Foreign Bodies n n n Foreign body ingestion

Foreign Bodies n n n Foreign body ingestion Foreign body aspiration Toddlers n n Oral exploration Lack posterior dentition Easy distractibility Cognitive development (edible? )

Foreign Body Ingestion n n n Coins – 75% Bones (mainly fish bone) Meat Vegetable matter False teeth Less than 24 hours in most

Foreign Body Ingestion n n Parental suspicion Symptoms n n Physical exam n n Choking, coughing, dysphagia, odynophagia Drooling, refuses p. o. , fussy child Respiratory compromise

Foreign Body Ingestion Common locations n n n n Tonsils Vallecula epiglottica Pyriform sinuses Cricopharyngeus Aorta/left mainstem bronchus Gastroesophageal junction
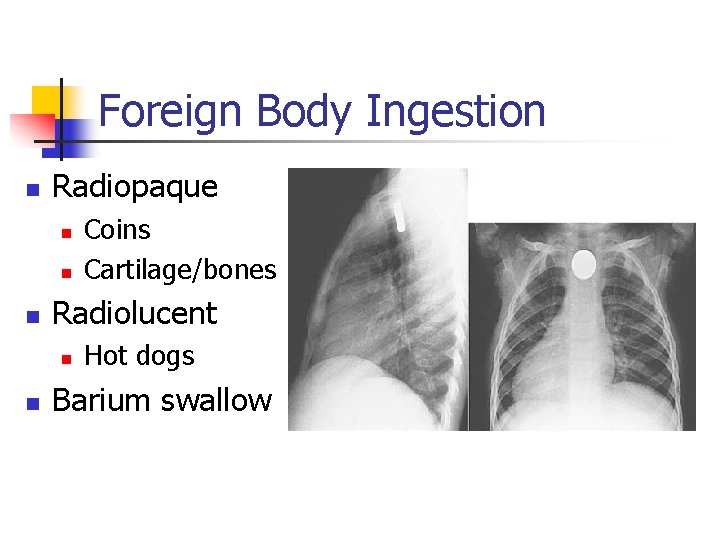
Foreign Body Ingestion n Radiopaque n n n Radiolucent n n Coins Cartilage/bones Hot dogs Barium swallow
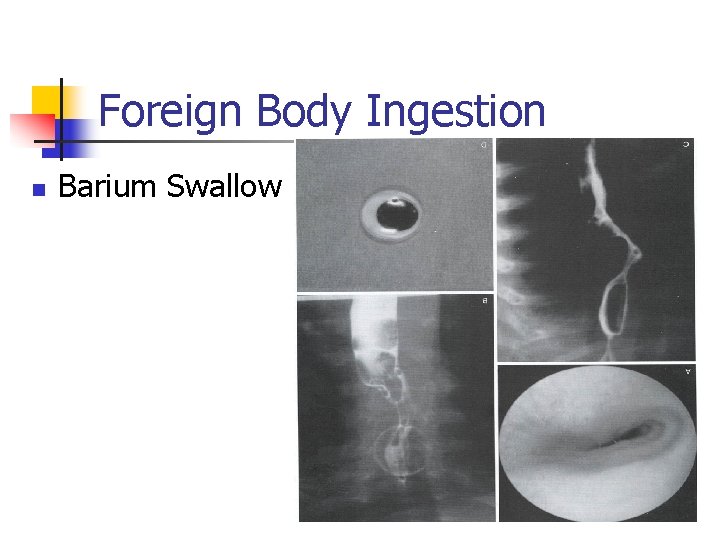
Foreign Body Ingestion n Barium Swallow

Foreign Body Ingestion n Observation n Recent ingestion Blunt object Endoscopy n n n Complete obstruction Airway compromise Impacted Caustics Anomalies

Foreign Body Ingestion n Removal n n General anesthesia Intubated Esophagoscopy Examine for ulceration/perforation

Foreign Body Ingestion n Disc batteries n n Emergency Na. OH, KOH, mercury n n n 1 hour – mucosal damage 2 to 4 hours – muscular layers 8 to 12 hours – perforation Esophagoscopy Observation for gastric location for 4 -7 days Laparotomy for bowel perforation

