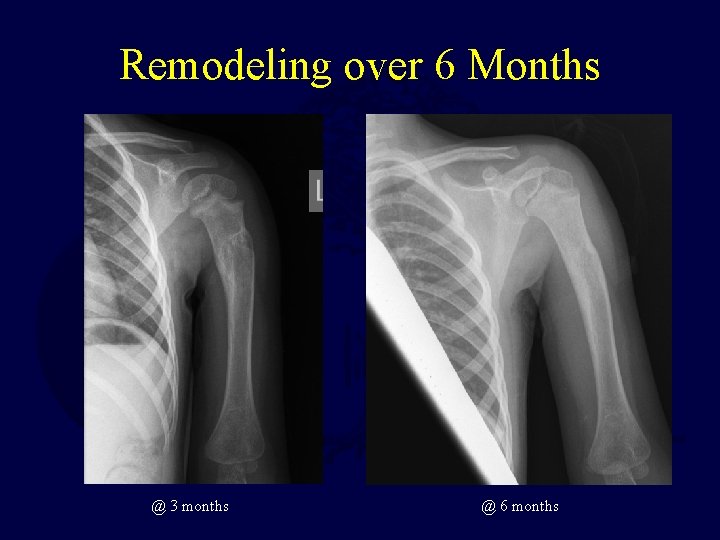
Remodeling over 6 Months @ 3 months @ 6 months

Treatment Principles. Proximal Humerus • Closed treatment for vast majority • If markedly displaced, attempt closed reduction and immobilize – Reduction is unlikely to hold without fixation • Reserve closed vs. open reduction and pinning for fractures with significant displacement – (> Neer II) in older adolescents, recurrent displacement • Open reduction if soft tissue prevents reduction – Deltoid, capsule, long head of biceps

Proximal Humerus – Acceptable Alignment • Great remodeling potential – 80% of humeral length contributed by proximal physis • Shoulder ROM is compensatory • Age dependent? – A few studies state that even older adolescents have acceptable functional outcomes after nonoperative treatment of proximal humerus fxs • Closed reduction not usually successful, nearly impossible to maintain reduced position

Shoulder Immobilization • Closed treatment options: – Coaptation splint – Collar and cuff – Sling and swathe – Hanging arm cast
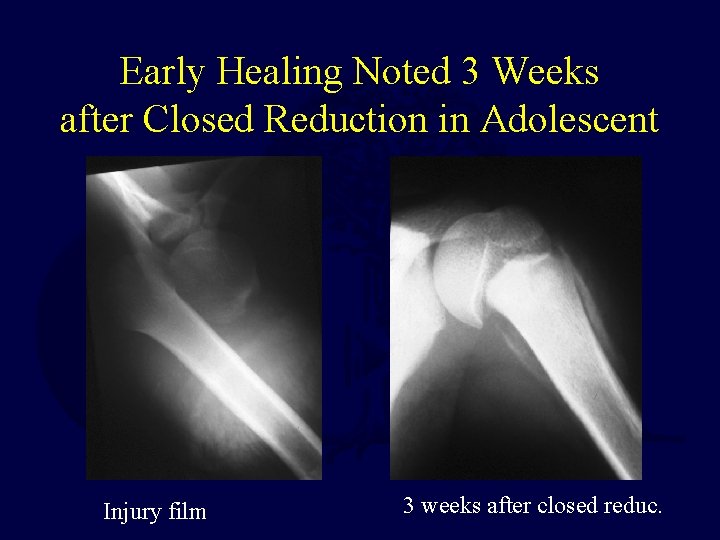
Early Healing Noted 3 Weeks after Closed Reduction in Adolescent Injury film 3 weeks after closed reduc.

