Foundations of Interprofessional Collaboration FIPC An Introduction to

Foundations of Interprofessional Collaboration (FIPC): An Introduction to Team. STEPPS® LEVEL 3 Overview of Clinical Management of Anaphylaxis for Pharmacy Students

Anaphylaxis Definition “A serious allergic reaction that is rapid in onset and may cause death. ” National Institute of Allergy and Infectious Disease and the Food Allergy and Anaphylaxis Network
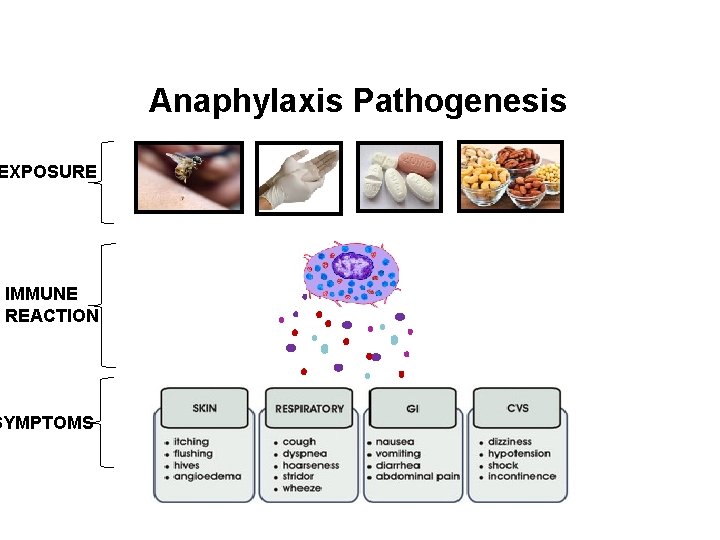
Anaphylaxis Pathogenesis EXPOSURE IMMUNE REACTION SYMPTOMS
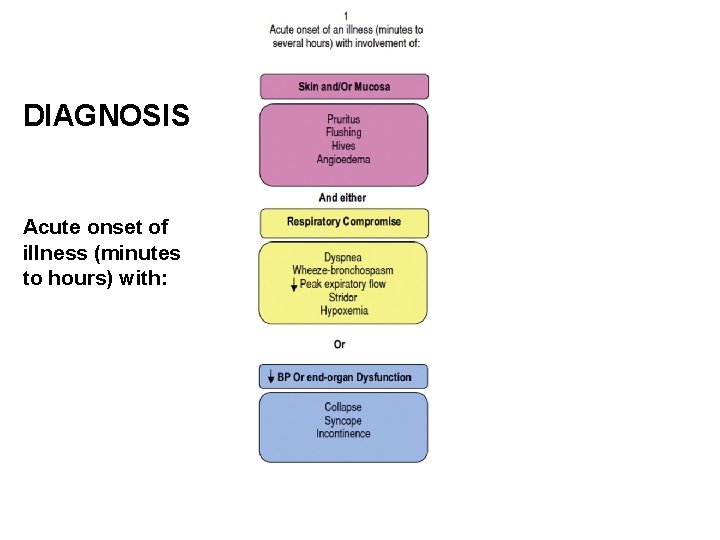
DIAGNOSIS Acute onset of illness (minutes to hours) with:
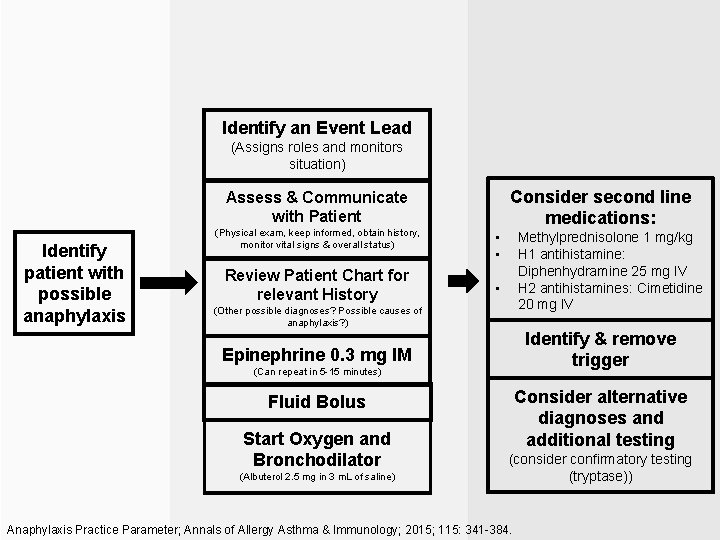
Identify an Event Lead (Assigns roles and monitors situation) Consider second line medications: Assess & Communicate with Patient Identify patient with possible anaphylaxis (Physical exam, keep informed, obtain history, monitor vital signs & overall status) Review Patient Chart for relevant History • • Methylprednisolone 1 mg/kg H 1 antihistamine: Diphenhydramine 25 mg IV H 2 antihistamines: Cimetidine 20 mg IV • (Other possible diagnoses? Possible causes of anaphylaxis? ) Identify & remove trigger Epinephrine 0. 3 mg IM (Can repeat in 5 -15 minutes) Consider alternative diagnoses and additional testing Fluid Bolus Start Oxygen and Bronchodilator (Albuterol 2. 5 mg in 3 m. L of saline) (consider confirmatory testing (tryptase)) Anaphylaxis Practice Parameter; Annals of Allergy Asthma & Immunology; 2015; 115: 341 -384.

Inpatient Use of Epinephrine for Anaphylaxis • Intramuscular Preferred – Improved absorption in mid-outer thigh • Exact dosing for adults and children – 0. 01 mg/kg IM (max dose of 0. 5 mg at once) – Guidelines recommend 0. 3 mg IM for adults and re-assess • Caution: Epinephrine dilutions cause of many medication errors- double check! – Use 1 mg/ml (or labeled 1: 1000) concentration • Reassess in 5 -15 minutes, may repeat if needed – Tip: Note time administered and alert when repeat dose could be given if needed • No Contraindications to Epi in anaphylaxis! – Monitoring, Drug Interactions, ADRs

Additional Inpatient Medications for Anaphylaxis • Bronchodilator – Albuterol 2. 5 mg in 3 m. L normal saline – Nebulized • Corticosteroids – Limited evidence to support use but often given to prevent second phase of anaphylaxis – Onset 4 -6 hours – Methylprednisolone 1 mg/kg/day IV push • Antihistamine (H 1 and H 2 Antagonists) – Limited evidence to support use but often administered to treat urticaria – Diphenhydramine 25 mg IV push – Famotidine 20 mg IV push

Drug-Induced Anaphylaxis • All medications used immediately preceding anaphylaxis should be reviewed (any medicine could cause it)! • Common drugs associated with Type 1 allergic drug reactions include: – Beta-lactams – Quinolones – Neuromuscular blocking agents – Platinum chemotherapy agents – Foreign proteins (e. g. , rituximab)

Role of Pharmacist in Rapid Response Team • Collect information (or provide input for team leader) related to medication therapy • Assist team in assessing the patient and provide assessments related to medication therapy • Provide therapeutic recommendations (e. g. , therapy options, dosing, calculations, monitoring) • Prepare medications • Provide mutual support to other members of the team as needed
- Slides: 9