Foreign Body Ingestion n Complication Perforation of esophagus Subcutaneous/mediastinal emphysema Mediastinal abscess Break of the aorta Esophageal fistula/stricture

n Perforation n n Tachycardia Tachypnea Fever Chest pain

Foreign Body Ingestion n Balloon Catheter Extraction n Effective in 90% Endoscopy for failures Complications n n Emesis Epistaxis Laryngospasm Airway compromise
Foreign Body Ingestion n Postoperative management Fasting >7 d for perforation

Foreign Body Aspiration n Vegetable matter in 70 -80% n n Peanuts & other nuts (35%) Carrot pieces, beans, sunflower & watermelon seeds Metallic objects Plastic objects

Foreign Body Aspiration n Bronchi – 80 -90% n Right mainstem most common n n Carina Less divergent angle Greater diameter Trachea Larynx n n Larger objects, irregular edges Conforming objects

Foreign Body Aspiration n History n n n n Choking Gagging Wheezing Hoarseness Dysphonia Can mimic asthma, croup, pneumonia “A positive history must never be ignored, while a negative history may be misleading”

Foreign Body Aspiration n n Choking episode with coughing, gagging or wheezing Asymptomatic interval n n 20 -50% not detected for one week Inflammation and Complications n n n n Cough Emphysema Obstructive atelectasis Hemoptysis Pneumonia Lung abscess Fever

Foreign Body Aspiration n Physical exam n Larynx/cervical trachea n n Intrathoracic trachea n n Inspiratory or biphasic stridor Prolonged expiratory wheeze Bronchi n n Unequal breath sounds Diagnostic triad - <50% n n Unilateral wheeze Cough Ipsilaterally diminished breath sounds Fiberoptic laryngoscopy

Foreign Body Aspiration n Radiography n n n PA & lateral views of chest & neck Inspiration & expiration Lateral decubitus views Airway fluoroscopy 25% have normal radiography
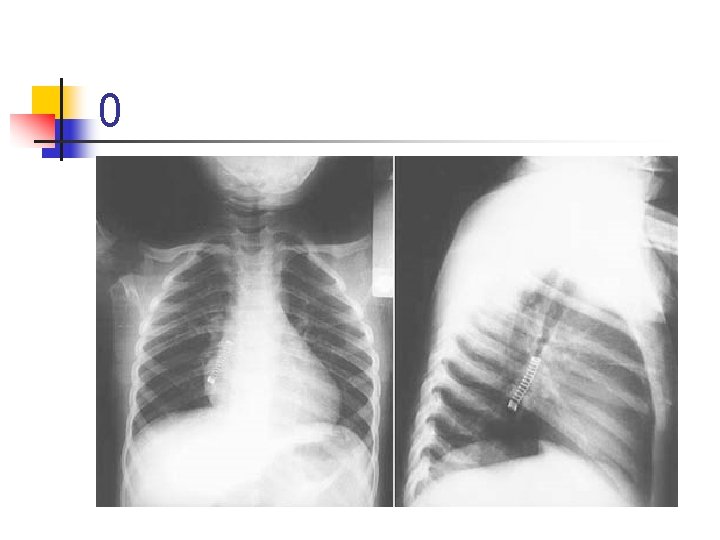
0

Foreign Body Aspiration
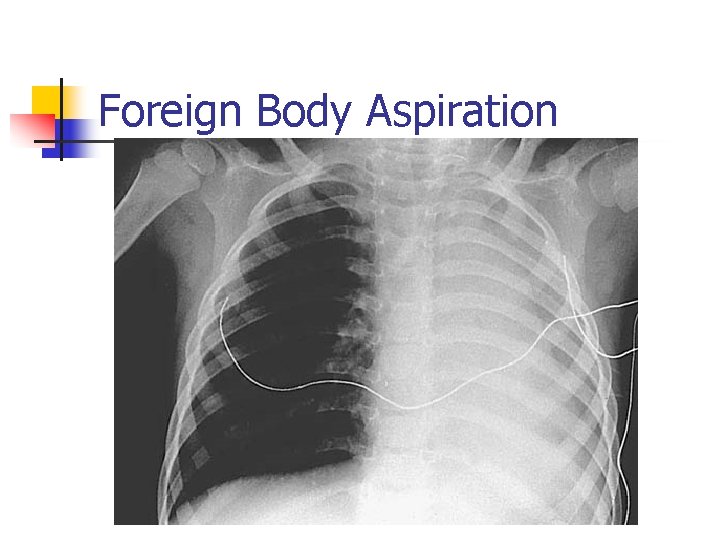
Foreign Body Aspiration