Pinning Proximal Humerus • Usually don’t need to • Most recent studies quote high complication rates (pin migration, infection) • Even in older adolescents some remodeling occurs • Few functional deficits • If used, leave pins long and bend outside skin, consider threaded tip pins
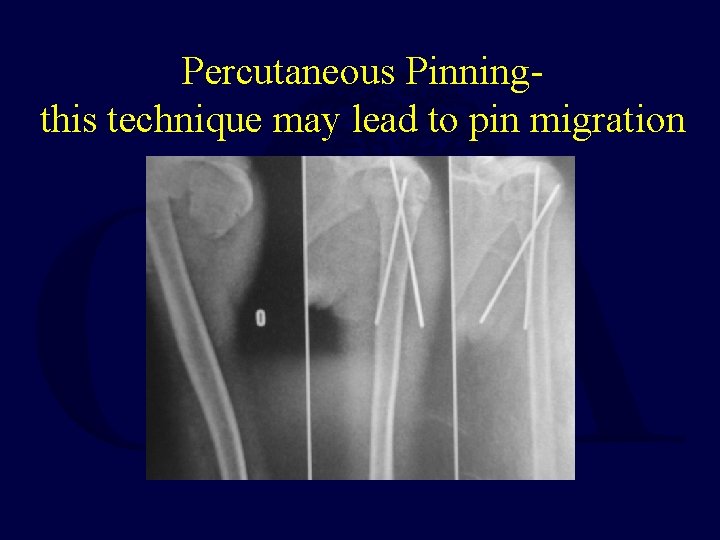
Percutaneous Pinningthis technique may lead to pin migration
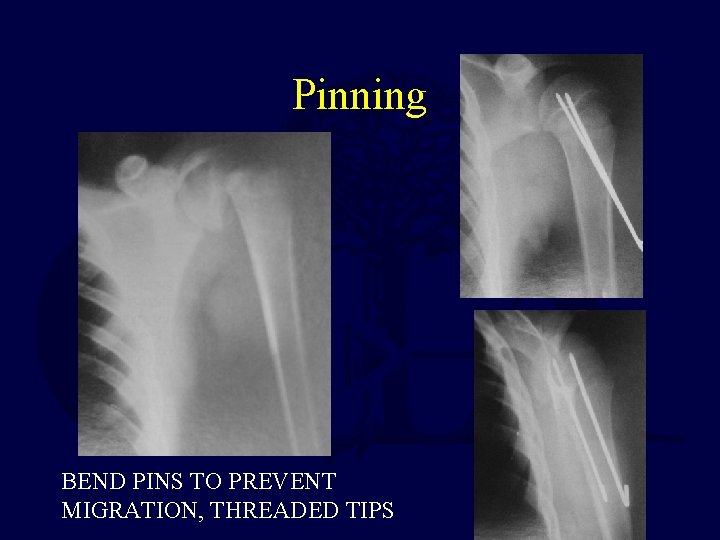
Pinning BEND PINS TO PREVENT MIGRATION, THREADED TIPS
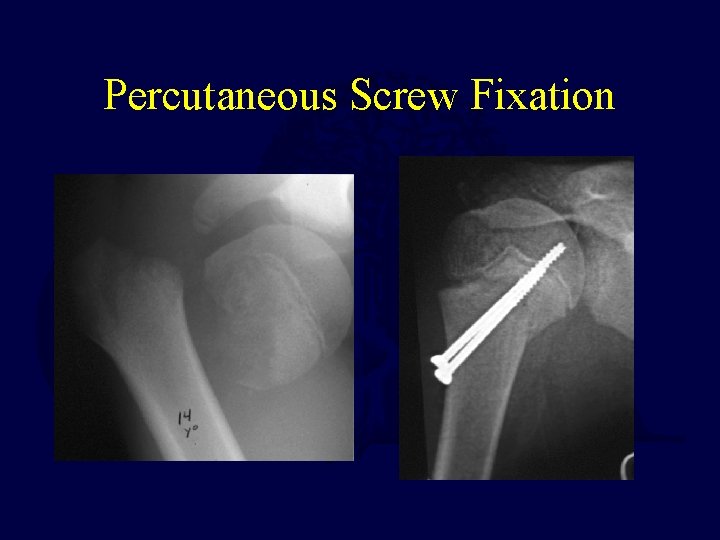
Percutaneous Screw Fixation
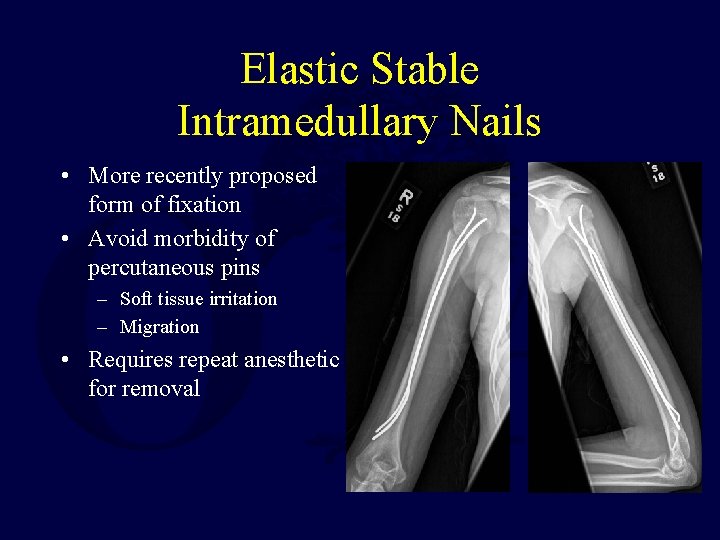
Elastic Stable Intramedullary Nails • More recently proposed form of fixation • Avoid morbidity of percutaneous pins – Soft tissue irritation – Migration • Requires repeat anesthetic for removal
