Forensic Toxicology OConnor Role of Forensic Toxicology Forensic



















- Slides: 22

Forensic Toxicology O’Connor

Role of Forensic Toxicology • Forensic toxicologists detect & identify drugs & poisons in body fluids, tissues, & organs in matters that pertain to violations of criminal laws. • Ethyl alcohol is the most heavily abused drug in Western countries.

Ethyl Alcohol • All evidence shows ethyl alcohol (which is legal if over 21) is the most heavily abused drug, causing 40% of all traffic deaths in the US. • Nearly 17, 500 fatalities/year are alcohol related & over 2 million injuries requiring hospital care.

Toxicology • Detect and isolate drugs in the body to determine their influence on human behavior. • Knowing how the body metabolizes alcohol is key to understanding its effects. • Knowledge made development of instruments to measure presence & concentration of alcohol.

Metabolism of Alcohol • Metabolism- body breaks down one chemical into chemicals that are easier for it to eliminate. • Three basic steps: • 1. Absorption • 2. distribution • 3. elimination

Metabolism of Alcohol • Step 1 Absorption • Consumed as a colorless liquid in a mixture • Appears in blood w/in minutes • Increases in concentration as it is absorbed by stomach & sm. intestines into bloodstream • Absorption to the blood allows the alcohol to be carried to all parts of the body

Distribution • The body is 2/3 water and the alcohol gets distributed evenly through the bodies liquid parts. • The timeframe for rate of absorption/distribution: • Total time taken to consume • Amount consumed • Quantity & type of food present in stomach • Size of individual consuming total volume of liquid present in the body)

Elimination • As the alcohol is circulated by bloodstream, the body begins to eliminate it by two processes, oxidation & excretion. • 95 -98% is oxidized to CO 2 & H 2 O starting in the liver • In the presence of enzyme alcohol dehydrogenase it is converted into acetaldehyde and then to acetic acid which is broken down throughout the body to CO 2 & H 2 O • Remaining 2 -5% is excreted unchanged in the breath, urine & perspiration (in proportion to level in blood stream)

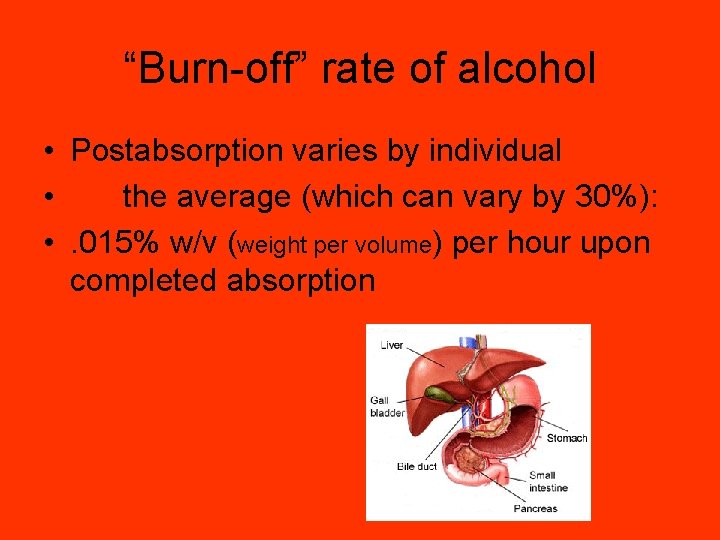
“Burn-off” rate of alcohol • Postabsorption varies by individual • the average (which can vary by 30%): • . 015% w/v (weight per volume) per hour upon completed absorption

BAC- blood alcohol Concentration • Best way to determine- remove a portion of the brain & analyze for alcohol content • (problematic for the living) • Blood alcohol levels are the legally accepted standard for measurement in the living. (postmortem- brain, cerebrospinal fluid, or vitreous humor is tested)

Taking Measurements • Measure concentration in Blood test • Measure alcohol content in breath

Henry’s Law is applied: • When a volatile chemical is dissolved in a liquid & is brought to equilibrium with air, there is a fixed ratio between the concentration of the volatile compound in air & its concentration in the liquid & this ratio is constant for a given temperature. • Breathe leaves the mouth at an ave. of 34°C, the ratio of alcohol in the blood; to alcohol in the aveolar air is approximately 2, 100 to 1. (1 ml of blood same amt. alcohol as 2, 100 ml of breath)

Testing for Intoxication • Hundreds of thousands of motorists tested annually. • Breathe testing, quick- convenient & reliable • (early in absorption process- breathe test will show higher levels than blood tests; but match effects on the brain)

Breathalyzer • • Developed in 1954 by R. F. Borkenstein modified over years- basic principles still apply. Breathalyzer replaced chemical free devises: Infrared & fuel-cell-based devices controlled by microprocessors. Process: Start with field sobriety test Nothing taken orally for 15 min. prior to test. Take two test samples minutes apart

Field Sobriety test • Used to determine an individuals physical impairment & to justify further testing • Series of psychophysical tests: • Horizontal-gaze nystagmus (follow pen light w/ eyes) • walk & turn • One-leg stand

Higher BAC: Higher physical impairment • . 10% BAC = eye jerk before eye has moved 45° • Other drugs can trigger this effect, phencyclidine, barbituates, & other depressants) • Walk/turn & one-leg stand are divided attention tasks. Requiring ability to understand & carry out more than 2 instructions: this ability is affected by blood-alcohol levels.

Blood Analysis • Forensic toxicologists must devise an analytical scheme to detect, isolate, & identify toxic drug substances extracted from biological fluid, tissues, and organs.

• A screening test gives quick insight into the likelihood that a specimen contains a drug substance. • Positive results arising from a screening test are tentative at best and must be verified with a confirmation test.

• The most widely used screening tests are thinlayer chromatography, gas chromatography, and immunoassay. • Gas chromotography/mass spectrometry is generally accepted as the confirmation test of choice.

• Once a drug is extracted & identified, a toxicologist may be required to judge the drug’s effect on an individual’s natural performance or physical state. • This is different depending on whether the individual is a live or deceased.

• Field sobriety results come into play for the living. (much easier to use in court since video camera’s were added to police vehicles) • Deceased, requires the ME to determine cause of death, for this the ME and toxicologist work together.

Alcohol Intoxication vs Drug Induced Intoxication • Alcohol intoxication is widely recognized, police are highly trained for & the courts are accustomed to the effects. • Drug Induced Intoxication is harder to recognize. In the 1970 s they developed & tested a series of clinical & psychophysical examinations that a trained police officer could use. The program is now used nationwide to train drug recognition experts (DRE); a 3 -5 month training program is required to certify.