Foreign Body Aspiration
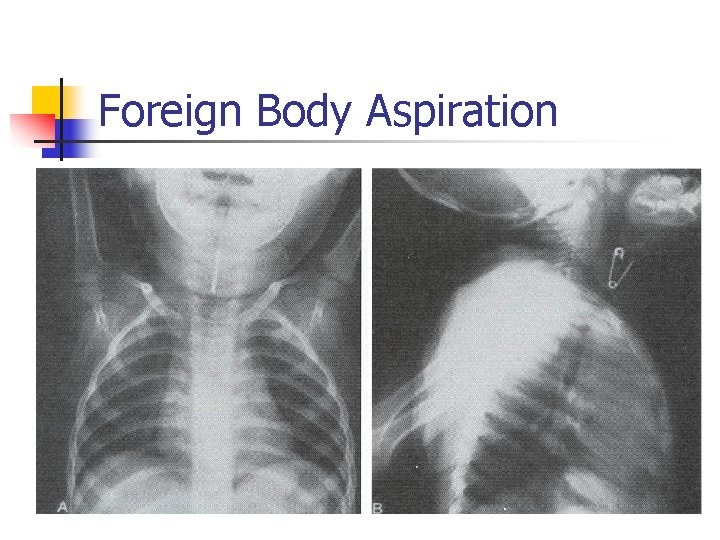
Foreign Body Aspiration

Foreign Body Aspiration n n Goal of treatment Prompt endoscopic removal under conditions of maximal safety and minimal trauma

Foreign Body Aspiration n Usually NOT A DIRE EMERGENCY n n Trained personnel Instruments assembled and checked Await for emptying of stomach Find duplicate FB to test instruments and techniques
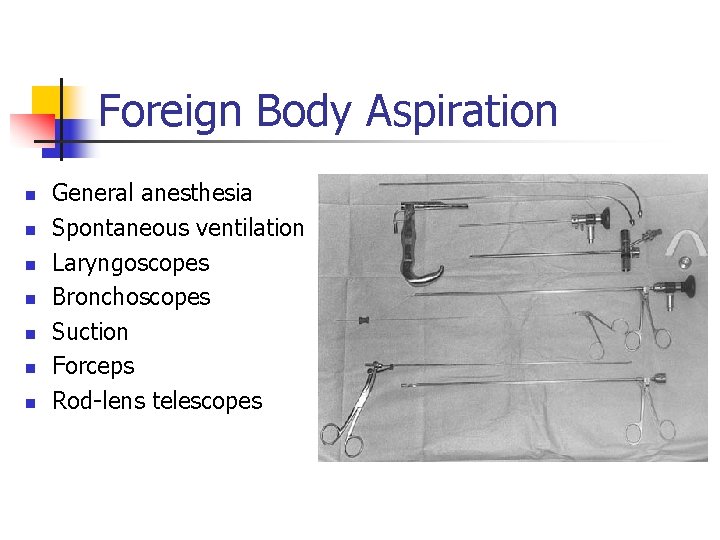
Foreign Body Aspiration n n n General anesthesia Spontaneous ventilation Laryngoscopes Bronchoscopes Suction Forceps Rod-lens telescopes

Foreign Body Aspiration n n Ready to assume airway during induction Laryngoscopy n n Topical anesthesia Examination of upper airway Atraumatic insertion of bronchoscope Bronchoscopy n Attached to ventilating circuit

Foreign Body Aspiration n Bronchoscopy n n Suction opposite bronchus Advance to foreign body Atraumatically grasp foreign body Repeat bronchoscopy n n Suction bronchus Multiple foreign bodies in 5 -19% Remove granulation tissue Topical vasoconstrictors for bleeding

Foreign Body Aspiration n Slipped foreign body n n Push back into bronchus Sharp foreign body n Advance bronchoscope over FB

Foreign Body Aspiration n Complications n Pneumonia n n Atelectasis n n n Antibiotics, physiotherapy Expectant management, physiotherapy Pneumothorax Pneumomediastinum

Caustic Ingestion n n 5, 000 lye ingestions in children < 5 years Most in kitchen High family stress Suicide attempts in adults

Caustic Ingestion n Alkalis – p. H > 7 n n Acids – p. H < 7 n n Liquefaction necrosis Coagulation necrosis Bleaches – p. H = 7 n Irritants

Caustic Ingestion n n Amount Type Concentration Time of contact

Caustic Ingestion n n Grade 1 - superficial injury Grade 2 – transmucosal injury Grade 3 – transmural injury Circumferential vs. localized injury

Caustic Ingestion n Acute phase(1 -2 w) Local General Latent period(1 -2 w) Stricture formation

Caustic Ingestion n n Initial management requires diagnosis History Obtain container Poison control Emesis?