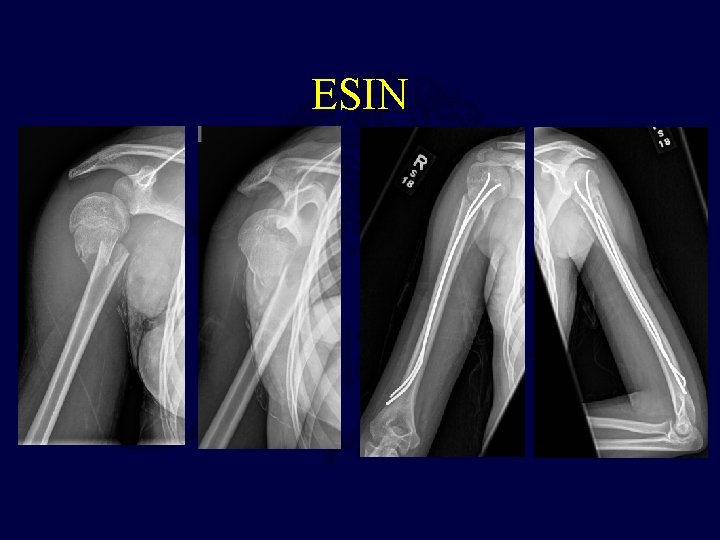
ESIN
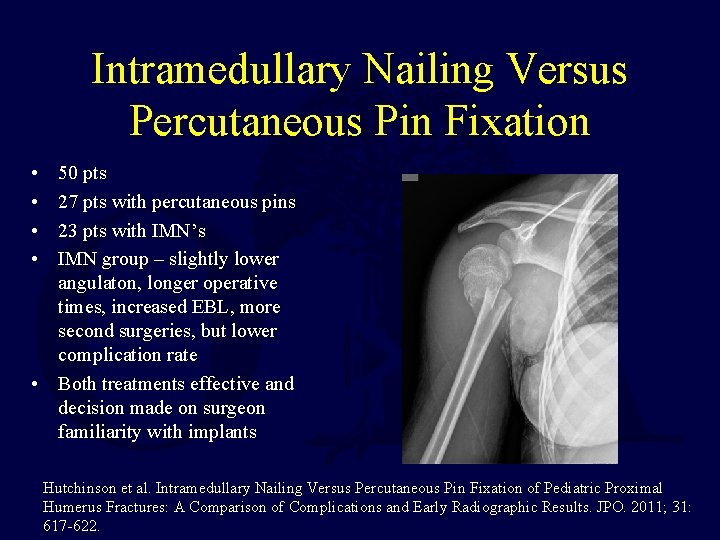
Intramedullary Nailing Versus Percutaneous Pin Fixation • • 50 pts 27 pts with percutaneous pins 23 pts with IMN’s IMN group – slightly lower angulaton, longer operative times, increased EBL, more second surgeries, but lower complication rate • Both treatments effective and decision made on surgeon familiarity with implants Hutchinson et al. Intramedullary Nailing Versus Percutaneous Pin Fixation of Pediatric Proximal Humerus Fractures: A Comparison of Complications and Early Radiographic Results. JPO. 2011; 31: 617 -622.

Complications of Proximal Humerus Fractures • Malunion with loss of shoulder ROM – rarely functionally significant • Shortening – up to 3 -4 cm seemingly well tolerated • Neurologic and vascular compromise less common than in adults

Humeral Shaft Fractures in Children • Neonates – birth trauma • Neonates to age 3 – consider possible nonaccidental trauma • Age 3 -12 – often pathologic fracture through benign bone tumor or cyst • Older than age 12 – treatment like adults
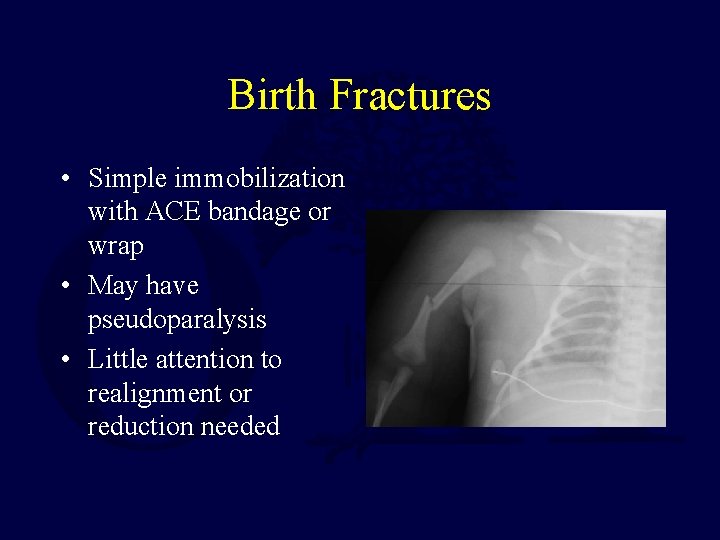
Birth Fractures • Simple immobilization with ACE bandage or wrap • May have pseudoparalysis • Little attention to realignment or reduction needed
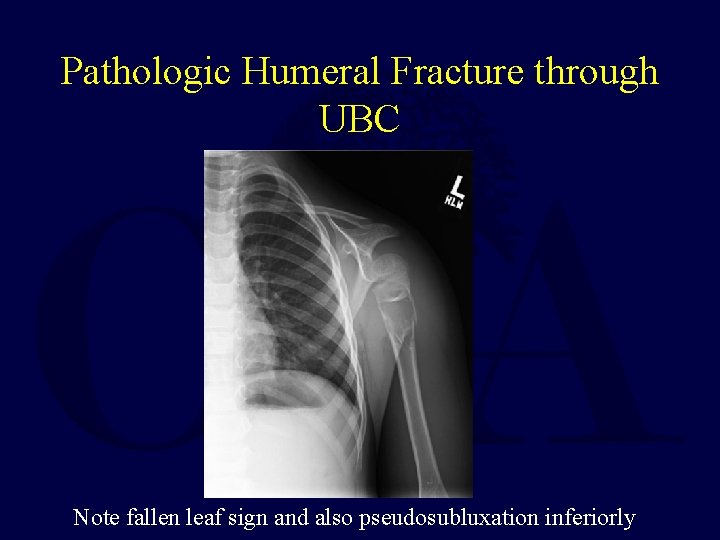