Caustic Ingestion n Laryngeal injury? n n Severe injury? n n Hoarseness, stridor, dyspnea Odynophagia, drooling, refusal of food Perforation? n Chest pain, abdominal pain, rigidity

Caustic Ingestion n Neighboring injury n n Oropharynx n n Examination of lips, chin, hands, chest, clothing Suction, lighting, restraint Larynx/hypopharynx n Flexible fiberoptic scope, mirror

Caustic Ingestion n Radiologic exam n n Chest & neck radiographs Barium swallow n Will not reveal 1 st and 2 nd degree injuries

Caustic Ingestion n n Esophagoscopy in virtually all patients at 24 -48 hours post-ingestion < 24 hours – underestimation of injury > 48 -72 hours with risk of iatrogenic perforation – barium swallow Rigid vs. flexible debatable Endoscopy to upper limit of severe burn

Caustic Ingestion n Bleach ingestion n n 5 -6% sodium hypochlorite Produce ulceration Normal oropharynx – barium swallow Burned oropharynx - esophagoscopy

Caustic Ingestion n Goal of treatment Preventing permanent injury or stricture in esophagus n

Caustic Ingestion n Dilution n n Neutralizing substances contraindicated n n Water or milk Exothermic reaction Analgesics

Caustic Ingestion n Antibiotics n Pro n n n Con n n Decrease bacterial counts Reduction in granulation Influx of gram negatives Mask infection No reduction in strictures Ampicillin – 50 mg/kg/day

Caustic Ingestion n n Steroids Prednisone – 2 mg/kg/day x 21 days then taper Most effective for grade 2 injuries Strictures easier to manage

Caustic Ingestion n Prevention of acid reflux n n H 2 blockers Proton pump inhibitors

Caustic Ingestion n Nasogastric tube Esophageal stent Prevent adherence of anterior and posterior walls of esophagus

Caustic Ingestion n n Strictures develop in 10 -15% Dilation n n Prograde Retrograde Balloon catheters Esophageal replacement

Caustic Ingestion n Prograde dilation n Jackson silk-woven bougies Hurst dilators Maloney dilators

Caustic Ingestion n Retrograde dilation n n Safer? Tucker dilators

Caustic Ingestion n n Gruntzig balloon catheter Radial direction of dilation
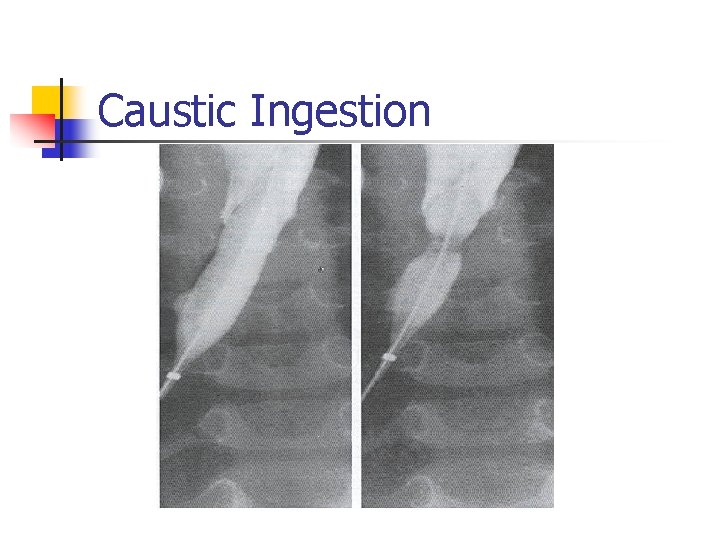
Caustic Ingestion

Caustic Ingestion n n Esophageal replacement Colonic interposition Jejunal interposition Gastric pull-ups

Caustic Ingestion n n Esophageal carcinoma 1, 000 x increased risk 13 to 71 years after injury Better prognosis than usual esophageal cancer

Caustic Ingestion
- Slides: 56