Pathologic Humeral Fracture through UBC Note fallen leaf sign and also pseudosubluxation inferiorly
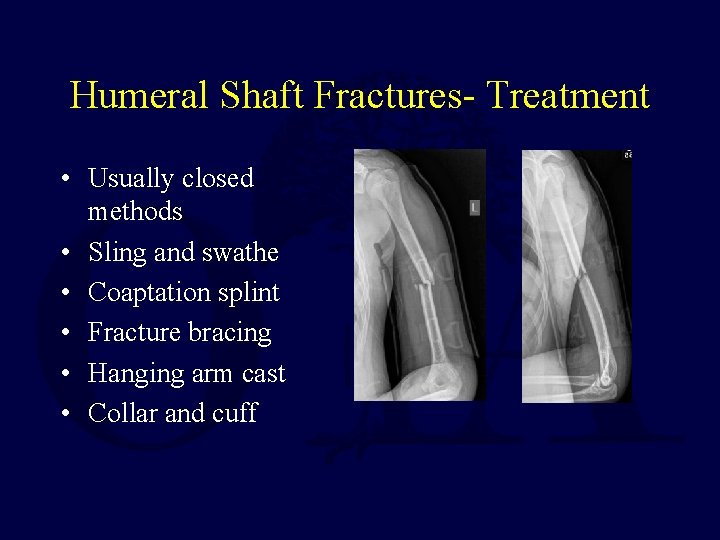
Humeral Shaft Fractures- Treatment • Usually closed methods • Sling and swathe • Coaptation splint • Fracture bracing • Hanging arm cast • Collar and cuff
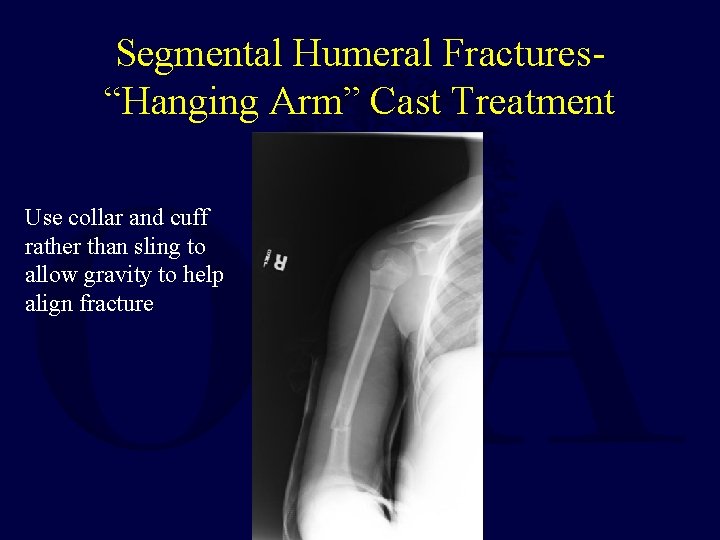
Segmental Humeral Fractures“Hanging Arm” Cast Treatment Use collar and cuff rather than sling to allow gravity to help align fracture
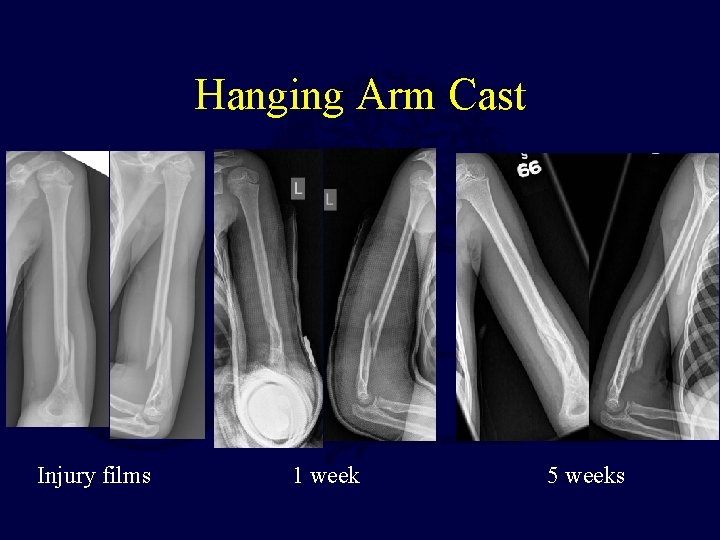
Hanging Arm Cast Injury films 1 week 5 weeks
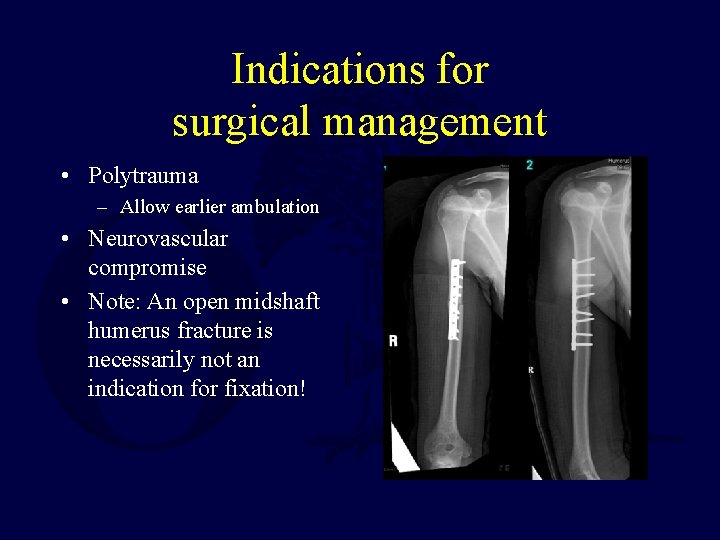
Indications for surgical management • Polytrauma – Allow earlier ambulation • Neurovascular compromise • Note: An open midshaft humerus fracture is necessarily not an indication for fixation!

Humeral Shaft Outcomes • Malunion common, but usually little functional loss • Remodels well • Initial fx shortening may be compensated for by later overgrowth • Nonunion uncommon • Radial nerve palsy less common, if occurs usually neuropraxia

Bibliography • • • • • Bishop & Flatow: Pediatric Shoulder Trauma. CORR 432: 41 -8, 2005. Wirth & Rockwood: Acute and chronic traumatic injuries of the sternoclavicular joint. J Am Acad Orthop Surg 4: 268– 278, 1996. Worman &Leagus: Intrathoracic injury following retrosternal dislocation of the clavicle. J Trauma 7: 416– 423, 1967. Canadian Ortho Trauma Society. Nonop treatment compared with plate fixation of displaced midshaft clavicle fxs. JBJS-Am 89(1): 1 -10, 07. Schnall et al: Congenital pseudarthrosis of the clavicle: a review of the literature and surgical results of six cases. J Pediatr Orthop 8: 316– 21, 1988. Kubiak & Slongo: Operative treatment of clavicle fractures in children. J Pediatr Orthop 22: 736– 9, 2002. Endrizzi et al: Nonunion of the clavicle treated with plate fixation. J Shoulder Elbow Surg 17: 951 -3, 2008. Tossy JD, Mead NC, Sigmond HM: Acromioclavicular separation: useful and practical classification for treatment. Clin Orthop 28: 111 -9, 1963. Rockwood CA, Williams GR, Youg DC: Disorders of the acromioclavicular joint. In: Rockwood CA, Masten FA II, editors. The shoulder. Philadelphia: Saunders; 1998. p. 483 -553. Ideberg R: Unusual glenoid fractures. Acta Orthop Scand 58: 191 -2, 1987. Goss TP: Fractures of the glenoid cavity. J Bone Joint Surg [Am] 74: 299 -305, 1992. Goss TP. Scapular Fractures and Dislocations: Diagnosis and Treatment. J Am Acad Orthop Surg. Jan 1995; 3(1): 22 -33. Curtis RJ: Operative management of children's fractures of the shoulder region. Orthop Clin North Am 1990; 21: 315 -324. Lee S, et al: Open Reducion and Internal Fixation of a Glenoid Fossa Fracture in a Child: A Case Report and Review of the Literature. J Orthop Trauma 11: 452 -4, 1997. Neer & Horowitz: Fractures of the proximal humeral epiphyseal plate. Orthopedics 41: 24 -31, 1965. Dobbs, et al: Severely displaced proximal humeral epiphyseal fractures. J Pediatr Orthop 23: 208 -15, 2003. Fernandez et al: Treatment of severely displaced proximal humerus fractures in children with retrograde ESIN. Injury 39: 1453 -9, 2008. Vander Have et al: Operative versus nonoperative treatment of midshaft clavicle fractures in adolescents. J Pediatric Ortho 2010; 30: 307 -311. Schulz et al: Functional and radiographic outcomes of nonoperative treatment of displaced adolescent clavicle fractures. JBJS Am 2013; 95: 115965. Hutchinson et al. Intramedullary nailing versus percutaneous pin fixation of pediatric proximal humerus fractures: A comparison of complications and early radiographic results. J Pediatric Ortho 2011; 31: 617 -622. If you would like to volunteer as an author for the Resident Slide Project or recommend updates to any of the following slides, please send an e-mail to ota@aaos. org E-mail OTA about Questions/Comments Return to Pediatrics Index
- Slides: 61